Effects of Corrective Exercises on Lumbar Lordotic Angle Correction: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Data Sources and Search Strategy
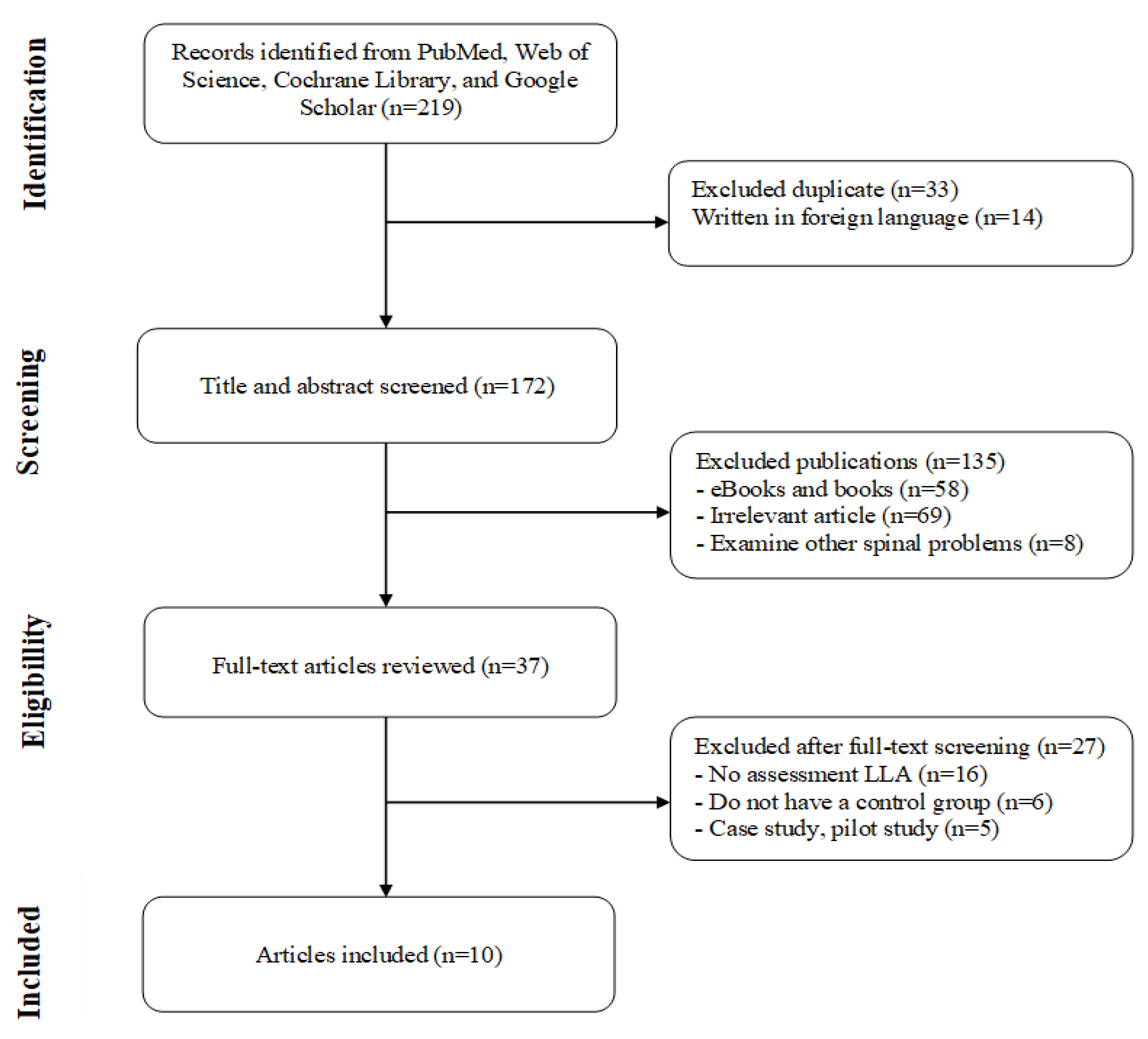
2.3. Study Selection
2.4. Data Extraction and Quality Assessment
2.5. Data Synthesis and Analysis
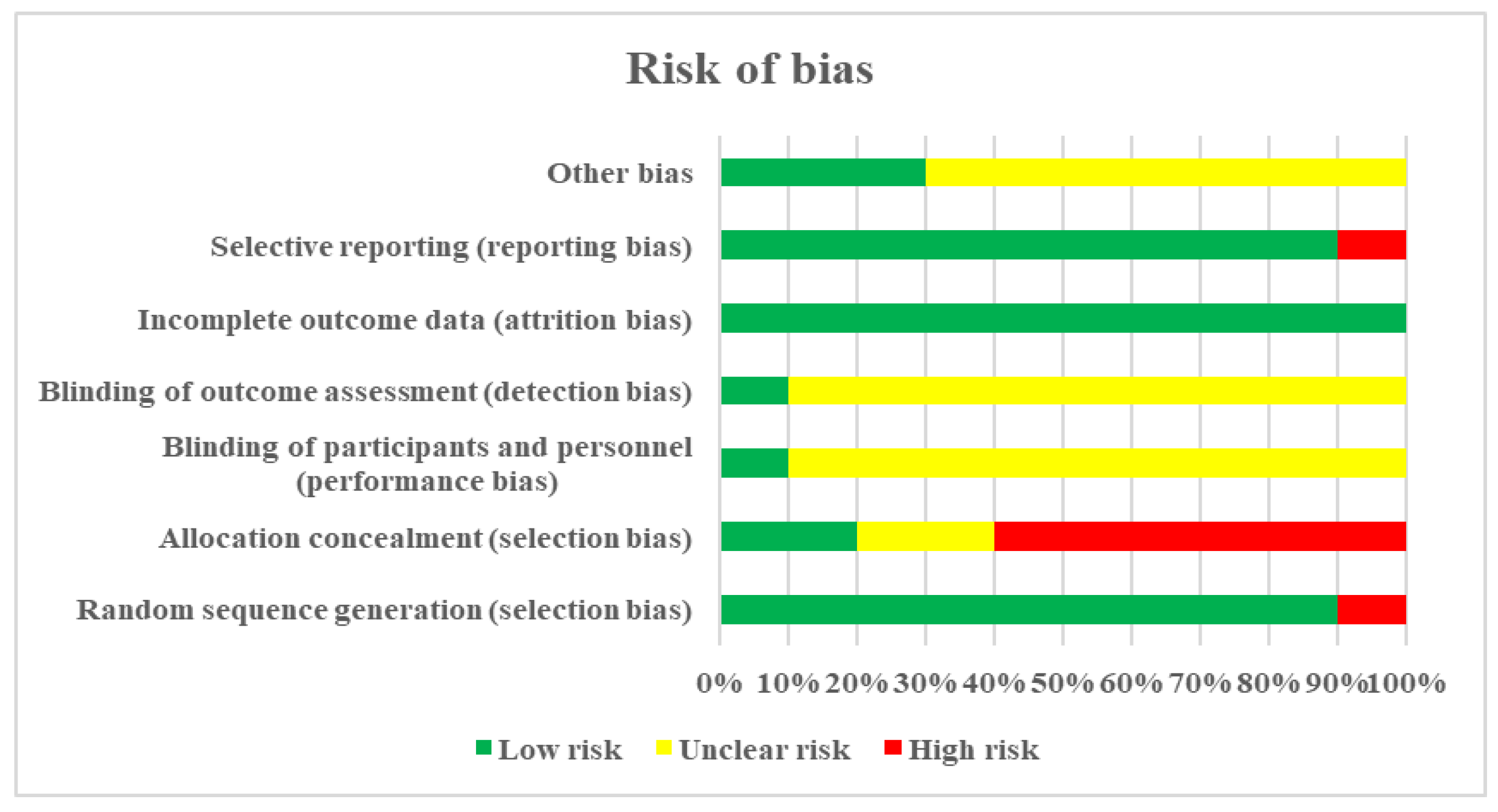
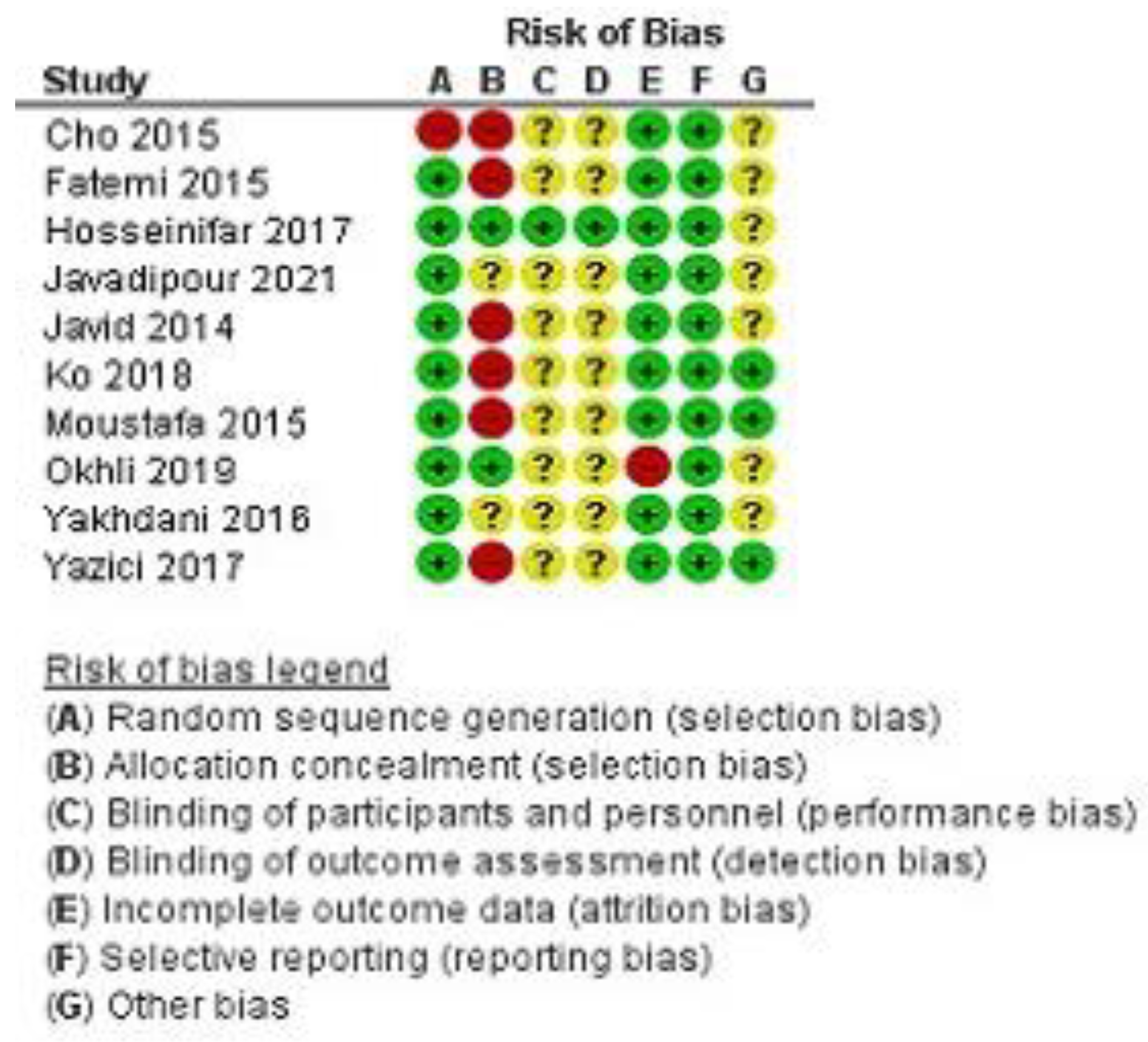
2.6. Medicine Risk of Bias
3. Results
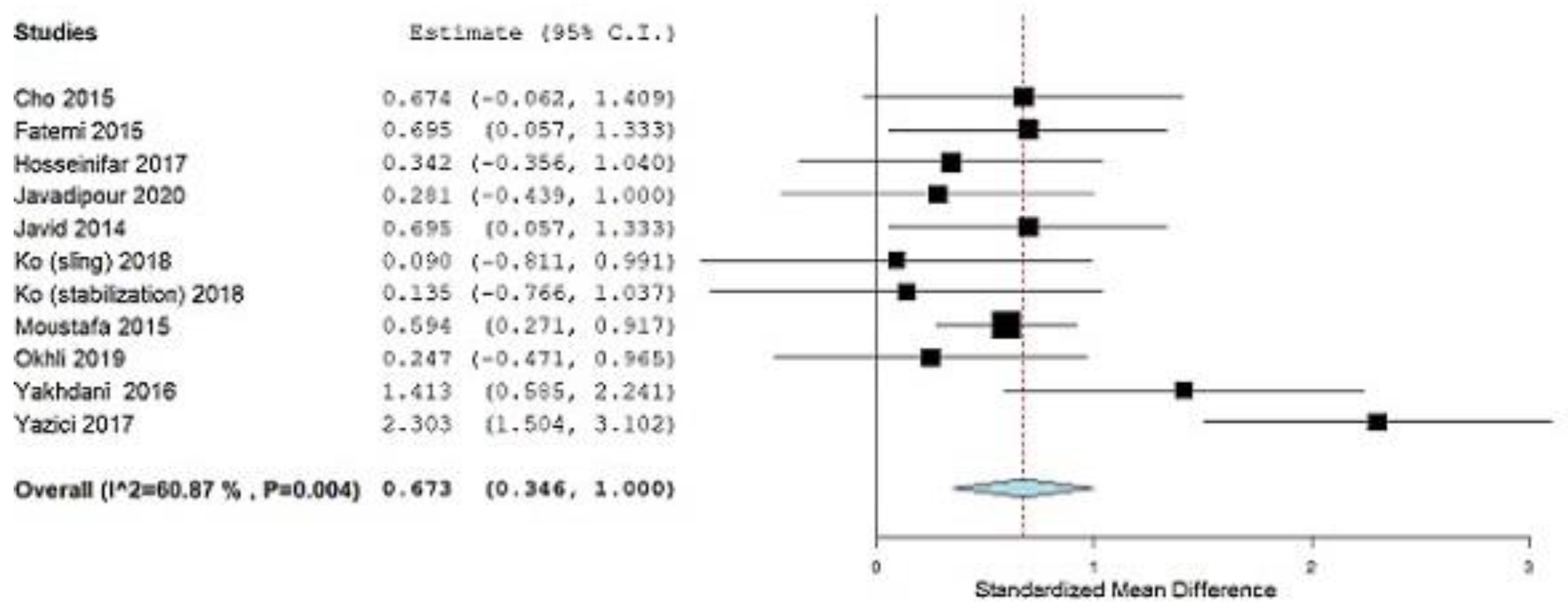
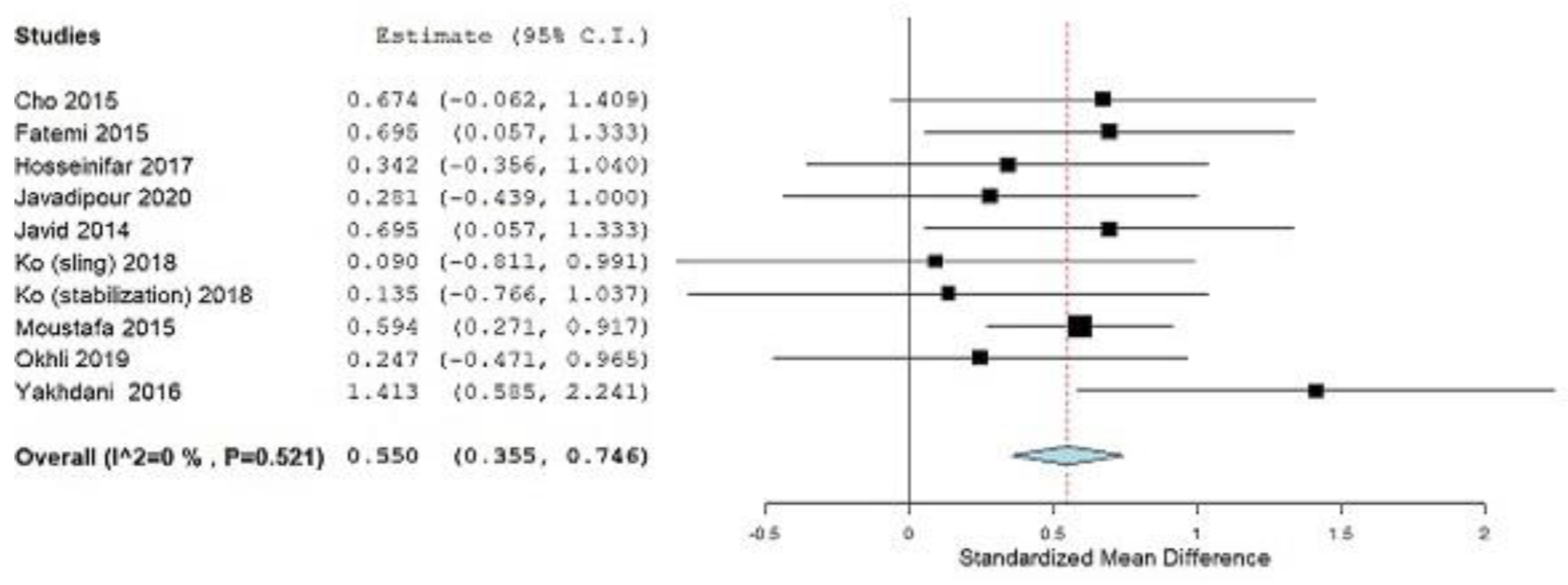
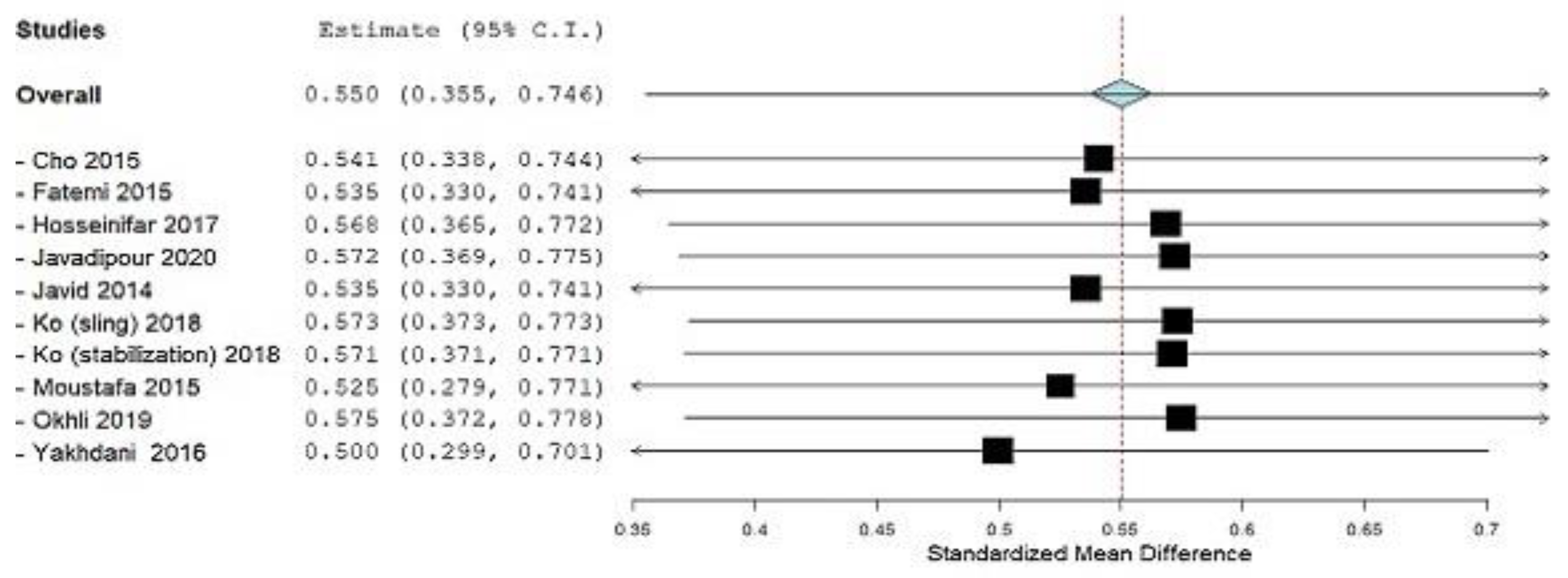
3.1. Meta-Analysis
3.1.1. Lumbar Lordotic Angle
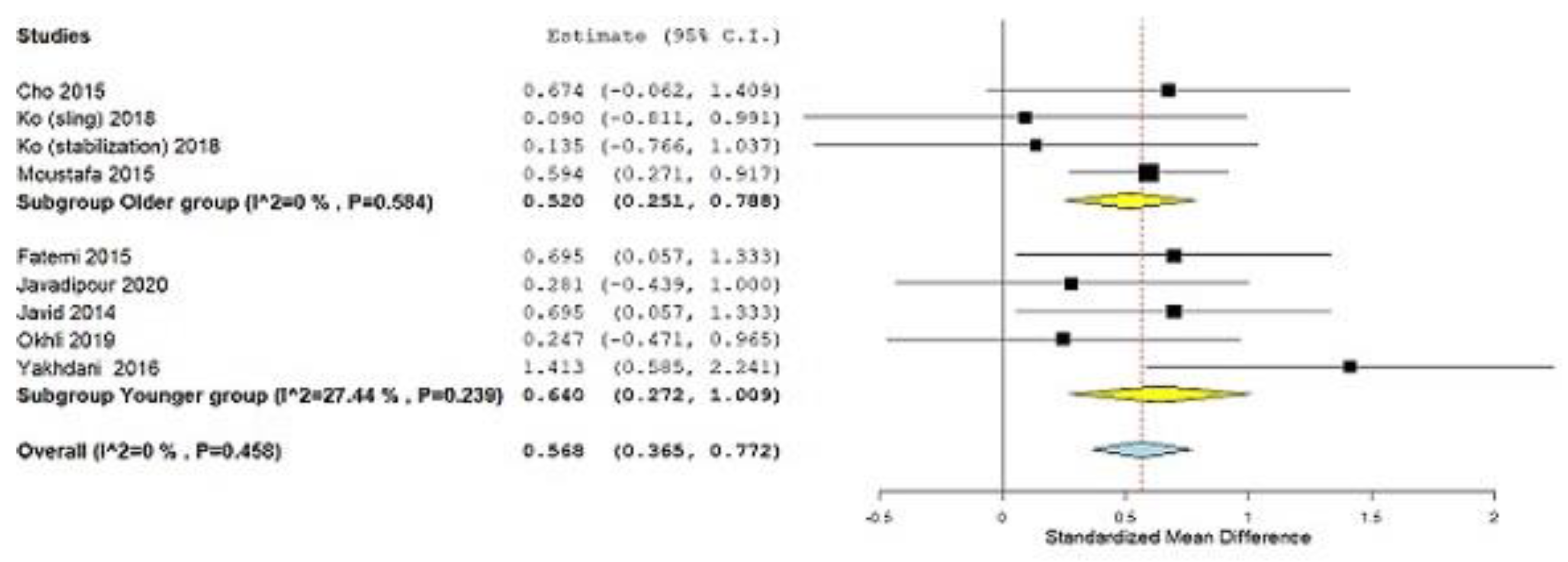
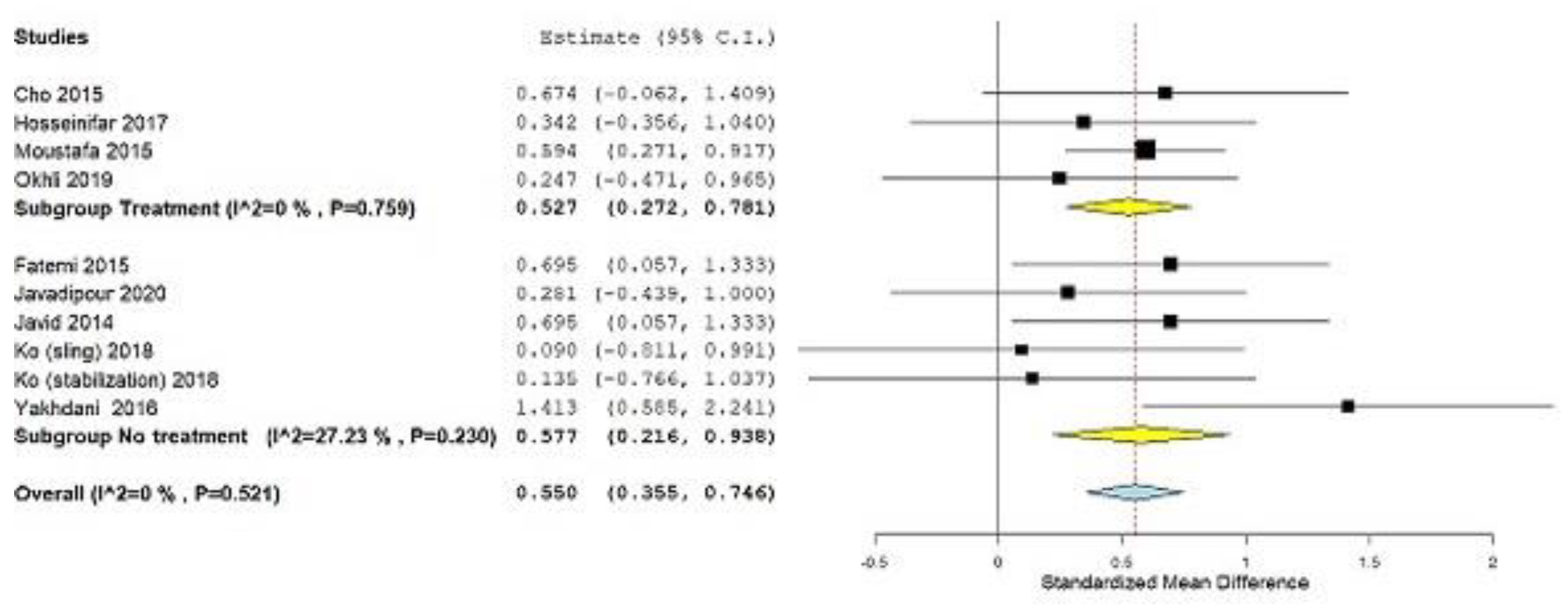
3.1.2. Subgroup Analysis
4. Discussion
4.1. Summary of Main Results
4.2. Overall Completeness and Applicability of Evidence
4.3. Quality of the Evidence
4.4. Potential Biases in the Review Process
4.5. Agreements and Disagreements with Other Studies or Reviews
4.6. Limitations and Future Studies
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kim, H.J. Determinants Related with Quality of Life in Patients with Chronic Low Back Pain. Master’s Thesis, Kosin University, Busan, Korea, 2013. [Google Scholar]
- Fritz, J.M.; Cleland, J.A.; Speckman, M.; Brennan, G.P.; Hunter, S.J. Physical therapy for acute low back pain: Associations with subsequent healthcare costs. Spine 2008, 33, 1800–1805. [Google Scholar] [CrossRef] [PubMed]
- Lehto, M.; Hurme, M.; Alaranta, H.; Einola, S.; Falck, B.; Järvinen, M.; Kalimo, H.; Mattila, M.; Paljärvi, L. Connective tissue changes of the multifidus muscle in patients with lumbar disc herniation. An immunohistologic study of collagen types I and III and fibronectin. Spine 1989, 14, 302–309. [Google Scholar] [CrossRef] [PubMed]
