Comparison of the Percentage of Voids in the Canal Filling of a Calcium Silicate-Based Sealer and Gutta Percha Cones Using Two Obturation Techniques
Abstract
:1. Introduction
2. Results
3. Discussion
4. Materials and Methods
4.1. Preparation of Plastic Tooth Samples
4.2. Preparation of Plastic Tooth Samples
Obturation of the Plastic Tooth Samples
4.3. Micro-CT Imaging and Analysis
4.4. Statistical Analysis
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ray, H.A.; Trope, M. Periapical status of endodontically treated teeth in relation to the technical quality of the root filling and the coronal restoration. Int. Endod. J. 1995, 28, 12–18. [Google Scholar] [CrossRef] [PubMed]
- Siqueira, J.F., Jr.; Rocas, I.N.; Alves, F.R.; Campos, L.C. Periradicular status related to the quality of coronal restorations and root canal fillings in a Brazilian population. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2005, 100, 369–374. [Google Scholar] [CrossRef] [PubMed]
- Hommez, G.; Coppens, C.; De Moor, R. Periapical health related to the quality of coronal restorations and root fillings. Int. Endod. J. 2002, 35, 680–689. [Google Scholar] [CrossRef] [PubMed]
- Vertucci, F.J. Root canal anatomy of the human permanent teeth. Oral Surg. Oral Med. Oral Pathol. 1984, 58, 589–599. [Google Scholar] [CrossRef]
- De Pablo, O.V.; Estevez, R.; Peix Sanchez, M.; Heilborn, C.; Cohenca, N. Root anatomy and canal configuration of the permanent mandibular first molar: A systematic review. J. Endod. 2010, 36, 1919–1931. [Google Scholar] [CrossRef] [PubMed]
- Jho, W.; Park, J.W.; Kim, E.; Song, M.; Seo, D.G.; Yang, D.K.; Shin, S.J. Comparison of root canal filling quality by mineral trioxide aggregate and gutta percha cones/AH plus sealer. Dent. Mater. J. 2016, 35, 644–650. [Google Scholar] [CrossRef] [PubMed]
- Iglecias, E.F.; Freire, L.G.; de Miranda Candeiro, G.T.; Dos Santos, M.; Antoniazzi, J.H.; Gavini, G. Presence of voids after continuous wave of condensation and single-cone obturation in mandibular molars: A micro-computed tomography analysis. J. Endod. 2017, 43, 638–642. [Google Scholar] [CrossRef] [PubMed]
- Jeong, J.W.; DeGraft-Johnson, A.; Dorn, S.O.; Di Fiore, P.M. Dentinal tubule penetration of a calcium silicate-based root canal sealer with different obturation methods. J. Endod. 2017, 43, 633–637. [Google Scholar] [CrossRef] [PubMed]
- Silva Almeida, L.H.; Moraes, R.R.; Morgental, R.D.; Papper, F.G. Are premixed calcium silicate-based endodontic sealers comparable to conventional materials? A systematic review of in vitro studies. J. Endod. 2017, 43, 527–535. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Li, Z.; Peng, B. Ex vivo cytotoxicity of a new calcium silicate–based canal filling material. Int. Endod. J. 2010, 43, 769–774. [Google Scholar] [CrossRef] [PubMed]
- Zhou, H.M.; Shen, Y.; Zheng, W.; Li, L.; Zheng, Y.F.; Haapasalo, M. Physical properties of 5 root canal sealers. J. Endod. 2013, 39, 1281–1286. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Li, Z.; Peng, B. Assessment of a new root canal sealer’s apical sealing ability. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2009, 107, e79–e82. [Google Scholar] [CrossRef] [PubMed]
- Min, K.S. Clinical use of a premixed MTA-based root canal sealer. J. Korean Soc. Dent. Mater. 2016, 43, 4–5. [Google Scholar]
- Wu, M.K.; Ozok, A.R.; Wesselink, P.R. Sealer distribution in root canals obturated by three techniques. Int. Endod. J. 2000, 33, 340–345. [Google Scholar] [CrossRef] [PubMed]
- Maruchi. Maruchi Products: Endoseal MTA. Wonju, South Korea: Maruchi. Available online: http://www.endocem.com/maruchi/c_eng_product/index.php?nia=endoseal_mta (accessed on 13 July 2017).
