Development and Validity of an Intrapartum Self-Assessment Scale Aimed at Instilling Midwife-Led Care Competencies Used at Freestanding Midwifery Units
Abstract
1. Introduction
2. Materials and Methods
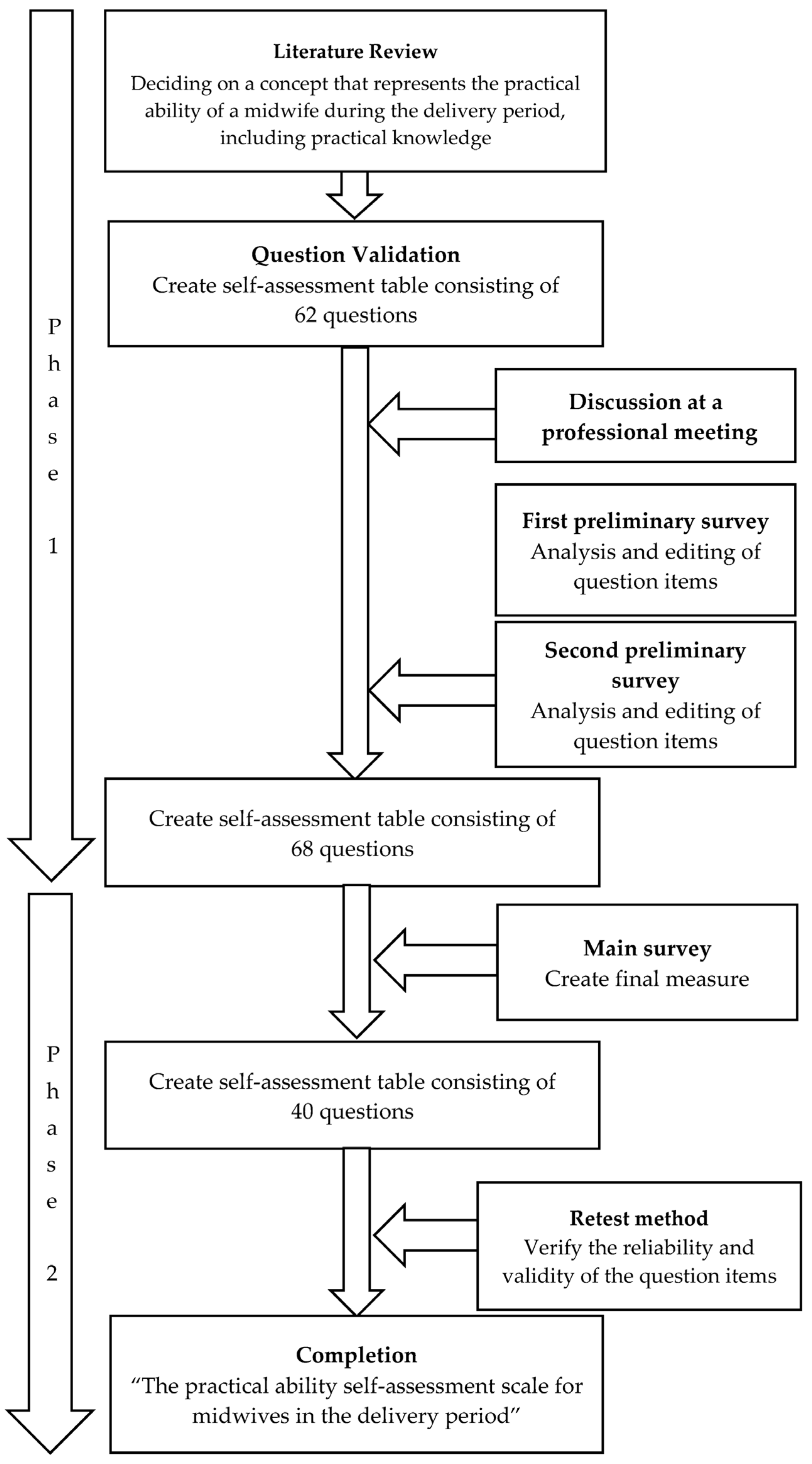
2.1. Phase 1: Item Development and Questionnaire Drafting
2.2. Phase 2: Evaluation of the Scale’s Validity and Reproducibility
2.2.1. Survey
2.2.2. Survey Validity and Stability Confirmation (Statistical Analysis)
Item Analysis
Compositional Concept Validity
Internal Consistency
Stability
Criterion-Related Validity
Ethics
3. Results
3.1. Phase 1: Item Development and Questionnaire Drafting
3.1.1. Literature Review and Question Validation
3.1.2. Discussion at a Professional Meeting
3.1.3. First Preliminary Survey
3.1.4. Second Preliminary Survey
3.2. Phase 2: Evaluation of Tool’s Validity and Reproducibility
3.2.1. Survey Participants
3.2.2. Confirmation of Survey Validity and Reproducibility
Item Analysis
Compositional Concept Validity
Internal Consistency
Stability
Criterion-Related Validity
Completion of the Self-Assessment Scale for Midwives’ Practice
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Voon, S.T.; Lay, J.T.S.; San, W.T.W.; Shorey, S.; Lim, S.K.S. Comparison of midwife-led care and obstetrician-led care on maternal and neonatal outcomes in Singapore: A retrospective cohort study. Midwifery 2017, 53, 53–71. [Google Scholar] [CrossRef]
- Hailemeskel, S.; Alemu, K.; Christensson, K.; Tesfahum, F.; Lindgren, H. Midwife-led continuity of care increases women’s satisfaction with antenatal, intrapartum, and postpartum care: North Shoa, Amhara regional, Ethiopia: A quasi-experimental study. Women Birth 2022, 35, 553–562. [Google Scholar] [CrossRef] [PubMed]
