Improving the Evidence-Based Practice Skills of Entry-Level Physiotherapy Students through Educational Interventions: A Scoping Review of Literature
Abstract
:1. Introduction
2. Materials and Methods
2.1. Protocol and Registration
2.2. Eligibility Criteria
- published in the English, French, German, or Italian language (as spoken by the authors) with full text;
- published in an internationally peer-reviewed journal that is indexed amongst the specified databases (PubMed and Eric);
- published within a timeframe between 11th of July 2012 and the 27th of March 2023;
- focused on educational interventions to increase EBP competence amongst physiotherapy students, as long as containing this set of two elements: entry-level physiotherapy students and EBP;
- quantitative and/or qualitative estimates of the effectiveness of the EBP educational approach on EBP-related competence, knowledge, attitudes, skills, and experiences were performed.
2.3. Search Strategy
- outlined key terms and Boolean operators to use;
- identified the electronic databases to conduct the search;
- identified the process for performing a systematic search;
- established the timeframe for the search;
- defined procedures for data extraction, processing, and interpretation.
- the articles identified through keywords from the databases were initially assessed for duplication, and the duplicates were removed;
- a screening based on titles and abstracts was conducted as an action to assess the eligibility criteria of the selected articles;
- a screening for eligibility criteria based on the full text of the remaining articles followed;
- the final list of remaining articles was included in the scoping review.
2.4. Study Selection and Data Extraction
- bibliographic information;
- study design;
- study population;
- educational intervention;
- duration of intervention;
- key findings and outcomes.
2.5. Synthesis of Results
3. Results
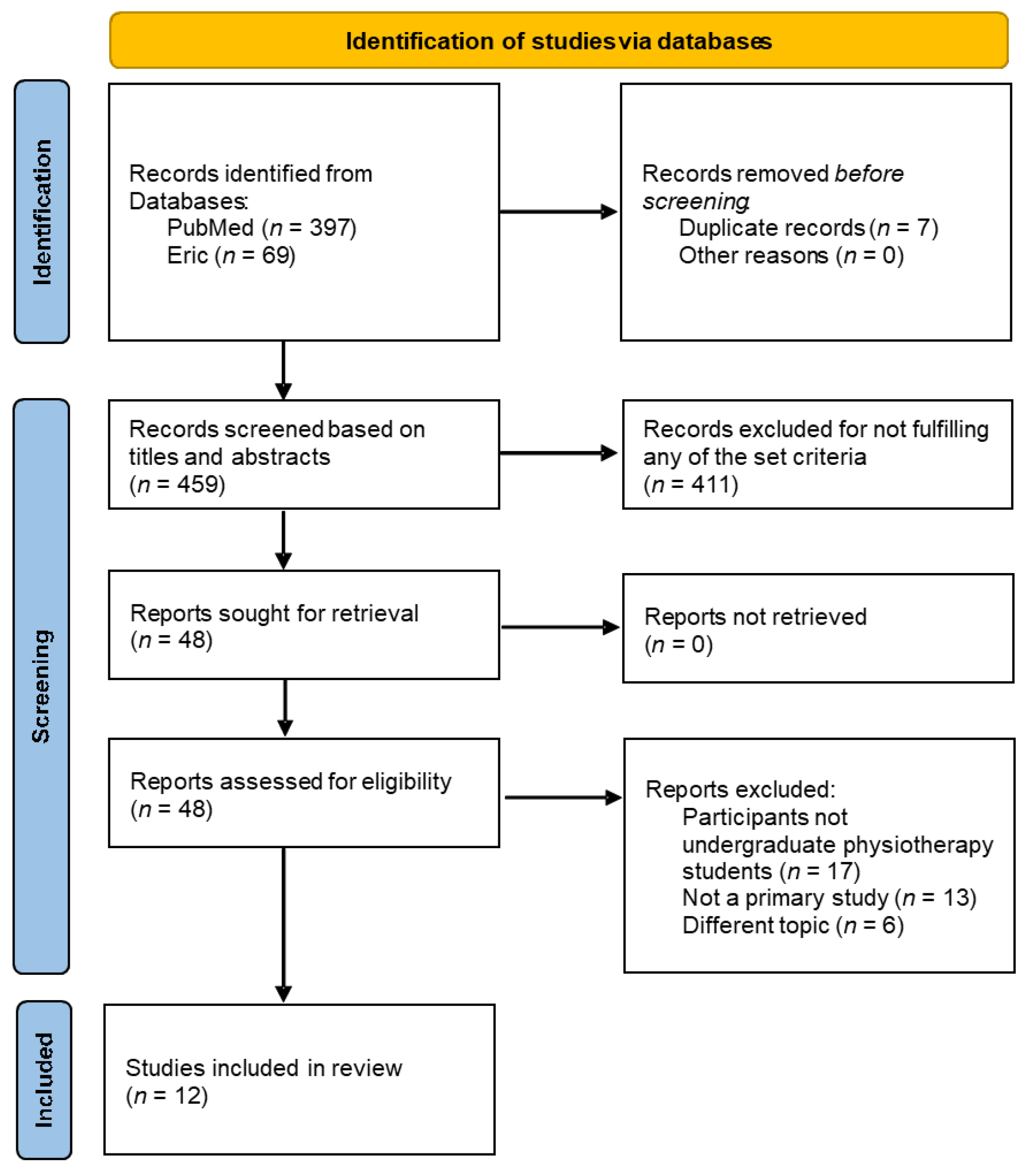
3.1. Study Selection
3.2. Effectiveness of Learning Methods (First Objective)
| Author(s), Year, Country | Aims | Participants | Intervention (Exposure) and Duration | Assessments | Key Findings |
|---|---|---|---|---|---|
| Arienti et al., 2021, Italy [12] | To evaluate the effectiveness of evidence-based practice (EBP) using Students 4 Best Evidence (S4BE) as an educational tool. To teach EBP competencies to undergraduate physiotherapy (PT) students. | The sample included 121 students completing a bachelor’s degree in PT at an Italian university. | Using S4BE platform as digital problem-based learning (DPBL) for EBP. Included were 24 educational training hours using S4BE blog, carried out over a 5-month period, with a total of 6 sessions, each 4 h in length. The first 5 sessions completed in first 3 months—last session completed after 2 months of clinical training. | All students completed an evidence-based practice questionnaire (EBPQ2), a validated tool for the evaluation of EBP competencies at the beginning of the laboratory (T0) and at the end (T1). | The students showed a significant improvement in all domains (p < 0.001), except in the sympathy domain, where the percentage score decreased from 71% to 60%. The best improvements were reached in the domains of terminology (54% to 65%) and in practice (41% to 55%). |
| Nair et al., 2021, India [10] | To identify perceived barriers to EBP among PT students. | A total of 182 final-year students, 112 interns, and 135 postgraduate students. | No intervention. | A total of 429 PT students participated in a survey where they self-reported barriers to EBP. The survey was a 12-item self-reported measure broadly divided into three domains: training-related barriers, organizational barriers, and personal barriers. | Most participants reported insufficient time, poor understanding of statistical analysis, and lack of research skills, formal training, and access to paid articles, along with poor ability to critically appraise articles, and bad infrastructure facilities as barriers towards practicing EBP. |
