Clinical Characteristics and Rehabilitation Strategies for the Stomatognathic System Disturbances in Patients with Stroke: A Systematic Review
Abstract
1. Introduction
2. Methods
2.1. Registration and Protocol
2.2. Search Strategy
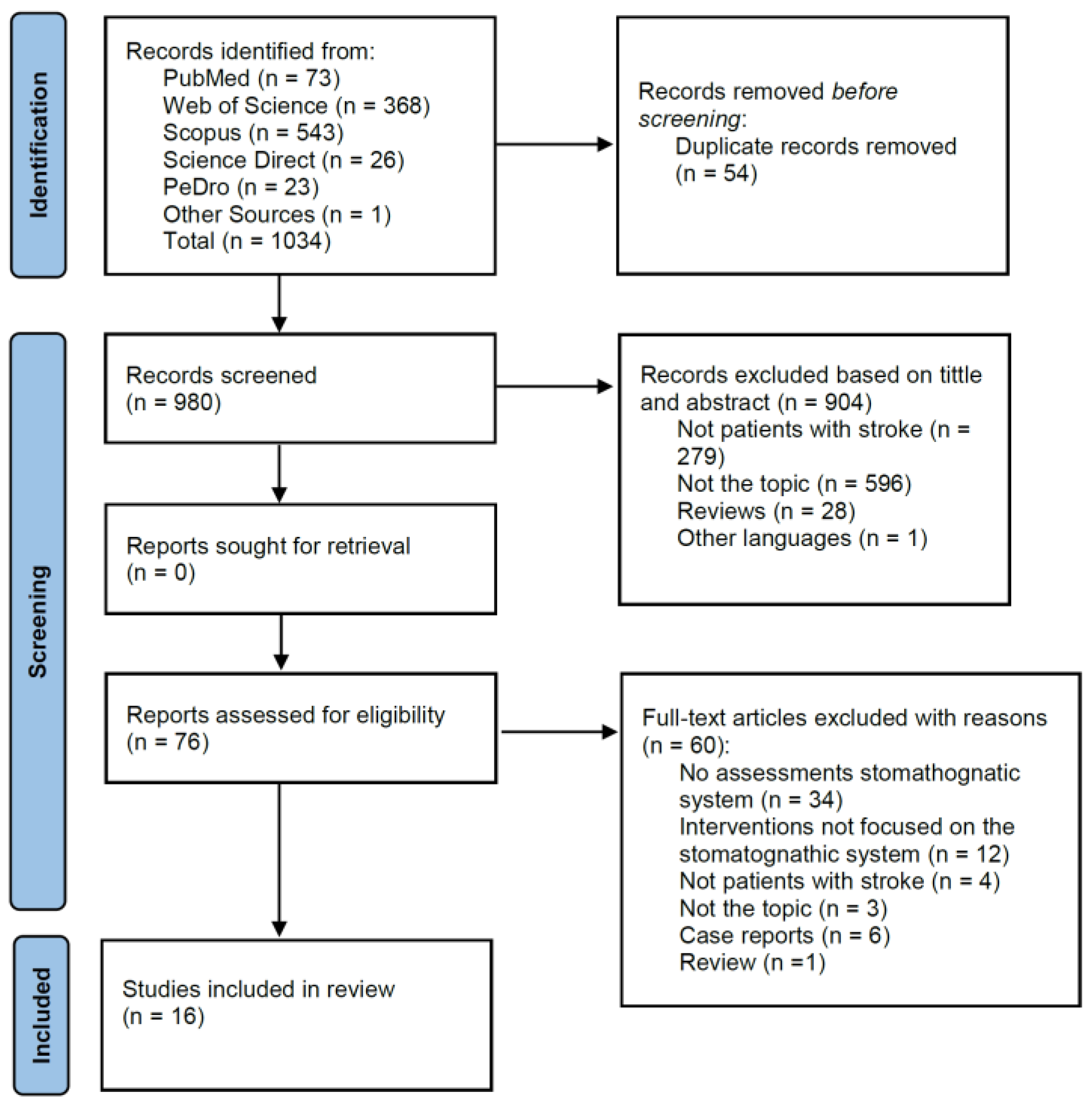
2.3. Selection Strategy
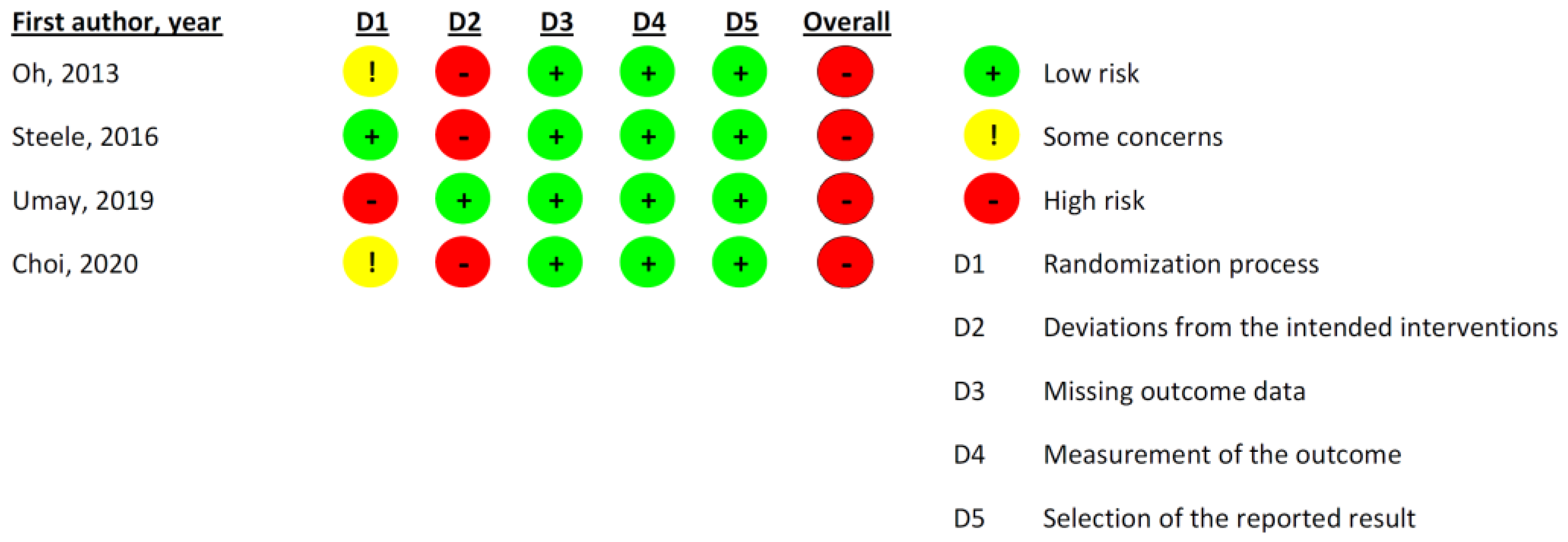
2.4. Study Quality Assessment
3. Results
3.1. Structural Changes in the Stomatognathic System in Patients with Stroke
3.2. Stomatognathic System Dysfunctions in Patients with Stroke
3.3. Rehabilitation Strategies for Stomatognathic System Disturbances
3.4. Methodological Quality
4. Discussions
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lozano, R.; Naghavi, M.; Foreman, K.; Lim, S.; Shibuya, K.; Aboyans, V.; Abraham, J.; Adair, T.; Aggarwal, R.; Ahn, S.Y.; et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2095–2128. [Google Scholar] [CrossRef]
- Gomes, G.G.C.; Palinkas, M.; da Silva, G.P.; Gonçalves, C.R.; Lopes, R.F.T.; Verri, E.D.; Fabrin, S.C.V.; Fioco, E.M.; Siéssere, S.; Regalo, S.C.H. Bite force, thickness, and thermographic patterns of masticatory muscles post-hemorrhagic stroke. J. Stroke Cerebrovasc. Dis. 2022, 31, 106173. [Google Scholar] [CrossRef] [PubMed]
- Schimmel, M.; Leemann, B.; Christou, P.; Schnider, A.; Mueller, F.; Kiliaridis, S. Masseter muscle thickness in hospitalised stroke patients. J. Oral Rehabil. 2010, 37, 726–730. [Google Scholar] [CrossRef]
- Yilmaz, V.; Aras, B.; Umay, E. Temporomandibular joint dysfunction and impaired stomatognathic alignment: A problem beyond swallowing in patients with stroke. Indian J. Otolaryngol. Head Neck Surg. 2020, 72, 329–334. [Google Scholar] [CrossRef]
- Zieliński, G.; Filipiak, Z.; Ginszt, M.; Matysik-Woźniak, A.; Rejdak, R.; Gawda, P. The organ of vision and the stomatognathic system—Review of association studies and evidence-based discussion. Brain Sci. 2022, 12, 14. [Google Scholar] [CrossRef]
- Cuccia, A.; Caradonna, C. The relationship between the stomatognathic system and body posture. Clinics 2009, 64, 61–66. [Google Scholar] [CrossRef]
- Dursun, Ö.; Çankaya, T. Assessment of temporomandibular joint dysfunction in patients with stroke. J. Stroke Cerebrovasc. Dis. 2018, 27, 2141–2146. [Google Scholar] [CrossRef]
- Hägg, M.; Tibbling, L. Effect of oral IQoro R and palatal plate training in post-stroke, four-quadrant facial dysfunction and dysphagia: A comparison study. Acta Otolaryngol. 2015, 135, 962–968. [Google Scholar] [CrossRef]
- Hegedűs, B. The potential role of thermography in determining the efficacy of stroke rehabilitation. J. Stroke Cerebrovasc. Dis. 2018, 27, 309–314. [Google Scholar] [CrossRef]
- Gedrange, T.; Kunert-keil, C.; Heinemann, F.; Dominiak, M. Tissue engineering and oral rehabilitation in the stomatognathic system. Biomed. Res. Int. 2017, 2017, 4519568. [Google Scholar] [CrossRef]
- Dai, R.; Lam, O.L.; Lo, E.C.; Li, L.S.; Wen, Y.; McGrath, C. Orofacial functional impairments among patients following stroke: A systematic review. Oral. Dis. 2015, 21, 836–849. [Google Scholar] [CrossRef]
- Umay, E.K.; Yilmaz, V.; Gundogdu, I.; Ozturk, E.; Gurcay, E.; Karaahmet, O.; Saylam, G.; Ceylan, T.; Cakci, A. What happens to swallowing muscles after stroke? A prospective randomized controlled electrophysiological study. Neurol. India 2019, 67, 1459–1466. [Google Scholar] [CrossRef]
