How Long Does Adaption Last for? An Update on the Psychological Impact of the Confinement in Portugal
Abstract
:1. Introduction
2. Materials and Methods
3. Results
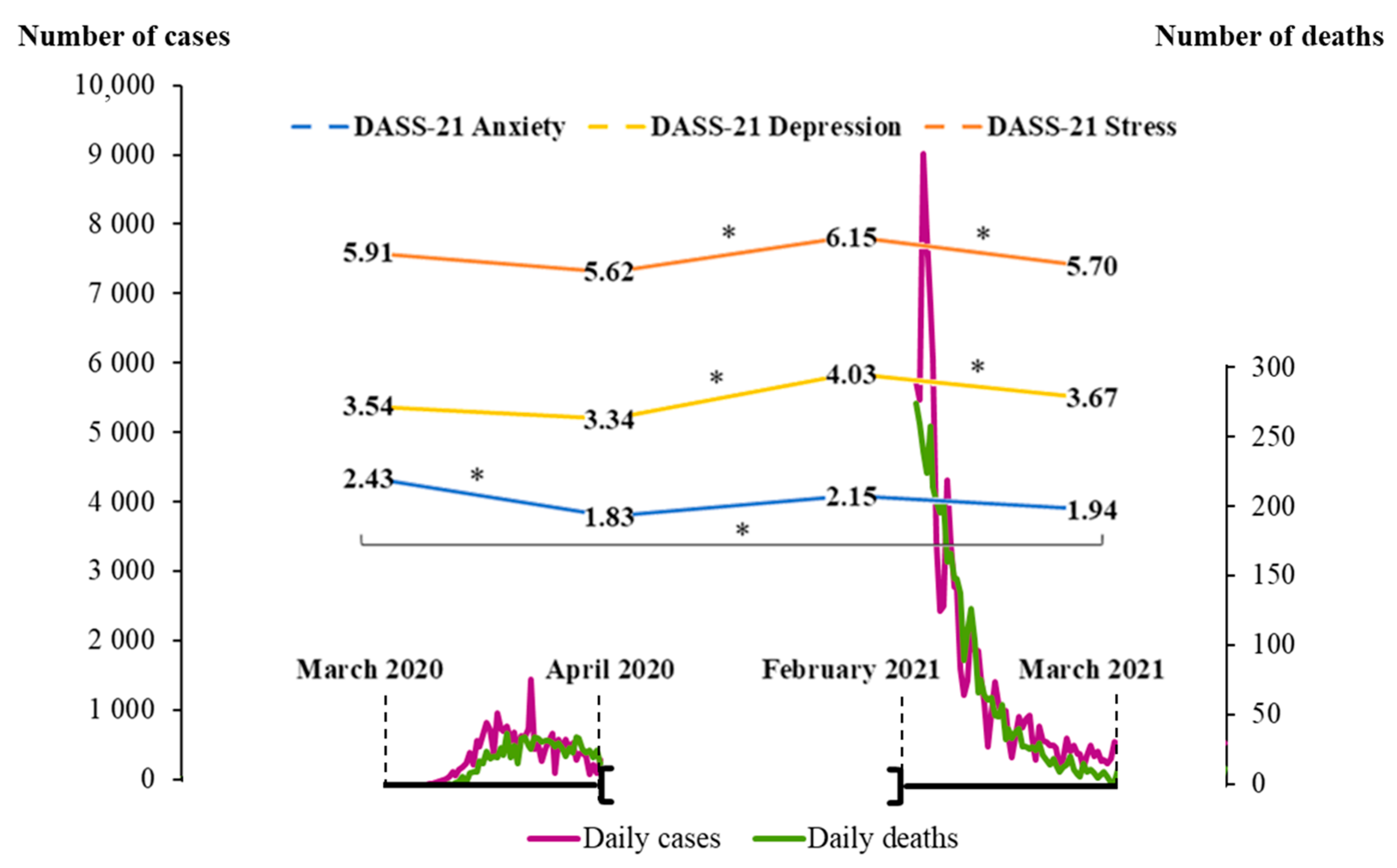
3.1. Evolution of the Psychological Symptoms and the Epidemiological Context in Portugal
3.2. Severity of the Psychological Symptoms
3.3. DASS-21: A Comparison of Confinements
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Zhang, J.; Wu, W.; Zhao, X.; Zhang, W. Recommended psychological crisis intervention response to the 2019 novel coronavirus pneumonia outbreak in China: A model of West China Hospital. Precis. Clin. Med. 2020, 3, 3–8. [Google Scholar] [CrossRef] [Green Version]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Hossain, M.M.; Sultana, A.; Purohit, N. Mental Health Outcomes of Quarantine and Isolation for Infection Prevention: A Systematic Umbrella Review of the Global Evidence. Epidemiol. Health 2020, 42, e2020038. [Google Scholar] [CrossRef] [PubMed]
- Paulino, M.; Dumas-Diniz, R.; Brissos, S.; Brites, R.; Alho, L.; Simões, M.R.; Silva, C.F. COVID-19 in Portugal: Exploring the immediate psychological impact on the general population. Psychol. Health Med. 2021, 26, 44–55. [Google Scholar] [CrossRef] [PubMed]
- Moreira, P.S.; Ferreira, S.; Couto, B.; Machado-Sousa, M.; Fernández, M.; Raposo-Lima, C.; Sousa, N.; Picó-Pérez, M.; Morgado, P. Protective Elements of Mental Health Status during the COVID-19 Outbreak in the Portuguese Population. Int. J. Environ. Res. Public Health 2021, 18, 1910. [Google Scholar] [CrossRef] [PubMed]
- Rubin, G.J.; Wessely, S. The psychological effects of quarantining a city. BMJ 2020, 368, m313. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- DiGiovanni, C.; Conley, J.; Chiu, D.; Zaborski, J. Factors influencing compliance with quarantine in Toronto during the 2003 SARS outbreak. Biosecur. Bioterror.Biodef. Strateg. Pract. Sci. 2004, 2, 265–272. [Google Scholar] [CrossRef] [PubMed]
- Hall, M.J.; Norwood, A.E.; Fullerton, C.S.; Gifford, R.; Ursano, R.J. The Psychological Burden of Bioterrorism. J. Aggress. Maltreat. Trauma 2008, 2, 293–304. [Google Scholar] [CrossRef]
- Schimmenti, A.; Billieux, J.; Starcevic, V. The four horsemen of fear: An integrated model of understanding fear experiences during the COVID-19 pandemic. Clin. Neuropsychiatry 2020, 17, 41–45. [Google Scholar]
- Lemyre, L.; Johnson, C.; Corneil, W. Psychosocial considerations for mass decontamination. Radiat. Prot. Dosim. 2010, 142, 17–23. [Google Scholar] [CrossRef] [Green Version]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; Ho, C.S.; Ho, R.C. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int. J. Environ. Res. Public Health 2020, 17, 1729. [Google Scholar] [CrossRef] [Green Version]
- Bendau, A.; Plag, J.; Kunas, S.; Wyka, S.; Ströhle, A.; Petzold, M.B. Longitudinal changes in anxiety and psychological distress, associated risk and protective factors during the first three months of the COVID-19 pandemic in Germany. Brain Behav. 2021, 11, e01964. [Google Scholar] [CrossRef]
