Long-Term Kinetics of Serological Antibodies against Vibrio cholerae Following a Clinical Cholera Case: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Methods
2.1. Data Sources and Searches
2.2. Study Selection
2.3. Data Extraction and Quality Assessment
2.4. Data Synthesis and Analysis
3. Results
3.1. Search Results
3.2. Study Characteristics
3.3. Antibody Kinetics
3.4. Meta-Analysis Results by Antibody Types
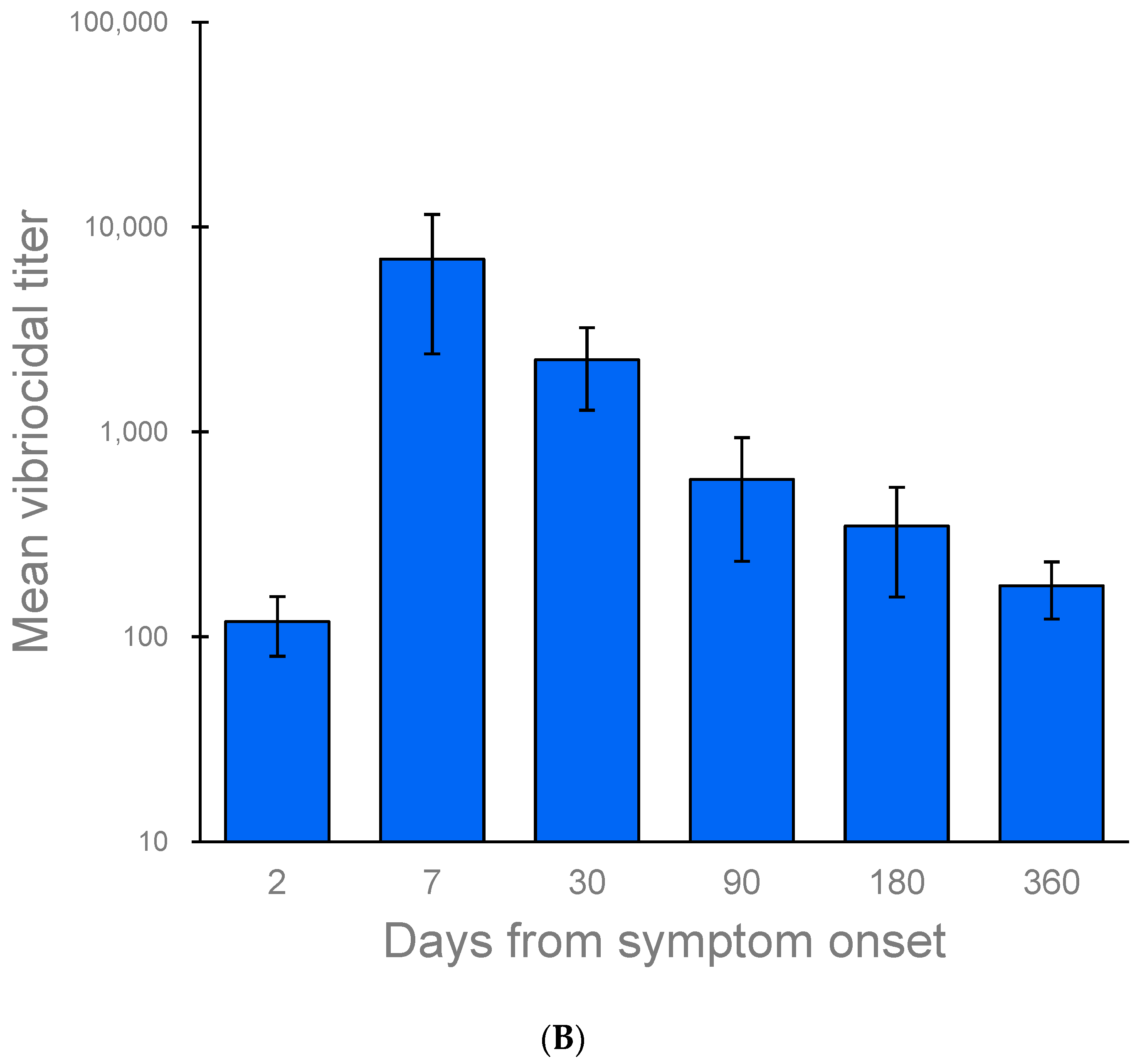
3.4.1. Vibriocidal Antibody Titers
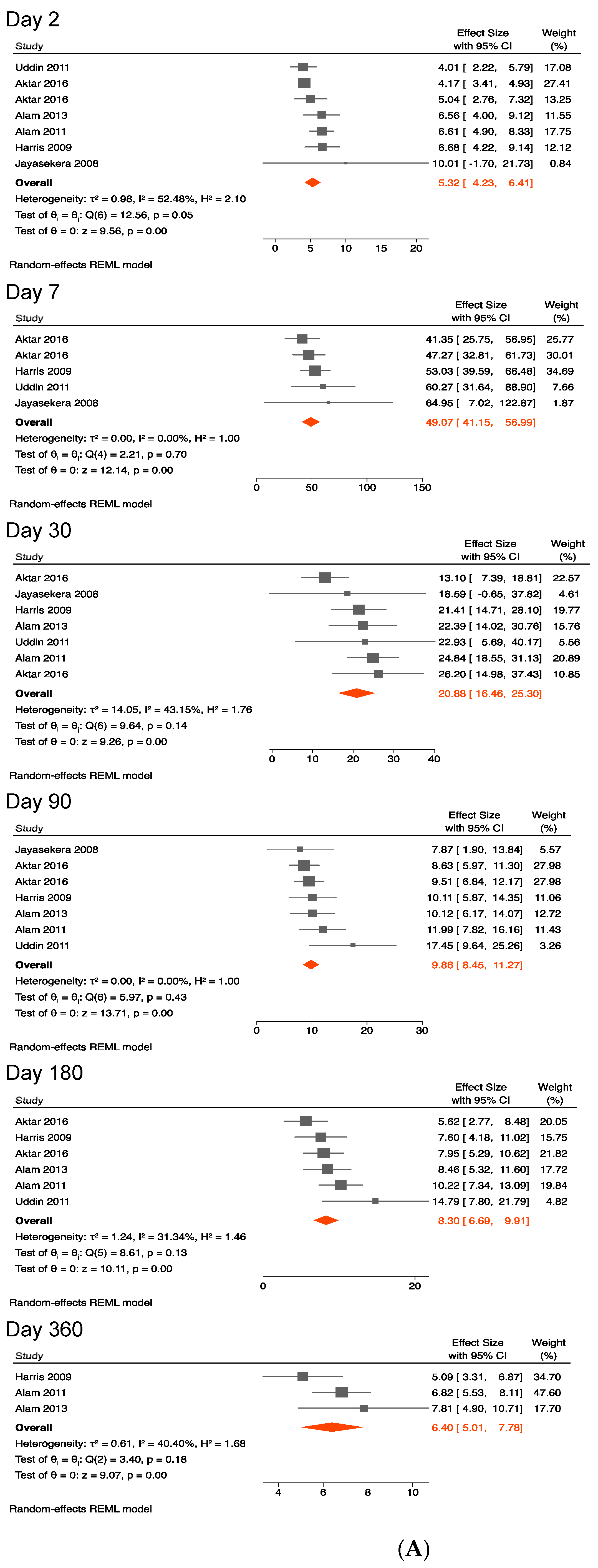
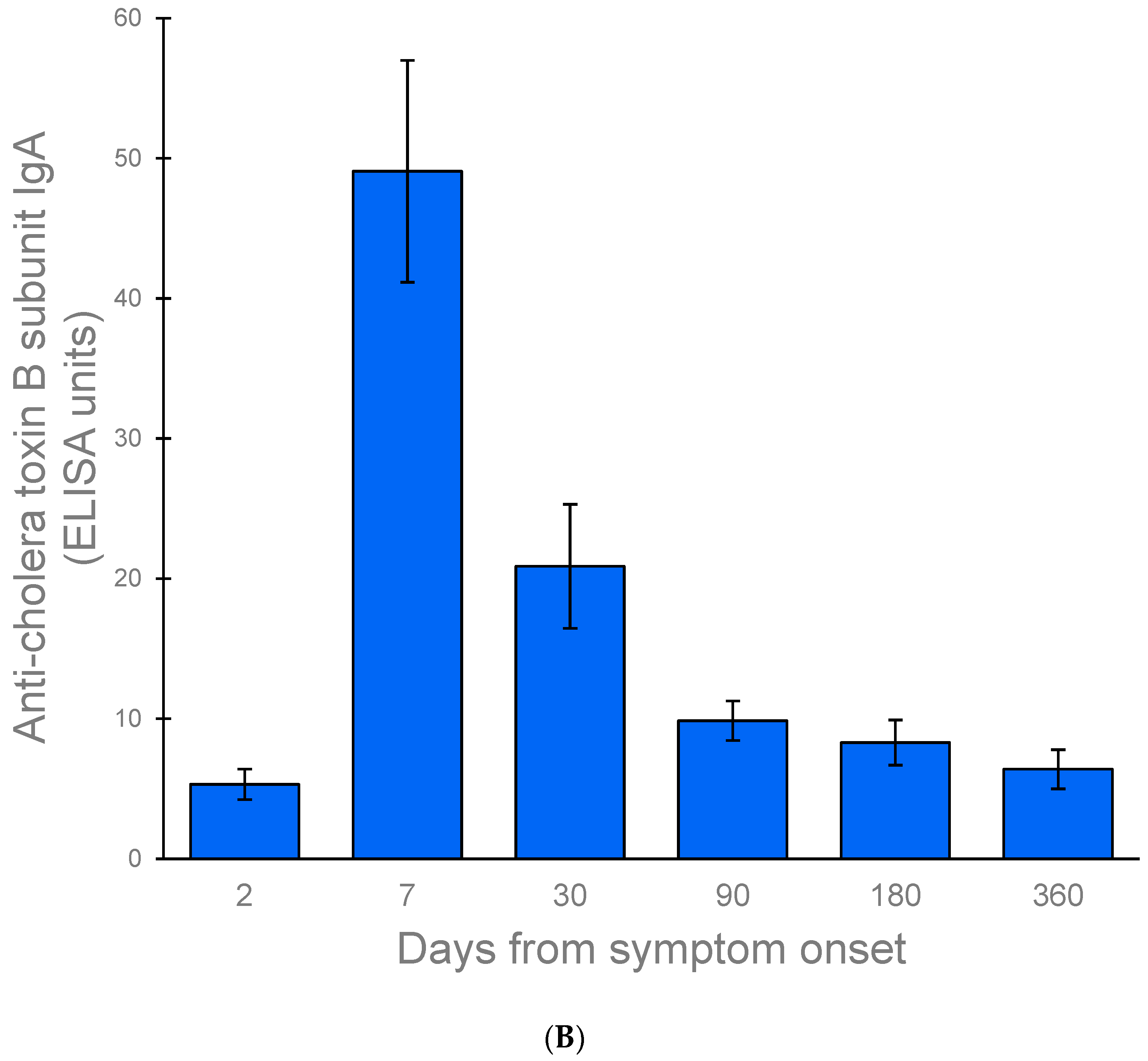
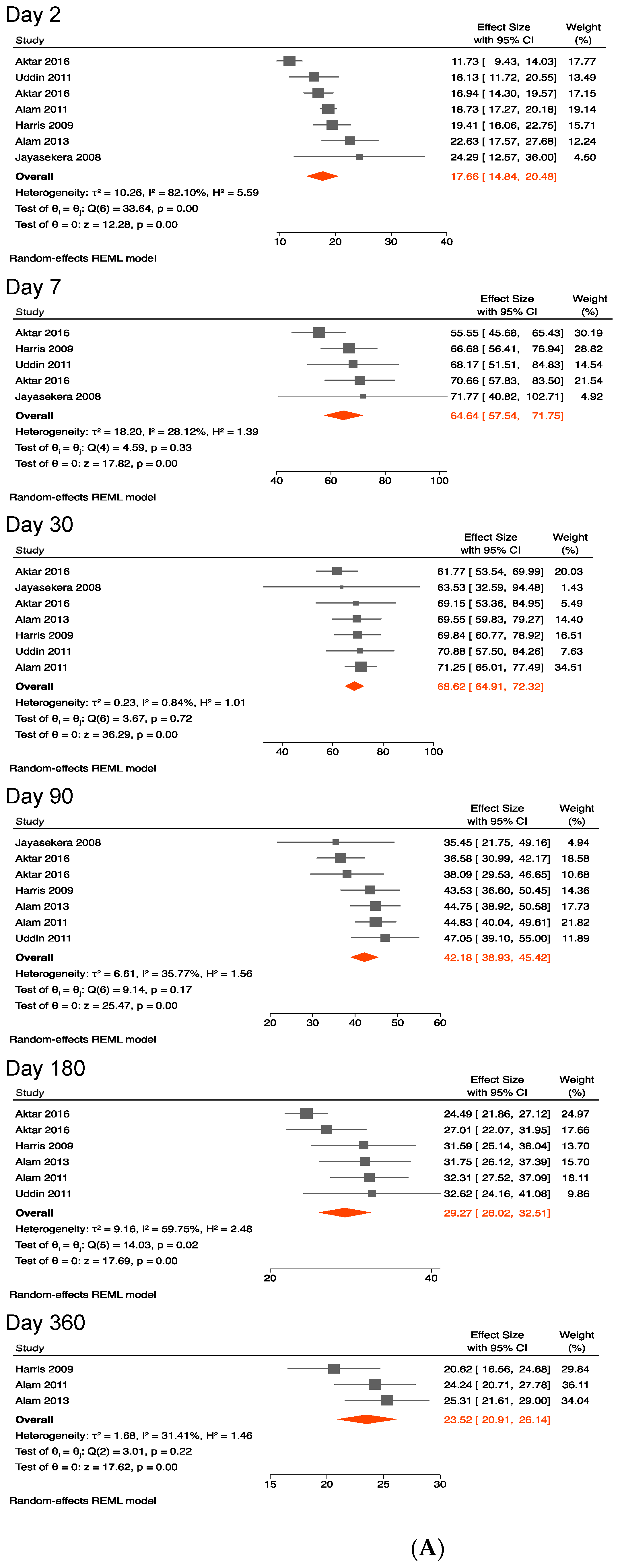
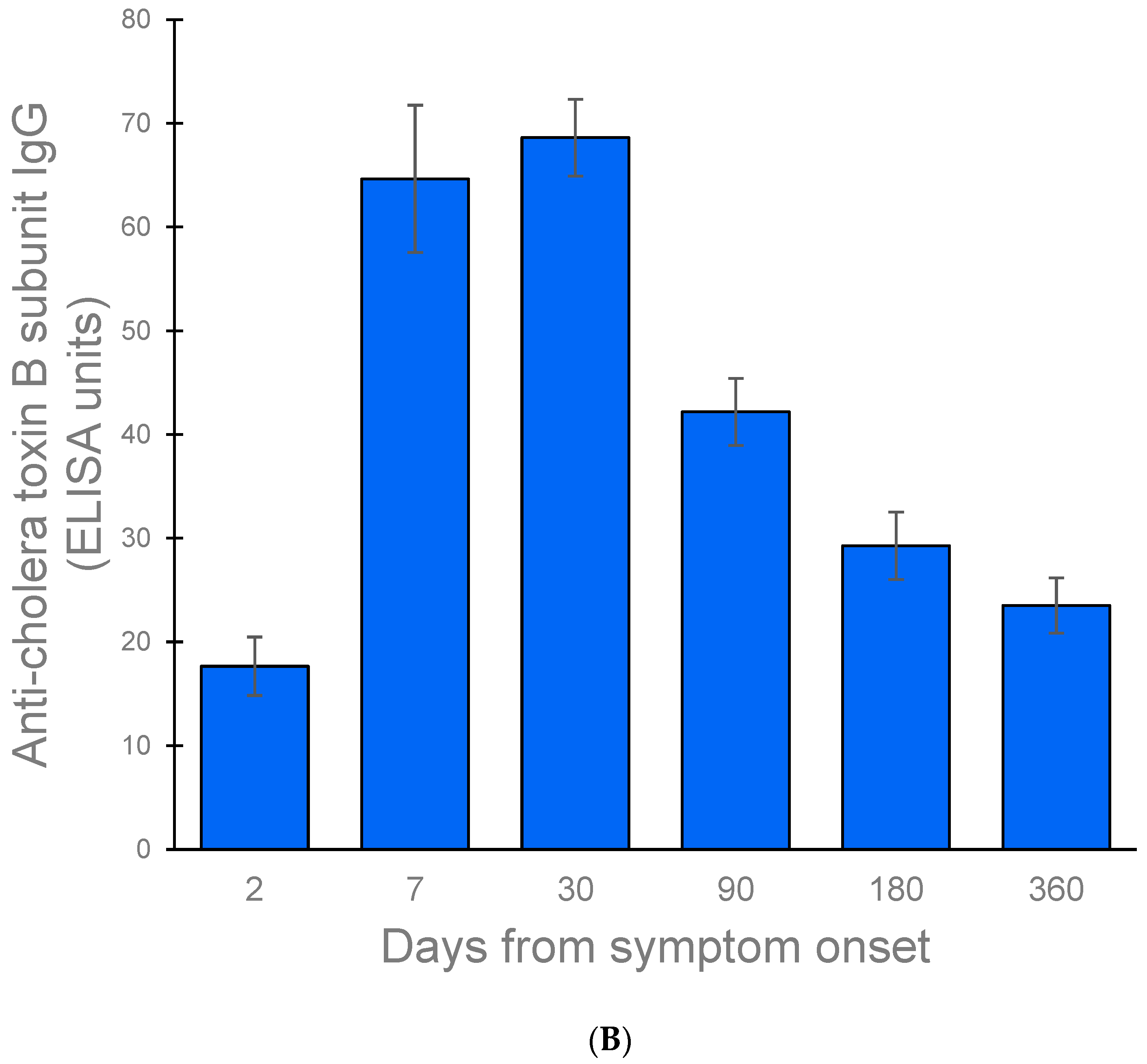
3.4.2. Antibody Responses against the B Subunit of the Cholera Toxin
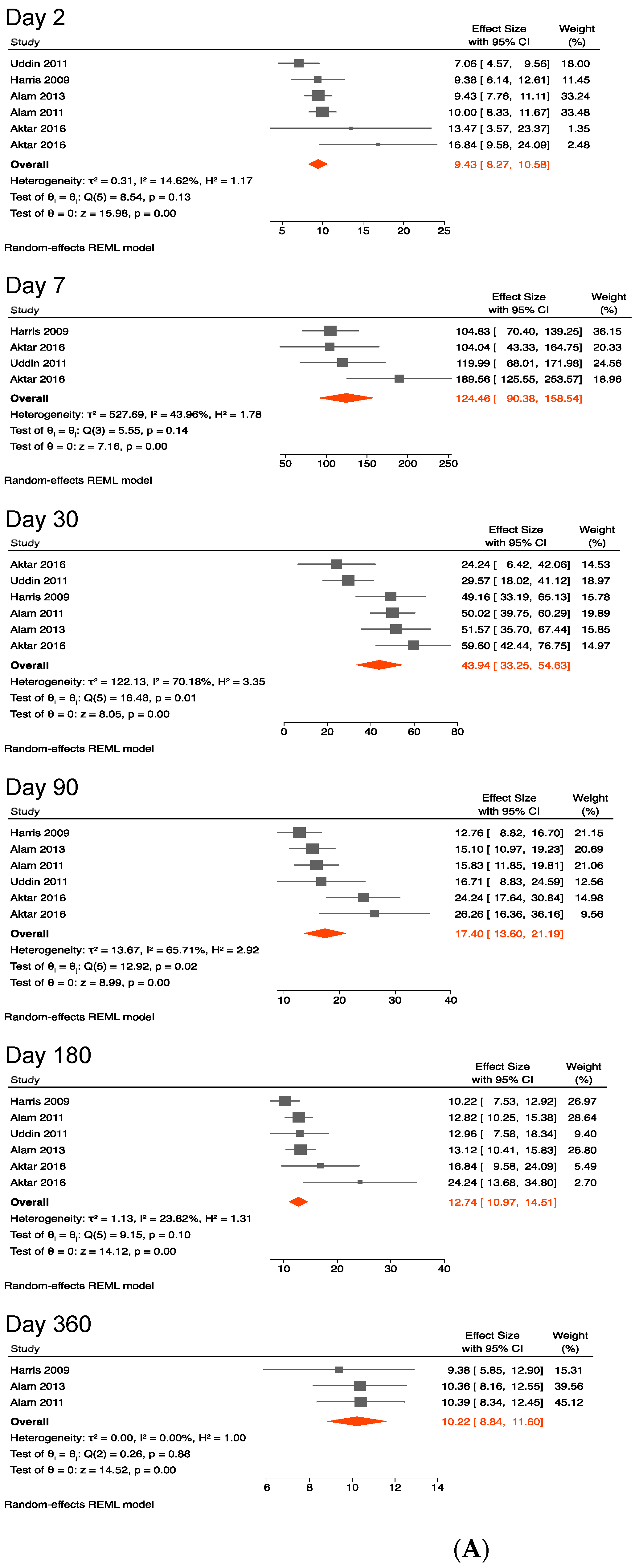
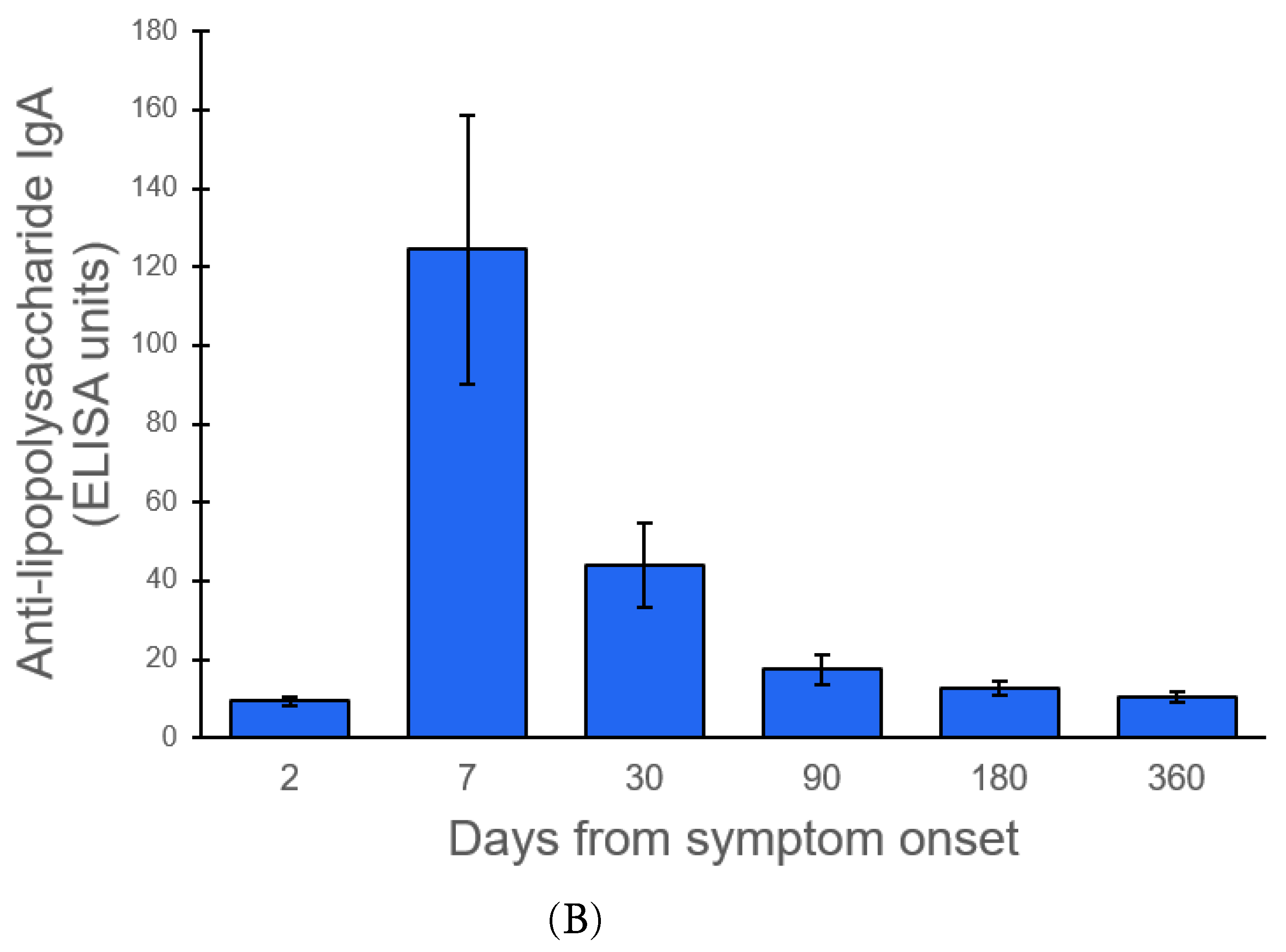
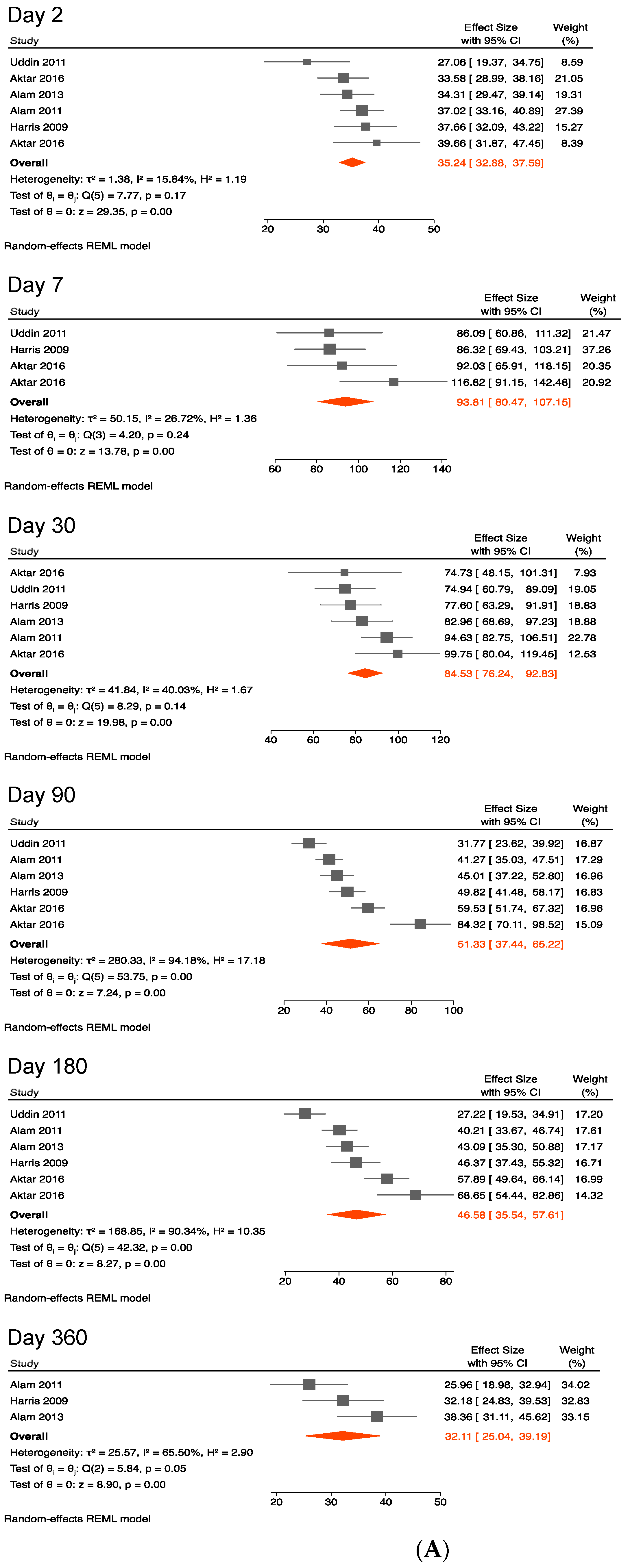
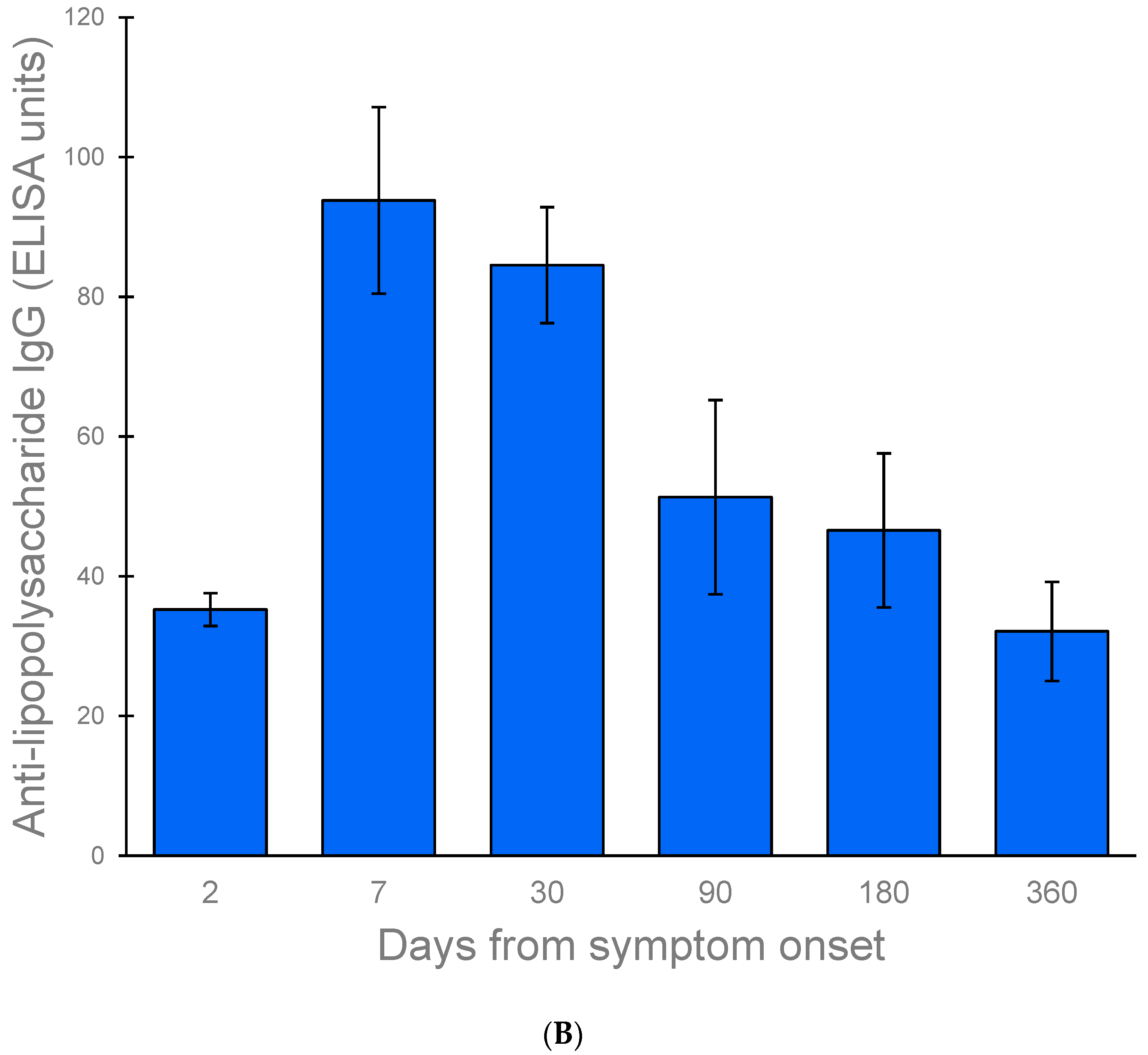
3.4.3. Antibody against Lipopolysaccharides of V. cholerae O1
4. Discussion
4.1. Vibriocidal Antibodies
4.2. Antibody Responses against the B Subunit of Cholera Toxins
4.3. Antibody against V. cholerae O1 Lipopolysaccharides
