Evaluating the Dissemination and Implementation of a Community Health Worker-Based Community Wide Campaign to Improve Fruit and Vegetable Intake and Physical Activity among Latinos along the U.S.-Mexico Border
Abstract
1. Introduction
1.1. Utilizing the Community-Wide Campaign Model for Health Behavior Augmentation
1.2. Dissemination and Implementation of Community-Wide Campaigns
1.3. Research Questions
2. Materials and Methods
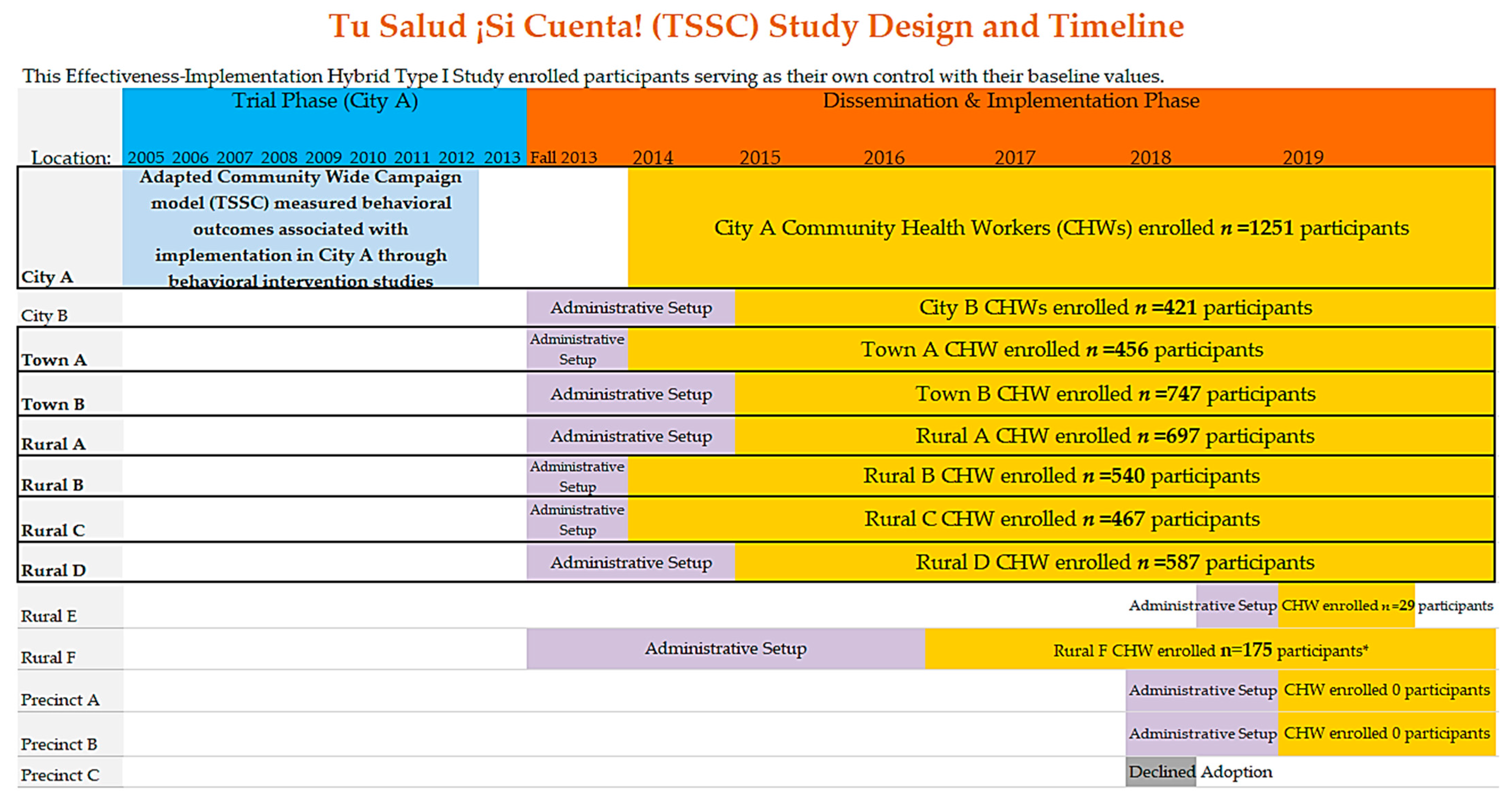
2.1. Study Design and Setting
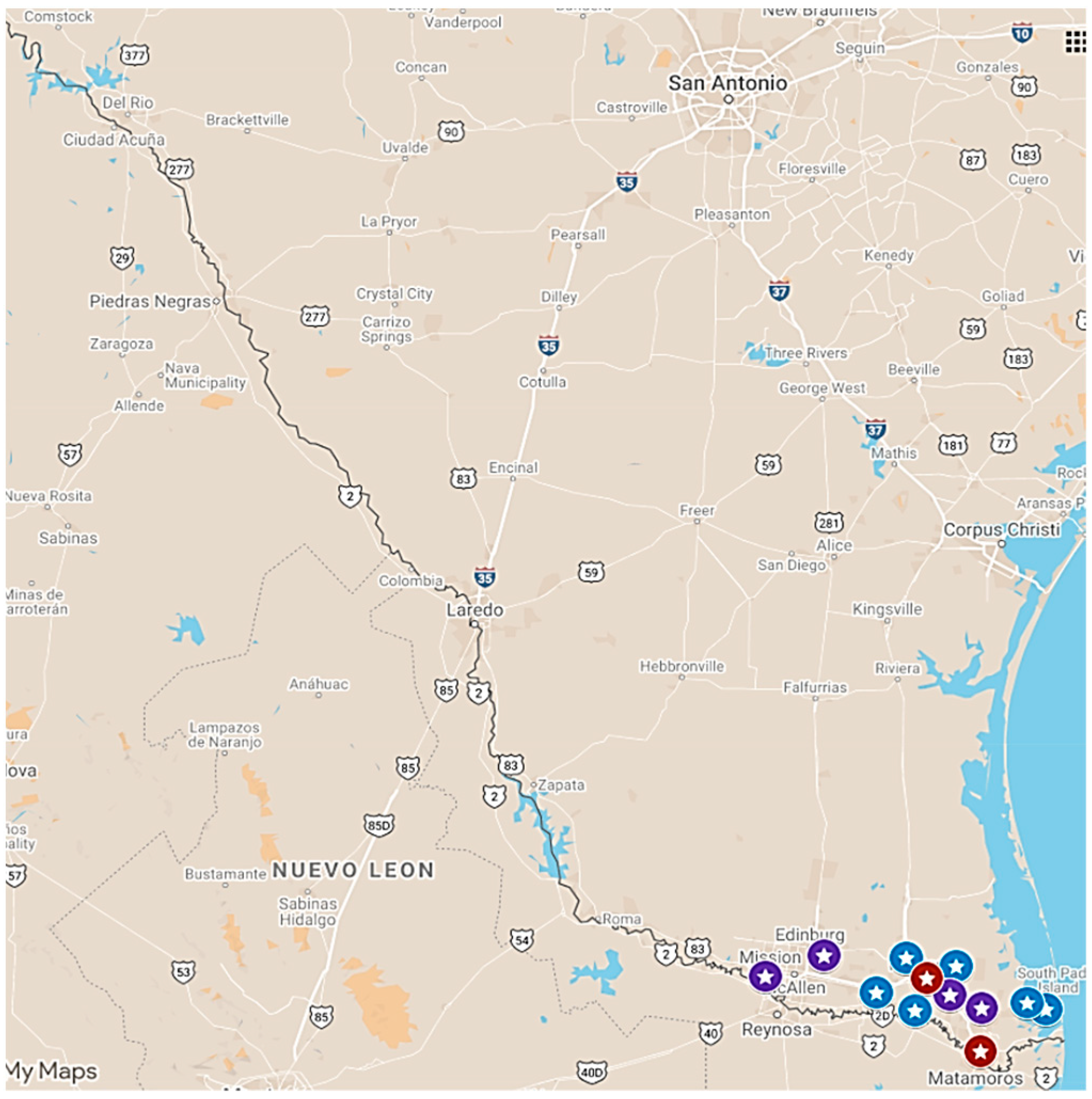
2.1.1. Implementing Locations
2.1.2. Tu Salud ¡Si Cuenta! Program Description and Implementation over Time
2.1.3. Tu Salud ¡Si Cuenta! Program Dissemination and Implementation
2.2. Measures
2.2.1. Sociodemographic Characteristics Measures
2.2.2. Fruit and Vegetable (FV) Consumption Measure
2.2.3. Physical Activity (PA) Measure
2.2.4. Participant Assignment to Locations
2.3. Statistical Analysis
3. Results
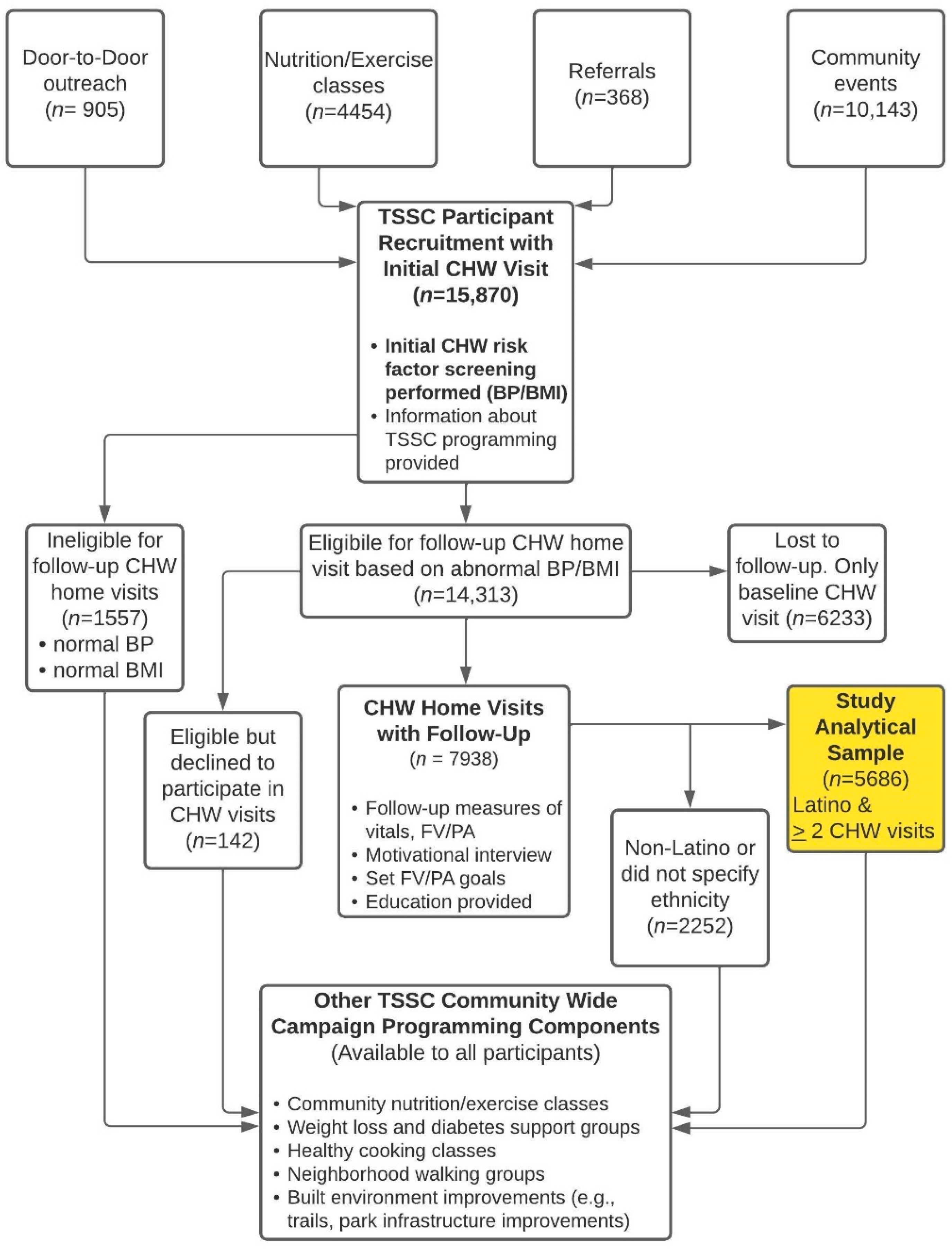
3.1. Intervention Reach
3.2. Intervention Effectiveness
3.2.1. Effectiveness Baseline Characteristics
3.2.2. Effectiveness across Municipalities on Fruit and Vegetable Consumption
3.2.3. Effectiveness across Municipalities on Meeting Physical Activity Guidelines