- Prati, G.; Mancini, A.D. The psychological impact of COVID-19 pandemic lockdowns: A review and meta-analysis of longitudinal studies and natural experiments. Psychol. Med. 2021, 51, 201–211. [Google Scholar] [CrossRef]
- Planchuelo-Gómez, Á.; Odriozola-González, P.; Irurtia, M.J.; de Luis-García, R. Longitudinal evaluation of the psychological impact of the COVID-19 crisis in Spain. J. Affect. Disord. 2020, 277, 842–849. [Google Scholar] [CrossRef]
- Picó-Pérez, M.; Ferreira, S.; Raposo-lima, C.; Machado-Sousa, M.; Morgado, P. Sociodemographic and lifestyle predictors of mental health adaptability during COVID-19 compulsory confinement: A longitudinal study in the Portuguese population. J. Affect. Disord. 2021, 295, 797–803. [Google Scholar] [CrossRef]
- Fancourt, D.; Steptoe, A.; Bu, F. Trajectories of anxiety and depressive symptoms during enforced isolation due to COVID-19 in England: A longitudinal observational study. Lancet Psychiatry 2021, 8, 141–149. [Google Scholar] [CrossRef]
- Jamieson, J.P.; Crum, A.J.; Goyer, J.P.; Marotta, M.E.; Akinola, M. Optimizing stress responses with reappraisal and mindset interventions: An integrated model. Anxiety Stress Coping 2018, 31, 245–261. [Google Scholar] [CrossRef]
- Pais-Ribeiro, J.; Honrado, A.; Leal, I. Contribuição para o estudo da adaptação portuguesa das Escalas de Ansiedade Depressão e Stress de Lovibond e Lovibond. Psicol. Saúde Doenlas 2004, 5, 229–239. [Google Scholar]
- Lovibond, P.F.; Lovibond, S.H. The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav. Res. Ther. 1995, 33, 335–343. [Google Scholar] [CrossRef]
- Reynolds, D.L.; Garay, J.R.; Deamond, S.L.; Moran, M.K.; Gold, W.; Styra, R. Understanding, compliance and psychological impact of the SARS quarantine experience. Epidemiol. Infect. 2008, 136, 997–1007. [Google Scholar] [CrossRef]
- Jungmann, S.M.; Witthöft, M. Health anxiety, cyberchondria, coping in the current COVID-19 pandemic: Which factors are related to coronavirus anxiety? J. Anxiety Disord. 2020, 73, 102239. [Google Scholar] [CrossRef]
- Canet-Juric, L.; Andrés, M.L.; Del Valle, M.; López-Morales, H.; Poó, F.; Galli, J.I.; Yerro, M.; Urquijo, S. A Longitudinal Study on the Emotional Impact Cause by the COVID-19 Pandemic Quarantine on General Population. Front. Psychol. 2020, 11, 1–17. [Google Scholar] [CrossRef]
- Ho, C.S.; Chee, C.Y.; Ho, R.C. Mental Health Strategies to Combat the Psychological Impact of COVID-19 Beyond Paranoia and Panic. Ann. Acad. Med. Singap. 2020, 49, 155–160. [Google Scholar] [CrossRef]
- Cava, M.A.; Fay, K.E.; Beanlands, H.J.; McCay, E.A.; Wignall, R. The experience of quarantine for individuals affected by SARS in Toronto. Public Health Nurs. 2005, 22, 398–406. [Google Scholar] [CrossRef]
