Evaluation of Energy Consumption in German Hospitals: Benchmarking in the Public Sector
Abstract
:1. Introduction
2. Results
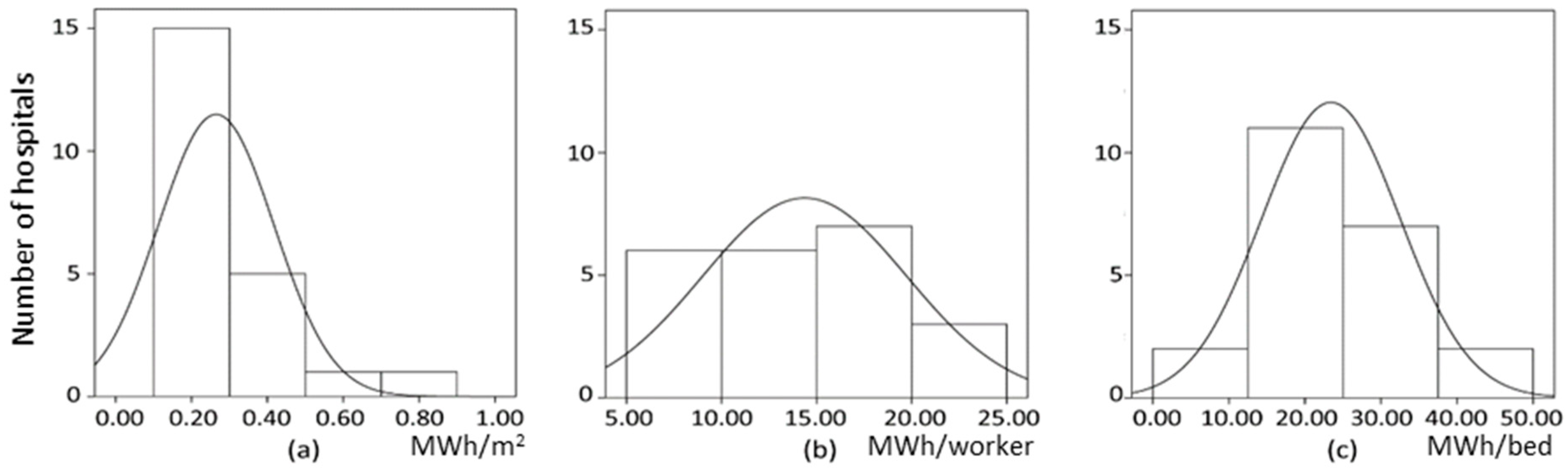
2.1. Morphological Analysis of Hospitals
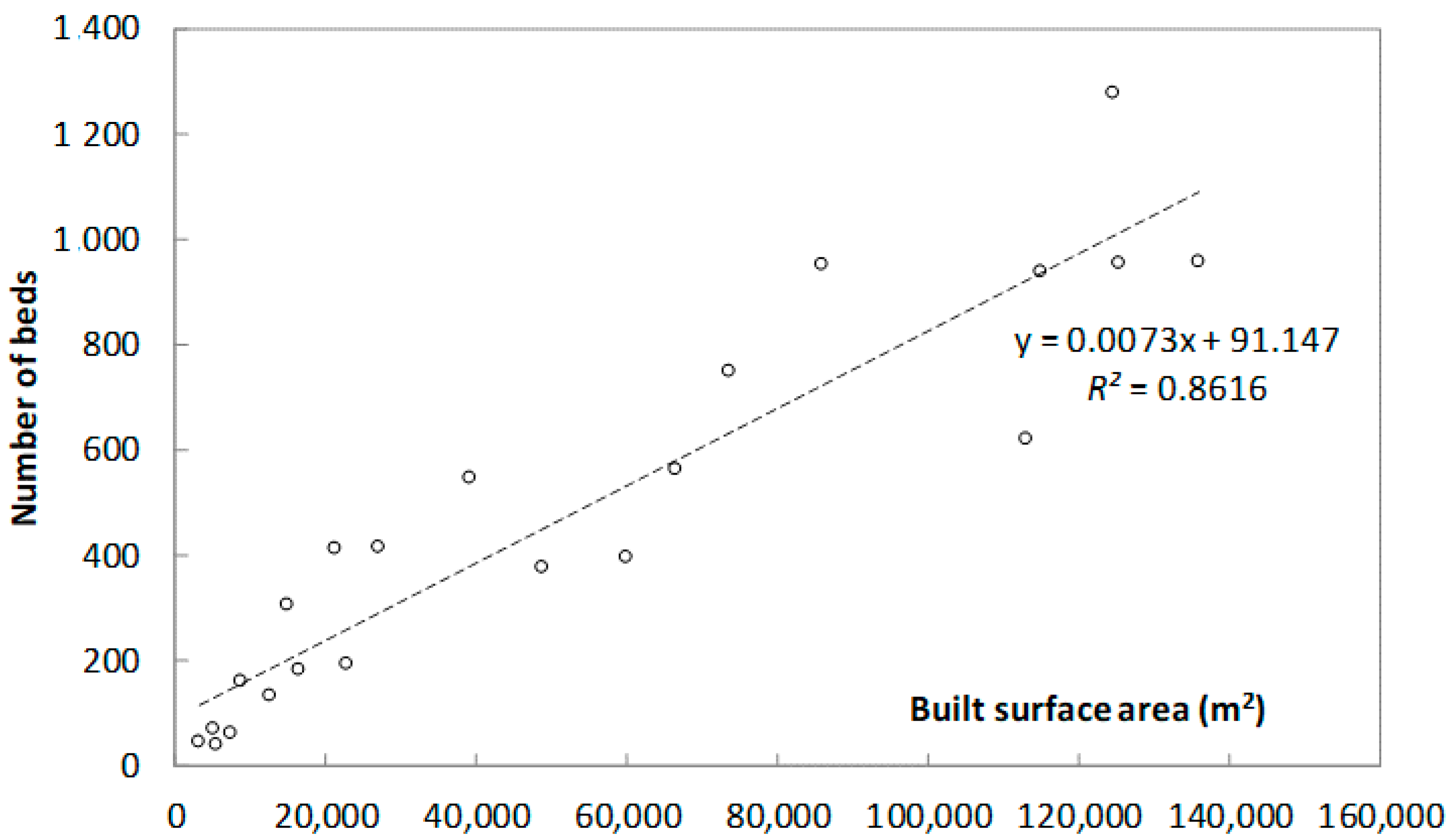
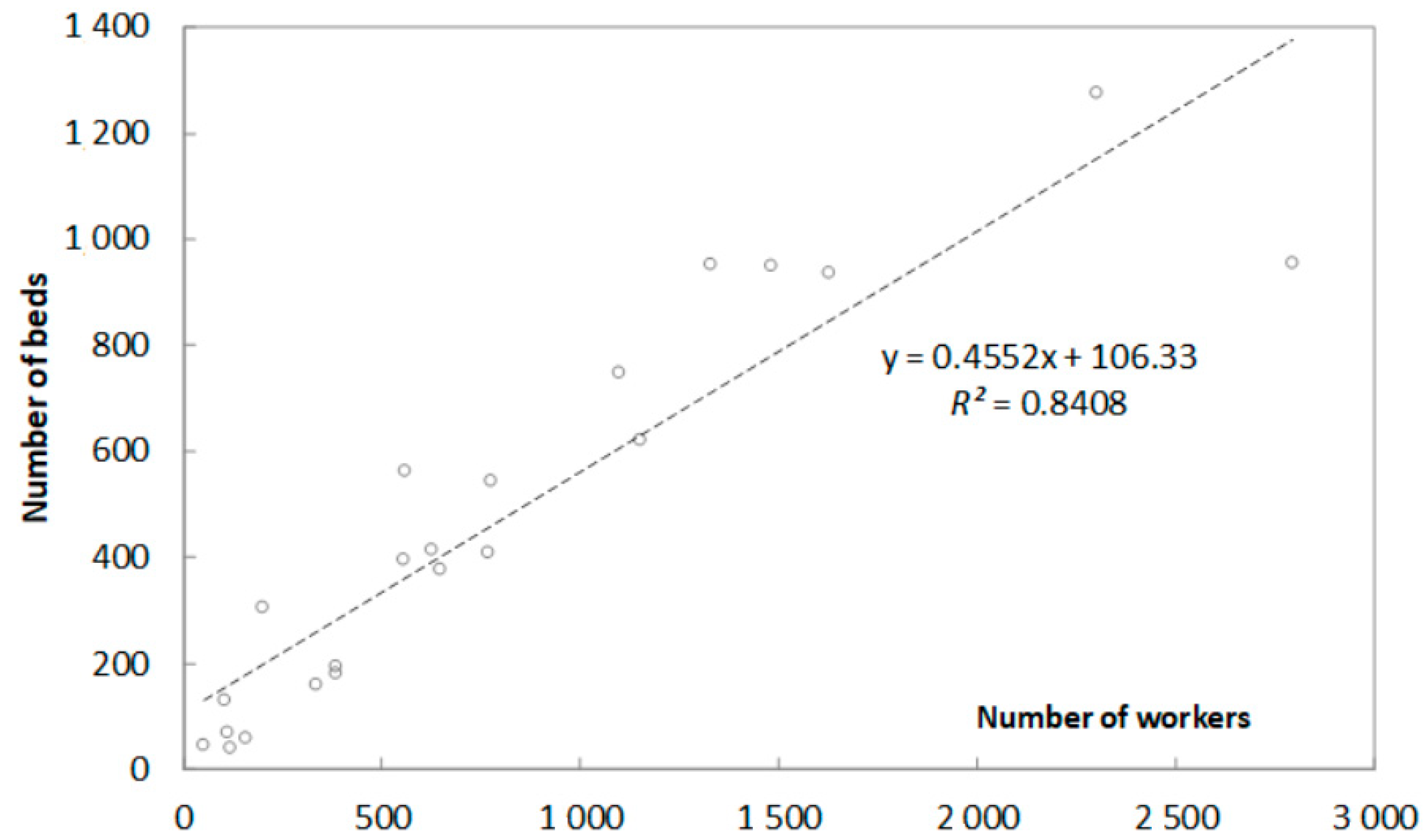
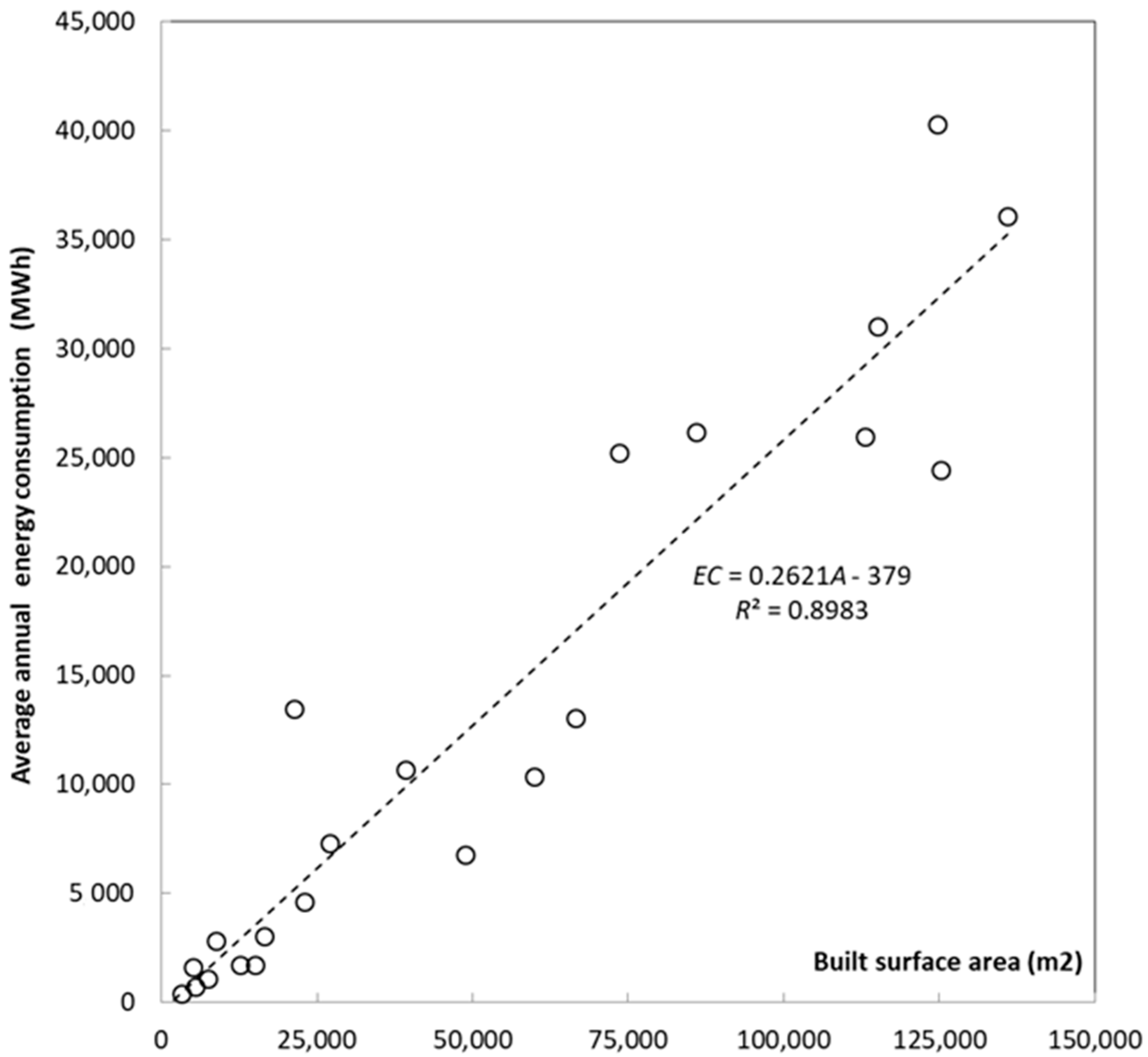
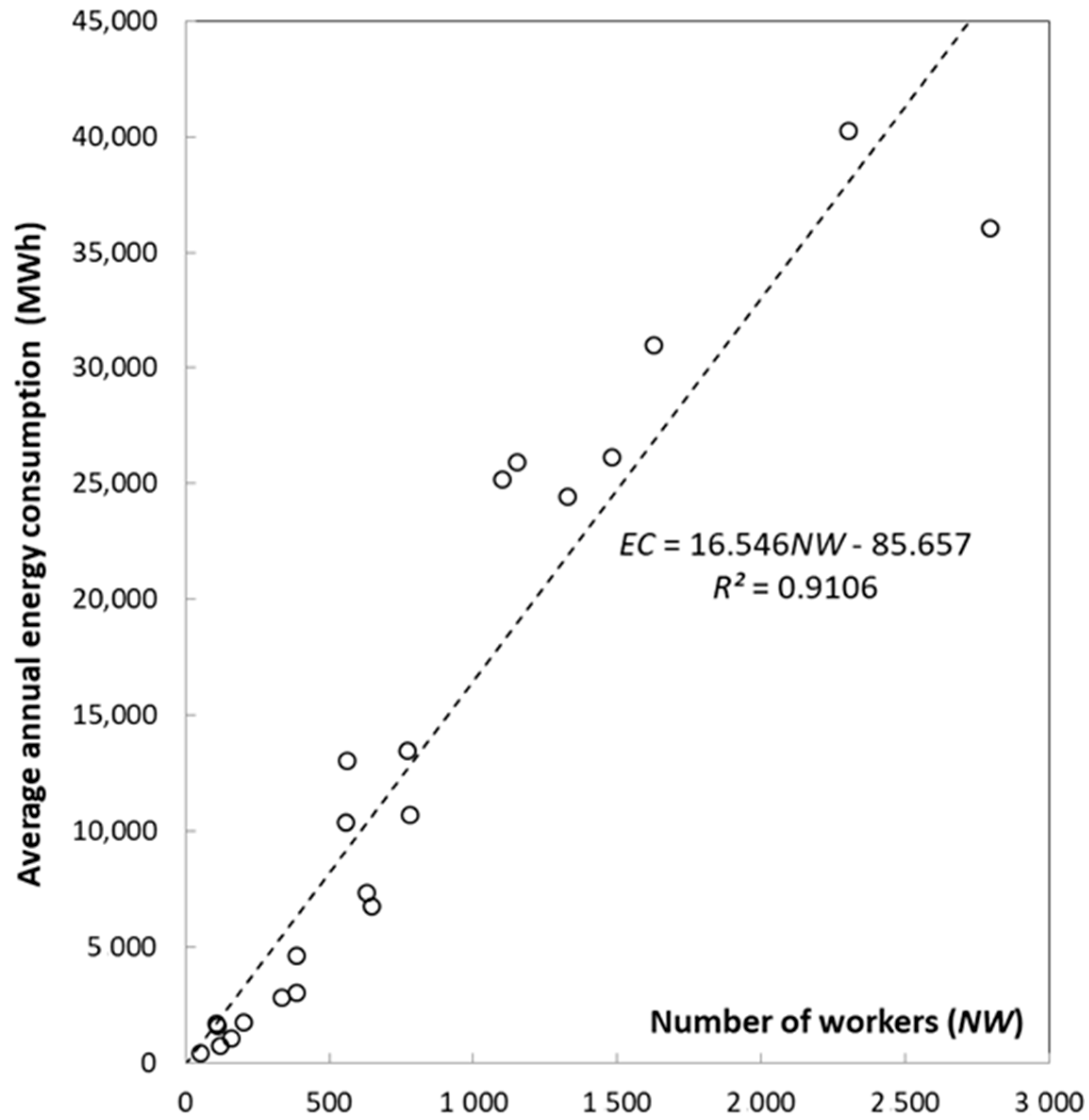
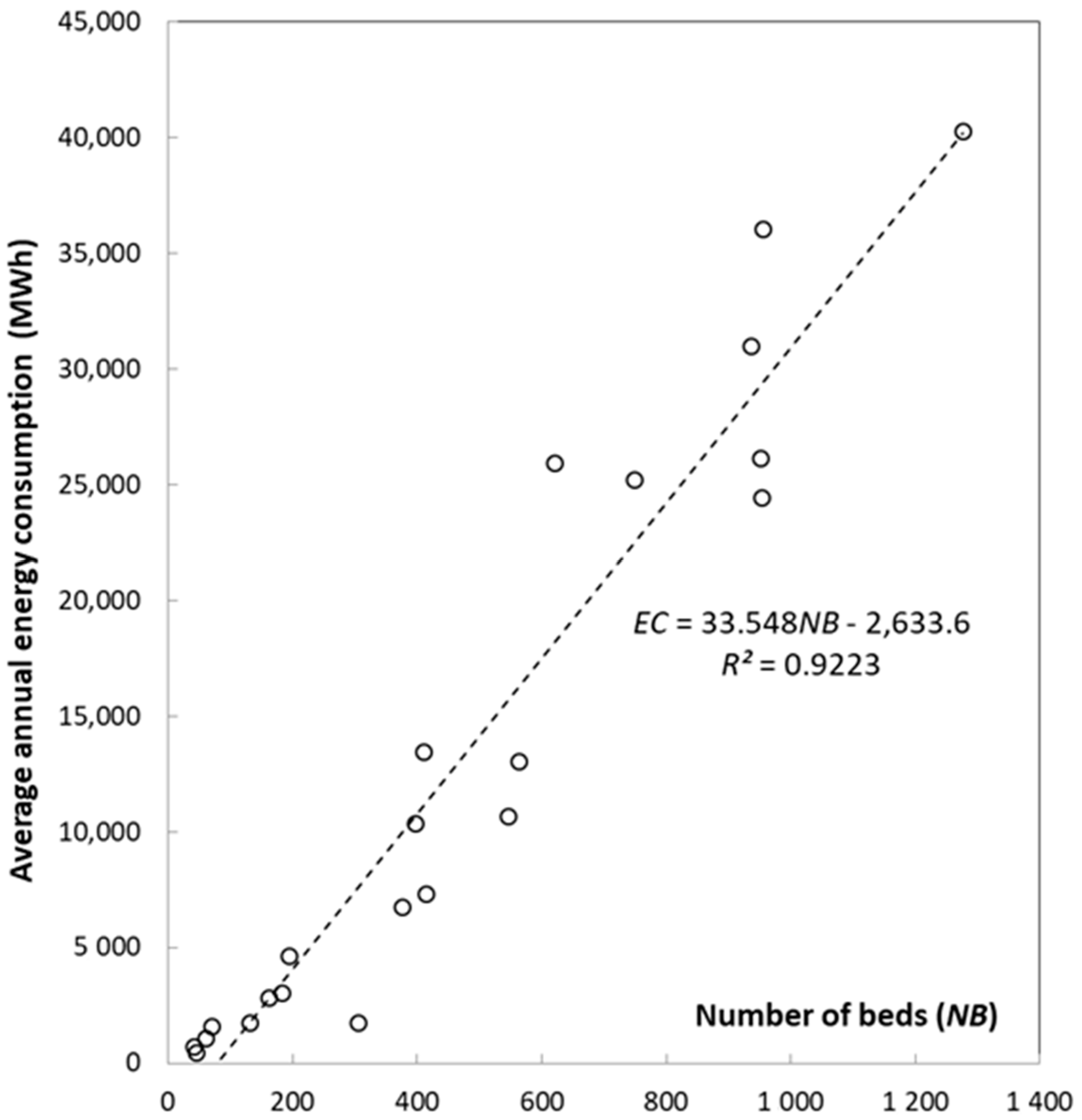
