Endoscopic Grading and Sampling of Gastric Precancerous Lesions: A Comprehensive Literature Review
Abstract
1. Introduction
2. Materials and Methods
3. Prevalence of Gastric Precancerous Lesions
4. Obstacles to Implementation in Clinical Practice and How to Overcome Them
5. Endoscopic Staging of Gastric Precancerous Lesions
5.1. Kimura–Takemoto Classification for CAG
5.2. Endoscopic Grading of Gastric Intestinal Metaplasia (EGGIM) Classification for GIM
5.3. Comparison with OLGIM
5.4. Assessment of Gastric Cancer Risk
5.5. Gastric Cancer Risk in Autoimmune Gastritis (AIG)
5.6. The Role of Artificial Intelligence (AI)
6. Sampling of Gastric Precancerous Lesions
6.1. Significance of OLGA and OLGIM Staging Systems in GC Risk Assessment
6.2. Impact of Reduced Biopsy Numbers on Environmental and Procedural Costs
7. Critical Appraisal of the Evidence and Future Research Targets
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Bray, F.; Laversanne, M.; Sung, H.; Ferlay, J.; Siegel, R.L.; Soerjomataram, I.; Jemal, A. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA A Cancer J. Clin. 2024, 74, 229–263. [Google Scholar] [CrossRef] [PubMed]
- Reim, D.; Loos, M.; Vogl, F.; Novotny, A.; Schuster, T.; Langer, R.; Becker, K.; Hofler, H.; Siveke, J.; Bassermann, F.; et al. Prognostic implications of the seventh edition of the international union against cancer classification for patients with gastric cancer: The Western experience of patients treated in a single-center European institution. J. Clin. Oncol. 2013, 31, 263–271. [Google Scholar] [CrossRef] [PubMed]
- Correa, P. A human model of gastric carcinogenesis. Cancer Res. 1988, 48, 3554–3560. [Google Scholar]
- Triantafyllou, K.; Papadopoulos, V.; Emanouil, T.; Gkolfakis, P.; Damaskou, V.; Tziatzios, G.; Panayiotides, I.G.; Vafiadis, I.; Ladas, S.D. Eradication of Helicobacter pylori Infection Restores ki67, p53, and Cyclin D1 Immunoreactivity in the Human Gastric Epithelium. Clin. Med. Insights Gastroenterol. 2016, 9, 73–78. [Google Scholar] [CrossRef] [PubMed]
- Abdelfatah, M.M.; Barakat, M.; Ahmad, D.; Ibrahim, M.; Ahmed, Y.; Kurdi, Y.; Grimm, I.S.; Othman, M.O. Long-term outcomes of endoscopic submucosal dissection versus surgery in early gastric cancer: A systematic review and meta-analysis. Eur. J. Gastroenterol. Hepatol. 2019, 31, 418–424. [Google Scholar] [CrossRef] [PubMed]
- Shichijo, S.; Hirata, Y.; Niikura, R.; Hayakawa, Y.; Yamada, A.; Ushiku, T.; Fukayama, M.; Koike, K. Histologic intestinal metaplasia and endoscopic atrophy are predictors of gastric cancer development after Helicobacter pylori eradication. Gastrointest. Endosc. 2016, 84, 618–624. [Google Scholar] [CrossRef] [PubMed]
- Pimentel-Nunes, P.; Libânio, D.; Marcos-Pinto, R.; Areia, M.; Leja, M.; Esposito, G.; Garrido, M.; Kikuste, I.; Megraud, F.; Matysiak-Budnik, T.; et al. Management of epithelial precancerous conditions and lesions in the stomach (MAPS II): European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter and Microbiota Study Group (EHMSG), European Society of Pathology (ESP), and Sociedade Portuguesa de Endoscopia Digestiva (SPED) guideline update 2019. Endoscopy 2019, 51, 365–388. [Google Scholar] [CrossRef] [PubMed]