- El-Hamalawy, F.A. A Newly Developed Exercise Program for Treatment of Mechanical Low Back Pain Associated with Accentuated Lumbar Lordosis. J. Am. Sci. 2011, 7, 58–70. [Google Scholar]
- Morningstar, M.W. Strength gains through lumbar lordosis restoration. J. Chiropr. Med. 2003, 2, 137–141. [Google Scholar] [CrossRef][Green Version]
- Swärd, L.; Eriksson, B.; Peterson, L. Anthropometric characteristics, passive hip flexion, and spinal mobility in relation to back pain in athletes. Spine 1990, 15, 376–382. [Google Scholar] [CrossRef]
- Cyriax, J. Textbook of Orthopedic Medicine: Diagnosis of Soft Tissue Lesions, 7th ed.; Balliere Tindall: London, UK, 1978; p. 848. [Google Scholar]
- Hultman, G.; Saraste, H.; Ohlsen, H. Anthropometry, spinal canal width, and flexibility of the spine and hamstring muscles in 4555yearold men with and without low back pain. J. Spinal Disord. 1992, 5, 245–253. [Google Scholar] [CrossRef]
- Cailliet, R. Low Back Pain Syndrome, 5th ed.; F. A. Davis Company: Philadelphia, PA, USA, 1995; p. 341. [Google Scholar]
- Lin, R.M.; Jou, I.M.; Yu, C.Y. Lumbar lordosis: Normal adults. J. Formos. Med. Assoc. 1992, 91, 329–333. [Google Scholar]
- Berlemann, U.; Jeszenszky, D.; Bühler, D.W.; Harms, J. The role of lumbar lordosis, vertebral endplate inclination, disk height, and facet orientation in degenerative Spondylolisthesis. J. Spinal Disord. 1999, 12, 68–73. [Google Scholar] [CrossRef]
- Neumann, D.A. Kinesiology of the Musculoskeletal System-e-Book: Foundations for Rehabilitation; Elsevier Health Sciences; Elsevier: Amsterdam, The Netherlands, 2016. [Google Scholar]
- Kendall, F.P.; McCreary, E.K.; Provance, P.G.; Rodgers, M.; Romani, W. Muscles: Testing and Function with Posture and Pain; Lippincott Williams & Wilkins: Baltimore, MD, USA, 2005; pp. 1–100. [Google Scholar]
