The Mediating Role of Resilience and Life Satisfaction in the Relationship between Stress and Burnout in Medical Students during the COVID-19 Pandemic
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Survey Questionnaire
2.3. Statistical Analysis
3. Results
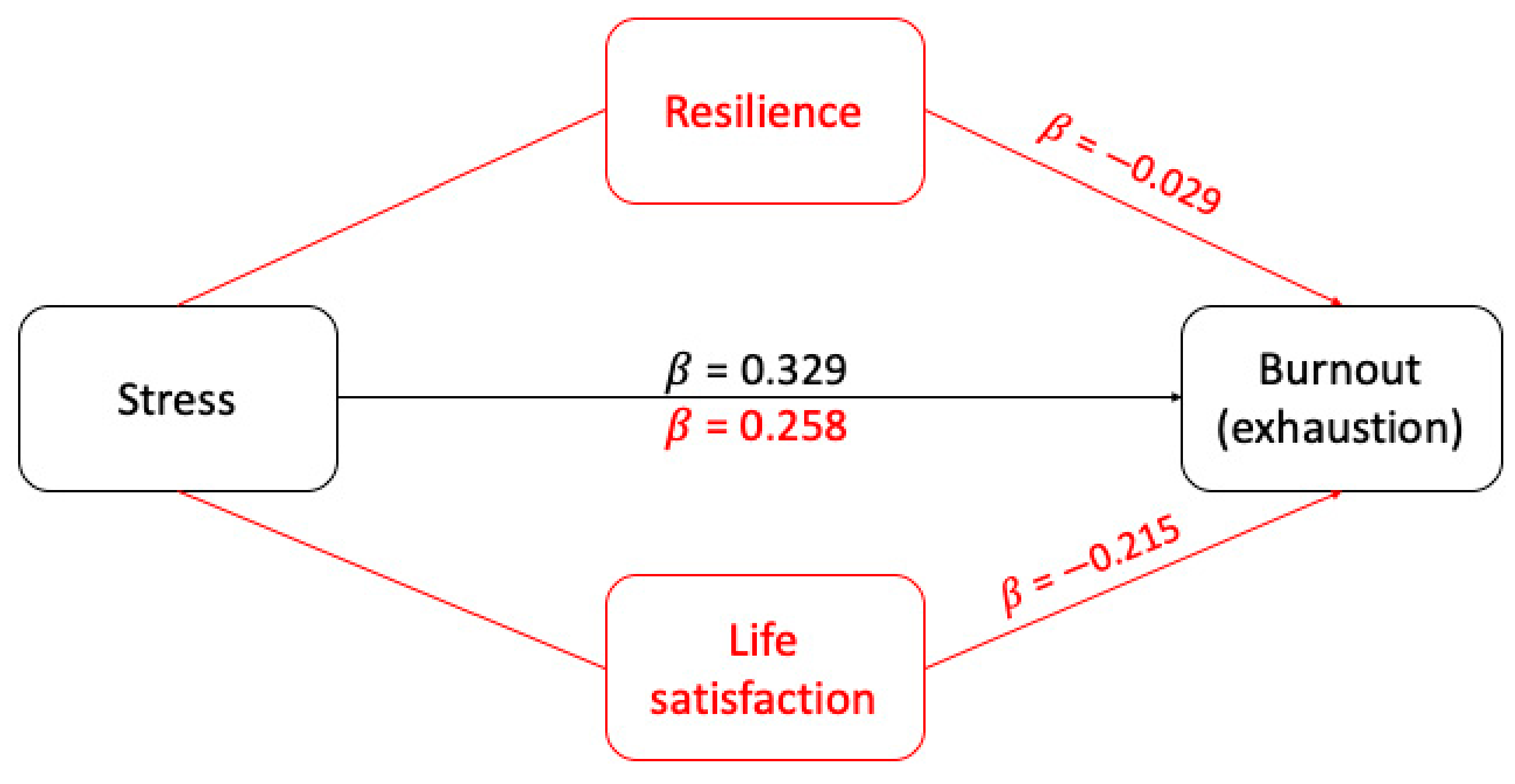
3.1. The Mediating Effect of Resilience and Life Satisfaction on the Relationship between Stress and Exhaustion Burnout
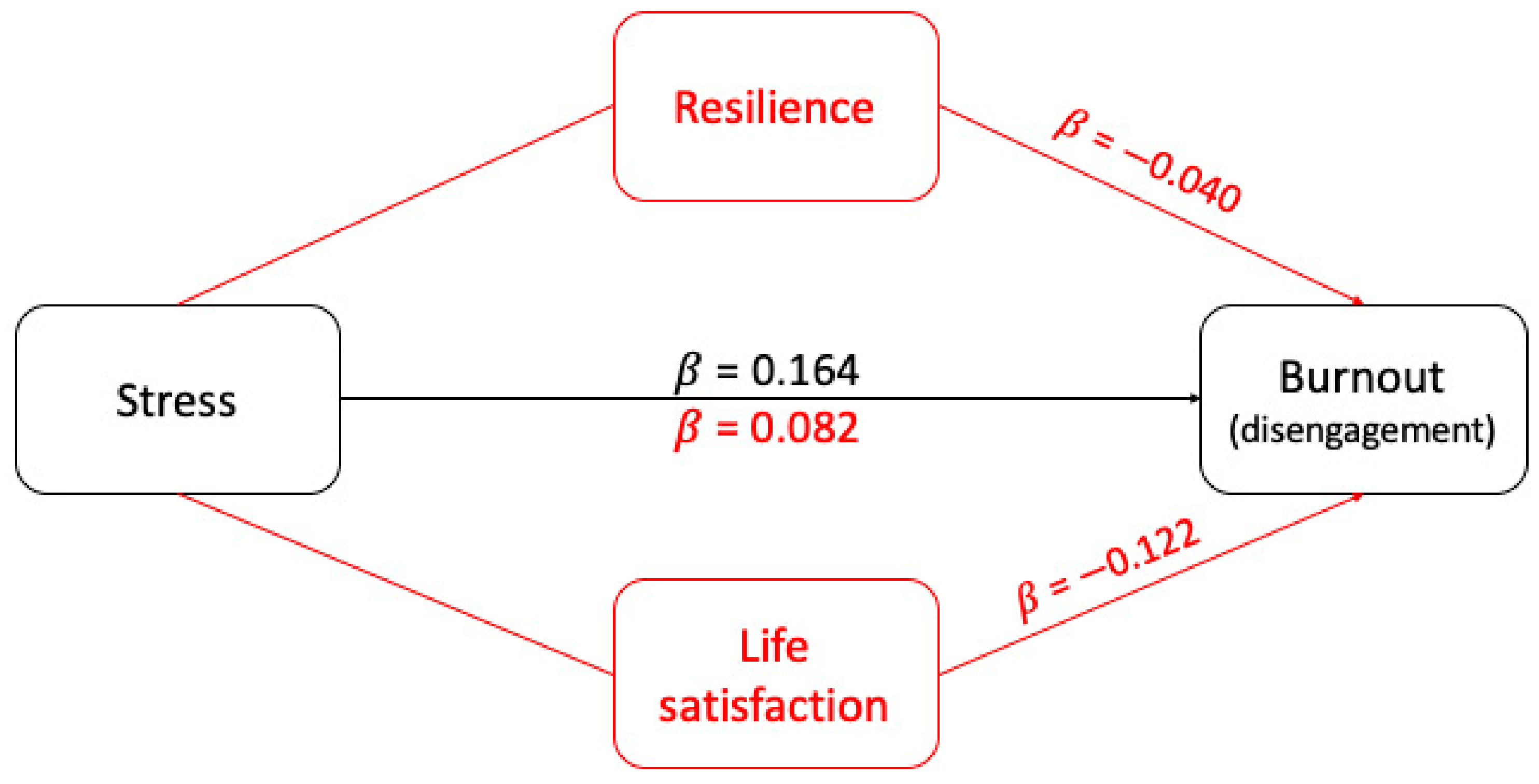
3.2. Mediating Effect of Resilience and Life Satisfaction on the Relationship between Stress and Disengagement Burnout
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chahrour, M.; Assi, S.; Bejjani, M.; Nasrallah, A.A.; Salhab, H.; Fares, M.Y.; Khachfe, H.H. A Bibliometric Analysis of COVID-19 Research Activity: A Call for Increased Output. Cureus 2020, 12, e7357. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Coronavirus Disease (COVID-19) Pandemic. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 5 April 2021).