- Oh, D.; Kang, T.; Kim, S. Effect of stomatognathic alignment exercise on temporomandibular joint function and swallowing function of stroke patients with limited mouth opening. J. Phys. Ther. Sci. 2013, 25, 1325–1329. [Google Scholar] [CrossRef][Green Version]
- Schimmel, M.; Ono, T.; Lam, O.L.T.; Müller, F. Oro-facial impairment in stroke patients. J. Oral. Rehabil. 2017, 44, 313–326. [Google Scholar] [CrossRef]
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A. PRISMA-P Group Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1. [Google Scholar] [CrossRef]
- Bordoni, B.; Varacallo, M. Anatomy, head and neck, temporomandibular joint. [Updated 2022 Jul 25]. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2022. Available online: https://www.ncbi.nlm.nih.gov/books/NBK538486/ (accessed on 25 December 2022).
- Hong, Q.N.; Pluye, P.; Fàbregues, S.; Bartlett, G.; Boardman, F.; Cargo, M. Mixed Methods Appraisal Tool (MMAT): User guide. McGill 2018, 1–11. [Google Scholar]
- Sterne, J.A.C.; Savović, J.; Page, M.J.; Elbers, R.G.; Blencowe, N.S.; Boutron, I.; Cates, C.J.; Cheng, H.Y.; Corbett, M.S.; Eldridge, S.M.; et al. RoB 2: A revised tool for assessing risk of bias in randomised trials. BMJ 2019, 366, l4898. [Google Scholar] [CrossRef]
- Kim, I.S.; Han, T.R. Influence of mastication and salivation on swallowing in stroke patients. Arch. Phys. Med. Rehabil. 2005, 86, 1986–1990. [Google Scholar] [CrossRef]
- Schimmel, M.; Leemann, B.; Christou, P.; Kiliaridis, S.; Schnider, A.; Herrmann, F.R.; Müller, F. Oral health-related quality of life in hospitalised stroke patients. Gerodontology 2011, 28, 3–11. [Google Scholar] [CrossRef]
- Kawasaka, T.; Shimodozono, M.; Ogata, A.; Tanaka, N.; Kawahira, K. Salivary secretion and occlusal force in patients with unilateral cerebral stroke. Int. J. Neurosci. 2010, 120, 355–360. [Google Scholar] [CrossRef]
- Schimmel, M.; Leemann, B.; Herrmann, F.R.; Kiliaridis, S.; Schnider, A.; Müller, F. Masticatory function and bite force in stroke patients. J. Dent. Res. 2011, 90, 230–234. [Google Scholar] [CrossRef]
- Schimmel, M.; Leemann, B.; Christou, P.; Kiliaridis, S.; Herrmann, F.R.; Müller, F. Quantitative assessment of facial muscle impairment in patients with hemispheric stroke. J Oral Rehabil. 2011, 38, 800–809. [Google Scholar] [CrossRef]
- Schimmel, M.; Leemann, B.; Schnider, A.; Herrmann, F.R.; Kiliaridis, S.; Müller, F. Changes in oro-facial function and hand-grip strength during a 2 -year observation period after stroke. Clin. Oral. Investig. 2013, 17, 867–876. [Google Scholar] [CrossRef]
- Steele, C.M.; Bayley, M.T.; Peladeau-Pigeon, M.; Nagy, A.; Namasivayam, A.M.; Stokely, S.L.; Wolkin, T. A randomized trial comparing two tongue-pressure resistance training protocols for post-stroke dysphagia. Dysphagia 2016, 31, 452–461. [Google Scholar] [CrossRef]
- Schimmel, M.; Voegeli, G.; Duvernay, E.; Leemann, B.; Müller, F.; Müller, F. Oral tactile sensitivity and masticatory performance are impaired in stroke patients. J. Oral. Rehabil. 2017, 44, 163–171. [Google Scholar] [CrossRef]
- Alvater Ramos, M.; Garcia Moura, B.; Costa de Araujo, C.; Tsunoda del Antonio, T.; Machado da Silva, J.K. Temporomandibular dysfunction in patients with a history of stroke. Man Ther. Posturology Rehabil. J. 2020, 17, 1–5. [Google Scholar]