- Libanio, D.; Ortigao, R.; Pimentel-Nunes, P.; Dinis-Ribeiro, M. Improving the Diagnosis and Treatment of Early Gastric Cancer in the West. GE Port. J. Gastroenterol. 2022, 29, 299–310. [Google Scholar] [CrossRef] [PubMed]
- Pimentel-Nunes, P.; Libanio, D.; Lage, J.; Abrantes, D.; Coimbra, M.; Esposito, G.; Hormozdi, D.; Pepper, M.; Drasovean, S.; White, J.R.; et al. A multicenter prospective study of the real-time use of narrow-band imaging in the diagnosis of premalignant gastric conditions and lesions. Endoscopy 2016, 48, 723–730. [Google Scholar] [CrossRef]
- Eshmuratov, A.; Nah, J.C.; Kim, N.; Lee, H.S.; Lee, H.E.; Lee, B.H.; Uhm, M.S.; Park, Y.S.; Lee, D.H.; Jung, H.C.; et al. The correlation of endoscopic and histological diagnosis of gastric atrophy. Dig. Dis. Sci. 2010, 55, 1364–1375. [Google Scholar] [CrossRef]
- Capelle, L.G.; Haringsma, J.; de Vries, A.C.; Steyerberg, E.W.; Biermann, K.; van Dekken, H.; Kuipers, E.J. Narrow band imaging for the detection of gastric intestinal metaplasia and dysplasia during surveillance endoscopy. Dig. Dis. Sci. 2010, 55, 3442–3448. [Google Scholar] [CrossRef] [PubMed]
- Marcos, P.; Brito-Gonçalves, G.; Libânio, D.; Pita, I.; Castro, R.; Sá, I. Endoscopic grading of gastric intestinal metaplasia on risk assessment for early gastric neoplasia: Can we replace histology assessment also in the West? Gut 2020, 69, 1762–1768. [Google Scholar] [CrossRef] [PubMed]
- Ford, A.C.; Yuan, Y.; Forman, D.; Hunt, R.; Moayyedi, P. Helicobacter pylori eradication for the prevention of gastric neoplasia. Cochrane Database Syst. Rev. 2020, 7, Cd005583. [Google Scholar] [CrossRef] [PubMed]
- Weck, M.N.; Brenner, H. Prevalence of chronic atrophic gastritis in different parts of the world. Cancer Epidemiol. Biomark. Prev. 2006, 15, 1083–1094. [Google Scholar] [CrossRef] [PubMed]
- Marques-Silva, L.; Areia, M.; Elvas, L.; Dinis-Ribeiro, M. Prevalence of gastric precancerous conditions: A systematic review and meta-analysis. Eur. J. Gastroenterol. Hepatol. 2014, 26, 378–387. [Google Scholar] [CrossRef]
- Yin, Y.; Liang, H.; Wei, N.; Zheng, Z. Prevalence of chronic atrophic gastritis worldwide from 2010 to 2020: An updated systematic review and meta-analysis. Ann. Palliat. Med. 2022, 11, 3697–3703. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Jiang, F.; Wu, C.Y.; Leung, W.K. Prevalence and temporal trend of gastric preneoplastic lesions in Asia: A systematic review with meta-analysis. United Eur. Gastroenterol. J. 2023, 12, 139–151. [Google Scholar] [CrossRef] [PubMed]
- Pimenta-Melo, A.R.; Monteiro-Soares, M.; Libanio, D.; Dinis-Ribeiro, M. Missing rate for gastric cancer during upper gastrointestinal endoscopy: A systematic review and meta-analysis. Eur. J. Gastroenterol. Hepatol. 2016, 28, 1041–1049. [Google Scholar] [CrossRef]
