Examining the Landscape of Prognostic Factors and Clinical Outcomes for Cancer Control
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Data Collection
2.2.1. Sampling and Recruitment of Study Participants
2.2.2. Interview Procedure
2.3. Data Analysis
3. Results
3.1. Participant Characteristics
3.2. Scope of Currently Collected Prognostic Factors and Outcomes
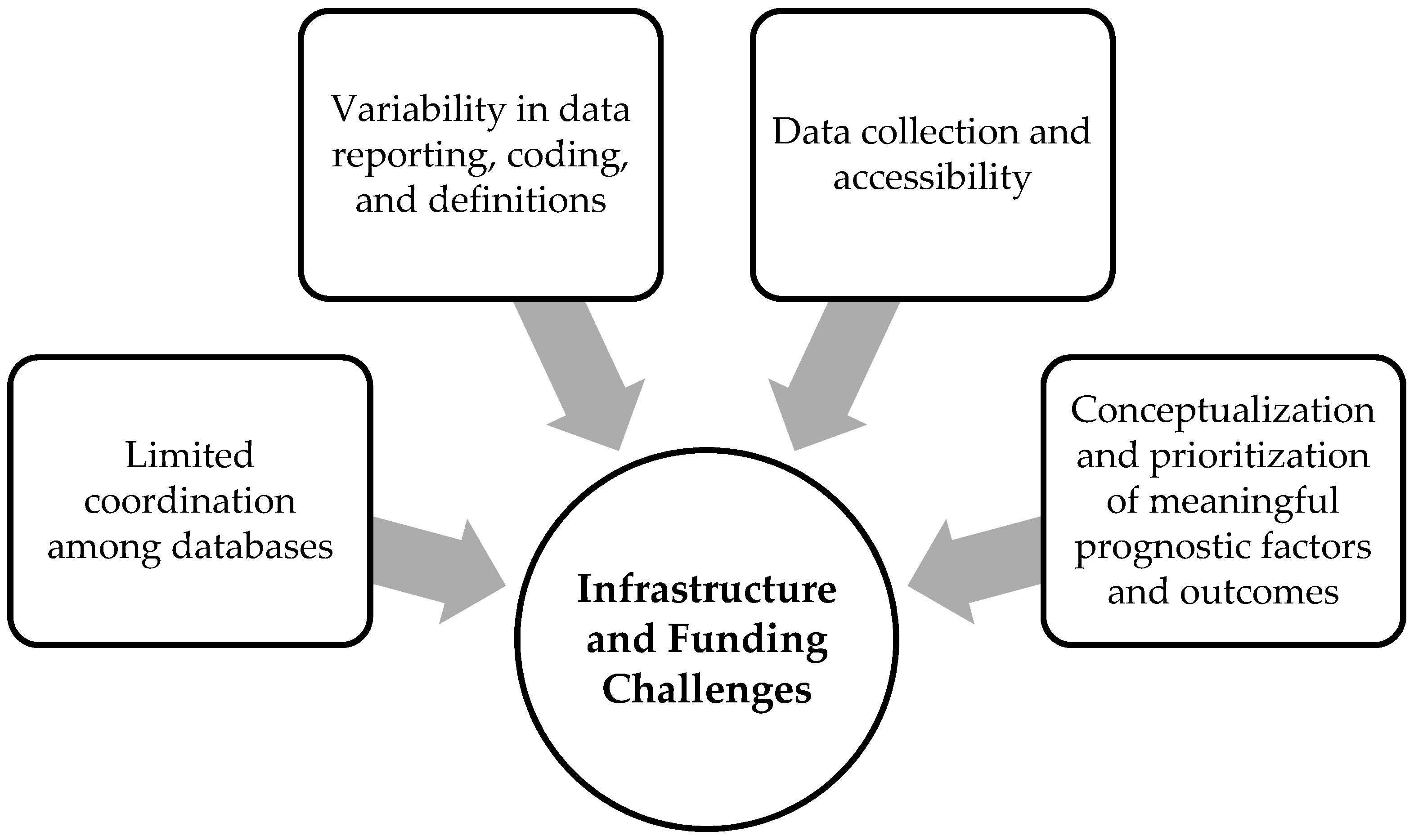
3.3. Infrstructure and Funding Challenges
3.3.1. Data Collection and Accessibility
3.3.2. Limited Coordination among Databases
3.3.3. Variability in Data Reporting, Coding, and Definitions
3.3.4. Conceptualization and Prioritization of Meaningful Prognostic Factors and Outcomes
3.4. Future Priorities for Cancer Control
3.4.1. Global Investment and Intention in Cancer Surveillance
3.4.2. Data Governance and Exchange Globally
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Moons, K.G.M.; Royston, P.; Vergouwe, Y.; Grobbee, D.E.; Altman, D.G. Prognosis and prognostic research: What, why, and how? BMJ 2009, 338, b375. [Google Scholar] [CrossRef]
- Ruffini, E.; Weder, W.; Filosso, P.L.; Girard, N. 56—Thymic Tumors. In IASLC Thoracic Oncology, 2nd ed.; Pass, H.I., Ball, D., Scagliotti, G.V., Eds.; Elsevier: Philadelphia, PA, USA, 2018; pp. 569–589.e4. [Google Scholar]
- Mierzynska, J.; Piccinin, C.; Pe, M.; Martinelli, F.; Gotay, C.; Coens, C.; Mauer, M.; Eggermont, A.; Groenvold, M.; Bjordal, K.; et al. Prognostic value of patient-reported outcomes from international randomised clinical trials on cancer: A systematic review. Lancet Oncol. 2019, 20, e685–e698. [Google Scholar] [CrossRef]
- Hui, D.; Paiva, C.E.; del Fabbro, E.G.; Steer, C.; Naberhuis, J.; van de Wetering, M.; Fernandez-Ortega, P.; Morita, T.; Suh, S.Y.; Bruera, E.; et al. Prognostication in advanced cancer: Update and directions for future research. Support Care Cancer 2019, 27, 1973–1984. [Google Scholar] [CrossRef]
- Miller, K. Prognosis in cancer. Lancet Oncol. 2008, 9, 711. [Google Scholar] [CrossRef]
- Gramling, R.; Carroll, T.; Epstein, R.M. Chapter 40—What Is Known About Prognostication in Advanced Illness? In Evidence-Based Practice in Palliative Medicine; Goldstein, N.E., Morrison, R.S., Eds.; W.B. Saunders: Philadelphia, PA, USA, 2013; pp. 228–234. [Google Scholar]
- Glare, P.; Sinclair, C.; Downing, M.; Stone, P.; Maltoni, M.; Vigano, A. Predicting survival in patients with advanced disease. Eur. J. Cancer 2008, 44, 1146–1156. [Google Scholar] [CrossRef] [PubMed]
- Riley, R.D.; Abrams, K.R.; Sutton, A.J.; Lambert, P.C.; Jones, D.R.; Heney, D.; Burchill, S.A. Reporting of prognostic markers: Current problems and development of guidelines for evidence-based practice in the future. Br. J. Cancer 2003, 88, 1191–1198. [Google Scholar] [CrossRef]
- Chen, V.W.; Hsieh, M.C.; Charlton, M.E.; Ruiz, B.A.; Karlitz, J.; Altekruse, S.F.; Ries, L.A.; Jessup, J.M. Analysis of stage and clinical/prognostic factors for colon and rectal cancer from SEER registries: AJCC and collaborative stage data collection system. Cancer 2014, 120 (Suppl. 23), 3793–3806. [Google Scholar] [CrossRef]
