Effects of Health Anxiety, Social Support, and Coping on Dissociation with Mediating Role of Perceived Stress during the COVID-19 Pandemic
Abstract
1. Introduction
1.1. Perceived Stress
1.2. Social Support
1.3. Health Anxiety
1.4. Coping
1.5. Gender
1.6. Lockdown
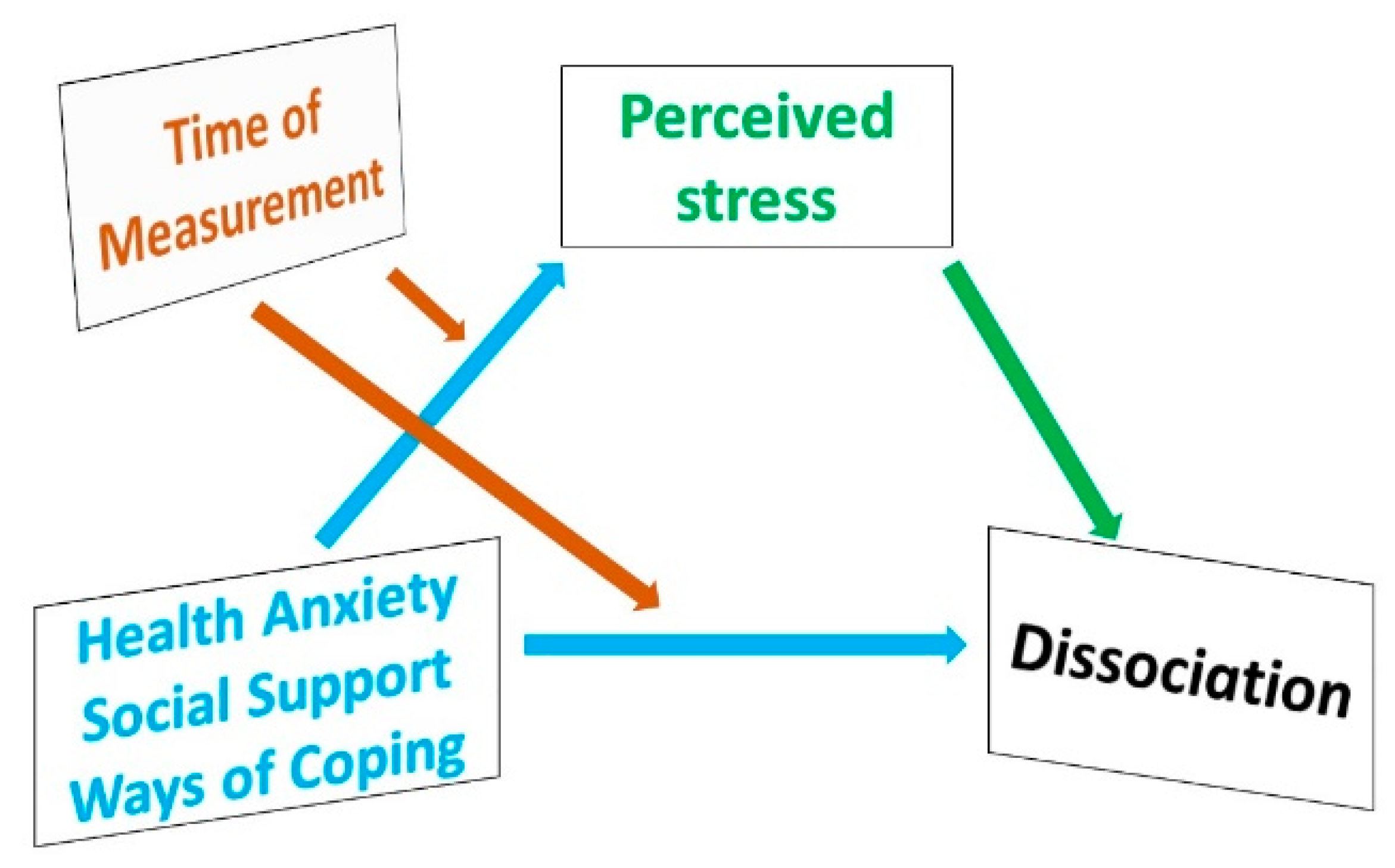
1.7. Aims of the Study
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Participants and Sampling
2.3. Survey Instruments
2.3.1. The Perceived Stress Scale (PSS)
2.3.2. Multidimensional Scale of Perceived Social Support (MSPSS)
2.3.3. Short Health Anxiety Inventory (SHAI)
2.3.4. Ways of Coping Questionnaire (WCQ)
2.3.5. The Dissociative Experiences Scale (DES)
2.3.6. Data Analysis
3. Results
3.1. Descriptive and Correlational Analysis
3.2. Moderated Mediation Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. Coronavirus Disease (COVID-19) Outbreak Situation. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 15 December 2022).
- About Hungary. Hungary—COVID-19. Available online: http://abouthungary.hu/coronavirus/ (accessed on 15 December 2022).
- Xiong, J.; Lipsitz, O.; Nasri, F.; Lui, L.M.W.; Gill, H.; Phan, L.; Chen-Li, D.; Iacobucci, M.; Ho, R.; Majeed, A.; et al. Impact of COVID-19 pandemic on mental health in the general population: A systematic review. J. Affect. Disord. 2020, 277, 55–64. [Google Scholar] [CrossRef] [PubMed]
- Rajkumar, R.P. COVID-19 and mental health: A review of the existing literature. Asian J. Psychiatry 2020, 52, 102066. [Google Scholar] [CrossRef] [PubMed]
- Vindegaard, N.; Benros, M.E. COVID-19 pandemic and mental health consequences: Systematic review of the current evidence. Brain Behav. Immun. 2020, 89, 531–542. [Google Scholar] [CrossRef] [PubMed]
- Aknin, L.B.; De Neve, J.E.; Dunn, E.W.; Fancourt, D.E.; Goldberg, E.; Helliwell, J.F.; Jones, S.P.; Karam, E.; Layard, R.; Lyubomirsky, S.; et al. Mental Health During the First Year of the COVID-19 Pandemic: A Review and Recommendations for Moving Forward. Perspect. Psychol. Sci. 2022, 17, 915–936. [Google Scholar] [CrossRef]
- Leigh-Hunt, N.; Bagguley, D.; Bash, K.; Turner, V.; Turnbull, S.; Valtorta, N.; Caan, W. An overview of systematic reviews on the public health consequences of social isolation and loneliness. Public Health 2017, 152, 157–171. [Google Scholar] [CrossRef]
- Onyeaka, H.; Anumudu, C.K.; Al-Sharify, Z.T.; Egele-Godswill, E.; Mbaegbu, P. COVID-19 pandemic: A review of the global lockdown and its far-reaching effects. Sci. Prog. 2021, 104, 368504211019854. [Google Scholar] [CrossRef]
- Prati, G.; Mancini, A.D. The psychological impact of COVID-19 pandemic lockdowns: A review and meta-analysis of longitudinal studies and natural experiments. Psychol. Med. 2021, 51, 201–211. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Birmes, P.; Brunet, A.; Benoit, M.; Defer, S.; Hatton, L.; Sztulman, H.; Schmitt, L. Validation of the Peritraumatic Dissociative Experiences Questionnaire self-report version in two samples of French-speaking individuals exposed to trauma. Eur. Psychiatry 2005, 20, 145–151. [Google Scholar] [CrossRef]
- Daglis, T. The Increase in Addiction during COVID-19. Encyclopedia 2021, 1, 1257–1266. [Google Scholar] [CrossRef]
- Černis, E.; Evans, R.; Ehlers, A.; Freeman, D. Dissociation in relation to other mental health conditions: An exploration using network analysis. J. Psychiatr Res. 2021, 136, 460–467. [Google Scholar] [CrossRef]
- Manchia, M.; Gathier, A.W.; Yapici-Eser, H.; Schmidt, M.V.; de Quervain, D.; van Amelsvoort, T.; Bisson, J.I.; Cryan, J.F.; Howes, O.D.; Pinto, L.; et al. The impact of the prolonged COVID-19 pandemic on stress resilience and mental health: A critical review across waves. Eur. Neuropsychopharmacol. 2022, 55, 22–83. [Google Scholar] [CrossRef] [PubMed]
- Dubey, S.; Biswas, P.; Ghosh, R.; Chatterjee, S.; Dubey, M.J.; Chatterjee, S.; Lahiri, D.; Lavie, C.J. Psychosocial impact of COVID-19. Diabetes Metab. Syndr. 2020, 14, 779–788. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Wen, W.; Zhang, H.; Ni, J.; Jiang, J.; Cheng, Y.; Zhou, M.; Ye, L.; Feng, Z.; Ge, Z.; et al. Anxiety, depression, and stress prevalence among college students during the COVID-19 pandemic: A systematic review and meta-analysis. J. Am. Coll. Health 2021, 1, 1–8. [Google Scholar] [CrossRef]
- Elharake, J.A.; Akbar, F.; Malik, A.A.; Gilliam, W.; Omer, S.B. Mental Health Impact of COVID-19 among Children and College Students: A Systematic Review. Child Psychiatry Hum. Dev. 2022, 11, 1–13. [Google Scholar] [CrossRef]
- Van der Kolk, B.A.; van der Hart, O. Pierre Janet and the breakdown of adaptation in psychological trauma. Am. J. Psychiatry 1989, 146, 1530–1540. [Google Scholar] [CrossRef]
- Bernstein, E.M.; Putnam, F.W. Development, reliability, and validity of a dissociation scale. J. Nerv. Ment. Dis. 1986, 174, 727–735. [Google Scholar] [CrossRef] [PubMed]
