Creation of a Métis-Specific Instrument for Cancer Screening: A Scoping Review of Cancer-Screening Programs and Instruments
Abstract
1. Introduction
Who Are the Métis
2. Materials and Methods
2.1. Data Sources
2.2. Search Strategy
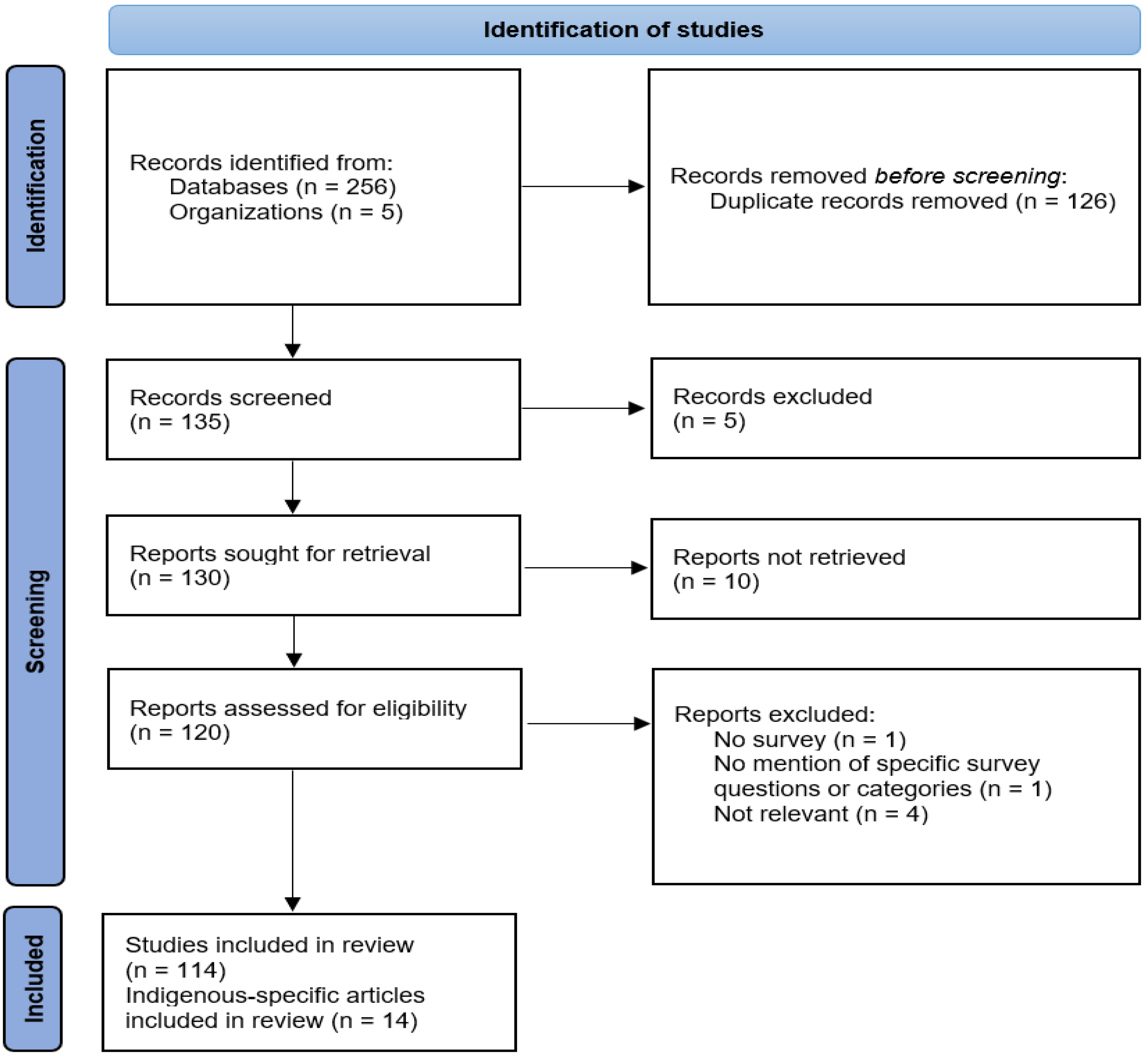
2.3. Study Selection
2.4. Data Collection
2.5. Data Charting
3. Results
3.1. Themes across the Included Articles
3.2. Creation of a Métis-Specific Cancer-Screening Instrument
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Statistics Canada. Cancer Screening, 2017. 2018. Available online: https://www150.statcan.gc.ca/n1/pub/82-625-x/2018001/article/54977-eng.htm (accessed on 7 December 2022).
