Moving Forward from Moral Injury: A Mixed Methods Study Investigating the Use of 3MDR for Treatment-Resistant PTSD
Abstract
1. Introduction
Multi-modal Motion-Assisted Memory Desensitization and Reconsolidation (3MDR)
2. Materials and Methods
2.1. Study Design
2.2. Sample and Setting
2.3. Sample Size
2.4. Intervention
2.5. Data Collection
2.6. Quantitative Data
2.7. Qualitative Data
2.8. Data Analysis and Triangulation
2.9. Quantitative Analysis
2.10. Qualitative Measures
3. Results
3.1. Demographics
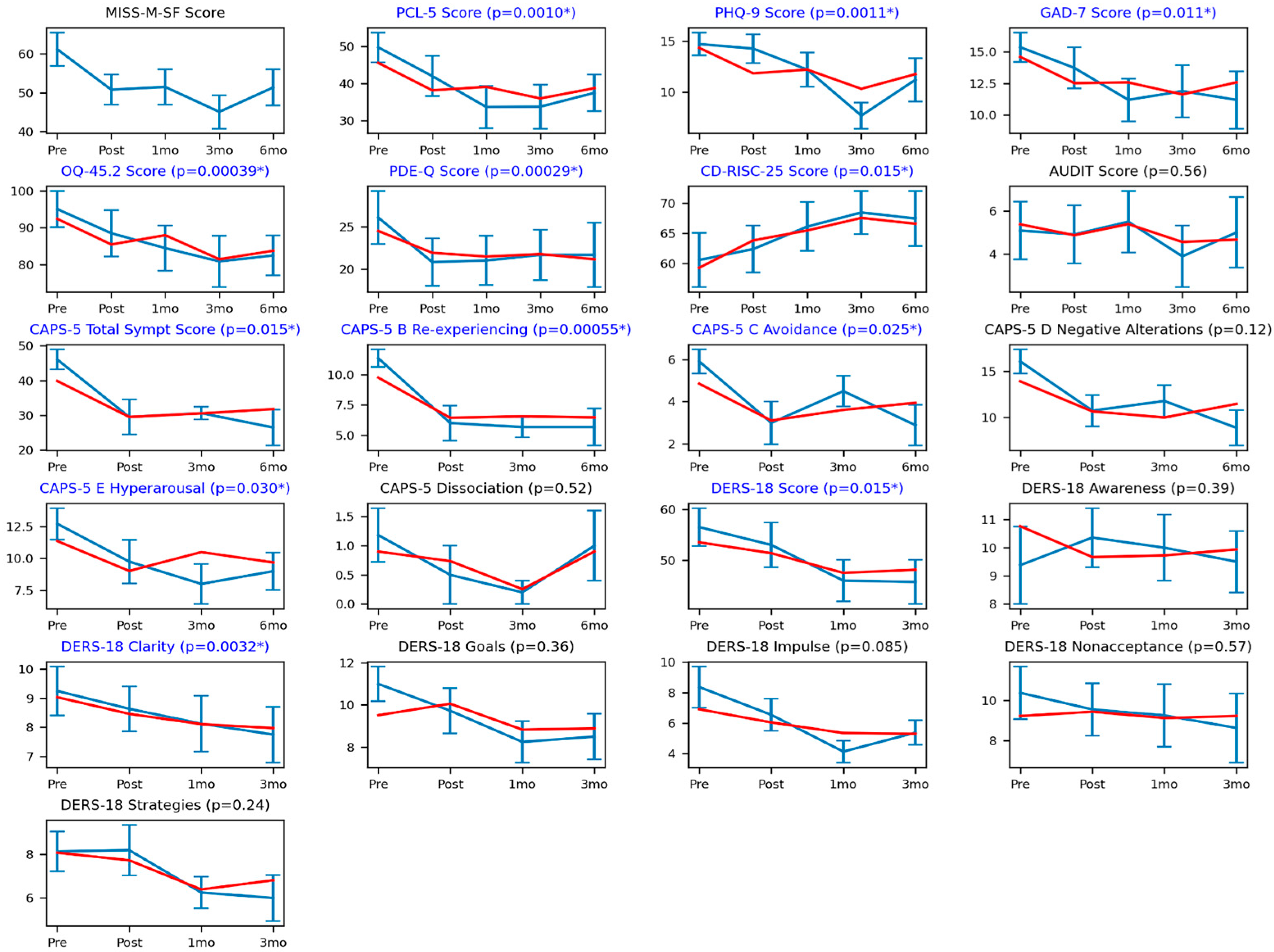
3.2. Quantitative Results
3.3. Qualitative Results
3.3.1. Realities of War
“First time out, you know, everyone was smiling, we were having a good time and by the end of the tour, you’re basically threatening to kill kids.”(P13)
One of the pictures I have over there is a painting of what they would do with the children, they would skeet shoot them, throw them in the air and see if they could hit them with bayonets, things like that. It was a little troubling [laughing](P10)
“If you can’t dump it, you gotta file that in the back of our head, because there is still a mission that needs to go on and nobody wants to talk about that shit, ok? So, (…) unfortunately, sometimes that [door] gets cracked open and I could never shut that door completely, I could never file completely in the back of my mind to make sure that I could get rid of it.”(P19)
I couldn’t do anything because I wasn’t allowed to do anything. I didn’t do what I wanted to. It doesn’t make it okay.”(P11)
“How do I go and do this [mission] when I know it is wrong? Like, morally it’s wrong. Ethically, it’s wrong. But I’m told I gotta do this. What do you do? How do you function with that? And you know, I don’t mean squeezing the trigger. I don’t mean lobbing artillery. I don’t mean driving over stuff. It’s the fact of, people are hurt and they need help, there are good people and bad people.”(P19)
“[I felt] abandoned… When there were a lot of us, after those two weeks [spent cleaning up after the traumatic event], we were just cut loose. We were given one day off then told to go back [to regular duties]…just by the organization in general.”(P6)
3.3.2. Wrestling Scruples
“But we don’t understand that those that are left behind carry the pain, it stays with them, that we feel nothing, barren…”(P13)
“I felt trapped in my little existence, I guess, like, shit… This is the way it’s going to be from now until whenever it ended you know. And that was scary…very depressing. Like trapped. I was stuck there… I’m going to have to put up with this all the time. And eventually, it’s going to crush me.”(P6)
“Why did you do this? Like why couldn’t you get along? I was always told, ‘work things out, trust people…’ All I saw was the good and never the bad …My whole life got shattered right there and then. All I wrote about when I came back was the devastation of what I saw. I did feel devastated. I felt the heartless[ness] of people.”(P3)
“This feeling of being lost really. Not understanding, not being able to comprehend… comprehend what happened.”(P7)
The word shame is … a … Huge. You take pride in everything you have accomplished. When you don’t live up to that persona, even in your own mind or even to those around you, it’s… it’s painful.”(P13)
