Exercise Intervention Changes the Perceptions and Knowledge of Non-Communicable Disease Risk Factors among Women from a Low-Resourced Setting
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
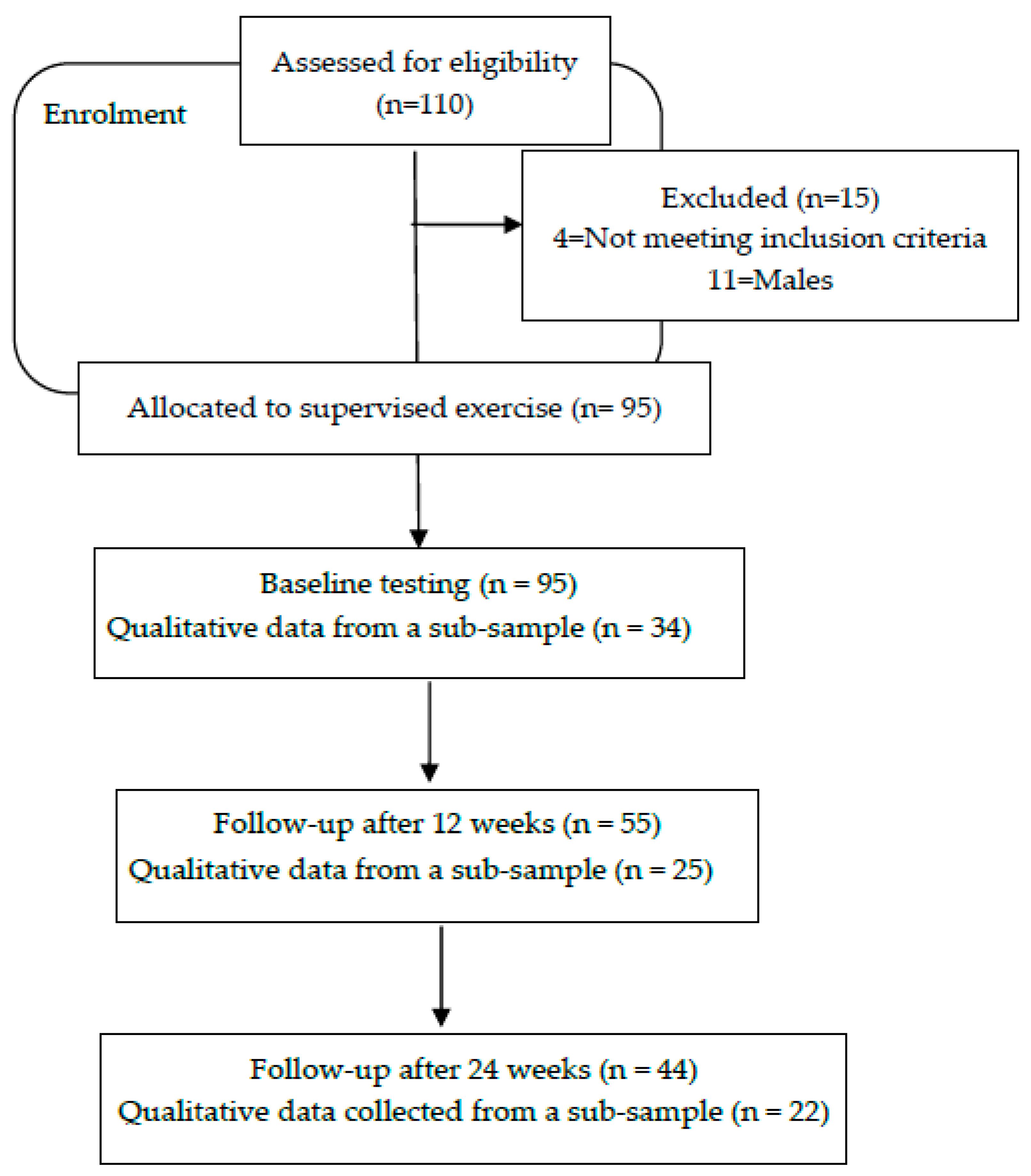
2.2. Population and Sampling
2.3. Supervised Exercise
2.4. Data Collection
2.4.1. Qualitative Data Collection
2.4.2. Quantitative Data Collection
2.5. Data Analysis
2.5.1. Qualitative Data Analysis
2.5.2. Quantitative Statistical Analysis
2.5.3. Mixed-Methods Analysis
2.6. Rigour
2.7. Ethical Considerations
3. Results
3.1. Characteristics of the Study Participants
3.2. Qualitative Findings
3.3. Quantitative Findings
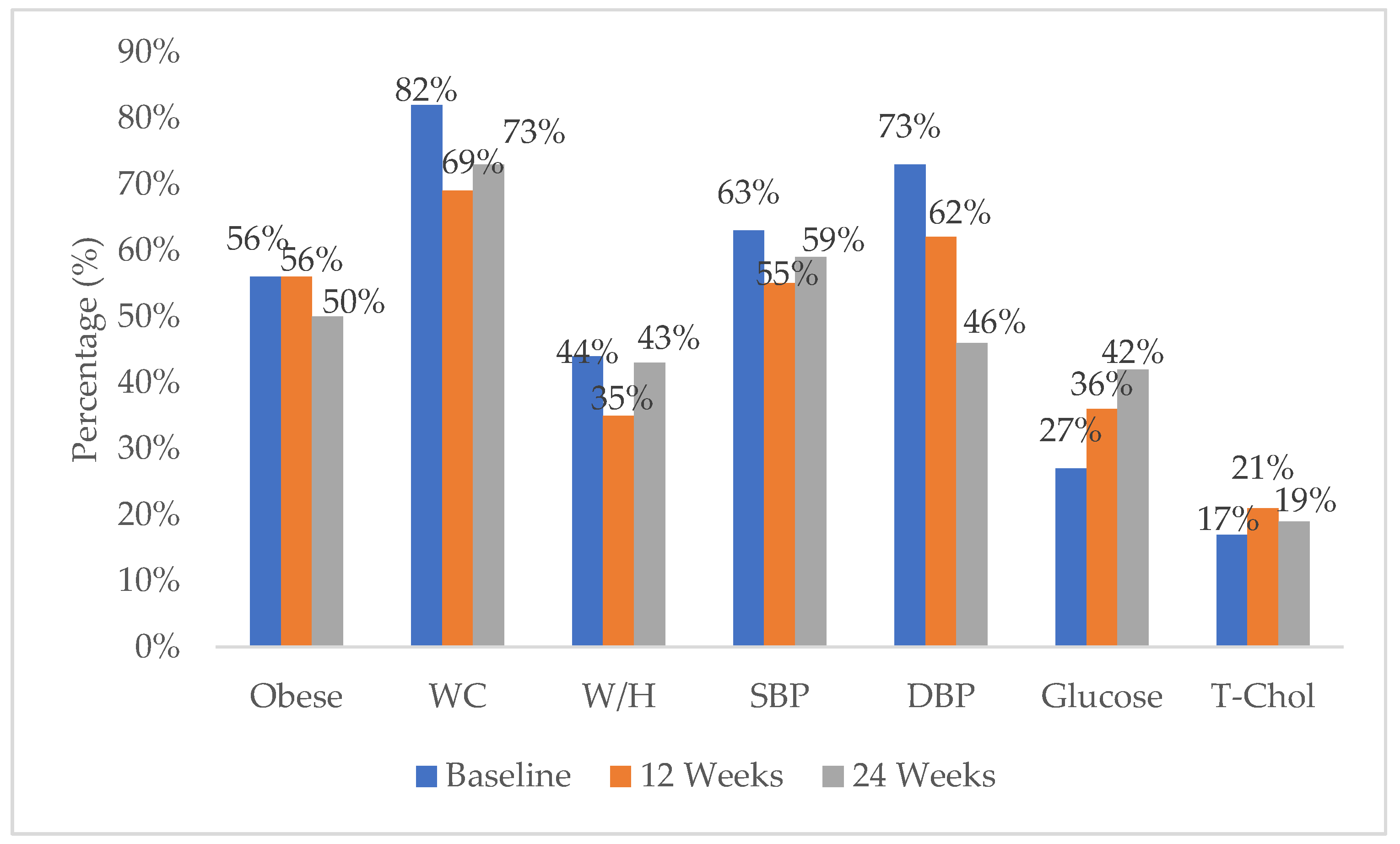
3.3.1. Prevalence of NCD Risk Factors
3.3.2. NCD Risk Factors over Time
3.3.3. Knowledge of Risk Factors for NCDs and PA
3.4. Mixed-Methods Findings
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Anderson, E.; Durstine, J.L. Physical activity, exercise, and chronic diseases: A brief review. Sports Med. Health Sci. 2019, 1, 3–10. [Google Scholar] [CrossRef]
- Guthold, R.; Stevens, G.A.; Riley, L.M.; Bull, F.C. Worldwide trends in insufficient physical activity from 2001 to 2016: A pooled analysis of 358 population-based surveys with 1.9 million participants. Lancet Glob. Health 2018, 6, 1077–1086. [Google Scholar] [CrossRef]
- Warburton, D.E.R.; Bredin, S.S.D. Reflections on Physical Activity and Health: What Should We Recommend? Can. J. Cardiol. 2016, 32, 495–504. [Google Scholar] [CrossRef] [PubMed]
- Scott, A.L.; Hu, W.; Rangarajan, S.; Gasevic, D.; Leong, D.; Iqbal, R.; Casanova, A.; Swaminathan, S.; Anjana, R.M.; Kumar, R.; et al. The effect of physical activity on mortality and cardiovascular disease in 130,000 people from 17 high-income, middle-income, and low-income countries: The PURE study. Lancet 2017, 390, 2643–2654. [Google Scholar]
- Puoane, T.R.; Tsolekile, L.P.; Caldbick, S.; Igumbor, E.U.; Meghnath, K.; Sanders, D. Chronic non-communicable diseases in South Africa: Progress and challenges. S. Afr. Health Rev. 2012, 2012, 115–126. [Google Scholar]
- World Health Organization (WHO). Global Status Report on Noncommunicable Diseases 2014; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- World Health Organization (WHO). Noncommunicable Diseases Country Profiles 2018; WHO: Geneva, Switzerland, 2018. [Google Scholar]