2.2. Correlation between Average Annual Energy Consumption and Built Surface Area, Number of Workers, and Number of Beds
2.3. Results of the Statistical ANOVA
2.3.1. Study of Energy Consumption per HCNB
2.3.2. Energy Consumption as Related to GDP
2.3.3. Energy Consumption as Related GL
2.3.4. Study of Energy Consumption in Time Intervals
2.3.5. Indicators of Average Annual Energy Consumption in Public Hospitals in Germany
3. Discussion
4. Materials and Methods
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Eckelman, M.J.; Sherman, J. Environmental impacts of the US healthcare system and effects on public health. PLoS ONE 2016, 11, e0157014. [Google Scholar] [CrossRef] [PubMed]
- Verband der Krankenhausdirektoren Deutschlands eV. KLINERGIE 2020. 2018. Available online: https://www.vkd-online.de/aktuelles/archiv/klinergie-2020/ (accessed on 29 March 2018). (In German).
- Christiansen, N.; Kaltschmitt, M.; Dzukowski, F.; Isensee, F. Electricity consumption of medical plug loads in hospital laboratories: Identification, evaluation, prediction and verification. Energy Build. 2015, 107, 392–406. [Google Scholar] [CrossRef]
- Daschner, F.; Kummerer, K.; Scherrer, M.; Hubner, P.; Metz, L. Krankenhäuser, Arztpraxen, Apotheken und Andere Einrichtungen des Gesundheitswesens; Bristol-Myers Squibb: New York, NY, USA, 2001. (In German) [Google Scholar]
- Intelligent Energy Europe. El Uso Racional de la Energía en Los Edificios Públicos. 2007. Available online: http://www.cecu.es/campanas/medio%20ambiente/Guia%20Edif%20Publicos.pdf/ (accessed on 29 March 2018). (In Spanish).
