Are Crohn’s Disease Patients Limited in Sport Practise? An UltraEndurance Case–Control Study Response
Abstract
:1. Introduction
2. Case Report
3. Methods
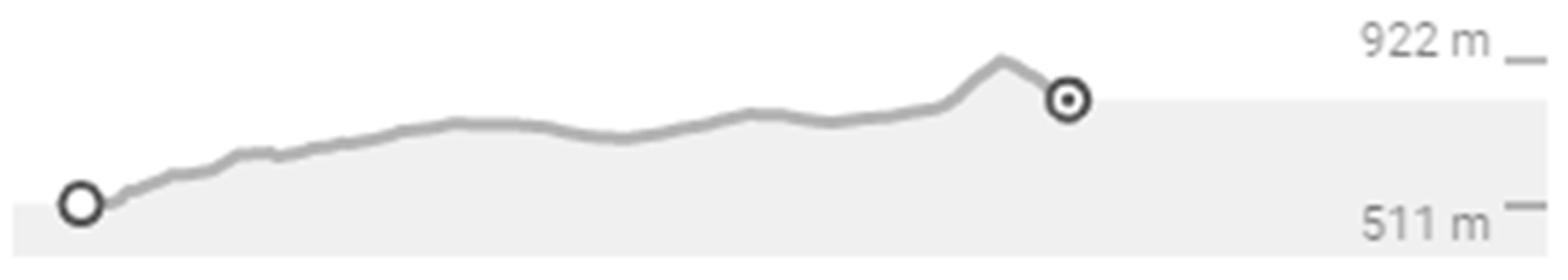
3.1. Ultra-Endurance Event
3.2. Evaluation of the Participants
- Thirty-two hours prior to the ultra-endurance event, analysing basal heart rate variability (HRV). Data were collected with the participants lying in a bed after waking up (8:00 a.m.);
- Seven hours prior to the ultra-endurance event, analysing HRV and body composition parameters. Data were collected with participant lying in a bed after waking up (8:00 a.m.);
- Ultra-endurance event: At 14:45 p.m. 1 h pre-event, HRV was collected (20 °C, 20% humidity). From 15:45 to 23:54 p.m., race HRV was collected (see Figure 2) (13 °C, 82% humidity), and from 23:54 p.m. to 00:54 a.m., post-event HRV was collected (5 °C, 85% humidity). Before, during, and after the ultra-endurance event, the following parameters were analysed: rating of perceived exertion, leg pain, blood glucose, blood oxygen saturation, heart rate, temperature, urine colourimetry, urine nitrates, protein, glucose, and pH. Hand strength, leg strength, and respiratory muscle strength were analysed before and after the event. All analyses were conducted following previous procedures and analysis systems [18].
3.3. Study Variables
- Rating of perceived exertion (RPE), Borg 6–20 scale [19];
- Perceived leg muscle pain in a self-reported 1–100 scale [17];
- Blood glucose concentration by the analysis of 5 µL of capillary finger blood using a portable analyser (One Touch Basic, LifeScan Inc., Madrid, Spain);
- Body temperature (BT) was measured by an armpit thermometer (digiT-40, Cammi Group SpA. Calvisano, Italia);
- Blood oxygen saturation and HR by a pulse oximeter (PO 30 Beurer Medical);
- Respiratory muscle strength by the forced vital capacity (FVC) using a QM-SP100 (Quirumed, Spain) spirometer in a maximum inhale–exhale cycle;
- Isometric hand strength by a grip dynamometer (Takei Kiki. Koyo, Japan);
- Leg strength manifestation was analysed by a horizontal jump test. Subjects performed a standardized warm-up comprising 2 × 10 vertical jumps with 30 s of recovery, and then, they performed two maximal horizontal jumps using the best attempt for the statistical analysis [20];
- Urine samples were collected to analyse dehydration levels by the urine colour chart (colour range 1–8; where 1 = very pale-yellow urine, reflected a good level of hydration, and 8 = very dark yellowish brown, reflected a significant level of dehydration) [21]. Urine nitrates, protein, glucose, and pH were measured with the Urine Combur-Test (Roche, Madrid, Spain) stripes [22];
- Body mass index (BMI), muscle mass, and fat mass were determined by using bioelectrical impedance analysis (InBody 720, Biospace Co., Ltd., Seoul, South Korea) [23];
- HRV measurements were recorded by a validated (Giles, Draper, and Neil, 2015) Polar V800 heart rate monitor (Polar, Kempele, Finland). The R-R series was analysed using Kubios HRV® software (version 2.1, Biosignal Analysis and Medical Imaging Group, University of Kuopio, Kuopio, Finland). The following variables were analysed: minimum, average, and maximal hear rate (HR, bpm); square root of the mean of the sum of the squared differences between adjacent normal R-R intervals (RMSSD, ms); percentage of differences between adjacent normal R-R intervals more than 50 milliseconds (PNN50, count); low (HF) and high (HF) frequency bands (LF) in normalized units (nu); LF/HF ratio; sensitivity of the short-term (SD1, ms) and long-term (SD2, ms) variability of the non-linear spectre of the HRV, and the approximate entropy of HRV (ApEn, ms).