- Alberta Health Services. Screening For Life—About Us. 2021. Available online: https://screeningforlife.ca/about-us-2/#what_is_screening (accessed on 13 October 2023).
- World Health Organization. Cancer—Screening and Early Detection 2010. Available online: https://www.who.int/europe/news-room/fact-sheets/item/cancer-screening-and-early-detection-of-cancer (accessed on 13 October 2023).
- World Health Organization. When Is Screening for Cancer the Right Course of Action? 2022. Available online: https://www.who.int/europe/news/item/02-02-2022-when-is-screening-for-cancer-the-right-course-of-action (accessed on 13 October 2023).
- Statistics Canada. Cancer Incidence and Mortality Trends, 1984 to 2020. 2022. Available online: https://www150.statcan.gc.ca/n1/daily-quotidien/220204/dq220204b-eng.htm (accessed on 13 October 2023).
- Public Health Agency of Canada. Cervical Cancer Facts and Figures. 2009. Available online: https://www.canada.ca/en/public-health/services/chronic-diseases/cancer/cervical-cancer-facts-figures.html (accessed on 16 October 2023).
- Hayward, A.; Wodtke, L.; Craft, A.; Robin, T.; Smylie, J.; McConkey, S.; Nychuk, A.; Healy, C.; Star, L.; Cidro, J. Addressing the need for indigenous and decolonized quantitative research methods in Canada. SSM—Popul. Health 2021, 15, 100899. [Google Scholar] [CrossRef] [PubMed]
- National Aboriginal History Organization. What Researchers Need from Metis Communities [Fact Sheet]; National Aboriginal History Organization, Ed.; First Nations, Inuit, & Metis Program; National Aboriginal History Organization: Ottawa, ON, Canada, 2010. [Google Scholar]
- Metis Nation of Alberta. History. 2022. Available online: https://albertametis.com/metis-in-alberta/history/ (accessed on 7 December 2022).
- Government of Canada. Indigenous Peoples and Communities. 2022. Available online: https://www.rcaanc-cirnac.gc.ca/eng/1100100013785/1529102490303 (accessed on 30 August 2023).
- Government of Alberta. 2021 Census of Canada Indigenous People. Updated 22 March 2023. Available online: https://open.alberta.ca/dataset/487a7294-06ac-481e-80b7-5566692a6b11/resource/257af6d4-902c-4761-8fee-3971a4480678/download/tbf-2021-census-of-canada-indigenous-people.pdf (accessed on 12 September 2023).
- Indigenous Relations. Metis Settlements and First Nations in Alberta Community Profiles. 2022, pp. 17–63. Available online: https://open.alberta.ca/dataset/d3004449-9668-4d02-bb88-f57d381a6965/resource/b842fced-7f67-42b3-adc2-65eee7f79974/download/ir-metis-settlements-and-first-nations-in-alberta-community-profiles-2022-04.pdf (accessed on 7 September 2023).