- Benke, G.; Leutgöb, K.; Varga, M.; Kolpek, M.; Greisberger, H. Das Energie Effiziente Krankenhaus (No. 22/2009); Berichte aus der Energie und Umweltforschung; Energie Markt Analyse GmbH, Österreichische Gesellschaft für Umwelt und Technik-ÖGUT: Wien, Austria, 2009. (In German) [Google Scholar]
- Thinate, N.; Wongsapai, W.; Damrongsak, D. Energy Performance Study in Thailand Hospital Building. Energy Procedia 2017, 141, 255–259. [Google Scholar] [CrossRef]
- Hu, S.; Chen, J.; Chuah, Y. Energy cost and consumption in a large acute hospital. Int. J. Arch. Sci. 2004, 5, 11–19. [Google Scholar]
- Rohde, T.; Martinez, R. Equipment and energy usage in a large teaching hospital in Norway. J. Healthc. Eng. 2015, 6, 419–434. [Google Scholar] [CrossRef] [PubMed]
- Umsicht, E.; Beier, D.I.C. Analyse des Energieverbrauchs und Exemplarische Best-Practice-Lösungen für Relevante Verbrauchssektoren in Krankenhäusern; Fraunhofer-Institut für Umwelt-, Sicherheits- und Energietechnik: Oberhausen, Germany, 2009. (In German) [Google Scholar]
- Tippkötter, R. Rationelle Energienutzung in Krankenhäusern: Leitfaden für Verwaltung und Betriebstechnik; Springer: Berlin/Heidelberg, Germany, 2003. (In German) [Google Scholar]
- Gesundheit, Kostennachweis der Krankenhäuser. In Fachserie 12 Reihe 6.3.; Statistisches Bundesamt: Wiesbaden, Germany, 2008. (In German)
- Samuels, M.L.; Witmer, J.A.; Schaffner, A.A. Statistics for the Life Sciences; Pearson Education: London, UK, 2012. [Google Scholar]
- Destatis. Krankenhausbetten: Deutschland Hat das Dichteste Versorgungsnetz der EU; Destatis: Wiesbaden, Germany, 2015; (In German).
- Destatis. Einrichtungen, Betten und Patientenbewegung; Destatis: Wiesbaden, Germany, 2016; (In German).
- García-Sanz-Calcedo, J.; Gómez-Chaparro, M. Quantitative Analysis of the Impact of Maintenance Management on the Energy Consumption of a Hospital in Extremadura (Spain). Sustain. Cities Soc. 2017, 30, 217–222. [Google Scholar] [CrossRef]
- Chiang, C.Y.; Yang, R.; Yang, K.H.; Lee, S.K. Performance Analysis of an Integrated Heat Pump with Air-Conditioning System for the Existing Hospital Building Application. Sustainability 2017, 9, 530. [Google Scholar] [CrossRef]
- García-Sanz-Calcedo, J.; López-Rodríguez, F. Analysis on the Performance of a High-Efficiency Administrative Building in Spain. Int. J. Green Energy 2017, 14, 55–62. [Google Scholar] [CrossRef]
- Loosemore, M.; Hsin, Y.Y. Customer-focused benchmarking for facilities management. Facilities 2001, 19, 464–476. [Google Scholar] [CrossRef]
- Morgenstern, P.; Li, M.; Raslan, R.; Ruyssevelt, P.; Wright, A. Benchmarking acute hospitals: Composite electricity targets based on departmental consumption intensities? Energy Build. 2016, 118, 277–290. [Google Scholar] [CrossRef]
- García-Sanz-Calcedo, J.; Al-Kassir, A.; Yusaf, T. Economic and Environmental Impact of Energy Saving in Healthcare Buildings. Appl. Sci. 2018, 8, 440. [Google Scholar] [CrossRef]
- González, A.G.; García-Sanz-Calcedo, J.; Salgado, D.R. A quantitative analysis of final energy consumption in hospitals in Spain. Sustain. Cities Soc. 2018, 36, 169–175. [Google Scholar] [CrossRef]
- Rodriguez, F.L.; Blazquez, F.C.; Vegas, C.P.S.; Celma, A.R.; Nieto, A.M.; Castro, S.S.; Giancola, E.; Tevar, J.A.F.; Ceramin, M.d.H.; Garcia Sanz-Calcedo, J.; et al. Edificio Peter: Un ejemplo de construcción bioclimática y de integración de energías renovables. DYNA 2011, 86, 212–221. (In Spanish) [Google Scholar] [CrossRef]
- Kolokotsa, D.; Pouliezos, A.; Stavrakakis, G.; Lazos, C. Predictive control techniques for energy and indoor environmental quality management in buildings. Build. Environ. 2009, 44, 1850–1863. [Google Scholar] [CrossRef]
- Singer, B.C.; Tschudi, W.F. High-Performance Healthcare Buildings: A Roadmap to Improved Energy Efficiency; No. LBNL-2737E; Ernest Orlando Lawrence Berkeley National Laboratory: Berkeley, CA, USA, 2009. [Google Scholar]
- Ekvall, T.; Hirschnitz-Garbers, M.; Eboli, F.; Śniegocki, A. A Systemic and Systematic Approach to the Development of a Policy Mix for Material Resource Efficiency. Sustainability 2016, 8, 373. [Google Scholar] [CrossRef]
- Morgenstern, P.; Raslan, R.; Ruyssevelt, P. Reducing hospital electricity use: An end-use perspective. In Proceedings of the 9th International Conference on Improving Energy Efficiency in Commercial Buildings and Smart Communities (IEECB&SC’16), Frankfurt, Germany, 16–18 March 2016. [Google Scholar]
- European Communities. Towards Sustainability: A European Community Programme of Policy and Action in Relation to the Environment and Sustainable Development; Office for Official Publications of the European Communities: Luxembourg, 1993. [Google Scholar]
- Iraldo, F.; Testa, F.; Frey, M. Is an environmental management system able to influence environmental and competitive performance? The case of the eco-management and audit scheme (EMAS) in the European Union. J. Clean. Prod. 2009, 17, 1444–1452. [Google Scholar] [CrossRef]
- European Commission, Environment EMAS. 2017. Available online: http://ec.europa.eu/environment/emas/index_en.htm/ (accessed on 1 April 2018).