- Ozamiz-Etxebarria, N.; Idoiaga Mondragon, N.; Dosil Santamaría, M.; Picaza Gorrotxategi, M. Psychological Symptoms During the Two Stages of Lockdown in Response to the COVID-19 Outbreak: An Investigation in a Sample of Citizens in Northern Spain. Front. Psychol. 2020, 11, 1491. [Google Scholar] [CrossRef]
- Miguel, C.; Castro, L.; Santos, J.P.M.; Serrão, C.; Duarte, I. Impact of COVID-19 on medicine lecturers’ mental health and emergency remote teaching challenges. Int. J. Environ. Res. Public Health 2021, 18, 6792. [Google Scholar] [CrossRef] [PubMed]
- Zis, P.; Artemiadis, A.; Bargiotas, P.; Nteveros, A.; Hadjigeorgiou, G.M. Medical studies during the COVID-19 pandemic: The impact of digital learning on burnout and mental health. Int. J. Environ. Res. Public Health 2021, 18, 349. [Google Scholar] [CrossRef] [PubMed]
- Lyons, Z.; Wilcox, H.; Leung, L.; Dearsley, O. COVID-19 and the mental well-being of Australian medical students: Impact, concerns and coping strategies used. Australas. Psychiatry 2020, 28, 649–652. [Google Scholar] [CrossRef]
- Moffat, K.J.; McConnachie, A.; Ross, S.; Morrison, J.M. First-year medical student stress and coping in a problem-based learning medical curriculum. Med. Educ. 2004, 38, 482–491. [Google Scholar] [CrossRef]
- McGuire, F.L. Psycho-social studies of medical students. Acad. Med. 1966, 41, 424–445. [Google Scholar] [CrossRef] [PubMed]
- Voltmer, E.; Kötter, T.; Spahn, C. Perceived medical school stress and the development of behavior and experience patterns in German medical students. Med. Teach. 2012, 34, 840–847. [Google Scholar] [CrossRef]
- Hope, V.; Henderson, M. Medical student depression, anxiety and distress outside North America: A systematic review. Med. Educ. 2014, 48, 963–979. [Google Scholar] [CrossRef] [PubMed]
- Schwenk, T.L.; Davis, L.; Wimsatt, L.A. Depression, Stigma, and Suicidal Ideation in Medical Students. JAMA 2010, 304, 1181. [Google Scholar] [CrossRef] [PubMed]
- Dyrbye, L.N.; Thomas, M.R.; Shanafelt, T.D. Medical Student Distress: Causes, Consequences, and Proposed Solutions. Mayo Clin. Proc. 2005, 80, 1613–1622. [Google Scholar] [CrossRef] [PubMed]
- Dyrbye, L.N.; Schwartz, A.; Downing, S.M.; Szydlo, D.W.; Sloan, J.A.; Shanafelt, T.D. Efficacy of a Brief Screening Tool to Identify Medical Students in Distress. Acad. Med. 2011, 86, 907–914. [Google Scholar] [CrossRef] [PubMed]
