The Usefulness of Spectral Mammography in Surgical Planning of Breast Cancer Treatment—Analysis of 999 Patients with Primary Operable Breast Cancer
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients and Procedures
2.2. Imaging Modalities
2.3. Histopathological Examination
2.4. Data Analysis and Statistical Method
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424, Erratum in 2020, 70, 313. [Google Scholar] [CrossRef] [PubMed]
- Wojciechowska, U.J. Cancer Incidence and Mortality in Poland. Polish National Cancer Registry, Oncology Center-Maria Skłodowska-Curie Institute. Available online: http://onkologia.org.pl (accessed on 12 December 2020).
- Coates, A.S.; Winer, E.P.; Goldhirsch, A.; Gelber, R.D.; Gnant, M.; Piccart-Gebhart, M.; Thürlimann, B.; Senn, H.J.; Panel Members. Tailoring therapies-improving the management of early breast cancer: St Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer 2015. Ann. Oncol. 2015, 26, 1533–1546. [Google Scholar] [CrossRef] [PubMed]
- Burstein, H.J.; Curigliano, G.; Loibl, S.; Dubsky, P.; Gnant, M.; Poortmans, P.; Colleoni, M.; Denkert, C.; Piccart-Gebhart, M.; Regan, M.; et al. Estimating the benefits of therapy for early-stage breast cancer: The St. Gallen International Consensus Guidelines for the primary therapy of early breast cancer 2019. Ann. Oncol. 2019, 30, 1541–1557. [Google Scholar] [CrossRef] [PubMed]
- Kunkler, I.H.; Williams, L.J.; Jack, W.J.; Cameron, D.A.; Dixon, J.M.; PRIME II Investigators. Breast-conserving surgery with or without irradiation in women aged 65 years or older with early breast cancer (PRIME II): A randomised controlled trial. Lancet Oncol. 2015, 16, 266–273. [Google Scholar] [CrossRef]
- Al-Gaithy, Z.K.; Yaghmoor, B.E.; Koumu, M.I.; Alshehri, K.A.; Saqah, A.A.; Alshehri, H.Z. Trends of mastectomy and breast-conserving surgery and related factors in female breast cancer patients treated at King Abdulaziz University Hospital, Jeddah, Saudi Arabia, 2009–2017: A retrospective cohort study. Ann. Med. Surg. 2019, 41, 47–52. [Google Scholar] [CrossRef] [PubMed]
- Milulescu, A.; Di Marino, L.; Peradze, N.; Toesca, A. Management of Multifocal-Multicentric Breast Cancer: Current Perspective. Chirurgia 2017, 112, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Rauch, G.M.; Hobbs, B.P.; Kuerer, H.M.; Scoggins, M.E.; Benveniste, A.P.; Park, Y.M.; Caudle, A.S.; Fox, P.S.; Smith, B.D.; Adrada, B.E.; et al. Microcalcifications in 1657 Patients with Pure Ductal Carcinoma in Situ of the Breast: Correlation with Clinical, Histopathologic, Biologic Features, and Local Recurrence. Ann. Surg. Oncol. 2016, 23, 482–489. [Google Scholar] [CrossRef]