- Hodges, P.W.; Moseley, G.L. Pain and motor control of the lumbopelvic region: Effect and possible mechanisms. J. Electromyogr. Kinesiol. 2003, 13, 361–370. [Google Scholar] [CrossRef]
- Wagner, H.; Liebetrau, A.; Schinowski, D.; Wulf, T.; De Lussanet, M.H.E. Spinal lordosis optimizes the requirements for a stable erect posture. Theor. Biol. Med. Model 2012, 9, 13. [Google Scholar] [CrossRef]
- Norris, C.M. Back Stability: Integrating Science and Therapy; Human Kinetics: Champaign, IL, USA, 2008; p. 347. [Google Scholar]
- Bouchard, S.; Tetreault, M. The Motor development of blind people. J. Vis. Impair. Blind. 2000, 105, 8–10. [Google Scholar]
- Akuthota, V.; Nadler, S.F. Core strengthening. Arch. Phys. Med. Rehabil. 2004, 85, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Widhe, T. Spine: Posture, mobility and pain. A longitudinal study from childhood to adolescence. Eur. Spine J. 2001, 10, 118–123. [Google Scholar] [CrossRef] [PubMed]
- Shirado, O.; Doi, T.; Akai, M.; Hoshino, Y.; Fujino, K.; Hayashi, K.; Marui, E.; Iwaya, T.; Japan Low Back-Pain Exercise Therapy Study; Investigators Japanese Orthopaedic Association; et al. Multicenter randomized controlled trial to evaluate the effect of home-based exercise on patients with chronic low back pain: The Japan low back pain exercise therapy study. Spine 2010, 35, 811–819. [Google Scholar] [CrossRef]
- Lee, S.K.; Jung, J.M.; Lee, S.Y. Gluteus medius muscle activation on stance phase according to various vertical load. J. Back Musculoskelet. Rehabil. 2013, 26, 159–161. [Google Scholar] [CrossRef]
- Kofotolis, N.; Kellis, E. Effects of two 4-week proprioceptive neuromuscular facilitation programs on muscle endurance, flexibility, and functional performance in women with chronic low back pain. Phys Ther 2006, 86, 1001–1012. [Google Scholar] [CrossRef]
