Condemn or Treat? The Influence of Adults’ Stigmatizing Attitudes on Mental Health Service Use for Children
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample
2.2. Measures
2.3. Model and Estimation
3. Results
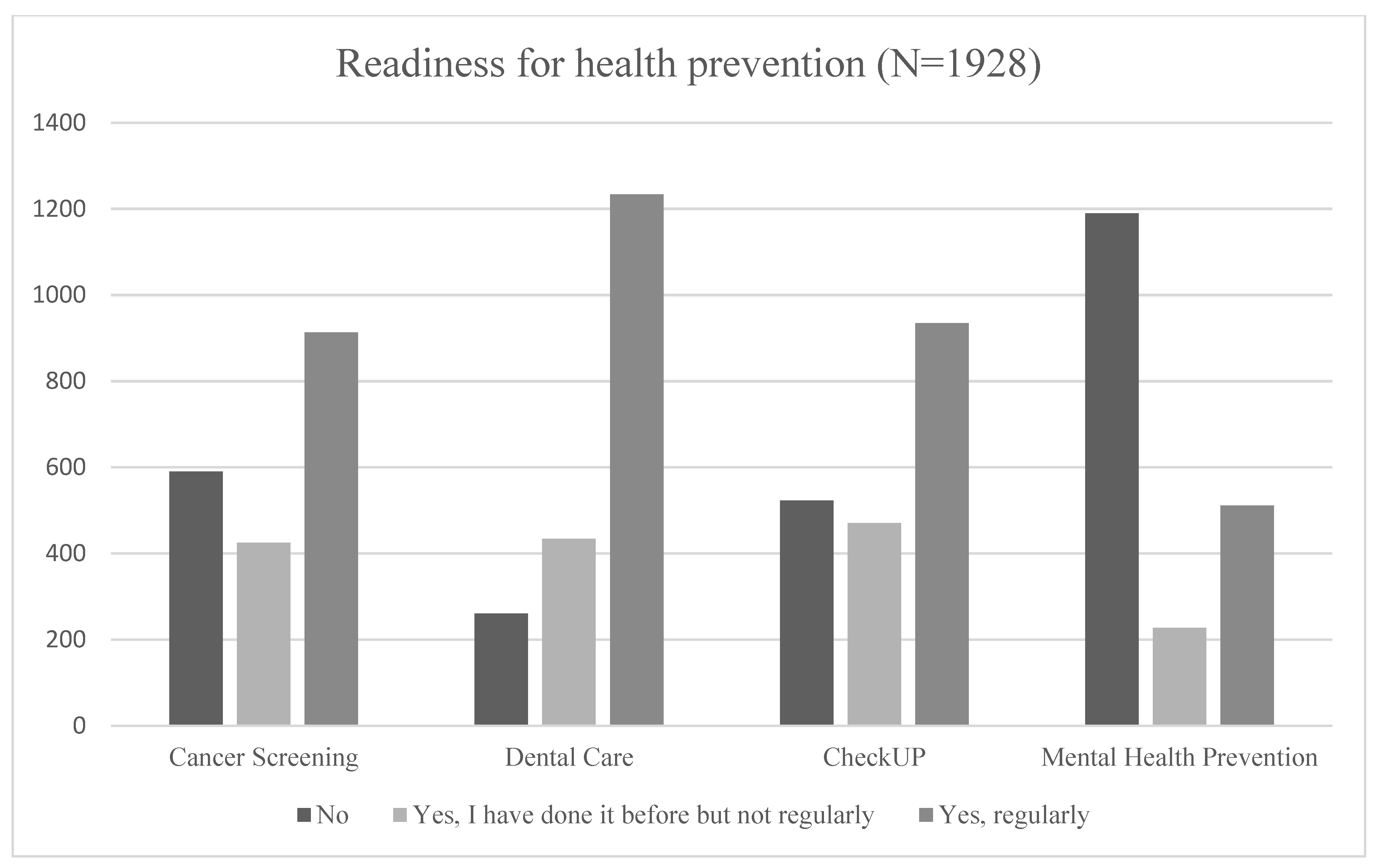
3.1. Descriptive Analysis
| Variables | Mean | Standard Deviation | Min | Max | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Adult help-seeking for children | 3.94 | 1.14 | 1 | 5 | |||||||||
| 2. Stigmatizing attitudes | 10.80 | 4.53 | 5 | 25 | 1.00 | ||||||||
| 3. Gender | 1.52 | 0.50 | 1 | 3 | −0.11 *** | 1.00 | |||||||
| 4. Age | 55.36 | 15.29 | 16 | 101 | 0.09 *** | 0.008 | 1.00 | ||||||
| 5. Education | 5.58 | 1.73 | 1 | 9 | −0.10 *** | −0.05 * | −0.15 *** | 1.00 | |||||
| 6. Income | 2036.86 | 1031.08 | 125 | 7500 | −0.07 ** | −0.09 *** | −0.11 *** | 0.34 *** | 1.00 | ||||
| 7. Adult history of psychotherapy | 0.18 | 0.47 | 0 | 2 | −0.13 *** | 0.11 *** | −0.06 ** | −0.02 | −0.08 *** | 1.00 | |||
| 8. Preventive health care | 4.53 | 2.54 | 0 | 8 | −0.15 *** | 0.26 *** | 0.17 *** | 0.05 * | 0.12 *** | 0.006 | 1.00 | ||
| 9. Family status | 0.99 | 0.86 | 0 | 2 | 0.02 | 0.03 | 0.12 *** | 0.004 | 0.01 | −0.09 *** | 0.11 *** | 1.00 | |
| 10. Readiness to disclose health problems | 6.72 | 2.22 | 2 | 10 | −0.26 *** | 0.12 *** | −0.02 | 0.04 | 0.08 *** | 0.03 | 0.29 *** | 0.09 *** | 1.00 |
3.2. Results from Estimation
4. Discussion
4.1. Limitations
4.2. Theoretical and Practical Implications
