Assessing the Expression of Emotions in Breast Cancer Survivors during the Time of Recovery: Perspective from Focus Groups
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants and Data Collection
- 1.
- Could you differentiate the emotional phases you have gone through during your illness?
- 2.
- Please, identify those people who were part of your more immediate social environment during your illness and the role played by them. Who has been your major support?
- 3.
- What decisions have you made about your illness? Could you describe those strategies you have used to cope with it?
- 4.
- You have to give advice to women who start experiencing breast cancer, what would you tell them?
2.3. Data Analysis
2.4. Ethical Considerations
3. Results
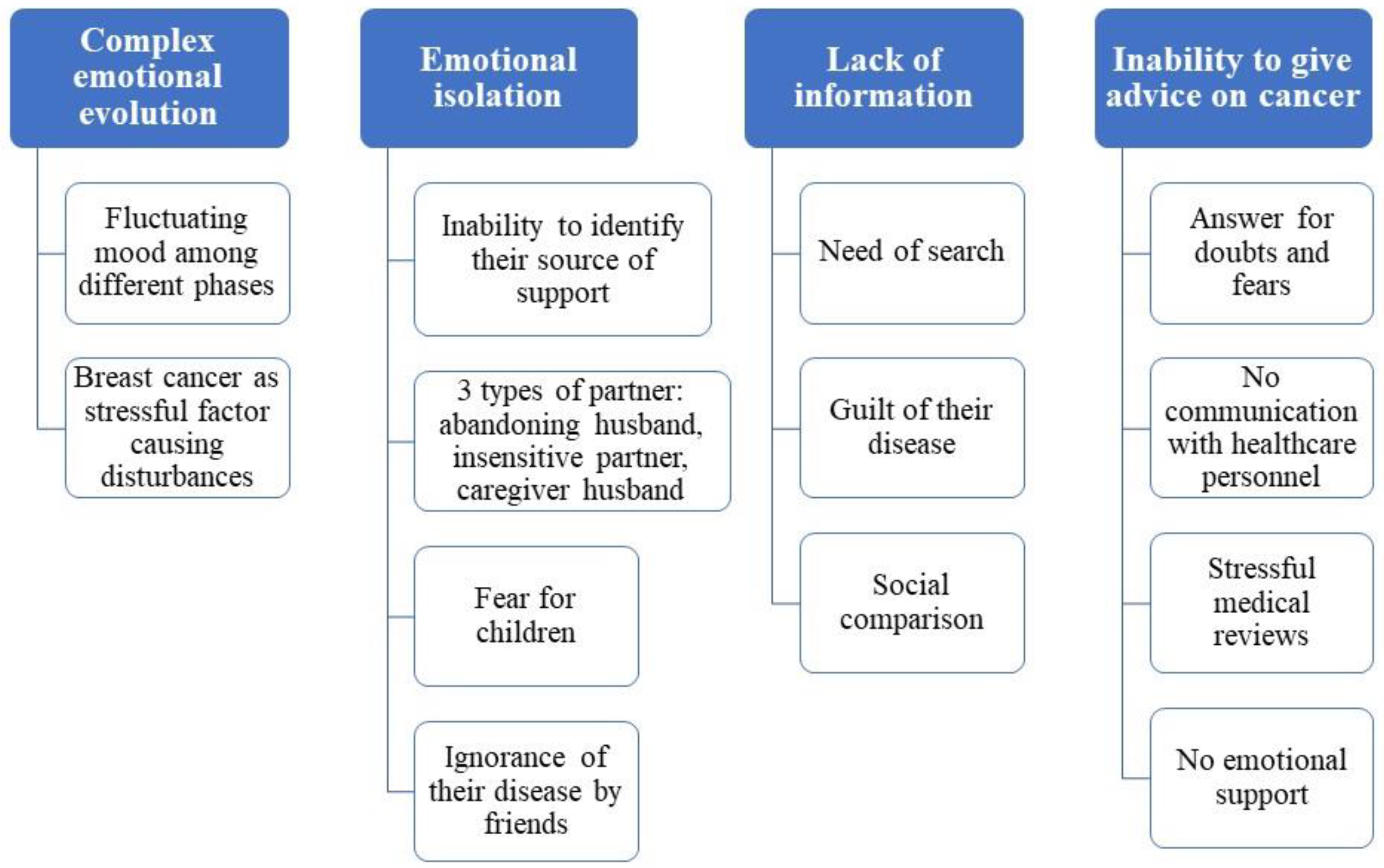
3.1. Major Findings
3.1.1. Theme 1: Complex Emotional Evolution in Breast Cancer Survivors
“What will my children think?”