4.4. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| First Author, Year | Time Frame/Enrollment Dates | Country | Study Design | Sample Size and Participants | Immune Markers of Interest | Antibody Isotypes | Type of Blood Sample | Vibrio cholerae O1 Serotype | Measurement Methods | Multiple Time Points for Blood Collection | Follow-Up Duration (Days) |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Azman, 2019 [35] | 2006 to 2015 (Bangladesh); and September 2013 to September 2014 (USA) | Bangladesh and USA | Prospective cohort | 38 North American volunteers (median age = 31; human challenge study) and 320 patients from Bangladesh (median age = 25) | Vibriocidal antibodies, and anti-CTB antibodies | IgA, IgG and IgM | Serum and plasma | Ogawa (n = 285); Inaba (n = 33) | ELISA | Day 0; 10; 28; 90; and 170 for volunteers; and day 2; 7; 30; 90; 180, 270, 365, 540, 720, and 900 for patients | 915 |
| Hossain, 2019 [36] | September 2013 to September 2014 (USA) | USA and Bangladesh | Prospective cohort | 38 North America volunteers (median age = 31; human challenge study) and 38 patients from Bangladesh (median age = 30) | OSP-specific antibodies | IgA, IgG and IgM | Serum and plasma | Inaba (n = 80) for patients | ELISA | Day 0; 10; 28; 90; and 170 for volunteers; and day 2; 7; 21 or 30; 90; 180 for patients | 170 to 180 |
| Aktar, 2016 [37] | February 2012 to April 2014 | Bangladesh | Prospective cohort | Cholera patients; n = 60 (2–5 y, n = 11; 6–17 y, n = 21; and 18–55 y, n = 28) | Vibriocidal antibodies; anti-CTB and anti-LPS antibodies | IgA and IgG | Plasma | Ogawa only | Guinea pig complement; ELISA | Days 2; 7; 30; 90; and 180 | 180 |
| Alam, 2013 [38] | December 2006 to May 2008 | Bangladesh | Prospective cohort | 30 (median age: 31) | Anti-CTB and LPS antibodies | IgA and IgG | Plasma | Ogawa (n = 20); Inaba (n = 10) | ELISA | Day 30; 90; 180; 270; and 360 | 360 |
| Alam, 2011 [39] | October 2008 and June 2010 | Bangladesh | Prospective cohort | Cholera patients (n = 70; adult) | Vibriocidal antibodies, anti-CTB and anti-LPS antibodies | IgA and IgG | Plasma | Ogawa (n = 55) and Inaba (15) | ELISA; ELISA | Day 3; 30; 90; 180; 270; and 360 | 360 |