- Choi, J.B.; Jung, Y.J.; Park, J. Comparison of 2 types of therapeutic exercise: Jaw opening exercise and head lift exercise for dysphagic stroke: A pilot study. Medicine 2020, 99, e22136. [Google Scholar] [CrossRef] [PubMed]
- Song, C.; Yu, Y.F.; Ding, W.L.; Yu, J.Y.; Song, L.; Feng, Y.N.; Zhang, Z.J. Quantification of the masseter muscle hardness of stroke patients using the MyotonPRO apparatus: Intra- and inter-rater reliability and its correlation with masticatory performance. Med. Sci. Monit. 2021, 27, e928109. [Google Scholar] [CrossRef]
- Axelsson, K.; Norberg, A.; Asplund, K. Eating after a stroke-towards an integrated view. Int. J. Nurs. Stud. 1984, 21, 93–99. [Google Scholar] [CrossRef]
- Westergren, A.; Karlsson, S.; Andersson, P.; Ohlsson, O.; Hallberg, I.R. Eating difficulties, need for assisted eating, nutritional status and pressure ulcers in patients admitted for stroke rehabilitation. J. Clin. Nurs. 2001, 10, 257–269. [Google Scholar] [CrossRef]
- Buescher, J.J. Temporomandibular joint disorders. Am. Fam. Physician 2007, 76, 1477–1482. [Google Scholar] [PubMed]
- Wright, A.J. An unusual but easily treatable cause of dysphagia and dysarthria. Br. Med. J. (Clin. Res. Ed.) 1985, 291, 1412–1413. [Google Scholar] [CrossRef][Green Version]
- Helkimo, E.; Carlsson, G.E.; Carmeli, Y. Bite force in patients with functional disturbances of the masticatory system. J. Oral. Rehabil. 1975, 2, 397–406. [Google Scholar] [CrossRef] [PubMed]
- Bianchini, E.M.G.; Paiva, G.; de Andrade, C.R.F. Mandibular movement patterns during speech in subjects with temporomandibular disorders and in asymptomatic individuals. Cranio 2008, 26, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Shaffer, S.M.; Brismée, J.M.; Sizer, P.S.; Courtney, C.A. Temporomandibular disorders. Part 2: Conservative management. J. Man Manip. Ther. 2014, 22, 13–23. [Google Scholar] [CrossRef] [PubMed]
- Durham, J.; Newton-John, T.R.O.; Zakrzewska, J.M. Temporomandibular disorders. BMJ 2015, 350, h1154. [Google Scholar] [CrossRef]
- Miles, T.S.; Nordstrom, M.A. Afferent and cortical control of human masticatory muscles. Adv. Exp. Med. Biol. 2002, 508, 443–449. [Google Scholar]
- Lindström, I.; Protto, S.; Khan, N.; Hernesniemi, J.; Sillanpää, N.; Oksala, N. Association of masseter area and radiodensity with three-month survival after proximal anterior circulation occlusion. J. Neurointerv. Surg. 2021, 13, 25–29. [Google Scholar] [CrossRef]
- Park, H.; Oh, D.; Yoon, T.; Park, J. Effect of effortful swallowing training on tongue strength and oropharyngeal swallowing function in stroke patients with dysphagia: A double-blind, randomized controlled trial. Int. J. Lang Commun. Disord. 2019, 54, 479–484. [Google Scholar] [CrossRef]
- Iwatsu, H.; Ikuta, Y.; Shinoda, K. Deep friction massage on the masticatory muscles in stroke patients increases biting force. J. Phys. Ther. Sci. 2001, 13, 17–20. [Google Scholar] [CrossRef]
- Bentsianov, B.; Blitzer, A. Facial anatomy. Clin. Dermatol. 2004, 22, 3–13. [Google Scholar] [CrossRef] [PubMed]
- Morecraft, R.J.; Stilwell-Morecraft, K.S.; Rossing, W.R. The motor cortex and facial expression: New insights from neuroscience. Neurologist 2004, 10, 235–249. [Google Scholar] [CrossRef] [PubMed]