“What a situation for my husband!”
“My mother is so old”.
“It’s not fair that this should happen to me”.
“Healthcare personnel do not treat me as I deserve”
“Health professionals do not understand me”.
“I don’t need anything from anyone”.
“I’m an adult and self-sufficient person”.
“Everything I’ve done so far is useless”
“My life is meaningless”.
“This is beyond my control”
“It is something that does not depend on me”.
3.1.2. Theme 2: Emotional Isolation
“There were many people who disappeared after knowing my diagnosis”.
“If things were not going well until that moment, everything was destroyed with the disease”.
“I can’t complain at home, because my husband behaves as if nothing happens. Then, I am trying to be the same person as always”.
“He makes me even more nervous with that overprotection that it is not good for me”.
“I only ask that this disease allows me to be with them until they are self-sufficient”.
“I wish that this disease finishes with me”.
“There are people who don’t want to help, they just want to know”.
3.1.3. Theme 3: Lack of Information
“I needed to know the enemy to face it”.
“I have gotten into this, I have to go out”.
3.1.4. Theme 4: Inability to Give Advice on Breast Cancer to Other Women
“I have not yet discovered what to do with my life”.
“Who am I to advise?”.
“Am I going to die?”
“How do I explain to my relatives what happens to me?”
“Why me? What does it depend on?”
“Will health professional help me enough? Are they telling me the truth?”
“What is the medical treatment? Will I keep my breast?”
“What are the sexual repercussions? Will my husband help me?”
“Will my family withstand this situation?”.
“The Sword of Damocles was hanging over my head”.
4. Discussion
- Providing care to patients from a more humanistic point of view, also including their relatives.
- Ensuring that they have a high quality of life, in spite of breast cancer.
- Reducing the impact of hospital dynamics on people that are not used to health services.
- Providing information to patients and families about their emotional state.
- Explaining them the best ways to share and show feelings within the family sphere.
- Teaching the patient how to detect negative feelings and handle them through emotional self-control techniques.
- Patient perception about themselves, their disease and mood.
- Coping resources, such as health resources, social and problem-solving skills, social support, economic and personal resources, and their relationship with healthcare personnel.
- Patient’s ability to overcome breast cancer.
- Physical and emotional signs of stress.
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef] [PubMed]
- Galceran, J.; Ameijide, A.; Carulla, M.; Mateos, A.; Quirós, J.R.; Rojas, D.; Alemán, A.; Torrella, A.; Chico, M.; Vicente, M.; et al. Cancer incidence in Spain, 2015. Clin. Transl. Oncol. 2017, 19, 799–825. [Google Scholar] [CrossRef] [PubMed]
- Saeedi-Saedi, H.; Shahidsales, S.; Koochak-Pour, M.; Sabahi, E.; Moridi, I. Evaluation of emotional distress in breast cancer patients. Iran. J. Cancer Prev. 2015, 8, 36–41. [Google Scholar]
- Montazeri, A. Health-related quality of life in breast cancer patients: A bibliographic review of the literature from 1974 to 2007. J. Exp. Clin. Cancer Res. 2008, 27, 32. [Google Scholar] [CrossRef] [PubMed]
- Moorey, S.; Cort, E.; Kapari, M.; Monroe, B.; Hansford, P.; Mannix, K.; Henderson, M.; Fisher, L.; Hotopf, M. A cluster randomized controlled trial of cognitive behaviour therapy for common mental disorders in patients with advanced cancer. Psychol. Med. 2009, 39, 713–723. [Google Scholar] [CrossRef]