- World Health Organization (WHO). WHO Guidelines on Physical Activity and Sedentary Behaviour; WHO: Geneva, Switzerland, 2020. [Google Scholar]
- Cabral, M.; Martins, J.; Elias, C.; Nelas, R.; Rosa, V.; Sarmento, H.; Marques, A.; Nicola, P.J. Physical activity recommendations to benefit health:knowledge and perceptions among college students. Eur. J. Public Health 2018, 28, 290–296. [Google Scholar] [CrossRef]
- Berry, N.M.; Nolan, R.; Dollman, J. Associations of awareness of physical activity recommendations for health and self-reported physical activity behaviours among adult South Australians. J. Sci. Med. Sport 2016, 19, 837–842. [Google Scholar] [CrossRef]
- Fredriksson, S.V.; Alley, S.J.; Rebar, A.L.; Hayman, M.; Vandelanotte, C.; Schoeppe, S. How are different levels of knowledge about physical activity associated with physical activity behaviour in Australian adults? PLoS ONE 2018, 13, 0207003. [Google Scholar] [CrossRef]
- Botha, C.R.; Moss, S.J.; Kolbe-Alexander, T.L. “Be active!” Revisiting the South African food-based dietary guideline for activity. S. Afr. J. Clin. Nutr. 2013, 26, 18–27. [Google Scholar]
- Shisana, O.; Labadarios, D.; Rehle, T.; Simbayi, L.; Zuma, K.; Dhansay, A.; Reddy, P.; Parker, W.; Hoosain, E.; Naidoo, P.; et al. South African National Health and Nutrition Examination Survey, 2012 SANHANES-1, 2014 Edit; HSRC Press: Cape Town, South Africa, 2014. [Google Scholar]
- Oviedo, G.R.; Tamulevicius, N.; Onagbiye, S.O.; Phidza, M.; Sedumedi, C.; Cameron, M.; Moss, S.J. Quality of life, physical activity and cardiorespiratory fitness in black African women: B-Healthy project. Qual. Life Res. 2019, 29, 987–997. [Google Scholar] [CrossRef]
- Cois, A.; Day, C. Obesity trends and risk factors in the South African adult population. BMC Obes. 2015, 2, 42. [Google Scholar] [CrossRef] [PubMed]
- Okop, K.; Mukumbang, F.C.; Mathole, T.; Levitt, N.; Puoane, T. Perceptions of body size, obesity threat and the willingness to lose weight among black South African adults: A qualitative study. BMC Public Health 2016, 16, 365. [Google Scholar] [CrossRef] [PubMed]
- E Draper, C.; Davidowitz, K.J.; Goedecke, J.H. Perceptions relating to body size, weight loss and weight-loss interventions in black South African women: A qualitative study. Public Health Nutr. 2016, 19, 548–556. [Google Scholar] [CrossRef]