- Flesia, L.; Monaro, M.; Mazza, C.; Fietta, V.; Colicino, E.; Segatto, B.; Roma, P. Predicting Perceived Stress Related to the Covid-19 Outbreak through Stable Psychological Traits and Machine Learning Models. J. Clin. Med. 2020, 9, 3350. [Google Scholar] [CrossRef]
- Van Bavel, J.J.; Baicker, K.; Boggio, P.S.; Capraro, V.; Cichocka, A.; Cikara, M.; Crockett, M.J.; Crum, A.J.; Douglas, K.M.; Druckman, J.N.; et al. Using social and behavioural science to support COVID-19 pandemic response. Nat. Hum. Behav. 2020, 4, 460–471. [Google Scholar] [CrossRef]
- Somma, A.; Gialdi, G.; Krueger, R.F.; Markon, K.E.; Frau, C.; Lovallo, S.; Fossati, A. Dysfunctional personality features, non-scientifically supported causal beliefs, emotional problems during the first month of the COVID-19 pandemic in Italy. Pers. Individ. Differ. 2020, 165, 110139. [Google Scholar] [CrossRef]
- Duan, L.; Zhu, G. Psychological interventions for people affected by the COVID-19 epidemic. Lancet Psychiatry 2020, 7, 300–302. [Google Scholar] [CrossRef]
- Banerjee, D. The COVID-19 outbreak: Crucial role the psychiatrists can play. Asian J. Psychiatr. 2020, 50, 102014. [Google Scholar] [CrossRef]
- Sprang, G.; Silman, M. Posttraumatic stress disorder in parents and youth after health-related disasters. Disaster Med. Public Health Prep. 2013, 7, 105–110. [Google Scholar] [CrossRef]
- Kim, H.C.; Yoo, S.Y.; Lee, B.H.; Lee, S.H.; Shin, H.S. Psychiatric findings in suspected and confirmed middle east respiratory syndrome patients quarantined in hospital: A retrospective chart analysis. Psychiatry Investig. 2018, 15, 355–360. [Google Scholar] [CrossRef] [PubMed]
- He, Z.; Chen, J.; Pan, K.; Yue, Y.; Cheung, T.; Yuan, Y.; Du, N.; Zhao, Y.; Feng, Y.; Zhou, D.; et al. The development of the ‘COVID-19 Psychological Resilience Model’ and its efficacy during the COVID-19 pandemic in China. Int. J. Biol. Sci. 2020, 16, 2828–2834. [Google Scholar] [CrossRef] [PubMed]
- Serafini, G.; Parmigiani, B.; Amerio, A.; Aguglia, A.; Sher, L.; Amore, M. The psychological impact of COVID-19 on the mental health in the general population. QJM 2020, 113, 529–535. [Google Scholar] [CrossRef] [PubMed]
- Polizzi, C.; Lynn, S.J.; Perry, A. Stress and coping in the time of COVID-19: Pathways to resilience and recovery. Clin. Neuropsychiatry 2020, 17, 59–62. [Google Scholar] [PubMed]
- Bai, Y.; Lin, C.C.; Lin, C.Y.; Chen, J.Y.; Chue, C.M.; Chou, P. Survey of stress reactions among health care workers involved with the SARS outbreak. Psychiatr. Serv. 2004, 55, 1055–1057. [Google Scholar] [CrossRef]
- Xiang, Y.T.; Yang, Y.; Li, W.; Zhang, L.; Zhang, Q.; Cheung, T.; Ng, C.H. Timely mental health care for the 2019 novel coronavirus outbreak is urgently needed. Lancet Psychiatry 2020, 7, 228–229. [Google Scholar] [CrossRef] [Green Version]
- Connor, J.; Madhavan, S.; Mokashi, M.; Amanuel, H.; Johnson, N.R.; Pace, L.E.; Bartz, D. Health risks and outcomes that disproportionately affect women during the Covid-19 pandemic: A review. Soc. Sci. Med. 2020, 266, 113364. [Google Scholar] [CrossRef]