- Brock, T.; Chowdhury, M.A.; Carr, T.; Panahi, A.; Friesen, M.; Groot, G. Métis Peoples and Cancer: A Scoping Review of Literature, Programs, Policies and Educational Material in Canada. Curr. Oncol. 2021, 28, 5101–5123. [Google Scholar] [CrossRef] [PubMed]
- Withrow, D.R.; Amartey, A.; Marrett, L.D. Cancer risk factors and screening in the off-reserve First Nations, Métis and non-Aboriginal populations of Ontario. Chronic Dis. Inj. Can. 2014, 34, 103–112. [Google Scholar] [CrossRef] [PubMed]
- Crouse, A.; Sadrzadeh, S.M.H.; de Koning, L.; Naugler, C. Sociodemographic correlates of fecal immunotesting for colorectal cancer screening. Clin. Biochem. 2015, 48, 105–109. [Google Scholar] [CrossRef] [PubMed]
- Mazereeuw, M.V.; Withrow, D.R.; Nishri, E.D.; Tjepkema, M.; Vides, E.; Marrett, L.D. Cancer incidence and survival among Métis adults in Canada: Results from the Canadian census follow-up cohort (1992–2009). CMAJ 2018, 190, E320–E326. [Google Scholar] [CrossRef]
- Hutchinson, P.; Tobin, P.; Muirhead, A.; Robinson, N. Closing the gaps in cancer screening with First Nations, Inuit, and Métis populations: A narrative literature review. J. Indig. Wellbeing 2018, 3, 3–17. [Google Scholar]
- Canadian Institutes of Health Research; Natural Sciences and Engineering Research Council of Canada; Social Sciences and Humanities Research Council of Canada. Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans—TCPS 2 (2022). 2022. Available online: https://ethics.gc.ca/eng/policy-politique_tcps2-eptc2_2022.html (accessed on 31 August 2023).
- National Aboriginal History Organization. Principles of Ethical Métis Research. Available online: https://fnim.sehc.com/getmedia/bd0ef9fd-a05d-4b01-9cbd-6a7ca93f4f22/PrinciplesofEthicalMetisResearch-descriptive_001.pdf.aspx?ext=.pdf (accessed on 31 August 2023).
- The First Nations Information Governance Centre. The First Nations Principles of OCAP®. 2023. Available online: https://fnigc.ca/ocap-training/ (accessed on 31 August 2023).
- Statistics Canada. Canadian Community Health Survey(CCHS)—Annual Component—2020. 2020. Available online: https://www23.statcan.gc.ca/imdb/p3Instr.pl?Function=assembleInstr&Item_Id=1262397 (accessed on 30 August 2023).
- Tomić, S.D.; Ćorić, A.; Tomić, S.; Mujičić, E.; Malenković, J.; Šljivo, A.; Malenković, G. Cervical Cancer Prevention Knowledge (Cckp-64) among Female Students in Novi Sad, Serbia during COVID-19 Pandemic. Healthcare 2023, 11, 1400. [Google Scholar] [CrossRef]
- Sharif Nia, H.; Behmanesh, F.; Kwok, C.; Firouzbakht, M.; Ebadi, A.; Nikpour, M. Breast cancer screening beliefs questionnaire: Psychometric properties of the Persian version. BMC Women’s Health 2020, 20, 184. [Google Scholar] [CrossRef]
- Bingham, B.; Moniruzzaman, A.; Patterson, M.; Sareen, J.; Distasio, J.; O’Neil, J.; Somers, J.M. Gender differences among Indigenous Canadians experiencing homelessness and mental illness. BMC Psychol. 2019, 7, 57. [Google Scholar] [CrossRef]
- Métis Nation of Ontario. A Place in the Circle: Understanding and Supporting Two-Spirit People 2022. Available online: https://www.metisnation.org/wp-content/uploads/2022/09/2S-Awareness-Resource_2022a.pdf (accessed on 27 January 2023).