- Purepong, N.; Jitvimonrat, A.; Boonyong, S.; Thaveeratitham, P.; Pensri, P. Effect of flexibility exercise on lumbar angle: A study among non-specific low back pain patients. J. Bodyw. Mov. Ther. 2012, 16, 236–243. [Google Scholar] [CrossRef]
- Willson, J.D.; Dougherty, C.P.; Ireland, M.L.; Davis, I.M. Core stability and its relationship to lower extremity function and injury. J. Am. Acad. Orthop. Surg. 2005, 13, 316–325. [Google Scholar] [CrossRef]
- Panjabi, M.M. Clinical spinal instability and low back pain. J. Electromyogr. Kinesiol. 2003, 13, 371–379. [Google Scholar] [CrossRef]
- Moldovan, M. Therapeutic considerations and recovery in low back pain: Williams vs McKenzie. Timis. Phys. Educ. Rehabil. J. 2012, 5, 58–64. [Google Scholar] [CrossRef]
- Ariyoshi, M.; Mutoh, Y. Aquatic exercises for lumbago. Jpn. J. Sports Sci. 1991, 10, 494–503. [Google Scholar]
- Van Tubergen, A.; Landewé, R.; Van Der Heijde, D.; Hidding, A.; Wolter, N.; Asscher, M.; Falkenbach, A.; Genth, E.; Thè, H.G.; Van Der Linden, S. Combined spaexercise therapy is effective in patients with ankylosing spondylitis: Random Control Trial. Arthritis Care Res. 2001, 45, 430–438. [Google Scholar] [CrossRef]
- Haynes, W. Core stability and the unstable platform device. J. Bodyw. Mov. Ther. 2004, 8, 88–103. [Google Scholar] [CrossRef]
- Pederson, J.S.; Kirkesola, G.; Magnussen, R.; Kuffel, E.E.; Seiler, S.; Katch, F.I. Sling exercise training improves balance, Kicking velocity and torso stabilization strength in elite soccer players. Med. Sci. Sports Exerc. 2006, 38, 243–250. [Google Scholar] [CrossRef]
- Lee, J.S.; Yang, S.H.; Koog, Y.H.; Jun, H.-J.; Kim, S.-H.; Kim, K.-J. Effectiveness of sling exercise for chronic low back pain: A systematic review. J. Phys. Ther. Sci. 2014, 26, 1301–1306. [Google Scholar] [CrossRef] [PubMed]