I’m worried that it means we were a little less than human and more mechanical in what we did. It was all mechanical… you follow the checklist; you do what you’re trained to do. Could we have done more? The honest answer is no, but we don’t know.”(P19)
“Every time the kids fight, and someone gets hurt, I just see the crying face of this little girl looking up at me and not knowing if I’m there to help or hurt. Just so little and dependent on everyone around her to help (…) I’m not looking at my grandson or kids like they’re this little girl, but it automatically takes me back to this coppery smell in the air, all that blood, and then the eyes.”(P19)
3.3.3. Moral Sensemaking
[3MDR] showed me how not to suppress the emotional aspect, but just come to grips with it (…). How you feel is how you feel. There is nothing wrong with feeling that way, but understand why you feel that way.”(P19)
“Weight on my neck, stopping me from doing what I need to do with my kids—guilt, pain, sorry, the feeling that I might actually be human. I might have emotions aside from what I’ve been trained to deal with.”(P2)
“The pain that I didn’t know was there… Never even considered… I buried it so deep that I just left it where I put it. And I open that box. Once the box is open, it basically gets poured out. And either… you can make the decision to either fill the box back up or just leave it on the ground. And I think I have left it on the ground.”(P13)
Maybe I was just there to give somebody a little bit of dignity in death. And I think that kind of helped [me].”(P6)
“Stuff still gets under my skin; I’m human. I still have reactions, I just don’t blow up about it.”(P19)
“Started to realize there is good and bad everywhere, no matter where you go.”(P2)
“Well I’m saying goodbye to my, my.. demon and my…shame; my perceived shame [strong emphasis]”(P13)
“I was very closed, I was very closed off; primarily to my family, but you know, to everyone I was very closed. I never wanted to say anything because you know what, I would stay open. [broken up] Everyone has parts of their own pasts that they have to deal with. Who am I to dump more crap on someone’s head? Right? Unfortunately, what wound up happening was me trying to internalize it was tearing me apart.”(P19)
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 3rd ed.; American Psychiatric Association Publications: Arlington, VA, USA, 1980. [Google Scholar]
- Shay, J. Achilles in Vietnam: Combat Trauma and the Undoing of Character; Scribner: New York, NY, USA, 2010. [Google Scholar]
- Litz, B.T.; Stein, N.; Delaney, E.; Lebowitz, L.; Nash, W.P.; Silva, C.; Maguen, S. Moral injury and moral repair in war veterans: A preliminary model and intervention strategy. Clin. Psychol. Rev. 2009, 29, 695–706. [Google Scholar] [CrossRef]
- Jinkerson, J.D. Defining and assessing moral injury: A syndrome perspective. Traumatology 2016, 22, 122–130. [Google Scholar] [CrossRef]
- Battles, A.R.; Bravo, A.J.; Kelley, M.L.; White, T.D.; Braitman, A.L.; Hamrick, H.C. Moral injury and PTSD as mediators of the associations between morally injurious experiences and mental health and substance use. Traumatology 2018, 24, 246–254. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association Publications: Arlington, VA., USA, 2013. [Google Scholar]