3.2.4. Effectiveness by Location on Fruit and Vegetable Intake and Physical Activity
3.3. Program Adoption
3.4. Program Implementation
3.5. Program Maintenance
4. Discussion
4.1. Reach
4.2. Effectiveness
4.3. Adoption
4.4. Implementation
4.5. Maintenance
4.6. Limitations
4.7. Strengths
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AOR | Adjusted odds ratio |
| BMI | body mass index |
| BP | blood pressure |
| CHW | Community health worker |
| CI | Confidence interval |
| CWC | Community-wide campaign |
| FPL | Federal poverty level |
| FV | Fruit and vegetable consumption |
| IQR | Interquartile range |
| MET | Metabolic equivalent |
| NCD | Non-communicable disease |
| OR | Odds ratio |
| PA | Physical activity |
| RE-AIM | Reach, effectiveness, adoption, implementation, and maintenance analysis model |
| RR | Relative risk |
| SD | Standard deviation |
| SPH | School of Public Health [University of Texas Health Science Center at Houston] |
| TSSC | Tu Salud ¡Si Cuenta! (Your Health Matters!) initiative |
References
- 2015–2020 Dietary Guidelines for Americans, 8th ed.; U.S. Department of Health and Human Services: Washington, DC, USA, 2015. Available online: https://health.gov/dietaryguidelines/2015/guidelines/externalicon (accessed on 10 May 2021).