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Solmi, M.; Radua, J.; Olivola, M.; Croce, E.; Soardo, L.; de Pablo, G.S.; Shin, J., II; Kirkbride, J.B.; Jones, P.; Kim, J.H.; et al. Age at onset of mental disorders worldwide: Large-scale meta-analysis of 192 epidemiological studies. Mol. Psychiatry 2021, 27, 281–295. [Google Scholar] [CrossRef] [PubMed]
- Kato, N.; Yanagawa, T.; Fujiwara, T.; Morawska, A. Prevalence of Children’s Mental Health Problems and the Effectiveness of Population-Level Family Interventions. J. Epidemiol. 2015, 25, 507–516. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Berglund, P.; Demler, O.; Jin, R.; Merikangas, K.R.; Walters, E.E. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch. Gen. Psychiatry 2005, 62, 593–602. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Avenevoli, S.; Costello, E.J.; Georgiades, K.; Green, J.G.; Gruber, M.J.; He, J.-P.; Koretz, D.; McLaughlin, K.A.; Petukhova, M.; et al. Prevalence, Persistence, and Sociodemographic Correlates of DSM-IV Disorders in the National Comorbidity Survey Replication Adolescent Supplement. Arch. Gen. Psychiatry 2012, 69, 372–380. [Google Scholar] [CrossRef]
- Green, H.; McGinnity, A.; Meltzer, H.; Ford, T.; Goodman, R. Mental Health of Children and Young People in Great Britain, 2004; Palgrave Macmillan: Basingstoke, UK; New York, NY, USA, 2005. [Google Scholar] [CrossRef]
- Lawrence, D.; Johnson, S.; Hafekost, J.; Katrina Boterhoven de Haan Sawyer, M.; Ainley, J.; Zubrick, S. The Mental Health of Children and Adolescents: Report on the Second Australian Child and Adolescent Survey of Mental Health and Wellbeing; Department of Health: Canberra, Australia, 2015; Available online: https://research.acer.edu.au/well_being/1 (accessed on 28 November 2022).