- Sammlung EMAS Umwelterklaerungen. 2018. Available online: http://www.emas.de/teilnahme/umwelterklaerungen/sammlung/ (accessed on 6 April 2018). (In German).
- Deutsches Krankenhaus Gesellschaft. Deutsches Krankenhauverzeichnis. 2018. Available online: http://dkg.promato.de/de/suche/Regional.html/ (accessed on 1 April 2018). (In German).
- Sleiman, H.A.; Hempel, S.; Traversari, R.; Bruinenberg, S. An assisted workflow for the early design of nearly zero emission healthcare buildings. Energies 2017, 10, 993. [Google Scholar] [CrossRef]
- Lindner, M.; Bachhiesl, U.; Stigler, H. Das Exergiekonzept als Analysemethode am Beispiel Deutschlands. In Proceedings of the 13th Symposium Energieinnovation, Graz, Austria, 12–14 April 2014. (In German). [Google Scholar]
- Devore, J.; Farnum, N.; Doi, J. Applied Statistics for Engineers and Scientists; Nelson Education: Scarborough, ON, Canada, 2013. [Google Scholar]
- Norm DIN 4710:2003-01. In Statistics on German Meteorological Data for Calculating the Energy Requirements for Heating and Air Conditioning Equipment; Beuth Verlag: Berlin, Germany, 2003.
- Barnett, V.; Lewis, T. Outliers in Statistical Data; Wiley: Hoboken, NJ, USA, 1974. [Google Scholar]
| Factors | Distribution Regarding Factors |
|---|---|
| Hospital category based on number of beds (HCNB) | HCNB 1: <200 beds |
| HCNB 2: 200–500 beds | |
| HCNB 3: 500–1000 beds | |
| HCNB 4: >1000 beds | |
| Gross domestic product (GDP) | GDP 1: €35,001–€40,000 |
| GDP 2: €40,001–€45,000 | |
| GDP 3: >€45,001 | |
| Heating degrees-day year (HDDY) | HDDY 1: 1000–1250 °C |
| HDDY 2: 1250–1500 °C | |
| HDDY 3: 1500–1750 °C | |
| HDDY 4: 1750–2000 °C | |
| HDDY 5: 2000–2250 °C | |
| HDDY 6: 2250–2500 °C | |
| HDDY 7: >2501 °C | |
| Cooling degrees-day year (CDDY) | CDDY 1: ≤100 °C |
| CDDY 2: 101–200 °C | |
| CDDY 3: 201–300 °C | |
| CDDY 4: 301–400 °C | |
| CDDY 5: >401 °C | |
| Geographic location (GL) | Bavaria |
| Baden-Württemberg | |
| Bremen | |
| North Rhine-Westphalia | |
| Hessen | |
| Range of years | 2005–2009 |
| 2010–2015 |
| Indicators Consumption Ratios | Experiments Factors (p-Value) | |||||
|---|---|---|---|---|---|---|
| HCNB | GDP | HDDY | CDDY | GL | Period 2005–2009 and 2010–2015 | |
| 0.44 | 0.01 * | 0.18 | 0.14 | 0.04 * | 0.54 | |
| 0.00 * | 0.43 | 0.24 | 0.19 | 0.74 | 0.64 | |
| 0.01 * | 0.04 * | 0.25 | 0.17 | 0.11 | 0.02 * | |
| Hospital Category | MeanDiff | SEM | t Value | Prob | Sig. | LCL | UCL |
|---|---|---|---|---|---|---|---|
| HCNB 1–HCNB 2 | −2.52 | 4.09 | −0.62 | 0.54 | 0 | −11.11 | 6.07 |
| HCNB 3–HCNB 2 | 9.14 | 4.20 | 2.18 | 0.04 | 1 | 0.32 | 17.96 |
| HCNB 3–HCNB 1 | 11.66 | 3.71 | 3.14 | 0.01 | 1 | 3.87 | 19.46 |
| HCNB 4–HCNB 2 | 14.54 | 6.00 | 2.42 | 0.03 | 1 | 1.93 | 27.14 |