- Colon-Ramos, U.; Thompson, F.E.; Yaroch, A.L.; Moser, R.P.; McNeel, T.S.; Dodd, K.W.; Atienza, A.A.; Sugerman, S.B.; Nebeling, L. Differences in Fruit and Vegetable Intake among Hispanic Subgroups in California: Results from the 2005 California Health Interview Survey. J. Am. Diet. Assoc. 2009, 109, 1878–1885. [Google Scholar] [CrossRef] [PubMed]
- Neighbors, C.J.; Marquez, D.X.; Marcus, B.H. Leisure-time physical activity disparities among Hispanic subgroups in the United States. Am. J. Public Health 2008, 98, 1460–1464. [Google Scholar] [CrossRef] [PubMed]
- Dunstan, D.; Barr, E.; Healy, G.; Salmon, J.; Shaw, J.; Balkau, B.; Magliano, D.; Cameron, A.; Zimmet, P.; Owen, N. Television viewing time and mortality the Australian diabetes, obesity and lifestyle study (AusDiab). Circulation 2010, 121, 384–391. [Google Scholar] [CrossRef] [PubMed]
- Marquez, D.X.; Neighbors, C.J.; Bustamante, E.E. Leisure time and occupational physical activity among racial or ethnic minorities. Med. Sci. Sports Exerc. 2010, 42, 1086–1093. [Google Scholar] [CrossRef]
- Dietary Guidelines for Americans. 2005. Available online: http://www.health.gov/dietaryguidelines/dga2005/document/pdf/DGA2005.pdf (accessed on 28 April 2021).
- Department of Health and Human Services (DHHS). Executive Summary: Physical Activity Guidelines for Americans, 2nd ed.; U.S. Department of Health and Human Services: Washington, DC, USA. Available online: https://health.gov/sites/default/files/2019-10/PAG_ExecutiveSummary.pdf (accessed on 18 May 2021).
- Go, A.S.; Mozaffarian, D.; Roger, V.L.; Benjamin, E.J.; Berry, J.D.; Borden, W.B.; Bravata, D.M.; Dai, S.; Ford, E.S.; Fox, C.S.; et al. Heart disease and stroke statistics-2013 update: A report from the American Heart Association. Circulation 2013, 127, e6–e245. [Google Scholar] [CrossRef]
- Heredia, N.I.; Lee, M.; Mitchell-Bennett, L.; Reininger, B.M. Tu salud ¡Sí cuenta! your health matters! A Community-wide campaign in a Hispanic Border Community in Texas. J. Nutr. Educ. Behav. 2017, 49, 801–809.e1. [Google Scholar] [CrossRef][Green Version]
- Warren, T.Y.; Barry, V.; Hooker, S.P.; Sui, X.; Church, T.S.; Blair, S.N. Sedentary behaviors increase risk of cardiovascular disease mortality in men. Med. Sci. Sports Exerc. 2010, 42, 879. [Google Scholar] [CrossRef]
- Grøntved, A.; Hu, F.B. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: A meta-analysis. JAMA 2011, 305, 2448–2455. [Google Scholar] [CrossRef]
- Edwardson, C.L.; Gorely, T.; Davies, M.J.; Gray, L.J.; Khunti, K.; Wilmot, E.G.; Yates, T.; Biddle, S.J. Association of sedentary behaviour with metabolic syndrome: A meta-analysis. PLoS ONE 2012, 7, e34916. [Google Scholar] [CrossRef]
- Reininger, B.M.; Wang, J.; Fisher-Hoch, S.P.; Boutte, A.; Vatcheva, K.; McCormick, J.B. Non-communicable diseases and preventive health behaviors: A comparison of Hispanics nationally and those living along the US-Mexico border. BMC Public Health 2015, 15, 564. [Google Scholar] [CrossRef]
- Machado de Rezende, L.F.; de Sa, T.H.; Markozannes, G.; Rey-Lopez, J.P.; Lee, I.M.; Tsilidis, K.K.; Ioannidis, J.P.A.; Eluf-Neto, J. Physical activity and cancer: An umbrella review of the literature including 22 major anatomical sites and 770,000 cancer cases. Br. J. Sports Med. 2018, 52, 826–833. [Google Scholar] [CrossRef] [PubMed]
- Fisher-Hoch, S.P.; Vatcheva, K.P.; Laing, S.T.; Hossain, M.M.; Rahbar, M.H.; Hanis, C.L.; Brown, H.S., III; Rentfro, A.R.; Reininger, B.M.; McCormick, J.B. Missed Opportunities for Diagnosis and Treatment of Diabetes, Hypertension, and Hypercholesterolemia in a Mexican American Population, Cameron County Hispanic Cohort, 2003–2008. Prev. Chronic Dis. 2012, 9, 110298. [Google Scholar] [CrossRef] [PubMed]
- Campaigns and Informational Approaches to Increase Physical Activity: Community-Wide Campaigns. Available online: https://www.thecommunityguide.org/findings/physical-activity-community-wide-campaigns (accessed on 13 May 2021).
- Heredia, N.I.; Lee, M.; Reininger, B.M. Exposure to a community-wide campaign is associated with physical activity and sedentary behavior among Hispanic adults on the Texas Mexico border. BMC Public Health 2017, 17, 883. [Google Scholar] [CrossRef]
- Vidoni, M.L.; Lee, M.; Mitchell-Bennett, L.; Reininger, B.M. Home visit intervention promotes lifestyle changes: Results of an RCT in Mexican Americans. Am. J. Prev. Med. 2019, 57, 611–620. [Google Scholar] [CrossRef]
- Spencer, L.; Adams, T.B.; Malone, S.; Roy, L.; Yost, E. Applying the transtheoretical model to exercise: A systematic and comprehensive review of the literature. Health Promot. Pract. 2006, 7, 428–443. [Google Scholar] [CrossRef]
- Marshall, S.J.; Biddle, S.J. The transtheoretical model of behavior change: A meta-analysis of applications to physical activity and exercise. Ann. Behav. Med. 2001, 23, 229–246. [Google Scholar] [CrossRef]
- Jo, H.S.; Song, Y.L.A.; Yoo, S.; Lee, H. Effectiveness of a province-wide walking campaign in Korea on the stages of change for physical activity. Int. J. Sport Exerc. Psychol. 2010, 8, 433–445. [Google Scholar] [CrossRef]
- Leavy, J.E.; Rosenberg, M.; Bauman, A.E.; Bull, F.C.; Giles-Corti, B.; Shilton, T.; Maitland, C.; Barnes, R. Effects of find thirty every day®: Cross-sectional findings from a western Australian population-wide mass media campaign, 2008–2010. Health Educ. Behav. 2013, 40, 480–492. [Google Scholar] [CrossRef]
- Sharpe, P.A.; Burroughs, E.L.; Granner, M.L.; Wilcox, S.; Hutto, B.E.; Bryant, C.A.; Peck, L.; Pekuri, L. Impact of a community-based prevention marketing intervention to promote physical activity among middle-aged women. Health Educ. Behav. 2010, 37, 403–423. [Google Scholar] [CrossRef]