- Merikangas, K.R.; He, J.-P.; Burstein, M.; Swendsen, J.; Avenevoli, S.; Case, B.; Georgiades, K.; Heaton, L.; Swanson, S.; Olfson, M. Service Utilization for Lifetime Mental Disorders in U.S. Adolescents: Results of the National Comorbidity Survey–Adolescent Supplement (NCS-A). J. Am. Acad. Child Adolesc. Psychiatry 2010, 50, 32–45. [Google Scholar] [CrossRef]
- Oh, E.; Mathers, M.; Hiscock, H.; Wake, M.; Bayer, J. Professional help seeking for young children with mental health problems. Aust. J. Psychol. 2015, 67, 187–195. [Google Scholar] [CrossRef]
- Hintzpeter, B.; Metzner, F.; Pawils, S.; Bichmann, H.; Kamtsiuris, P.; Ravens-Sieberer, U.; Klasen, F.; The Bella Study Group. Inanspruchnahme von ärztlichen und psychotherapeutischen Leistungen durch Kinder und Jugendliche mit psychischen Auffälligkeiten. Kindh. Entwickl. 2014, 23, 229–238. [Google Scholar] [CrossRef]
- Campion, J.; Bhui, K.; Bhugra, D. European Psychiatric Association (EPA) guidance on prevention of mental disorders. Eur. Psychiatry J. Assoc. Eur. Psychiatr. 2012, 27, 68–80. [Google Scholar] [CrossRef]
- Wang, P.S.; Angermeyer, M.; Borges, G.; Bruffaerts, R.; Chiu, W.T.; De Girolamo, G.; Fayyad, J.; Gureje, O.; Haro, J.M.; Huang, Y.; et al. Delay and failure in treatment seeking after first onset of mental disorders in the World Health Organization’s World Mental Health Survey Initiative. World Psychiatry 2007, 6, 177–185. [Google Scholar]
- Kaushik, A.; Kostaki, E.; Kyriakopoulos, M. The stigma of mental illness in children and adolescents: A systematic review. Psychiatry Res. 2016, 243, 469–494. [Google Scholar] [CrossRef]
- Logan, D.E.; King, C.A. Parental facilitation of adolescent mental health service utilization: A conceptual and empirical review. Clin. Psychol. Sci. Pract. 2001, 8, 319–333. [Google Scholar] [CrossRef]
- Reardon, T.; Harvey, K.; Baranowska, M.; O’Brien, D.; Smith, L.; Creswell, C. What do parents perceive are the barriers and facilitators to accessing psychological treatment for mental health problems in children and adolescents? A systematic review of qualitative and quantitative studies. Eur. Child Adolesc. Psychiatry 2017, 26, 623–647. [Google Scholar] [CrossRef] [PubMed]
- Corrigan, P. How stigma interferes with mental health care. Am. Psychol. 2004, 59, 614–625. [Google Scholar] [CrossRef] [PubMed]
- Hinshaw, S.P. The stigmatization of mental illness in children and parents: Developmental issues, family concerns, and research needs. J. Child Psychol. Psychiatry 2005, 46, 714–734. [Google Scholar] [CrossRef] [PubMed]
- Schomerus, G.; Angermeyer, M.C. Stigma and its impact on help-seeking for mental disorders: What do we know? Epidemiol. Psichiatr. Soc. 2008, 17, 31–37. [Google Scholar] [CrossRef] [PubMed]
- Dempster, R.; Wildman, B.; Keating, A. The Role of Stigma in Parental Help-Seeking for Child Behavior Problems. J. Clin. Child Adolesc. Psychol. 2013, 42, 56–67. [Google Scholar] [CrossRef] [PubMed]
- Gronholm, P.C.; Ford, T.; Roberts, R.E.; Thornicroft, G.; Laurens, K.R.; Evans-Lacko, S. Mental Health Service Use by Young People: The Role of Caregiver Characteristics. PLoS ONE 2015, 10, e0120004. [Google Scholar] [CrossRef]