- Stein, N.R.; Mills, M.A.; Arditte, K.; Mendoza, C.; Borah, A.M.; Resick, P.A.; Brett, T.L.; Strong Star Consortium. A scheme for categorizing traumatic military events. Behav. Modif. 2012, 36, 787–807. [Google Scholar] [CrossRef]
- Vermetten, E.; Jetly, R. A critical outlook on combat-related PTSD: Review and case reports of guilt and shame as drivers for moral injury. Mil. Behav. Health 2018, 6, 156–164. [Google Scholar] [CrossRef]
- Atuel, H.R.; Barr, N.; Jones, E.; Greenberg, N.; Williamson, V.; Schumacher, M.R.; Vermetten, E.; Jetly, R.; Castro, C.A. Understanding moral injury from a character domain perspective. J. Theor. Philos. Psychol. 2021, 41, 155–173. [Google Scholar] [CrossRef]
- Barnes, H.A.; Hurley, R.A.; Taber, K.H. Moral injury and PTSD: Often co-occurring yet mechanistically different. J. Neuropsychiatry Clin. Neurosci. 2019, 31, A4-103. [Google Scholar] [CrossRef]
- Hall, N.A.; Everson, A.T.; Billingsley, M.R.; Miller, M.B. Moral injury, mental health and behavioural health outcomes: A systematic review of the literature. Clin. Psychol. Psychother. 2022, 29, 92–110. [Google Scholar] [CrossRef] [PubMed]
- Griffin, B.J.; Purcell, N.; Burkman, K.; Litz, B.T.; Bryan, C.J.; Schmitz, M.; Villierme, C.; Walsh, J.; Maguen, S. Moral injury: An integrative review. J. Trauma. Stress 2019, 32, 350–362. [Google Scholar] [CrossRef] [PubMed]
- Williamson, V.; Stevelink, S.A.M.; Greenberg, N. Occupational moral injury and mental health: Systematic review and meta-analysis. Br. J. Psychiatry 2018, 212, 339–346. [Google Scholar] [CrossRef] [PubMed]
- Hamblen, J.L.; Norman, S.B.; Sonis, J.H.; Phelps, A.J.; Bisson, J.I.; Nunes, V.D.; Megnin-Viggars, O.; Forbes, D.; Riggs, D.S.; Schnurr, P. A guide to guidelines for the treatment of posttraumatic stress disorder in adults: An update. Psychotherapy (Chic) 2019, 56, 359–373. [Google Scholar] [CrossRef]
- Forbes, D.; Pedlar, D.; Adler, A.B.; Bennett, C.; Bryant, R.; Busuttil, W.; Cooper, J.; Creamer, M.C.; Fear, N.T.; Greenberg, N.; et al. Treatment of military-related post-traumatic stress disorder: Challenges, innovations, and the way forward. Int. Rev. Psychiatry 2019, 31, 95–110. [Google Scholar] [CrossRef]
- Hamner, M.B.; Robert, S.; Frueh, B.C. Treatment-resistant posttraumatic stress disorder: Strategies for intervention. CNS Spectr. 2004, 9, 740–752. [Google Scholar] [CrossRef]
- Jones, C.; Smith-MacDonald, L.; Miguel-Cruz, A.; Lentz, L.; Pike, A.; Brémault-Phillips, S. Tackling trauma with technology: Treating chronic combat-related PTSD in Canadian Armed Forces personnel and veterans with 3MDR. Annu. Rev. CyberTherapy Telemed. 2020, 18, 235–239. [Google Scholar]
- Steenkamp, M.M.; Litz, B.T.; Gray, M.J.; Lebowitz, L.; Nash, W.; Conoscenti, L.; Amidon, A.; Lang, A. A brief exposure-based intervention for service members with PTSD. Cogn. Behav. Pract. 2011, 18, 98–107. [Google Scholar] [CrossRef]
