Noise Indicators Relating to Non-Auditory Health Effects in Children—A Systematic Literature Review
Abstract
1. Introduction
2. Procedure
2.1. Search and Screening Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Search Procedure
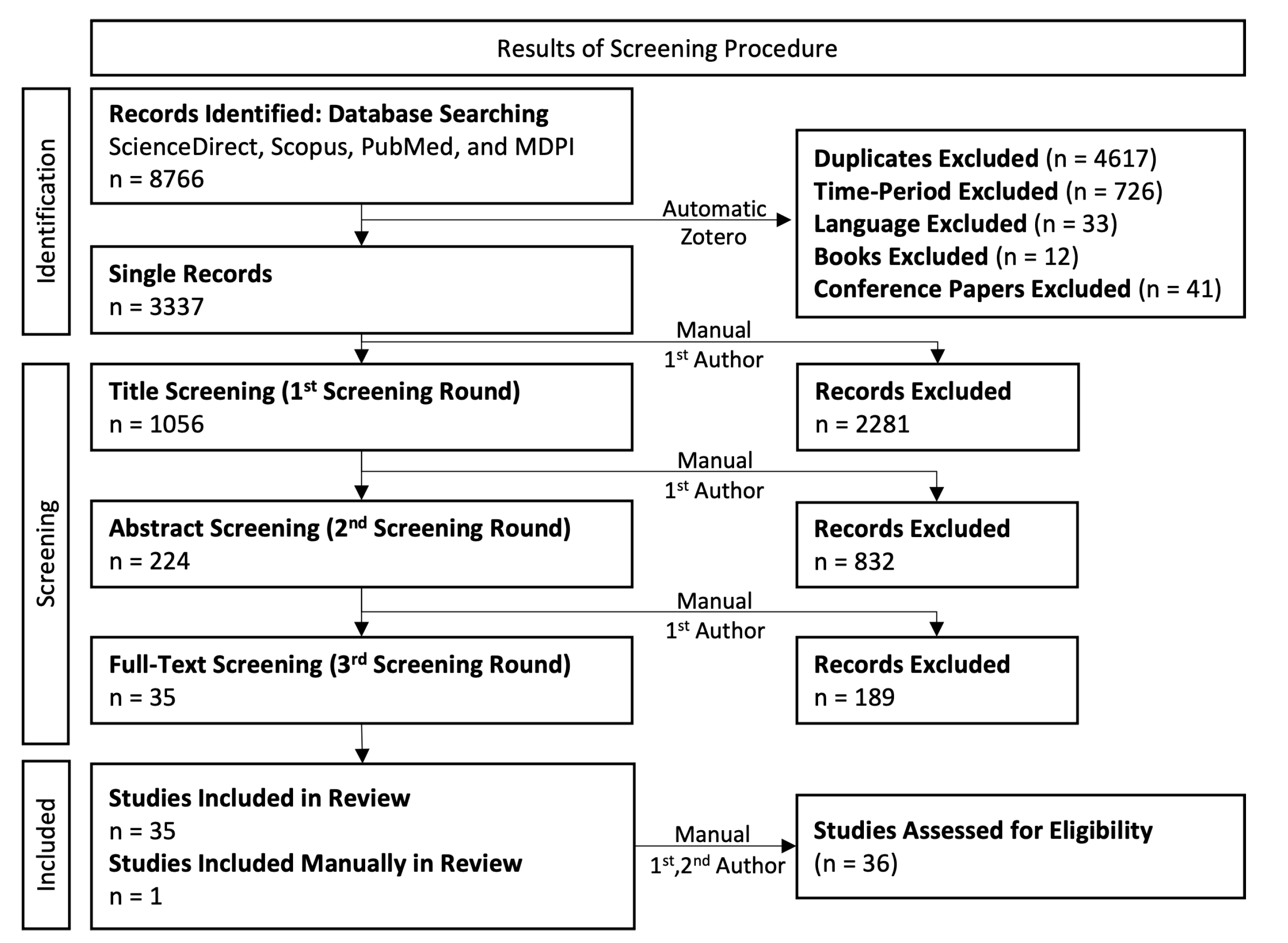
2.4. Screening Procedure
2.5. Criteria for Assessing the Risk of Bias
3. Results
3.1. Results Overview per Health-Effect
3.2. Noise-Induced Effects and Noise Indicators
3.2.1. Cardiovascular Effects
3.2.2. Neuroendocrine Effects
3.2.3. Cognitive Development Effects
3.2.4. Cognitive Performance Effects
3.2.5. Well-Being Dimensions
3.2.6. Mental Health Effects
3.2.7. Sleep Effects
4. Discussion
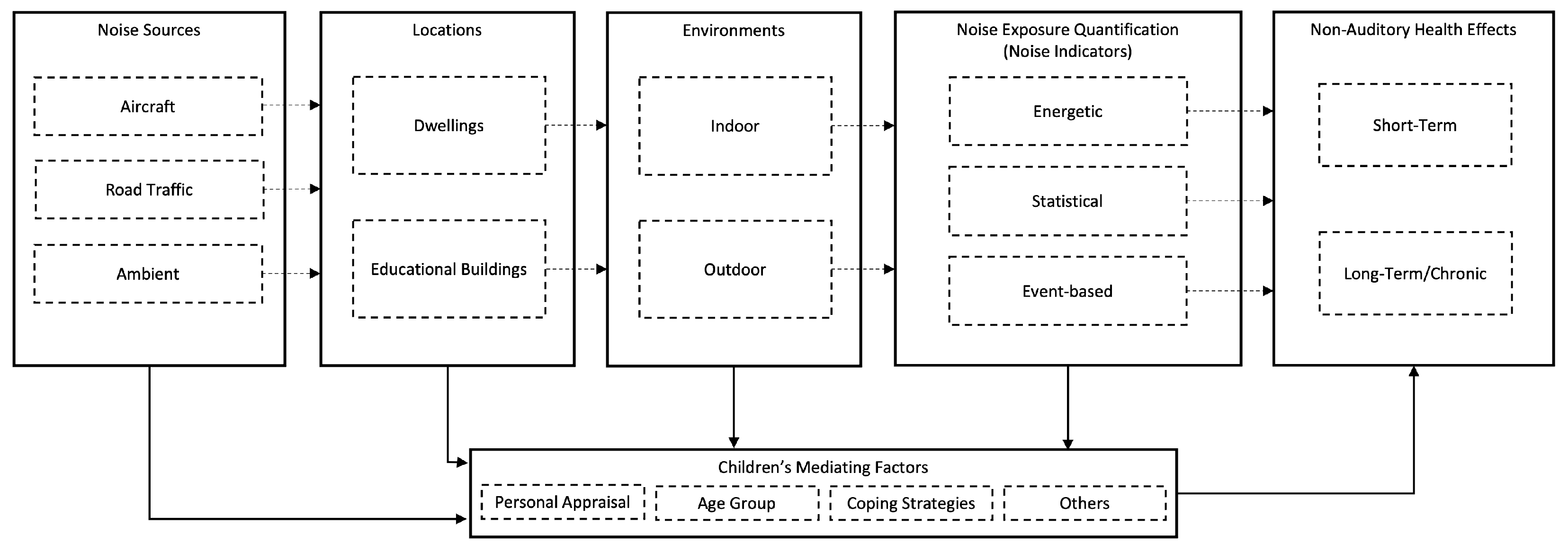
4.1. Conceptual Framework
4.1.1. Noise Source
4.1.2. Locations and Environments
4.1.3. Noise Indicators
4.1.4. Children and Mediating Factors
4.1.5. Matching between Noise Indicators and Noise-Induced Health Effects
4.2. Quality of Evidence
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stansfeld, S.; Haines, M.; Brown, B. Noise and health in the urban environment. Rev. Environ. Health 2000, 15, 43–82. [Google Scholar] [CrossRef] [PubMed]
- van Kamp, I.; Davies, H. Noise and health in vulnerable groups: A review. Noise Health 2013, 15, 153. [Google Scholar] [CrossRef] [PubMed]
- Stansfeld, S.; Clark, C. Health Effects of Noise Exposure in Children. Curr. Environ. Health Rep. 2015, 2, 171–178. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Burden of Disease from Environmental Noise Burden of Disease from Environmental Noise. Quantification of Healthy Life Years Lost in Europe; WHO: Geneva, Switzerland, 2011.
- Park, B.; Choi, H.G.; Lee, H.J.; An, S.Y.; Kim, S.W.; Lee, J.S.; Hong, S.K.; Kim, H.J. Analysis of the Prevalence of and Risk Factors for Tinnitus in a Young Population. Otol. Neurotol. 2014, 35, 1218–1222. [Google Scholar] [CrossRef]
- Evans, G.W.; Monika, B.; Staffan, H. Chronic Noise Exposure and Physiological Response: A Prospective Study of Children Living under Environmental Stress. Psychol. Sci. 1998, 9, 75–77. [Google Scholar] [CrossRef]
- Cohen, S.; Evans, G.W.; Krantz, D.S.; Stokols, D. Physiological, Motivational, and Cognitive Effects of Aircraft Noise on Children Moving from the Laboratory to the Field. Am. Psychol. 1980, 35, 231–243. [Google Scholar] [CrossRef] [PubMed]
- Weinmann, T.; Ehrenstein, V.; Kries, R.V.; Nowak, D.; Radon, K. Subjective and objective personal noise exposure and hypertension: An epidemiologic approach. Int. Arch. Occup. Environ. Health 2012, 85, 363–371. [Google Scholar] [CrossRef] [PubMed]
- Evans, G.W.; Staffan, H.; Monika, B. Chronic Noise and Psychological Stress. Psychol. Stress 1995, 6, 333–338. [Google Scholar] [CrossRef]