| Uddin, 2011 [40] | Not reported | Bangladesh | Prospective cohort | 18; Patients had severe cholera. Median age = 30 | Anti-CTB and LPS antibodies | IgA and IgG | Duodenal biopsy and plasma | Ogawa (n = 16); Inaba (n = 2) | ELISA | Day 2; 7; 30; 90; 180; and 360 | 360 |
| Kendall, 2010 [41] | April 2007 to April 2009 | Bangladesh | Prospective cohort | n = 41 (26 of these were frozen samples) Mean age = 30 | Vibriocidal antibodies; anti-CTB and anti-LPS antibodies | IgA, IgG, and IgM | Plasma | Ogawa (n = 32); Inaba (n = 9) | ELISA | Day 2; 7; 30; 90 | 90 |
| Harris, 2009 [42] | December 2006 to May 2008 | Bangladesh | Prospective cohort | Cholera patients (n = 39; median age: 24 y) | Vibriocidal antibodies, TcpA, anti-CTB, ASC and LPS responses | IgA and IgG | Serum and plasma | Ogawa (n = 26) and Inaba (n = 13) | Guinea pig complement; ELISA | Day 2; 7; 30; 90; 180; 270; and 360 | 360 |
| Jayasekera, 2008 [43] | December 2006 to May 2007 | Bangladesh | Prospective cohort | 14 (mean ag: 30). Patients had severe cholera | Vibriocidal antibodies; anti-CTB and anti-LPS antibodies | IgA and IgG | Serum | Ogawa (n = 7); Inaba (n = 7) | ELISA | Day 2; 7; 30; 90 | 90 |
| Risk of Bias Assessment | ||||
|---|---|---|---|---|