- Masannat, Y.A.; Agrawal, A.; Maraqa, L.; Fuller, M.; Down, S.K.; Tang, S.; Pang, D.; Kontos, M.; Romics, L.; Heys, S.D. Multifocal and multicentric breast cancer, is it time to think again? Ann. R. Coll. Surg. Engl. 2020, 102, 62–66. [Google Scholar] [CrossRef]
- Fiorica, J.V. Breast Cancer Screening, Mammography, and other Modalities. Clin. Obstet. Gynecol. 2016, 59, 688–709. [Google Scholar] [CrossRef]
- Jochelson, M. Advanced imaging techniques for the detection of breast cancer. Am. Soc. Clin. Oncol. Educ. Book 2012, 65–69. [Google Scholar] [CrossRef]
- Dodelzon, K.; Simon, K.; Dou, E.; Levy, A.D.; Michaels, A.Y.; Askin, G.; Katzen, J.T. Performance of 2D Synthetic Mammography Versus Digital Mammography in the Detection of Microcalcifications at Screening. AJR Am. J. Roentgenol. 2020, 214, 1436–1444. [Google Scholar] [CrossRef]
- Clauser, P.; Nagl, G.; Helbich, T.H.; Pinker-Domenig, K.; Weber, M.; Kapetas, P.; Bernathova, M.; Baltzer, P.A.T. Diagnostic performance of digital breast tomosynthesis with a wide scan angle compared to full-field digital mammography for the detection and characterization of microcalcifications. Eur. J. Radiol. 2016, 85, 2161–2168. [Google Scholar] [CrossRef]
- Hofvind, S.; Holen, Å.S.; Aase, H.S.; Houssami, N.; Sebuødegård, S.; Moger, T.A.; Haldorsen, I.S.; Akslen, L.A. Two-view digital breast tomosynthesis versus digital mammography in a population-based breast cancer screening programme (To-Be): A randomised, controlled trial. Lancet Oncol. 2019, 20, 795–805, Erratum in 2019, 20, e346. [Google Scholar] [CrossRef]
- Jochelson, M.S.; Lobbes, M.B.I. Contrast-enhanced Mammography: State of the Art. Radiology 2021, 299, 36–48. [Google Scholar] [CrossRef] [PubMed]
- Steinhof-Radwańska, K.; Grażyńska, A.; Barczyk-Gutkowska, A.; Kajor, M.; Powązka, P.; Lorek, A.; Szlachta-Świątkowska, E.; Morawska, I.; Okas, K.; Lelek, Z.; et al. The new method, the old problem-role of contrast-enhanced spectral mammography in the diagnosis of breast cancer among Polish women. Pol. J. Radiol. 2020, 85, e381–e386. [Google Scholar] [CrossRef] [PubMed]
- Lee-Felker, S.A.; Tekchandani, L.; Thomas, M.; Gupta, E.; Andrews-Tang, D.; Roth, A.; Sayre, J.; Rahbar, G. Newly Diagnosed Breast Cancer: Comparison of Contrast-enhanced Spectral Mammography and Breast MR Imaging in the Evaluation of Extent of Disease. Radiology 2017, 285, 389–400. [Google Scholar] [CrossRef] [PubMed]