- Forster, D.A.; McLachlan, H.L.; Davey, M.A.; Biro, M.A.; Farrell, T.; Gold, L.; Flood, M.; Shafiei, T.; Waldenström, U. Continuity of care by a primary midwife (caseload midwifery) increases women’s satisfaction with antenatal, intrapartum and postpartum care: Results from the COSMOS randomized controlled trial. BMC Pregnancy Childbirth 2016, 3, 16–28. [Google Scholar] [CrossRef] [PubMed]
- Betrán, A.P.; Temmerman, M.; Kingdon, C.; Mohiddin, A.; Opiyo, N.; Torloni, M.R.; Zhang, J.; Musana, O.; Wanyonyi, S.Z.; Gülmezoglu, A.M.; et al. Interventions to reduce unnecessary caesarean sections in healthy women and babies. Lancet 2018, 392, 1358–1368. [Google Scholar] [CrossRef]
- Larsson, B.; Hildingsson, I.; Ternström, E.; Rubertsson, C.; Karlström, A. Women’s experience of midwife-led counselling and its influence on childbirth fear: A qualitative study. Women Birth 2019, 32, e88–e94. [Google Scholar] [CrossRef] [PubMed]
- Vital Statistics of Japan. Births and Percentages by Place of Birth in Urban-Rural Areas and by Year. Available online: https://www.e-stat.go.jp/dbview?sid=0003411600 (accessed on 30 September 2022).
- Walsh, D.; Spiby, H.; Grigg, C.P.; Dodwell, M.; McCourt, C.; Culley, L.; Bishop, S.; Wilkinson, J.; Coleby, D.; Pacanowski, L.; et al. Mapping midwifery and obstetric units in England. Midwifery 2018, 56, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health, Labour and Welfare. The 16th Study Group on Review of Medical Plan, etc.—Toward a Mid-term Review of the Medical Plan for Perinatal Care/Pediatric Care. Available online: https://www.mhlw.go.jp/content/10800000/000571647.pdf (accessed on 30 September 2022).
- Ministry of Health, Labour and Welfare. Study Group on the Perinatal Medical System: Compilation of Opinions. Available online: https://www.mhlw.go.jp/file/05-Shingikai-10801000-Iseikyoku-Soumuka/0000145749.pdf (accessed on 30 September 2022).