- Ko, K.J.; Ha, G.C.; Yook, Y.S.; Kang, S.-J. Effects of 12-week lumbar stabilization exercise and sling exercise on lumbosacral region angle, lumbar muscle strength, and pain scale of patients with chronic low back pain. J. Phys. Ther. Sci. 2018, 30, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Skaf, G.S.; Ayoub, C.M.; Domloj, N.T.; Turbay, M.J.; El-Zein, C.; Hourani, M.H. Effect of age and lordotic angle on the level of lumbar disc herniation. Adv. Orthop. 2011, 2011, 950576. [Google Scholar] [CrossRef]
- Okhli, H.; Hojjati, H.; Akhoundzadeh, G. Comparing the Effect of the Corrective Exercises of America’s National Academy of Sports Medicine and Pilates on the Correction of Lordosis among Female High School Students in Golestan Province in 2018. Int. J. Sch. Health 2019, 6, 1–6. [Google Scholar]
- Yazici, A.G.; Mohammadi, M. The effect of corrective exercises on the thoracic kyphosis and lumbar lordosis of boy students. Turk. J. Sport Exerc. 2017, 19, 177–181. [Google Scholar] [CrossRef]
- Shirazi, S.A.; Haghighi, F.M.; Alavi, S.M.; Nezhad, F.F.; Emami, F. Is application of Kinesio tape to treat hyperlordosis more effective on abdominal muscles or hamstrings? J. Res. Med. Sci. 2018, 23, 9. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.; Thomas, J.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.; Welch, V.; Flemyng, E. Cochrane Handbook for Systematic Reviews of Interventions; John Wiley & Sons: Chichester, UK, 2019. [Google Scholar]
- Wallace, B.C.; Dahabreh, I.J.; Trikalinos, T.A.; Lau, J.; Trow, P.; Schmid, C.H. Closing the gap between methodologists and end-users: R as a computational back-end. J. Stat. Softw. 2012, 49, 1–15. [Google Scholar] [CrossRef]