- Jassim, G.A.; Whitford, D.L.; Grey, I.M. Psychological interventions for women with non-metastatic breast cancer. In Cochrane Database of Systematic Reviews; Jassim, G.A., Ed.; John Wiley & Sons, Ltd.: Chichester, UK, 2010. [Google Scholar]
- Scheier, M.F.; Helgeson, V.S.; Schulz, R.; Colvin, S.; Berga, S.L.; Knapp, J.; Gerszten, K. Moderators of interventions designed to enhance physical and psychological functioning among younger women with early-stage breast cancer. J. Clin. Oncol. 2007, 25, 5710–5714. [Google Scholar] [CrossRef]
- Aarts, J.W.F.; Deckx, L.; van Abbema, D.L.; Tjan-Heijnen, V.C.G.; van den Akker, M.; Buntinx, F. The relation between depression, coping and health locus of control: Differences between older and younger patients, with and without cancer. Psychooncology 2015, 24, 950–957. [Google Scholar] [CrossRef]
- Groarke, A.; Curtis, R.; Kerin, M. Cognitive-behavioural stress management enhances adjustment in women with breast cancer. Br. J. Health Psychol. 2013, 18, 623–641. [Google Scholar] [CrossRef]
- Gudenkauf, L.M.; Antoni, M.H.; Stagl, J.M.; Lechner, S.C.; Jutagir, D.R.; Bouchard, L.C.; Blomberg, B.B.; Glück, S.; Derhagopian, R.P.; Giron, G.L.; et al. Brief cognitive–behavioral and relaxation training interventions for breast cancer: A randomized controlled trial. J. Consult. Clin. Psychol. 2015, 83, 677–688. [Google Scholar] [CrossRef]
- Maass, S.W.M.C.; Roorda, C.; Berendsen, A.J.; Verhaak, P.F.M.; de Bock, G.H. The prevalence of long-term symptoms of depression and anxiety after breast cancer treatment: A systematic review. Maturitas 2015, 82, 100–108. [Google Scholar] [CrossRef]
- Stagl, J.M.; Bouchard, L.C.; Lechner, S.C.; Blomberg, B.B.; Gudenkauf, L.M.; Jutagir, D.R.; Glück, S.; Derhagopian, R.P.; Carver, C.S.; Antoni, M.H. Long-term psychological benefits of cognitive-behavioral stress management for women with breast cancer: 11-year follow-up of a randomized controlled trial. Cancer 2015, 121, 1873–1881. [Google Scholar] [CrossRef] [PubMed]
- Amiel, C.R.; Fisher, H.M.; Carver, C.S.; Antoni, M.H. The importance of stress management among postresection breast cancer patients. Futur. Oncol. 2016, 12, 2771–2774. [Google Scholar] [CrossRef]
- Maass, S.W.M.C.; Brandenbarg, D.; Boerman, L.M.; Verhaak, P.F.M.; de Bock, G.H.; Berendsen, A.J. Fatigue among long-term breast cancer survivors: A controlled cross-sectional study. Cancers 2021, 13, 1301. [Google Scholar] [CrossRef]
- White-Means, S.; Dapremont, J.; Davis, B.D.; Thompson, T. Who can help us on this journey? African American woman with breast cancer: Living in a city with extreme health disparities. Int. J. Environ. Res. Public Health 2020, 17, 1126. [Google Scholar] [CrossRef] [PubMed]
- Aguiar-Fernández, F.; Rodríguez-Castro, Y.; Botija, M.; Martínez-Román, R. Experiences of female breast cancer survivors concerning their return to work in Spain. Behav. Sci. 2021, 11, 135. [Google Scholar] [CrossRef] [PubMed]
- Foley, G.; Timonen, V. Using grounded theory method to capture and analyze health care experiences. Health Serv. Res. 2015, 50, 1195–1210. [Google Scholar] [CrossRef]
- Critical Appraisal Skills Programme (CASP). Critical Appraisal Skills Programme CASP Qualitative Studies Checklist. CASP Online 2018, 1. Available online: http://www.casp-uk.net/casp-tools-checklists (accessed on 15 February 2022).