4. Results
5. Discussion
Limitation of the Study
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Baumgart, D.C.; Sandborn, W.J. Crohn’s disease. Lancet 2020, 380, 1590–1605. [Google Scholar] [CrossRef]
- Burisch, J.; Jess, T.; Martinato, M.; Lakatos, P.L.; On Behalf of ECCO-EpiCom. The burden of inflammatory bowel disease in Europe. J. Crohn’s Colitis 2013, 7, 322–337. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Saltin, B. Evidence for prescribing exercise as therapy in chronic disease. Scand. J. Med. Sci. Sports 2006, 16, 3–63. [Google Scholar] [CrossRef] [PubMed]
- Roberts, C.K.; Barnard, R.J. Effects of exercise and diet on chronic disease. J. Appl. Physiol. 2005, 98, 3–30. [Google Scholar] [CrossRef] [PubMed]
- Pérez, C.A. Prescription of physical exercise in Crohn’s disease. J. Crowns Colitis 2009, 3, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Lykouras, D.; Karkoulias, K.; Triantos, C. Physical exercise in patients with inflammatory bowel disease. J. Crohn’s Colitis 2017, 11, 1024. [Google Scholar] [CrossRef] [PubMed]
- Reboredo, M.M.; Pinheiro, B.V.; Chebli, J.M.F. Physical exercise programs in patients with inflammatory bowel disease. J. Crohn’s Colitis 2017, 11, 1286. [Google Scholar] [CrossRef]
- D’Incà, R.; Varnier, M.; Mestriner, C.; Martines, D.; D’Odorico, A.; Sturniolo, G.C. Effect of moderate exercise on Crohn’s disease patients in remission. Ital. J. Gastroenterol. Hepatol. 1999, 31, 205–210. [Google Scholar]
- Ng, V.; Millard, W.; Lebrun, C.; Howard, J. Low-intensity exercise improves quality of life in patients with Crohn’s disease. Clin. J. Sport Med. 2007, 17, 384–388. [Google Scholar] [CrossRef]
- Robinson, R.J.; Krzywicki, T.; Almond, L.; al-Azzawi, F.; Abrams, K.; Iqbal, S.J.; Mayberry, J.F. Effect of a low-impact exercise program on bone mineral density in Crohn’s disease: A randomized controlled trial. Gastroenterology 1998, 115, 36–41. [Google Scholar] [CrossRef]
- Tew, G.A.; Leighton, D.; Carpenter, R.; Anderson, S.; Langmead, L.; Ramage, J.; Faulkner, J.; Coleman, E.; Fairhurst, C.; Seed, M.; et al. High-intensity interval training and moderate-intensity continuous training in adults with Crohn’s disease: A pilot randomised controlled trial. BMC Gastroenterol. 2019, 19, 19. [Google Scholar] [CrossRef]
- Fragala, M.S.; Kraemer, W.J.; Denegar, C.R.; Maresh, C.M.; Mastro, A.M.; Volek, J.S. Neuroendocrine-immune interactions and responses to exercise. Sports Med. 2011, 41, 621–639. [Google Scholar] [CrossRef]
- Awick, E.A.; Ehlers, D.K.; Aguiñaga, S.; Daugherty, A.M.; Kramer, A.F.; McAuley, E. Effects of a randomized exercise trial on physical activity, psychological distress and quality of life in older adults. Gen. Hosp. Psychiatry 2017, 49, 44–50. [Google Scholar] [CrossRef]
- Chan, D.; Robbins, H.; Rogers, S.; Clark, S.; Poullis, A. Inflammatory bowel disease and exercise: Results of a Crohn’s and Colitis UK survey. Frontline Gastroenterol. 2014, 5, 44–48. [Google Scholar] [CrossRef]