- Grabe, H.J.; Rainermann, S.; Spitzer, C.; Gänsicke, M.; Freyberger, H.J. The relationship between dimensions of alexithymia and dissociation. Psychother. Psychosom. 2000, 69, 128–131. [Google Scholar] [CrossRef]
- Waller, N.; Putnam, F.W.; Carlson, E.B. Types of dissociation and dissociative types: A taxometric analysis of dissociative experiences. Psychol. Methods 1996, 1, 300–321. [Google Scholar] [CrossRef]
- Spitzer, C.; Barnow, S.; Freyberger, H.J.; Grabe, H.J. Recent developments in the theory of dissociation. World Psychiatry 2006, 5, 82–86. [Google Scholar]
- Lynn, C.D. Adaptive and Maladaptive Dissociation: An Epidemiological and Anthropological Comparison and Proposition for an Expanded Dissociation Model. Anthropol. Conscious 2005, 16, 16–49. [Google Scholar] [CrossRef]
- Van der Kolk, B.A.; Fisler, R. Dissociation and the fragmentary nature of traumatic memories: Overview and exploratory study. J. Trauma. Stress 1995, 8, 505–525. [Google Scholar] [CrossRef] [PubMed]
- Schauer, M.; Elbert, T. Dissociation following traumatic stress: Etiology and treatment. J. Psychol. 2010, 218, 109–127. [Google Scholar] [CrossRef]
- La Rosa, V.L.; Gori, A.; Faraci, P.; Vicario, C.M.; Craparo, G. Traumatic Distress, Alexithymia, Dissociation, and Risk of Addiction During the First Wave of COVID-19 in Italy: Results from a Cross-sectional Online Survey on a Non-clinical Adult Sample. Int. J. Ment. Health Addict. 2022, 20, 3128–3144. [Google Scholar] [CrossRef]
- Chiara, C.; Giorgio, V.; Claudio, B.; Virginia, C.; Antonio, D.C.; Carlo, L. Escaping the Reality of the Pandemic: The Role of Hopelessness and Dissociation in COVID-19 Denialism. JPM 2022, 12, 1302. [Google Scholar] [CrossRef]
- Velotti, P.; Civilla, C.; Rogier, G.; Beomonte Zobel, S. A Fear of COVID-19 and PTSD Symptoms in Pathological Personality: The Mediating Effect of Dissociation and Emotion Dysregulation. Front. Psychiatry 2021, 23, 590021. [Google Scholar] [CrossRef]
- Azoulay, E.; Cariou, A.; Bruneel, F.; Demoule, A.; Kouatchet, A.; Reuter, D.; Souppart, V.; Combes, A.; Klouche, K.; Argaud, L.; et al. Symptoms of Anxiety, Depression, and Peritraumatic Dissociation in Critical Care Clinicians Managing Patients with COVID-19. A Cross-Sectional Study. Am. J. Respir. Crit. Care Med. 2020, 202, 1388–1398. [Google Scholar] [CrossRef] [PubMed]
- Savage, M.J.; James, R.; Magistro, D.; Donaldson, J.; Healy, L.C.; Nevill, M.; Hennis, P.J. Mental health and movement behaviour during the COVID-19 pandemic in UK university students: Prospective cohort study. MENPA 2020, 19, 100357. [Google Scholar]
- De Wachter, D.; Lange, A.; Vanderlinden, J.; Pouw, J.; Strubbe, E. The influence of current stress on dissociative experiences: An exploratory study in a non-clinical population. J. Trauma Dissociation 2006, 7, 87–96. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Syme, S.L. Social Support and Health, 1st ed.; Academic Press: San Fransisco, CA, USA, 1985; pp. 3–22. [Google Scholar]
- House, J.S.; Umberson, D.; Landis, K.R. Structures and processes of social support. Annu. Rev. Sociol. 1988, 14, 293–318. [Google Scholar] [CrossRef]
- Saltzman, L.Y.; Hansel, T.C.; Bordnick, P.S. Loneliness, isolation, and social support factors in post-COVID-19 mental health. Psychol. Trauma 2020, 12, S55–S57. [Google Scholar] [CrossRef] [PubMed]
- Szkody, E.; Stearns, M.; Stanhope, L.; McKinney, C. Stress-Buffering Role of Social Support during COVID-19. Fam. Process 2021, 60, 1002–1015. [Google Scholar] [CrossRef] [PubMed]
- Li, F.; Luo, S.; Mu, W.; Li, Y.; Ye, L.; Zheng, X.; Xu, B.; Ding, Y.; Ling, P.; Zhou, M.; et al. Effects of sources of social support and resilience on the mental health of different age groups during the COVID-19 pandemic. BMC Psychiatry 2021, 21, 16. [Google Scholar] [CrossRef] [PubMed]
- Grey, I.; Arora, T.; Thomas, J.; Saneh, A.; Tohme, P.; Abi-Habib, R. The role of perceived social support on depression and sleep during the COVID-19 pandemic. Psychiatry Res. 2020, 293, 113452. [Google Scholar] [CrossRef]
- Labrague, L.J.; De Los Santos, J.A.A.; Falguera, C.C. Social and emotional loneliness among college students during the COVID-19 pandemic: The predictive role of coping behaviors, social support, and personal resilience. Perspect. Psychiatr. Care 2021, 57, 1578–1584. [Google Scholar] [CrossRef]
- Baranyi, A.; Leithgöb, O.; Kreiner, B.; Tanzer, K.; Ehrlich, G.; Hofer, H.P.; Rothenhäusler, H.B. Relationship between posttraumatic stress disorder, quality of life, social support, and affective and dissociative status in severely injured accident victims 12 months after trauma. Psychosomatics 2010, 51, 237–247. [Google Scholar] [CrossRef] [PubMed]
- Coronas, R.; García-Parés, G.; Viladrich, C.; Santos, J.M.; Menchón, J.M. Clinical and sociodemographic variables associated with the onset of posttraumatic stress disorder in road traffic accidents. Depress. Anxiety 2008, 25, E16–E23. [Google Scholar] [CrossRef] [PubMed]