- Cohen, J. The Concepts of Power Analysis BT—Statistical Power Analysis for the Behavioral Sciences; Revised Edition; Lawrence Erlbaum Associates: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Yakhdani, H.F.; Kamran, S.; Abasi, H.; Kordi, M.H.; Abedinzadeh, S. Comparison of eight weeks of training in the water and land on changes in lumbar lordosis of girl students of Yazd City. J. Clin. Physiother. Res. 2016, 2, 182–186. [Google Scholar]
- Fatemi, R.; Javid, M.; Najafabadi, E.M. Effects of William training on lumbosacral muscles function, lumbar curve and pain. J. Back Musculoskelet. Rehabil. 2015, 28, 591–597. [Google Scholar] [CrossRef] [PubMed]
- Javid, M.; Najafabadi, E.; Motlagh, K.; Fatemi, R. The effects of 8 weeks corrective training on lumbar angle and flexibility of lumbosacral muscles in females with hyperlordosis; William’s intervention. Int. J. Res. Stud. Biosci. 2014, 2, 116–125. [Google Scholar]
- Cho, I.; Jeon, C.; Lee, S.; Lee, D.; Hwangbo, G. Effects of lumbar stabilization exercise on functional disability and lumbar lordosis angle in patients with chronic low back pain. J. Phys. Ther. Sci. 2015, 27, 1983–1985. [Google Scholar] [CrossRef]
- Hosseinifar, M.; Ghiasi, F.; Akbari, A.; Ghorbani, M. The effect of stabilization exercises on lumbar lordosis in patients with low back pain. Ann. Trop. Med. Public Health 2017, 10, 1779–1784. [Google Scholar]
- Javadipour, Z.; Sedaghati, P.; Ahmadabadi, S. The effects of combining core stability with stretching exercises on pain intensity and motor function in people with chronic nonspecific low back pain with and without hyperlordosis. Ann. Appl. Sport Sci. 2021, 9, e908. [Google Scholar] [CrossRef]
- Moustafa, I.M.; Diab, A.A. The effect of adding forward head posture corrective exercises in the management of lumbosacral radiculopathy: A randomized controlled study. J. Manip. Physiol. Ther. 2015, 38, 167–178. [Google Scholar] [CrossRef]