- Lewin, J. Comparison of Contrast-Enhanced Mammography and Contrast-Enhanced Breast MR Imaging. Magn. Reson. Imaging Clin. N. Am. 2018, 26, 259–263. [Google Scholar] [CrossRef]
- Covington, M.F. Contrast-Enhanced Mammography Implementation, Performance, and Use for Supplemental Breast Cancer Screening. Radiol. Clin. N. Am. 2021, 59, 113–128. [Google Scholar] [CrossRef]
- Blum, K.S.; Rubbert, C.; Mathys, B.; Antoch, G.; Mohrmann, S.; Obenauer, S. Use of contrast-enhanced spectral mammography for intramammary cancer staging: Preliminary results. Acad. Radiol. 2014, 21, 1363–1369. [Google Scholar] [CrossRef]
- Patel, B.K.; Lobbes, M.B.I.; Lewin, J. Contrast Enhanced Spectral Mammography: A Review. Semin. Ultrasound CT MRI 2018, 39, 70–79. [Google Scholar] [CrossRef]
- Zhou, M.R.; Tang, Z.H.; Li, J.; Fan, J.H.; Pang, Y.; Yang, H.J.; Zheng, S.; Bai, J.Q.; Lv, N.; Qiao, Y.L.; et al. Clinical and pathologic features of multifocal and multicentric breast cancer in chinese women: A retrospective cohort study. J. Breast Cancer 2013, 16, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Bozzini, A.; Renne, G.; Meneghetti, L.; Bandi, G.; Santos, G.; Vento, A.R.; Menna, S.; Andrighetto, S.; Viale, G.; Cassano, E.; et al. Sensitivity of imaging for multifocal-multicentric breast carcinoma. BMC Cancer 2008, 8, 275. [Google Scholar] [CrossRef]
- Lang, Z.; Wu, Y.; Li, C.; Li, X.; Wang, X.; Qu, G. Multifocal and Multicentric Breast Carcinoma: A Significantly More Aggressive Tumor than Unifocal Breast Cancer. Anticancer Res. 2017, 37, 4593–4598. [Google Scholar] [CrossRef] [PubMed]
- Rezo, A.; Dahlstrom, J.; Shadbolt, B.; Rodins, K.; Zhang, Y.; Davis, A.J.; ACT & SENSW BCTG. Tumor size and survival in multicentric and multifocal breast cancer. Breast 2011, 20, 259–263. [Google Scholar] [CrossRef] [PubMed]
- Djordjevic-Jovanovic, L.; Karanikolic, A.; Bojic, T.; Pesic, I.; Djordjevic, M.; Marinkovic, M. Characteristics and outcomes of patients with multifocal/multicentric and unifocal breast cancer. J. BUON 2017, 22, 652–657. [Google Scholar] [PubMed]
- Alexander, M.; Acosta Gonzalez, G.; Malerba, S.; Hochman, T.; Goldberg, J.D.; Darvishian, F. Multifocal Invasive Ductal Cancer: Distinguishing Independent Tumor Foci from Multiple Satellites. Int. J. Surg. Pathol. 2017, 25, 298–303. [Google Scholar] [CrossRef] [PubMed]