- Evans, G.W.; Lercher, P.; Meis, M.; Ising, H.; Kofler, W.W. Community noise exposure and stress in children. J. Acoust. Soc. Am. 2001, 109, 1023–1027. [Google Scholar] [CrossRef]
- Ising, H.; Rebentisch, E.; Babisch, W.; Sharp, D.; Baumgsrtner, H. Medically Relevant Effects of Noise from Military Low-Altitude Flights-Results of an Interdisciplinary Pilot Study. Environ. Int. 1990, 16, 411–423. [Google Scholar] [CrossRef]
- Cohen, S.; Glass, D.C.; Singer, J.E. Apartment Noise, Auditory Discrimination, and Reading Ability in Children. J. Exp. Soc. Psychol. 1973, 9, 407–422. [Google Scholar] [CrossRef]
- Hygge, S.; Evans, G.W.; Bullinger, M. A Prospective Study of Some Effects of Aircraft Noise on Cognitive Performance in Schoolchildren. Psychol. Sci. 2002, 13, 469–474. [Google Scholar] [CrossRef] [PubMed]
- Ando, Y.; Nakane, Y.; J, J.E. Effects of Aircraft Noise on the Mental Work of Pupils. J. Sound Vib. 1975, 43, 683–691. [Google Scholar] [CrossRef]
- Bullinger, M.; Hygge, S.; Evans, G.; Meis, M.; Mackensen, S. The Psychological Cost of Aircraft Noise for Children* Psychologische Beeintrachtigung von Kindern durch Fluglarm. Zentralblatt Hyg. Umweltmed. 1998, 202, 99. [Google Scholar]
- Eberhardt, J.L. The Influence of Road Traffic Noise on Sleep. J. Sound Vib. 1988, 127, 449–455. [Google Scholar] [CrossRef]
- Ising, H.; Ising, M. Chronic Cortisol Increases in the First Half of the Night Caused by Road Traffic Noise. Noise Health 2002, 4, 13–21. [Google Scholar] [PubMed]
- Christensen, J.S.; Hjortebjerg, D.; Raaschou-Nielsen, O.; Ketzel, M.; Sørensen, T.I.; Sørensen, M. Pregnancy and childhood exposure to residential traffic noise and overweight at 7 years of age. Environ. Int. 2016, 94, 170–176. [Google Scholar] [CrossRef] [PubMed]
- Dzhambov, A.M.; Markevych, I.; Lercher, P. Associations of residential greenness, traffic noise, and air pollution with birth outcomes across Alpine areas. Sci. Total Environ. 2019, 678, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Schell, L.M. Environmental Noise and Human Prenatal Growth. Am. J. Phys. Anthropol. 1981, 56, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Schell, L.M.; Ando, Y. Postnatal Growth of Children in Relation to Noise From Osaka International Airport. J. Sound Vib. 1991, 151, 371–382. [Google Scholar] [CrossRef]
- Bistrup, M. Prevention of Adverse Effects of Noise on Children. Noise Health 2003, 5, 59–64. [Google Scholar] [PubMed]
- Münzel, T.; Gori, T.; Babisch, W.; Basner, M. Cardiovascular effects of environmental noise exposure. Eur. Heart J. 2014, 35, 829–836. [Google Scholar] [CrossRef] [PubMed]
- Staatsen, B.A.M.; Nijland, H.A.; van Kempem, E.M.M.; de Hollander, A.E.M.; Franssen, A.E.M.; van Kamp, I. Assessment of Health Impacts and Policy Options in Relation to Transport-Related Noise Exposures; RIVM: Utrecht, The Netherlands, 2004.