- Belinchón-deMiguel, P.; Clemente-Suárez, V.J. Nutrition, hydration and ergogenic aids strategies in ultraendurance mountain events. J. Sports Med. Phys. Fitness 2019, 59, 791. [Google Scholar] [CrossRef]
- Costa, R.J.S.; Snipe, R.M.J.; Kitic, C.M.; Gibson, P.R. Systematic review: Exercise-induced gastrointestinal syndrome—implications for health and intestinal disease. Aliment. Pharmacol. Ther. 2017, 46, 246–265. [Google Scholar] [CrossRef]
- Sánchez-Molina, J.; Tronero-Aguilera, J.F.; Clemente-Suárez, V.J. Psychophysiological respond in a swimming ultra-endurance event. J. Sports Med. Phys. Fit. 2020, 61, 140–145. [Google Scholar] [CrossRef]
- Santos, S.; Parraca, J.A.; Fernandes, O.; Villafaina, S.; Clemente-Suarez, V.J.; Melo, F. The Effect of Expertise during Simulated Flight Emergencies on the Autonomic Response and Operative Performance in Military Pilots. Int. J. Environ. Res. Public Health 2020, 19, 9141. [Google Scholar] [CrossRef]
- Borg, G. Perceived exertion as an indicator of somatic stress. Scand. J. Rehabil. Med. 1970, 2, 92–98. [Google Scholar]
- Clemente-Suárez, V.J.; Delgado-Moreno, R.; González, B.; Ortega, J.; Ramos-Campo, D.J. Amateur endurance triathletes’ performance is improved independently of volume or intensity based training. Physiol. Behav. 2018, S0031-9384, 30182–30183. [Google Scholar] [CrossRef]
- Armstrong, L.E.; Soto, J.A.H.; Hacker, F.T.; Casa, D.J.; Kavouras, S.; Maresh, C.M. Urinary indices during dehydration, exercise and rehydratation. Occup. Health Ind. Med. 1998, 8, 345–355. [Google Scholar]
- Hormeño-Holgado, A.J.; Clemente-Suárez, V.J. Psychophysiological monitorization in a special operation selection course. J. Med. Syst. 2019, 43, 47. [Google Scholar] [CrossRef]
- Suarez, V.; Campo, D.; Gonzalez-Rave, J. Modifications to body composition after running an alpine marathon: Brief clinical report. Int. Sport J. 2011, 12, 133–140. [Google Scholar]
- Taxonera, C.; Barreiro-de-Acosta, M.; Bastida, G.; Martinez-Gonzalez, J.; Merino, O.; García-Sánchez, V.; Gisbert, J.P.; Marín-Jiménez, I.; López-Serrano, P.; Gómez-García, M.; et al. Outcomes of medical and surgical therapy for entero-urinary fistulas in Crohn’s disease. J. Crohn’s Colitis 2016, 10, 657–662. [Google Scholar] [CrossRef]
- Scozzari, G.; Arezzo, A.; Morino, M. Enterovesical fistulas: Diagnosis and management. Tech. Coloproctol. 2010, 14, 293–300. [Google Scholar] [CrossRef]
- Chlíbková, D.; Rosemann, T.; Posch, L.; Matoušek, R.; Knechtle, B. Pre-and post-race hydration status in hyponatremic and non-hyponatremic ultra-endurance athletes. Chin. J. Physiol. 2016, 59, 173–183. [Google Scholar] [CrossRef]
- Wiroth, J.B.; Filippi, J.; Schneider, M.; Al-Jaouni, R.; Horvais, N.; Gavarry, O.; Bermon, S.; Hébuterne, X. Muscle performance in patients with Crohn’s disease in clinical remission. Inflamm. Bowel Dis. 2005, 11, 296–303. [Google Scholar] [CrossRef]