- Hui, S.S.-C.; Hui, G.P.-S.; Xie, Y.J. Association between Physical Activity Knowledge and Levels of Physical Activity in Chinese Adults with Type 2 Diabetes. PLoS ONE 2014, 9, 115098. [Google Scholar] [CrossRef] [PubMed]
- Loock, H.V.; Wilders, C.J.; Strydom, G.L.; Ellis, S.M. Leisure time physical activity participation in women (30–65 years) with high coronary heart disease risk indicators: Physical activity and fitness. Afr. J. Phys. Health Educ. Recreat. Danc. 2011, 17, 624–635. [Google Scholar]
- Makamu, S.J. Perceptions and Knowledge of Black Africans on Physical Activity and Non-Communicable Diseases. Ph.D. Thesis, North-West University, Potchefstroom, South Africa, 2015. [Google Scholar]
- Kaba, Z.; Khamisa, N.; Tshuma, N. Age-group differences in risk perceptions of non-communicable diseases among adults in Diepsloot township, Johannesburg, South Africa: A cross-sectional study based on the Health Belief Model. S. Afr. Med. J. 2017, 107, 797–804. [Google Scholar] [CrossRef] [PubMed]
- Onagbiye, S.O.; Tshwaro, R.M.T.; Barry, A.; Marie, Y. Physical Activity and Non-communicable Disease Risk Factors: Knowledge and Perceptions of Youth in a Low Resourced Community in the Western Cape. Open Public Health J. 2019, 12, 558–566. [Google Scholar] [CrossRef]
- Bateman, L.B.; Hall, A.G.; Anderson, W.A.; Cherrington, A.L.; Helova, A.; Judd, S.; Kimberly, R.; Oates, G.R.; Osborne, T.; Ott, C.; et al. Exploring COVID-19 Vaccine Hesitancy Among Stakeholders in African American and Latinx Communities in the Deep South Through the Lens of the Health Belief Model. Am. J. Health Promot. 2021, 36, 288–295. [Google Scholar] [CrossRef]
- Rosenstock, I.M. Historical Origins of the Health Belief Model. Health Educ. Monogr. 1974, 2, 328–335. [Google Scholar] [CrossRef]
- Rosenstock, I.M.; Strecher, V.J.; Becker, M.H. Social Learning Theory and the Health Belief Model. Health Educ. Q. 1988, 15, 175–183. [Google Scholar] [CrossRef]
- Creswell, J.W.; Fetters, M.D.; Ivankova, N.V. Designing A Mixed Methods Study in Primary Care. Ann. Fam. Med. 2004, 2, 7–12. [Google Scholar] [CrossRef] [PubMed]
- Punch, K.; Oancea, A. Mixed Methods Research. In Introduction to Research Methods in Education, 2nd ed.; SAGE Publications Ltd.: Thousand Oaks, CA, USA, 2014; p. 398. [Google Scholar]