- Parkin, D.M.; Bray, F. Evaluation of data quality in the cancer registry: Principles and methods Part II. Completeness. Eur. J. Cancer 2009, 45, 756–764. [Google Scholar] [CrossRef]
- Zachary, I.; Boren, S.A.; Simoes, E.; Jackson-Thompson, J.; Davis, J.W.; Hicks, L. Information Management in Cancer Registries: Evaluating the Needs for Cancer Data Collection and Cancer Research. Online J. Public Health Inf. 2015, 7, e213. [Google Scholar] [CrossRef]
- Jiang, W.; Kang, Y.; Shi, G.Y.; Zhang, H.Y.; Cai, L.; Sun, X.W.; Sun, L.C.; Sui, G.J. Comparisons of multiple characteristics between young and old lung cancer patients. Chin. Med. J. 2012, 125, 72–80. [Google Scholar] [PubMed]
- Johnson, D.R.; Galanis, E. Incorporation of prognostic and predictive factors into glioma clinical trials. Curr. Oncol. Rep. 2013, 15, 56–63. [Google Scholar] [CrossRef] [PubMed]
- Srigley, J.R.; Amin, M.; Boccon-Gibod, L.; Egevad, L.; Epstein, J.I.; Humphrey, P.A.; Mikuz, G.; Newling, D.; Nilsson, S.; Sakr, W.; et al. Prognostic and predictive factors in prostate cancer: Historical perspectives and recent international consensus initiatives. Scand. J. Urol. Nephrol. 2005, 39 (Suppl. 216), 8–19. [Google Scholar] [CrossRef]
- Sheu, S.J.; Wei, I.L.; Chen, C.H.; Yu, S.; Tang, F.I. Using snowball sampling method with nurses to understand medication administration errors. J. Clin. Nurs. 2009, 18, 559–569. [Google Scholar] [CrossRef] [PubMed]
- Sundler, A.J.; Lindberg, E.; Nilsson, C.; Palmer, L. Qualitative thematic analysis based on descriptive phenomenology. Nurs. Open 2019, 6, 733–739. [Google Scholar] [CrossRef]
- Gospodarowicz, M.; O’Sullivan, B.; Sobin, L.H. Prognostic Factors in Cancer, 3rd ed.; Union for International Cancer Control; John Wiley & Sons: Hoboken, NJ, USA, 2006. [Google Scholar]
- Guest, G.; Namey, E.; Chen, M. A simple method to assess and report thematic saturation in qualitative research. PLoS ONE 2020, 15, e0232076. [Google Scholar] [CrossRef] [PubMed]
- Gospodarowicz, M.; Mackillop, W.; O’Sullivan, B.; Sobin, L.; Henson, D.; Hutter, R.V.; Wittekind, C. Prognostic factors in clinical decision making. Cancer 2001, 91, 1688–1695. [Google Scholar] [CrossRef]
- Brierley, J.D.; Gospodarowicz, M.K.; Wittekind, C. Union for International Cancer Control. In TNM Classification of Malignant Tumors; Wiley: New York, NY, USA, 2017; ISBN 978-1-119-26357-9. [Google Scholar]
- Brierley, J.D.; Gospodarowicz, M.; Wittekind, C. TNM Classification of Malignant Tumours, 8th ed.; Wiley-Blackwell: Hoboken, NJ, USA, 2016; ISBN 978-1-119-26356-2. [Google Scholar]
- Sculier, J.P.; Chansky, K.; Crowley, J.J.; van Meerbeeck, J.; Goldstraw, P. The impact of additional prognostic factors on survival and their relationship with the anatomical extent of disease expressed by the 6th Edition of the TNM Classification of Malignant Tumors and the proposals for the 7th Edition. J. Thorac. Oncol. 2008, 3, 457–466. [Google Scholar] [CrossRef]
- Galon, J.; Fridman, W.H.; Pages, F. The adaptive immunologic microenvironment in colorectal cancer: A novel perspective. Cancer Res. 2007, 67, 1883–1886. [Google Scholar] [CrossRef]