- Saraswathi, I.; Saikarthik, J.; Senthil Kumar, K.; Madhan Srinivasan, K.; Ardhanaari, M.; Gunapriya, R. Impact of COVID-19 outbreak on the mental health status of undergraduate medical students in a COVID-19 treating medical college: A prospective longitudinal study. PeerJ 2020, 8, e10164. [Google Scholar] [CrossRef]
- Jennings, M. Medical Student Burnout: Interdisciplinary Exploration and Analysis. J. Med. Humanit. 2009, 30, 253–269. [Google Scholar] [CrossRef]
- Elmer, T.; Mepham, K.; Stadtfeld, C. Students under lockdown: Comparisons of students’ social networks and mental health before and during the COVID-19 crisis in Switzerland. PLoS ONE 2020, 15, e0236337. [Google Scholar] [CrossRef] [PubMed]
- Halperin, S.J.; Henderson, M.N.; Prenner, S.; Grauer, J.N. Prevalence of anxiety and depression among medical students during the Covid-19 pandemic: A cross-sectional study. J. Med. Educ. Curric. Dev. 2021, 8, 1–7. [Google Scholar] [CrossRef]
- Rolak, S.; Keefe, A.M.; Davidson, E.L.; Aryal, P.; Parajuli, S. Impacts and challenges of United States medical students during the COVID-19 pandemic. World J. Clin. Cases 2020, 8, 3136–3141. [Google Scholar] [CrossRef] [PubMed]
- Adedoyin, O.B.; Soykan, E. COVID-19 pandemic and online learning: The challenges and opportunities. Interact. Learn. Environ. 2020, 7, 1–13. [Google Scholar] [CrossRef]
- Freudenberger, H.J. Staff Burn-Out. J. Soc. Issues 1974, 30, 159–165. [Google Scholar] [CrossRef]
- World Health Organization. Burnout an “Occupational Phenomenon”: International Classification of Diseases. 2019. Available online: https://www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases (accessed on 26 July 2021).
- Almeida, G.D.C.; Souza, H.R.D.; Almeida, P.C.D.; Almeida, B.D.C.; Almeida, G.H. The prevalence of burnout syndrome in medical students. Arch. Clin. Psychiatry (São Paulo) 2016, 43, 6–10. [Google Scholar] [CrossRef]
- Shanafelt, T.D.; Dyrbye, L.N.; West, C.P.; Sinsky, C.A. Potential Impact of Burnout on the US Physician Workforce. Mayo Clin. Proc. 2016, 91, 1667–1668. [Google Scholar] [CrossRef] [PubMed]
- Molodynski, A.; Lewis, T.; Kadhum, M.; Farrell, S.M.; Lemtiri Chelieh, M.; Falcão De Almeida, T.; Masri, R.; Kar, A.; Volpe, U.; Moir, F.; et al. Cultural variations in wellbeing, burnout and substance use amongst medical students in twelve countries. Int. Rev. Psychiatry 2021, 33, 37–42. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S.E.; Leiter, M.P. Maslach Burn. Inventory Man, 4th ed.; Mind Garden: Menlo Park, CA, USA, 2016; Available online: https://www.mindgarden.com (accessed on 26 July 2021).