- Adams, R. Revised Physical Activity Readiness Questionnaire. Can. Fam. Physician 1999, 45, 992, 995, 1004, 1005. [Google Scholar] [PubMed]
- Pescatello, L.S.; Riebe, D.; Thompson, P.D. (Eds.) American college of sports medicine. In ACSM’s Guidelines for Exercise Testing and Prescription, 9th ed.; Lippincott Williams & Wilkins: Baltimore, MD, USA, 2014. [Google Scholar]
- Onagbiye, S.O.; Moss, S.J.; Cameron, M. Managing noncommunicable diseases in an African community: Effects, compliance, and barriers to participation in a 4-week exercise intervention. Int. Q. Community Health Educ. 2016, 36, 165–176. [Google Scholar] [CrossRef] [PubMed]
- Government Gazette 16021. Regulations defining the scope of profession of biokinetics. In Notice R17469; Government Press: Pretoria, South Africa, 1994; p. 3. [Google Scholar]
- Borg, G. Borg’s Perceived Exertion and Pain Scales; Human Kinetics Publishers: Champaign, IL, USA, 1998. [Google Scholar]
- Marfell-Jones, M.J.; Stewart, A.D.; De Ridder, J.H. International Standards for Anthropometric Assessment; International Society for the Advancement of Kinanthropometry: Wellington, New Zealand, 2012. [Google Scholar]
- ROCHE Diagnostics. Accutrend ® Plus User’s Manual; Roche Diagnostics GmbH: Mannheim, Germany, 2012; p. 120. [Google Scholar]
- CamNTech Ltd. The Actiheart User Manual No. 20; CamNtecch Ltd.: Fenstanton, Cambridgeshire, UK, 2020; pp. 1–101. [Google Scholar]
- Bergman, H.E.; Reeve, B.B.; Moser, R.P.; Scholl, S.; Klein, W.M. Development of a comprehensive heart disease knowledge questionnaire. Am. J. Health Educ. 2011, 42, 74–87. [Google Scholar] [CrossRef][Green Version]
- Pienaar, P.; De Swardt, M.; De Vries, M.; Roos, H.; Joubert, G. Physical activity knowledge, attitudes and practices of the elderly in Bloemfontein old age homes. S. Afr. Fam. Pract. 2004, 46, 17–19. [Google Scholar] [CrossRef]
- Elo, S.; Kyngäs, H. The qualitative content analysis process. J. Adv. Nurs. 2008, 62, 107–115. [Google Scholar] [CrossRef]
- Seidel, J.V. Appendix E: Qualitative Data Analysis QDA: A Model of the Process Noticing, Collecting, Thinking about Things. 1998, pp. 1–15. Available online: http://www.qualisresearch.com/DownLoads/qda.pdf (accessed on 22 February 2022).