| Author, Year, Reference | Selection of Participants (4 Stars Could Be Awarded) | Comparability (2 Stars Could Be Awarded) | Outcome (3 Stars Could Be Awarded) | Total Score (A Maximum of 9 Stars Could Be Awarded) |
| Representativeness of the Exposed Cohort; Selection of Controls; Ascertainment of Exposure; Demonstration That Outcome of Interest Was Not Present at the Start of the Study | Comparability of Cohorts on the Basis of the Design or Analysis; Additional Factors | Assessment of Outcome; Adequate Follow-Up Period for Outcome of Interest to Occur; Complete Follow-Up (All Subjects Accounted for) | ||
| Azman, 2019 [35] | *** | ** | *** | 8 |
| Hossain, 2019 [36] | *** | ** | *** | 8 |
| Aktar, 2016 [37] | *** | * | ** | 6 |
| Alam, 2013 [38] | **** | ** | *** | 9 |
| Alam, 2011 [39] | *** | * | ** | 6 |
| Uddin, 2011 [40] | ** | ** | *** | 7 |
| Kendall, 2010 [41] | *** | * | ** | 6 |
| Harris, 2009 [42] | *** | ** | *** | 8 |
| Jayasekera, 2008 [43] | ** | ** | ** | 6 |
References
- World Health Organization (WHO). Cholera. Available online: https://www.who.int/health-topics/cholera#tab=tab_1 (accessed on 24 May 2022).