- Carrell, D.S.; Halgrim, S.; Tran, D.T.; Buist, D.S.; Chubak, J.; Chapman, W.W.; Savova, G. Using natural language processing to improve efficiency of manual chart abstraction in research: The case of breast cancer recurrence. Am. J. Epidemiol. 2014, 179, 749–758. [Google Scholar] [CrossRef]
- Warren, J.L.; Yabroff, K.R. Challenges and opportunities in measuring cancer recurrence in the United States. J. Natl. Cancer Inst. 2015, 107, djv134. [Google Scholar] [CrossRef]
- Xu, Y.; Kong, S.; Cheung, W.Y.; Bouchard-Fortier, A.; Dort, J.C.; Quan, H.; Buie, E.M.; McKinnon, G.; Quan, M.L. Development and validation of case-finding algorithms for recurrence of breast cancer using routinely collected administrative data. BMC Cancer 2019, 19, 210. [Google Scholar] [CrossRef]
- Basch, E. Patient-Reported Outcomes—Harnessing Patients’ Voices to Improve Clinical Care. N. Engl. J. Med. 2017, 376, 105–108. [Google Scholar] [CrossRef] [PubMed]
- Sisodia, R.C.; Dankers, C.; Orav, J.; Joseph, B.; Meyers, P.; Wright, P.; Amand, D.S.; del Carmen, M.; Ferris, T.; Heng, M.; et al. Factors Associated with Increased Collection of Patient-Reported Outcomes Within a Large Health Care System. JAMA Netw. Open 2020, 3, e202764. [Google Scholar] [CrossRef]
- Chow, A.; Mayer, E.K.; Darzi, A.W.; Athanasiou, T. Patient-reported outcome measures: The importance of patient satisfaction in surgery. Surgery 2009, 146, 435–443. [Google Scholar] [CrossRef] [PubMed]
- Basch, E.; Deal, A.M.; Dueck, A.C.; Scher, H.I.; Kris, M.G.; Hudis, C.; Schrag, D. Overall Survival Results of a Trial Assessing Patient-Reported Outcomes for Symptom Monitoring During Routine Cancer Treatment. JAMA 2017, 318, 197–198. [Google Scholar] [CrossRef] [PubMed]
- Willems, S.M.; Abeln, S.; Feenstra, K.A.; de Bree, R.; van der Poel, E.F.; de Jong, R.J.B.; Heringa, J.; van den Brekel, M.W.M. The potential use of big data in oncology. Oral. Oncol. 2019, 98, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Rutella, S.; Cannarile, M.A.; Gnjatic, S.; Gomes, B.; Guinney, J.; Karanikas, V.; Karkada, M.; Kirkwood, J.M.; Kotlan, B.; Masucci, G.V.; et al. Society for Immunotherapy of Cancer clinical and biomarkers data sharing resource document: Volume I—Conceptual challenges. J. Immunother. Ther. Cancer 2020, 8, e001389. [Google Scholar] [CrossRef] [PubMed]
- Andersen, M.R.; Storm, H.H. Cancer registration, public health and the reform of the European data protection framework: Abandoning or improving European public health research? Eur. J. Cancer 2015, 51, 1028–1038. [Google Scholar] [CrossRef]
- Ellis, L.; Woods, L.M.; Estève, J.; Eloranta, S.; Coleman, M.P.; Rachet, B. Cancer incidence, survival and mortality: Explaining the concepts. Int. J. Cancer 2014, 135, 1774–1782. [Google Scholar] [CrossRef] [PubMed]