- Neri, A.; Marrelli, D.; Megha, T.; Bettarini, F.; Tacchini, D.; De Franco, L.; Roviello, F. Clinical significance of multifocal and multicentric breast cancers and choice of surgical treatment: A retrospective study on a series of 1158 cases. BMC Surg. 2015, 15, 1. [Google Scholar] [CrossRef]
- Sardanelli, F.; Giuseppetti, G.M.; Panizza, P.; Bazzocchi, M.; Fausto, A.; Simonetti, G.; Lattanzio, V.; Del Maschio, A.; Italian Trial for Breast MR in Multifocal/Multicentric Cancer. Sensitivity of MRI versus mammography for detecting foci of multifocal, multicentric breast cancer in Fatty and dense breasts using the whole-breast pathologic examination as a gold standard. AJR Am. J. Roentgenol. 2004, 183, 1149–1157. [Google Scholar] [CrossRef]
- Losurdo, L.; Fanizzi, A.; Basile, T.M.A.; Bellotti, R.; Bottigli, U.; Dentamaro, R.; Didonna, V.; Lorusso, V.; Massafra, R.; Tamborra, P.; et al. Radiomics Analysis on Contrast-Enhanced Spectral Mammography Images for Breast Cancer Diagnosis: A Pilot Study. Entropy 2019, 21, 1110. [Google Scholar] [CrossRef]
- Mori, M.; Akashi-Tanaka, S.; Suzuki, S.; Daniels, M.I.; Watanabe, C.; Hirose, M.; Nakamura, S. Diagnostic accuracy of contrast-enhanced spectral mammography in comparison to conventional full-field digital mammography in a population of women with dense breasts. Breast Cancer 2017, 24, 104–110. [Google Scholar] [CrossRef]
- Tennant, S.L.; James, J.J.; Cornford, E.J.; Chen, Y.; Burrell, H.C.; Hamilton, L.J.; Girio-Fragkoulakis, C. Contrast-enhanced spectral mammography improves diagnostic accuracy in the symptomatic setting. Clin. Radiol. 2016, 71, 1148–1155. [Google Scholar] [CrossRef]
- Łuczyńska, E.; Niemiec, J.; Hendrick, E.; Heinze, S.; Jaszczyński, J.; Jakubowicz, J.; Sas-Korczyńska, B.; Rys, J. Degree of Enhancement on Contrast Enhanced Spectral Mammography (CESM) and Lesion Type on Mammography (MG): Comparison Based on Histological Results. Med. Sci. Monit. 2016, 22, 3886–3893. [Google Scholar] [CrossRef]
- Lobbes, M.B.; Lalji, U.; Houwers, J.; Nijssen, E.C.; Nelemans, P.J.; van Roozendaal, L.; Smidt, M.L.; Heuts, E.; Wildberger, J.E. Contrast-enhanced spectral mammography in patients referred from the breast cancer screening programme. Eur. Radiol. 2014, 24, 1668–1676. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.; Huang, J.M.; Zhang, K.; Xia, L.J.; Feng, L.; Yang, P.; Zhang, M.Y.; Xiao, W.; Lin, H.X.; Yu, Y.H. Diagnostic Value of Contrast-Enhanced Spectral Mammography for Screening Breast Cancer: Systematic Review and Meta-analysis. Clin. Breast Cancer 2018, 18, e985–e995. [Google Scholar] [CrossRef] [PubMed]