- Bäck, L.; Hildingsson, I.; Sjöqvist, C.; Karlström, A. Developing competence and confidence in midwifery-focus groups with Swedish midwives. Women Birth 2012, 30, e32–e38. [Google Scholar] [CrossRef] [PubMed]
- Hunter, M.; Smythe, E.; Spence, D. Confidence: Fundamental to midwives providing labour care in freestanding midwifery-led units. Midwifery 2018, 66, 176–181. [Google Scholar] [CrossRef]
- Grigg, C.P.; Tracy, S.K.; Tracy, M.; Daellenbach, R.; Kensington, M.; Monk, A.; Schmied, V. Evaluating maternity units: A prospective cohort study of freestanding midwife-led primary maternity units in New Zealand-clinical outcomes. BMJ Open 2017, 7, e016288. [Google Scholar] [CrossRef]
- McFarlamd, A.K.; Jones, J.; Luchsinger, J.; Kissler, K.; Smith, D.C. The experiences of midwives in integrated maternity care: A qualitative metasynthesis. Midwifery 2020, 80, 102544. [Google Scholar]
- Japanese Midwives Association. List of Midwifery Centers in Japan. Available online: https://www.midwife.or.jp/general/birthcenter_list.html (accessed on 7 January 2023).
- Ministry of Health, Labour and Welfare. Guidelines for Establishing a System for Perinatal Care. Available online: https://www.mhlw.go.jp/file/06-Seisakujouhou-10800000-Iseikyoku/4_2.pdf (accessed on 7 January 2023).
- Lyons, J. Reflective education for professional practice: Discovering knowledge from experience. Nurse Educ. Today 1999, 19, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Nicol, J.S.; Dosser, I. Understanding reflective practice. Nurs. Stand. 2016, 30, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Berg, M. A midwifery model of care for childbearing women at high risk: Genuine caring in caring for the genuine. J. Perinat. Educ. 2005, 14, 9–21. [Google Scholar] [CrossRef] [PubMed]
- Leinweber, J.; Creedy, D.K.; Rowe, H.; Gamble, J. Assessing emotional aspects of midwives’ intrapartum care: Development of the emotional availability and responsiveness in intrapartum care scale. Midwifery 2019, 74, 84–90. [Google Scholar] [CrossRef] [PubMed]
- Bojö, A.K.F.S.; Hall-Lord, M.L.; Axelsson, O.; Udén, G.; Larsson, B.W. Midwifery care: Development of an instrument to measure quality based on the World Health Organization’s classification of care in normal birth. J. Clin. Nurs. 2004, 13, 75–83. [Google Scholar] [CrossRef] [PubMed]
- Masaoka, K. Decision-making by midwives in practice on stages of labor. J. Jpn. Acad. Midwifery 2003, 17, 6–14. (In Japanese) [Google Scholar] [CrossRef]
- Watanabe, J.; Emisu, F.; Katsuno, T. Characteristics of care made by expert midwives in first stage of labor. J. Jpn. Acad. Health Sci. 2010, 13, 21–30. (In Japanese) [Google Scholar]
- Masaoka, K.; Maruyama, T. Midwive’s focus in intrapartal care and the relationship between the difference in focus and experience. Hokkaido J. Matern. Health 2010, 39, 7–13. (In Japanese) [Google Scholar]
- Masaoka, K.; Maruyama, T. Midwives’ viewpoints on the connection between information and experience concerning intrapartal care. J. Jpn. Acad. Midwifery 2009, 23, 16–25. (In Japanese) [Google Scholar] [CrossRef]
- Ochiai, M.; Kano, N. The formation process and structure of practice-based knowledge in midwifery care during labor and delivery. Acta Sci. Val. Univ. Praefectvralis Ibarakinesis 2015, 20, 25–35. (In Japanese) [Google Scholar]
- Masaoka, K.; Maruyama, T. Narrative analysis to identify practice-based knowledge in labor and delivery care in midwifery. Jpn. J. Health Behav. Sci. 2011, 26, 158–168. (In Japanese) [Google Scholar]
- Japan Institute of Midwifery Evaluation. What Is an Advanced Midwife? Available online: https://www.josan-hyoka.org/advanced/advanced/ (accessed on 7 January 2023).
- Andrew, L.C.; Howard, B.L. A First Course in Factor Analysis, 2nd ed.; Psychology Press: New York, NY, USA, 2013. [Google Scholar]
- International Confederation of Midwives. Essential Competencies for Midwifery Practice. 2018 UPDATE. Available online: https://www.internationalmidwives.org/assets/files/general-files/2018/10/icm-competencies---english-document_final_oct-2018.pdf (accessed on 30 September 2022).