- Siesling, S.; Louwman, W.J.; Kwast, A.; van den Hurk, C.; O’Callaghan, M.; Rosso, S.; Zanetti, R.; Storm, H.; Comber, H.; Steliarova-Foucher, E.; et al. Uses of cancer registries for public health and clinical research in Europe: Results of the European Network of Cancer Registries survey among 161 population-based cancer registries during 2010–2012. Eur. J. Cancer 2015, 51, 1039–1049. [Google Scholar] [CrossRef] [PubMed]
- Nikiema, J.N.; Jouhet, V.; Mougin, F. Integrating cancer diagnosis terminologies based on logical definitions of SNOMED CT concepts. J. Biomed. Inform. 2017, 74, 46–58. [Google Scholar] [CrossRef] [PubMed]
- Krumm, R.; Semjonow, A.; Tio, J.; Duhme, H.; Bürkle, T.; Haier, J.; Dugas, M.; Breil, B. The need for harmonized structured documentation and chances of secondary use—Results of a systematic analysis with automated form comparison for prostate and breast cancer. J. Biomed. Inform. 2014, 51, 86–99. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Chow, Z.L.; Indave, B.I.; Lokuhetty, M.D.S.; Ochiai, A.; Cree, I.A.; White, V.A. Misleading terminology in pathology: Lack of definitions hampers communication. Virchows Arch 2021, 479, 425–430. [Google Scholar] [CrossRef]
- Rolland, B.; Reid, S.; Stelling, D.; Warnick, G.; Thornquist, M.; Feng, Z.; Potter, J.D. Toward Rigorous Data Harmonization in Cancer Epidemiology Research: One Approach. Am. J. Epidemiol. 2015, 182, 1033–1038. [Google Scholar] [CrossRef] [PubMed]
- Eden, M.; Harrison, S.; Griffin, M.; Lambe, M.; Pettersson, D.; Gavin, A.; Brewster, D.H.; Lin, Y.; Johannesen, T.B.; Milne, R.L.; et al. Impact of variation in cancer registration practice on observed international cancer survival differences between International Cancer Benchmarking Partnership (ICBP) jurisdictions. Cancer Epidemiol. 2019, 58, 184–192. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Liang, F.; Tannock, I. Use and misuse of common terminology criteria for adverse events in cancer clinical trials. BMC Cancer 2016, 16, 392. [Google Scholar] [CrossRef]
- White, M.C.; Babcock, F.; Hayes, N.S.; Mariotto, A.B.; Wong, F.L.; Kohler, B.A.; Weir, H.K. The history and use of cancer registry data by public health cancer control programs in the United States. Cancer 2017, 123 (Suppl. 24), 4969–4976. [Google Scholar] [CrossRef] [PubMed]
- Chen, V.W.; Eheman, C.R.; Johnson, C.J.; Hernandez, M.N.; Rousseau, D.; Styles, T.S.; West, D.W.; Hsieh, M.; Hakenewerth, A.M.; Celaya, M.O.; et al. Enhancing cancer registry data for comparative effectiveness research (CER) project: Overview and methodology. J. Regist. Manag. 2014, 41, 103–112. [Google Scholar]
| Prognostic Factors and Outcomes | Category | Data Points Reported by Participants | Representative Quotes |
|---|---|---|---|
| Disease Characteristics | Tumour Characteristics |
| “…Standardizing the quality of pathology reporting would be part of this exercise because if you don’t get reliable pathology reporting, like grade or degree of differentiation and so on, you’re likely to end up with inaccurate information.” (P03) |
| Anatomic disease extent |
| “…it’s very difficult to understand outcomes if you can’t adjust for the stage or understand the stage (at presentation). I think stage is a surrogate for access challenges in low- and middle-income countries—those can be geographic, financial, and cultural” (P01) | |