- Kitchiner, N.J.; Lewis, C.; Roberts, N.P.; Bisson, J.I. Active duty and ex-serving military personnel with post-traumatic stress disorder treated with psychological therapies: Systematic review and meta-analysis. Eur. J. Psychotraumatology 2019, 10, 1684226. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.; Smith-MacDonald, L.; Brown, M.R.G.; Vandehy, J.; Grunnet-Jepsen, R.; Ordek, V.P.; Kruger, S.; Ayres Gerhart, A.; Van Veelen, N.; Nijdam, M.J.; et al. The Redesign and Validation of Multimodal Motion-Assisted Memory Desensitization and Reconsolidation Hardware and Software: Mixed Methods, Modified Delphi-Based Validation Study. JMIR Hum. Factors 2022, 9, e33682. [Google Scholar] [CrossRef]
- Vermetten, E.; Meijer, L.; van der Wurff, P.; Mert, A. The effect of military motion-assisted memory desensitization and reprocessing treatment on the symptoms of combat-related post traumatic stress disorder: First preliminary results. Annu. Rev. Cybertherapy Telemed. 2013, 11, 125–128. [Google Scholar]
- van Gelderen, M.J.; Nijdam, M.J.; Vermetten, E. An Innovative Framework for Delivering Psychotherapy to Patients With Treatment-Resistant Posttraumatic Stress Disorder: Rationale for Interactive Motion-Assisted Therapy. Front. Psychiatry 2018, 9, 176. [Google Scholar] [CrossRef] [PubMed]
- van Gelderen, M.J.; Nijdam, M.; Haagen, J.; Vermetten, E. Interactive Motion-Assisted Exposure Therapy for Veterans with Treatment-Resistant Posttraumatic Stress Disorder: A Randomized Controlled Trial. Psychother. Psychosom. 2020, 89, 215–227. [Google Scholar] [CrossRef]
- Bisson, J.; van Deursen, R.; Hannigan, B.; Kitchiner, N.; Barawi, K.; Jones, K.; Pickles, T.; Skipper, J.; Young, C.; Abbott, L.R.; et al. Randomized controlled trial of multi-modular motion-assisted memory desensitization and reconsolidation (3MDR) for male military veterans with treatment-resistant post-traumatic stress disorder. Acta Psychiatr. Scand. 2020, 142, 141–151. [Google Scholar] [CrossRef] [PubMed]
- Jones, C.; Smith-MacDonald, L.; Brown, M.R.G.; Pike, A.; Vermetten, E.; Brémault-Phillips, S. Quantitative changes in mental health measures with 3MDR treatment for Canadian military members and veterans. Brain Behav. 2022, 12, e2694. [Google Scholar] [CrossRef] [PubMed]
- Roy, M.J.; Bellini, P.; Kruger, S.E.; Dunbar, K.; Atallah, H.; Haight, T.; Vermetten, E. Randomized controlled trial of motion-assisted exposure therapy for posttraumatic stress disorder after mild traumatic brain injury, with and without an eye movement task. Front. Virtual Real. 2022, 3, 1005774. [Google Scholar] [CrossRef]
- Borges, L.M.; Bahraini, N.H.; Holliman, B.D.; Gissen, M.R.; Lawson, W.C.; Barnes, S.M. Veterans’ perspectives on discussing moral injury in the context of evidence-based psychotherapies for PTSD and other VA treatment. J. Clin. Psychol. 2020, 76, 377–391. [Google Scholar] [CrossRef] [PubMed]
- Farnsworth, J.K.; Drescher, K.D.; Nieuwsma, J.A.; Walser, R.B.; Currier, J.M. The role of moral emotions in military trauma: Implications for the study and treatment of moral injury. Rev. Gen. Psychol. 2014, 18, 249–262. [Google Scholar] [CrossRef]
- Farnsworth, J.K. Is and ought: Descriptive and prescriptive cognitions in military-related moral injury. J. Trauma. Stress 2019, 32, 373–381. [Google Scholar] [CrossRef] [PubMed]