- Müri, R.M. Cortical control of facial expression. J. Comp. Neurol. 2016, 524, 1578–1585. [Google Scholar] [CrossRef] [PubMed]
- English, C.; McLennan, H.; Thoirs, K.; Coates, A.; Bernhardt, J. Loss of skeletal muscle mass after stroke: A systematic review. Int. J. Stroke 2010, 5, 395–402. [Google Scholar] [CrossRef] [PubMed]
- Fabricius, J.; Kothari, S.F.; Kothari, M. Assessment and rehabilitation interventions for central palsy in patients with acquired brain injury: A systematic review. Brain. Inj. 2021, 35, 511–519. [Google Scholar] [CrossRef]
- Umay, E.; Gurcay, E.; Ozturk, E.A.; Akyuz, E.U. Is sensory-level electrical stimulation effective in cerebral palsy children with dysphagia? A randomized controlled clinical trial. Acta. Neurol. Belg. 2020, 120, 1097–1105. [Google Scholar] [CrossRef]
- Matsuo, K.; Palmer, J.B. Anatomy and physiology of feeding and swallowing: Normal and abnormal. Phys. Med. Rehabil. Clin. N. Am. 2008, 19, 691–707. [Google Scholar] [CrossRef]
- Steele, C.M.; Cichero, J.A. Physiological factors related to aspiration risk: A systematic review. Dysphagia 2014, 29, 295–304. [Google Scholar] [CrossRef]
- Daniels, S.K.; Brailey, K.; Foundas, A.L. Lingual discoordination and dysphagia following acute stroke: Analyses of lesion localization. Dysphagia 1999, 14, 85–92. [Google Scholar] [CrossRef]
- Svensson, P.; Romaniello, A.; Arendt-Nielsen, L.; Sessle, B.J. Plasticity in corticomotor control of the human tongue musculature induced by tongue-task training. Exp. Brain Res. 2003, 152, 42–51. [Google Scholar] [CrossRef]
- Hori, K.; Ono, T.; Iwata, H.; Nokubi, T.; Kumakura, I. Tongue pressure against hard palate during swallowing in post-stroke patients. Gerodontology 2005, 22, 227–233. [Google Scholar] [CrossRef]
- Ertekin, C.; Aydogdu, I. Neurophysiology of swallowing. Clin. Neurophysiol. 2003, 114, 2226–2244. [Google Scholar] [CrossRef]
- Chiaramonte, R.; Vecchio, M. Dysarthria and stroke. The effectiveness of speech rehabilitation. A systematic review and meta-analysis of the studies. Eur. J. Phys. Rehabil. Med. 2021, 57, 24–43. [Google Scholar] [CrossRef]
- De Cock, E.; Oostra, K.; Bliki, L.; Volkaerts, A.S.; Hemelsoet, D.; De Herdt, V.; Batens, K. Dysarthria following acute ischemic stroke: Prospective evaluation of characteristics, type and severity. Int. J. Lang Commun. Disord. 2021, 56, 549–557. [Google Scholar] [CrossRef]
- Robertson, S. The efficacy of oro-facial and articulation exercises in dysarthria following stroke. Int. J. Lang Commun. Disord. 2001, 36, S292–S297. [Google Scholar] [CrossRef]
| First Author, Year, Reference | Inclusion Criteria | Exclusion Criteria | Sample (Total Sample, Number of Groups) | Mean Age (Per Group) ± SD (Total and Per Group) | Gender (% Women Per Group) | Time Since Stroke (Mean ± SD; Mean, Range) | Setting |
|---|---|---|---|---|---|---|---|
| kim, 2005 [19] |
|
| Total: n = 20 2 groups: EG (n = 10) CG (n = 10) | 64.6 y (50, 82) | EG: 50 CG: 50 | 9.8 w (2, 24 w) | Department of Rehabilitation Medicine, Clinical Research Institute, National University Hospital, Seoul, Korea |
| Kawasaka, 2010 [21] |
|
| Total: n = 60 2 groups: EG (n = 30) CG (n = 30) | EG = 61.4 ± 2.3 y CG = 63.4 ± 3.1 y | EG: 53.33 CG: 63.33 | 8.3 ± 2.1 mo | Kirishima Rehabilitation Center of Kagoshima, University Hospital, Japan |
| Schimmel, 2010 [3] |