- Porter, N.; Kershaw, A.; Ollerhead, J. Adverse Effects of Night-Time Aircraft Noise: Review of 1992 UK Findings and Introduction to New UK Work. In Proceedings of the 29th International Congress and Exhibition on Noise Control Engineering, Nice, France, 27–30 August 2000. [Google Scholar]
- Spreng, M. Noise induced nocturnal cortisol secretion and tolerable overhead flights. Noise Health 2004, 6, 35. [Google Scholar] [PubMed]
- Babisch, W.; Ising, H.; Gallacher, J. Health status as a potential effect modifier of the relation between noise annoyance and incidence of ischaemic heart disease. Occup. Environ. Med. 2003, 60, 739–745. [Google Scholar] [CrossRef] [PubMed]
- Brink, M. A review of potential mechanisms in the genesis of long-term health effects due to noise-induced sleep disturbances. In Proceedings of the Internoise 2012—41st International Congress on Noise Control Engineering, New York, NY, USA, 19–22 August 2012. [Google Scholar]
- Lavandier, C.; Delaitre, P.; Ribeiro, C. Global and local sound quality indicators for urban context based on perceptive and acoustic variables. In Proceedings of the Euronoise 2015, Maastricht, The Netherlands, 31 May–3 June 2015; pp. 1471–1476. [Google Scholar]
- Bartalucci, C.; Borchi, F.; Carfagni, M.; Governi, L.; Luzzi, S.; Aspuru, I.; Gaudibert, P.; Wolfert, H. LIFE+2010 QUADMAP Project: Results obtained from the analysis of data collected during the application of the new methodology to the pilot quiet areas. Noise Mapp. 2019, 6, 22–37. [Google Scholar] [CrossRef]
- Shield, B.M.; Dockrell, J.E. The Effects of Noise on Children at School: A Review. Build. Acoust. 2003, 10, 97–116. [Google Scholar] [CrossRef]
- Can, A.; Aumond, P.; Michel, S.; de Coensel, B.; Ribeiro, C.; Botteldooren, D.; Lavandier, C. Comparison of noise indicators in an urban context. In Proceedings of the Inter-Noise 2016, 45th International Congress and Exposition of Noise Control Engineering, Hamburg, Germany, 21–24 August 2016. [Google Scholar]
- Makarewicz, R.; Galuszka, M.; Kokowski, P. Evaluation of aircraft noise measurements. Noise Control Eng. J. 2014, 62, 83–89. [Google Scholar] [CrossRef]
- Sofaer, N.; Stratch, D. The need for systematic reviews of reasons. Bioethics 2012, 26, 315–328. [Google Scholar] [CrossRef]
- World Health Organization. WHO Handbook for Guideline Development; WHO: Geneva, Switzerland, 2012. [Google Scholar]
- Van Kempen, E.; Casas, M.; Pershagen, G.; Foraster, M. Cardiovascular and Metabolic Effects of Environmental Noise Systematic Evidence Review in the Framework of the Development of the WHO Environmental Noise Guidelines for the European Region; RIVM: Utrecht, The Netherlands, 2017.