- Korol, S. Familial and social support as protective factors against the development of dissociative identity disorder. J. Trauma Dissociation 2008, 9, 249–267. [Google Scholar] [CrossRef]
- Abramowitz, J.S.; Braddock, A. Hypochondriasis and Health Anxiety, 1st ed.; Hogrefe Publishing: Cambridge, UK, 2011; pp. 1–9. [Google Scholar]
- Asmundson, G.J.G.; Taylor, S. How health anxiety influences responses to viral outbreaks like COVID-19: What all decision-makers, health authorities, and health care professionals need to know. J. Anxiety Disord. 2020, 71, 102211. [Google Scholar] [CrossRef] [PubMed]
- Robinson, E.; Sutin, A.R.; Daly, M.; Jones, A. A systematic review and meta-analysis of longitudinal cohort studies comparing mental health before versus during the COVID-19 pandemic in 2020. J. Affect. Disord. 2022, 296, 567–576. [Google Scholar] [CrossRef]
- Li, Y.; Wang, A.; Wu, Y.; Han, N.; Huang, H. Impact of the COVID-19 Pandemic on the Mental Health of College Students: A Systematic Review and Meta-Analysis. Front. Psychol. 2021, 12, 669119. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, R.; Folkman, S. Stress, Appraisal, and Coping, 1st ed.; Springer Publishing: New York, NY, USA, 1984; pp. 1–60. [Google Scholar]
- Erick, T.B. Knowledge, Attitudes, Anxiety, and Coping Strategies of Students during COVID-19 Pandemic. J. Loss Trauma 2020, 25, 635–642. [Google Scholar] [CrossRef]
- Budimir, S.; Probst, T.; Pieh, C. Coping strategies and mental health during COVID-19 lockdown. J. Ment. Health 2021, 30, 156–163. [Google Scholar] [CrossRef]
- Li, S.; Liu, H.; Bai, X.W. The “psychological eye of typhoon” effect in wenchuan “5.12” earthquake. Sci. Technol. Rev. 2009, 27, 87–89. [Google Scholar]
- Huang, L.; Lei, W.; Xu, F.; Liu, H.; Yu, L. Emotional responses and coping strategies in nurses and nursing students during Covid-19 outbreak: A comparative study. PLoS ONE 2020, 15, e0237303. [Google Scholar] [CrossRef]
- Lazarus, R.S.; Folkman, S. Transactional theory and research on emotions and coping. EJP 1987, 1, 141–169. [Google Scholar] [CrossRef]
- Kar, N.; Kar, B.; Kar, S. Stress and coping during COVID-19 pandemic: Result of an online survey. Psychiatry Res. 2021, 295, 113598. [Google Scholar] [CrossRef]
- Pashazadeh Kan, F.; Raoofi, S.; Rafiei, S.; Khani, S.; Hosseinifard, H.; Tajik, F.; Raoofi, N.; Ahmadi, S.; Aghalou, S.; Torabi, F.; et al. A systematic review of the prevalence of anxiety among the general population during the COVID-19 pandemic. J. Affect. Disord. 2021, 293, 391–398. [Google Scholar] [CrossRef]
- Thibaut, F.; van Wijngaarden-Cremers, P.J.M. Women’s Mental Health in the Time of COVID-19 Pandemic. Front. Glob. Womens Health 2020, 1, 588372. [Google Scholar] [CrossRef]
- Sundarasen, S.; Chinna, K.; Kamaludin, K.; Nurunnabi, M.; Baloch, G.M.; Khoshaim, H.B.; Hossain, S.F.A.; Sukayt, A. Psychological Impact of COVID-19 and Lockdown among University Students in Malaysia: Implications and Policy Recommendations. Int. J. Environ. Res. Public Health 2020, 17, 6206. [Google Scholar] [CrossRef] [PubMed]
- Commodari, E.; La Rosa, V.L.; Carnemolla, G.; Parisi, J. The psychological impact of the lockdown on Italian university students during the first wave of COVID-19 pandemic: Psychological experiences, health risk perceptions, distance learning, and future perspectives. MJCP 2021, 9, 1–19. [Google Scholar]
- Almeida, M.; Shrestha, A.D.; Stojanac, D.; Miller, L.J. The impact of the COVID-19 pandemic on women’s mental health. Arch. Womens Ment. Health 2020, 23, 741–748. [Google Scholar] [CrossRef] [PubMed]
- Sahu, P. Closure of Universities Due to Coronavirus Disease 2019 (COVID-19): Impact on Education and Mental Health of Students and Academic Staff. Cureus 2020, 12, e7541. [Google Scholar] [CrossRef] [PubMed]
- Chaturvedi, K.; Vishwakarma, D.K.; Singh, N. COVID-19 and its impact on education, social life and mental health of students: A survey. Child. Youth Serv. Rev. 2021, 121, 105866. [Google Scholar] [CrossRef] [PubMed]
- Kaparounaki, C.K.; Patsali, M.E.; Mousa, D.V.; Papadopoulou, E.V.K.; Papadopoulou, K.K.K.; Fountoulakis, K.N. University students’ mental health amidst the COVID-19 quarantine in Greece. Psychiatry Res. 2020, 290, 113111. [Google Scholar] [CrossRef]
- Eysenbach, G. Improving the quality of Web surveys: The Checklist for Reporting Results of Internet E-Surveys (CHERRIES). J. Med. Internet Res. 2004, 6, e34. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Spacapan, S.; Oskamp, S. The Social Psychology of Health, 1st ed.; SAGE Publications: Thousand Oaks, CA, USA, 1988; pp. 31–67. [Google Scholar]
- Stauder, A.; Thege, B.K. Az Észlelt Stressz Kérdőív (PSS) Magyar Verziójának Jellemzői. Mentálhig Pszichoszomatika 2006, 7, 203–216. [Google Scholar] [CrossRef]