- Clemente-Suárez, V.J. Psychophysiological response and energy balance during a 14-h ultraendurance mountain running event. Appl. Physiol. Nutr. Metab. 2015, 40, 269–273. [Google Scholar] [CrossRef]
- Belinchón-deMiguel, P.; Clemente-Suárez, V.J. Psychophysiological, body composition, biomechanical and autonomic modulation analysis procedures in an ultraendurance mountain race. J. Med. Syst. 2018, 42, 32. [Google Scholar] [CrossRef]
- Sousa, C.V.; Nikolaidis, P.T.; Clemente-Suárez, V.J.; Rosemann, T.; Knechtle, B. Pacing and performance analysis of the World’s Fastest Female Ultra-Triathlete in 5x and 10x Ironman. Int. J. Environ. Res. Public Health 2020, 17, 1543. [Google Scholar] [CrossRef]
- Magro, D.O.; Cazzo, E.; Kotze, P.; Vasques, A.C.J.; Martinez, C.A.R.; Chaim, E.A.; Geloneze, B.; Pareja, J.C.; Coy, C.S.R. Glucose Metabolism Parameters and Post-Prandial GLP-1 and GLP-2 Release Largely Vary in Several Distinct Situations: A Controlled Comparison Among Individuals with Crohn’s Disease and Individuals with Obesity Before and After Bariatric Surgery. Obes. Surg. 2018, 28, 378–388. [Google Scholar] [CrossRef] [PubMed]
- Oray, M.; Abu Samra, K.; Ebrahimiadib, N.; Meese, H.; Foster, C.S. Long-term side effects of glucocorticoids. Expert Opin. Drug Saf. 2016, 15, 457–465. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Children and Adolescents: Standards of Medical Care in Diabetes—2018. Diabetes Care 2018, 41 (Suppl. S1), S126–S136. [Google Scholar]
- Phillips, S.; Green, H.J.; Tarnopolsky, M.A.; Heigenhauser, G.J.; Grant, S.M. Progressive effect of endurance training on metabolic adaptations in working skeletal muscle. Am. J. Physiol. Endoc. M 1996, 270, E265–E272. [Google Scholar] [CrossRef]
- Romanovsky, A.A. Skin temperature: Its role in thermoregulation. Acta Physiol. 2014, 210, 498–507. [Google Scholar] [CrossRef]
- Herborn, K.A.; Graves, J.L.; Jerem, P.; Evans, N.P.; Nager, R.; McCafferty, D.J.; McKeegan, D.E. Skin temperature reveals the intensity of acute stress. Physiol. Behav. 2015, 152, 225–230. [Google Scholar] [CrossRef]
- Sánchez-Molina, J.; Robles-Pérez, J.J.; Clemente-Suárez, V.J. Psychophysiological and specific fine motor skill modifications in a checkpoint action. J. Med. Syst. 2019, 43, 90. [Google Scholar] [CrossRef]
- Rüst, C.A.; Knechtle, B.; Knechtle, P.; Wirth, A.; Rosemann, T. Body mass change and ultraendurance performance: A decrease in body mass is associated with an increased running speed in male 100-km ultramarathoners. J. Strength Cond. Res. 2012, 26, 1505–1516. [Google Scholar] [CrossRef]
- Armstrong, L.E.; Casa, D.J.; Emmanuel, H.; Ganio, M.S.; Klau, J.F.; Lee, E.C.; Maresh, C.M.; McDermott, B.P.; Stearns, R.L.; Vingren, J.L.; et al. Nutritional, physiological, and perceptual responses during a summer ultraendurance cycling event. J. Strength Cond. Res. 2012, 26, 307–318. [Google Scholar] [CrossRef]