- Tajiri, H.; Dinis-Ribeiro, M. How I inspect the stomach. Gastrointest. Endosc. 2019, 89, 1106–1108. [Google Scholar] [CrossRef]
- Bisschops, R.; Areia, M.; Coron, E.; Dobru, D.; Kaskas, B.; Kuvaev, R.; Pech, O.; Ragunath, K.; Weusten, B.; Familiari, P.; et al. Performance measures for upper gastrointestinal endoscopy: A European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative. Endoscopy 2016, 48, 843–864. [Google Scholar] [CrossRef]
- Emura, F.; Sharma, P.; Arantes, V.; Cerisoli, C.; Parra-Blanco, A.; Sumiyama, K.; Araya, R.; Sobrino, S.; Chiu, P.; Matsuda, K. Principles and practice to facilitate complete photodocumentation of the upper gastrointestinal tract: World Endoscopy Organization position statement. Dig. Endosc. 2020, 32, 168–179. [Google Scholar] [CrossRef] [PubMed]
- Duez, L.; Gkolfakis, P.; Bastide, M.; Vuckovic, C.; Musala, C.; Van Gossum, M.; Hoyois, A.; Mulkay, J.P.; Eisendrath, P. Premedication with simethicone for improving the quality of gastric mucosal visualization: A double-blind randomized controlled trial. Endosc. Int. Open 2022, 10, E1343–E1349. [Google Scholar] [CrossRef]
- Beilenhoff, U.; Biering, H.; Blum, R.; Brljak, J.; Cimbro, M.; Dumonceau, J.M.; Hassan, C.; Jung, M.; Kampf, B.; Neumann, C.; et al. Reprocessing of flexible endoscopes and endoscopic accessories used in gastrointestinal endoscopy: Position Statement of the European Society of Gastrointestinal Endoscopy (ESGE) and European Society of Gastroenterology Nurses and Associates (ESGENA)-Update 2018. Endoscopy 2018, 50, 1205–1234. [Google Scholar] [CrossRef]
- Romańczyk, M.; Ostrowski, B.; Kozłowska-Petriczko, K.; Pawlak, K.M.; Kurek, K.; Zatorski, H.; Koziej, M.; Romańczyk, T.; Wosiewicz, P.; Marek, T.; et al. Scoring system assessing mucosal visibility of upper gastrointestinal tract: The POLPREP scale. J. Gastroenterol. Hepatol. 2022, 37, 164–168. [Google Scholar] [CrossRef]
- Teh, J.L.; Tan, J.R.; Lau, L.J.; Saxena, N.; Salim, A.; Tay, A.; Shabbir, A.; Chung, S.; Hartman, M.; So, J.B. Longer examination time improves detection of gastric cancer during diagnostic upper gastrointestinal endoscopy. Clin. Gastroenterol. Hepatol. 2015, 13, 480–487.e2. [Google Scholar] [CrossRef]
- Kimura, K.; Takemoto, T. An Endoscopic Recognition of the Atrophic Border and its Significance in Chronic Gastritis. Endoscopy 1969, 1, 87–97. [Google Scholar] [CrossRef]
- Waddingham, W.; Graham, D.; Banks, M.; Jansen, M. The evolving role of endoscopy in the diagnosis of premalignant gastric lesions. F1000Research 2018, 7, 715. [Google Scholar] [CrossRef] [PubMed]
- Kimura, K.; Satoh, K.; Ido, K.; Taniguchi, Y.; Takimoto, T.; Takemoto, T. Gastritis in the Japanese stomach. Scand. J. Gastroenterol. Suppl. 1996, 214, 17–20; discussion 21–23. [Google Scholar] [CrossRef]
- Kono, S.; Gotoda, T.; Yoshida, S.; Oda, I.; Kondo, H.; Gatta, L.; Naylor, G.; Dixon, M.; Moriyasu, F.; Axon, A. Can endoscopic atrophy predict histological atrophy? Historical study in United Kingdom and Japan. World J. Gastroenterol. 2015, 21, 13113–13123. [Google Scholar] [CrossRef]