- Arrighi, E.; Jovell, A.J.; Navarro, M.D.; Font, A. Desarrollo del cuestionario español para medir necesidades no cubiertas de supervivientes de cáncer (CESC) [Development of Spanish questionnaire to measure Cancer Survivors’ Unmet Needs (CaSUN)]. Psicooncología 2014, 11, 117–128. [Google Scholar] [CrossRef]
- Boyes, A.; Girgis, A.; Lecathelinais, C. Brief assessment of adult cancer patients’ perceived needs: Development and validation of the 34-item supportive care needs survey (SCNS-SF34). J. Eval. Clin. Pract. 2009, 15, 602–606. [Google Scholar] [CrossRef]
- Jacobsen, P.B. Clinical practice guidelines for the psychosocial care of cancer survivors: Current status and future prospects. Cancer 2009, 115, 4419–4429. [Google Scholar] [CrossRef]
- Aaronson, N.K.; Ahmedzai, S.; Bergman, B.; Bullinger, M.; Cull, A.; Duez, N.J.; Filiberti, A.; Flechtner, H.; Fleishman, S.B.; de Haes, J.C. The European Organization for Research and Treatment of Cancer QLQ-C30: A quality-of-life instrument for use in international clinical trials in oncology. J. Natl. Cancer Inst. 1993, 85, 365–376. [Google Scholar] [CrossRef]
- Carver, C.; Scheier, M.; Weintraub, J. Assessing coping strategies: A theoretically based approach. J. Pers. Soc. Psychol. 1989, 56, 267–283. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, D.P.; Hillier, V.F. A scaled version of the General Health Questionnaire. Psychol. Med. 1979, 9, 139–145. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Salgado, C. Sampling in qualitative research: Basic principles and some controversies. Cien. Saude Colet. 2012, 17, 613–619. [Google Scholar] [CrossRef] [PubMed]
- Patton, M.Q. Qualitative Research & Evaluation Methods; Sage Publisher: Thousand Oaks, CA, USA, 2002; ISBN 0761919716. [Google Scholar]
- Victorson, D.; Garcia, S.F.; Sanford, S.; Snyder, M.A.; Lampert, S.; Salsman, J.M. A qualitative focus group study to illuminate the lived emotional and social impacts of cancer and its treatment on young adults. J. Adolesc. Young Adult Oncol. 2019, 8, 649–659. [Google Scholar] [CrossRef]
- Brandão, T.; Tavares, R.; Schulz, M.S.; Matos, P.M. Measuring emotion regulation and emotional expression in breast cancer patients: A systematic review. Clin. Psychol. Rev. 2016, 43, 114–127. [Google Scholar] [CrossRef]
- Morgan, D.L.; Bottorff, J.L. Advancing our craft: Focus group methods and practice. Qual. Health Res. 2010, 20, 579–581. [Google Scholar] [CrossRef] [PubMed]
- Hellerstedt-Börjesson, S.; Nordin, K.; Fjällskog, M.-L.; Holmström, I.K.; Arving, C. Women treated for breast cancer experiences of chemotherapy-induced pain. Cancer Nurs. 2016, 39, 464–472. [Google Scholar] [CrossRef][Green Version]
- Miyashita, M.; Ohno, S.; Kataoka, A.; Tokunaga, E.; Masuda, N.; Shien, T.; Kawabata, K.; Takahashi, M. Unmet information needs and quality of life in young breast cancer survivors in Japan. Cancer Nurs. 2015, 38, E1–E11. [Google Scholar] [CrossRef]
- Castillo, A.; Mendiola, J.; Tiemensma, J. Emotions and coping strategies during breast cancer in latina women: A focus group study. Hisp. Health Care Int. 2019, 17, 96–102. [Google Scholar] [CrossRef]