- Cheuvront, S.N.; Haymes, E.M. Thermoregulation and marathon running. Sports Med. 2001, 31, 743–762. [Google Scholar] [CrossRef]
- Prinsloo, G.E.; Rauch, H.G.; Derman, W.E. A brief review and clinical application of heart rate variability biofeedback in sports, exercise, and rehabilitation medicine. Phys. Sportsmed. 2014, 42, 88–99. [Google Scholar] [CrossRef]
- Hottenrott, K.; Hoos, O.; Esperer, H.D. Heart rate variability and physical exercise. Current status. Herz 2006, 31, 544–552. [Google Scholar] [CrossRef]
- Roldas, G.; Pedrel Carballido, C.; Capdevila, L.; Villegas García, J. Variabilidad de la frecuencia cardíaca: Concepto, medidas y relación con aspectos clínicos (I). Arch. Med. Deporte 2008, 123, 41–47. [Google Scholar]
- Aubert, A.E.; Seps, B.; Beckers, F. Heart rate variability in athletes. Sports Med. 2003, 33, 889–919. [Google Scholar] [CrossRef]
- Bustamante-Sánchez, Á.; Clemente-Suárez, V.J. Psychophysiological Response to Disorientation Training in Different Aircraft Pilots. Appl. Psychophysiol. Biofeedback 2020, 45, 241–247. [Google Scholar] [CrossRef]
- Bustamante-Sánchez, Á.; Tornero-Aguilera, J.F.; Fernández-Elías, V.E.; Hormeno-Holgado, A.J.; Dalamitros, A.A.; Clemente-Suárez, V.J. Effect of Stress on Autonomic and Cardiovascular Systems in Military Population: A Systematic Review. Cardiol. Res. Pract. 2020, 2020, 7986249. [Google Scholar] [CrossRef]
- Czaplinski, A.; Yen, A.A.; Appel, S.H. Forced vital capacity (FVC) as an indicator of survival and disease progression in an ALS clinic population. J. Neurol. Neurosurg. Psychiatry 2006, 77, 390–392. [Google Scholar] [CrossRef] [PubMed]
- Veqar, Z.; Imtiyaz, S. Vibration Therapy in Management of Delayed Onset Muscle Soreness (DOMS). J. Clin. Diagn. Res. 2014, 8, LE01–LE04. [Google Scholar] [CrossRef]
- Ward, S.; Pearce, A.J.; Pietrosimone, B.; Bennell, K.; Clark, R.; Bryant, A.L. Neuromuscular deficits after peripheral joint injury: A neurophysiological hypothesis. Muscle Nerve 2015, 51, 327–332. [Google Scholar] [CrossRef]
- Gil-Cabrera, J.; Tornero Aguilera, J.F.; Sanchez-Tena, M.A.; Alvarez-Peregrina, C.; Valbuena-Iglesias, C.; Clemente-Suárez, V.J. Aviation-associated spatial disorientation and incidence of visual illusions survey in military pilots. Int. J. Aerosp. Psychol. 2021, 31, 17–24. [Google Scholar] [CrossRef]
- Clemente-Suárez, V.J.; Robles-Pérez, J.J. Mechanical, physical, and physiological analysis of symmetrical and asymmetrical combat. J. Strength Cond. Res. 2013, 27, 2420–2426. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Molina, J.; Robles-Pérez, J.J.; Clemente-Suárez, V.J. Psychophysiological and fine motor skill differences of elite and non-elite soldiers in an urban combat simulation. Mil. Psychol. 2019, 31, 425–432. [Google Scholar] [CrossRef]