- Na, H.K.; Choi, K.D.; Park, Y.S.; Kim, H.J.; Ahn, J.Y.; Lee, J.H.; Jung, K.W.; Kim, D.H.; Song, H.J.; Lee, G.H.; et al. Endoscopic scoring system for gastric atrophy and intestinal metaplasia: Correlation with OLGA and OLGIM staging: A single-center prospective pilot study in Korea. Scand. J. Gastroenterol. 2022, 57, 1097–1104. [Google Scholar] [CrossRef] [PubMed]
- Take, S.; Mizuno, M.; Ishiki, K.; Yoshida, T.; Ohara, N.; Yokota, K.; Oguma, K.; Okada, H.; Yamamoto, K. The long-term risk of gastric cancer after the successful eradication of Helicobacter pylori. J. Gastroenterol. 2011, 46, 318–324. [Google Scholar] [CrossRef]
- Sekikawa, A.; Fukui, H.; Sada, R.; Fukuhara, M.; Marui, S.; Tanke, G.; Endo, M.; Ohara, Y.; Matsuda, F.; Nakajima, J.; et al. Gastric atrophy and xanthelasma are markers for predicting the development of early gastric cancer. J. Gastroenterol. 2016, 51, 35–42. [Google Scholar] [CrossRef]
- Song, J.H.; Kim, S.G.; Jin, E.H.; Lim, J.H.; Yang, S.Y. Risk Factors for Gastric Tumorigenesis in Underlying Gastric Mucosal Atrophy. Gut Liver 2017, 11, 612–619. [Google Scholar] [CrossRef] [PubMed]
- Sugimoto, M.; Ban, H.; Ichikawa, H.; Sahara, S.; Otsuka, T.; Inatomi, O.; Bamba, S.; Furuta, T.; Andoh, A. Efficacy of the Kyoto Classification of Gastritis in Identifying Patients at High Risk for Gastric Cancer. Intern. Med. 2017, 56, 579–586. [Google Scholar] [CrossRef] [PubMed]
- Xiao, S.; Fan, Y.; Yin, Z.; Zhou, L. Endoscopic grading of gastric atrophy on risk assessment of gastric neoplasia: A systematic review and meta-analysis. J. Gastroenterol. Hepatol. 2021, 36, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Esposito, G.; Pimentel-Nunes, P.; Angeletti, S.; Castro, R.; Libanio, D.; Galli, G.; Lahner, E.; Di Giulio, E.; Annibale, B.; Dinis-Ribeiro, M. Endoscopic grading of gastric intestinal metaplasia (EGGIM): A multicenter validation study. Endoscopy 2019, 51, 515–521. [Google Scholar] [CrossRef] [PubMed]
- Castro, R.; Rodriguez, M.; Libanio, D.; Esposito, G.; Pita, I.; Patita, M.; Santos, C.; Pimentel-Nunes, P.; Dinis-Ribeiro, M. Reliability and accuracy of blue light imaging for staging of intestinal metaplasia in the stomach. Scand. J. Gastroenterol. 2019, 54, 1301–1305. [Google Scholar] [CrossRef] [PubMed]
- Zhang, G.; Zheng, J.; Zheng, L.; Yu, S.; Jiang, C.; Lin, W.; Li, D.; Qu, L.; Wang, W. Gastric intestinal metaplasia assessment between linked color imaging based on endoscopy and pathology. Scand. J. Gastroenterol. 2021, 56, 103–110. [Google Scholar] [CrossRef] [PubMed]
- Fang, S.; Fu, Y.; Du, S.; Wang, L.; Qing, X.; Luo, X.; Song, G.; Yang, Y.; Wei, W. The role of the endoscopic grading of gastric intestinal metaplasia in assessing gastric cancer risk: A systematic review and meta-analysis. Front. Oncol. 2022, 12, 1018248. [Google Scholar] [CrossRef] [PubMed]
- Kawamura, M.; Koike, T.; Ogata, Y.; Matsumoto, R.; Yano, K.; Hiratsuka, T.; Ohyama, H.; Sato, I.; Kayada, K.; Suzuki, S.; et al. Endoscopic Grading of Gastric Intestinal Metaplasia Using Magnifying and Nonmagnifying Narrow-Band Imaging Endoscopy. Diagnostics 2022, 12, 3012. [Google Scholar] [CrossRef] [PubMed]