- Zainal, N.Z.; Nik-Jaafar, N.R.; Baharudin, A.; Sabki, Z.A.; Ng, C.G. Prevalence of depression in breast cancer survivors: A systematic review of observational studies. Asian Pacific J. Cancer Prev. 2013, 14, 2649–2656. [Google Scholar] [CrossRef]
- Eng, J.A.; Clough-Gorr, K.; Cabral, H.J.; Silliman, R.A. Predicting 5- and 10-year survival in older women with early-stage breast cancer: Self-rated health and walking ability. J. Am. Geriatr. Soc. 2015, 63, 757–762. [Google Scholar] [CrossRef] [PubMed]
- Karakoyun-Celik, O.; Gorken, I.; Sahin, S.; Orcin, E.; Alanyali, H.; Kinay, M. Depression and anxiety levels in woman under follow-up for breast cancer: Relationship to coping with cancer and quality of life. Med. Oncol. 2010, 27, 108–113. [Google Scholar] [CrossRef] [PubMed]
- Grégoire, C.; Bragard, I.; Jerusalem, G.; Etienne, A.-M.; Coucke, P.; Dupuis, G.; Lanctôt, D.; Faymonville, M.-E. Group interventions to reduce emotional distress and fatigue in breast cancer patients: A 9-month follow-up pragmatic trial. Br. J. Cancer 2017, 117, 1442–1449. [Google Scholar] [CrossRef] [PubMed]
- Font, A.; Rodríguez, E. Eficacia de la terapia de grupo en cáncer de mama: Variaciones de la calidad de vida [Efficacy of group therapy in breast cancer: Variations in qualiry of life]. Psicooncologia 2004, 1, 67–86. [Google Scholar]
- Rajandram, R.K.; Ho, S.M.; Samman, N.; Chan, N.; McGrath, C.; Zwahlen, R.A. Interaction of hope and optimism with anxiety and depression in a specific group of cancer survivors: A preliminary study. BMC Res. Notes 2011, 4, 519. [Google Scholar] [CrossRef]
- Sanchez, L.; Fernandez, N.; Calle, A.P.; Ladera, V.; Casado, I.; Sahagun, A.M. Long-term treatment for emotional distress in women with breast cancer. Eur. J. Oncol. Nurs. 2019, 42, 126–133. [Google Scholar] [CrossRef]
- Pitman, A.; Suleman, S.; Hyde, N.; Hodgkiss, A. Depression and anxiety in patients with cancer. Br. Med. J. 2018, 361, k1415. [Google Scholar] [CrossRef]
- Li, L.; Yang, Y.; He, J.; Yi, J.; Wang, Y.; Zhang, J.; Zhu, X. Emotional suppression and depressive symptoms in women newly diagnosed with early breast cancer. BMC Womens Health 2015, 15, 91. [Google Scholar] [CrossRef]
- Holst-Hansson, A.; Idvall, E.; Bolmsjö, I.; Wennick, A. Hoping to reach a safe haven—Swedish families’ lived experience when a family member is diagnosed with breast cancer. Eur. J. Oncol. Nurs. 2017, 31, 52–58. [Google Scholar] [CrossRef]
- Janz, N.K.; Friese, C.R.; Li, Y.; Graff, J.J.; Hamilton, A.S.; Hawley, S.T. Emotional well-being years post-treatment for breast cancer: Prospective, multi-ethnic, and population-based analysis. J. Cancer Surviv. 2014, 8, 131–142. [Google Scholar] [CrossRef]
- Levkovich, I.; Cohen, M.; Alon, S.; Kuchuk, I.; Nissenbaum, B.; Evron, E.; Pollack, S.; Fried, G. Symptom cluster of emotional distress, fatigue and cognitive difficulties among young and older breast cancer survivors: The mediating role of subjective stress. J. Geriatr. Oncol. 2018, 9, 469–475. [Google Scholar] [CrossRef] [PubMed]
- Spiegel, D. Mind matters in cancer survival. Psychooncology 2012, 21, 588–593. [Google Scholar] [CrossRef] [PubMed]
- Jones, L.; Leach, L.; Chambers, S.; Occhipinti, S. Scope of practice of the breast care nurse: A comparison of health professional perspectives. Eur. J. Oncol. Nurs. 2010, 14, 322–327. [Google Scholar] [CrossRef] [PubMed]