- Ford, T.; Hamilton, H.; Meltzer, H.; Goodman, R. Predictors of Service Use for Mental Health Problems Among British Schoolchildren. Child Adolesc. Ment. Health 2008, 13, 32–40. [Google Scholar] [CrossRef]
- Hoffer, R.; Fröhlich-Gildhoff, K. Inanspruchnahme von Hilfe und Versorgung bei psychischen Auffälligkeiten im Kindergartenalter. Kindh. Entwickl. 2019, 28, 33–45. [Google Scholar] [CrossRef]
- Ryan, S.M.; Jorm, A.F.; Toumbourou, J.W.; Lubman, D. Parent and family factors associated with service use by young people with mental health problems: A systematic review. Early Interv. Psychiatry 2015, 9, 433–446. [Google Scholar] [CrossRef]
- Wichstrøm, L.; Belsky, J.; Jozefiak, T.; Sourander, A.; Berg-Nielsen, T.S. Predicting Service Use for Mental Health Problems Among Young Children. Pediatrics 2014, 133, 1054–1060. [Google Scholar] [CrossRef] [PubMed]
- Zwaanswijk, M.; VAN DER Ende, J.; Verhaak, P.F.; Bensing, J.M.; Verhulst, F.C. Help-Seeking for Child Psychopathology: Pathways to Informal and Professional Services in The Netherlands. J. Am. Acad. Child Adolesc. Psychiatry 2005, 44, 1292–1300. [Google Scholar] [CrossRef] [PubMed]
- Girio-Herrera, E.; Owens, J.S.; Langberg, J.M. Perceived Barriers to Help-Seeking Among Parents of At-Risk Kindergarteners in Rural Communities. J. Clin. Child Adolesc. Psychol. 2013, 42, 68–77. [Google Scholar] [CrossRef] [PubMed]
- Harwood, M.D.; O’Brien, K.A.; Carter, C.G.; Eyberg, S.M. Mental Health Services for Preschool Children in Primary Care: A Survey of Maternal Attitudes and Beliefs. J. Pediatr. Psychol. 2008, 34, 760–768. [Google Scholar] [CrossRef]
- Murry, V.M.; Heflinger, C.A.; Suiter, S.V.; Brody, G.H. Examining perceptions about mental health care and help-seeking among rural African American families of adolescents. J. Youth Adolesc. 2011, 40, 1118–1131. [Google Scholar] [CrossRef]
- Bühring, P. Psychotherapie im europäischen Vergleich—Deutschland gut aufgestellt. Dtsch. Ärzteblatt 2011, 4, 149. [Google Scholar]
- Bundes Psychotherapeuten Kammer. Wege zur Psychotherapie. Berlin. August 2021. Available online: https://www.bptk.de/wp-content/uploads/2021/08/bptk_patientenbroschuere_2021.pdf (accessed on 28 November 2022).
- Deutsche Gesellschaft für Psychiatrie und Psychotherapie; Psychosomatik und Nervenheilkunde e. V. Forschung und Versorgung Weltweit: Global Mental Health. 2022. Available online: https://www.dgppn.de/schwerpunkte/global-mental-health.html (accessed on 28 July 2022).
- Nier, H. Europäische Länder mit den Meisten Psychiatern. Statista. 10 October 2019. Available online: https://de.statista.com/infografik/19604/europaeische-laender-mit-den-meisten-psychiatern/ (accessed on 28 July 2022).
- Fegert, J.M.; Kölch, M.; Krüger, U. Versorgung Psychisch Kranker Kinder und Jugendlicher in Deutschland- Bestandsaufnahme und Bedarfsanalyse; Bundesministerium für Gesundheit, 2017; Available online: https://www.bundesgesundheitsministerium.de/service/publikationen/details/versorgung-psychisch-kranker-kinder-und-jugendlicher-in-deutschland-bestandsaufnahme-und-bedarfsanalyse.html (accessed on 28 November 2022).