- Drescher, K.D.; Currier, J.M.; Nieuwsma, J.A.; McCormick, W.; Carroll, T.D.; Sims, B.M.; Cauterucio, C. A qualitative examination of VA chaplains’ understandings and interventions related to moral injury in military veterans. J. Relig. Health 2018, 57, 2444–2460. [Google Scholar] [CrossRef]
- van Veelen, N.; Jones, C.; Nijdam, M.; Bremault-Phillips, S.; Vermetten, E. Divergent thinking as a working model for 3MDR in posttraumatic stress disorder. 2022; unpublished manuscript. [Google Scholar]
- Jones, C.; Smith-MacDonald, L.; Miguel-Cruz, A.; Pike, A.; van Gelderen, M.; Lentz, L.; Shiu, M.Y.; Tang, E.; Sawalha, J.; Greenshaw, A.; et al. Virtual Reality-Based treatment for military members and veterans with combat-related Posttraumatic Stress Disorder: Protocol for a multimodular motion-assisted memory desensitization and reconsolidation randomized control trial. JMIR Res. Protoc. 2020, 9, e20620. [Google Scholar] [CrossRef] [PubMed]
- Koenig, H.; Ames, D.; Youssef, N.; Oliver, J.P.; Volk, F.; Teng, E.J.; Haynes, K.; Erickson, Z.D.; Arnold, I.; O’Garo, K.; et al. Screening for Moral Injury: The Moral Injury Symptom Scale—Military Version Short Form. Mil. Med. 2018, 183, e659–e665. [Google Scholar] [CrossRef]
- Blake, D.D.; Weathers, F.W.; Nagy, L.M.; Kaloupek, D.G.; Gusman, F.D.; Charney, D.S.; Keane, T.M. The development of a clinician-administered PTSD scale. J. Trauma. Stress 1995, 8, 75–90. [Google Scholar] [CrossRef]
- Renshaw, K.D.; Caska, C.M. Relationship Distress in Partners of Combat Veterans: The role of Partners’ Perceptions of Posttraumatic Stress Symptoms. Behav. Ther. 2012, 43, 416–426. [Google Scholar] [CrossRef]
- Kroenke, K.; Spintzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.; Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch Intern Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef] [PubMed]
- Lambert, M.J.; Hansen, N.B.; Umphress, V.; Lunnen, K.; Okiishi, J.; Burlingame, G.; Reisinger, C.W. Administration and Scoring Manual for the Outcome Questionnaire (OQ45.2); American Professional Credentialing Services: Wilmington, DE, USA, 1996. [Google Scholar]
- Birmes, P.; Brunet, A.; Carreras, D.; Ducasse, J.L.; Charlet, J.P.; Lauque, D.; Sztulman, H.; Schmitt, L. The predictive power of peritraumatic dissociation and acute stress symptoms for posttraumatic stress symptoms: A three-month prospective study. Am. J. Psychiatry 2003, 160, 1337–1339. [Google Scholar] [CrossRef]
- Connor, K.M.; Davidson, J.R.T. Development of a new resilience scale: The Connor-Davidson Resilience Scale (CD-RISC). Depress. Anxiety 2003, 18, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Bradley, K.A.; Bush, K.R.; Epler, A.J.; Dobie, D.J.; Davis, T.M.; Sporleder, J.L.; Maynard, C.; Burman, M.L.; Kivlahan, D.R. Two brief alcohol-screening tests From the Alcohol Use Disorders Identification Test (AUDIT): Validation in a female Veterans Affairs patient population. Arch. Intern. Med. 2003, 163, 821–829. [Google Scholar] [CrossRef]
- Victor, S.E.; Klonsky, E.D. Validation of a brief version of the Difficulties in Emotion Regulation Scale (DERS-18) in five samples. J. Psychopathol. Behav. Assess. 2016, 38, 582–589. [Google Scholar] [CrossRef]