- Demerouti, E.; Bakker, A.B.; Vardakou, I.; Kantas, A. The convergent validity of two burnout instruments: A multitrait-multimethod analysis. Eur. J. Psychol. Assess. 2003, 19, 12–23. [Google Scholar] [CrossRef]
- Kristensen, T.S.; Borritz, M.; Villadsen, E.; Christensen, K.B. The Copenhagen Burnout Inventory: A new tool for the assessment of burnout. Work Stress 2005, 19, 192–207. [Google Scholar] [CrossRef]
- Schaufeli, W.B.; Leiter, M.P.; Maslach, C.; Jackson, S.E. Maslach burnout inventory–General survey. In The Maslach Burnout Inventory-Test Manual; Maslach, C., Jackson, E.S., Leiter, M.P., Eds.; Consulting Psychologists Press: Palo Alto, CA, USA, 1996; pp. 19–26. [Google Scholar]
- Halbesleben, J.R.B.; Demerouti, E. The construct validity of an alternative measure of burnout: Investigating the English translation of the Oldenburg Burnout Inventory. Work Stress 2005, 19, 208–220. [Google Scholar] [CrossRef]
- Demerouti, E.; Mostert, K.; Bakker, A.B. Burnout and work engagement: A thorough investigation of the independency of both constructs. J. Occup. Health Psychol. 2010, 15, 209–222. [Google Scholar] [CrossRef]
- Reis, D.; Xanthopoulou, D.; Tsaousis, I. Measuring job and academic burnout with the Oldenburg Burnout Inventory (OLBI): Factorial invariance across samples and countries. Burn. Res. 2015, 2, 8–18. [Google Scholar] [CrossRef]
- Demerouti, E.; Nachreiner, F. Zur spezifitat von burnout fur dienstleistungsberufe: Fakt oder artefakt? [The specificity of burnout in human services: Fact or artifact?]. Z. Arbeitswiss 1998, 52, 82–89. [Google Scholar]
- Campos, J.A.D.B.; Carlotto, M.S.; Marôco, J. Oldenburg Burnout Inventory–student version: Cultural adaptation and validation into Portuguese. Psicol. Reflex. Crít. 2012, 25, 709–718. [Google Scholar] [CrossRef]
- Wing, T.; Pey, Y.C.; Subramaniam, V.; Ab Raof, N.A.; Ting, O.W.; Ahmad, M.H.H. Prevalence of Burnout in Medical and Non-medical Undergraduate Malaysian Students in Various International Universities–A Cross-Sectional Study. J. Adv. Med. Res. 2018, 25, 1–13. [Google Scholar] [CrossRef]
- Ishak, W.W.; Nikravesh, R.; Lederer, S.; Perry, R.; Ogunyemi, D.; Bernstein, C. Burnout in medical students: A systematic review. Clin. Teach. 2013, 10, 242–245. [Google Scholar] [CrossRef] [PubMed]
- West, C.P.; Dyrbye, L.N.; Sinsky, C.; Trockel, M.; Tutty, M.; Nedelec, L.; Carlasare, L.E.; Shanafelt, T.D. Resilience and Burnout Among Physicians and the General US Working Population. JAMA Netw. Open 2020, 3, e209385. [Google Scholar] [CrossRef] [PubMed]
- Keeton, K.; Fenner, D.; Johnson, T.; Hayward, R. Predictors of physician career satisfaction, work-life balance, and burnout. Obstet. Gynecol. 2007, 109, 949–955. [Google Scholar] [CrossRef] [PubMed]
- Gheihman, G.; Cooper, C.; Simpkin, A. Everyday Resilience: Practical Tools to Promote Resilience Among Medical Students. J. Gen. Intern. Med. 2018, 34, 498–501. [Google Scholar] [CrossRef] [PubMed]
- Wagnild, G.M.; Young, H.M. Development and psychometric evaluation of the Resilience Scale. J. Nurs. Meas. 1993, 1, 165–178. [Google Scholar]
- Wright, B.; Richmond Mynett, J. Training medical students to manage difficult circumstances—A curriculum for resilience and resourcefulness? BMC Med. Educ. 2019, 19, 280. [Google Scholar] [CrossRef]