| Number (%) of Patients | |
|---|---|
| Age (years) | |
| 30–39 | 1 (1.2%) |
| 40–49 | 31 (37.3%) |
| 50–59 | 33 (39.8%) |
| 60–69 | 16 (19.3%) |
| 70–79 | 2 (2.4%) |
| Marital status | |
| Married/with partner | 47 (56.6%) |
| Widowed | 4 (4.8%) |
| Single | 11 (13.3%) |
| Separated/divorced | 14 (16.9%) |
| No answer/do not know | 7 (8.4%) |
| Children | |
| Yes | 67 (80.7%) |
| No | 16 (19.3%) |
| Education | |
| Elementary school | 22 (26.5%) |
| Secondary school or similar | 31 (37.3%) |
| Higher education | 28 (33.7%) |
| No answer/do not know | 2 (2.4%) |
| Employment situation | |
| Employed | 39 (47.0%) |
| Unemployed | 9 (10.8%) |
| Housewife | 12 (14.5%) |
| Retired | 13 (15.7%) |
| Temporary incapacity for work | 5 (6.0%) |
| No answer/do not know | 5 (6.0%) |
| Number (%) of Patients | |
|---|---|
| Disease stage | |
| I | 5 (6.0%) |
| II | 69 (83.1%) |
| III | 6 (7.2%) |
| Cured | 1 (1.2%) |
| No answer/do not know | 2 (2.4%) |
| Prognosis (defined by patients) | |
| Good | 25 (30.1%) |
| Bad | 29 (34.9%) |
| Not defined | 27 (32.5%) |
| No answer/do not know | 2 (2.4%) |
| Treatment | |
| Chemotherapy | 79 (95.2%) |
| Radiotherapy | 62 (74.7%) |
| Endocrine therapy | 30 (36.1%) |
| Surgery | 79 (95.2%) |
| Type of surgery | |
| Tumorectomy | 5 (6.0%) |
| Simple mastectomy | 40 (48.2%) |
| Radical mastectomy | 36 (43.4%) |
| Current situation of disease | |
| Without recurrence | 43 (51.8%) |
| Follow-up after recurrence | 28 (33.7%) |
| Active disease | 8 (9.6%) |
| No answer/do not know | 4 (4.8%) |
| Interval between reviews | |
| Three months | 15 (18.1%) |
| Six months | 24 (28.9%) |
| One year | 22 (26.5%) |
| More than one year | 16 (19.3%) |
| No answer/do not know | 6 (7.2%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sanchez, L.; Fernandez, N.; Calle, A.P.; Ladera, V.; Casado, I.; Bayon, E.; Garcia, I.; Sahagun, A.M. Assessing the Expression of Emotions in Breast Cancer Survivors during the Time of Recovery: Perspective from Focus Groups. Int. J. Environ. Res. Public Health 2022, 19, 9672. https://doi.org/10.3390/ijerph19159672
Sanchez L, Fernandez N, Calle AP, Ladera V, Casado I, Bayon E, Garcia I, Sahagun AM. Assessing the Expression of Emotions in Breast Cancer Survivors during the Time of Recovery: Perspective from Focus Groups. International Journal of Environmental Research and Public Health. 2022; 19(15):9672. https://doi.org/10.3390/ijerph19159672
Chicago/Turabian StyleSanchez, Leticia, Nelida Fernandez, Angela P. Calle, Valentina Ladera, Ines Casado, Enrique Bayon, Isaias Garcia, and Ana M. Sahagun. 2022. "Assessing the Expression of Emotions in Breast Cancer Survivors during the Time of Recovery: Perspective from Focus Groups" International Journal of Environmental Research and Public Health 19, no. 15: 9672. https://doi.org/10.3390/ijerph19159672
APA StyleSanchez, L., Fernandez, N., Calle, A. P., Ladera, V., Casado, I., Bayon, E., Garcia, I., & Sahagun, A. M. (2022). Assessing the Expression of Emotions in Breast Cancer Survivors during the Time of Recovery: Perspective from Focus Groups. International Journal of Environmental Research and Public Health, 19(15), 9672. https://doi.org/10.3390/ijerph19159672