- Westergren, A.; Edin, K.; Walsh, D.; Christianson, M. Autonomous and dependent-The dichotomy of birth: A feminist analysis of birth plans in Sweden. Midwifery 2019, 68, 56–64. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, H.M. Role of verbal and non-verbal communication of health care providers in general satisfaction with birth care: A cross-sectional study in government health settings of Erbil City, Iraq. Reprod. Health 2020, 17, 35. [Google Scholar] [CrossRef] [PubMed]
- Larsson, B.W.; Bojö, A.K.S.; Starrin, B.; Larsson, G. Birthgiving women’s feelings and perceptions of quality of intrapartal care: A nationwide Swedish cross-sectional study. J. Clin. Nurs. 2011, 20, 1168–1177. [Google Scholar] [CrossRef]
- Mazúchová, L.; Kelčíková, S.; Štofaníková, L.; Kopincová, J.; Malinovská, N.; Grendár, M. Satisfaction of Slovak women with psychosocial aspects of care during childbirth. Midwifery 2020, 86, 102711. [Google Scholar] [CrossRef]
- Nieuwenhuijze, M.J.; Korstjens, I.; Jonge, A.D.; Vries, R.D.; Janssen, A.L. On speaking terms: A Delphi study on shared decision-making in maternity care. BMC Pregnancy Childbirth 2014, 14, 223. [Google Scholar] [CrossRef]
- Urbutė, A.; Paulionytė, M.; Jonauskaitė, D.; Machtejevienė, E.; Nadišauskienė, R.J.; Dambrauskas, Ž.; Dobožinskas, P.; Kliučinskas, M. Perceived changes in knowledge and confidence of doctors and midwives after the completion of the Standardized Trainings in Obstetrical Emergencies. Medicina 2017, 53, 403–409. [Google Scholar] [CrossRef]
- Alhassan, A.; Fuseini, A.G.; Osman, W.; Adam, A.B. Knowledge and experience of neonatal resuscitation among midwives in Tamale. Nurs. Res. Pract. 2019, 2019, 3652608. [Google Scholar] [CrossRef]
- Renfrew, M.J.; McFadden, A.; Bastos, M.H.; Campbell, J.; Channon, A.A.; Cheung, N.F.; Silva, D.R.A.D.; Downe, S.; Kennedy, H.P.; Malata, A.; et al. Midwifery and quality care: Findings from a new evidence-informed framework for maternal and newborn care. Lancet 2014, 384, 1129–1145. [Google Scholar] [CrossRef]
- Grig, C.P.; Tracy, S.K.; Tracy, M.; Schmie, V.; Monk, A. Transfer from primary maternity unit to tertiary hospital in New Zealand-timing, frequency, reasons, urgency and outcomes: Part of the Evaluating Maternity Units study. Midwifery 2015, 31, 879–887. [Google Scholar] [CrossRef]
- Larkin, P.; Begley, C.M.; Devane, D. Women’s preferences for childbirth experiences in the Republic of Ireland; a mixed methods study. BMC Pregnancy Childbirth 2017, 17, 19. [Google Scholar] [CrossRef] [PubMed]
- Colley, S.; Kao, C.H.; Gau, M.; Cheng, S.F. Women’s perception of support and control during childbirth in The Gambia, a quantitative study on dignified facility-based intrapartum care. BMC Pregnancy Childbirth 2018, 18, 413. [Google Scholar] [CrossRef] [PubMed]
- Gepshtein, Y.; Horiuchi, S.; Eto, H. Independent Japanese midwives: A qualitative study of their practise and beliefs. Jpn. J. Nurs. Sci. 2007, 2, 85–93. [Google Scholar] [CrossRef]
- Tricas, J.G.; Giménez, M.R.B.; Tauste, A.P.; Sancho, S.L. Satisfaction with pregnancy and birth services: The quality of maternity care services as experienced by women. Midwifery 2011, 27, e231–e237. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, J.; Emisu, F. Clues to judgment made by expert midwives in assisting labor. J. Jpn. Acad. Midwifery 2010, 24, 53–64. (In Japanese) [Google Scholar] [CrossRef]