| Olsen et al., 2014, Norway [9] | To compare self-reported EBP behavior, abilities, and barriers during clinical placements reported by five cohorts of final-year PT students with different EBP exposure across the 3-year bachelor program. | PT total (n = 180) A cross-sectional study was conducted among five cohorts (2006–2010) with third year PT students at a university college in Norway. | No intervention. | Questionnaire with 42 items related to EBP behavior, ability, and barriers. The questionnaire contained three sections and took approximately 15 min to complete. Section 1 addressed background data such as sex, age, and access to internet. Section 2 and Section 3 consisted of items related to use of EBP during clinical placement. | Association between EBP exposure and students’ self-reported EBP behavior, abilities, and barriers was low for most items in the questionnaire. Correlations found for 8 items, related to information need, question formulation, use of checklists, searching, and ability to search for and critically appraise research evidence (strongest between EBP exposure level and ability to critically appraise research evidence (r = 0.41, p < 0.001). |
| Schweikhard et al. 2018, USA [11] | To measure how online library instructional tutorials implemented into an evidence-based practice course have impacted the information literacy skills of occupational therapy (OT) and physiotherapy graduate students. | PT and OT graduate students, total n = 180 following the EBP course during the period from 2012–2016. | Throughout the course occurrence (8 weeks in total), specifically designed online tutorials were introduced to PT and OT students as supplementary information to certain lecture topics. | A rubric was created to measure information literacy (IL) skills demonstrated in the students’ Step 5 Papers. The rubric scored components of strategies used in students’ searches and the three studies cited as the best evidence available for answering their clinical questions. | The rubric assessment of student Step 5 Papers reveals a statistically significant increase in student scores in their use of search terms and MeSH/subject headings (p = 0.00005), their use of limits (p = 0.03), and their citation of higher-level studies (p = 0.03). |
| Kloda et al., 2020, Canada [13] | To determine if a new, alternative clinical question framework was equally or more effective than patient, intervention, comparison, outcome (PICO) for improving students’ search skills, search results, and self-efficacy. | Completed both training and assessment: Control n = 34 Experimental n = 30 75 OT students and 76 PT students. These students were in either their final year of study toward their undergraduate degrees before a direct-entry master’s or in their qualifying year preceding the master’s degree program. | Randomized controlled trial (RCT) Two groups of PT and OT students assigned (control and experimental groups) each receiving 90 min of information literacy instruction from a librarian about formulating clinical questions and searching the literature using MEDLINE. Control group received instructions including the PICO question framework. Experimental group received instructions regarding the alternative framework (problem, intervention, population, outcome measure, time, context, professional stakeholder, and patient or family stakeholder). | At the outset of each instruction session, participants completed a demographic questionnaire and a short instrument measuring their information literacy self-efficacy (i.e., pre-test). This 12-item instrument was based on a longer, validated info-literacy self-efficacy instrument. Three weeks after the experimental and control groups received their instruction sessions, a data-gathering session was held for all participants. In this session, participants used the instrument for measuring their information literacy self-efficacy (i.e., post-test). | No differences in search performance or search skills (strategy and clinical question formulation) between groups. No differences in recall (p = 0.167), precision (p = 0.243), F-measure (p = 0.163), clinical question points (p = 0.653), search strategy (p = 0.676), identified concept questions (p = 0.178), or self-efficacy scores at pre-instruction (p = 0.941) or post-instruction (p = 0.772). Post-instruction self-efficacy scores were significantly higher than pre-instruction scores (t(63) = 2.627, p = 0.001). Alternative framework—as effective as PICO in teaching OT and PT students. |