- Zimet, G.D.; Dahlem, N.W.; Zimet, S.G.; Farley, G.K. The Multidimensional Scale of Perceived Social Support. J. Pers. Assess. 1988, 52, 30–41. [Google Scholar] [CrossRef]
- Papp-Zipernovszky, O.; Kékesi, M.Z.; Jámbori, S. A Multidimenzionális Észlelt Társas Támogatás Kérdőív magyar nyelvű validálása. Mentálhig Pszichoszomatika 2017, 18, 230–262. [Google Scholar] [CrossRef]
- Salkovskis, P.M.; Rimes, K.A.; Warwick, H.M.C. The Health Anxiety Inventory: Development and validation of scales for the measurement of health anxiety and hypochondriasis. Psychol. Med. 2002, 32, 843. [Google Scholar] [CrossRef] [PubMed]
- Köteles, F.; Simor, P.; Bárdos, G. Validation and psychometric evaluation of the Hungarian version of the Short Health Anxiety Inventory (SHAI). Mentálhigiéné Pszichoszomatika 2011, 12, 191–213. [Google Scholar] [CrossRef]
- Folkman, S.; Lazarus, R.S. If it changes it must be a process: Study of emotion and coping during three stages of a college examination. J. Pers. Soc. Psychol. 1985, 48, 150–170. [Google Scholar] [CrossRef] [PubMed]
- Sørlie, T.; Sexton, H.C. The factor structure of “The Ways of Coping Questionnaire” and the process of coping in surgical patients. Pers. Individ. Differ. 2001, 30, 961–975. [Google Scholar] [CrossRef]
- Rózsa, S.; Purebl, G.; Susánszky, É.; Kő, N.; Szádóczky, E.; Réthelyi, J.; Danis, I.; Skrabski, Á.; Kopp, M. Dimensions of coping: Hungarian adaptation of the Ways of Coping Questionnaire. Mentálhigiéné Pszichoszomatika 2008, 9, 217–241. [Google Scholar] [CrossRef]
- Carlson, E.B.; Putnam, F.W. Dissociation: An update on the Dissociative Experience Scale. Univ. Oregon. Sch. Bank 1993, 6, 16–27. [Google Scholar]
- Perczel-Forintos, D.; Ajtay, G.; Barna, C.; Kiss, Z.; Komlósi, S. Kérdőívek, Becslőskálák a Klinikai Pszichológiában, 3rd ed.; Semmelweis Kiadó: Budapest, Hungary, 2018; p. 230. [Google Scholar]
- Alberts, N.M.; Hadjistavropoulos, H.D.; Jones, S.L.; Sharpe, D. The Short Health Anxiety Inventory: A systematic review and meta-analysis. J. Anxiety Disord. 2013, 27, 68–78. [Google Scholar] [CrossRef] [PubMed]
- Vanderlinden, J.; Van Dyck, R.; Vandereycken, W.; Vertommen, H. The Dissociation Questionnaire (Dis-G): Development, reliability and validity of a new self-reporting Dissociation Questionnaire. Acta Psychiatr. Belg. 1994, 94, 53–54. [Google Scholar]
- Chu, J.A. Rebuilding Shattered Lives: Treating Complex PTSD and Dissociative Disorders, 2nd ed.; John Wiley & Sons Inc.: Hoboken, NJ, USA, 2011. [Google Scholar]
- Andrew, F.H. Introduction to Mediation, Moderation, and Conditional Process Analysis, 2nd ed.; The Guilford Press: New York, NY, USA, 2018; p. 588. [Google Scholar]
- Paul, F.D.; John, A.O. Dissociation and the Dissociative Disorders: DSM-V and Beyond, 1st ed.; Routledge: Oxfordshire, UK, 2009; pp. 145–154. [Google Scholar]
- Asmundson, G.J.; Abramowitz, J.S.; Richter, A.A.; Whedon, M. Health anxiety: Current perspectives and future directions. Curr. Psychiatry Rep. 2010, 12, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Ray, S.; Ray, R.; Singh, N.; Paul, I. Dissociative experiences and health anxiety in panic disorder. Indian J. Psychiatry 2021, 63, 70–73. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.; Zheng, Y.; Xiong, S.; Zhang, W.; Guo, S. The Effect of Perceived Threat Avoidability of COVID-19 on Coping Strategies and Psychic Anxiety Among Chinese College Students in the Early Stage of COVID-19 Pandemic. Front. Psychiatry 2022, 3, 854698. [Google Scholar] [CrossRef]
- Rodriguez, L.M.; Litt, D.M.; Stewart, S.H. Drinking to cope with the pandemic: The unique associations of COVID-19-related perceived threat and psychological distress to drinking behaviors in American men and women. Addict. Behav. 2020, 110, 106532. [Google Scholar] [CrossRef] [PubMed]
- Biddle, N.; Sollis, K. Determinants of Participation in a Longitudinal Survey during the COVID-19 Pandemic: The Case of a Low-Infection Country; Bristol University Press: Bristol, UK, 2021. [Google Scholar]
| Factor | ||||
|---|---|---|---|---|
| 1 | 2 | 3 | 4 | |
| item4 | 0.772 | |||
| item3 | 0.635 | |||
| item5 | 0.499 | |||
| item1 | 0.414 | |||
| item15 | 0.31 | |||
| item9 | 0.565 | |||
| item8 | 0.551 | |||
| item16 | 0.425 | |||
| item10 | 0.399 | |||
| item14 | 0.304 | |||
| item7 | 0.231 | |||
| item2 | 0.984 | |||
| item11 | 0.68 | |||
| item6 | 0.50 | |||
| item13 | 0.383 | |||
| item12 | 0.335 | |||
| Minimum | Maximum | Mean1 (SD1); Mean2 (SD2) | α1, α2 | |
|---|---|---|---|---|
| DES | 0.00 | 100.00 | 19.193(18.052); 23.386(21.120) | 0.948; 0.961 |
| DES amnesia | 0.00 | 100.00 | 11.599(16.172);16.617(20.171) | 0.864; 0.909 |
| DES depersonalization | 0.00 | 100.00 | 13.746(19.880); 17.696(22.441) | 0.864; 0.883 |
| DES absorption | 0.00 | 100.00 | 32.233(24.127); 35.845(27.306) | 0.883; 0.919 |
| PSS | 0.00 | 4.00 | 2.328(.841); 2.179(.912) | 0.864; 0.869 |