- Zheng, J.; Zhang, G.; Gao, C.; Xu, G.; Lin, W.; Jiang, C.; Li, D.; Wang, W. Linked color imaging-based endoscopic grading of gastric intestinal metaplasia and histological gastritis staging in the assessment of gastric cancer risk. Scand. J. Gastroenterol. 2022, 57, 1374–1380. [Google Scholar] [CrossRef]
- Kawamura, M.; Uedo, N.; Koike, T.; Kanesaka, T.; Hatta, W.; Ogata, Y.; Oikawa, T.; Iwai, W.; Yokosawa, S.; Honda, J.; et al. Kyoto classification risk scoring system and endoscopic grading of gastric intestinal metaplasia for gastric cancer: Multicenter observation study in Japan. Dig. Endosc. 2022, 34, 508–516. [Google Scholar] [CrossRef]
- Kishino, M.; Nonaka, K. Endoscopic Features of Autoimmune Gastritis: Focus on Typical Images and Early Images. J. Clin. Med. 2022, 11, 3523. [Google Scholar] [CrossRef]
- Terao, S.; Suzuki, S.; Yaita, H.; Kurahara, K.; Shunto, J.; Furuta, T.; Maruyama, Y.; Ito, M.; Kamada, T.; Aoki, R.; et al. Multicenter study of autoimmune gastritis in Japan: Clinical and endoscopic characteristics. Dig. Endosc. 2020, 32, 364–372. [Google Scholar] [CrossRef] [PubMed]
- Ayaki, M.; Aoki, R.; Matsunaga, T.; Manabe, N.; Fujita, M.; Kamada, T.; Kobara, H.; Masaki, T.; Haruma, K. Endoscopic and Upper Gastrointestinal Barium X-ray Radiography Images of Early-stage Autoimmune Gastritis: A Report of Two Cases. Intern. Med. 2021, 60, 1691–1696. [Google Scholar] [CrossRef] [PubMed]
- Shi, Y.; Wei, N.; Wang, K.; Tao, T.; Yu, F.; Lv, B. Diagnostic value of artificial intelligence-assisted endoscopy for chronic atrophic gastritis: A systematic review and meta-analysis. Front. Med. 2023, 10, 1134980. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Q.; Chi, T. Deep learning model can improve the diagnosis rate of endoscopic chronic atrophic gastritis: A prospective cohort study. BMC Gastroenterol. 2022, 22, 133. [Google Scholar] [CrossRef]
- Tao, X.; Zhu, Y.; Dong, Z.; Huang, L.; Shang, R.; Du, H.; Wang, J.; Zeng, X.; Wang, W.; Wang, J.; et al. An artificial intelligence system for chronic atrophic gastritis diagnosis and risk stratification under white light endoscopy. Dig. Liver Dis. 2024. [CrossRef]
- Li, N.; Yang, J.; Li, X.; Shi, Y.; Wang, K. Accuracy of artificial intelligence-assisted endoscopy in the diagnosis of gastric intestinal metaplasia: A systematic review and meta-analysis. PLoS ONE 2024, 19, e0303421. [Google Scholar] [CrossRef]
- Isajevs, S.; Liepniece-Karele, I.; Janciauskas, D.; Moisejevs, G.; Funka, K.; Kikuste, I.; Vanags, A.; Tolmanis, I.; Leja, M. The effect of incisura angularis biopsy sampling on the assessment of gastritis stage. Eur. J. Gastroenterol. Hepatol. 2014, 26, 510–513. [Google Scholar] [CrossRef]
- Mao, X.Y.; Xu, S.F.; Liu, Q.; Jiang, J.X.; Zhang, H.H.; Sang, H.M.; Zhang, G.X. Anatomical predilection of intestinal metaplasia based on 78,335 endoscopic cases. Saudi J. Gastroenterol. 2016, 22, 154–160. [Google Scholar] [CrossRef]