- Chigangaidze, R.K. Risk Factors and Effects of the Morbus: COVID-19 through the Biopsychosocial Model and Ecological Systems Approach to Social Work Practice. Soc. Work Public Health 2021, 36, 98–117. [Google Scholar] [CrossRef]
- Han, Y.; Jang, J.; Cho, E.; Choi, K.-H. Investigating how individual differences influence responses to the COVID-19 crisis: The role of maladaptive and five-factor personality traits. Pers. Individ. Differ. 2021, 176, 110786. [Google Scholar] [CrossRef]
- Morales-Vives, F.; Dueñas, J.M.; Vigil-Colet, A.; Camarero-Figuerola, M. Psychological Variables Related to Adaptation to the COVID-19 Lockdown in Spain. Front. Psychol. 2020, 11, 565634. [Google Scholar] [CrossRef]
| DASS-21 Subscales | Severity Levels | March 2020 (%) | April 2020 (%) | February 2021 (%) | March 2021 (%) |
|---|---|---|---|---|---|
| Stress | Normal | 70.8 | 72.7 | 70.5 | 74.5 |
| Mild | 13.4 | 10.6 | 9.0 | 9.6 | |
| Moderate | 7.8 | 8.7 | 9.3 | 6.8 | |
| Severe | 7.1 | 5.0 | 9.6 | 6.8 | |
| Extremely Severe | 0.9 | 3.1 | 1.6 | 2.2 | |
| Depression | Normal | 69.6 | 71.7 | 65.2 | 69.3 |
| Mild | 13.4 | 11.2 | 13.7 | 9.9 | |
| Moderate | 12.1 | 11.5 | 12.1 | 13.0 | |
| Severe | 3.2 | 2.8 | 5.3 | 5.0 | |
| Extremely Severe | 1.9 | 2.8 | 3.7 | 2.8 | |
| Anxiety | Normal | 74.5 | 82.3 | 79.8 | 78.9 |
| Mild | 10.2 | 7.1 | 7.8 | 11.2 | |
| Moderate | 7.8 | 5.3 | 4.7 | 4.3 | |
| Severe | 3.7 | 3.1 | 2.8 | 3.1 | |
| Extremely Severe | 3.7 | 2.2 | 5.0 | 2.5 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Costa, A.D.; Fernandes, A.; Ferreira, S.; Couto, B.; Machado-Sousa, M.; Moreira, P.; Morgado, P.; Picó-Pérez, M. How Long Does Adaption Last for? An Update on the Psychological Impact of the Confinement in Portugal. Int. J. Environ. Res. Public Health 2022, 19, 2243. https://doi.org/10.3390/ijerph19042243
Costa AD, Fernandes A, Ferreira S, Couto B, Machado-Sousa M, Moreira P, Morgado P, Picó-Pérez M. How Long Does Adaption Last for? An Update on the Psychological Impact of the Confinement in Portugal. International Journal of Environmental Research and Public Health. 2022; 19(4):2243. https://doi.org/10.3390/ijerph19042243
Chicago/Turabian StyleCosta, Ana Daniela, Afonso Fernandes, Sónia Ferreira, Beatriz Couto, Mafalda Machado-Sousa, Pedro Moreira, Pedro Morgado, and Maria Picó-Pérez. 2022. "How Long Does Adaption Last for? An Update on the Psychological Impact of the Confinement in Portugal" International Journal of Environmental Research and Public Health 19, no. 4: 2243. https://doi.org/10.3390/ijerph19042243
APA StyleCosta, A. D., Fernandes, A., Ferreira, S., Couto, B., Machado-Sousa, M., Moreira, P., Morgado, P., & Picó-Pérez, M. (2022). How Long Does Adaption Last for? An Update on the Psychological Impact of the Confinement in Portugal. International Journal of Environmental Research and Public Health, 19(4), 2243. https://doi.org/10.3390/ijerph19042243