| SHAI | 1.00 | 3.44 | 1.963(.443); 1.876(.445) | 0.865; 0.860 |
| MSPSS_others | 1.00 | 7.00 | 4.689(1.951); 4.677(1.906) | 0.927; 0.925 |
| MSPSS_family | 1.00 | 7.00 | 4.988(1.708); 4.812(1.694) | 0.909; 0.886 |
| MSPSS_friends | 1.00 | 7.00 | 4.690(1.732); 4.727(1.171) | 0.923; 0.931 |
| WCQ_wishfulthinking | 0.00 | 3.00 | 2.017(.676); 1.925(0.764) | 0.733; 0.783 |
| WCQ_goal-oriented | 0.00 | 3.00 | 1.844(.719); 1.957(0.753) | 0.797; 0.814 |
| WCQ_seeksupport | 0.00 | 3.00 | 1.285(.783); 1.425(0.823) | 0.801; 0.820 |
| WCQ_thinkover | 0.00 | 3.00 | 1.611(.785); 1.840(0.745) | 0.719; 0.711 |
| WCQ_avoid | 0.00 | 3.00 | 1.544(.750); 1.555(0.753) | 0.807; 0.785 |
| Minimum | Maximum | Mean1 (SD1); Mean2 (SD2) | α1, α2 | |
|---|---|---|---|---|
| DES | 0.00 | 100.00 | 16.796(15.244); 18.226(15.760) | 0.939; 0.938 |
| DES amnesia | 0.00 | 85.00 | 10.076(13.708); 10.961(13.767) | 0.932; 0.822 |
| DES depersonalization | 0.00 | 96.00 | 10.435(16.621); 12.361(16.808) | 0.861; 0.860 |
| DES absorption | 0.00 | 100.00 | 28.878(15.244); 31.356(22.612) | 0.863; 0.870 |
| PSS | 0.07 | 4.00 | 2.149(.833); 2.050(.863) | 0.911; 0.908 |
| SHAI | 1.00 | 4.00 | 1.912(.420); 1.936(.423) | 0.866; 0.862 |
| MSPSS_others | 1.00 | 5.00 | 4.552(.871); 4.356(1.049) | 0.905; 0.915 |
| MSPSS_family | 1.00 | 5.00 | 3.871(1.138); 3.644(1.259) | 0.914; 0.931 |
| MSPSS_friends | 1.00 | 5.00 | 4.178(1.060); 3.920(1.226) | 0.934; 0.935 |
| WCQ_humor | 0.00 | 3.00 | 1.707(1.103); 1.672(1.130) | |
| WCQ_positive | 0.00 | 3.00 | 1.374(.735); 1.402(0.784) | 0.697; 0.746 |
| WCQ_distancing | 0.00 | 3.00 | 0.800(.950); 0.901(613) | 0.505; 0.591 |
| WCQ_outer_persepctive | 0.00 | 3.00 | 1.716(.726); 1.776(0.808) | 0.591; 0.673 |
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 DES | |||||||||||||
| 2 DES_amnesia | 0.800 *** | ||||||||||||
| 3 DES_deperson | 0.856 *** | 0.685 *** | |||||||||||
| 4 DES_absorption | 0.936 *** | 0.628 *** | 0.701 *** | ||||||||||
| 5 Perceived stress | 0.436 *** | 0.268 *** | 0.351 *** | 0.473 *** | |||||||||
| 6. SHAI | 0.393 *** | 0.253 *** | 0.327 *** | 0.423 *** | 0.481 *** | ||||||||
| 7. MSPSS_others | −0.139 ** | −0.59 | −0.197 *** | −0.107 * | −0.199 *** | −0.168 *** | |||||||
| 8. MSPSS_family | −0.171 *** | −0.116 * | −0.183 *** | −0.155 *** | −0.287 *** | −0.220 *** | 0.530 *** | ||||||
| 9. MSPSS_friends | −0.145 *** | −0.048 | −0.180 *** | −0.119 ** | −0.221 *** | −0.147 *** | 0.610 *** | 0.518 *** | |||||
| 10. WCQ_wishfulthink | 0.413 *** | 0.262 *** | 0.351 *** | 0.443 *** | 0.480 *** | 0.411 *** | −0.025 | −0.107 * | −0.006 | ||||
| 11. WCQ_goal-oriented | −0.061 | −0.005 | −0.069 | −0.068 | −0.283 *** | −0.095 * | 0.265 *** | 0.279 *** | 0.260 *** | 0.165 *** | |||
| 12. WCQ_seeksupport | −0.072 | 0.049 | −0.061 | −0.104 * | −0.152 *** | −0.048 | 0.462 *** | 0.383 *** | 0.479 *** | 0.053 | 0.427 *** | ||
| 13. WCQ_thinkover | 0.106 * | 0.111 * | 0.099* | 0.095 * | −0.145 *** | 0.073 | 0.169 *** | 0.205 *** | 0.145 *** | 0.283 *** | 0.540 *** | 0.398 *** | |
| 14. WCQ_avoid | 0.163 *** | 0.123 ** | 0.160*** | 0.125 ** | −0.014 | −0.011 | −0.163*** | −0.048 | −0.126 ** | 0.240 *** | 0.312 *** | −0.036 | 0.293 *** |
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 DES | ||||||||||||
| 2 DES_amnesia | 0.809 *** | |||||||||||
| 3 DES_deperson | 0.818 *** | 0.603 *** | ||||||||||
| 4 DES_absorption | 0.952 *** | 0.684 *** | 0.682 *** | |||||||||
| 5 Perceived stress | 0.450 *** | 0.340 *** | 0.372 *** | 0.438 *** | ||||||||
| 6. SHAI | 0.316 *** | 0.213 *** | 0.278 *** | 0.304 *** | 0.437 *** | |||||||
| 7. MSPSS_others | −0.200 *** | −0.185 *** | −0.215 *** | −0.159 *** | −0.265 *** | −0.124 *** | ||||||
| 8. MSPSS_family | −0.285 *** | −0.244 *** | −0.245 *** | −0.265 *** | −0.395 *** | −0.222 *** | 0.526 *** | |||||
| 9. MSPSS_friends | −0.158 *** | −0.121 *** | −0.186 *** | −0.125 *** | −0.274 *** | −0.208 *** | 0.562 *** | 0.481 *** | ||||
| 10.WCQ_humor | −0.039 | −0.031 | 0.008 | −0.053 | −0.274 *** | −0.210 *** | 0.111 *** | 0.153 *** | 0.198 *** | |||
| 11. WCQ_positive | −0.078 ** | −0.066 * | −0.042 | −0.070 * | −0.400 *** | −0.241 *** | 0.235 *** | 0.329 *** | 0.269 *** | 0.444 *** | ||
| 12. WCQ_distancing | 0.322 *** | 0.240 *** | 0.296 *** | 0.307 *** | 0.367 *** | 0.247 *** | −0.095 *** | −0.153 *** | −0.050 | 0.032 | 0.002 | |
| 13.WCQ_outer_pers | 0.006 | −0.005 | 0.022 | 0.010 | −0.164 *** | −0.071 * | 0.228 *** | 0.200 *** | 0.297 *** | 0.259 *** | 0.468 *** | 0.137 *** |
| Dependent Variables | Independent Variables | Indirect Effects | Direct Effects | Index of Moderated Mediation | ||
|---|---|---|---|---|---|---|
| Measurement 1 | Measurement 2 | Measurement 1 | Measurement 2 | |||
| absorption | SHAI | 3.930 * (2.817; 5.253) | 4.617 * (2.958; 6.441) | 5.890 * (2.772; 9.008) | 7.044 * (1.284; 12.083) | 0.687 (−1.012; 2.437) |