- Varbanova, M.; Wex, T.; Jechorek, D.; Rohl, F.W.; Langner, C.; Selgrad, M.; Malfertheiner, P. Impact of the angulus biopsy for the detection of gastric preneoplastic conditions and gastric cancer risk assessment. J. Clin. Pathol. 2016, 69, 19–25. [Google Scholar] [CrossRef]
- Khomeriki, S.G.; Bordin, D.S.; Khomeriki, N.M.; Parfenchikova, E.V.; Nikolskaya, K.A.; Ivanova, V.A.; Chebotareva, M.V.; Gretskaya, M.L.; Voynovan, I.N.; Kiriukova, M.A.; et al. The Impact of the Angulus Biopsy on the Detection of Staging and the Grading of Chronic Gastritis. Diagnostics 2023, 13, 2928. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.I.; Kook, M.C.; Cho, S.J.; Lee, J.Y.; Kim, C.G.; Joo, J.; Choi, I.J. Effect of biopsy site on detection of gastric cancer high-risk groups by OLGA and OLGIM stages. Helicobacter 2017, 22, e12442. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, F.; Ogata, D.C.; Mello, C.A.L. Role of Incisura Angularis Biopsy in Gastritis Staging and Risk Assessment of Gastric Cancer. Arq. De Gastroenterol. 2023, 60, 478–489. [Google Scholar] [CrossRef]
- Esposito, G.; Dinis-Ribeiro, M. Gastric intestinal metaplasia: Can we abandon random biopsies. Endosc. Int. Open 2022, 10, E280–E281. [Google Scholar] [CrossRef] [PubMed]
- Buxbaum, J.L.; Hormozdi, D.; Dinis-Ribeiro, M.; Lane, C.; Dias-Silva, D.; Sahakian, A.; Jayaram, P.; Pimentel-Nunes, P.; Shue, D.; Pepper, M.; et al. Narrow-band imaging versus white light versus mapping biopsy for gastric intestinal metaplasia: A prospective blinded trial. Gastrointest. Endosc. 2017, 86, 857–865. [Google Scholar] [CrossRef]
- Faknak, N.; Pittayanon, R.; Tiankanon, K.; Lerttanatum, N.; Sanpavat, A.; Klaikaew, N.; Rerknimitr, R. Performance status of targeted biopsy alone versus Sydney protocol by non-NBI expert gastroenterologist in gastric intestinal metaplasia diagnosis. Endosc. Int. Open 2022, 10, E273–E279. [Google Scholar] [CrossRef]
- Cho, S.J.; Choi, I.J.; Kook, M.C.; Nam, B.H.; Kim, C.G.; Lee, J.Y.; Ryu, K.W.; Kim, Y.W. Staging of intestinal- and diffuse-type gastric cancers with the OLGA and OLGIM staging systems. Aliment. Pharmacol. Ther. 2013, 38, 1292–1302. [Google Scholar] [CrossRef] [PubMed]
- Rugge, M.; Genta, R.M.; Fassan, M.; Valentini, E.; Coati, I.; Guzzinati, S.; Savarino, E.; Zorzi, M.; Farinati, F.; Malfertheiner, P. OLGA Gastritis Staging for the Prediction of Gastric Cancer Risk: A Long-term Follow-up Study of 7436 Patients. Am. J. Gastroenterol. 2018, 113, 1621–1628. [Google Scholar] [CrossRef] [PubMed]
- Na, Y.S.; Kim, S.G.; Cho, S.J. Risk assessment of metachronous gastric cancer development using OLGA and OLGIM systems after endoscopic submucosal dissection for early gastric cancer: A long-term follow-up study. Gastric Cancer 2023, 26, 298–306. [Google Scholar] [CrossRef]
- Yue, H.; Shan, L.; Bin, L. The significance of OLGA and OLGIM staging systems in the risk assessment of gastric cancer: A systematic review and meta-analysis. Gastric Cancer 2018, 21, 579–587. [Google Scholar] [CrossRef]