- Kanungo, S.; Azman, A.S.; Ramamurthy, T.; Deen, J.; Dutta, S. Cholera. Lancet 2022, 399, 1429–1440. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Cholera vaccines: WHO position paper—August 2017. Wkly. Epidemiol. Rec. 2017, 92, 477–498. [Google Scholar]
- Lipp, E.K.; Huq, A.; Colwell, R.R. Effects of global climate on infectious disease: The cholera model. Clin. Microbiol. Rev. 2002, 15, 757–770. [Google Scholar] [CrossRef] [PubMed]
- Alam, M.; Sultana, M.; Nair, G.B.; Siddique, A.K.; Hasan, N.A.; Sack, R.B.; Sack, D.A.; Ahmed, K.U.; Sadique, A.; Watanabe, H.; et al. Viable but nonculturable Vibrio cholerae O1 in biofilms in the aquatic environment and their role in cholera transmission. Proc. Natl. Acad. Sci. USA 2007, 104, 17801–17806. [Google Scholar] [CrossRef] [PubMed]
- Muzembo, B.A.; Kitahara, K.; Ohno, A.; Debnath, A.; Okamoto, K.; Miyoshi, S.-I. Cholera rapid diagnostic tests for the detection of Vibrio cholerae O1: An updated meta-analysis. Diagnostics 2021, 11, 2095. [Google Scholar] [CrossRef]
- Yoon, S.H.; Waters, C.M. Vibrio cholerae. Trends Microbiol. 2019, 27, 806–807. [Google Scholar] [CrossRef]
- Clemens, J.D.; Nair, G.B.; Ahmed, T.; Qadri, F.; Holmgren, J. Cholera. Lancet 2017, 390, 1539–1549. [Google Scholar] [CrossRef]
- Hu, D.; Liu, B.; Feng, L.; Ding, P.; Guo, X.; Wang, M.; Cao, B.; Reeves, P.R.; Wang, L. Origins of the current seventh cholera pandemic. Proc. Natl. Acad. Sci. USA 2016, 113, E7730–E7739. [Google Scholar] [CrossRef]
- Leung, D.T.; Chowdhury, F.; Calderwood, S.B.; Qadri, F.; Ryan, E.T. Immune responses to cholera in children. Expert Rev. Anti-Infect. Ther. 2012, 10, 435–444. [Google Scholar] [CrossRef]
- Legros, D. Partners of the global task force on cholera control global cholera epidemiology: Opportunities to reduce the burden of cholera by 2030. J. Infect. Dis. 2018, 218, S137–S140. [Google Scholar] [CrossRef]
- Muzembo, B.A.; Kitahara, K.; Debnath, A.; Ohno, A.; Okamoto, K.; Miyoshi, S.-I. Cholera outbreaks in India, 2011–2020: A systematic review. Int. J. Environ. Res. Public Health 2022, 19, 5738. [Google Scholar] [CrossRef] [PubMed]
- Goma Epidemiology Group. Public health impact of Rwandan refugee crisis: What happened in Goma, Zaire, in July 1994? Lancet 1995, 345, 339–344. [Google Scholar] [CrossRef]
- Camacho, A.; Bouhenia, M.; Alyusfi, R.; Alkohlani, A.; Naji, M.A.M.; de Radiguès, X.; Abubakar, A.M.; Almoalmi, A.; Seguin, C.; Sagrado, M.J.; et al. Cholera epidemic in Yemen, 2016–2018: An analysis of surveillance data. Lancet Glob. Health 2018, 6, e680–e690. [Google Scholar] [CrossRef]
- Ingelbeen, B.; Hendrickx, D.; Miwanda, B.; Van Der Sande, M.A.; Mossoko, M.; Vochten, H.; Riems, B.; Nyakio, J.-P.; Vanlerberghe, V.; Lunguya, O.; et al. Recurrent cholera outbreaks, democratic republic of the Congo, 2008–2017. Emerg. Infect. Dis. 2019, 25, 856–864. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Cholera outbreak—Haiti, October 2010. MMWR Morb. Mortal. Wkly. Rep. 2010, 59, 1411. [Google Scholar]
- Ali, M.; Nelson, A.; Lopez, A.L.; Sack, D.A. Updated global burden of cholera in endemic countries. PLoS Negl. Trop. Dis. 2015, 9, e0003832. [Google Scholar] [CrossRef]
- Barzilay, E.J.; Schaad, N.; Magloire, R.; Mung, K.S.; Boncy, J.; Dahourou, G.A.; Mintz, E.D.; Steenland, M.W.; Vertefeuille, J.F.; Tappero, J.W. Cholera surveillance during the haiti epidemic—The first 2 Years. N. Engl. J. Med. 2013, 368, 599–609. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Cholera outbreak, Zimbabwe. Wkly. Epidemiol. Rec. 2009, 84, 50–52. [Google Scholar]
- Azman, A.S.; Luquero, F.J.; Ciglenecki, I.; Grais, R.F.; Sack, D.A.; Lessler, J. The impact of a one-dose versus two-dose oral cholera vaccine regimen in outbreak settings: A modeling study. PLoS Med. 2015, 12, e1001867. [Google Scholar] [CrossRef]
- Teoh, S.L.; Kotirum, S.; Hutubessy, R.C.W.; Chaiyakunapruk, N. Global economic evaluation of oral cholera vaccine: A systematic review. Hum. Vaccines Immunother. 2017, 14, 420–429. [Google Scholar] [CrossRef]
- Ali, M.; Emch, M.; Park, J.K.; Yunus, M.; Clemens, J. Natural cholera infection-derived immunity in an endemic setting. J. Infect. Dis. 2011, 204, 912–918. [Google Scholar] [CrossRef] [PubMed]
- Pasetti, M.F.; Levine, M.M. Insights from natural infection-derived immunity to cholera instruct vaccine efforts. Clin. Vaccine Immunol. 2012, 19, 1707–1711. [Google Scholar] [CrossRef]
- Metcalf, C.J.E.; Farrar, J.; Cutts, F.T.; Basta, N.E.; Graham, A.L.; Lessler, J.; Ferguson, N.M.; Burke, D.S.; Grenfell, B.T. Use of serological surveys to generate key insights into the changing global landscape of infectious disease. Lancet 2016, 388, 728–730. [Google Scholar] [CrossRef]
- Leung, T.; Matrajt, L. Protection afforded by previous Vibrio cholerae infection against subsequent disease and infection: A review. PLoS Negl. Trop. Dis. 2021, 15, e0009383. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.M.; Rahman, M.A.; Mohasin, M.; Riyadh, M.A.; Leung, D.; Alam, M.M.; Chowdhury, F.; Khan, A.I.; Weil, A.A.; Aktar, A.; et al. Memory B cell responses to Vibrio cholerae O1 lipopolysaccharide are associated with protection against infection from household contacts of patients with cholera in Bangladesh. Clin. Vaccine Immunol. 2012, 19, 842–848. [Google Scholar] [CrossRef]
- Mukhopadhyay, S.; Nandi, B.; Ghose, A. Antibodies (IgG) to lipopolysaccharide of Vibrio cholerae O1 mediate protection through inhibition of intestinal adherence and colonisation in a mouse model. FEMS Microbiol. Lett. 2000, 185, 29–35. [Google Scholar] [CrossRef][Green Version]
- Ryan, E.T.; Leung, D.T.; Jensen, O.; Weil, A.A.; Bhuiyan, T.R.; Khan, A.I.; Chowdhury, F.; LaRocque, R.C.; Harris, J.B.; Calderwood, S.B.; et al. Systemic, mucosal, and memory immune responses following cholera. Trop. Med. Infect. Dis. 2021, 6, 192. [Google Scholar] [CrossRef]
- Benenson, A.S.; Saad, A.; Paul, M. Serological studies in cholera. I. Vibrio agglutinin response of cholera patients determined by a microtechnique. Bull. World Health Organ. 1968, 38, 267. [Google Scholar]
- Harris, J.B.; Larocque, R.C.; Chowdhury, F.; Khan, A.I.; Logvinenko, T.; Faruque, A.S.G.; Ryan, E.T.; Qadri, F.; Calderwood, S.B. Susceptibility to Vibrio cholerae infection in a cohort of household contacts of patients with cholera in Bangladesh. PLoS Negl. Trop. Dis. 2008, 2, e221. [Google Scholar] [CrossRef]
- Harris, J.B. Cholera: Immunity and prospects in vaccine development. J. Infect. Dis. 2018, 218, S141–S146. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Wells, G.A.; Shea, B.; O’Connell, D.; Pereson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle–Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 13 March 2022).