| MSPSS_others | −0.000 (0.283; −0.565) | 4.617 * (2.958; 6.441) | 0.197 (−0.592; 0.989) | −0.597 (−3.161; 1.968) | 0.197 (−0.558; 0.971) | |
| MSPSS_family | −1.149 * (−1.590; −0.732) | −0.940 * (−1.5656; −0.316) | −2.322 * (−3.597; −1.048) | −3.902 * (−5.944; −1.859) | −0.209 (−0.384; 0.836) | |
| MSPSS_friends | −0.244 (−0.738; 0.219) | −0.824 * (−1.486; −0.165) | 0.627 (−0.777; 2.032) | −0.289 (−2.452; 1.875) | −0.580 (−1.250; 0.057) | |
| WCQ_humor | −0.568 * (−0.980; −0.192) | −0.967 * (−1.629; −0.352) | 0.706 (−1.439; 2.850) | 0.104 (−1.108; 1.316) | −0.400 (−1.095; 0.271) | |
| WCQ_positive | −2.232 * (−2.994; −1.538) | −2.470 * (−3.594; −1.434) | 4.191 * (2.157; 6.225) | 2.697 (−0.581; 5.976) | −0.238 (−1.243; 0.775) | |
| WCQ_distancing | 3.949 * (2.954; 5.007) | 3.637 * (2.386; 5.016) | 4.887 * (2.407; 7.367) | 5.678 * (1.725; 9.632) | −0.312 (−1.540; 0.968) | |
| WCQ_outer_pers | 0.142 (−0.450; 0.748) | 0.053 (−0.834; 0.939) | 0.7034 (−1.270; 2.677) | −1.856 (−5.215; 1.503) | −0.089 (−1.077; 0.903) | |
| depersonalization | SHAI | 1.834 * (1.174; 2.595) | 2.155 * (1.239; 3.254) | 4.984 * (2.499; 7.470) | 5.311 * (0.720; 9.902) | 0.321 (−0.497; 1.167) |
| MSPSS_others | 0.000 (−0.258; 0.271) | 0.092 (−0.279; 0.482) | −2.042 * (−3.449; −0.635) | −2.611 * (−4.655; −0.567) | 0.092 (−0.275; 0.476) | |
| MSPSS_family | −0.536 * (−0.788; −0.313) | −0.438 * (−0.764; −0.149) | −1.414 * (−2.430; −0.397) | −2.034 * (−3.663; −0.405) | 0.098 (−0.188; 0.402) | |
| MSPSS_friends | −0.114 (−0.359; 0.110) | −0.385 * (−0.722; −0.069) | 0.068 (−1.052; 1.187) | −0.195 (−1.920; 1.530) | −0.271 (−0.606; 0.415) | |
| WCQ_humor | −0.265 * (−0.479; −0.084) | −0.452 * (−0.782; −0.154) | 0.715 (−0.251; 1.681) | 1.061 (−0.649; 2.770) | −0.186 (−0.512; 0.139) | |
| WCQ_positive | −1.042 * (−1.493; −0.637) | −1.153 (−1.783; 0.607) | 2.354 * (0.732; 3.976) | 2.115 (−0.499; 4.729) | −0.111 (−0.608; 0.381) | |
| WCQ_distancing | 1.849 * (1.216; 2.556) | 1.703 * (1.019; 2.525) | 4.091 * (2.117; 6.065) | 7.481 * (4.334; 10.628) | −0.146 (−0.765; 0.464) | |
| WCQ_outer_pers | 0.066 (−0.221; 0.369) | 0.025 (−0.388; 0.452) | 0.802 (−1.200; 1.949) | 1.366 (−2.928; 2.430) | −0.041 (−0.515; 0.444) | |
| amnesia | SHAI | 1.576 * (0.980; 2.336) | 1.851 * (1.068; 2.839) | 1.768 (−0.364; 3.901) | 1.136 (−2.803; 5.075) | 0.275 (−0.415; 0.986) |
| MSPSS_others | 0.000 (−0.240; 0.226) | 0.079 (−0.250; 0.406) | −0.722 (−1.928; 0.485) | −1.864 * (−3.617; −0.111) | 0.079 (−0.231; 0.410) | |
| MSPSS_family | −0.460 * (−0.681; −0.269) | −0.377 * (−0.674; −0.132) | −1.155 * (−2.027; −2.083) | −1.993 * (−3.390; −0.596) | 0.0838 (−0.167; 0.339) | |
| MSPSS_friends | −0.097 (−0.301; 0.096) | −0.328 * (−0.623; −0.064) | 0.484 (−0.477; 1.444) | −0.341 (−1.821; 1.138) | −0.231 (−0.516; 0.028) | |
| WCQ_humor | −0.229 * (−0.415; −0.077) | −0.390 * (−0.694; −0.133) | 0.183 (0.665; −0.646) | 1.435 (−0.030; 2.901) | −0.161 (−0.4709; 0.106) | |
| WCQ_positive | −0.893 * (−1.296; −0.543) | −0.989 * (−1.572; −0.511) | 1.770 * (0.379; 3.162) | 1.211 (−1.032; 3.453) | −0.095 (−0.552; 0.326) | |
| WCQ_distancing | 1.580 * (1.020; 2.215) | 1.456 * (0.854; 2.179) | 3.092 * (1.396; 4.788) | 3.373 * (0.669; 6.077) | −0.125 (−0.667; 0.398) | |
| WCQ_outer_pers | 0.057 (−0.193; 0.308) | 0.021 (−0.334; 0.407) | −0.473 (−1.824; 0.877) | −1.282 (−3.5809; 1.016) | −0.035 (−0.441; 0.372) | |
| Dissociation sum | SHAI | 2.447 * (1.688; 3.293) | 2.875 * (0.582; 4.092) | 4.214 * (1.989; 6.440) | 4.4969 * (0.386; 8.607) | 0.427 (−0.651; 1.557) |
| MSPSS_others | −0.000 (−0.349; 0.353) | 0.122 (−0.373; 0.611) | −0.892 (−2.151; 0.368) | −1.691 (−3,52; 0.139) | 0.123 (−0.358; 0.591) | |
| MSPSS_family | −0.715 * (−1.004; −0.458) | −0.585 * (−0.993; −0.195) | −1.630 * (−2.540; −0.721) | −2.643 * (−4.101; −1.185) | 0.130 (−0.258; 0.536) | |
| MSPSS_friends | −0.151 (−0.445; 0.144) | −0.512 * (−0.930; −0.110) | 0.392 (−0.609; 1.395) | −0.275 (−1.819; 1.269) | −0.361 (−0.776; 0.030) | |
| WCQ_humor | −0.354 * (−0.625; −0.113) | −0.603 * (−1.035; −0.222) | 0.334 (−0.531; 1.199) | 1.067 (−0.463; 2.598) | −0.249 (−0.702; 0.168) | |
| WCQ_positive | −1.389 * (−1.900; −0.935) | −1.537 * (−2.268; −0.868) | 2.772 (1.320; 4.224) | 2.008 (−0.332; 4.348) | −0.148 (−0.798; 0.523) | |
| WCQ_distancing | 2.459 * (1.787; 3.177) | 2.265 * (1.467; 3.180) | 4.023 * (2.254; 5.793) | 5.511 * (2.690; 8.331) | −0.194 (−1.009; 0.590) | |
| WCQ_outer_pers | 0.088 (−0.287; 0.456) | 0.033 (−0.548; 0.609) | 0.202 (−1.207; 1.611) | −1.129 (−3.527; 1.269) | −0.055 (−0.672; 0.577) | |
| Dependent Variables | Independent Variables | Indirect Effects | Direct Effects | Index of Moderated Mediation | ||
|---|---|---|---|---|---|---|
| Measurement 1 | Measurement 2 | Measurement 1 | Measurement 2 | |||
| absorption | SHAI | 3.841 * (1.963; 5.974) | 3.304 * (1.157; 6.103) | 9.230 * (3.532; 14.928) | 19.143 * (10.651; 27.636) | −0.537 (−2.802; 1.822) |