3.3. Experiences of Learning Methods (Second Objective)
| Author(s), Year, Country | Aims | Participants | Intervention (Exposure) and Duration | Assessments | Key Findings |
|---|---|---|---|---|---|
| Johnson et al., 2021, Norway [15] | To explore health and social care students’ experiences of learning about evidence-based practice (EBP) using the mobile application EBPsteps during their clinical placements. | Undergraduate students: social education (SE) n = 132 occupational therapy (OT) n = 26 physiotherapy (PT) n = 66 | EBPsteps app, during one training period, no length in weeks | Four focus groups were conducted with a convenience sample of students from three undergraduate degree programs: occupational therapy, physical therapy, and social education. | The EBPsteps app was a relevant tool for learning EBP. Students need more knowledge and encouragement from clinical instructors to use EBPsteps app. The use of aps should be mandatory in the curriculum. |
| McMahon et al., 2016, Ireland [14] | To explore, using structured group feedback sessions (SGFS), final-year PT students’ perceptions of ability to work on a primary health care team upon graduation. | PT (n = 68) from four higher education institutions in Ireland participated. | EBP teaching in the curriculum. No specific intervention using EBP for the students who had primary health care experience. A four-year Bachelor of Science physiotherapy degree program | Group opinion obtained using structured 90 min group feedback sessions. | Final-year students felt that EBP teaching in the curriculum supported their learning and increased their confidence in their ability to take up employment in primary health care. |
| Olsen et al., 2013, Norway [16] | To explore beliefs, experiences, and attitudes related to third-year students’ use of EBP in clinical physiotherapy education among students, clinical instructors, and visiting teachers. | PT (n = 16) clinical instructors n = 9 visiting teachers n = 4 | One-year introduction to EBP, two-year advance teaching to EBP, and three-year obligatory studies Three-year bachelor program (180 ECTS-credits) | Six focus group interviews were conducted: three with sixteen students, two with nine clinical instructors, and one with four visiting teachers. In addition, one individual interview and one interview in a pair were conducted with clinical instructors. | In clinical practice, students attempt to apply EBP, but they saw themselves as novices. Students prioritize their practice experience over learning to use EBP in clinical patients’ situations. Students perceived a need for role models in EBP. |
| Author(s), Year, Country | Aims | Participants | Intervention (Exposure) and Duration | Assessments | Key Findings |
|---|---|---|---|---|---|
| Rotor et al., 2020, Philippines [17] | To determine influence of evidence-based practice (EBP) on knowledge, attitudes, and practice among physiotherapy (PT) graduates. To compare graduates’ EBP clinical practice profile to their EBP knowledge and attitudes. To explore graduates’ views on their own EBP education and how it influenced their clinical practice. | Five cohorts of PT graduates from a five-year entry-level BS program. Quantitative survey and qualitative open-ended questions (n = 77). Qualitative, focus groups (n = 8). | EBP activities embedded in the curriculum of the fourth and fifth year. | After graduation (2–7 years), participants were surveyed and interviewed, providing quantitative and qualitative data. | EBP activities: positive impact on students graduating with good knowledge, confidence, and positive EBP attitudes, not sufficient for graduates to overcome barriers hindering EBP uptake in their postgraduate clinical practice. Lack of physiotherapists’ autonomy in Philippines—the main barrier for EBP. |