- ATLAS. Ti Scientific Software Development GmbH, “ATLAS. Ti.”; Scientific Software Development GmbH: Berlin, Germany, 2015. [Google Scholar]
- Morse, J.M. The Significance of Saturation. Qual. Health Res. 1995, 5, 147–149. [Google Scholar] [CrossRef]
- Creswell, J.W.; Clark, V.L.P. Designing and Conducting Mixed METHODS Research, 2nd ed.; Sage Publications: Los Angeles, CA, USA, 2011. [Google Scholar]
- Krueger, R.A.; Casey, M. Focus Groups: A Practical Guide for Applied Research, 5th ed.; Sage: Thousand Oaks, CA, USA, 2015. [Google Scholar]
- Kidd, P.S.; Parshall, M.B. Getting the focus and the group: Enhancing analytical rigor in focus group research. Qual. Health Res. 2000, 10, 293–308. [Google Scholar] [CrossRef]
- Amankwaa, L. Creating protocols for trustworthiness in qualitative research. J. Cult. Divers. 2016, 23, 121–127. [Google Scholar]
- Cyr, J. The Pitfalls and Promise of Focus Groups as a Data Collection Method. Sociol. Methods Res. 2015, 45, 231–259. [Google Scholar] [CrossRef]
- World Medical Association. Ethical principles for medical research involving human subjects: World medical association declaration of Helsinki. J. Am. Med. Assoc. 2013, 310, 2191–2194. [Google Scholar] [CrossRef] [PubMed]
- Becker, M.H.; Drachman, R.H.; Kirscht, J.P. A new approach to explaining sick-role behavior in low-income populations. Am. J. Public Health 1974, 64, 205–216. [Google Scholar] [CrossRef] [PubMed]
- Boateng, D.; Wekesah, F.; Browne, J.L.; Agyemang, C.; Agyei-Baffour, P.; Aikins, A.D.-G.; Smit, H.A.; Grobbee, D.E.; Klipstein-Grobusch, K. Knowledge and awareness of and perception towards cardiovascular disease risk in sub-Saharan Africa: A systematic review. PLoS ONE 2017, 12, 0189264. [Google Scholar] [CrossRef] [PubMed]
- Surka, S.; Steyn, K.; Everett-Murphy, K.; Gaziano, T.A.; Levitt, N. Knowledge and perceptions of risk for cardiovascular disease: Findings of a qualitative investigation from a low-income peri-urban community in the Western Cape, South Africa. Afr. J. Prim. Health Care Fam. Med. 2015, 7, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Sallis, R. Exercise is medicine: A call to action for physicians to assess and prescribe exercise. Physician Sportsmed. 2015, 43, 22–26. [Google Scholar] [CrossRef]
- Devanathan, R.; Esterhuizen, T.M.; Govender, R.D. Overweight and obesity amongst Black women in Durban, KwaZulu-Natal: A’disease’of perception in an area of high HIV prevalence. Afr. J. Prim. Health Care Fam. Med. 2013, 5, 1–7. [Google Scholar] [CrossRef]
- Hamer, M.; Bruwer, E.J.; De Ridder, J.H.; Swanepoel, M.; Kengne, A.P.; Cockeran, M.; Malan, L. The association between seven-day objectively measured habitual physical activity and 24 h ambulatory blood pressure: The SABPA study. J. Hum. Hypertens. 2017, 31, 409–414. [Google Scholar] [CrossRef]
- Moss, S.J.; Onagbiye, S.O.; Cameron, M. Preferred physical activity among Setswana-speaking community-dwelling adults in Potchefstroom. S. Afr. J. Res. Sport Phys. Educ. Recreat. 2017, 39, 97–110. [Google Scholar]
- Silva, K.S.; Garcia, L.M.T.; Rabacow, F.M.; de Rezende, L.F.M.; de Sá, T.H. Physical activity as part of daily living: Moving beyond quantitative recommendations. Prev. Med. 2017, 96, 160–162. [Google Scholar] [CrossRef]
- Smit, W.; de Lannoy, A.; Dover, R.V.H.; Lambert, E.V.; Levitt, N.; Watson, V. Making unhealthy places: The built environment and non-communicable diseases in Khayelitsha, Cape Town. Health Place 2016, 39, 196–203. [Google Scholar] [CrossRef]
- Sehole, M.D.B.; Van Der Heever, H. Changing behaviour of people living with non-communicable diseases in Hammanskraal, South Africa. Afr. J. Phys. Act. Health Sci. 2017, 2017, 93–105. [Google Scholar]
- Dorman, J.S.; Valdez, R.; Liu, T.; Wang, C.; Rubinstein, W.S.; O’Neill, S.M.; Acheson, L.S.; Ruffin, M.T.; Khoury, M.J. Health beliefs among individuals at increased familial risk for type 2 diabetes: Implications for prevention. Diabetes Res. Clin. Pract. 2012, 96, 156–162. [Google Scholar] [CrossRef] [PubMed]
- Hay-Smith, E.; McClurg, D.; Frawley, H.C.; Dean, S. Exercise adherence: Integrating theory, evidence and behaviour change techniques. Physiotherapy 2016, 102, 7–9. [Google Scholar] [CrossRef] [PubMed]
| Variable | Number (%) |
|---|---|
| Socio-economic variables | |
| Highest level of education: | |
| No schooling | 35% |
| High school | 61% |
| Diploma | 3% |
| Employment status | |
| Employed | 17% |
| Unemployed | 59% |
| Unable to work or retired | 24% |
| Marital status | |