- Jennings, C.A.; Berry, T.R.; Carson, V.; Culos-Reed, S.N.; Duncan, M.J.; Loitz, C.C.; McCromack, G.R.; McHugh, T.L.F.; Spence, J.C.; Vallance, J.K.; et al. UWALK: The development of a multi-strategy, community-wide physical activity program. Transl. Behav. Med. 2017, 7, 16–27. [Google Scholar] [CrossRef]
- Gubbels, J.S.; Mathisen, F.K.S.; Samdal, O.; Lobstein, T.; Kohl, L.F.; Leversen, I.; Lakerveld, J.; Kremers, S.P.; van Assema, P. The assessment of ongoing community-based interventions to prevent obesity: Lessons learned. BMC Public Health 2015, 15, 216. [Google Scholar] [CrossRef] [PubMed]
- Baker, P.R.; Francis, D.P.; Soares, J.; Weightman, A.L.; Foster, C. Community-wide interventions for increasing physical activity. Cochrane Database Syst. Rev. 2015, 4, CD008366. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.T.; Drewnosksi, A.; Kumanyika, S.; Glass, T.A. A systems-oriented multilevel framework for addressing obesity in the 21st century. Prev. Chronic Dis. 2009, 6, A82. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2722412/pdf/PCD63A82.pdf (accessed on 15 December 2021). [PubMed]
- Fleishhacker, S.; Robert, E.; Camplain, R.; Evenson, K.R.; Gittelsohn, J. Promoting Physical Activity among Native American Youth: A Systematic Review of the Methodology and Current Evidence of Physical Activity Interventions and Community-wide Initiatives. J. Racial Ethn. Health Disparities 2016, 3, 608–624. [Google Scholar] [CrossRef] [PubMed]
- Compernolle, S.; de Cocker, K.; Lakerveld, J.; Mackenbach, J.D.; Nijpels, G.; Oppert, J.M.; Rutter, H.; Teixeira, P.J.; Cardon, G.; De Bourdeaudhuij, I. A RE-AIM evaluation of evidence-based multi-level interventions to improve obesity-related behaviours in adults: A systematic review (the SPOTLIGHT project). Int. J. Behav. Nutr. Phys. Act. 2014, 11, 147. [Google Scholar] [CrossRef] [PubMed]
- Reininger, B.M.; Mitchell-Bennett, L.; Lee, M.; Gowen, R.Z.; Barroso, C.S.; Gay, J.L.; Saldana, M.V. Tu salud, ¡Si cuenta!: Exposure to a community-wide campaign and its associations with physical activity and fruit and vegetable consumption among individuals of Mexican descent. Soc. Sci. Med. 2015, 13, 98–106. [Google Scholar] [CrossRef]
- Green, L.W.; Ottoson, J.M.; García, C.; Hiatt, R.A. Diffusion theory and knowledge dissemination, utilization, and integration in public health. Ann. Rev. Public Health 2009, 30, 151–174. [Google Scholar] [CrossRef]
- Brownson, R.; Colditz, G.; Proctor, E.; Colditz, G. The promise and challenges of dissemination and implementation research. In Dissemination and Implementation Research in Health: Translating Science to Practice, 1st ed.; Brownson, R., Colditz, G., Proctor, E., Eds.; Oxford University Press: New York, NY, USA, 2012; pp. 3–22. [Google Scholar]
- Brownson, R.C.; Colditz, G.; Proctor, E.; Rabin, B.A.; Brownson, R. Developing the terminology for dissemination and implementation research. In Dissemination and Implementation Research in Health: Translating Science to Practice, 2nd ed.; Brownson, R.C., Colditz, G., Proctor, E., Eds.; Oxford University Press: New York, NY, USA, 2017; pp. 23–51. [Google Scholar]
- Puska, P.; Vartiainen, E.; Laatikainen, T.; Jousilahti, P.; Paavola, M. The North Karelia Project: From North Karelia to National Action; The National Institute for Health and Welfare (THL): Helsinki, Finland, 2009; pp. 85–102.
- Puska, P.; Ståhl, T. Health in All Policies—The Finnish Initiative: Background, principles, and current issues. Ann. Rev. Public Health 2010, 31, 315–328. [Google Scholar] [CrossRef]
- Lewis, B.A.; Napolitano, M.A.; Buman, M.P.; Williams, D.M.; Nigg, C.R. Future directions in physical activity intervention research: Expanding our focus to sedentary behaviors, technology, and dissemination. J. Behav. Med. 2017, 40, 112–126. [Google Scholar] [CrossRef]
- Glasgow, R.E.; Vogt, T.M.; Boles, S.M. Evaluating the Public Health Impact of Health Promotion Interventions: The RE-AIM Framework. Am. J. Public Health 1999, 89, 1322–1327. [Google Scholar] [CrossRef]
- Curran, G.M.; Bauer, M.; Mittman, B.; Pyne, J.M.; Stetler, C. Effectiveness-implementation Hybrid Designs: Combining Elements of Clinical Effectiveness and Implementation Research to Enhance Public Health Impact. Med. Care 2012, 50, 217–226. [Google Scholar] [CrossRef] [PubMed]
- Harris, A.D.; McGregor, J.C.; Perencevich, E.N.; Furuno, J.P.; Zhu, J.; Peterson, D.E.; Finkelstein, J. The Use and Interpretation of Quasi-Experimental Studies in Medical Informatics. J. Am. Med. Inform. Assoc. 2006, 13, 16–23. [Google Scholar] [CrossRef] [PubMed]
- Fisher-Hoch, S.P.; Rentfro, A.R.; Salinas, J.J.; Perez, A.; Brown, H.S.; Reininger, B.M.; Restrepo, B.I.; Wilson, J.G.; Hossain, M.M.; Rahbar, M.H.; et al. Socioeconomic status and prevalence of obesity and diabetes in a Mexican American community, Cameron County, Texas, 2004–2007. Prev. Chronic Dis. 2010, 7, A53. Available online: http://www.cdc.gov/pcd/issues/2010/may/09_0170.htm (accessed on 23 August 2021). [PubMed]
- Ryabov, I.; Merino, S. Recent Demographic Change in the Rio Grande Valley of Texas: The Importance of Domestic Migration. J. Borderl. Stud. 2017, 2, 211–231. [Google Scholar] [CrossRef][Green Version]
- United States Census Bureau. Poverty Status in the Past 12 Months: 2010 American Community Survey 1-Year Estimates Subject Tables. Available online: https://data.census.gov/cedsci/table?q=poverty%20cameron%20county%20hidalgo%20county&tid=ACSST1Y2010.S1701 (accessed on 25 August 2021).
- Transforming Persistent Poverty in America: How Community Development Financial Institutions Drive Economic Opportunity. Robert Wood Johnson Foundation and NeighborWorks America. Available online: https://www.ruraltransformation.org/wp-content/uploads/2020/03/Transforming_Persistent_Poverty_in_America_-_Policy-Paper-PRT-_FINAL.pdf (accessed on 22 May 2021).