- Clement, S.; Schauman, O.; Graham, T.; Maggioni, F.; Evans-Lacko, S.; Bezborodovs, N.; Morgan, C.; Rüsch, N.; Brown, J.S.L.; Thornicroft, G. What is the impact of mental health-related stigma on help-seeking? A systematic review of quantitative and qualitative studies. Psychol. Med. 2015, 45, 11–27. [Google Scholar] [CrossRef]
- Judd, F.; Komiti, A.; Jackson, H. How Does Being Female Assist Help-Seeking for Mental Health Problems? Aust. N. Z. J. Psychiatry 2008, 42, 24–29. [Google Scholar] [CrossRef]
- Gagné, S.; Vasiliadis, H.-M.; Préville, M. Gender differences in general and specialty outpatient mental health service use for depression. BMC Psychiatry 2014, 14, 135. [Google Scholar] [CrossRef]
- Kovess-Masfety, V.; Boyd, A.; Van de Velde, S.; De Graaf, R.; Vilagut, G.; Haro, J.M.; Florescu, S.; O’Neill, S.; Weinberg, L.; Alonso, J.; et al. Are there gender differences in service use for mental disorders across countries in the European Union? Results from the EU-World Mental Health survey. J. Epidemiol. Community Health 2014, 68, 649–656. [Google Scholar] [CrossRef]
- Spoth, R.; Redmond, C.; Shin, C. Modeling factors influencing enrollment in family-focused preventive intervention research. Prev. Sci. 2000, 1, 213–225. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.Y.; Hwang, J.; Ball, J.G.; Lee, J.; Albright, D.L. Is health literacy associated with mental health literacy? Findings from Mental Health Literacy Scale. Perspect. Psychiatr. Care 2019, 56, 393–400. [Google Scholar] [CrossRef] [PubMed]
- Shivram, R.; Bankart, J.; Meltzer, H.; Ford, T.; Vostanis, P.; Goodman, R. Service utilization by children with conduct disorders: Findings from the 2004 Great Britain child mental health survey. Eur. Child Adolesc. Psychiatry 2009, 18, 555–563. [Google Scholar] [CrossRef] [PubMed]
- Vostanis, P.; Meltzer, H.; Goodman, R.; Ford, T. Service utilisation by children with conduct disorders. Eur. Child Adolesc. Psychiatry 2003, 12, 231–238. [Google Scholar] [CrossRef]
- Turner, E.; Liew, J. Children’s Adjustment and Child Mental Health Service Use: The Role of Parents’ Attitudes and Personal Service Use in an Upper Middle Class Sample. Community Ment. Health J. 2009, 46, 231–240. [Google Scholar] [CrossRef] [PubMed]
- Boydell, K.M.; Pong, R.; Volpe, T.; Tilleczek, K.; Wilson, E.; Lemieux, S. Family perspectives on pathways to mental health care for children and youth in rural communities. J. Rural. Health 2006, 22, 182–188. [Google Scholar] [CrossRef] [PubMed]
- Klasen, F.; Meyrose, A.-K.; Otto, C.; Reiss, F.; Ravens-Sieberer, U. Psychische Auffälligkeiten von Kindern und Jugendlichen in Deutschland. Ergeb. der Physiol. 2017, 165, 402–407. [Google Scholar] [CrossRef]
- Bellettiere, J.; Chuang, E.; Hughes, S.; Quintanilla, I.; Hofstetter, C.R.; Hovell, M.F. Association Between Parental Barriers to Accessing a Usual Source of Care and Children’s Receipt of Preventive Services. Public Health Rep. 2017, 132, 316–325. [Google Scholar] [CrossRef]
- Smith, L.E.; Amlôt, R.; Weinman, J.; Yiend, J.; Rubin, G.J. A systematic review of factors affecting vaccine uptake in young children. Vaccine 2017, 35, 6059–6069. [Google Scholar] [CrossRef]
- Torun, S.D.; Torun, F.; Catak, B. Healthcare workers as parents: Attitudes toward vaccinating their children against pandemic influenza A/H1N1. BMC Public Health 2010, 10, 596. [Google Scholar] [CrossRef]
- Whittle, J.G. Attendance patterns and dental health of parents and children. Community Dent. Health 1993, 10, 235–242. [Google Scholar] [PubMed]
- Rajab, L.D.; Petersen, P.E.; Bakaeen, G.; Hamdan, M.A. Oral health behaviour of schoolchildren and parents in Jordan. Int. J. Paediatr. Dent. 2002, 12, 168–176. [Google Scholar] [CrossRef] [PubMed]
- Dosreis, S.; Barksdale, C.L.; Sherman, A.; Maloney, K.; Charach, A. Stigmatizing Experiences of Parents of Children With a New Diagnosis of ADHD. Psychiatr. Serv. 2010, 61, 811–816. [Google Scholar] [CrossRef] [PubMed]
- Schnyder, N.; Panczak, R.; Groth, N.; Schultze-Lutter, F. Association between mental health-related stigma and active help-seeking: Systematic review and meta-analysis. Br. J. Psychiatry 2017, 210, 261–268. [Google Scholar] [CrossRef]
- Corrigan, P.W.; Michaels, P.J.; Vega, E.; Gause, M.; Watson, A.C.; Rüsch, N. Self-stigma of mental illness scale—Short form: Reliability and validity. Psychiatry Res. 2012, 199, 65–69. [Google Scholar] [CrossRef]
- Bundesministerium für Bildung und Forschung. Allgemeinbildende Schulen—Datenportal des BMBF. 2022. Available online: https://www.datenportal.bmbf.de/portal/de/G202.html (accessed on 28 July 2022).