- Wallas, A.E.; Eriksson, C.; Bonamy, A.K.E.; Gruzieva, O.; Kull, I.; Ögren, M.; Pyko, A.; Sjöström, M.; Pershagen, G. Traffic noise and other determinants of blood pressure in adolescence. Int. J. Hyg. Environ. Health 2019, 222, 824–830. [Google Scholar] [CrossRef]
- Babisch, W.; Neuhauser, H.; Thamm, M.; Seiwert, M. Blood pressure of 8–14 year old children in relation to traffic noise at home—Results of the German Environmental Survey for Children (GerES IV). Sci. Total Environ. 2009, 407, 5839–5843. [Google Scholar] [CrossRef]
- Belojevic, G.; Jakovljevic, B.; Stojanov, V.; Paunovic, K.; Ilic, J. Urban road-traffic noise and blood pressure and heart rate in preschool children. Environ. Int. 2008, 34, 226–231. [Google Scholar] [CrossRef]
- Van Kempen, E.; van Kamp, I.; Nilsson, M.; Lammers, J.; Emmen, H.; Clark, C.; Stansfeld, S. The role of annoyance in the relation between transportation noise and children’s health and cognition. J. Acoust. Soc. Am. 2010, 128, 2817–2828. [Google Scholar] [CrossRef] [PubMed]
- Lercher, P.; Evans, G.W.; Widmann, U. The ecological context of soundscapes for children’s blood pressure. J. Acoust. Soc. Am. 2013, 134, 773–781. [Google Scholar] [CrossRef] [PubMed]
- Wallas, A.; Eriksson, C.; Gruzieva, O.; Lind, T.; Pyko, A.; Sjöström, M.; Ögren, M.; Pershagen, G. Road traffic noise and determinants of saliva cortisol levels among adolescents. Int. J. Hyg. Environ. Health 2018, 221, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Cantuaria, M.L.; Usemann, J.; Proietti, E.; Blanes-Vidal, V.; Dick, B.; Flück, C.E.; Rüedi, S.; Héritier, H.; Wunderli, J.M.; Latzin, P.; et al. Glucocorticoid metabolites in newborns: A marker for traffic noise related stress? Environ. Int. 2018, 117, 319–326. [Google Scholar] [CrossRef]
- Haines, N.; Stansfeld, S.; Job, R.; Berglund, B.; Head, J. Chronic aircraft noise exposure, stress responses, mental health and cognitive performance in school children. Psychol. Med. 2001, 31, 265–277. [Google Scholar] [CrossRef] [PubMed]
- Clark, C.; Head, J.; Stansfeld, S.A. Longitudinal effects of aircraft noise exposure on children’s health and cognition: A six-year follow-up of the UK RANCH cohort. J. Environ. Psychol. 2013, 35, 1–9. [Google Scholar] [CrossRef]
- Klatte, M.; Spilski, J.; Mayerl, J.; Möhler, U.; Lachmann, T.; Bergström, K. Effects of Aircraft Noise on Reading and Quality of Life in Primary School Children in Germany: Results From the NORAH Study. Environ. Behav. 2017, 49, 390–424. [Google Scholar] [CrossRef]
- Stansfeld, S.; Berglund, B.; Clark, C.; Lopez-Barrio, I.; Fischer, P.; Öhrström, E.; Haines, M.; Head, J.; Hygge, S.; van Kamp, I.; et al. Aircraft and road traffic noise and children’s cognition and health: A cross-national study. Lancet 2005, 365, 1942–1949. [Google Scholar] [CrossRef] [PubMed]
- Seabi, J.; Cockcroft, K.; Goldschagg, P.; Greyling, M. A prospective follow-up study of the effects of chronic aircraft noise exposure on learners’ reading comprehension in South Africa. J. Expo. Sci. Environ. Epidemiol. 2015, 25, 84–88. [Google Scholar] [CrossRef]
- Haines, M.; Stansfeld, S.; Soames Job, R.; Berglund, B.; Head, J. A follow-up study of effects of chronic aircraft noise exposure on child stress responses and cognition. Int. J. Epidemiol. 2001, 30, 839–845. [Google Scholar] [CrossRef] [PubMed]
- Clark, C.; Martin, R.; Kempen, E.V.; Alfred, T.; Head, J.; Davies, H.W.; Haines, M.M.; Barrio, I.L.; Matheson, M.; Stansfeld, S.A. Exposure-effect relations between aircraft and road traffic noise exposure at school and reading comprehension: The RANCH project. Am. J. Epidemiol. 2006, 163, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Matsui, T.; Stansfeld, S.; Haines, M.; Head, J. Children’s Cognition and Aircraft Noise Exposure at Home—The West London Schools Study. Noise Health 2004, 7, 49–58. [Google Scholar] [PubMed]
- Matheson, M.; Clark, C.; Martin, R.; van Kempen, I.; Haines, M.; Lopez-Bario, I.; Hygge, S.; Stansfeld, S. The Effects of Road Traffic Noise Exposure on children’s Episodic Memory: The RANCH Project. Noise Health 2010, 12, 244–254. [Google Scholar] [PubMed]
- Xie, H.; Kang, J.; Tompsett, R. The impacts of environmental noise on the academic achievements of secondary school students in Greater London. Appl. Acoust. 2011, 72, 551–555. [Google Scholar] [CrossRef]
- Pujol, S.; Levain, J.P.; Houot, H.; Petit, R.; Berthillier, M.; Defrance, J.; Lardies, J.; Masselot, C.; Mauny, F. Association between ambient noise exposure and school performance of children living in an urban area: A cross-sectional population-based study. J. Urban Health 2014, 91, 256–271. [Google Scholar] [CrossRef] [PubMed]