- Lin, Y.K.; Lin, C.-D.; Lin, B.Y.-J.; Chen, D.-Y. Medical students’ resilience: A protective role on stress and quality of life in clerkship. BMC Med. Educ. 2019, 19, 473. [Google Scholar] [CrossRef]
- Jordan, R.K.; Shah, S.S.; Desai, H.; Tripi, J.; Mitchell, A.; Worth, R.G. Variation of stress levels, burnout, and resilience throughout the academic year in first-year medical students. PLoS ONE 2020, 15, e0240667. [Google Scholar] [CrossRef] [PubMed]
- Serrão, C.; Castro, L.; Teixeira, A.; Rodrigues, A.R.; Duarte, I. Resilience in Physicians: Contributions to the Validation of the European Portuguese version of the Resilience Scale. Acta Médica Port. 2021, 34, 10. [Google Scholar] [CrossRef]
- Jenkins, T.M.; Kim, J.; Hu, C.; Hickernell, J.C.; Watanaskul, S.; Yoon, J.D. Stressing the journey: Using life stories to study medical student wellbeing. Adv. Health Sci. Educ. 2018, 23, 767–782. [Google Scholar] [CrossRef]
- Mavor, K.I.; McNeill, K.G.; Anderson, K.; Kerr, A.; O’Reilly, E.; Platow, M.J. Beyond prevalence to process: The role of self and identity in medical student well-being. Med. Educ. 2014, 48, 351–360. [Google Scholar] [CrossRef]
- Thompson, G.; McBride, R.B.; Hosford, C.C.; Halaas, G. Resilience Among Medical Students: The Role of Coping Style and Social Support. Teach. Learn. Med. 2016, 28, 174–182. [Google Scholar] [CrossRef] [PubMed]
- Rahimi, B.; Baetz, M.; Bowen, R.; Balbuena, L. Resilience, stress, and coping among Canadian medical students. Can. Med. Educ. J. 2014, 5, e5–e12. [Google Scholar] [CrossRef] [PubMed]
- Dyrbye, L.N.; Power, D.V.; Massie, F.S.; Eacker, A.; Harper, W.; Thomas, M.R.; Szydlo, D.W.; Sloan, J.A.; Shanafelt, T.D. Factors associated with resilience to and recovery from burnout: A prospective, multi-institutional study of US medical students. Med. Educ. 2010, 44, 1016–1026. [Google Scholar] [CrossRef]
- Yu, J.; Chae, S. The mediating effect of resilience on the relationship between the academic burnout and psychological well-being of medical students. Korean J. Med. Educ. 2020, 32, 13–21. [Google Scholar] [CrossRef] [PubMed]
- McLuckie, A.; Matheson, K.M.; Landers, A.L.; Landine, J.; Novick, J.; Barrett, T.; Dimitropoulos, G. The Relationship Between Psychological Distress and Perception of Emotional Support in Medical Students and Residents and Implications for Educational Institutions. Acad. Psychiatry 2017, 42, 41–47. [Google Scholar] [CrossRef]
- Cho, E.; Jeon, S. The role of empathy and psychological need satisfaction in pharmacy students burnout and well-being. BMC Med. Edu. 2019, 19, 43. [Google Scholar] [CrossRef] [PubMed]
- Hopkins, L.; Morgan, H.; Buery-Joyner, S.D.; Craig, L.B.; Everett, E.N.; Forstein, D.A.; Graziano, S.C.; Hampton, B.S.; McKenzie, M.L.; Page-Ramsey, S.M.; et al. To the Point: A prescription for well-being in medical education. Am. J. Obstet. Gynecol. 2019, 221, 542–548. [Google Scholar] [CrossRef] [PubMed]
- Marina, S.; Duarte, I.; Ricou, M. Informed consent in clinical research in Portugal: Promotion of good practices. Acta Méd. Port. 2020, 33, 453–455. [Google Scholar] [CrossRef]
- Trigo, M.; Canudo, N.; Branco, F.; Silva, D. Estudo das propriedades psicométricas da Perceived Stress Scale (PSS) na população portuguesa. Psychologica 2010, 53, 353–378. [Google Scholar] [CrossRef]