- Higgins, J.P.T.; Thompson, S.G. Quantifying heterogeneity in a meta-analysis. Stat. Med. 2002, 21, 1539–1558. [Google Scholar] [CrossRef] [PubMed]
- Azman, A.S.; Lessler, J.; Luquero, F.J.; Bhuiyan, T.R.; Khan, A.I.; Chowdhury, F.; Kabir, A.; Gurwith, M.; Weil, A.A.; Harris, J.B.; et al. Estimating cholera incidence with cross-sectional serology. Sci. Transl. Med. 2019, 11, eaau6242. [Google Scholar] [CrossRef] [PubMed]
- Hossain, M.; Islam, K.; Kelly, M.; Mayo Smith, L.M.; Charles, R.C.; Weil, A.A.; Bhuiyan, T.R.; Kováč, P.; Xu, P.; Calderwood, S.B.; et al. Immune responses to O-specific polysaccharide (OSP) in North American adults infected with Vibrio cholerae O1 Inaba. PLoS Negl. Trop. Dis. 2019, 13, e0007874. [Google Scholar] [CrossRef]
- Aktar, A.; Rahman, M.A.; Afrin, S.; Faruk, M.O.; Uddin, T.; Akter, A.; Sami, M.I.N.; Yasmin, T.; Chowdhury, F.; Khan, A.I.; et al. O-specific polysaccharide-specific memory B cell responses in young children, older children, and adults infected with Vibrio cholerae O1 Ogawa in Bangladesh. Clin. Vaccine Immunol. 2016, 23, 427–435. [Google Scholar] [CrossRef]
- Alam, M.M.; Arifuzzaman, M.; Ahmad, S.M.; Hosen, M.I.; Rahman, M.A.; Rashu, R.; Sheikh, A.; Ryan, E.T.; Calderwood, S.B.; Qadri, F. Study of avidity of antigen-specific antibody as a means of understanding development of long-term immunological memory after Vibrio cholerae O1 infection. Clin. Vaccine Immunol. 2013, 20, 17–23. [Google Scholar] [CrossRef]
- Alam, M.M.; Riyadh, M.A.; Fatema, K.; Rahman, M.A.; Akhtar, N.; Ahmed, T.; Chowdhury, M.I.; Chowdhury, F.; Calderwood, S.B.; Harris, J.B.; et al. Antigen-specific memory B-cell responses in Bangladeshi adults after one- or two-dose oral killed cholera vaccination and comparison with responses in patients with naturally acquired cholera. Clin. Vaccine Immunol. 2011, 18, 844–850. [Google Scholar] [CrossRef]
- Uddin, T.; Harris, J.B.; Bhuiyan, T.R.; Shirin, T.; Uddin, M.I.; Khan, A.I.; Chowdhury, F.; LaRocque, R.C.; Alam, N.H.; Ryan, E.T.; et al. Mucosal immunologic responses in cholera patients in Bangladesh. Clin. Vaccine Immunol. 2011, 18, 506–512. [Google Scholar] [CrossRef]
- Kendall, E.A.; Tarique, A.A.; Hossain, A.; Alam, M.M.; Arifuzzaman, M.; Akhtar, N.; Chowdhury, F.; Khan, A.I.; LaRocque, R.C.; Harris, J.B.; et al. Development of immunoglobulin M memory to both a T-cell-independent and a T-cell-dependent antigen following infection with Vibrio cholerae O1 in Bangladesh. Infect. Immun. 2010, 78, 253–259. [Google Scholar] [CrossRef][Green Version]
- Harris, A.M.; Bhuiyan, M.S.; Chowdhury, F.; Khan, A.I.; Hossain, A.; Kendall, E.A.; Rahman, A.; LaRocque, R.C.; Wrammert, J.; Ryan, E.T.; et al. Antigen-specific memory B-cell responses to Vibrio cholerae O1 infection in Bangladesh. Infect. Immun. 2009, 77, 3850–3856. [Google Scholar] [CrossRef]
- Jayasekera, C.R.; Harris, J.B.; Bhuiyan, S.; Chowdhury, F.; Khan, A.I.; Faruque, A.S.G.; Larocque, R.C.; Ryan, E.T.; Ahmed, R.; Qadri, F.; et al. Cholera toxin–specific memory B cell responses are induced in patients with dehydrating diarrhea caused by Vibrio cholerae O1. J. Infect. Dis. 2008, 198, 1055–1061. [Google Scholar] [CrossRef] [PubMed]
- Charles, R.C.; Kelly, M.; Tam, J.M.; Akter, A.; Hossain, M.; Islam, K.; Biswas, R.; Kamruzzaman, M.; Chowdhury, F.; Khan, A.I.; et al. Humans surviving cholera develop antibodies against Vibrio cholerae O-specific polysaccharide that inhibit pathogen motility. mBio 2020, 11, e02847-20. [Google Scholar] [CrossRef] [PubMed]
- Levine, M.M.; Black, R.; Clements, M.L.; Cisneros, L.; Nalin, D.R.; Young, C.R. Duration of infection-derived immunity to cholera. J. Infect. Dis. 1981, 143, 818–820. [Google Scholar] [CrossRef] [PubMed]
- Holmgren, J. An update on cholera immunity and current and future cholera vaccines. Trop. Med. Infect. Dis. 2021, 6, 64. [Google Scholar] [CrossRef] [PubMed]
- Iyer, A.S.; Harris, J.B. Correlates of protection for cholera. J. Infect. Dis. 2021, 224, S732–S737. [Google Scholar] [CrossRef] [PubMed]
- Johnson, R.A.; Uddin, T.; Aktar, A.; Mohasin, M.; Alam, M.M.; Chowdhury, F.; Harris, J.B.; Larocque, R.C.; Bufano, M.K.; Yu, Y.; et al. Comparison of immune responses to the O-specific polysaccharide and lipopolysaccharide of Vibrio cholerae O1 in Bangladeshi adult patients with cholera. Clin. Vaccine Immunol. 2012, 19, 1712–1721. [Google Scholar] [CrossRef]
- Desai, S.N.; Cravioto, A.; Sur, D.; Kanungo, S. Maximizing protection from use of oral cholera vaccines in developing country settings: An immunological review of oral cholera vaccines. Hum. Vaccines Immunother. 2014, 10, 1457–1465. [Google Scholar] [CrossRef]