- Gratz, K.; Roemer, L. Multidimensional Assessment of Emotion Regulation and Dysregulation: Development, Factor Structure, and Initial Validation of the Difficulties in Emotion Regulation Scale. J. Psychopathol. Behav. Assess. 2004, 26, 41–54. [Google Scholar] [CrossRef]
- Schoonenboom, J.; Johnson, R.B. How to Construct a Mixed Methods Research Design. Koln. Z. Soz. Sozpsychol. 2017, 69 (Suppl. 2), 107–131. [Google Scholar] [CrossRef] [PubMed]
- Benjamini, Y.; Hochberg, Y. Controlling the false discovery rate: A practical and powerful approach to multiple testing (PDF). J. R. Stat. Soc. Ser. B Methodol. 1995, 57, 289–300. [Google Scholar] [CrossRef]
- Braun, V.; Clark, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Koenig, H.G.; Youssef, N.A.; Pearce, M. Assessment of moral injury in veterans and active duty military personnel with PTSD: A review. Front. Psychiatry 2019, 10, 443. [Google Scholar] [CrossRef] [PubMed]
- Levi-Belz, Y.; Greene, T.; Zerach, G. Associations between moral injury, PTSD clusters, and depression among Israeli veterans: A network approach. Eur. J. Psychotraumatol. 2020, 11, 1736411. [Google Scholar] [CrossRef] [PubMed]
- Budden, A. The Role of Shame in Posttraumatic Stress Disorder: A Proposal for a Socio-Emotional Model for DSM-V. Soc. Sci. Med. 2009, 69, 1032–1039. [Google Scholar] [CrossRef] [PubMed]
- Dorahy, M.J. The Impact of Dissociation, Shame, and Guilt on Interpersonal Relationships in Chronically Traumatized Individuals: A Pilot Study. J. Trauma. Stress 2010, 23, 653–656. [Google Scholar] [CrossRef]
- Dorahy, M.J.; Hanna, D. Shame, Intimacy and Self-Definition: An Assessment of the Emotional Foundation and Intimate Relationship Consequences of an Introjective Personality Orientation. J. Nerv. Ment. Dis. 2012, 200, 699–704. [Google Scholar] [CrossRef]
- Chu, J.A. Rebuilding Shattered Lives: Treating Complex PTSD and Dissociative Disorders, 2nd ed.; John Wiley & Sons: Hoboken, NJ, USA, 2011. [Google Scholar]
- Dorahy, M.J.; Corry, M.; Shannon, M.; Webb, K.; McDermott, B.; Ryan, M.; Dyer, K.F.W. Complex Trauma and Intimate Relationships: The Impact of Shame, Guilt and Dissociation. J. Affect. Disord. 2013, 147, 72–79. [Google Scholar] [CrossRef]
- Raudales, A.M.; Preston, T.J.; Albanese, B.J.; Schmidt, N.B. Emotion Dysregulation as a Maintenance Factor for Posttraumatic Stress Symptoms: The Role of Anxiety Sensitivity. J. Clin. Psychol. 2020, 76, 2183–2197. [Google Scholar] [CrossRef] [PubMed]
- Spies, J.P.; Cwik, J.C.; Willmund, G.D.; Knaevelsrud, C.; Schumacher, S.; Niemeyer, H.; Engel, S. Associations between difficulties in emotion regulation and post-traumatic stress disorder in deployed service members of the German Armed Forces. Front. Psychiatry 2020, 11, 576553. [Google Scholar] [CrossRef] [PubMed]
- Roemer, L.; Litz, B.T.; Orsillo, S.M.; Wagner, A.W. A Preliminary Investigation of the Role of Strategic Withholding of Emotions in PTSD. J. Trauma. Stress 2001, 14, 149–156. [Google Scholar] [CrossRef]
- Smith-MacDonald, L.; Raffin-Bouchal, S.; Reay, G.; Ewashen, C.; Konnert, C.; Sinclair, S. Transitioning fractured identities: A grounded theory of veterans’ experiences of operational stress injuries. Traumatology 2020, 26, 235–245. [Google Scholar] [CrossRef]