- Sorin, V.; Faermann, R.; Yagil, Y.; Shalmon, A.; Gotlieb, M.; Halshtok-Neiman, O.; Ben-David, M.A.; Sklair-Levy, M. Contrast-enhanced spectral mammography (CESM) in women presenting with palpable breast findings. Clin. Imaging 2020, 61, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Jochelson, M.S.; Dershaw, D.D.; Sung, J.S.; Heerdt, A.S.; Thornton, C.; Moskowitz, C.S.; Ferrara, J.; Morris, E.A. Bilateral contrast-enhanced dual-energy digital mammography: Feasibility and comparison with conventional digital mammography and MR imaging in women with known breast carcinoma. Radiology 2013, 266, 743–751. [Google Scholar] [CrossRef] [PubMed]
- Tang, S.; Xiang, C.; Yang, Q. The diagnostic performance of CESM and CE-MRI in evaluating the pathological response to neoadjuvant therapy in breast cancer: A systematic review and meta-analysis. Br. J. Radiol. 2020, 93, 20200301. [Google Scholar] [CrossRef]
- Raikhlin, A.; Curpen, B.; Warner, E.; Betel, C.; Wright, B.; Jong, R. Breast MRI as an adjunct to mammography for breast cancer screening in high-risk patients: Retrospective review. AJR Am. J. Roentgenol. 2015, 204, 889–897, Erratum in AJR Am. J. Roentgenol. 2015, 204, 1137. [Google Scholar] [CrossRef]
- Iacconi, C.; Galman, L.; Zheng, J.; Sacchini, V.; Sutton, E.J.; Dershaw, D.; Morris, E.A. Multicentric Cancer Detected at Breast MR Imaging and Not at Mammography: Important or Not? Radiology 2016, 279, 378–384. [Google Scholar] [CrossRef]
- Obdeijn, I.M.; Mann, R.M.; Loo, C.C.E.; Lobbes, M.; Voormolen, E.M.C.; van Deurzen, C.H.M.; de Bock, G.; Hereditary Breast Ovarian Cancer Research Group Netherlands (HEBON) ; Hooning, M.J. The supplemental value of mammographic screening over breast MRI alone in BRCA2 mutation carriers. Breast Cancer Res. Treat. 2020, 181, 581–588. [Google Scholar] [CrossRef]
- Perono Biacchiardi, C.; Brizzi, D.; Genta, F.; Zanon, E.; Camanni, M.; Deltetto, F. Breast cancer preoperative staging: Does contrast-enhanced magnetic resonance mammography modify surgery? Int. J. Breast Cancer 2011, 2011, 757234. [Google Scholar] [CrossRef][Green Version]
- Tsina, G.; Simon, P. Breast magnetic resonance imaging and its impact on the surgical treatment of breast cancer. Obstet. Gynecol. Int. 2014, 2014, 632074. [Google Scholar] [CrossRef] [PubMed]