- Oliveira, M.; Sousa Machado, T. Tradução e validação da Escala de Resiliência para Estudantes do Ensino Superior. Análise Psicológica 2011, 29, 579–591. [Google Scholar] [CrossRef][Green Version]
- Diener, E.D.; Emmons, R.A.; Larsen, R.J.; Griffin, S. The satisfaction with life scale. J. Pers. Assess. 1985, 49, 71–75. [Google Scholar] [CrossRef]
- Simões, A. Ulterior validação de uma escala de satisfação com a vida (SWLS) [Validation of a life satisfaction scale]. Rev. Port. Pedagog. 1992, 26, 503–515. [Google Scholar]
- Greenland, S. Modeling and variable selection in epidemiologic analysis. Am. J. Public Health 1989, 79, 340–349. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Jackson, S.E. The measurement of experienced burnout. J. Organ. Behav. 1981, 2, 99–113. [Google Scholar] [CrossRef]
- Serrão, C.; Duarte, I.; Castro, L.; Teixeira, A. Burnout and Depression in Portuguese Healthcare Workers during the COVID-19 Pandemic—The Mediating Role of Psychological Resilience. Int. J. Environ. Res. Public Health 2021, 18, 636. [Google Scholar] [CrossRef] [PubMed]
| n (%) | |
|---|---|
| Sex | |
| Female | 349 (75) |
| Male | 113 (25) |
| Civil status | |
| Married/De facto union | 10 (2) |
| Divorced/Single | 452 (98) |
| Has children | 9 (2) |
| Academic year | |
| 1st | 100 (22) |
| 2nd | 52 (11) |
| 3rd | 68 (15) |
| 4th | 67 (14) |
| 5th | 92 (20) |
| 6th | 83 (18) |
| Attending this academic year for the 1st time | 443 (96) |
| Holds special status at faculty | 60 (13) |
| Holds worker-student status | 37 (8) |
| Is living away from home | 87 (19) |
| Currently living with how many other people | |
| 0 | 15 (3) |
| 1 | 44 (10) |
| 2 | 124 (27) |
| 3 | 189 (41) |
| 4 or more | 90 (19) |
| Physical exercise | 316 (68) |
| Leaves the house how often | |
| Occasionally | 249 (54) |
| 1–2 times per week | 134 (29) |
| ≥3 times per week | 79 (17) |
| Has means for keeping up with classes | |
| Supplements/stimulants | |
| Extracurricular activities | 197 (43) |
| Stressful life event | 203 (44) |
| Psychological support | 84 (18) |
| Has taken a COVID-19 test | |
| No, but would like to | 154 (33) |
| No, doesn’t want to | 298 (68) |
| Yes, has the result | 10 (2) |
| Step 1 (β) | Step 2 (β) | Step 3a (β) | Step 3b (β) | Step 4 (β) | |
|---|---|---|---|---|---|
| Male gender | −1.289 | −0.226 | −0.337 | −0.407 | −0.443 |
| Age | 0015 | 0.078 | 0.086 | 0.05 | 0.063 |
| Civil status | |||||
| Married or non-marital partnership | Reference | Reference | Reference | Reference | Reference |
| Divorced or single | 3.37 | 1.884 | 2.084 | 1.748 | 1.937 |
| Has children | 2.23 | −0.819 | −0.488 | −0.578 | −0.391 |
| Academic year | −0.198 | −0.131 | −0.164 | −0.508 | −0.175 |
| Special status | −0.852 | −0.476 | −0.493 | −0.608 | −0.585 |
| Leaves the house how often | |||||
| Occasionally | Reference | Reference | Reference | Reference | Reference |
| 1–2 times per week | −0.452 | −0.375 | −0.389 | −0.258 | −0.3 |
| ≥3 times per week | −0.678 | −0.385 | −0.337 | −0.358 | −0.329 |
| Means for keeping up with classes | −2.107 | −0.577 | −0.496 | −0.753 | −0.644 |
| Supplements/stimulants | 0.991 | 0.317 | 0.389 | 0.371 | 0.411 |
| Physical exercise | −1.578 | −1.099 | −0.887 | −1.08 | −0.924 |