|
| Total: n = 55 2 groups: EG (n = 31) CG (n = 24) | EG = 69.0 ± 12.7 y CG = 68.8 ± 10.8 y | EG: 41.9 CG: 45.8 | 42.3 ± 14.4 d (18, 85) | Division of Neuro-rehabilitation at the Department for Clinical Neurosciences of the University Hospitals of Geneva |
| Schimmel, 2011a [20] |
|
| Total: n = 55 2 groups: EG (n = 31) CG (n = 24) | EG = 69.0 ± 12.7 y CG = 68.8 ± 10.8 y | EG: 41.9 CG: 45.8 | 42.3 ± 14.4 d | Division of Neuro-rehabilitation at the Department for Clinical Neurosciences of the University Hospitals of Geneva |
| Schimmel, 2011b [22] |
|
| Total: n = 55 2 groups: EG (n = 31) CG (n = 24) | EG = 69.0 ± 12.7 y CG = 68.8 ± 10.8 y | EG: 41.9 CG: 45.8 | 42.3 ± 14.4 d | Division of Neurorehabilitation of the Department of Clinical Neurosciences of the University Hospitals of Geneva, Switzerland |
| Schimmel, 2011c [23] |
|
| Total: n = 49 2 groups: EG (n = 27) CG (n = 22) | EG = 68.7 ± 12.9 y CG = 69.0 ± 11.2 y | EG: 44.45 CG:45.45 | 43.8 ± 14.2 d | Division of Neurorehabilitation of the Department of Clinical Neurosciences of the University Hospitals of Geneva, Switzerland |
| Schimmel, 2013 [24] |
|
| Total: n = 20 2 groups: EG (n = 10) CG (n = 10) | EG: n = 64.1 ± 17.4 y CG: n = 64.4 ± 18.6 y | EG: 40 CG: 40 | >6 mo | Division of Neurorehabilitation of the Department of Clinical Neurosciences of the University Hospitals of Geneva, Switzerland |
| Oh, 2013 [13] |
|
| Total: n = 14 2 groups: EG (n = 7) CG (n = 7) | EG = 53.71 ± 12.46 y CG = 56.14 ± 12.31 y | EG: 28.57 CG: 28.57 | EG: 43.00 ± 27.90 mo CG: 13.57 ± 16.53 mo | Wonkwang University Hospital, Republic of Korea |
| Steele, 2016 [25] |
|
| Total: n = 14 2 groups: TPPT (n = 7) TPSAT (n = 7) | TPPT: 74.85 TPSAT: 67.14 | Male: 64.3 Female: 35.7 | 70 d (range 18–150) | Three stroke rehabilitation centers in Ontario, Canada |
| Schimmel, 2017 [26] |
|
| Total: n = 54 2 groups: EG (n = 27 CG (n = 27) | EG = 64.3 ± 14.1 y CG = 60.8 ± 14.3 y | EG: 70.37 CG: 62.96 | EG: 31.00 ± 54.00 d | Division of Neurorehabilitation of the Department of Clinical Neurosciences of the University Hospitals of Geneva, Switzerland |
| Dursun, 2018 [7] |
|
| Total: n = 100 2 groups: EG (n = 50) CG (n = 50) | EG = 62.16 ± 11.41 y CG = 59.7 ± 9.62 y | NR | NR | Bolu Izzet Baysal Physical Therapy and Rehabilitation Education and Research Hospital. Bolu and Düzce cities. |
| Altvater Ramos, 2019 [27] |
|
| n = 11 1 group | 55–70 y | NR | >3 mo | Physical therapy and rehabilitation center from Universidade Estadual do Norte do Paraná (UENP), Jacarezinho, Paraná |
| Umay, 2019 [12] |
|
| Total: n = 102 2 groups: EG (n = 51) CG (n = 51) | EG = 63.68 ± 9.13 y CG = 65.41 ± 8.47 y | EG: 41.2 CG: 35.3 | 20–60 d | Physical Medicine and Rehabilitation Clinic, Ankara Diskapi Yildirim Beyazit Education and Research Hospital, Ankara Turkey |
| Yilzman, 2020 [4] |
|
| n = 30 1 group | 68.73 ± 4.79 y | 26.7 | 8.00 ± 2.22 mo | Physical Medicine and Rehabilitation Clinic and Rehabilitation Center Hospital, Kastamonu, Turkey |
| Choi, 2020 [28] |
|
| Total: n = 21 2 groups: JOE group (n = 11) HLE group (n = 10) | JOE group: n = 63.47 ± 7.65 y HLE group: n = 61.24 ± 9.73 y | 57.14 | 1 to 5 m | Two hospitals in South Korea |
| Song, 2021 [29] |
|
| n = 20 1 group | 47.65 ± 9.16 y | 50 | <1 y | Luoyang Orthopaedic Hospital of Henan Province, China |