| Married | 39% |
| Single | 38% |
| Widowed | 21% |
| Persons in household | |
| 1–3 | 33% |
| 4–6 | 54% |
| >6 | 14% |
| Household income | |
| Less than R100,000 | 83% |
| R100,000–R250,000 | 9% |
| R250,000–R400,000 | 8% |
| Theme | Category | Sub-Category | Quotation |
|---|---|---|---|
| Baseline | |||
| Individual perceptions | Increased risk | Genetics | Participant D3_01: “You get NCDs among relatives who stay together in the same house; you can’t prevent NCDs as they are hereditary” |
| Modifying factors | Knowledge of NCDs | Lack of knowledge about NCDs | Participant D3_01: “I don’t understand diabetes. Isn’t diabetes caused by the lack of vitamins in the body?” |
| Knowledge of PA | Lack of knowledge about PA | Participant D1_01: “I don’t know what other push-ups there are” | |
| Likelihood of action | Benefits of PA | PA lowers fat in the heart | Participant D2_01: “PA makes your heart not to be full of fat” |
| Barriers to PA | Fear of injury | Participant D1_01: “On the TV grannies that play soccer, I always saw them; they kick the ball and score. I’m ‘oh my God, I wish I was also there’. So now [I am] here because my knees are so painful, looks like they will break” | |
| 12 weeks | |||
| Individual perceptions | Increased risk | Modern diet | Participant D6_01: “Milo, fruit and wild berries were like medicine. When we stopped eating those things, we started having high blood pressure and diabetes” |
| Seriousness of NCDs | Disease complications | Participant D6_01: “When you have hurt your leg and have a sore, it doesn’t heal; you will go to amputate the leg. That is what I understand about diabetes” | |
| Modifying factors | Knowledge of NCDs | Personal diagnoses | Participant D8_01: “I was told I have heart failure at the hospital” |
| Knowledge of PA | Brisk walking | Participant D8_01: I was pacing every morning as the doctor had instructed. When I went for the check-up, the doctor said my heart is fine” | |
| Cues to action | Encouragement from medical professionals | Participant D6_01: The doctor spoke that we should keep on gyming because our diabetes is fine” | |
| Likelihood of action | Benefits of PA | Enjoyment | Participant D5_03: “The exercise group is fun; it helps with something” |
| 24 weeks | |||
| Individual perceptions | Increased risk | Modern diet | Participant D10_01: “The food we eat these days causes us to be prone to NCDs” |
| Seriousness of NCDs | NCDs are life threatening | Participant D12_01: “NCDs are dangerous diseases. When you have any NCD, you know your life is in danger” | |
| Modifying factors | Knowledge of NCDs | Lack of knowledge about NCD risk factors | Participant D10_01: “I don’t know what diabetes is, but I was told I have a disease called diabetes, they said what kind of food we should eat” |
| Knowledge about PA | Exercise group encourages capacity building | Participant D12_01: “My husband leaves at 5 am to go to work. When he leaves, I get up from the blankets, go to the sitting room and do the exercises we do in the exercise group” | |
| Cues to action | Awareness through media | Participant D9_01: “I heard on the radio they said eating and sitting and a child that does not play, watching TV the whole day, gets kidney disease and diabetes” | |
| Likelihood of action | Benefits of PA | Disease control | Participant D11_01: “When you are active, high blood pressure becomes level” |
| NCD Risk Factor | N | Baseline M ± SD | 12 Weeks M ± SD | 24 Weeks M ± SD | p | |
|---|---|---|---|---|---|---|
| Weight (kg) | 41 | 76.2 ± 19.2 | 75.4 ± 19.6 | 74.9 ± 19.8 | 0.03 | 0.09 |
| BMI (kg/m2) | 41 | 32 ± 7.8 | 31 ± 7.9 | 31 ± 7.8 | <0.001 | 0.18 |
| Waist (cm) | 41 | 92.7 ± 13.33 | 88.6 ± 12.99 | 89.9 ± 13.04 | <0.001 | 0.23 |
| W/H ratio | 41 | 0.87 ± 0.92 | 0.83 ± 0.76 | 0.84 ± 0.67 | <0.001 | 0.23 |
| SBP (mmHg) | 41 | 140 ± 16 | 133 ± 13 | 135 ± 13 | 0.08 | 0.06 |
| DBP (mmHg) | 41 | 85 ± 13 | 82 ± 11 | 80 ± 11 | 0.02 | 0.09 |
| Glucose (mmol/L) | 37 | 5.0 [1.2–12.3] | 6.3 [1.6–21.5] | 5.7 [2.9–15.0] | 0.09 | 0.06 |
| T-chol (mmol/L) | 37 | 4.1 ± 1.3 | 4.2 ± 9.6 | 3.9 ± 1.3 | 0.21 | 0.04 |
| PAL | 27 | 1.40 ± 0.19 | 1.55 ± 0.53 | 1.45 ± 0.24 | 0.79 | 0.01 |
| Activity (counts/min) | 27 | 19.73 ± 13.26 | 20.65 ± 8.54 | 17.69 ± 11.40 | 0.17 | 0.07 |
| AEE (kcal/week) | 27 | 448.44 [31.00–2219.00] | 503.47 [23.00–3439.00] | 421.05 [1.00–1075] | 0.86 | 0.04 |
| MVPA (min/day) | 27 | 43.97 [0–437.0] | 57.24 [0–757.0] | 44.84 [0–175.0] | 0.35 | 0.04 |