- Haines, M.M.; Stansfeld, S.A.; Head, J.; Job, R.F. Multilevel modelling of aircraft noise on performance tests in schools around Heathrow Airport London. J. Epidemiol. Community Health 2002, 56, 139–144. [Google Scholar] [CrossRef]
- Shield, B.M.; Dockrell, J.E. The effects of environmental and classroom noise on the academic attainments of primary school children. J. Acoust. Soc. Am. 2008, 123, 133–144. [Google Scholar] [CrossRef] [PubMed]
- Van Kempen, E.; van Kamp, I.; Lebret, E.; Lammers, J.; Emmen, H.; Stansfeld, S. Neurobehavioral effects of transportation noise in primary schoolchildren: A cross-sectional study. Environ. Health 2010, 9, 25. [Google Scholar] [CrossRef] [PubMed]
- Ali, S.A.A. Study effects of school noise on learning achievement and annoyance in Assiut city, Egypt. Appl. Acoust. 2013, 74, 602–606. [Google Scholar] [CrossRef]
- Silva, L.T.; Oliveira, I.S.; Silva, J.F. The impact of urban noise on primary schools. Perceptive evaluation and objective assessment. Appl. Acoust. 2016, 106, 2–9. [Google Scholar] [CrossRef]
- van Kempen, E.E.; van Kamp, I.; Stellato, R.K.; Lopez-Barrio, I.; Haines, M.M.; Nilsson, M.E.; Clark, C.; Houthuijs, D.; Brunekreef, B.; Berglund, B.; et al. Children’s annoyance reactions to aircraft and road traffic noise. J. Acoust. Soc. Am. 2009, 125, 895–904. [Google Scholar] [CrossRef] [PubMed]
- Minichilli, F.; Gorini, F.; Ascari, E.; Bianchi, F.; Coi, A.; Fredianelli, L.; Licitra, G.; Manzoli, F.; Mezzasalma, L.; Cori, L. Annoyance judgment and measurements of environmental noise: A focus on italian secondary schools. Int. J. Environ. Res. Public Health 2018, 15, 208. [Google Scholar] [CrossRef] [PubMed]
- Birk, M.; Ivina, O.; Klot, S.V.; Babisch, W.; Heinrich, J. Road traffic noise: Self-reported noise annoyance versus GIS modelled road traffic noise exposure. J. Environ. Monit. 2011, 13, 3237–3245. [Google Scholar] [CrossRef]
- Dockrell, J.E.; Shield, B. Children’s perceptions of their acoustic environment at school and at home. J. Acoust. Soc. Am. 2004, 115, 2964–2973. [Google Scholar] [CrossRef] [PubMed]
- Tiesler, C.M.; Birk, M.; Thiering, E.; Kohlböck, G.; Koletzko, S.; Bauer, C.P.; Berdel, D.; Berg, A.V.; Babisch, W.; Heinrich, J.; et al. Exposure to road traffic noise and children’s behavioural problems and sleep disturbance: Results from the GINIplus and LISAplus studies. Environ. Res. 2013, 123, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Stansfeld, S.A.; Clark, C.; Cameron, R.M.; Alfred, T.; Head, J.; Haines, M.M.; van Kamp, I.; van Kempen, E.; Lopez-Barrio, I. Aircraft and road traffic noise exposure and children’s mental health. J. Environ. Psychol. 2009, 29, 203–207. [Google Scholar] [CrossRef]
- Hjortebjerg, D.; Andersen, A.M.N.; Christensen, J.S.; Ketzel, M.; Raaschou-Nielsen, O.; Sunyer, J.; Julvez, J.; Forns, J.; Sørensen, M. Exposure to road traffic noise and behavioral problems in 7-year-old children: A cohort study. Environ. Health Perspect. 2016, 124, 228–234. [Google Scholar] [CrossRef]
- Weyde, K.V.; Krog, N.H.; Oftedal, B.; Evandt, J.; Magnus, P.; Øverland, S.; Clark, C.; Stansfeld, S.; Aasvang, G.M. Nocturnal road traffic noise exposure and children’s sleep duration and sleep problems. Int. J. Environ. Res. Public Health 2017, 14, 491. [Google Scholar] [CrossRef] [PubMed]
- Lim, J.; Kweon, K.; Kim, H.W.; Cho, S.W.; Park, J.; Sim, C.S. Negative impact of noise and noise sensitivity on mental health in childhood. Noise Health 2018, 20, 199–211. [Google Scholar] [PubMed]
- Crombie, R.; Clark, C.; Stansfeld, S.A. Environmental noise exposure, early biological risk and mental health in nine to ten year old children: A cross-sectional field study. Environ. Health 2011, 10, 39. [Google Scholar] [CrossRef] [PubMed]
- Belojevic, G.; Evans, G.W.; Paunovic, K.; Jakovljevic, B. Traffic noise and executive functioning in urban primary school children: The moderating role of gender. J. Environ. Psychol. 2012, 32, 337–341. [Google Scholar] [CrossRef]
- Öhrström, E.; Hadzibajramovic, E.; Holmes, M.; Svensson, H. Effects of road traffic noise on sleep: Studies on children and adults. J. Environ. Psychol. 2006, 26, 116–126. [Google Scholar] [CrossRef]
- Weyde, K.V.; Krog, N.H.; Oftedal, B.; Magnus, P.; Øverland, S.; Stansfeld, S.; Nieuwenhuijsen, M.J.; Vrijheid, M.; Pascual, M.D.C.; Aasvang, G.M. Road traffic noise and children’s inattention. Environ. Health 2017, 16, 127. [Google Scholar] [CrossRef] [PubMed]
- Airports Commission. Airports Commission: Final Report; Technical Report; Airports Commission: London, UK, 2015.