- Fisher-Hoch, S.P.; Vatcheva, K.P.; Rahbar, M.H.; McCormick, J.B. Undiagnosed Diabetes and Pre-Diabetes in Health Disparities. PLoS ONE 2015, 10, e0133135. [Google Scholar] [CrossRef]
- Eyler, A.A.; Brownson, R.C.; Bacak, S.J.; Housemann, R.A. The epidemiology of walking for physical activity in the United States. Basic Sci. Epidemiol. 2003, 35, 1529–1536. [Google Scholar] [CrossRef]
- Marcus, B.H.; Hartman, S.J.; Larsen, B.A.; Pekmezi, D.; Dunsiger, S.I.; Linke, S.; Marquez, B.; Gans, K.M.; Bock, B.C.; Mendoza-Vasconez, A.S.; et al. Pasos Hacia La Salud: A randomized controlled trial of an internet-delivered physical activity intervention for Latinas. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 62. [Google Scholar] [CrossRef]
- Poverty Status in the Past 12 Months. 2018 American Community Survey 5-Year Estimates Subject Tables. Available online: https://data.census.gov/cedsci/table?q=brownsville,%20harlingen,%20los%20fresnos,%20san%20benito,%20hidalgo%20county,%20combes,%20los%20indios,%20port%20isabel,%20rio%20hondo,%20laguna%20vista,%20la%20feria%20texas%20poverty%20rates&tid=ACSST5Y2018.S1701 (accessed on 27 August 2021).
- Reininger, B.M.; Barroso, C.S.; Mitchell-Bennett, L.; Cantu, E.; Fernandez, M.E.; Gonzalez, D.A.; Chavez, M.; Freeberg, D.; McAlister, A. Process evaluation and participatory methods in an obesity-prevention media campaign for Mexican Americans. Health Promot. Pract. 2010, 11, 347–357. [Google Scholar] [CrossRef]
- Parra-Medina, D.; Morales-Campos, D.Y.; Mojica, C.; Ramirez, A.G. Promotora outreach, education and navigation support for HPV vaccination to Hispanic women with unvaccinated daughters. J. Cancer Educ. 2015, 30, 353–359. [Google Scholar] [CrossRef]
- Keller, C.S.; Cantue, A. Camina por Salud: Walking in Mexican-American women. Appl. Nurs. Res. 2008, 21, 110–113. [Google Scholar] [CrossRef]
- Crespo, N.C.; Elder, J.P.; Ayala, G.X.; Slymen, D.J.; Campbell, N.R.; Sallis, J.F.; McKenzie, T.L.; Baquero, B.; Arredondo, E.M. Results of a multi-level intervention to prevent and control childhood obesity among Latino children: The Aventuras para Niños study. Ann. Behav. Med. 2012, 43, 84–100. [Google Scholar] [CrossRef] [PubMed]
- Perales, J.; Reininger, B.M.; Lee, M.J.; Linder, S.H. Participants’ perceptions of interactions with community health workers who promote behavior change: A qualitative characterization from participants with normal, depressive, and anxious mood states. Int. J. Equity Health 2018, 17, 19. [Google Scholar] [CrossRef] [PubMed]
- Larsen, B.A.; Noble, M.L.; Murray, K.E.; Marcus, B.H. Physical activity in Latino men and women: Facilitators, barriers, and interventions. Am. J. Life Med. 2014, 9, 4–30. [Google Scholar] [CrossRef]
- Marcus, B.H.; Dunsiger, S.I.; Pekmezi, D.W.; Larsen, B.A.; Bock, B.C.; Gans, K.M.; Marquez, B.; Morrow, K.M.; Tilkemeier, P. The seamos saludables study: A randomized controlled physical activity trial of Latinas. Am. J. Prev. Med. 2013, 45, 598–605. [Google Scholar] [CrossRef] [PubMed]
- Brown, L.D.; Vasquez, D.; Lopez, D.I. Addressing Hispanic Obesity Disparities Using a Community Health Worker Model Grounded in Motivational Interviewing. Am. J. Health Promot. 2021, 36, 259–268. [Google Scholar] [CrossRef]
- McLeroy, K.R.; Bibeau, D.; Steckler, A.; Glanz, K. An ecological perspective on health promotion programs. Health Educ. Q. 1988, 15, 351–377. [Google Scholar] [CrossRef]
- HHS Poverty Guidelines for 2020. Available online: https://aspe.hhs.gov/poverty-guidelines (accessed on 27 May 2021).
- Cappuccio, F.P.; Rink, E.; Perkins-Porras, L.; McKay, C.; Hilton, S.; Steptoe, A. Estimation of fruit and vegetable intake using a two-item dietary questionnaire: A potential tool for potential tool for primary health care workers. Nutr. Metab. Cardiovasc. Dis. 2003, 13, 12–19. [Google Scholar] [CrossRef]
- Sharkey, J.R.; Dean, W.R.; Johnson, C.M. Association of Household and Community Characteristics with Adult and Child Food Insecurity among Mexican-Origin Households in Colonias along the Texas-Mexico Border. Int. J. Equity Health 2011, 10, 19. [Google Scholar] [CrossRef]
- Gartrell, V. Validating the Dietary Intake Questions from the Tu Salud, Si Cuenta! Questionnaire. Master’s Thesis, The University of Texas School of Public Health, Houston, TX, USA, 2009. [Google Scholar]
- Thiagarajah, K.; Fly, A.D.; Hoelscher, D.M.; Bai, Y.; Lo, K.; Leone, A.; Shertzer, J.A. Validating the food behavior questions from the elementary school SPAN questionnaire. J. Nutr. Educ. Behav. 2008, 40, 305–310. [Google Scholar] [CrossRef]
- Godin, G.; Shephard, R.J. Godin leisure-time exercise questionnaire. Med. Sci. Sports Exerc. 1997, 29, s36–s38. [Google Scholar]
- Walker, T.J.; Heredia, N.I.; Reininger, B.M. Examining the Validity, Reliability, and Measurement Invariance of the Social Support for Exercise Scale among Spanish- and English-Language Hispanics. Hisp. J. Behav. Sci. 2019, 41, 427–443. [Google Scholar] [CrossRef] [PubMed]
- Miller, D.J.; Freedson, P.S.; Kline, G.M. Comparison of activity levels using the Caltrac accelerometer and five questionnaires. Med. Sci. Sports Exerc. 1994, 26, 376–382. [Google Scholar] [CrossRef] [PubMed]
- Cancela Carral, J.M.; Ballsteros, J.L.; Perez, C.A.; Mosquera Morono, M.B. Análisis de fiabilidad y validez de tres cuestionarios de autoinforme para valorar la actividad física realizada por adolescentes españolesAnalysis of the reliability and validity of three self-report questionnaires to assess physical activity among Spanish adolescents. Gac. Sanit. 2016, 30, 333–338. [Google Scholar] [PubMed]
- United States Department of Health and Human Services. Physical Activity Guidelines for Americans, 2nd ed.; U.S. Department of Health and Human Services: Washington, DC, USA, 2019. Available online: https://health.gov/sites/default/files/2019-09/Physical_Activity_Guidelines_2nd_edition.pdf (accessed on 27 May 2021).