- Williamson, V.; Murphy, D.; Stevelink, S.A.; Allen, S.; Jones, E.; Greenberg, N. The impact of trauma exposure and moral injury on UK military veterans: A qualitative study. Eur. J. Psychotraumatology 2020, 11, 1704554. [Google Scholar] [CrossRef] [PubMed]
- Protopopescu, A.; Boyd, J.E.; O’Connor, C.; Rhind, S.G.; Jetly, R.; Lanius, R.A.; McKinnon, M.C. Examining the Associations Among Moral Injury, Difficulties with Emotion Regulation, and Symptoms of PTSD, Depression, Anxiety, and Stress Among Canadian Military Members and Veterans: A Preliminary Study. J. Mil. Veteran Fam. Health 2021, 7, 71–80. [Google Scholar] [CrossRef]
- Kidwell, M.C.; Kerig, P.K. To Trust is to Survive: Toward a Developmental Model of Moral Injury. J. Child Adolesc. Trauma 2021, 1–17. [Google Scholar] [CrossRef]
- Brémault-Phillips, S.; Pike, A.; Scarcella, F.; Cherwick, T. Spirituality and Moral Injury Among Military Personnel: A Mini-Review. Front. Psychiatry 2019, 10, 276. [Google Scholar] [CrossRef]
- Kopacz, M.S.; Ames, D.; Koenig, H.G. Association Between Trust and Mental, Social, and Physical Health Outcomes in Veterans and Active Duty Service Members with Combat-Related PTSD Symptomatology. Front. Psychiatry 2018, 9, 408. [Google Scholar] [CrossRef] [PubMed]
- Chesnut, R.P.; Richardson, C.B.; Morgan, N.R.; Bleser, J.A.; Perkins, D.F.; Vogt, D.; Copeland, L.A.; Finley, E. Moral Injury and Social Well-Being: A Growth Curve Analysis. J. Trauma. Stress 2020, 33, 587–597. [Google Scholar] [CrossRef]
- Houtsma, C.; Khazem, L.R.; Green, B.A.; Anestis, M.D. Isolating Effects of Moral Injury and Low Post-Deployment Support Within the US Military. Psychiatry Res. 2017, 247, 194–199. [Google Scholar] [CrossRef]
- Koenig, H.G.; Ames, D.; Youssef, N.A.; Oliver, J.P.; Volk, F.; Teng, E.J.; Haynes, K.; Erickson, Z.D.; Arnold, I.; O’Garo, K.; et al. The Moral Injury Symptom Scale–Military Version. J. Relig. Health 2018, 57, 249–265. [Google Scholar] [CrossRef] [PubMed]
- Currier, J.M.; Farnsworth, J.K.; Drescher, K.D.; McDermott, R.C.; Sims, B.M.; Albright, D.L. Development and Evaluation of the Ex- pressions of Moral Injury Scale—Military Version. Clin. Psychol. Psychother. 2017, 25, 474–488. [Google Scholar] [CrossRef]
- McCormack, L.; Ell, L. Complex Psychosocial Distress Post- Deployment in Veterans: Reintegration Identity Disruption and Challenged Moral Integrity. Traumatology 2017, 23, 240–249. [Google Scholar] [CrossRef]
- Currier, J.M.; Holland, J.M.; Malott, J. Moral Injury, Meaning Making, and Mental Health in Returning Veterans. J. Clin. Psychol. 2015, 71, 229–240. [Google Scholar] [CrossRef]
- Bravo, A.J.; Kelley, M.L.; Mason, R.; Ehlke, S.J.; Vinci, C.; Redman, J.C. Rumination as a Mediator of the Associations Between Moral Injury and Mental Health Problems in Combat-Wounded Veterans. Traumatology 2020, 26, 52–60. [Google Scholar] [CrossRef] [PubMed]
- Boska, R.L.; Capron, D.W. Exploring the Maladaptive Cognitions of Moral Injury Within a Primarily Combat-Trauma Military Sample. Psychol. Trauma: Theory Res. Pract. Policy 2021, 13, 861–869. [Google Scholar] [CrossRef] [PubMed]
- Leung, A.K.; Kim, S.; Polman, E.; Ong, L.S.; Qiu, L.; Goncalo, J.A.; Sanchez-Burks, J. Embodied Metaphors and Creative “Acts”. Psychol. Sci. 2012, 23, 502–509. [Google Scholar] [CrossRef] [PubMed]