- González-Gálvez, N.; Gea-García, G.M.; Marcos-Pardo, P.J. Effects of exercise programs on kyphosis and lordosis angle: A systematic review and meta-analysis. PLoS ONE 2019, 14, e0216180. [Google Scholar] [CrossRef]
| Study | N | Program Type | Outcome | Lordotic | Age | Sessions | Duration | Instrument to |
|---|---|---|---|---|---|---|---|---|
| Angle | Per Week | Measure Angle | ||||||
| Cho 2015 [44] | 30 | Lumbar stabilization exercise | LLA | 32.1° ± 3.3° | 48 ± 6.9 | (3× week) | 6 weeks | Plain |
| Conservative treatment | 32.3° ± 3.5° | 44 ± 6.7 | radiography | |||||
| Fatemi 2015 [42] | 40 | William training | LLA | 55.22° ± 6.00° | 15–18 | (3× week) | 8 weeks | Flexible ruler |
| Control group (no treatment) | 54.48° ± 6.54° | |||||||
| Hosseinifar 2018 [45] | 32 | Stabilization exercise | LLA | 27.63° ± 3.3° | 18–50 | (6× week) | 2 weeks | Flexible ruler |
| Control group (physiotherapy protocol) | 27.63° ± 4.7° | |||||||
| Javadipour 2020 [46] | 30 | Stretching-core stability exercises | LLA | 62.25° ± 3.88° | 13–15 | (3× week) | 8 weeks | Flexible ruler |
| Control group (no treatment) | 62.25° ± 3.88° | |||||||
| Javid 2014 [43] | 40 | William training | LLA | 55.22° ± 6.00° | 15–18 | (3× week) | 8 weeks | Flexible ruler |
| Control group (no treatment) | 54.48° ± 6.54° | |||||||
| Ko 2018 [32] | 29 | Lumbar stabilization exercise | LLA | 40.0° ± 1.5° | 43.1 ± 3.7 | (3× week) | 12 weeks | ViewRex |
| Sling exercise | 38.9° ± 2.1° | 43.6 ± 4.5 | system | |||||
| Control group (no treatment) | 40.0° ± 2.4° | 41.3 ± 3.8 | ||||||
| Moustafa 2015 [47] | 154 | Corrective exercises | LLA | 49.5° ± 3.4° | 49.1 ± 4.9 | (2× week) first 4 weeks | 10 weeks | Formetric |
| Control group (standard care) | 49.3° ± 3.2° | 50.5 ± 4.8 | (3× week) second 6 weeks | system | ||||