| ActiHeart® (days worn) | 27 | 6 ± 1 | 6 ± 1 | 6 ± 2 | 0.37 | 1.00 |
| Heart disease knowledge (n) | 40 | 12 [2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20] | 14 [2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19] | 14 [7,8,9,10,11,12,13,14,15,16,17,18,19,20] | <0.001 | 0.18 |
| Physical activity knowledge (n) | 40 | 9 [5,6,7,8,9,10] | 9 [6,7,8,9,10] | 9 [6,7,8,9,10] | 0.01 | 0.12 |
| Survey Questions | Baseline (n = 95) n (%) | 12 Weeks (n = 55) n (%) | 24 Weeks (n = 43) n (%) |
|---|---|---|---|
| Polyunsaturated fats are healthier for the heart than saturated fats. | 21 (22) | 35 (64) | 18 (42) |
| Women are less likely to get heart disease after menopause than before. | 10 (11) | 18 (33) | 14 (33) |
| Having had chickenpox increases the risk of getting heart disease. | 24 (25) | 13 (24) | 21 (49) |
| Eating a lot of red meat increases heart disease risk. | 50 (53) | 35 (64) | 28 (65) |
| Most people can tell whether or not they have high blood pressure. | 31 (33) | 9 (16) | 16 (37) |
| Trans-fats are healthier for the heart than most other kinds of fats. | 12 (13) | 4 (7) | 4 (9) |
| The most important cause of heart attacks is stress. | 4 (4) | 2 (4) | 1 (2) |
| Walking and gardening are considered types of exercise that can lower heart disease risk. | 87 (92) | 55 (100) | 40 (93) |
| Most of the cholesterol in an egg is in the white part of the egg. | 23 (24) | 28 (51) | 11 (26) |
| Smokers are more likely to die of lung cancer than heart disease. | 5 (5) | 4 (7) | 1 (2) |
| Taking an aspirin each day decreases the risk of getting heart disease. | 44 (46) | 16 (30) | 29 (67) |
| Dietary fibre lowers blood cholesterol. | 66 (70) | 52 (95) | 27 (63) |
| Heart disease is the leading cause of death in the United States. | 64 (67) | 32 (58) | 27 (63) |
| The healthiest exercise for the heart involves rapid breathing for a sustained period. | 56 (60) | 26 (47) | 17 (40) |
| Turning pale or grey is a symptom of having a heart attack. | 32 (34) | 21 (38) | 24 (56) |
| A healthy person′s pulse should return to normal within 15 min after exercise. | 59 (62) | 35 (64) | 27 (63) |
| Sudden trouble seeing in one eye is a common symptom of heart attack. | 39 (41) | 64 (35) | 25 (58) |
| Cardiopulmonary resuscitation (CPR) helps to clear clogged blood vessels. | 7 (7) | 19 (16) | 9 (21) |
| HDL refers to “good” cholesterol, and LDL refers to “bad” cholesterol. | 43 (45) | 11 (20) | 11 (26) |
| Arterial defibrillation is a procedure where hardened arteries are opened to increase blood flow. | 10 (11) | 5 (9) | 7 (16) |
| Feeling weak, lightheaded, or faint is a common symptom of having a heart attack. | 47 (50) | 29 (53) | 25 (58) |
| Taller people are more at risk of getting heart disease. | 47 (50) | 35 (64) | 28 (65) |
| “High” blood pressure is defined as 110/80 (systolic/diastolic) or higher. | 32 (34) | 19 (35) | 24 (56) |
| Most women are more likely to die from breast cancer than heart disease. | 4 (4) | 5 (9) | 9 (21) |
| Margarine with liquid safflower oil is healthier than margarine with hydrogenated soy oil. | 38 (40) | 38 (69) | 24 (56) |
| People who have diabetes are at higher risk of getting heart disease. | 64 (67) | 47 (86) | 26 (61) |
| Men and women experience many of the same symptoms of a heart attack. | 44 (46) | 31 (56) | 26 (61) |
| Eating a high fibre diet increases the risk of getting heart disease. | 34 (36) | 41 (75) | 26 (61) |
| Heart disease is better defined as a short-term illness than a chronic, long-term illness. | 36 (38) | 39 (71) | 24 (56) |
| Many vegetables are high in cholesterol. | 75 (79) | 50 (91) | 30 (70) |
| Tot Average percentage of correct scores | 39% | 45% | 47% |
| Item | Baseline (n = 95) n (%) | 12 Weeks (n = 55) n (%) | 24 Weeks (n = 43) n (%) |
|---|---|---|---|
| Physical activity is only suitable for some individuals, e.g., elite sports people/young people/Caucasians | 59 (62) | 46 (84) | 24 (56) |
| Exercise reduces high blood glucose (sugar) levels/diabetic complications | 58 (61) | 52 (95) | 42 (98) |
| Physical activity of moderate intensity at least five times a week has positive effects on health | 90 (95) | 55 (100) | 40 (93) |
| Exercise decreases physical dependence | 66 (70) | 49 (89) | 37 (86) |
| Thirty minutes of physical activity everyday supports weight loss | 84 (88) | 51 (93) | 39 (91) |
| Physical activity is good for your blood pressure no matter your age, weight, race, or gender | 90 (95) | 52 (93) | 39 (91) |
| Physical activity causes/worsens pain | 75 (79) | 48 (87) | 39 (91) |