- Nieuwsma, J.A.; Walser, R.D.; Farnsworth, J.K.; Drescher, K.D.; Meador, K.G.; Nash, W.P. Possibilities Within Acceptance and Commitment Therapy for Approaching Moral Injury. Curr. Psychiatry Rev. 2015, 11, 193–206. [Google Scholar] [CrossRef]
- Currier, J.M.; McCormick, W.; Drescher, K.D. How do Morally Injurious Events Occur? A Qualitative Analysis of Perspectives of Veterans with PTSD. Traumatology 2015, 21, 106–116. [Google Scholar] [CrossRef]
- Kopacz, M.S.; Lockman, J.; Lusk, J.; Bryan, C.J.; Park, C.L.; Sheu, S.C.; Gibson, W.C. How Meaningful is Meaning-Making? New Ideas Psychol. 2019, 54, 76–81. [Google Scholar] [CrossRef]
- Litz, B.T.; Kerig, P.K. Conceptual challenges, methodological issues, and clinical applications. J. Trauma. Stress 2019, 32, 341–349. [Google Scholar] [CrossRef]
| Gender | Age | Marital Status | Employment Status | |
|---|---|---|---|---|
| Female: 1 (9%) Male: 10 (91%) | 30–39 years: 2 (18%) 40–49 years: 6 (55%) 50–54 years: 3 (27%) mean: 45.4 ± 6.8 years range: 30.9 to 54.3 years | Common-law: 2 (18%) Divorced: 1 (9%) Married: 5 (45%) Separated: 1 (9%) Single: 2 (18%) | No: 5 (45%) Yes: 6 (55%) | |
| Military Status | Enrollment Era | Rank | Element | Years of Service |
| Active: 3 (27%) Veteran: 8 (73%) | 1976–1990: 2 (18%) 1991–2000: 8 (73%) 2001–2015: 1 (9%) | Junior NCM: 6 (55%) Senior NCM: 4 (36%) Unknown: 1 (9%) | Air: 2 (18%) Land: 9 (82%) | 5–10 years: 2 (18%) 11–15 years: 1 (9%) 20+ years: 8 (73%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Smith-MacDonald, L.; Jones, C.; Brown, M.R.G.; Dunleavy, R.S.; VanderLaan, A.; Kaneva, Z.; Hamilton, T.; Burback, L.; Vermetten, E.; Brémault-Phillips, S. Moving Forward from Moral Injury: A Mixed Methods Study Investigating the Use of 3MDR for Treatment-Resistant PTSD. Int. J. Environ. Res. Public Health 2023, 20, 5415. https://doi.org/10.3390/ijerph20075415
Smith-MacDonald L, Jones C, Brown MRG, Dunleavy RS, VanderLaan A, Kaneva Z, Hamilton T, Burback L, Vermetten E, Brémault-Phillips S. Moving Forward from Moral Injury: A Mixed Methods Study Investigating the Use of 3MDR for Treatment-Resistant PTSD. International Journal of Environmental Research and Public Health. 2023; 20(7):5415. https://doi.org/10.3390/ijerph20075415
Chicago/Turabian StyleSmith-MacDonald, Lorraine, Chelsea Jones, Matthew R. G. Brown, Rachel S. Dunleavy, Annelies VanderLaan, Zornitsa Kaneva, Tristin Hamilton, Lisa Burback, Eric Vermetten, and Suzette Brémault-Phillips. 2023. "Moving Forward from Moral Injury: A Mixed Methods Study Investigating the Use of 3MDR for Treatment-Resistant PTSD" International Journal of Environmental Research and Public Health 20, no. 7: 5415. https://doi.org/10.3390/ijerph20075415
APA StyleSmith-MacDonald, L., Jones, C., Brown, M. R. G., Dunleavy, R. S., VanderLaan, A., Kaneva, Z., Hamilton, T., Burback, L., Vermetten, E., & Brémault-Phillips, S. (2023). Moving Forward from Moral Injury: A Mixed Methods Study Investigating the Use of 3MDR for Treatment-Resistant PTSD. International Journal of Environmental Research and Public Health, 20(7), 5415. https://doi.org/10.3390/ijerph20075415