- Capar, I.D.; Saygili, G.; Ergun, H.; Gok, T.; Arslan, H.; Ertas, H. Effects of root canal preparation, various filling techniques and retreatment after filling on vertical root fracture and crack formation. Dent. Traumatol. 2015, 31, 302–307. [Google Scholar] [CrossRef] [PubMed]
- Sagsen, B.; Ustun, Y.; Demirbuga, S.; Pala, K. Push-out bond strength of two new calcium silicate-based endodontic sealers to root canal dentine. Int. Endod. J. 2011, 44, 1088–1091. [Google Scholar] [CrossRef] [PubMed]
- Gandolfi, M.G.; Parrilli, A.P.; Fini, M.; Prati, C.; Dummer, P.M. 3D micro-CT analysis of the interface voids associated with Thermafil root fillings used with AH Plus or a flowable MTA sealer. Int. Endod. J. 2013, 46, 253–263. [Google Scholar] [CrossRef] [PubMed]
- El Sayed, M.A.; Taleb, A.A.; Balbahaith, M.S. Sealing ability of three single-cone obturation systems: An in vitro glucose leakage study. J. Conserv. Dent. 2013, 16, 489–493. [Google Scholar] [CrossRef] [PubMed]
- Jung, M.; Lommel, D.; Klimek, J. The imaging of root canal obturation using micro-CT. Int. Endod. J. 2005, 38, 617–626. [Google Scholar] [CrossRef] [PubMed]
- Wolf, M.; Kupper, K.; Reimann, S.; Beimann, S.; Bourauel, C.; Frentzen, M. 3D analyses of interface voids in root canals filled with different sealer materials in combination with warm gutta-percha technique. Clin. Oral Investig. 2014, 18, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Hammad, M.; Qualtrough, A.; Silikas, N. Evaluation of root canal obturation: A three-dimensional in vitro study. J. Endod. 2009, 35, 541–544. [Google Scholar] [CrossRef] [PubMed]