| Host-related prognostic factors | Demographics |
| “…we don’t collect ethnicity data routinely in our health data sets, and it’s very challenging to understand structural inequalities in health care, access, and uptake as a result of the ethnic and sociocultural variables if you don’t collect that data.” (P01) |
| Co-morbidities |
| “In an ideal world, we would have a robust marker of co-morbidity…co-morbidity would be very problematic and probably lack uniformity” (P02) “We could probably include five or ten different things across all cancers that would be really important to have, like smoking status, body mass index, alcohol exposure.” (P02) | |
| Environment-related prognostic factors & Social Determinants of Health | Access to treatment |
| “…how a patient pays at the point of care—do they have to pay out of pocket, is there a government-funded insurance scheme, a social insurance scheme, is it private insurance, or is there a tax payer funded health system that includes cancer care?” (P01) “…something that is often missing is reasons for non-treatment. Is it because they were not referred? Is it because they saw the doctor, and it was not recommended, or is it because it was recommended, and the patient elected not to have it, and if so, what was the reason? Fear, personal preference values, financial toxicity?” (P02) |
| Quality of Care |
| ||
| Outcomes | Disease Outcomes |
| “We’re really interested in binary outcomes. Does the patient survive and for how long?” (P08) “In an ideal world, date of relapse, some patient-reported outcomes, quality of life data. That would be the core group of outcomes.” (P03) |
| Quality of Life Outcomes |
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Giuliani, M.E.; Giannopoulos, E.; Gospodarowicz, M.K.; Broadhurst, M.; O’Sullivan, B.; Tittenbrun, Z.; Johnson, S.; Brierley, J. Examining the Landscape of Prognostic Factors and Clinical Outcomes for Cancer Control. Curr. Oncol. 2021, 28, 5155-5166. https://doi.org/10.3390/curroncol28060432
Giuliani ME, Giannopoulos E, Gospodarowicz MK, Broadhurst M, O’Sullivan B, Tittenbrun Z, Johnson S, Brierley J. Examining the Landscape of Prognostic Factors and Clinical Outcomes for Cancer Control. Current Oncology. 2021; 28(6):5155-5166. https://doi.org/10.3390/curroncol28060432
Chicago/Turabian StyleGiuliani, Meredith Elana, Eleni Giannopoulos, Mary Krystyna Gospodarowicz, Michaela Broadhurst, Brian O’Sullivan, Zuzanna Tittenbrun, Sonali Johnson, and James Brierley. 2021. "Examining the Landscape of Prognostic Factors and Clinical Outcomes for Cancer Control" Current Oncology 28, no. 6: 5155-5166. https://doi.org/10.3390/curroncol28060432
APA StyleGiuliani, M. E., Giannopoulos, E., Gospodarowicz, M. K., Broadhurst, M., O’Sullivan, B., Tittenbrun, Z., Johnson, S., & Brierley, J. (2021). Examining the Landscape of Prognostic Factors and Clinical Outcomes for Cancer Control. Current Oncology, 28(6), 5155-5166. https://doi.org/10.3390/curroncol28060432