- Kwok, C.; Fethney, J.; White, K. Breast cancer screening practices among Chinese-Australian women. Eur. J. Oncol. Nurs. 2012, 16, 247–252. [Google Scholar] [CrossRef]
- Kwok, C.; Fethney, J.; White, K. Chinese Breast Cancer Screening Beliefs Questionnaire: Development and psychometric testing with Chinese-Australian women. J. Adv. Nurs. 2010, 66, 191–200. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.Y.; Lee, E.E.; Rhee, Y.S.; Yang, E.Y.; Shin, J.H.; Lee, S. Adaptation and validation of the health belief model scale for colorectal cancer screening. Nurs. Health Sci. 2020, 22, 355–363. [Google Scholar] [CrossRef] [PubMed]
- Baena-Cañada, J.M.; Rosado-Varela, P.; Expósito-Álvarez, I.; González-Guerrero, M.; Nieto-Vera, J.; Benítez-Rodríguez, E. Women’s perceptions of breast cancer screening. Spanish screening programme survey. Breast 2014, 23, 883–888. [Google Scholar] [CrossRef] [PubMed]
- Cerigo, H.; Macdonald, M.E.; Franco, E.L.; Brassard, P. Awareness and knowledge about human papillomavirus among Inuit women in Nunavik, Quebec. J. Community Health Public Health Promot. Dis. Prev. 2011, 36, 56–62. [Google Scholar] [CrossRef] [PubMed]
- Blaes, A.; Vogel, R.I.; Nagler, R.H.; Allen, A.; Mason, S.; Teoh, D.; Talley, K.; Raymond, N.C.; Wyman, J.F. Breast Cancer Screening Practices for High-Risk Women: A Cross-Sectional Survey of Primary Care Providers. J. Women’s Health 2020, 29, 686–692. [Google Scholar] [CrossRef] [PubMed]
- Champion, V.; Skinner, C.S.; Menon, U. Development of a self-efficacy scale for mammography. Res. Nurs. Health 2005, 28, 329–336. [Google Scholar] [CrossRef]
- Khazaee-Pool, M.; Majlessi, F.; Montazeri, A.; Pashaei, T.; Gholami, A.; Ponnet, K. Development and psychometric testing of a new instrument to measure factors influencing women’s breast cancer prevention behaviors (ASSISTS). BMC Women’s Health 2016, 16, 40. [Google Scholar]
- Kwok, C.; Endrawes, G.; Lee, C.F. Breast Cancer Screening Beliefs Questionnaire: Psychometric properties assessment of the Arabic version. Eur. J. Oncol. Nurs. 2016, 20, 42–48. [Google Scholar] [CrossRef]
- Smith, A.; Christopher, S.; McCormick, A.K. Development and implementation of a culturally sensitive cervical health survey: A community-based participatory approach. Women Health 2004, 40, 67–86. [Google Scholar] [CrossRef]
- Amlani, B.; Radaelli, F.; Bhandari, P. A survey on colonoscopy shows poor understanding of its protective value and widespread misconceptions across Europe. PLoS ONE 2020, 15, e0233490. [Google Scholar] [CrossRef]
- Lopez-McKee, G. Development of the mammography beliefs and attitudes questionnaire for low-health-literacy Mexican-American women. Online J. Issues Nurs. 2010, 16, 7. [Google Scholar] [CrossRef] [PubMed]
- Ndikum-Moffor, F.M.; Braiuca, S.; Daley, C.M.; Gajewski, B.J.; Engelman, K.K. Assessment of mammography experiences and satisfaction among American Indian/Alaska Native women. Womens Health Issues 2013, 23, e395–e402. [Google Scholar] [CrossRef] [PubMed]
- Wampler, N.S.; Ryschon, T.; Manson, S.M.; Buchwald, D. Knowledge, Attitudes, and Beliefs Regarding Breast Cancer Among American Indian Women From the Northern Plains. J. Appl. Gerontol. 2006, 25 (Suppl. 1), 44S–59S. [Google Scholar] [CrossRef]
- Brown, S.R.; Nuno, T.; Joshweseoma, L.; Begay, R.C.; Goodluck, C.; Harris, R.B. Impact of a community-based breast cancer screening program on Hopi women. Prev. Med. 2011, 52, 390–393. [Google Scholar] [CrossRef] [PubMed]