- Somma, F.; Cretella, G.; Carotenuto, M.; Pecci, R.; Bedini, R.; De Biasi, M.; Angerame, D. Quality of thermoplasticized and single point root fillings assessed by micro-computed tomography. Int. Endod. J. 2011, 44, 362–369. [Google Scholar] [CrossRef] [PubMed]
- Saunders, W.P.; Saunders, E.M. Coronal leakage as a cause of failure in root-canal therapy: A review. Endod. Dent. Traumatol. 1994, 10, 105–108. [Google Scholar] [CrossRef] [PubMed]
- Alshehri, M.; Alamri, H.M.; Alshwaimi, E.; Kujan, O. Micro-computed tomographic assessment of quality of obturation in the apical third with continuous wave vertical compaction and single match taper sized cone obturation techniques. Scanning 2016, 38, 352–356. [Google Scholar] [CrossRef] [PubMed]
- Camilleri, J. Sealers and warm gutta percha obturation techniques. J. Endod. 2015, 41, 72–78. [Google Scholar] [CrossRef] [PubMed]
- Weine, F.S.; Healey, H.J.; Gerstein, H.; Evanson, L. Canal configuration in the mesiobuccal root of the maxillary first molar and its endodontic significance. J. Endod. 2012, 38, 1305–1308. [Google Scholar] [CrossRef] [PubMed]
- Schneider, S.W. A comparison of canal preparations in straight and curved root canals. Oral Surg. Oral Med. Oral Pathol. 1971, 32, 271–275. [Google Scholar] [CrossRef]
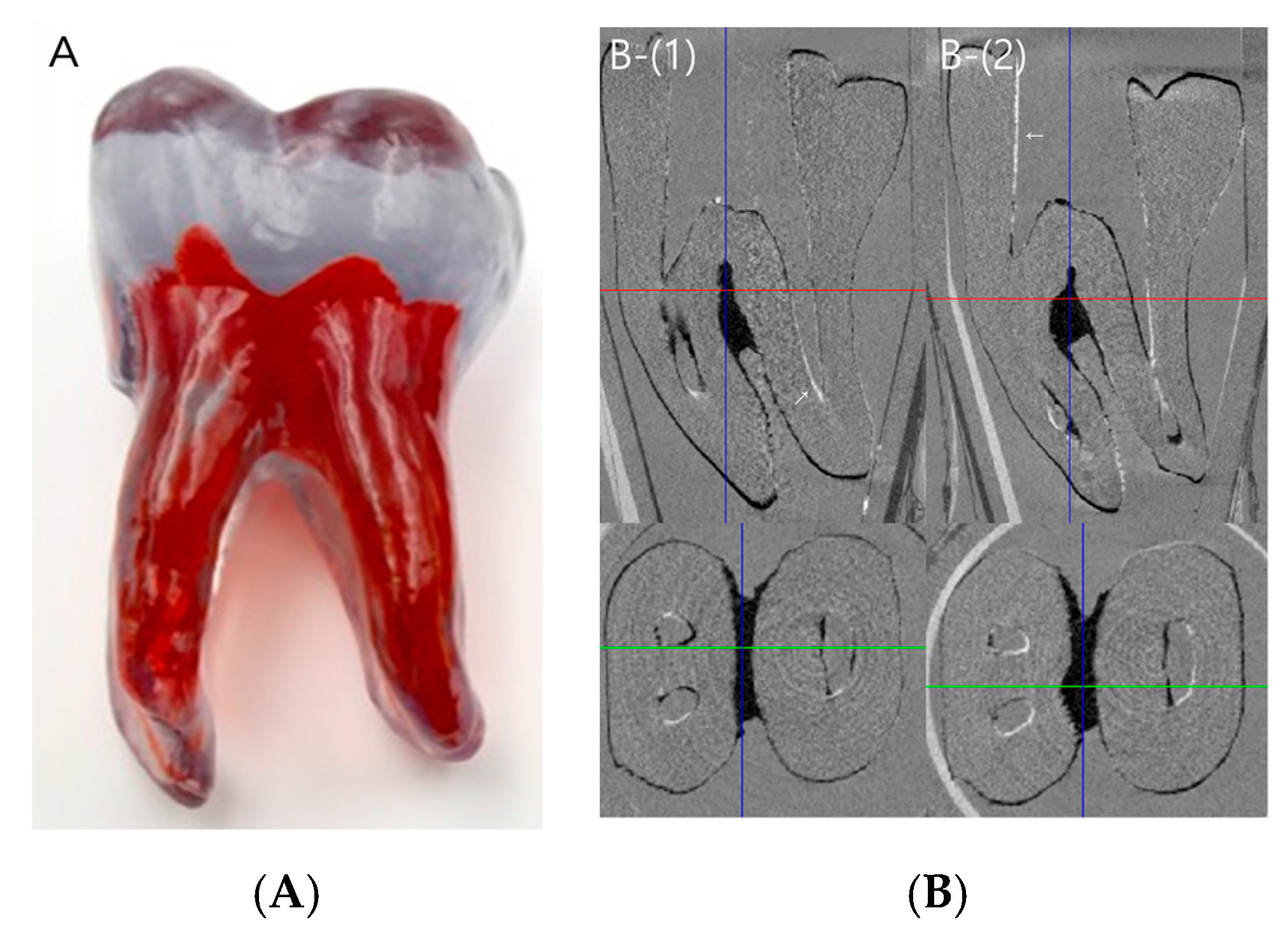
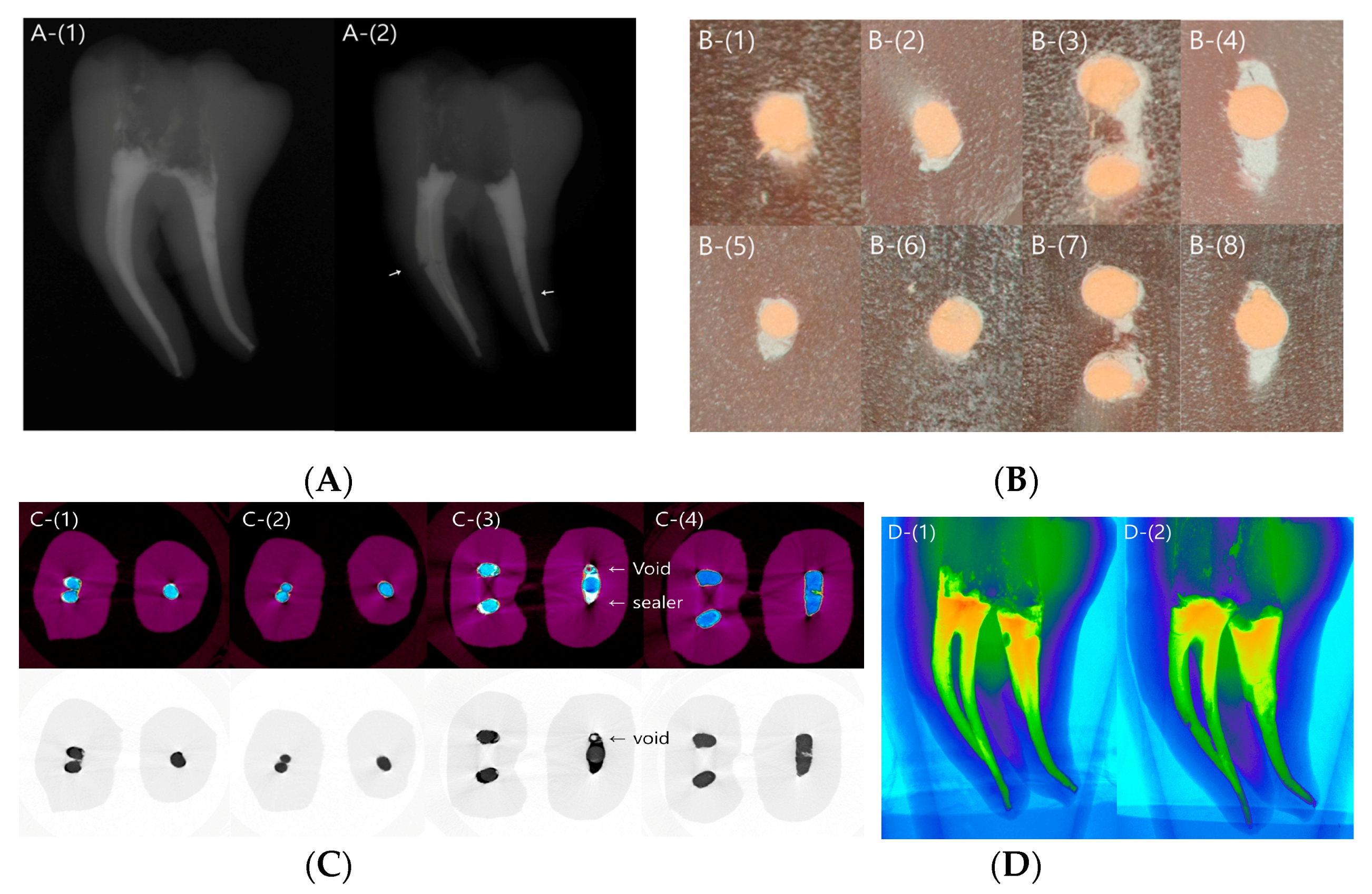
| Canal | Area | SC | CW | Overall p-Value |
|---|---|---|---|---|
| Mesial | Apical | 3.86 ± 0.11 | 3.61 ± 0.11 | Method: 0.56 Location < 0.05 * Method × Location < 0.05 * |
| Coronal | 5.30 ± 0.14 | 5.48 ± 0.14 | ||
| Distal | Apical | 3.87 ± 0.12 | 3.74 ± 0.12 | |