| MSPSS_others | 0.079 (−0.213; 0.381) | −0.087 (−0.597; 0.420) | 0.043 (−1.376; 1.462) | 0.697 (−1.370; 2.765) | −0.166 (−0.730; 0.369) | |
| MSPSS_family | −0.167 (−0.546; 0.164) | −0.380 (−0.996; 0.159) | 0.2938 (−1.210; 1.798) | 1.300 (−0.978; 3.578) | −0.213 (−0.836; 0.340) | |
| MSPSS_friends | −0.420 * (−0.830; −0.067) | −0.574 * (−1.254; −0.018) | −0.205 (−1.792; 1.382) | 1.379 (−0.994; 3.752) | −0.153 (−0.792; 0.482) | |
| WCQ_wishfulthinking | 3.628 * (2.010; 5.093) | 5.1169 * (2.720; 7.976) | 8.604 * (4.659; 12.550) | 5.835 * (0.524; 11.147) | 1.488 * (0.121; 3.353) | |
| WCQ_goal-oriented | −2.561 * (−4.038; −1.299) | −0.678 (−2.118; 0.515) | −1.765 (−5.691; 2.161) | 2.682 (−8.164; 2.377) | 1.883 * (0.524; 3.508) | |
| WCQ_seeksupport | 0.735 (−0.048; 1.598) | 0.255 (−0.791; 1.397) | −3.924 * (−7.353; −0.494) | 2.451 (−9.0807; 0.552) | −0.480 (−1.749; 0.771) | |
| WCQ_thinkover | −1.472 * (−2.597; −0.622) | −0.939 (−2.273; 0.234) | 4.187 (0.694; 7.680) | 5.244 (−0.014; 10.502) | 0.533 (−0.793; 2.036) | |
| WCQ_avoid | −0.087 (−0.839; 0.722) | −0.006 (−1.056; 1.219) | 3.575 * (0.269; 6.882) | −4.392 (−1.056; 1.219) | 0.081 (−1.224; 1.455) | |
| depersonalization | SHAI | 1.393 * (0.080; 2.913) | 1.198 * (0.046; 2.888) | 6.512 * (1.340; 11.683) | 3.923 * (6.111; 21.527) | −0.195 (−1.186; 0.779) |
| MSPSS_others | 0.029 (−0.086; 0.161) | −0.031 (−0.248; 0.174) | −0.732 (−2.019; 0.555) | −0.394 (−2.268; 1.480) | −0.060 (−0.309; 0.151) | |
| MSPSS_family | −0.060 (−0.251; 0.051) | −0.137 (−0.456; 0.053) | 0.281 (−1.083; 1.645) | 0.771 (−1.295; 2.837) | −0.077 (−0.370; 0.132) | |
| MSPSS_friends | −0.152 (−0.374; 0.003) | −0.207 (−0.522; 0.029) | −0.918 (−2.357; 0.521) | 0.054 (−2.098; 2.206) | −0.055 (−0.311; 0.206) | |
| WCQ_wishfulthinking | 1.410 * (0.136; 2.710) | 1.988 * (0.189; 3.863) | 6.189 * (2.624; 9.754) | 1.139 (−3.660; 5.938) | 0.578 (−0.010; 1.511) | |
| WCQ_goal-oriented | −0.930 * (−1.939; −0.037) | −0.246 (−1.007; 0.193) | −2.143 (−5.701; 1.415) | −2.963 (−7.740; 1.813) | 0.683 (0.004; 1.578) | |
| WCQ_seeksupport | 0.264 (−0.041; 0.725) | 0.092 (−0.319; 0.641) | 0.225 (−2.883; 3.333) | 2.221 (−4.254; 4.477) | −0.173 (−0.763; 0.335) | |
| WCQ_thinkover | −0.532 * (−1.219; −0.033) | −0.339 (−0.969; 0.103) | 2.121 (−1.045; 5.287) | 1.749 (−3.017; 6.515) | 0.193 (−0.285; 0.909) | |
| WCQ_avoid | −0.031 (−0.358; 0.304) | −0.002 (−0.504; 0.474) | 4.226 * (1.211; 7.240) | 0.258 (−4.131; 4.648) | 0.029 (−0.552; 0.570) | |
| amnesia | SHAI | 1.417 * (0.373; 2.709) | 1.219 * (0.244; 2.571) | 4.507 (−0.022; 9.036) | 9.654 * (2.904; 16.404) | −0.198 (−1.172; 0.684) |
| MSPSS_others | 0.029 (−0.082; 0.154) | −0.032 (−0.237; 0.160) | −0.135 (−1.260; 0.991) | −0.641 (−2.280; 0.998) | −0.061 (−0.300; 0.136) | |
| MSPSS_family | −0.061 (−0.220; 0.055) | −0.139 (−0.421; 0.056) | 0.041 (−1.152; 1.235) | 0.053 (−1.754; 1.861) | −0.077 (−0.334; 0.133) | |
| MSPSS_friends | −0.152 * (−0.338; −0.014) | −0.207 (−0.487; 0.009) | 0.420 (−0.839; 1.679) | −0.474 (−2.357; 1.409) | −0.055 (−0.294; 0.192) | |
| WCQ_wishfulthinking | 1.401 * (0.454; 2.457) | 1.975 * (0.631; 3.547) | 2.809 (−0.314; 5.931) | −0.765 (−4.969; 3.439) | 0.575 * (0.015; 1.431) | |
| WCQ_goal-oriented | −0.959 * (−1.744; −0.260) | −0.254 (−0.936; 0.179) | −1.278 (−4.390; 1.834) | −2.443 (−6.621; 1.735) | 0.705 * (0.124; 1.444) | |
| WCQ_seeksupport | 0.270 (−0.014; 0.693) | 0.094 (−0.317; 0.564) | 1.486 (−1.232; 4.205) | 1.407 (−2.412; 5.225) | −0.177 (−0.742; 0.266) | |
| WCQ_thinkover | −0.552 * (−1.146; −0.119) | −0.352 (−0.976; 0.078) | 2.724 (−0.043; 5.490) | 0.485 (−3.679; 4.650) | 0.200 (−0.300; 0.836) | |
| WCQ_avoid | −0.032 (−0.339; 0.271) | −0.002 (−0.452; 0.455) | 3.633 * (0.992; 6.273) | 1.129 (−2.716; 4.973) | 0.030 (−0.496; 0.571) | |
| Dissociation sum | SHAI | 2.217 * (0.998; 3.695) | 1.907 * (0.583; 3.790) | 6.750 * (2.199; 11.300) | 14.205 * (7.423; 20.987) | −0.310; (−0.634; 1.081) |
| MSPSS_others | −0.125 (0.046; 0.233) | −0.050 (−0.357; 0.247) | −0.274 (−1.407; 0.859) | −0.112 (−1.763; 1.538) | −0.096 (−0.439; 0.225) | |
| MSPSS_family | −0.096 (−0.328; 0.084) | −0.219 (−0.587; 0.087) | 0.205 (−0.995; 1.406) | 0.708 (−1.111; 2.527) | −0.122 (−0.495; 0.210) | |
| MSPSS_friends | −0.241 * (−0.500; −0.035) | −0.330 (−0.730; 0.005) | −0.234 (−1.503; 1.034) | 0.320 (−1.577; 2.216) | −0.088 (−0.456; 0.300) | |
| WCQ_wishfulthinking | 2.146 * (1.025; 3.424) | 3.027 * (1.440; 4.886) | 5.867 * (2.724; 9.011) | 2.070 (−2.162; 6.301) | 0.880 * (0.059; 1.962) | |
| WCQ_goal-oriented | −1.484 * (−2.449; −0.655) | −0.393 (−1.330; 0.316) | −1.729 (−4.862; 1.405) | −2.767 (−6.973; 1.440) | 1.091 * (0.262; 2.098) | |
| WCQ_seeksupport | 0.423 (−0.016; 1.009) | 0.147 (−0.453; 0.869) | −0.737 (−3.475; 3.000) | −0.915 (−4.760; 2.929) | −0.276 (−1.056; 0.484) | |