- Yun, C.Y.; Kim, N.; Lee, J.; Lee, J.Y.; Hwang, Y.J.; Lee, H.S.; Yoon, H.; Shin, C.M.; Park, Y.S.; Kim, J.W.; et al. Usefulness of OLGA and OLGIM system not only for intestinal type but also for diffuse type of gastric cancer, and no interaction among the gastric cancer risk factors. Helicobacter 2018, 23, e12542. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez de Santiago, E.; Dinis-Ribeiro, M.; Pohl, H.; Agrawal, D.; Arvanitakis, M.; Baddeley, R.; Bak, E.; Bhandari, P.; Bretthauer, M.; Burga, P.; et al. Reducing the environmental footprint of gastrointestinal endoscopy: European Society of Gastrointestinal Endoscopy (ESGE) and European Society of Gastroenterology and Endoscopy Nurses and Associates (ESGENA) Position Statement. Endoscopy 2022, 54, 797–826. [Google Scholar] [CrossRef] [PubMed]
- Pohl, H.; Baddeley, R. Carbon footprint of gastroenterology practice. Gut 2023, 72, 2210–2213. [Google Scholar] [CrossRef] [PubMed]
- Castro, R.; Esposito, G. A single vial is enough in the absence of endoscopic suspected intestinal metaplasia-less is more! Scand. J. Gastroenterol. 2019, 54, 673–677. [Google Scholar] [CrossRef] [PubMed]
- Gordon, I.O.; Sherman, J.D.; Leapman, M. Life Cycle Greenhouse Gas Emissions of Gastrointestinal Biopsies in a Surgical Pathology Laboratory. Am. J. Clin. Pathol. 2021, 156, 540–549. [Google Scholar] [CrossRef] [PubMed]
- Cho, J.H.; Jin, S.Y.; Park, S. Carbon footprint and cost reduction by endoscopic grading of gastric intestinal metaplasia using narrow-band imaging. J. Gastroenterol. Hepatol. 2024, 39, 942–948. [Google Scholar] [CrossRef] [PubMed]
- Dekker, E.; Houwen, B.; Puig, I.; Bustamante-Balén, M.; Coron, E.; Dobru, D.E.; Kuvaev, R.; Neumann, H.; Johnson, G.; Pimentel-Nunes, P.; et al. Curriculum for optical diagnosis training in Europe: European Society of Gastrointestinal Endoscopy (ESGE) Position Statement. Endoscopy 2020, 52, 899–923. [Google Scholar] [CrossRef]
- Houwen, B.; Hassan, C.; Hazewinkel, Y.; Vleugels, J.L.A.; Dinis-Ribeiro, M.; Greuter, M.J.E.; Coupé, V.M.H.; Dekker, E. Methodological framework for development of competence standards for optical diagnosis in gastrointestinal endoscopy: European Society of Gastrointestinal Endoscopy (ESGE) Position Statement. Endoscopy 2022, 54, 84–87. [Google Scholar] [CrossRef]

| Narrow-Band Imaging (NBI) | i-Scan | Linked-Color Imaging (LCI) | |
|---|---|---|---|
| Manufacturer | Olympus Co., Tokyo, Japan | PENTAX Co., Tokyo, Japan | Fujifilm Co., Tokyo, Japan |
| Mode of action | Contrasting light is focused on a narrow area (30 nm) with wavelengths of 415 ± 15 nm (blue) and 540 ± 15 nm (green); differences in mucosal lesions are expressed in color and detailed images including surface mucosal blood vessels | Software-based dynamic image-enhancement technology improving surface enhancement (SE), contrast enhancement (CE), tone enhancement (TE), and tone enhancement mode g improves the visualization of grimly lit far-fi. SE emphasizes contrast based on the data obtained from each pixel and is useful for the detection of