- Locher, B.; Piquerez, A.; Habermacher, M.; Ragettli, M.; Röösli, M.; Brink, M.; Cajochen, C.; Vienneau, D.; Foraster, M.; Müller, U.; et al. Differences between Outdoor and Indoor Sound Levels for Open, Tilted, and Closed Windows. Int. J. Environ. Res. Public Health 2018, 15, 149. [Google Scholar] [CrossRef] [PubMed]
- Kelly, Y.; Kelly, J.; Sacker, A. Time for bed: Associations with cognitive performance in 7-year-old children: A longitudinal population-based study. J. Epidemiol. Community Health 2013, 67, 926–931. [Google Scholar] [CrossRef] [PubMed]
- Zannin, P.H.T.; Marcon, C.R. Objective and subjective evaluation of the acoustic comfort in classrooms. Appl. Ergon. 2007, 38, 675–680. [Google Scholar] [CrossRef] [PubMed]
- Jahangeer, F. Acoustic comfort in the living environment and its association with noise representation: A systematic review. SHS Web Conf. 2019, 64, 3–12. [Google Scholar] [CrossRef][Green Version]
- Rasmussen, B. Sound insulation between dwellings—Comparison of national requirements in Europe and interaction with acoustic classification schemes. In Proceedings of the 23rd International Congress on Acoustics, Aachen, Germany, 9–13 September 2019. [Google Scholar]
- Secchi, S.; Brambilla, G.; Casini, D.; Cellai, G. A Method to Estimate Students’ Exposure to Road Traffic Noise Events. Environments 2018, 5, 39. [Google Scholar] [CrossRef]
- Berglund, B.; Lindvall, T.; Schwela, D.H. Guidelines for Community Noise; World Health Organization: Geneva, Switzerland, 1999.
- Fletcher, H.; Manson, W. Loudness, Its Definition, Measurement and Calculation. J. Acoust. Soc. Am. 1933, 5, 82–108. [Google Scholar] [CrossRef]
- Charbonneau, J.; Novak, C.; Gaspar, R.; Ule, H. A-weighting the equal loudness contours. J. Acoust. Soc. Am. 2012, 131, 3502–3508. [Google Scholar] [CrossRef]
- Gozalo, G.R.; Carmona, J.T.; Morillas, J.B.; Vílchez-Gómez, R.; Escobar, V.G. Relationship between objective acoustic indices and subjective assessments for the quality of soundscapes. Appl. Acoust. 2015, 97, 1–10. [Google Scholar] [CrossRef]
- Shepherd, D.; Heinonen-Guzejev, M.; Hautus, M.J.; Heikkilä1, K. Elucidating the relationship between noise sensitivity and personality. Noise Health 2015, 17, 165–171. [Google Scholar] [CrossRef]
- Cohen, S.; Krantz, D.S.; Evans, G.; Stokols, D.; Kelly, S. Aircraft noise and children: Longitudinal and cross-sectional evidence on adaptation to noise and the effectiveness of noise abatement. J. Personal. Soc. Psychol. 1981, 40, 331–345. [Google Scholar] [CrossRef]
- Janssen, S.A.; Centen, M.R.; Vos, H.; van Kamp, I. The effect of the number of aircraft noise events on sleep quality. Appl. Acoust. 2014, 84, 9–16. [Google Scholar] [CrossRef]
- Park, J.; Payne, C. Effects of noise level and difficulty of task in performing division. J. Appl. Psychol. 1963, 47, 367–368. [Google Scholar] [CrossRef]
| Key Terms | Search Terms |
|---|---|
| {Noise Exposure} | “noise indicator(s)”, “noise index(ces)”, “noise metric(s)”, “noise exposure”, |
| “environmental noise”, “urban noise”, “industrial noise”, “ambient noise”, | |
| “traffic noise” and “aircraft noise” | |
| {Health Effects} | annoyance, “cognitive performance”, “cognitive development”, cognition, |
| “mental disorder(s)”, “mental health”, psycho[physio]logical, rest[oration], | |
| sleep, and stress | |
| {Children} | neonatal, fetus, new-born, infant(s), baby(ies), toddler(s), adolescent(s), |
| juvenile(s), student(s), and child(ren) |
| Criterion | Inclusion | Exclusion | |
|---|---|---|---|
| (A) | Time Period | 2000–2020 | <2020 |
| (B) | Language | English | Non-English |
| (C) | Literature | Research and review articles | Books and conference papers |
| (D) | Noise Sources | Aircraft, road-traffic, and ambient * | Others |
| (E) | Noise Indicators | Objective | Subjective |
| (F) | Locations | Educational and residential buildings | Others |
| (G) | Environments | Indoor and outdoor | - |
| (H) | Health Effects | Psychophysiological, cognitive, mental, | Others |
| health, and sleep effects | |||
| (I) | Participants | Children (<18 yrs) | Adults (≥18 yrs) |
| (J) | Others | - Healthy and normal hearing children | - Unclear or absence of noise |
| - Multi-exposure and adults-children | exposure in statistical analyses | ||
| studies without combined results | - Reproduction-based noise | ||
| from loudspeakers/headphones |
| Bias Criterion | Bias Description | Risk of Bias |
|---|---|---|