| Lennon et al., 2019, Ireland [19] | To assess the influence of changes in early EBP instructional delivery from content-based learning to an interactive problem-based learning approach. | Two cohorts of PT students in a four-year entry-level Bachelor of Science program. | One EBP module in the second year, titled “Application of Physical Agents”. In the first cohort, the module was content-based; in the second cohort, it was problem-based. | Following both modules, students completed a standard university anonymized online survey providing both quantitative and qualitative data. Before and after the problem-based module, quantitative self-report evidence-based practice profile questionnaire (EBPPQ) data were collected. | Practice-based learning (PBL) approach: effective at promoting early EBP, improvements in EBP knowledge, confidence, and practice, preferred by students identifying with interactive, collaborative, and experiential nature of PBL, improved students’ understanding, achievement of outcomes, teaching, increased overall satisfaction. |
| McEvoy et al., 2018, Australia [6] | To investigate and integrate quantitative changes in EBP outcomes among PT students and qualitative students’ perceptions of factors impacting changes in selected EBP outcomes. | A single cohort of PT students in a four-year entry level BS-program. Quantitative pre-post (N = 56). Qualitative, focus groups (N = 21). | All participants completed three formal and multifaceted EBP courses in the first, second and fourth year. | Before and after EBP training, quantitative self-report data were collected on actual EBP knowledge. After EBP training, qualitative data were collected on students’ perceptions of EBP courses, current use of EBP, and role models during the PT program. | EBP training: improved EBP relevance, confidence, practice, improved knowledge of research evidence competencies (K-REC) actual knowledge. |
| Bozzolan et al., 2014, Italy [18] | To evaluate EBP knowledge and skills among PT students. To investigate EBP clinical behaviors of the students. Explore the students’ EBP perceptions and attitudes. | Three different cohorts of first- (n = 26), second- (n = 28), and third- (n = 19) year PT students, in a three-year entry-level Bachelor of Science program (n = 73). | An integrated educational curriculum on EBP (seven months) formed by three concurrent courses offered to three different groups: Formal EBP courses (first and second years). Internship EBP assignments (all three years) EBP journal club (second and third years). | Before and after EBP curriculum, quantitative data collection in all groups using A-Fresno Test for rehabilitation professionals with six additional questions from the A-Fresno test for PT. During and after EBP curriculum, qualitative data collected by inspecting internship documents for EBP clinical behaviors and with interviews on EBP perceptions and attitudes. | Combination of formal courses and internship assignments improved EBP knowledge/skills. EBP activities only during internship did not result in improvements. Students in focus groups valued EBP but perceived many barriers, described clinical teachers as obstacles or models, and highlighted the importance of being assigned to professionals willing or able to use EBP. |
3.4. Influence of EBP in Physiotherapy Education
4. Discussion
5. Conclusions
- EBP exerts a positive influence on entry-level physiotherapy education programs, regardless of how it is integrated into the curriculum;
- EBP enhances the quality of teaching and facilitates students’ gains in theoretical knowledge and practical skills;
- There exists a range of perceived barriers to the application of EBP, from intellectual aspects (such as a lack of critical thinking, scientific knowledge, and skills) to technical aspects (including equipment, prioritization, and time constraints).