- Lee, W.C.; Serag, H.; Lancaster, D. Challenges to Address Health Disparities by Using Community Health Workers and Promotores (CHW/Ps) in Galveston County. Tex. Public Health J. 2018, 70, 13–17. [Google Scholar]
- Beaudoin, C.E.; Fernandez, C.; Wall, J.L.; Farley, T.A. Promoting healthy eating and physical activity: Short-term effects of a mass media campaign. Am. J. Prev. Med. 2007, 32, 217–223. [Google Scholar] [CrossRef]
- Kamada, M.; Kitayuguchi, J.; Inoue, S.; Ishikawa, Y.; Nishiuchi, H.; Okada, S.; Harada, K.; Kamioka, H.; Shiwaku, K. A community-wide campaign to promote physical activity in middle-aged and elderly people: A cluster randomized controlled trial. Int. J. Behav. Nutr. Phys. Act. 2013, 10, 44. [Google Scholar] [CrossRef]
- Galaviz, K.I.; Harden, S.M.; Smith, E.; Blackman, K.C.A.; Berrey, L.M.; Mama, S.K.; Almeida, F.A.; Lee, R.E.; Estabrooks, P.A. Physical activity promotion in Latin American populations: A systematic review on issues of internal and external validity. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 77. [Google Scholar] [CrossRef]
- Glasgow, R.E.; Harden, S.M.; Gaglio, B.; Rabin, B.; Smith, M.L.; Porter, G.C.; Ory, M.G.; Estabrooks, P.A. RE-AIM Planning and Evaluation Framework: Adapting to New Science and Practice With a 20-Year Review. Front. Public Health 2019, 7, 64. [Google Scholar] [CrossRef]
- Lee, R.E.; Reese-Smith, J.Y.; Mama, S.K.; Medina, A.V.; Wolfe, K.L.; Estabrooks, P.A. Reach and representativeness of ethnic minority women in the health is power study: A longitudinal analysis. Transl. Behav. Med. 2017, 7, 106–114. [Google Scholar] [CrossRef]
- Reger, B.; Wootan, M.G.; Booth-Butterfield, S. A comparison of different approaches to promote community wide dietary change. Am. J. Prev. Med. 2000, 18, 271–275. [Google Scholar] [CrossRef]
- Reger, B.; Wootan, M.G.; Booth-Butterfield, S.; Smith, H. 1% or less: A community-based nutrition campaign. Public Health Rep. 1998, 113, 410–419. [Google Scholar] [PubMed]
- Fortmann, S.P.; Taylor, C.B.; Flora, J.A.; Winkleby, M.A. Effect of community health education on plasma cholesterol levels and diet: The Stanford Five-City Project. Am. J. Epidemiol. 1993, 137, 1039–1055. [Google Scholar] [CrossRef] [PubMed]
- Vanassema, P.; Steenbakkers, M.; Kok, G.; Eriksen, M.; Devries, H. Results of the Dutch Community Project “Healthy Bergeyk”. Prev. Med. 1994, 23, 394–401. [Google Scholar] [CrossRef] [PubMed]
- Mohammadifard, N.; Kelishadi, R.; Safavi, M.; Sarrafzadegan, N.; Sajadi, F.; Sadri, G.H.; Maghroon, M.; Alikhasi, H.; Heydari, S.; Sarmadi, F. Effect of a community-based intervention on nutritional behaviour in a developing country setting: The Isfahan Healthy Heart Programme. Public Health Nutr. 2009, 12, 1422–1430. [Google Scholar] [CrossRef] [PubMed]
- Dergance, J.M.; Mouton, C.P.; Lichtenstein, M.J.; Hazuda, H.P. Potential mediators of ethnic differences in physical activity in older Mexican Americans and European Americans: Results from the San Antonio longitudinal study of aging. J. Am. Geriatr. Soc. 2005, 53, 1240–1247. [Google Scholar] [CrossRef] [PubMed]
- Oppenheimer, G.M.; Blackburn, H.; Puska, P. From Framingham to North Karelia to U.S. Community-Based Prevention Programs: Negotiating Research Agenda for Coronary Heart Disease in the Second Half of the 20th Century. Public Health Rev. 2011, 33, 450–483. [Google Scholar] [CrossRef]
- Portillo, E.M.; Vasquez, D.; Brown, L.D. Promoting Hispanic Immigrant Health via Community Health Workers and Motivational Interviewing. Int. Q. Community Health Educ. 2020, 41, 3–6. [Google Scholar] [CrossRef]
- De Cocker, K.A.; De Bourdeaudhuji, I.M.; Brown, W.J.; Cardon, G.M. Effects of “10,000 Steps Ghent”: A Whole-Community Intervention. Am. J. Prev. Med. 2007, 33, 455–463. [Google Scholar] [CrossRef]
- Kamada, M.; Kitayuguchi, J.; Abe, T.; Tuguri, M.; Inoue, S.; Ishikawa, Y.; Bauman, A.; Lee, I.M.; Miyachi, M.; Kawachi, I. Community-wide intervention and population-level physical activity: A 5-year cluster randomized trial. Int. J. Epidemiol. 2017, 47, 642–653. [Google Scholar] [CrossRef]
- Reininger, B.M.; Mitchell-Bennett, L.A.; Lee, M.; Yeh, P.G.; Dave, A.C.; Park, S.K.; Xu, T.; Ochoa-Del Toro, A.G. Scaling a Community-Wide Campaign Intervention to Manage Hypertension and Weight Loss. Front. Med. 2021, 8, 661353. [Google Scholar] [CrossRef]
- Hotez, P.J. Noncommunicable Diseases: A Globalization of Disparity? PLoS Med. 2015, 12, e1001859. [Google Scholar] [CrossRef] [PubMed]
- Allen, L.; Williams, J.; Townsend, N.; Mikkelsen, B.; Roberts, N.; Foster, C.; Wickramasinghe, K. Socioeconomic status and non-communicable disease behavioural risk factors in low-income and lower-middle-income countries: A systematic review. Lancet Glob. Health 2017, 5, e277–e289. [Google Scholar] [CrossRef]
- Lloyd-Jones, D.; Adams, R.; Carnethon, M.; De Simone, G.; Ferguson, T.B.; Flegal, K.; Ford, E.; Furie, K.; Go, A.; Greenlund, K. Heart disease and stroke statistics-2009 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2009, 119, e21–e181. [Google Scholar] [CrossRef] [PubMed]
- Myers, H.F.; Rodriguez, N. Acculturation and physical health in racial and ethnic minorities. In Acculturation: Advances in Theory, Measurement, and Applied Research; Chun, K.M., Balls Organista, P., Marín, G., Eds.; American Psychological Association: Washington, DC, USA, 2003; pp. 163–185. [Google Scholar]
- Leviton, L.C. Generalizing about public health interventions: A mixed-methods approach to external validity. Ann. Rev. Public Health 2017, 38, 371–391. [Google Scholar] [CrossRef]
- Rabin, B.A.; Brownson, R.C.; Kerner, J.F.; Glasgow, R.E. Methodologic Challenges in Disseminating Evidence-Based Interventions to Promote Physical Activity. Am. J. Prev. Med. 2006, 31, 24–34. [Google Scholar] [CrossRef]