- Vicente-Rodriguez, M.; Clemente-Suárez, V.J. Psychophysiological anxiety response of a rescue helicopter crew in a crane rescue manoeuvre. BMJ Mil. Health 2020, 167, 413–417. [Google Scholar] [CrossRef] [PubMed]
- Hormeño-Holgado, A.J.; Clemente-Suárez, V.J. Effect of different combat jet manoeuvres in the psychophysiological response of professional pilots. Physiol. Behav. 2019, 208, 112559. [Google Scholar] [CrossRef]
- Clemente-Suárez, V.J.; Robles-Pérez, J.J.; Herrera-Mendoza, K.; Herrera-Tapias, B.; Fernández-Lucas, J. Psychophysiological response and fine motor skills in high-altitude parachute jumps. High Alt. Med. Biol. 2017, 18, 392–399. [Google Scholar] [CrossRef]
- Delgado-Moreno, R.; Robles-Pérez, J.J.; Clemente-Suárez, V.J. Combat stress decreases memory of warfighters in action. J. Med. Syst. 2017, 41, 124. [Google Scholar] [CrossRef]
- Delgado-Moreno, R.; Robles-Pérez, J.J.; Aznar-Laín, S.; Clemente-Suárez, V.J. Effect of experience and psychophysiological modification by combat stress in soldier’s memory. J. Med. Syst. 2019, 43, 150. [Google Scholar] [CrossRef]
- Tornero-Aguilera, J.F.; Clemente-Suárez, V.J. Effect of experience, equipment and fire actions in psychophysiological response and memory of soldiers in actual underground operations. Int. J. Psychophysiol. 2018, 128, 40–46. [Google Scholar] [CrossRef]
- Belinchón-Demiguel, P.; Tornero-Aguilera, J.F.; Dalamitros, A.; Nikolaidis, P.T.; Rosemann, T.; Knechtle, B.; Clemente-Suárez, V.J. Multidisciplinary analysis of differences between finisher and non-finisher ultra-endurance mountain athletes. Front. Physiol. 2019, 10, 1507. [Google Scholar] [CrossRef]
- Belinchón-Demiguel, P.; Ruisoto, P.; Knechtle, B.; Nikolaidis, P.T.; Herrera-Tapias, B.; Clemente-Suárez, V.J. Predictors of Athlete’s Performance in Ultra-Endurance Mountain Races. Int. J. Environ. Res. Public Health 2021, 18, 956. [Google Scholar] [CrossRef]
- Belinchón-Demiguel, P.; Ruisoto-Palomera, P.; Clemente-Suárez, V.J. Psychophysiological Stress Response of a Paralympic Athlete During an Ultra-Endurance Event. A Case Study. J. Med. Syst. 2019, 43, 70. [Google Scholar] [CrossRef] [PubMed]

| Montreal Crohn’s Disease Classification * | Age (Years) | Height (cm) | Weight (kg) | Fat Mass (kg) | Muscle Mass (kg) | Training (min/Week) | |
|---|---|---|---|---|---|---|---|
| Crohn’s disease participant | A3 L3 B1 | 41 | 178 | 77.7 | 17.7 | 33.7 | 322.4 |
| Non-Crohn’s disease participant | - | 36 | 174 | 68.8 | 13.1 | 31.6 | 350.3 |
| Time | Urine Colourimetry | Urine Nitrates | Urine pH | Urine Protein (mg/dL) | Urine Glucose (mg/dL) | ||||||
| Crohn’s Disease participant | 14:16 | 2 | 0 | 5 | 0 | 0 | |||||
| 19:45 | 1 | 0 | 5 | 1 | 1 | ||||||
| 23:56 | 2 | 0 | 5 | 1 | 1 | ||||||
| Non-Crohn’s Disease participant | 14:16 | 1 | 0 | 5 | 0 | 0 | |||||
| 19:45 | 1 | 0 | 5 | 0 | 0 | ||||||
| 23:56 | 1 | 0 | 5 | 0 | 0 | ||||||