| First Author, Year, Reference | Design | Intervention/Control | Frequency (Min Per Sesion/Sessions Per w)/Intervention Duration (w) | Structures of the Stomatognathic System Assessed | Outcome Measures (Device, Tool) | Main Results |
|---|---|---|---|---|---|---|
| kim, 2005 [19] | Non-randomized study | Saliva, masticatory performance | Spitting and weight measure of salivary flow for 30 min. Total chew duration oral phase from the time of the test food. | Saliva flow rate was significantly lower in stroke patients. Stroke patients chewed for a longer time. | ||
| Kawasaka, 2010 [21] | Non-randomized study | Teeth | Modified cotton swab method for salivary secretion. Oclusal force. | Salivary secretion was reduced in cerebral stroke patients. Lower oclusal force in hemi-plegic side with normal denture. | ||
| Schimmel, 2010 [3] | Quantitative descriptive study | Masseter muscle | Masseter thickness. | In EG, the masseter muscle in the affected side was thinner than the non-affected side. | ||
| Schimmel, 2011a [20] | Non-randomized study | Masticatory efficiency, lip | Two color mixing test. Lip force. OHIP. | Significant difference in chewing efficiency between EG and CG. Maximum lip force was significantly lower in CG. OHRQoL was significantly reduced in stroke patients. | ||
| Schimmel, 2011b [22] | Non-randomized study | Teeth, lips | Two color-gum mixing-test. Maximum voluntary bit force. Lip force. Lip seal. | Masticatory efficiency and maximum lip force were significantly reduced in EG. Maximum bite force was not significantly different between both sides and between EG and EC. | ||
| Schimmel, 2011c [23] | Non-randomized study | Facial muscles (frontalis, lower facial and orbicularis oris muscles) | Quantitative assessment of facial muscle function. House–Brackmann scale. | Lower facial muscles were more affected than the upper ones, showing muscular weakness in the EG and reduced tonus of the affected orbicularis muscle. | ||
| Schimmel, 2013 [24] | Non-randomized study | Teeth, lips, masseter muscle | DMFT. Color-mixing ability test. Maximum restraining lip force. Maximum voluntary bite force. Masseter muscle thickness. | Chewing efficiency: significatly less efficient in stroke patients. Maximum restraining lip force: significantly lower in stroke patients. Maximum voluntary bite force: difference in the cortical control of the jaw closing muscles and those of the upper limb. Masseter muscle thickness: significant difference between contra- and ipsilesional sides, but not between stroke and control groups. | ||
| Oh, 2013 [13] | Randomized controlled trial | EG and CG: functional training in their routine rehabilitation EG group: stomatognathic alignment exercise, active ROM exercises for the neck and TMJ | 60/3/4 | Neck muscles, TMJ | Range of mouth opening. Neck mobility. CMI. MASA. | Significant changes on the opening, CMI, and MASA scores between the EG and CG. Neck mobility: EG showed significant differences between pre- and post-test values in all measures. |
| Steele, 2016 [25] | A randomized trial | TPSAT: strength targets and accuracy targets TPPT: real saliva swallows | -/2–3/8–12 | Tongue | Tongue strength: VFFS. | A significant treatment effect was found in both outcomes. No significant differences between both treatments. |