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Sackett, D.L. Clinical epidemiology. Am. J. Epidemiol. 1969, 89, 125–128. [Google Scholar] [CrossRef]
- Kyriakoulis, K.; Patelarou, A.; Laliotis, A.; Wan, A.C.; Matalliotakis, M.; Tsiou, C.; Patelarou, E. Educational Strategies for Teaching Evidence-Based Practice to Undergraduate Health Students: Systematic Review. J. Educ. Eval. Health Prof. 2016, 13, 34. [Google Scholar] [CrossRef] [PubMed]
- Guyatt, G. Evidence-Based Medicine. JAMA 1992, 268, 2420. [Google Scholar] [CrossRef]
- Larsen, C.M.; Terkelsen, A.S.; Carlsen, A.-M.F.; Kristensen, H.K. Methods for Teaching Evidence-Based Practice: A Scoping Review. BMC Med. Educ. 2019, 19, 259. [Google Scholar] [CrossRef]
- Howard, B.; Diug, B.; Ilic, D. Methods of Teaching Evidence-Based Practice: A Systematic Review. BMC Med. Educ. 2022, 22, 742. [Google Scholar] [CrossRef] [PubMed]
- McEvoy, M.P.; Lewis, L.K.; Luker, J. Changes in Physiotherapy Students’ Knowledge and Perceptions of EBP from First Year to Graduation: A Mixed Methods Study. BMC Med. Educ. 2018, 18, 109. [Google Scholar] [CrossRef] [PubMed]
- Arksey, H.; O’Malley, L. Scoping Studies: Towards a Methodological Framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef]
- Olsen, N.R.; Lygren, H.; Espehaug, B.; Nortvedt, M.W.; Bradley, P.; Bjordal, J.M. Evidence-Based Practice Exposure and Physiotherapy Students’ Behaviour during Clinical Placements: A Survey. Physiother. Res. Int. 2014, 19, 238–247. [Google Scholar] [CrossRef]
- Nair, S.P.; Panhale, V.P.; Nair, N. Perceived Barriers to Evidence-Based Practice among Physiotherapy Students. J. Educ. Health Promot. 2021, 10, 17. [Google Scholar] [CrossRef]
- Schweikhard, A.J.; Hoberecht, T.; Peterson, A.; Randall, K. The Impact of Library Tutorials on the Information Literacy Skills of Occupational Therapy and Physical Therapy Students in an Evidence-Based Practice Course: A Rubric Assessment. Med. Ref. Serv. Q. 2018, 37, 43–59. [Google Scholar] [CrossRef]
- Arienti, C.; Lazzarini, S.G.; Pollet, J.; Negrini, S. Students 4 Best Evidence as a Digital Problem-Based Learning Method to Improve Evidence-Based Practice Competencies in Undergraduate Physiotherapy Students: An Observational Study. BMJ Evid. Based Med. 2021, 26, 251–252. [Google Scholar] [CrossRef]
- Kloda, L.A.; Boruff, J.T.; Cavalcante, A.S. A Comparison of Patient, Intervention, Comparison, Outcome (PICO) to a New, Alternative Clinical Question Framework for Search Skills, Search Results, and Self-Efficacy: A Randomized Controlled Trial. J. Med. Libr. Assoc. 2020, 108, 185–194. [Google Scholar] [CrossRef] [PubMed]
- McMahon, S.; O’Donoghue, G.; Doody, C.; O’Neill, G.; Barrett, T.; Cusack, T. Standing on the Precipice: Evaluating Final-Year Physiotherapy Students’ Perspectives of Their Curriculum as Preparation for Primary Health Care Practice. Physiother. Can. 2016, 68, 188–196. [Google Scholar] [CrossRef] [PubMed]
- Johnson, S.G.; Titlestad, K.B.; Larun, L.; Ciliska, D.; Olsen, N.R. Experiences with Using a Mobile Application for Learning Evidence-Based Practice in Health and Social Care Education: An Interpretive Descriptive Study. PLoS ONE 2021, 16, e0254272. [Google Scholar] [CrossRef] [PubMed]
- Olsen, N.R.; Bradley, P.; Lomborg, K.; Nortvedt, M.W. Evidence Based Practice in Clinical Physiotherapy Education: A Qualitative Interpretive Description. BMC Med. Educ. 2013, 13, 52. [Google Scholar] [CrossRef]