| HCNB 4–HCNB 1 | 17.06 | 5.67 | 3.01 | 0.01 | 1 | 5.15 | 28.97 |
| HCNB 4–HCNB 3 | 5.39 | 5.75 | 0.94 | 0.36 | 0 | −6.68 | 17.47 |
| Hospital | GL | Climatic Zone [36] | Hospital Category (HCNB) | GDP | HDDY | CDDY |
|---|---|---|---|---|---|---|
| Bezirkskrankenhaus-Kaufbeuren | Bavaria | 15 | HCNB 2 | GDP 2 | HDDY 4 | CDDY 2 |
| Klinik Immenstadt | 15 | HCNB 1 | HDDY 5 | CDDY 2 | ||
| Klinik Sonthofen | 15 | HCNB 1 | HDDY 5 | CDDY 3 | ||
| Klinik Oberstdorf | 15 | HCNB 1 | HDDY 5 | CDDY 2 | ||
| KH Rotthalmünster | 13 | HCNB 1 | HDDY 3 | CDDY 2 | ||
| KH Vilshofen | 13 | HCNB 1 | HDDY 5 | CDDY 3 | ||
| KH Wegscheid | 10 | HCNB 1 | HDDY 3 | CDDY 3 | ||
| Klinikum Bogenhausen | 13 | HCNB 3 | HDDY 4 | CDDY 2 | ||
| Klinikum Harlaching | 13 | HCNB 3 | HDDY 4 | CDDY 2 | ||
| Klinikum Neuperlach | 13 | HCNB 3 | HDDY 4 | CDDY 2 | ||
| Klinikum Schwabing | 13 | HCNB 3 | HDDY 4 | CDDY 2 | ||
| Klinik Thalkirchen Strasse | 13 | HCNB 1 | HDDY 4 | CDDY 2 | ||
| Klinikum Karlsruhe | Baden-Württemberg | 12 | HCNB 4 | GDP 2 | HDDY 3 | CDDY 5 |
| Psychiatric Clinics | 12 | HCNB 2 | HDDY 3 | CDDY 5 | ||
| Klinikum Bad-Hersfeld | Hessen | 7 | HCNB 3 | GDP 1 | HDDY 5 | CDDY 5 |
| Orthopädie Bad-Hersfeld | 7 | HCNB 1 | HDDY 5 | CDDY 5 | ||
| Klinikum Bremen-Mitte | Bremen | 3 | HCNB 4 | GDP 3 | HDDY 4 | CDDY 5 |
| Diakonie-Krankenhaus | 3 | HCNB 2 | HDDY 4 | CDDY 5 | ||
| LWL-Klinik Münster | North Rhine-Westphalia | 5 | HCNB 2 | GDP 1 | HDDY 3 | CDDY 1 |
| LVR-Klinikums Düsseldorf | 5 | HCNB 3 | HDDY 3 | CDDY 1 | ||
| LVR Klinik Bedburg-Hau | 5 | HCNB 4 | HDDY 3 | CDDY 5 | ||
| LVR Kliniken at the Standort Viersen | 5 | HCNB 3 | HDDY 3 | CDDY 5 | ||
| LWL-Klinik Lengerich | 5 | HCNB 2 | HDDY 3 | CDDY 1 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
González González, A.; García-Sanz-Calcedo, J.; Rodríguez Salgado, D. Evaluation of Energy Consumption in German Hospitals: Benchmarking in the Public Sector. Energies 2018, 11, 2279. https://doi.org/10.3390/en11092279
González González A, García-Sanz-Calcedo J, Rodríguez Salgado D. Evaluation of Energy Consumption in German Hospitals: Benchmarking in the Public Sector. Energies. 2018; 11(9):2279. https://doi.org/10.3390/en11092279
Chicago/Turabian StyleGonzález González, Alfonso, Justo García-Sanz-Calcedo, and David Rodríguez Salgado. 2018. "Evaluation of Energy Consumption in German Hospitals: Benchmarking in the Public Sector" Energies 11, no. 9: 2279. https://doi.org/10.3390/en11092279
APA StyleGonzález González, A., García-Sanz-Calcedo, J., & Rodríguez Salgado, D. (2018). Evaluation of Energy Consumption in German Hospitals: Benchmarking in the Public Sector. Energies, 11(9), 2279. https://doi.org/10.3390/en11092279