| Participants’ Selection | Participants randomly selected from a known population, AND response rate higher than 60% AND attribution rate less | Low |
| than 20% in the follow-up studies. | ||
| No random sampling OR response rate less than 60% or attributional rate higher than 20%. | High | |
| No sufficient information to judge. | Unclear | |
| Health Measurement Outcome | Objectively measured outcome OR taken from medical records OR taken from questionnaire using a knowing scale or | Low |
| validated assessment method. | ||
| Self-reported and not assessed using a knowing scale or validated assessment method. | High | |
| No sufficient information to judge. | Unclear | |
| Noise Exposure Assessment | For long-term exposure: Noise exposure assessment based on measurements for at least one week, OR noise models based on | Low |
| actual traffic data OR noise maps verified by noise measurement. | ||
| For short-term exposure: Noise exposure assessed by continuous measurements during the tasks. | ||
| For long-term exposure: Measurements less than of a week or not continuous measurements | High | |
| OR models not verified by measurements or actual traffic data. For short-term exposure: | ||
| Not continuous measurements during the tasks. | ||
| No sufficient information to judge. | Unclear | |
| Confounding Factors | All the important confounders have been considered in the analysis. | Low |
| Non adjustment of the important confounding factors. | High | |
| No sufficient information to judge. | Unclear | |
| Overall Bias Rating | All four ratings to bias “Low”. | Low |
| One or more “High” or “Unclear”. | High |
| Health Effect | Health Aspect | Parameter | Noise Source | Noise Indicators | Articles (%) |
|---|---|---|---|---|---|
| Psycho- physiological | Cardiovascular [37,38,39,40,41] | Systolic and diastolic blood pressure |   | , , | 10 |
| Neuroendocrine [41,42,43,44] | Cortisol, glucocorticoids, and metabolites |   | , , | 8 | |
| Cognitive | Development [44,45,46,47,48,49,50,51,52] | Attention, reading, short/ long-term memory |   | , | 18 |
| Performance [40,53,54,55,56,57] | Academic achievements, and cognitive functioning |    | , , , , , , , , | 12 | |
| Mental Health | Well-being Dimensions [41,44,45,46,47,49,58,59,60,61,62,63] | Annoyance, motivation, quality of life |    | , , , , , , , | 24 |
| [40,44,45,49,64,65,66,67,68,69,70] | Psychological morbidity, executive functioning, mental disorders, beha- vioural problems and dis- orders, perceived general, and mental health |    | , , , | 22 | |
| Sleep | [64,71,72] | Seep quality, waking-up episodes, sleepiness, dif- ficulties falling sleep |  | , , | 6 |
 : Aircraft noise,
: Aircraft noise,  : Road-traffic noise,
: Road-traffic noise,  : Ambient noise.
: Ambient noise. and
and  , respectively.
, respectively.
 and
and  , respectively.
, respectively.| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | |
|---|---|---|---|---|---|---|
| SBP | DBP | |||||
| Wallas et al., (2019) [37] † (n = 2597, 16 yrs) |  |  | + | + | L | |
| Babisch et al., (2009) [38] † (n = 1048, 10–14 yrs) |  |  | + | + | H | |
| Belojevic et al., (2008) [39] † (n = 328, 3–7 yrs) |  |   | + | − | H | |
| Van Kempen et al., (2010) [40] † (n = 2844, 9–11 yrs) |   |  | + | + | L | |
| Lercher et al., (2013) [41] † (n = 115, mean 10.1 yrs) |  |  | − | − | L | |
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | |||
|---|---|---|---|---|---|---|---|---|
| CL | CML | GL | GML | |||||
| Wallas et al., (2018) [42] ‡ (n = 1751, 16 yrs) |  |  | − | L | ||||
| Cantuaria et al., (2018) [43] ″ (n = 165, 5 wks) |  |  | − | + | − | + | L | |
| Haines et al., (2001) [44] † (n = 340, 8–11 yrs) |  |  | − | L | ||||
| Lercher et al., (2013) [41] † (n = 115, mean 10.1 yrs) |  |  | + | + | L | |||
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| SA | RD | WM | RGNM | RCLM | PM | |||||
| Clark et al., (2013) [45] ‡ (n = 461, 15–17 yrs) |  |  | − | L | ||||||
| Klatte et al., (2017) [46] † (n = 1243, 7–10 yrs) |  |   | , | + | H | |||||
| Stansfeld et al., (2005) [47] † (n = 2844, 9–10 yrs) |   |  | − | + | − | + | − | − | L | |
| Seabi et al., (2015) [48] ‡ (n = 650/178, 9–15/10–16 yrs) |  |  | − | H | ||||||
| Haines et al., (2001) [44] † (n = 340, 8–11 yrs) |  |  | + | − | + | − | L | |||
| Haines et al., (2001) [49] † (n = 275, 8–11 yrs) |  |  | + | + | L | |||||
| Clark et al., (2006) [50] †† (n = 2844, 9–10 yrs) |   |   | + | L | ||||||
| Matsui et al., (2004) [51] † (n = 236, 8–9 yrs) |  |  | − | − | − | + | L | |||