- Rudd, R.E.; Goldberg, J.; Dietz, W. A Five-Stage Model for Sustaining a Community Campaign. J. Health Commun. 1999, 4, 37–48. [Google Scholar] [CrossRef]
- Zapata, J.; Colistra, A.; Lesser, J.; Flores, B.; Zavala-Idar, A.; Moreno-Vasquez, A. Opioid Use Disorder ECHO: A Program Evaluation of a Project That Provides Knowledge and Builds Capacity for Community Health Workers in Medically Underserved Areas of South Texas. Issues Ment. Health Nurs. 2020, 42, 381–390. [Google Scholar] [CrossRef]
- Uriarte, J.A.; Cummings, A.D.L.; Lloyd, L.E. An Instructional Design Model for Culturally Competent Community Health Worker Training. Health Promot. Pract. 2014, 15, 56S–63S. [Google Scholar] [CrossRef]
- Knudsen, H.K.; Drainoni, M.L.; Gilbert, L.; Huerta, T.R.; Oser, C.B.; Aldrich, A.M.; Campbell, A.N.C.; Crable, E.L.; Garner, B.R.; Glasgow, L.M.; et al. Model and approach for assessing implementation context and fidelity in the HEALing Communities Study. Drug Alcohol Depend. 2020, 217, 108330. [Google Scholar] [CrossRef]
- Taber, D.R.; Stevens, J.; Murray, D.M.; Elder, J.P.; Webber, L.S.; Jobe, J.B.; Lytle, L.A. The Effect of a Physical Activity Intervention on Bias in Self-Reported Activity. Ann. Epidemiol. 2009, 19, 316–322. [Google Scholar] [CrossRef]
- Brenner, P.S.; DeLameter, J.D. Social Desirability Bias in Self-reports of Physical Activity: Is an Exercise Identity the Culprit? Soc. Indic. Res. 2014, 117, 489–504. [Google Scholar] [CrossRef]
- Subar, A.F.; Kirkpatrick, S.I.; Mittl, B.; Zimmerman, T.P.; Thompson, F.E.; Bingley, C.; Willis, G.; Islam, N.G.; Baranowski, T.; McNutt, S.; et al. The Automated Self-Administered 24-Hour Dietary Recall (ASA24): A Resource for Researchers, Clinicians and Educators from the National Cancer Institute. J. Acad. Nutr. Diet. 2012, 112, 1134–1137. [Google Scholar] [CrossRef] [PubMed]
| Community-Wide Campaign Components | Target Socioecological Level [56] | Operationalization of Component to Promote Fruit and Vegetable (FV) Consumption and Physical Activity (PA) |
|---|---|---|
| Risk Factor Screening | Individual | Provision of free and accessible health risk screening in home and community locations for:
|
| Mass and Social Media | Individual, Interpersonal | Delivery of regularly scheduled health promoting messages tailored to local culture and language (social media, radio, TV, print, text messaging), including sharing stories of weight loss and new PA classes in the community, using behavioral journalism featuring local role models. |
| Social Support and Tailored Health Education | Individual, Interpersonal, Organizational, Community | Community-based groups tailored to local culture, language and identified health needs of community members including:
|
| Environmental Changes | Community, Policy | Physical improvements identified and implemented by the locations including:
|
| Policy Improvements | Policy | Regulation improvements by locations including:
|
| Variable | Low Exposure (n = 4639) | High Exposure (n = 1047) | p-Value a |
|---|---|---|---|
| Age, years, mean (SD) | 46.87 (14.06) | 48.62 (14.13) | 0.8298 |
| Female, n (%) | 3644 (77.49%) | 819 (78.22%) | 0.8156 |
| Have insurance,n (%) | 1862 (40.14%) | 512 (48.95%) | <0.0001 |
| Length of follow-up, months, median (IQR) | 2.3 (1.1, 5.1) | 6.6 (4.9, 9.3) | <0.0001 |
| Number of program strategies receivedb, median (IQR), [min, max] | 2 (1, 2) [1,7] | 2 (1, 3) [1,7] | 0.0035 |
| Below federal poverty level,n (%) | 3312 (84.22%) | 706 (76.58%) | <0.0001 |
| Meeting PA guideline at Baseline,n (%) | 1747 (37.89%) | 443 (43.95%) | 0.0004 |
| Meeting Fruit & Vegetable guideline at Baseline, n (%) | 952 (20.60%) | 281 (27.50%) | <0.0001 |
| Baseline MET-minutes, mean (SD) | 166.35 (215.57) | 306.33 (266.88) | <0.0001 |
| Baseline FV consumption servings/day, mean (SD) | 3.15 (2.06) | 3.38 (2.24) | 0.0015 |
| Independent Variables Column: | Change in Total FV Consumption from Baseline to the Last CHW Visit | Change in Total PA MET-Minutes from Baseline to the Last CHW Visit | ||||||
|---|---|---|---|---|---|---|---|---|
| Unadjusted a | Adjusted b | Unadjusted c | Adjusted d | |||||
| Mean Difference in Change (95% CI) | p-Value | Mean Difference in Change (95% CI) | p-Value | Mean Difference in Change (95% CI) | p-Value | Mean Difference in Change (95% CI) | p-Value | |
| Exposure high vs. low | 0.67 (0.56, 0.79) | <0.0001 | 0.65 (0.53, 0.77) | <0.0001 | 168.55 (87.90, 249.21) | <0.0001 | 185.62 (105.87, 265.37) | <0.0001 |
| Estimated Mean change (95% CI)from baseline to the last CHW visit in each group | Low: 0.63 (0.58, 0.67) High: 1.30 (1.20, 1.40) | Low: 0.73 (0.65, 0.80) High: 1.38 (1.26, 1.50) | Low: 138.14 | Low: 210.67 | ||||
| (106.45, 169.83) | (162.09, 259.26) | |||||||
| High: 306.69 | High: 396.29 | |||||||
| (234.67, 378.72) | (316.80, 475.79) | |||||||
| # program strategies received | 0.16 (0.12, 0.20) | <0.0001 | 147.77 (120.83, 174.72) | <0.0001 | ||||
| Age, year | 0.002 (−0.001, 0.005) | 0.1663 | −9.26 (−11.28, −7.25) | <0.0001 | ||||
| Sex female vs. male | −0.06 (−0.16, 0.04) | 0.2438 | −30.21 (−98.24, 37.82) | 0.3840 | ||||
| Have insurance yes vs. no | 0.39 (0.29, 0.49) | <0.0001 | 161.72 (95.14, 228.30) | <0.0001 | ||||
| Poverty status below vs. above FPL | 0.05 (−0.07, 0.18) | 0.3789 | −66.04 (−147.10, −15.02) | 0.1103 | ||||
| Independent Variables Column: | Meeting FV Guideline by Last CHW Visit (n = 4411) | Meeting PA Guideline by Last CHW Visit (n = 3429) | ||||||
|---|---|---|---|---|---|---|---|---|
| Unadjusted a | Adjusted b | Unadjusted c | Adjusted d | |||||
| Odds Ratio (95% CI) | p-Value | Odds Ratio (95% CI) | p-Value | Odds Ratio (95% CI) | p-value | Odds Ratio (95% CI) | p-Value | |