- PONS Langenscheidt GmbH. Hauptschule—Deutsch-Englisch Übersetzung|PONS. 2022. Available online: https://de.pons.com/%C3%BCbersetzung/deutsch-englisch/Hauptschule (accessed on 22 July 2022).
- Statistisches Bundesamt. Abschluss der Allgemeinbildenden Polytechnischen Ober-Schule der Ehemaligen DDR. 2022. Available online: https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bildung-Forschung-Kultur/Bildungsstand/Glossar/abschluss-polytechnische-oberschule-DDR.html (accessed on 28 July 2022).
- Weiss, A.A. Specification tests in ordered logit and probit models. Econ. Rev. 1997, 16, 361–391. [Google Scholar] [CrossRef]
- Daykin, A.R.; Moffatt, P.G. Analyzing Ordered Responses: A Review of the Ordered Probit Model. Underst. Stat. 2002, 1, 157–166. [Google Scholar] [CrossRef]
- Sari, R.; Soytaş, U. Income and Education in Turkey: A Multivariate Analysis. Educ. Econ. 2006, 14, 181–196. [Google Scholar] [CrossRef]
- Henderson, C.; Evans-Lacko, S.; Flach, C.; Thornicroft, G. Responses to Mental Health Stigma Questions: The Importance of Social Desirability and Data Collection Method. Can. J. Psychiatry 2012, 57, 152–160. [Google Scholar] [CrossRef]
- Sayal, K.; Tischler, V.; Coope, C.; Robotham, S.; Ashworth, M.; Day, C.; Tylee, A.; Simonoff, E. Parental help-seeking in primary care for child and adolescent mental health concerns: Qualitative study. Br. J. Psychiatry 2010, 197, 476–481. [Google Scholar] [CrossRef]
- Dempster, R.; Davis, D.W.; Jones, V.F.; Keating, A.; Wildman, B. The Role of Stigma in Parental Help-Seeking for Perceived Child Behavior Problems in Urban, Low-Income African American Parents. J. Clin. Psychol. Med. Settings 2015, 22, 265–278. [Google Scholar] [CrossRef] [PubMed]
- Gulliver, A.; Griffiths, K.M.; Christensen, H. Perceived barriers and facilitators to mental health help-seeking in young people: A systematic review. BMC Psychiatry 2010, 10, 113. [Google Scholar] [CrossRef] [PubMed]
- Stiffman, A.R.; Pescosolido, B.; Cabassa, L.J. Building a model to understand youth service access: The gateway provider model. Ment. Health Serv. Res. 2004, 6, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Panda, P.K.; Gupta, J.; Chowdhury, S.R.; Kumar, R.; Meena, A.K.; Madaan, P.; Sharawat, I.K.; Gulati, S. Psychological and Behavioral Impact of Lockdown and Quarantine Measures for COVID-19 Pandemic on Children, Adolescents and Caregivers: A Systematic Review and Meta-Analysis. J. Trop. Pediatr. 2021, 67, fmaa122. [Google Scholar] [CrossRef] [PubMed]
- Samji, H.; Wu, J.; Ladak, A.; Vossen, C.; Stewart, E.; Dove, N.; Long, D.; Snell, G. Review: Mental health im-pacts of the COVID-19 pandemic on children and youth—A systematic review. Child Adolesc. Ment. Health 2022, 27, 173–189. [Google Scholar] [CrossRef] [PubMed]
- Ravens-Sieberer, U.; Erhart, M.; Devine, J.; Gilbert, M.; Reiss, F.; Barkmann, C.; Siegel, N.; Simon, A.; Hurrelmann, K.; Schlack, R.; et al. Child and Adolescent Mental Health During the COVID-19 Pandemic: Results of the Three-Wave Longitudinal COPSY Study. J. Adolesc. Health 2022, 71, 570–578. [Google Scholar] [CrossRef]
- Ajzen, I. The Theory of Planned Behavior. Organ. Behav. Hum. Decis. Process. 1991, 50, 179–211. [Google Scholar] [CrossRef]