| Time | Rating of Perceived Exertion | Leg Pain Perception | Glucose (mmol/L) | Blood Oxygen Saturation (%) | Heart Rate (bpm) | Temperature (°C) | Hand Strength (N) | Leg Strength (cm) | Forced Vital Capacity (mL) | Sit and Reach (cm) | |
| Crohn’s Disease participant | 14:16 | 7 | 15 | 8.2 | 99 | 73 | 35.6 | 45.5 | 120 | 5300 | 17 |
| 19:45 | 11 | 30 | 4.8 | 96 | 69 | 34.2 | |||||
| 23:56 | 20 | 100 | 4.6 | 96 | 72 | 34.6 | 38.1 | 73 | 3800 | 8 | |
| Non-Crohn’s Disease participant | 14:16 | 6 | 5 | 9.9 | 96 | 70 | 35.9 | 53.4 | 182 | 5200 | 22.5 |
| 19:45 | 10 | 35 | 4.7 | 97 | 63 | 36.0 | |||||
| 23:56 | 20 | 95 | 4.5 | 96 | 71 | 37.8 | 45.2 | 120 | 3850 | 11 | |
| Evaluation Moment | Mean HR (bpm) | Min HR (bpm) | Max HR (bpm) | RMSSD (ms) | LF/HF Ratio | SD1 (ms) | SD2 (ms) | |
|---|---|---|---|---|---|---|---|---|
| Crohn’s Disease participant | Pre 32 h | 60.7 | 54.1 | 78.6 | 24.3 | 9.75 | 17.26 | 54.0 |
| Pre 7 h | 57.64 | 51.4 | 70.3 | 32.7 | 9.76 | 23.1 | 69.7 | |
| Pre 1 h | 82.4 | 55.5 | 123.2 | 52.0 | 2.41 | 36.78 | 66.4 | |
| Event | 112 | 58.2 | 162.3 | 23.2 | 1.8 | 16.4 | 28.2 | |
| Post 1 h | 78 | 61.4 | 105.2 | 20.5 | 5.15 | 14.5 | 40.8 | |
| Non-Crohn’s Disease participant | Pre 32 h | 59 | 51 | 67 | 57.6 | 1.7 | 40.8 | 69.5 |
| Pre 7 h | 56 | 49.4 | 68.2 | 36.6 | 4.46 | 25.9 | 63.8 | |
| Pre 1 h | 77 | 49 | 138 | 58.7 | 3.62 | 41.6 | 91.3 | |
| Event | 113.8 | 58 | 166.1 | 13.1 | 9.9 | 9.2 | 31.2 | |
| Post 1 h | 73.5 | 50 | 106.8 | 41.3 | 17.69 | 29.3 | 96.0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tornero-Aguilera, J.F.; Sánchez-Molina, J.; Parraca, J.A.; Morais, A.; Clemente-Suárez, V.J. Are Crohn’s Disease Patients Limited in Sport Practise? An UltraEndurance Case–Control Study Response. Int. J. Environ. Res. Public Health 2022, 19, 10007. https://doi.org/10.3390/ijerph191610007
Tornero-Aguilera JF, Sánchez-Molina J, Parraca JA, Morais A, Clemente-Suárez VJ. Are Crohn’s Disease Patients Limited in Sport Practise? An UltraEndurance Case–Control Study Response. International Journal of Environmental Research and Public Health. 2022; 19(16):10007. https://doi.org/10.3390/ijerph191610007
Chicago/Turabian StyleTornero-Aguilera, José Francisco, Joaquín Sánchez-Molina, Jose A. Parraca, Ana Morais, and Vicente Javier Clemente-Suárez. 2022. "Are Crohn’s Disease Patients Limited in Sport Practise? An UltraEndurance Case–Control Study Response" International Journal of Environmental Research and Public Health 19, no. 16: 10007. https://doi.org/10.3390/ijerph191610007
APA StyleTornero-Aguilera, J. F., Sánchez-Molina, J., Parraca, J. A., Morais, A., & Clemente-Suárez, V. J. (2022). Are Crohn’s Disease Patients Limited in Sport Practise? An UltraEndurance Case–Control Study Response. International Journal of Environmental Research and Public Health, 19(16), 10007. https://doi.org/10.3390/ijerph191610007