| Exercise contributes to cholesterol control | 90 (95) | 53 (96) | 43 (100) |
| Physical activity contributes to a better state of mind | 92 (97) | 55 (100) | 43 (100) |
| Physical activity improves health and general wellbeing | 93 (98) | 55 (100) | 43 (100) |
| The average percentage of correct scores | 87% | 94% | 91% |
| Health Belief Model Constructs | Integrated Qualitative and Quantitative Results |
|---|---|
| Baseline | |
| Individual perceptions | Qualitative and quantitative data analyses show that participants’ perceptions of NCDs correspond with measured knowledge of NCD risk. Participants perceive increased risk to NCDs to be related only to non-modifiable risk factors. Scores on heart disease knowledge were lowest on medical and risk factors. |
| Modifying factors | NCD risk factors are prevalent among participants; however, participants demonstrate a lack of knowledge about NCDs risk factors. Although good knowledge of PA, participants perceive a lack of knowledge about types of PA. |
| Likelihood of action | Perceived benefits of PA include a reduction in fat in the heart. Participants mainly engaged in low-intensity PA, which may be related to the perceived fear of injury, a barrier to PA. |
| 12 Weeks | |
| Individual perceptions | Participants perceived increased risk of NCDs because of dietary changes from previous generations. Participants were generally knowledgeable about dietary risk factors for heart disease. Referring to disease complications, participants perceived that NCDs are serious conditions. |
| Modifying factors | A significant decrease in some NCD risk factors was coupled with improvements in heart disease knowledge. Participants reported knowledge of NCDs through personal diagnoses by medical professionals. Participants had more knowledge about PA. Medical professionals raised awareness for PA engagement. Participants knew about readily accessible forms of PA. |
| Likelihood of action | The enjoyment of PA was perceived to be a benefit of PA. In particular, PA engagement within a group. Objective PA measurements show that time spent in PA improved. Participants did not perceive any barriers to PA engagement. Surprisingly, they were not knowledgeable about the benefits of PA in NCD management. |
| 24 Weeks | |
| Individual perceptions | Participants perceived that the modern diet increases the risk of NCDs, and NCDs are serious conditions because they are life threatening. |
| Modifying factors | Participants show improvements in heart disease knowledge. On the other hand, they perceive a lack of knowledge about NCDs, though they are aware of the disease conditions through personal diagnoses. There were significant decreases in most NCD risk factors from baseline, including BMI and diastolic BP. Media campaigns raised awareness of the connection between PA and NCDs. PA knowledge improvements were seen. Participants had experiential knowledge of the types of exercises they could do. |
| Likelihood of action | Perceived benefits of PA included disease management. Participants did not perceive barriers to PA. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Makamu-Beteck, S.J.; Moss, S.J.; Watson, F.G.; Cameron, M. Exercise Intervention Changes the Perceptions and Knowledge of Non-Communicable Disease Risk Factors among Women from a Low-Resourced Setting. Int. J. Environ. Res. Public Health 2022, 19, 3474. https://doi.org/10.3390/ijerph19063474
Makamu-Beteck SJ, Moss SJ, Watson FG, Cameron M. Exercise Intervention Changes the Perceptions and Knowledge of Non-Communicable Disease Risk Factors among Women from a Low-Resourced Setting. International Journal of Environmental Research and Public Health. 2022; 19(6):3474. https://doi.org/10.3390/ijerph19063474
Chicago/Turabian StyleMakamu-Beteck, Sweetness Jabulile, Sarah Johannah Moss, Francois Gerald Watson, and Melainie Cameron. 2022. "Exercise Intervention Changes the Perceptions and Knowledge of Non-Communicable Disease Risk Factors among Women from a Low-Resourced Setting" International Journal of Environmental Research and Public Health 19, no. 6: 3474. https://doi.org/10.3390/ijerph19063474
APA StyleMakamu-Beteck, S. J., Moss, S. J., Watson, F. G., & Cameron, M. (2022). Exercise Intervention Changes the Perceptions and Knowledge of Non-Communicable Disease Risk Factors among Women from a Low-Resourced Setting. International Journal of Environmental Research and Public Health, 19(6), 3474. https://doi.org/10.3390/ijerph19063474