| Exposure high vs. low | 2.00 (1.64, 2.43) | <0.0001 | 2.02 (1.65, 2.47) | <0.0001 | 1.24 (1.10, 1.54) | 0.0393 | 1.36 (1.10, 1.68) | 0.0046 |
| # program strategies received | 1.30 (1.22, 1.39) | <0.0001 | 1.18 (1.10, 1.26) | <0.0001 | ||||
| Age, year | 1.00 (1.00, 1.01) | 0.2430 | 0.98 (0.97, 0.98) | <0.0001 | ||||
| Sex female vs. male | 1.18 (0.98, 1.42) | 0.0737 | 1.35 (1.12, 1.61) | 0.0014 | ||||
| Have insurance yes vs. no | 1.24 (1.04, 1.48) | 0.0151 | 1.36 (1.15, 1.63) | 0.0004 | ||||
| Poverty status below vs. above FPL | 1.02 (0.82, 1.26) | 0.8951 | 0.73 (0.59, 0.91) | 0.0005 | ||||
| Change in Total FV Consumption from Baseline to the Last CHW Visit a | |||||||
|---|---|---|---|---|---|---|---|
| Independent Variables Column: | City A (n = 1251) | Town A (n = 457) | Town B (n = 747) | Rural A (n = 702) | Rural B (n = 540) | Rural C (n = 467) | Rural D (n = 587) |
| Adjusted Mean Difference in Change and 95% Confidence Interval with p-Value | |||||||
| Exposure high vs. low | 0.63 (0.37, 0.88); p < 0.0001 | 1.45 (0.71, 2.19); p < 0.0001 | 0.62 (0.37, 0.88); p < 0.0001 | 0.63 (0.44, 0.83); p < 0.0001 | 0.71 (0.17, 1.24); p = 0.0097 | 0.74 (0.24, 1.26); p = 0.0041 | 0.44 (0.06, 0.82); p = 0.0242 |
| Estimated Mean change (95% CI)from baseline to the last CHW visit in each group | High: 1.28 (1.03, 1.53) | High: 2.13 (1.31, 2.95) | High: 1.15 (0.94, 1.36) | High: 1.37 (1.23, 1.50) | High: 1.62 (1.06, 2.18) | High: 2.20 (1.50, 2.91) | High: 0.99 (0.39, 1.59) |
| Low: 0.66 (0.48, 0.83) | Low: 0.68 (0.27, 1.09) | Low: 0.53 (0.40, 0.65) | Low: 0.73 (0.58, 0.89) | Low: 0.91 (0.61, 1.22) | Low: 1.45 (1.01, 1.90) | Low: 0.55 (0.03, 1.08) | |
| Meeting FV guideline at the last CHW visit b | |||||||
| City A (n = 708) | Town A (n = 304) | Town B (n = 422) | Rural A (n = 406) | Rural B (n = 307) | Rural C (n = 322) | Rural D (n = 432) | |
| Adjusted Odds Ratio and 95% confidence interval with p-value | |||||||
| Exposure high vs. low | 2.04 (1.41, 2.96); p = 0.0002 | 1.97 (0.77, 5.06); p = 0.1567 | 0.84 (0.38, 1.84); p = 0.6636 | 3.98 (2.19, 7.24); p < 0.0001 | 2.40 (1.20, 4.82); p = 0.0135 | 4.10 (1.36, 12.45); p = 0.0125 | 2.73 (0.94, 7.94); p = 0.0652 |
| Change in Total PA MET-minutes from baseline to the last CHW visit c | |||||||
| City A (n = 1251) | Town A (n = 456) | Town B (n = 747) | Rural A (n = 702) | Rural B (n = 540) | Rural C (n = 467) | Rural D (n = 587) | |
| Adjusted mean difference in change and 95% confidence interval with p-value | |||||||
| Exposure high vs. low | 38.55 (−102.20, 179.30); p = 0.5911 | 897.62 (541.05, 1254.19); p < 0.0001 | −171.11 (−345.97, 3.74); p = 0.0551 | 220.38 (65.05, 375.70); p = 0.0055 | −147.53 (−345.83, 50.76); p = 0.1445 | 290.94 (−55.44, 637.33); p = 0.0995 | 189.59 (−122.59, 501.65); p = 0.2333 |
| Estimated Mean change (95% CI)from baseline to the last CHW visit in each group | High: 34.64 (−104.02, 173.31) | High: 1409.83 (1031.81, 1787.85) | High: −122.60 (−308.31, 63.11) | High: 798.06 (692.83, 903.28) | High: 8.28 (−199.60, 216.16) | High: 586.94 (107.68, 1066.19) | High: −24.24 (−456.66, 408.15) |
| Low: −3.91 (−103.26, 95.45) | Low: 512.21 (350.98, 673.45) | Low: 48.52 (−42.99, 140.02) | Low: 577.68 (458.00, 697.35) | Low: 155.81 (42.09, 269.54) | Low: 295.99 (−5.86, 597.84) | Low: −213.82 (−706.87, 278.22) | |
| Meeting PA guideline at the last CHW visit d | |||||||
| City A (n = 1007) | Town A (n = 361) | Town B (n = 608) | Rural A (n = 445) | Rural B (n = 375) | Rural C (n = 375) | Rural D (n = 511) | |
| Adjusted Odds Ratio and 95% confidence interval with p-value | |||||||
| Exposure high vs. low | 1.15 (0.73, 1.82); p = 0.5382 | 3.84 (1.05, 13.95); p = 0.0414 | 1.38 (0.56, 3.39); p = 0.4903 | 2.42 (1.35, 4.32); p = 0.0029 | 1.00 (0.47, 2.10); p = 0.9923 | 5.41 (1.62, 18.08); p = 0.0061 | 1.14 (0.42, 3.08); p = 0.7933 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yeh, P.G.; Reininger, B.M.; Mitchell-Bennett, L.A.; Lee, M.; Xu, T.; Davé, A.C.; Park, S.K.; Ochoa-Del Toro, A.G. Evaluating the Dissemination and Implementation of a Community Health Worker-Based Community Wide Campaign to Improve Fruit and Vegetable Intake and Physical Activity among Latinos along the U.S.-Mexico Border. Int. J. Environ. Res. Public Health 2022, 19, 4514. https://doi.org/10.3390/ijerph19084514
Yeh PG, Reininger BM, Mitchell-Bennett LA, Lee M, Xu T, Davé AC, Park SK, Ochoa-Del Toro AG. Evaluating the Dissemination and Implementation of a Community Health Worker-Based Community Wide Campaign to Improve Fruit and Vegetable Intake and Physical Activity among Latinos along the U.S.-Mexico Border. International Journal of Environmental Research and Public Health. 2022; 19(8):4514. https://doi.org/10.3390/ijerph19084514
Chicago/Turabian StyleYeh, Paul Gerardo, Belinda M. Reininger, Lisa A. Mitchell-Bennett, Minjae Lee, Tianlin Xu, Amanda C. Davé, Soo Kyung Park, and Alma G. Ochoa-Del Toro. 2022. "Evaluating the Dissemination and Implementation of a Community Health Worker-Based Community Wide Campaign to Improve Fruit and Vegetable Intake and Physical Activity among Latinos along the U.S.-Mexico Border" International Journal of Environmental Research and Public Health 19, no. 8: 4514. https://doi.org/10.3390/ijerph19084514
APA StyleYeh, P. G., Reininger, B. M., Mitchell-Bennett, L. A., Lee, M., Xu, T., Davé, A. C., Park, S. K., & Ochoa-Del Toro, A. G. (2022). Evaluating the Dissemination and Implementation of a Community Health Worker-Based Community Wide Campaign to Improve Fruit and Vegetable Intake and Physical Activity among Latinos along the U.S.-Mexico Border. International Journal of Environmental Research and Public Health, 19(8), 4514. https://doi.org/10.3390/ijerph19084514