| Matheson et al., (2010) [52] † (n = 2844, 8–12 yrs) |   |  | + | + | − | L | ||||
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | ||||
|---|---|---|---|---|---|---|---|---|---|
| AA | LNG | MTH | SCN | CF | |||||
| Xie et al., (2011) [53] * (n = n.sp., 12–13 yrs) |  |  | − | H | |||||
| Pujol et al., (2014) [54] † (n = 587, 8–9 yrs) |  |   | , | + | + | L | |||
| Van Kempen et al., (2010) [40] † (n = 2844, 9–11 yrs) |   |  | + | L | |||||
| Haines et al., (2002) [55] † (n = 11,000, 11 yrs) |  |  | + | + | − | H | |||
| Shield et al., (2008) [56] * (n = n.sp./24, 7, 11/6–7, 10–11 yrs) |  |  | + | + | + | H | |||
| Van Kempen et al., (2010) [57] † (n = 553, 9–11 yrs) |   |   | + | L | |||||
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | ||
|---|---|---|---|---|---|---|---|
| ANN | MOT | QOL | |||||
| Clark et al., (2013) [45] ‡ (n = 461, 15–17 yrs) |  |  | + | L | |||
| Klatte et al., (2017) [46] † (n = 1243, 7–10 yrs) |  |   | , | + | + | H | |
| Ali (2013) [58] ′ (n = 300, 13–15 yrs) |  |  | + | H | |||
| Stansfeld et al., (2005) [47] † (n = 2844, 9–10 yrs) |   |  | + | L | |||
| Silva et al., (2016) [59] o (n = 213, 8–11 yrs) |  |  | , | + | H | ||
| Van Kempen et al., (2009) [60] † (n = 2844, 9–11 yrs) |   |   | + | L | |||
| Haines et al., (2001) [44] † (n = 340, 8–11 yrs) |  |  | + | − | H | ||
| Haines et al., (2001) [49] † (n = 275, 8–11 yrs) |  |  | + | L | |||
| Minichilli et al., (2018) [61] † (n = 521, 11–17 yrs) |  |  | + | H | |||
| Birk et al., (2011) [62] † (n = 951, 10 yrs) |  |  | + | H | |||
| Dockrell et al., (2004) [63] † (n = 2063, 6–7, 10–11 yrs) |  |  | + | H | |||
| Lercher et al., (2013) [41] † (n = 115, mean 10.1 yrs) |  |  | + | H | |||
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ES | CP | HI | PP | PSB | SDQ | AD | PH | BP | EF | |||||
| Clark et al., (2013) [45] ‡ (n = 461, 15–17 yrs) |  |  | − | − | − | − | L | |||||||
| Tiesler et al., (2013) [64] † (n = 872, 10 yrs) |  |  | + | − | + | − | − | − | H | |||||
| Stansfeld et al., (2009) [65] † (n = 2844, 9–10 yrs) |   |  | − | + | + | − | − | − | L | |||||
| Van Kempen et al., (2010) [40] † (n = 2844, 9–10 yrs) |   |  | − | L | ||||||||||
| Hjortebjerg et al., (2016) [66] | (n = 46,940, 9–11 yrs) |  |  | − | − | + | − | − | − | H | |||||
| Haines et al., (2001) [44] † (n = 340, 8–11 yrs) |  |  | − | − | − | − | − | − | − | L | ||||
| Haines et al., (2001) [49] † (n = 275, 8–11 yrs) |  |  | − | + | L | |||||||||
| Weyde et al., (2017) [67] †† (n = 1934/1384, 0/3–8 yrs) |  |  | + | L | ||||||||||
| Lim et al., (2018) [68] † (n = 918, 9–14 yrs) |  |  | + | H | ||||||||||
| Crombie et al., (2011) [69] † (n = 1900, 9–10 yrs) |   |  | − | + | + | − | L | |||||||
| Belojevic et al., (2012) [70] † (n = 311, 7–11 yrs) |  |   | + | H | ||||||||||
| Article (Participants, Age Range) | Noise Source (Assessment) | Location (Environment) | Noise Indicator | Outcomes | OBR | ||||
|---|---|---|---|---|---|---|---|---|---|
| DFS | SP | SQ | WE | FA | |||||
| Tiesler et al., (2013) [64] † (n = 872, 10 yrs) |  |  | + | + | H | ||||
| Ohrstrom et al., (2006) [71] † (n = 160, 9–12 yrs) |  |  | − | + | + | + | H | ||
| Weyde et al., (2017) [72] † (n = 2665, 7 yrs) |  |  | − | H | |||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Terzakis, M.E.; Dohmen, M.; van Kamp, I.; Hornikx, M. Noise Indicators Relating to Non-Auditory Health Effects in Children—A Systematic Literature Review. Int. J. Environ. Res. Public Health 2022, 19, 15633. https://doi.org/10.3390/ijerph192315633
Terzakis ME, Dohmen M, van Kamp I, Hornikx M. Noise Indicators Relating to Non-Auditory Health Effects in Children—A Systematic Literature Review. International Journal of Environmental Research and Public Health. 2022; 19(23):15633. https://doi.org/10.3390/ijerph192315633
Chicago/Turabian StyleTerzakis, Michail Evangelos, Maud Dohmen, Irene van Kamp, and Maarten Hornikx. 2022. "Noise Indicators Relating to Non-Auditory Health Effects in Children—A Systematic Literature Review" International Journal of Environmental Research and Public Health 19, no. 23: 15633. https://doi.org/10.3390/ijerph192315633
APA StyleTerzakis, M. E., Dohmen, M., van Kamp, I., & Hornikx, M. (2022). Noise Indicators Relating to Non-Auditory Health Effects in Children—A Systematic Literature Review. International Journal of Environmental Research and Public Health, 19(23), 15633. https://doi.org/10.3390/ijerph192315633