- Brown, S.R.; Joshweseoma, L.; Saboda, K.; Sanderson, P.; Ami, D.; Harris, R. Cancer screening on the Hopi reservation: A model for success in a Native American community. J. Community Health Public Health Promot. Dis. Prev. 2015, 40, 1165–1172. [Google Scholar] [CrossRef] [PubMed]
- Babyar, J. In search of Pan-American indigenous health and harmony. Glob. Health 2019, 15, 16. [Google Scholar] [CrossRef] [PubMed]
- Cavanagh, B.M.; Wakefield, C.E.; McLoone, J.K.; Garvey, G.; Cohn, R.J. Cancer survivorship services for indigenous peoples: Where we stand, where to improve? A systematic review. J. Cancer Surviv. 2016, 10, 330–341. [Google Scholar] [CrossRef]
- First Nations Information Governance Centre. National Report of the First Nations Regional Health Survey Phase 3. 2018: Ottawa; First Nations Information Governance Centre: Ottawa, ON, Canada, 2018; p. 181. [Google Scholar]
- Chow, S.; Bale, S.; Sky, F.; Wesley, S.; Beach, L.; Hyett, S.; Heiskanen, T.; Gillis, K.-J.; Paroschy Harris, C. The Wequedong Lodge Cancer Screening Program: Implementation of an opportunistic cancer screening pilot program for residents of rural and remote Indigenous communities in Northwestern Ontario, Canada. Rural. Remote Health 2020, 20, 5576. [Google Scholar] [CrossRef]
- Engelman, K.K.; Daley, C.M.; Gajewski, B.J.; Ndikum-Moffor, F.; Faseru, B.; Braiuca, S.; Joseph, S.; Ellerbeck, E.F.; Greiner, K.A. An assessment of American Indian women’s mammography experiences. BMC Womens Health 2010, 10, 34. [Google Scholar] [CrossRef]
- Haverkamp, D.; Perdue, D.G.; Espey, D.; Cobb, N. A survey of Indian Health Service and tribal health providers’ colorectal cancer screening knowledge, perceptions, and practices. J. Health Care Poor Underserved 2011, 22, 243–257. [Google Scholar] [CrossRef]
- Moreland, S.; Engelman, K.; Greiner, K.A.; Mayo, M.S. Papanicolaou testing among Native American and Hispanic populations. Ethn. Dis. 2006, 16, 223–227. [Google Scholar] [PubMed]
- Orians, C.E.; Erb, J.; Kenyon, K.L.; Lantz, P.M.; Liebow, E.B.; Joe, J.R.; Burhansstipanov, L. Public education strategies for delivering breast and cervical cancer screening in American Indian and Alaska Native populations. J. Public Health Manag. Pract. JPHMP 2004, 10, 46–53. [Google Scholar] [CrossRef] [PubMed]
- Sanderson, P.R.; Weinstein, N.; Teufel-Shone, N.; Martínez, M.E. Assessing colorectal cancer screening knowledge at tribal fairs. Prev. Chronic Dis. 2011, 8, A16. [Google Scholar] [PubMed]
- Solomon, T.G.; Gottlieb, N.H. Measures of American Indian traditionality and its relationship to cervical cancer screening. Health Care Women Int. 1999, 20, 493–504. [Google Scholar]
- Soonhee, R.; Burnette, C.E.; Kyoung Hag, L.; Yeon-Shim, L.; Goins, R.T. Correlates of Receipt of Colorectal Cancer Screening among American Indians in the Northern Plains. Soc. Work. Res. 2016, 40, 95–104. [Google Scholar] [CrossRef]
| Concept | Synonym (Keyword) | Synonym (MeSH) |
|---|---|---|
| Questionnaires | Survey*; questionnaire*; “instrument development”; psychometric*; scale*; metric*; benchmark*; matrix; measure*; indicator* | “surveys and questionnaires”; psychometrics; benchmarking |
| Evaluation | Knowledge; validat*; belief*; “psychometric testing”; assess*; evaluat* | Knowledge; health knowledge, attitudes, practice; validation study; culture; evaluation study |
| Cancer Screening Programs | “early detection of cancer”; “mass screening; “cancer prevention”; “cancer screening”; screen* adj3 cancer | “early detection of cancer”; mass screening |