| Extracurricular activities | −0.467 | −0.391 | −0.227 | −0.197 | −0.124 |
| Stressful life event | 1.121 | 0.197 | −0.206 | 0.124 | 0.15 |
| Psychological support | 1.674 | 0.776 | 0.527 | 0.575 | 0.439 |
| Has taken a COVID test | |||||
| No, but would like to | Reference | Reference | Reference | Reference | Reference |
| No, doesn’t want to | −0.664 | −0.515 | 0.466 | −0.614 | −0.049 |
| Yes, has the result | 0.757 | −0.09 | −0.158 | −0.158 | −0.55 |
| Stress | |||||
| Resilience | 0.329 | 0.276 | 0.258 | ||
| Life satisfaction | −0.039 | −0.029 | |||
| −0.17 | −0.215 |
| Step 1 (β) | Step 2 (β) | Step 3a (β) | Step 3b (β) | Step 4 (β) | |
|---|---|---|---|---|---|
| Age | −0.02 | 0.012 | 0.023 | −0.012 | 0.006 |
| Academic year | −0.203 | −0.097 | −0.139 | −0.139 | −0.159 |
| Special status | −0.887 | −0.707 | −0.69 | −0.793 | −0.749 |
| Leaves the house how often | |||||
| Occasionally | Reference | Reference | Reference | Reference | Reference |
| 1–2 times per week | 0.077 | 0.132 | 0.113 | 0.257 | 0.198 |
| ≥3 times per week | −0.517 | −0.319 | −0.253 | −0.296 | −0.251 |
| Volunteering | −0.606 | −0.45 | −0.469 | −0.356 | −0.404 |
| Means for keeping up with classes | −1.085 | −0.339 | −0.198 | −0.513 | −0.338 |
| Supplements/stimulants | −0.535 | 0.227 | 0.292 | 0.244 | 0.29 |
| Physical exercise | −0.538 | −0.291 | 0.001 | −0.255 | −0.031 |
| Stressful life event | 0.921 | 0.447 | 0.463 | 0.369 | 0.409 |
| Psychological support | 0.486 | −0.03 | −0.319 | −0.219 | −0.388 |
| Stress | 0.164 | 0.097 | 0.121 | 0.082 | |
| Resilience | −0.05 | −0.04 | |||
| Life satisfaction | −0.187 | −0.122 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Duarte, I.; Alves, A.; Coelho, A.; Ferreira, A.; Cabral, B.; Silva, B.; Peralta, J.; Silva, J.; Domingues, P.; Nunes, P.; et al. The Mediating Role of Resilience and Life Satisfaction in the Relationship between Stress and Burnout in Medical Students during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2022, 19, 2822. https://doi.org/10.3390/ijerph19052822
Duarte I, Alves A, Coelho A, Ferreira A, Cabral B, Silva B, Peralta J, Silva J, Domingues P, Nunes P, et al. The Mediating Role of Resilience and Life Satisfaction in the Relationship between Stress and Burnout in Medical Students during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2022; 19(5):2822. https://doi.org/10.3390/ijerph19052822
Chicago/Turabian StyleDuarte, Ivone, Ana Alves, Ana Coelho, Ana Ferreira, Beatriz Cabral, Bebiana Silva, João Peralta, Juliana Silva, Pedro Domingues, Pedro Nunes, and et al. 2022. "The Mediating Role of Resilience and Life Satisfaction in the Relationship between Stress and Burnout in Medical Students during the COVID-19 Pandemic" International Journal of Environmental Research and Public Health 19, no. 5: 2822. https://doi.org/10.3390/ijerph19052822
APA StyleDuarte, I., Alves, A., Coelho, A., Ferreira, A., Cabral, B., Silva, B., Peralta, J., Silva, J., Domingues, P., Nunes, P., Serrão, C., & Santos, C. (2022). The Mediating Role of Resilience and Life Satisfaction in the Relationship between Stress and Burnout in Medical Students during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health, 19(5), 2822. https://doi.org/10.3390/ijerph19052822