- Rotor, E.R.; Palad, Y.Y.; Cayco, C.S.; Perez, K.; Tiu, C.; Gorgon, E. Physical Therapists’ Evidence-Based Practice Profile and Perspectives of Entry-Level EBP Education: A Mixed Methods Study in the Philippines. Physiother. Theory Pract. 2022, 38, 1407–1418. [Google Scholar] [CrossRef]
- Bozzolan, M.; Simoni, G.; Balboni, M.; Fiorini, F.; Bombardi, S.; Bertin, N.; Da Roit, M. Undergraduate Physiotherapy Students’ Competencies, Attitudes and Perceptions after Integrated Educational Pathways in Evidence-Based Practice: A Mixed Methods Study. Physiother. Theory Pract. 2014, 30, 557–571. [Google Scholar] [CrossRef] [PubMed]
- Lennon, O.; Phelan, D.; Wallace, D.; King, J.; Barrett, T. “The More You Did, the More It Made Sense”: Problem-Based Learning to Improve Early Evidence-Based Practice in an Undergraduate Physiotherapy Professional Programme. Physiother. Res. Int. 2019, 24, e1774. [Google Scholar] [CrossRef] [PubMed]
- World Physiotherapy. Physiotherapist Education Framework; World Physiotherapy: London, UK, 2021. [Google Scholar]
- World Confederation for Physical Therapy. Policy Statement: Evidence-Based Practice; World Confederation for Physical Therapy: London, UK, 2019. [Google Scholar]
- Richardson, W.S.; Wilson, M.C.; Nishikawa, J.; Hayward, R.S. The Well-Built Clinical Question: A Key to Evidence-Based Decisions. ACP J. Club 1995, 123, A12–A13. [Google Scholar] [CrossRef] [PubMed]
- Andreae, M.O. Determination of Arsenic Species in Natural Waters. Anal. Chem. 1977, 49, 820–823. [Google Scholar] [CrossRef] [PubMed]
- Tateno, M.; Teo, A.R.; Ukai, W.; Kanazawa, J.; Katsuki, R.; Kubo, H.; Kato, T.A. Internet Addiction, Smartphone Addiction, and Hikikomori Trait in Japanese Young Adult: Social Isolation and Social Network. Front. Psychiatry 2019, 10, 455. [Google Scholar] [CrossRef] [PubMed]
- Collis, A.; Eggers, F. Effects of Restricting Social Media Usage on Wellbeing and Performance: A Randomized Control Trial among Students. PLoS ONE 2022, 17, e0272416. [Google Scholar] [CrossRef] [PubMed]
| Evidence-Based Practice (EBP) Influence | EBP Outcome |
|---|---|
| Positive | 9 |
| Negative | 0 |
| Barriers |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Boshnjaku, A.; Arnadottir, S.A.; Pallot, A.; Wagener, M.; Äijö, M. Improving the Evidence-Based Practice Skills of Entry-Level Physiotherapy Students through Educational Interventions: A Scoping Review of Literature. Int. J. Environ. Res. Public Health 2023, 20, 6605. https://doi.org/10.3390/ijerph20166605
Boshnjaku A, Arnadottir SA, Pallot A, Wagener M, Äijö M. Improving the Evidence-Based Practice Skills of Entry-Level Physiotherapy Students through Educational Interventions: A Scoping Review of Literature. International Journal of Environmental Research and Public Health. 2023; 20(16):6605. https://doi.org/10.3390/ijerph20166605
Chicago/Turabian StyleBoshnjaku, Arben, Solveig A. Arnadottir, Adrien Pallot, Marlies Wagener, and Marja Äijö. 2023. "Improving the Evidence-Based Practice Skills of Entry-Level Physiotherapy Students through Educational Interventions: A Scoping Review of Literature" International Journal of Environmental Research and Public Health 20, no. 16: 6605. https://doi.org/10.3390/ijerph20166605
APA StyleBoshnjaku, A., Arnadottir, S. A., Pallot, A., Wagener, M., & Äijö, M. (2023). Improving the Evidence-Based Practice Skills of Entry-Level Physiotherapy Students through Educational Interventions: A Scoping Review of Literature. International Journal of Environmental Research and Public Health, 20(16), 6605. https://doi.org/10.3390/ijerph20166605