| Schimmel, 2017 [26] | Non-randomized study | Lips, tongue, cheeks | Maximum voluntary bite force. Maximum restraining lip force. TDT and 2PD. Color-mixing ability test. | Bite and lip force: no significant difference between both groups. Lower lip force in the stroke group. TDT and 2PD were significantly higher on the affected side in stroke patients. Significantly lower chewing efficiency in stroke patients. | ||
| Dursun, 2018 [7] | Non-randomized study | TMJ, masticatory muscles | TMJ ROM. Fonseca questionnaire. Facial asymmetry. PPT of masticatory muscles. | TMJ ROM loss, facial asymmetry, and TMJD were more prevalent in stroke patients. PPT: middle part of the left temporalis muscle was more sensitive to pressure pain in stroke. | ||
| Altvater Ramos, 2019 [27] | Quantitative descriptive study | TMJ, temporal, sternocleidomastoid, masseter, and upper trapezius | Mandibular movement. TMJ, facial, and neck muscle PPT ROM cervical region. | 81.8% of the patients presented signs and symptoms related to TMD and most of them had a diagnosis of reduced disc displacement. Significant difference in the TMJ and masseter muscle PPT. Cervical ROM: decreased amplitude. | ||
| Umay, 2019 [12] | A prospective randomized controlled study | Intermittent galvanic stimulation to masseter muscles and cognitive, sensorimotor and respiratory rehabilitation + Standard dysphagia rehabilitation | 60–90/5/4 | Tongue, masseter, and orbicularis muscles | Sweep speed and sensitivity of the tongue, masseter, and orbicularis muscles. Electrical activity of submental muscles. | Tongue, masseter, and orbicularis muscles: lower muscle action potential amplitudes. EG presented longer swallowing intervals compared to the healthy control group. Significant improvement in muscle dynamic activity. |
| Yilzman, 2020 [4] | Quantitative non-randomized study | Active and active assisted ROM exercises for neck and TMJ, chin tuck, breathing and relaxing, and postural exercises + stroke rehabilitation program | 5/10/4 | TMJ and neck muscles | CMI. Cervical mobility. | All parameters were significantly improved both in 1st and 6th month evaluation. |
| Choi, 2020 [28] | Open-label, parallel-group, comparative study randomized trial | JOE group: JOE exercises using a resistance bar + traditional dysphagia treatment HLE group: HLE exercises + traditional dysphagia treatment | 30/5/6 | Digastric and mylohyoid muscles Hyoid bone | Digastric and mylohyoid muscle thickness. Kinematic movement of the hyoid bone. | Both groups showed a statistically significant increase in the thickness of the digastric and mylohyoid muscles and on the anterior and superior movement of the hyoid bone. |
| Song, 2021 [29] | Non-randomized study | Masseter muscle, masticatory performance | Masseter muscle stiffness and hardness. Masticatory performance. | Masseter muscle hardness and masticatory performance were significantly greater on the unaffected side. A statistically negative moderate correlation between the masseter muscle stiffness of the affected side and the masticatory performance was found. |
| Quantitative randomized controlled trials | 2.1. Randomization appropriately performed? | 2.2. Groups comparable at baseline? | 2.3. Complete outcome data? | 2.4. Outcome assessors blinded to the intervention provided? | 2.5. Participants adhere to the assigned intervention? | % Total |