- Sigridur, H.; Sigfridur, I.K. The primacy of the good midwife in midwifery services: An evolving theory of professionalism in midwifery. Scand. J. Caring Sci. 2011, 25, 806–817. [Google Scholar]
- Martin, G.J.H.; Bull, P. What features of the maternity unit promote obedient behavior from midwives? Clin. Eff. Nurs. 2006, 952, e221–e231. [Google Scholar] [CrossRef]
| Characteristic | N (%) | |
|---|---|---|
| Age (years) | 20–29 | 112 (27.9) |
| 30–39 | 119 (29.7) | |
| 40–49 | 107 (26.7) | |
| 50–59 | 55 (13.7) | |
| ≥60 | 7 (1.7) | |
| No answer | 1 (0.2) | |
| Institution | Hospital | 331 (82.5) |
| Clinic | 50 (12.5) | |
| freestanding midwifery units | 12 (3.0) | |
| No answer | 8 (2.0) | |
| Experience in birthing assistance (years) | mean ± SD | 10.57 ± 9.81 |
| <5 | 118 (29.4) | |
| 5–10 | 119 (29.7) | |
| 11–20 | 118 (29.4) | |
| 21–30 | 40 (9.9) | |
| ≥31 | 6 (1.5) | |
| CLoCMiP level 3 certification | Advanced midwife | 184 (45.9) |
| Non-advanced midwife | 217 (54.1) |
| Item | Score (mean ± SD) Title 3 | Intra-Class Correlation Coefficient | ||
|---|---|---|---|---|
| 1st | 2nd | Correlation Coefficient | 95% Confidence Interval | |
| Factor I | 56.52 ± 8.80 | 55.52 ± 8.98 | 0.702 *** | 0.596–0.784 |
| Factor II | 33.33 ± 6.67 | 33.02 ± 6.33 | 0.789 *** | 0.708–0.749 |
| Factor III | 32.63 ± 6.12 | 32.39 ± 5.71 | 0.757 *** | 0.666–0.825 |
| Factor IV | 26.16 ± 4.49 | 25.71 ± 4.44 | 0.699 *** | 0.591–0.782 |
| Total score | 148.64 ± 23.68 | 146.64 ± 23.70 | 0.794 *** | 0.715–0.853 |
| Item | Midwives under 25% of Total Scale (n = 101) | Midwives over 75% of Total Scale (n = 115) | p |
|---|---|---|---|
| Total score | 110.15 ± 15.8 a | 169.82 ± 11.3 | <0.001 |
| Advanced midwife | 22 (21.8%) b | 78 (67.8%) | <0.001 |
| Experience in birthing assistance (years) | 6.10 ± 6.22 a | 14.36 ± 7.75 | <0.001 |
| Number of assisted births | 145.87 ± 212.60 a | 554.09 ± 638.50 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Inoue, N.; Nakao, Y.; Yoshidome, A. Development and Validity of an Intrapartum Self-Assessment Scale Aimed at Instilling Midwife-Led Care Competencies Used at Freestanding Midwifery Units. Int. J. Environ. Res. Public Health 2023, 20, 1859. https://doi.org/10.3390/ijerph20031859
Inoue N, Nakao Y, Yoshidome A. Development and Validity of an Intrapartum Self-Assessment Scale Aimed at Instilling Midwife-Led Care Competencies Used at Freestanding Midwifery Units. International Journal of Environmental Research and Public Health. 2023; 20(3):1859. https://doi.org/10.3390/ijerph20031859
Chicago/Turabian StyleInoue, Naomi, Yuko Nakao, and Atsuko Yoshidome. 2023. "Development and Validity of an Intrapartum Self-Assessment Scale Aimed at Instilling Midwife-Led Care Competencies Used at Freestanding Midwifery Units" International Journal of Environmental Research and Public Health 20, no. 3: 1859. https://doi.org/10.3390/ijerph20031859
APA StyleInoue, N., Nakao, Y., & Yoshidome, A. (2023). Development and Validity of an Intrapartum Self-Assessment Scale Aimed at Instilling Midwife-Led Care Competencies Used at Freestanding Midwifery Units. International Journal of Environmental Research and Public Health, 20(3), 1859. https://doi.org/10.3390/ijerph20031859