- White, K.M.; Wellington, L. Predicting Participation in Group Parenting Education in an Australian Sample: The Role of Attitudes, Norms, and Control Factors. J. Prim. Prev. 2009, 30, 173–189. [Google Scholar] [CrossRef]
- Vogel, D.L.; Wade, N.G.; Hackler, A.H. Perceived public stigma and the willingness to seek counseling: The mediating roles of self-stigma and attitudes toward counseling. J. Couns. Psychol. 2007, 54, 40–50. [Google Scholar] [CrossRef]
- Berger-Jenkins, E.; McKay, M.; Newcorn, J.; Bannon, W.; Laraque, D. Parent Medication Concerns Predict Underutilization of Mental Health Services for Minority Children With ADHD. Clin. Pediatr. 2011, 51, 65–76. [Google Scholar] [CrossRef]
- Alonzo, D.; Popescu, M. Utilizing social media platforms to promote mental health awareness and help seek-ing in underserved communities during the COVID-19 pandemic. J. Educ. Health Promot. 2021, 10, 156. [Google Scholar] [CrossRef] [PubMed]
- Rüsch, N. Was tun gegen Stigma und seine Folgen? Übersicht zu Antistigma-Programmen in verschiedenen Be-reichen. Kerbe-Forum Für Soz. Psychiatr. 2022, 40, 22–24. [Google Scholar]
- Saha, K.; Torous, J.; Ernala, S.K.; Rizuto, C.; Stafford, A.; De Choudhury, M. A computational study of mental health awareness campaigns on social media. Transl. Behav. Med. 2019, 9, 1197–1207. [Google Scholar] [CrossRef] [PubMed]
- Lambert, M.; Härter, M.; Arnold, D.; Dirmaier, J.; Tlach, L.; Liebherz, S.; Sänger, S.; Karow, A.; Brandes, A.; Sielaff, G.; et al. Verbesserung von Aufklärung, Wissen und Stigmatisierung psychischer Erkrankungen in der Hamburger Bevölkerung. Psychiatr. Prax. 2015, 42, S9–S13. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, S.; Foo, J.C.; Nishida, A.; Ogawa, S.; Togo, F.; Sasaki, T. Mental health literacy programs for school teachers: A systematic review and narrative synthesis. Early Interv. Psychiatry 2019, 14, 14–25. [Google Scholar] [CrossRef]
- Corrigan, P.W.; Morris, S.B.; Michaels, P.J.; Rafacz, J.D.; Rüsch, N. Challenging the Public Stigma of Mental Illness: A Meta-Analysis of Outcome Studies. Psychiatr. Serv. 2012, 63, 963–973. [Google Scholar] [CrossRef]
- Graves, R.E.; Chandon, S.T.; Cassisi, J. Natural contact and stigma towards schizophrenia in African Americans: Is perceived dangerousness a threat or challenge response? Schizophr. Res. 2011, 130, 271–276. [Google Scholar] [CrossRef]
| Characteristics of Participants in Main Sample (N = 1928) | ||
|---|---|---|
| Gender | 924 (47.93%) Male, 1003 (52.02%) Female, 1 (0.05%) Nonbinary | |
| Age | Min: 16; Max: 101; Mean: 55.36; Standard Deviation: 15.30 | |
| Education | 1 (0.05%) | not specified/other graduation |
| 5 (0.26%) | pupil of a general education school | |
| 42 (2.18%) | without main school diploma | |
| 577 (29.93%) | main school diploma | |
| 603 (31.28%) | secondary school leaving certificate | |
| 219 (11.36%) | graduation from polytechnic high school | |
| 65 (3.37%) | specialized school degree | |
| 224 (11.62%) | general/subject-linked university entrance qualification | |
| 192 (9.96%) | completed university studies/studies at a university of applied sciences | |
| Equivalent income | 169 (8.77%) | < EUR 1000 |