- Turnbull, L.; Brown, S.; Harvey, I.; Olivier, C.; Drew, P.; Napp, V.; Hanby, A.; Brown, J. Comparative effectiveness of MRI in breast cancer (COMICE) trial: A randomised controlled trial. Lancet 2010, 375, 563–571. [Google Scholar] [CrossRef]
- Houben, I.P.; Vanwetswinkel, S.; Kalia, V.; Thywissen, T.; Nelemans, P.J.; Heuts, E.M.; Smidt, M.L.; Meyer-Baese, A.; Wildberger, J.E.; Lobbes, M. Contrast-enhanced spectral mammography in the evaluation of breast suspicious calcifications: Diagnostic accuracy and impact on surgical management. Acta Radiol. 2019, 60, 1110–1117. [Google Scholar] [CrossRef]
- Biganzoli, L.; Battisti, N.M.L.; Wildiers, H.; McCartney, A.; Colloca, G.; Kunkler, I.H.; Cardoso, M.J.; Cheung, K.L.; de Glas, N.A.; Trimboli, R.M.; et al. Updated recommendations regarding the management of older patients with breast cancer: A joint paper from the European Society of Breast Cancer Specialists (EUSOMA) and the International Society of Geriatric Oncology (SIOG). Lancet Oncol. 2021. [Google Scholar] [CrossRef]
- Cardoso, F.; Loibl, S.; Pagani, O.; Graziottin, A.; Panizza, P.; Martincich, L.; Gentilini, O.; Peccatori, F.; Fourquet, A.; Delaloge, S.; et al. The European Society of Breast Cancer Specialists recommendations for the management of young women with breast cancer. Eur. J. Cancer 2012, 48, 3355–3377. [Google Scholar] [CrossRef]
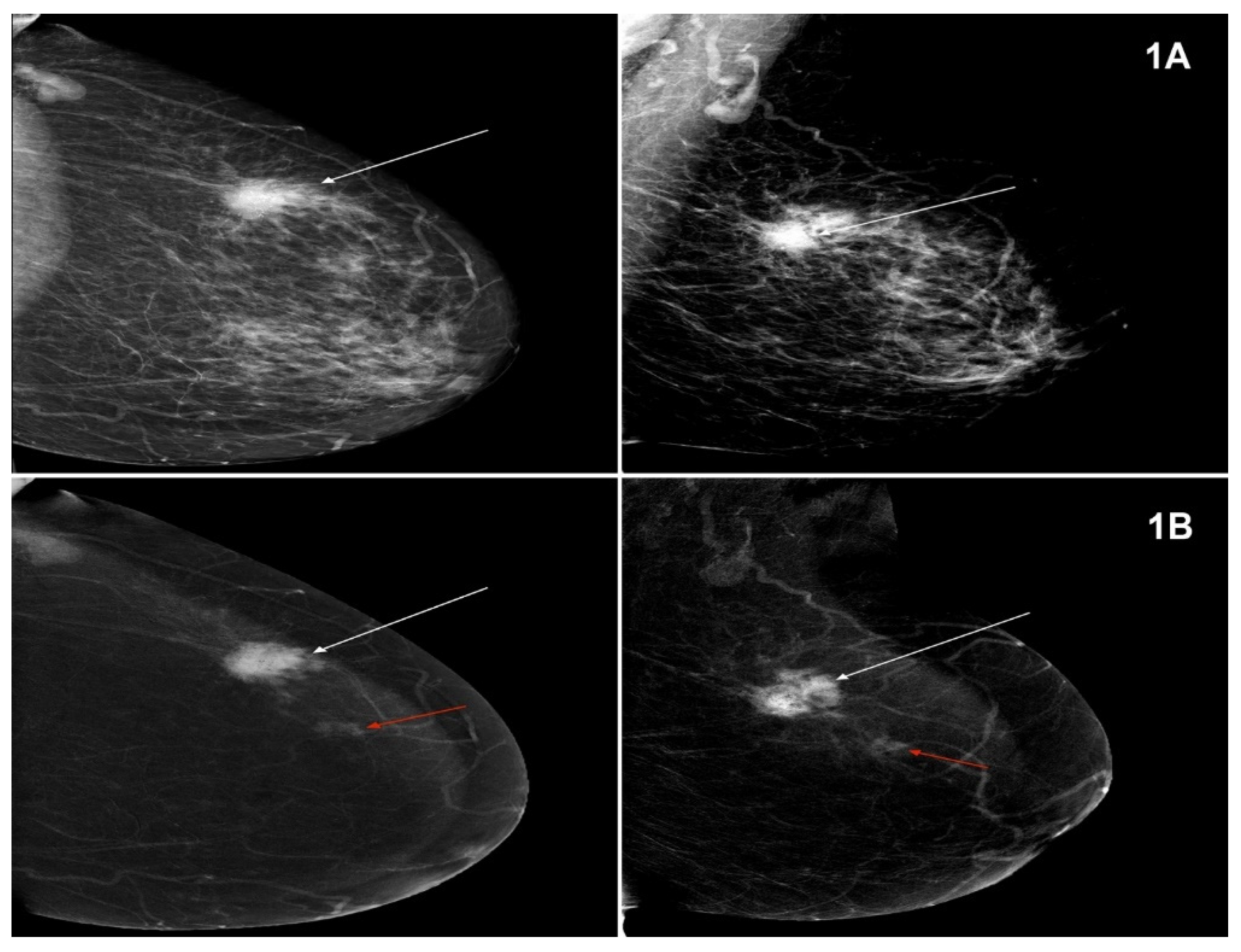
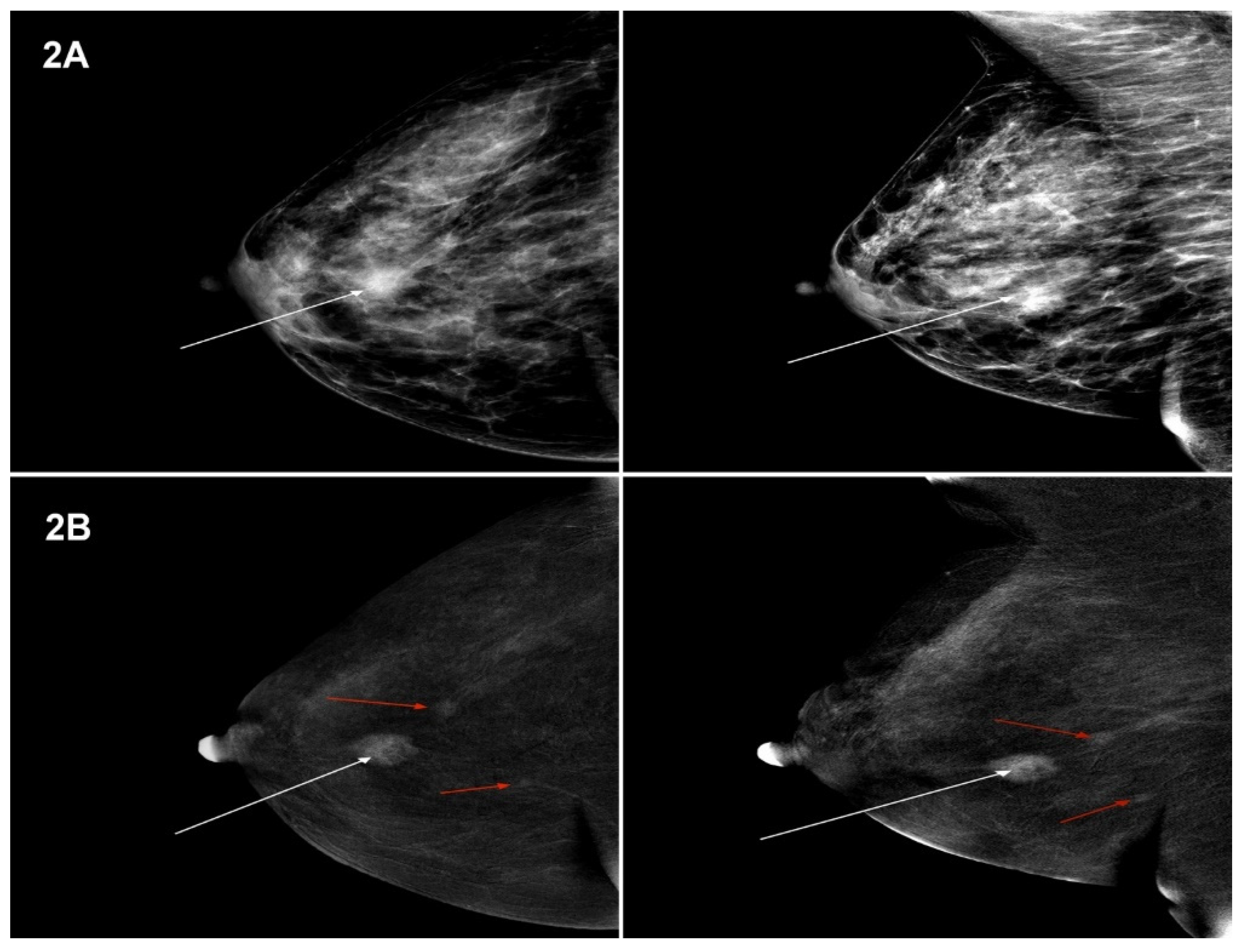
| MG | CESM | Row in Total n | |
|---|---|---|---|
| Unifocal n | MFMCC n | ||
| Unifocal | 779 | 164 | 943 |
| MFMCC | 9 | 47 | 56 |
| Total | 788 | 211 | 999 |
| Postoperative HP | MG | CESM | Method in Total n | ||
|---|---|---|---|---|---|
| Unifocal n | MFMCC n | Unifocal n | MFMCC n | ||
| Unifocal | 797 | 8 | 764 | 41 | 805 |
| MFMCC | 146 | 48 | 24 | 170 | 194 |
| Total | 943 | 56 | 788 | 211 | 999 |
| Surgical Procedure | n | % |
|---|---|---|
| Madden type radical mastectomy | 310 | 31.03 |
| Wide local excision (WLE) with sentinel lymph node biopsy (SLNB) | 333 | 33.33 |
| Wide local excision (WLE) with axillary lymph node dissection (ALND) | 79 | 7.91 |
| Total (simple) mastectomy | 31 | 3.10 |
| Total (simple) mastectomy with SLNB | 185 | 18.52 |
| Subcutaneous mastectomy with reconstruction with SLNB | 6 | 0.60 |
| Subcutaneous mastectomy with reconstruction with ALND | 2 | 0.20 |
| WLE | 53 | 5.31 |
| HP | All Occurrences n | MG-MFMCC n (%) | CESM-MFMCC n (%) |
|---|---|---|---|
| NST (carcinoma of no special type) | 631 | 37 (5.86) | 134 (21.24) |