| Coronal | 5.17 ± 0.17 | 5.72 ± 0.17 |
| Canal | Area | SC | CW | Overall p-Value |
|---|---|---|---|---|
| Mesial | Apical | 4.18 ± 0.36 | 5.39 ± 0.36 | Method: < 0.05 * Location < 0.05 * Method × Location < 0.05 * |
| Coronal | 2.94 ± 0.77 | 5.38 ± 0.77 | ||
| Distal | Apical | 4.00 ± 0.38 | 5.08 ± 0.38 | |
| Coronal | 3.62 ± 0.76 | 10.13 ± 0.89 |
| %Vout | Mesial | Apical | 0.13 |
| Coronal | 0.40 | ||
| Distal | Apical | 0.47 | |
| Coronal | <0.05 * | ||
| %Vin | Mesial | Apical | <0.05 * |
| Coronal | <0.05 * | ||
| Distal | Apical | 0.06 | |
| Coronal | <0.05 * | ||
| %Vtotal | Mesial | Apical | 0.07 |
| Coronal | <0.05 * | ||
| Distal | Apical | <0.05 * | |
| Coronal | <0.05 * |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, S.; Kim, S.; Park, J.-W.; Jung, I.-Y.; Shin, S.-J. Comparison of the Percentage of Voids in the Canal Filling of a Calcium Silicate-Based Sealer and Gutta Percha Cones Using Two Obturation Techniques. Materials 2017, 10, 1170. https://doi.org/10.3390/ma10101170
Kim S, Kim S, Park J-W, Jung I-Y, Shin S-J. Comparison of the Percentage of Voids in the Canal Filling of a Calcium Silicate-Based Sealer and Gutta Percha Cones Using Two Obturation Techniques. Materials. 2017; 10(10):1170. https://doi.org/10.3390/ma10101170
Chicago/Turabian StyleKim, Sohee, Sunil Kim, Jeong-Won Park, Il-Young Jung, and Su-Jung Shin. 2017. "Comparison of the Percentage of Voids in the Canal Filling of a Calcium Silicate-Based Sealer and Gutta Percha Cones Using Two Obturation Techniques" Materials 10, no. 10: 1170. https://doi.org/10.3390/ma10101170