| 400 (20.75%) | EUR 1000–149,999 | |
| 523 (27.13%) | EUR 1500–199,999 | |
| 458 (23.76%) | EUR 2000–249,999 | |
| 378 (19.61%) | > EUR 2500 | |
| Adult history of psychotherapy | 70 (3.63%) | Current psychotherapeutic/psychiatric treatment |
| 214 (11.10%) | Previous psychotherapeutic/psychiatric treatment | |
| 1644 (85.27%) | Never had a psychotherapeutic/psychiatric treatment | |
| Family status | 2 (0.10%) | No answer |
| 723 (37.50%) | No children | |
| 712 (36.93%) | Child(ren) and married/cohabitating | |
| 491 (25.47%) | Child(ren) and single/divorced/widowed/married and living separately | |
| Readiness to disclose mental health problems to social environment | 9 (0.47%) | No answer |
| 202 (10.48%) | I totally disagree | |
| 268 (13.90%) | I agree less | |
| 624 (32.37%) | I partly agree | |
| 474 (24.59%) | I pretty much agree | |
| 351 (18.21%) | I fully agree | |
| Readiness to disclose physical/somatic health problems to social environment | 13 (0.67%) | No answer |
| 119 (6.17%) | I totally disagree | |
| 235 (12.19%) | I agree less | |
| 621 (32.21%) | I partly agree | |
| 538 (27.90%) | I pretty much agree | |
| 402 (20.85%) | I fully agree | |
| Dependent Variable | Adult Help-Seeking for Children | |
|---|---|---|
| Independent Variables | Model 1 | Model 2 |
| Stigmatizing attitudes | −0.05 *** (0.005) | −0.01 *** (0.003) |
| Gender | 0.04 * (0.02) | |
| Age | −0.001 * (0.001) | |
| Education | 0.004 (0.01) | |
| Income | −0.3 × 10−4 ** (9.55 × 10−6) | |
| Adult history of psychotherapy | 0.04 ƚ (0.02) | |
| Preventive health care | 0.02 *** (0.005) | |
| Family status | 0.01 (0.01) | |
| Readiness to disclose health problems | 0.08 *** (0.02) | |
| Cut 1 | −1.92 (0.12) | −0.26 (0.07) |
| Cut 2 | −1.58 (0.10) | −0.06 (0.07) |
| Cut 3 | −1.00 (0.07) | 0.25 (0.10) |
| Cut 4 | −0.40 (0.05) | 0.53 (0.14) |
| Log likelihood | −2524.19 | −2256.69 |
| LR Chi2 | 140.38 *** | 522.74 *** |
| LR test on homogeneity | 18.56 *** | 89.79 *** |
| N | 1906 | 1906 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lange, S.; Gossmann, E.; Hofmann, S.; Fegert, J.M. Condemn or Treat? The Influence of Adults’ Stigmatizing Attitudes on Mental Health Service Use for Children. Int. J. Environ. Res. Public Health 2022, 19, 15951. https://doi.org/10.3390/ijerph192315951
Lange S, Gossmann E, Hofmann S, Fegert JM. Condemn or Treat? The Influence of Adults’ Stigmatizing Attitudes on Mental Health Service Use for Children. International Journal of Environmental Research and Public Health. 2022; 19(23):15951. https://doi.org/10.3390/ijerph192315951
Chicago/Turabian StyleLange, Stephanie, Emily Gossmann, Sophie Hofmann, and Jörg M. Fegert. 2022. "Condemn or Treat? The Influence of Adults’ Stigmatizing Attitudes on Mental Health Service Use for Children" International Journal of Environmental Research and Public Health 19, no. 23: 15951. https://doi.org/10.3390/ijerph192315951
APA StyleLange, S., Gossmann, E., Hofmann, S., & Fegert, J. M. (2022). Condemn or Treat? The Influence of Adults’ Stigmatizing Attitudes on Mental Health Service Use for Children. International Journal of Environmental Research and Public Health, 19(23), 15951. https://doi.org/10.3390/ijerph192315951