lesions. CE enhances the changes in the mucosal surface by adding a blue tint to the relatively dark area using the brightness data of the pixels. TE divides the image into red, green, and blue elements and then recombines a new image by transforming each element, emphasizing the changes. | The use of blue-violet wavelength, a short wavelength of 410 and 450 nm, in addition to the red, green, and blue wavelengths to improve mucosal abnormalities’ detection. The LCI amplifies both blue-violet- and white-light wavelengths; hence, bright red becomes more vivid, and the pale red becomes paler, improving lesion detection. |
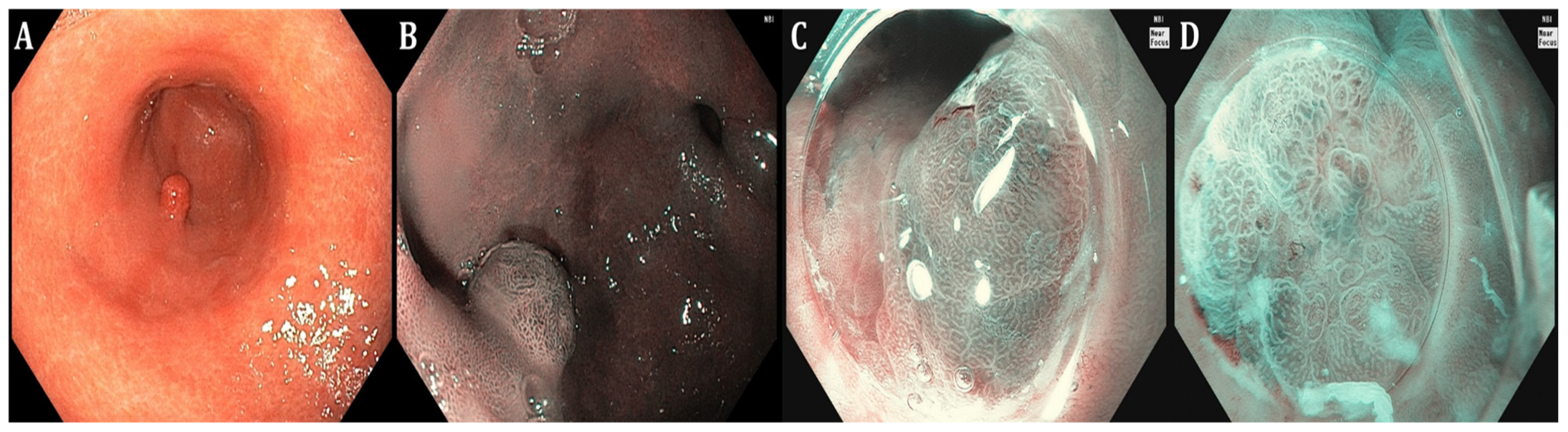
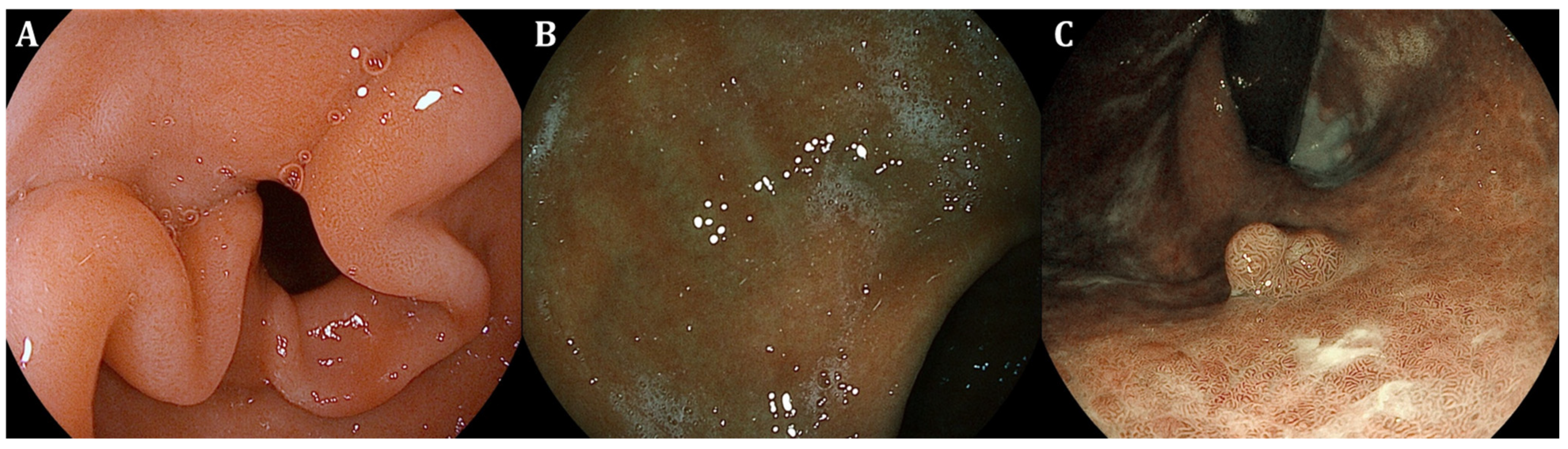
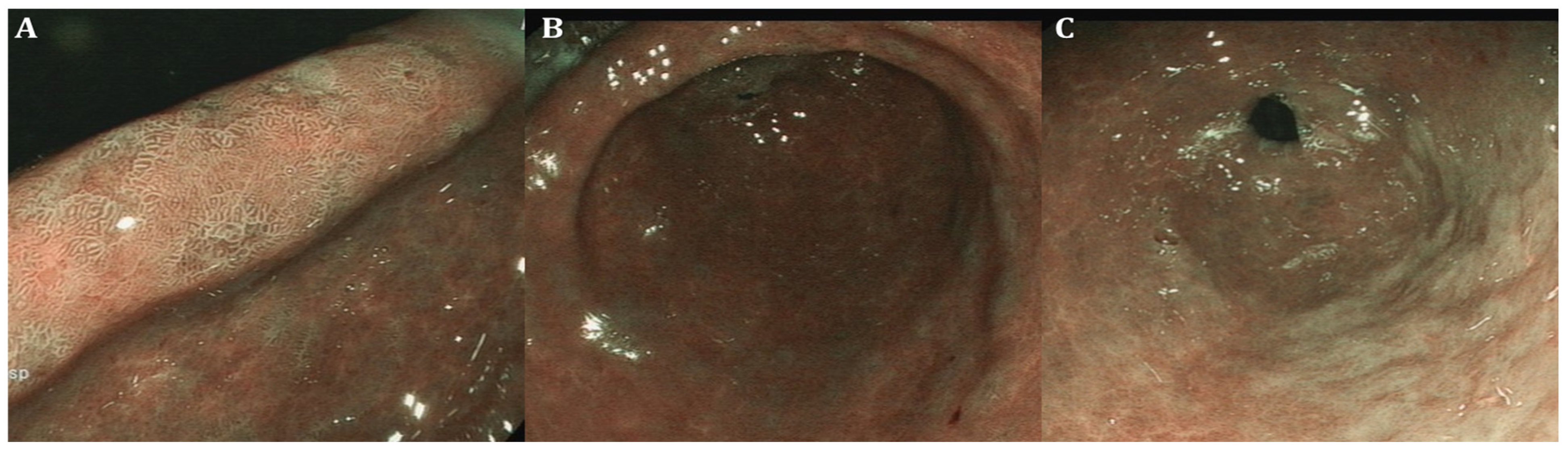
| GIM endoscopic findings | Light-blue crest (LBC) as fine blue–white line on the crest of the epithelial surface, white opaque substance (lipid droplets) obscuring the subepithelial capillaries, multiple pale, elevated patches | Elevated greyish white patches surrounded by pale and normal-color gastric mucosa or blotchy patchy erythema, lipid droplets termed white opaque substance (WOS), patchy reflections of blue–white located on epithelial margins termed light-blue crest | Lavender area, “Lavender color sign” (LCS); “Purple in Mist” (purple mixed with white on the epithelium, with signs of mist detected by non-magnifying LCI observation—PIM); “patchy lavender color” (patchy lavender color with a regular mucosal pattern and a clear border—PLC) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tziatzios, G.; Ziogas, D.Ι.; Gkolfakis, P.; Papadopoulos, V.; Papaefthymiou, A.; Mathou, N.; Giannakopoulos, A.; Gerasimatos, G.; Paraskeva, K.D.; Triantafyllou, K. Endoscopic Grading and Sampling of Gastric Precancerous Lesions: A Comprehensive Literature Review. Curr. Oncol. 2024, 31, 3923-3938. https://doi.org/10.3390/curroncol31070290
Tziatzios G, Ziogas DΙ, Gkolfakis P, Papadopoulos V, Papaefthymiou A, Mathou N, Giannakopoulos A, Gerasimatos G, Paraskeva KD, Triantafyllou K. Endoscopic Grading and Sampling of Gastric Precancerous Lesions: A Comprehensive Literature Review. Current Oncology. 2024; 31(7):3923-3938. https://doi.org/10.3390/curroncol31070290
Chicago/Turabian StyleTziatzios, Georgios, Dimitrios Ι. Ziogas, Paraskevas Gkolfakis, Vasilios Papadopoulos, Apostolis Papaefthymiou, Nikoletta Mathou, Athanasios Giannakopoulos, Gerasimos Gerasimatos, Konstantina D. Paraskeva, and Konstantinos Triantafyllou. 2024. "Endoscopic Grading and Sampling of Gastric Precancerous Lesions: A Comprehensive Literature Review" Current Oncology 31, no. 7: 3923-3938. https://doi.org/10.3390/curroncol31070290
APA StyleTziatzios, G., Ziogas, D. Ι., Gkolfakis, P., Papadopoulos, V., Papaefthymiou, A., Mathou, N., Giannakopoulos, A., Gerasimatos, G., Paraskeva, K. D., & Triantafyllou, K. (2024). Endoscopic Grading and Sampling of Gastric Precancerous Lesions: A Comprehensive Literature Review. Current Oncology, 31(7), 3923-3938. https://doi.org/10.3390/curroncol31070290