| WCQ_thinkover | −0.852 * (−1.567; −0.307) | −0.543 (−1.352; 0.141) | 3.011 * (0.222; 5.799) | 2.493 (−1.704; 6.690) | 0.309 (−0.462; 1.238) | |
| WCQ_avoid | −0.050 (−0.496; 0.427) | −0.003 (−0.646; 0.706) | 3.811 * (1.162; 6.460) | −1.001 (−4.858; 2.855) | 0.047 (−0.731; 0.813) | |
| Dependent Variables | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Perceived Stress | Absorption | Depersonalization | Amnesia | Dissociation | ||||||
| Independent Variable | Coeff | SE | Coeff | SE | Coeff | SE | Coeff | SE | Coeff | SE |
| Perceived stress | 8.611 *** | 0.842 | 4.019 *** | 0.671 | 3.453 *** | 0.576 | 5.361 *** | 0.601 | ||
| SHAI | 0.456 *** | 0.53 | 5.890 *** | 1.589 | 4.985 *** | 1.267 | 1.768 | 1.087 | 4.214 *** | 1.134 |
| MSPSS_others | −0.093 | 0.028 | 0.089 | 0.833 | −2.189 ** | 0.664 | −1.005 | 0.570 | −1.096 | 0.595 |
| MSPSS_family | −0.127 *** | 0.020 | −2.675 *** | 0.602 | −1.552 ** | 0.480 | −1.343 ** | 0.412 | −1.857 *** | 0.430 |
| MSPSS_friends | −0.044 | 0.023 | 0.416 | 0.666 | 0.007 | 0.531 | 0.295 | 0.456 | 0.239 | 0.475 |
| WCQ_humor | −0.076 *** | 0.019 | 0.228 | 0.560 | 0.789 | 0.446 | 0.460 | 0.383 | 0.492 | 0.400 |
| WCQ_pos | −0.264 *** | 0.032 | 3.880 *** | 0.964 | 2.307 ** | 0.768 | 1.636 * | 0.659 | 2.608 *** | 0.688 |
| WCQ_avoid | 0.448 *** | 0.036 | 5.092 *** | 1.112 | 4.982 *** | 0.886 | 3.168 *** | 0.761 | 4.414 *** | 0.794 |
| WCQ_out | 0.014 | 0.032 | 0.140 | 0.921 | 0.237 | 0.734 | −0.650 | 0.630 | −0.091 | 0.657 |
| Constant | 2.036 *** | 0.155 | −0.968 | 4.81 | −0.758 | 3.836 | 3.285 | 3.291 | 0.520 | 3.434 |
| R2 = 0.411 F(10,1186) = 82.65 *** | R2 = 0.244 F(11,1185) = 34.836 *** | R2 = 0.199 F(11,1185) = 26.818 *** | R2 = 0.130 F(11,1185) = 16.067 *** | R2 = 0.244 F(11,1185) = 38.685 *** | ||||||
| Dependent Variables | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Perceived Stress | Absorption | Depersonalization | Amnesia | Dissociation | ||||||
| Independent Variable | Coeff | SE | Coeff | SE | Coeff | SE | Coeff | SE | Coeff | SE |
| Perceived stress | - | - | 7.310 *** | 1.483 | 2.651 * | 1.346 | 2.697 * | 1.178 | 4.219 *** | 1.184 |
| SHAI | 0.525 *** | 0.087 | 9.230 ** | 2.900 | 6.512 * | 2.632 | 4.507 | 2.305 | 6.750 ** | 2.316 |
| MSPSS_others | 0.005 | 0.020 | 0.173 | 0.658 | −0.674 | 0.597 | −0.290 | 0.523 | −0.264 | 0.525 |
| MSPSS_family | −0.031 | 0.021 | 0.616 | 0.689 | 0.453 | 0.626 | 0.075 | 0.548 | 0.381 | 0.551 |
| MSPSS_friends | −0.063 ** | 0.023 | 0.147 | 0.748 | −0.706 | 0.679 | 0.190 | 0.595 | −0.123 | 0.598 |
| WCQ_wishful | 0.560 *** | 0.050 | 7.512 *** | 1.800 | 4.465 ** | 1.634 | 1.589 | 1.431 | 4.522 ** | 1.438 |
| WCQ_goaloriented | −0.274 *** | 0.054 | −2.248 | 1.779 | −2.496 | 1.615 | −1.708 | 1.414 | −2.151 | 1.421 |
| WCQ_seeksupport | 0.079 | 0.049 | −3.597 * | 1.571 | 0.506 | 1.426 | 1.684 | 1.249 | −0.469 | 1.255 |
| WCQ_avoid | −0.010 | 0.046 | 1.398 | 1.466 | 3.191 * | 1.331 | 2.176 | 1.293 | 2.893 * | 1.299 |
| WCQ_thinkover | −0.186 | 0.050 | 4.464 ** | 1.627 | 2.039 | 1.477 | 2.991 * | 1.165 | 2.527 * | 1.171 |
| Constant | 1.310 *** | 0.219 | −23.218 ** | 7.325 | −14.271 * | 6.649 | −13.786 * | 5.822 | −17.091 ** | 5.850 |
| R2 = 0.456 F(11,471) = 35.910 *** | R2 = 0.334 F(12,470) = 19.643 *** | R2 = 0.193 F(12,470) = 9.373 *** | R2 = 0.137 F(12,470) = 6.217 *** | R2 = 0.262 F(12,470) = 13.936 *** | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kolozsvári, L.R.; Rekenyi, V.; Garbóczy, S.; Hőgye-Nagy, Á.; Szemán-Nagy, A.; Sayed-Ahmad, M.; Héjja-Nagy, K. Effects of Health Anxiety, Social Support, and Coping on Dissociation with Mediating Role of Perceived Stress during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2023, 20, 5491. https://doi.org/10.3390/ijerph20085491
Kolozsvári LR, Rekenyi V, Garbóczy S, Hőgye-Nagy Á, Szemán-Nagy A, Sayed-Ahmad M, Héjja-Nagy K. Effects of Health Anxiety, Social Support, and Coping on Dissociation with Mediating Role of Perceived Stress during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2023; 20(8):5491. https://doi.org/10.3390/ijerph20085491
Chicago/Turabian StyleKolozsvári, László Róbert, Viktor Rekenyi, Szabolcs Garbóczy, Ágnes Hőgye-Nagy, Anita Szemán-Nagy, Mohamed Sayed-Ahmad, and Katalin Héjja-Nagy. 2023. "Effects of Health Anxiety, Social Support, and Coping on Dissociation with Mediating Role of Perceived Stress during the COVID-19 Pandemic" International Journal of Environmental Research and Public Health 20, no. 8: 5491. https://doi.org/10.3390/ijerph20085491
APA StyleKolozsvári, L. R., Rekenyi, V., Garbóczy, S., Hőgye-Nagy, Á., Szemán-Nagy, A., Sayed-Ahmad, M., & Héjja-Nagy, K. (2023). Effects of Health Anxiety, Social Support, and Coping on Dissociation with Mediating Role of Perceived Stress during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health, 20(8), 5491. https://doi.org/10.3390/ijerph20085491