| Okhli 2019 [34] | 45 | NASM | LLA | 53.7° ± 1.83° | 15.26 ± 1.03 | (3× week) | 8 weeks | Flexible ruler |
| Pilates exercises | 53.13° ± 1.73° | 15.02 ± 1.28 | ||||||
| Control group (no treatment) | N/A | 14.76 ± 1.13 | ||||||
| Yakhdani 2017 [41] | 42 | Water exercises | LLA | 68.43° ± 11.75° | 9–12 | N/A | 8 weeks | Flexible ruler |
| Land exercises | 63.18° ± 11.5° | |||||||
| Control group (no treatment) | 61.32° ± 6.43° | |||||||
| Yazici 2017 [35] | 40 | Corrective exercise | LLA | 48.23° ± 1.74° | 16.84 ± 1.84 | (3× week) | 8 weeks | Spinal Mouse |
| Control group (no treatment) | 48.51° ± 2.18° | device |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dimitrijević, V.; Šćepanović, T.; Milankov, V.; Milankov, M.; Drid, P. Effects of Corrective Exercises on Lumbar Lordotic Angle Correction: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2022, 19, 4906. https://doi.org/10.3390/ijerph19084906
Dimitrijević V, Šćepanović T, Milankov V, Milankov M, Drid P. Effects of Corrective Exercises on Lumbar Lordotic Angle Correction: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health. 2022; 19(8):4906. https://doi.org/10.3390/ijerph19084906
Chicago/Turabian StyleDimitrijević, Vanja, Tijana Šćepanović, Vukadin Milankov, Miroslav Milankov, and Patrik Drid. 2022. "Effects of Corrective Exercises on Lumbar Lordotic Angle Correction: A Systematic Review and Meta-Analysis" International Journal of Environmental Research and Public Health 19, no. 8: 4906. https://doi.org/10.3390/ijerph19084906
APA StyleDimitrijević, V., Šćepanović, T., Milankov, V., Milankov, M., & Drid, P. (2022). Effects of Corrective Exercises on Lumbar Lordotic Angle Correction: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 19(8), 4906. https://doi.org/10.3390/ijerph19084906