| Infiltrating lobular cancer | 144 | 11 (7.64) | 40 (27.78) |
| Special subtypes | 75 | 4 (5.33) | 16 (21.33) |
| DCIS HG | 70 | 0 (0.00) | 9 (12.86) |
| DCIS LG | 29 | 1 (3.45) | 2 (6.90) |
| LCIS (pleomorphic subtype) | 4 | 0 (0.00) | 0 (0.00) |
| Infiltrating ductolobular cancer | 46 | 3 (6.52) | 10 (21.74) |
| In total | 999 | 56 (5.61) | 211 (21.12) |
| Types of Conserving Procedures | Surgeries Planned on the Basis of MG n | Surgeries Performed upon Visualisation of MFMCC in CESM n | Number of Changes in the Scope of Procedure into Difference Kinds of Mastectomy n (%) | Local Radicalisation in the Group of Patients on Conserving Treatment with MFMCC n |
|---|---|---|---|---|
| WLE + ALND | 124 | 79 | 45 (7.7) | 2 |
| WLE | 57 | 53 | 4 (0.68) | 1 |
| WLE + SLNB | 401 | 333 | 68 (11.6) | 6 |
| In total | 582 | 465 | 116 (19.9) | 9 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lorek, A.; Steinhof-Radwańska, K.; Barczyk-Gutkowska, A.; Zarębski, W.; Paleń, P.; Szyluk, K.; Lorek, J.; Grażyńska, A.; Niemiec, P.; Gisterek, I. The Usefulness of Spectral Mammography in Surgical Planning of Breast Cancer Treatment—Analysis of 999 Patients with Primary Operable Breast Cancer. Curr. Oncol. 2021, 28, 2548-2559. https://doi.org/10.3390/curroncol28040232
Lorek A, Steinhof-Radwańska K, Barczyk-Gutkowska A, Zarębski W, Paleń P, Szyluk K, Lorek J, Grażyńska A, Niemiec P, Gisterek I. The Usefulness of Spectral Mammography in Surgical Planning of Breast Cancer Treatment—Analysis of 999 Patients with Primary Operable Breast Cancer. Current Oncology. 2021; 28(4):2548-2559. https://doi.org/10.3390/curroncol28040232
Chicago/Turabian StyleLorek, Andrzej, Katarzyna Steinhof-Radwańska, Anna Barczyk-Gutkowska, Wojciech Zarębski, Piotr Paleń, Karol Szyluk, Joanna Lorek, Anna Grażyńska, Paweł Niemiec, and Iwona Gisterek. 2021. "The Usefulness of Spectral Mammography in Surgical Planning of Breast Cancer Treatment—Analysis of 999 Patients with Primary Operable Breast Cancer" Current Oncology 28, no. 4: 2548-2559. https://doi.org/10.3390/curroncol28040232
APA StyleLorek, A., Steinhof-Radwańska, K., Barczyk-Gutkowska, A., Zarębski, W., Paleń, P., Szyluk, K., Lorek, J., Grażyńska, A., Niemiec, P., & Gisterek, I. (2021). The Usefulness of Spectral Mammography in Surgical Planning of Breast Cancer Treatment—Analysis of 999 Patients with Primary Operable Breast Cancer. Current Oncology, 28(4), 2548-2559. https://doi.org/10.3390/curroncol28040232