|---|---|---|---|---|---|---|
| Oh, 2013 [13] | Yes | No | Yes | Yes | No | 60% |
| Steele, 2016 [25] | Yes | Yes | No | Yes | Yes | 80% |
| Umay, 2019 [12] | No | Yes | Yes | Yes | Yes | 80% |
| Choi, 2020 [28] | Yes | Yes | No | No | No | 40% |
| Quantitative non-randomized | 3.1. Participants representative of the target population? | 3.2. Measurements appropriate regarding both the outcome and intervention (or exposure)? | 3.3. Complete outcome data? | 3.4. Confounders accounted for in the design and analysis? | 3.5. Intervention administered (or exposure occurred) as intended? | % Total |
| kim, 2005 [19] | Yes | Yes | Yes | Yes | Yes | 100% |
| Kawasaka, 2010 [21] | Yes | Yes | Yes | Yes | Yes | 100% |
| Schimmel, 2010 [3] | Yes | Yes | Yes | Yes | Yes | 100% |
| Schimmel, 2011a [20] | Yes | Yes | Yes | Yes | Yes | 100% |
| Schimmel, 2011b [22] | Yes | Yes | No | Yes | Yes | 80% |
| Schimmel, 2011c [23] | Yes | Yes | Yes | Yes | Yes | 100% |
| Schimmel, 2013 [24] | Yes | Yes | No | Yes | Yes | 80% |
| Schimmel, 2017 [26] | Yes | Yes | Yes | Yes | Yes | 100% |
| Dursun, 2018 [7] | Yes | Yes | Yes | Yes | Yes | 100% |
| Yilzman, 2020 [4] | Yes | Yes | Yes | Yes | Yes | 100% |
| Song, 2021 [29] | Yes | Yes | Yes | No | Yes | 80% |
| Quantitative descriptive | 4.1. Sampling strategy relevant to address the research question? | 4.2. Sample representative of the target population? | 4.3. Measurements appropriate? | 4.4. Risk of non-response bias low? | 4.5. Statistical analysis appropriate to answer the research question? | % Total |
| Altvater Ramos, 2019 [27] | No | No | Yes | Yes | Yes | 60% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zapata-Soria, M.; Cabrera-Martos, I.; López-López, L.; Ortiz-Rubio, A.; Granados-Santiago, M.; Ríos-Asín, I.; Valenza, M.C. Clinical Characteristics and Rehabilitation Strategies for the Stomatognathic System Disturbances in Patients with Stroke: A Systematic Review. Int. J. Environ. Res. Public Health 2023, 20, 657. https://doi.org/10.3390/ijerph20010657
Zapata-Soria M, Cabrera-Martos I, López-López L, Ortiz-Rubio A, Granados-Santiago M, Ríos-Asín I, Valenza MC. Clinical Characteristics and Rehabilitation Strategies for the Stomatognathic System Disturbances in Patients with Stroke: A Systematic Review. International Journal of Environmental Research and Public Health. 2023; 20(1):657. https://doi.org/10.3390/ijerph20010657
Chicago/Turabian StyleZapata-Soria, Mónica, Irene Cabrera-Martos, Laura López-López, Araceli Ortiz-Rubio, María Granados-Santiago, Izarbe Ríos-Asín, and Marie Carmen Valenza. 2023. "Clinical Characteristics and Rehabilitation Strategies for the Stomatognathic System Disturbances in Patients with Stroke: A Systematic Review" International Journal of Environmental Research and Public Health 20, no. 1: 657. https://doi.org/10.3390/ijerph20010657
APA StyleZapata-Soria, M., Cabrera-Martos, I., López-López, L., Ortiz-Rubio, A., Granados-Santiago, M., Ríos-Asín, I., & Valenza, M. C. (2023). Clinical Characteristics and Rehabilitation Strategies for the Stomatognathic System Disturbances in Patients with Stroke: A Systematic Review. International Journal of Environmental Research and Public Health, 20(1), 657. https://doi.org/10.3390/ijerph20010657