| Cancer Types | “breast cancer”; “breast neoplasm*”; “breast carcinoma”; “breast tumor*” ’ “breast tumour*”; “cervical cancer”; “cervical neoplasm*”; “cervical carcinoma”; “cervical tumor*”; “cervical tumour*”; “colorectal cancer”; “colorectal neoplasm*”; “colorectal carcinoma”; “colorectal tumor*”; “colorectal tumour*”; “colon cancer”; “colonic neoplasm*”; “colonic carcinoma”; “colonic tumour*”; “colonic tumor*”; “colon neoplasm*”; “colon carcinoma”; “colon tumor*”; “colon tumour*”; “rectal cancer”; “rectal neoplasm*”; “rectal carcinoma”; “rectal tumor*”; “rectal tumour*” | breast neoplasms; uterine cervical neoplasms; colorectal neoplasms; colonic neoplasms; rectal neoplasms |
| Cancer 1 | Cancer; neoplasm*; carcinoma; tumor*; tumour*; oncology; “medical oncology” | neoplasms; carcinoma; medical oncology |
| Breast/Cervix/Colon/Rectum | Breast; cervix | Breast; cervix uteri; colon; rectum |
| Breast/Cervical/Colorectal Cancer Screening | “breast cancer screening”; “cervical cancer screening”; “colorectal cancer screening”; screen* adj3 “breast cancer”; screen* adj3 “cervical cancer”; screen* adj3 “colorectal cancer”; mammography; mammogram*; “pap smear”; “Papanicolaou test”; “fecal immunochemical test”; “faecal immunochemical test”; “fecal occult blood test”; “faecal occult blood test”; colonoscopy | Mammography; Papanicolaou Test; occult blood; colonoscopy |
| Indigenous/Aboriginal 2 | Indigenous; Aboriginal; Metis; Inuit*; “First Nations”; “native people”; “native Canadian”; Maori; “native American” | indigenous peoples; indigenous Canadians; American natives; Indians, North American; Inuits; oceanic ancestry group |
| Umbrella Terms | Top Sub-Themes |
|---|---|
| Attitudes | Health motivation, general health motivation, general health checkup, asymptomatic screening, self-efficacy |
| Knowledge | Awareness of cure, purpose of screening, awareness of risk factors, awareness of screening practices |
| Behaviours | Screening history, screening behaviour(s) |
| Beliefs | Faith of cure, fate, perceived barriers, perceived benefits, perceived risk, perceived susceptibility, severity of cancer |
| Barriers | Embarrassment, lack of insurance, cost, language barriers, transportation, worry |
| Facilitators | Prior screening, good physician experience, social support, provider recommendation |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Letendre, A.; Khan, M.; Bartel, R.; Chiang, B.; James, A.; Shewchuk, B.; Kima, J.; Macphail, M.; Vaska, M.; Schwann, M.; et al. Creation of a Métis-Specific Instrument for Cancer Screening: A Scoping Review of Cancer-Screening Programs and Instruments. Curr. Oncol. 2023, 30, 9849-9859. https://doi.org/10.3390/curroncol30110715
Letendre A, Khan M, Bartel R, Chiang B, James A, Shewchuk B, Kima J, Macphail M, Vaska M, Schwann M, et al. Creation of a Métis-Specific Instrument for Cancer Screening: A Scoping Review of Cancer-Screening Programs and Instruments. Current Oncology. 2023; 30(11):9849-9859. https://doi.org/10.3390/curroncol30110715
Chicago/Turabian StyleLetendre, Angeline, Momtafin Khan, Reagan Bartel, Bonnie Chiang, Ashton James, Brittany Shewchuk, June Kima, Meghan Macphail, Marcus Vaska, Monica Schwann, and et al. 2023. "Creation of a Métis-Specific Instrument for Cancer Screening: A Scoping Review of Cancer-Screening Programs and Instruments" Current Oncology 30, no. 11: 9849-9859. https://doi.org/10.3390/curroncol30110715
APA StyleLetendre, A., Khan, M., Bartel, R., Chiang, B., James, A., Shewchuk, B., Kima, J., Macphail, M., Vaska, M., Schwann, M., Yang, H., & Kopciuk, K. A. (2023). Creation of a Métis-Specific Instrument for Cancer Screening: A Scoping Review of Cancer-Screening Programs and Instruments. Current Oncology, 30(11), 9849-9859. https://doi.org/10.3390/curroncol30110715