- Simanjuntak, C.H.; O’Hanley, P.; Punjabi, N.H.; Noriega, F.; Pazzaglia, G.; Dykstra, P.; Kay, B.; Budiarso, A.; Rifai, A.R.; Suharyono; et al. Safety, immunogenicity, and transmissibility of single-dose live oral cholera vaccine strain CVD l03-HgR in 24- to 59-month-old Indonesian children. J. Infect. Dis. 1993, 168, 1169–1176. [Google Scholar] [CrossRef]
- Haney, D.J.; Lock, M.D.; Gurwith, M.; Simon, J.K.; Ishioka, G.; Cohen, M.B.; Kirkpatrick, B.D.; Lyon, C.E.; Chen, W.H.; Sztein, M.B.; et al. Lipopolysaccharide-specific memory B cell responses to an attenuated live cholera vaccine are associated with protection against Vibrio cholerae infection. Vaccine 2018, 36, 2768–2773. [Google Scholar] [CrossRef]
- Weil, A.A.; Arifuzzaman, M.; Bhuiyan, T.R.; LaRocque, R.C.; Harris, A.M.; Kendall, E.A.; Hossain, A.; Tarique, A.A.; Sheikh, A.; Chowdhury, F.; et al. Memory T-Cell responses to Vibrio cholerae O1 infection. Infect. Immun. 2009, 77, 5090–5096. [Google Scholar] [CrossRef][Green Version]
- Richie, E.E.; Punjabi, N.H.; Sidharta, Y.Y.; Peetosutan, K.K.; Sukandar, M.M.; Wasserman, S.S.; Lesmana, M.M.; Wangsasaputra, F.F.; Pandam, S.S.; Levine, M.M.; et al. Efficacy trial of single-dose live oral cholera vaccine CVD 103-HgR in North Jakarta, Indonesia, a cholera-endemic area. Vaccine 2000, 18, 2399–2410. [Google Scholar] [CrossRef]
- McCarty, J.; Bedell, L.; de Lame, P.-A.; Cassie, D.; Lock, M.; Bennett, S.; Haney, D. Update on CVD 103-HgR single-dose, live oral cholera vaccine. Expert Rev. Vaccines 2021, 21, 9–23. [Google Scholar] [CrossRef] [PubMed]
- Weil, A.A.; Chowdhury, F.; Khan, A.I.; Leung, D.T.; Uddin, T.; Begum, Y.A.; Saha, N.C.; Charles, R.C.; Larocque, R.C.; Harris, J.B.; et al. Frequency of reexposure to Vibrio cholerae O1 evaluated by subsequent vibriocidal titer rise after an episode of severe cholera in a highly endemic area in Bangladesh. Am. J. Trop. Med. Hyg. 2012, 87, 921–926. [Google Scholar] [CrossRef] [PubMed]
- Mosley, W.H.; Ahmad, S.; Benenson, A.S.; Ahmed, A. The relationship of vibriocidal antibody titre to susceptibility to cholera in family contacts of cholera patients. Bull. World Health Organ. 1968, 38, 777–785. [Google Scholar] [PubMed]
- Ritter, A.S.; Chowdhury, F.; Franke, M.F.; Becker, R.L.; Bhuiyan, T.R.; Khan, A.I.; Saha, N.C.; Ryan, E.T.; Calderwood, S.B.; Larocque, R.C.; et al. Vibriocidal titer and protection from cholera in children. Open Forum Infect. Dis. 2019, 6, ofz057. [Google Scholar] [CrossRef] [PubMed]
- Glass, R.I.; Svennerholm, A.-M.; Khan, M.R.; Huda, S.; Huq, M.I.; Holmgren, J. Seroepidemiological studies of EI tor cholera in Bangladesh: Association of serum antibody levels with protection. J. Infect. Dis. 1985, 151, 236–242. [Google Scholar] [CrossRef]
- Okuno, T.; Kashige, N.; Satho, T.; Irie, K.; Hiramatsu, Y.; Sharmin, T.; Fukumitsu, Y.; Uyeda, S.; Yamada, S.; Harakuni, T.; et al. Expression and secretion of cholera toxin B subunit in lactobacilli. Biol. Pharm. Bull. 2013, 36, 952–958. [Google Scholar] [CrossRef]
- Baldauf, K.J.; Royal, J.; Hamorsky, K.T.; Matoba, N. Cholera toxin B: One subunit with many pharmaceutical applications. Toxins 2015, 7, 974–996. [Google Scholar] [CrossRef]
- Clemens, J.D.; Sack, D.A.; Harris, J.R.; Van Loon, F.; Chakraborty, J.; Ahmed, F.; Rao, M.R.; Khan, M.R.; Yunus, M.D.; Huda, N.; et al. Field trial of oral cholera vaccines in Bangladesh: Results from three-year follow-up. Lancet 1990, 335, 270–273. [Google Scholar] [CrossRef]
- Yuki, Y.; Nojima, M.; Hosono, O.; Tanaka, H.; Kimura, Y.; Satoh, T.; Imoto, S.; Uematsu, S.; Kurokawa, S.; Kashima, K.; et al. Oral MucoRice-CTB vaccine for safety and microbiota-dependent immunogenicity in humans: A phase 1 randomised trial. Lancet Microbe 2021, 2, e429–e440. [Google Scholar] [CrossRef]
- Aktar, A.; Rahman, M.A.; Afrin, S.; Akter, A.; Uddin, T.; Yasmin, T.; Sami, I.N.; Dash, P.; Jahan, S.R.; Chowdhury, F.; et al. Plasma and memory B cell responses targeting O-specific polysaccharide (OSP) are associated with protection against Vibrio cholerae O1 infection among household contacts of cholera patients in Bangladesh. PLoS Negl. Trop. Dis. 2018, 12, e0006399. [Google Scholar] [CrossRef] [PubMed]
- Sack, D.A.; Debes, A.K.; Ateudjieu, J.; Bwire, G.; Ali, M.; Ngwa, M.C.; Mwaba, J.; Chilengi, R.; Orach, C.C.; Boru, W.; et al. Contrasting epidemiology of cholera in Bangladesh and Africa. J. Infect. Dis. 2021, 224, S701–S709. [Google Scholar] [CrossRef] [PubMed]


| Days after Onset | Number of Studies (n) | Data Point (n) | Pooled Mean Vibriocidal Titer (95% CI) | Number of Studies (n) | Data Point (n) | Pooled Mean Vibriocidal Titer (95% CI) * |
|---|---|---|---|---|---|---|
| 2 | 4 | 4 | 123.20 (77.00, 169.40) | 5 | 6 | 123.00 (105.15, 140.85) |
| 7 | 3 | 3 | 6955.94 (2444.88, 11,466.99) | 4 | 5 | 4972.68 (2799.58, 7145.77) |
| 30 | 4 | 4 | 2247.32 (1300.71, 3193.92) | 5 | 6 | 1901.90 (1257.81, 2545.98) |
| 90 | 4 | 4 | 578.60 (267.43, 889.78) | 5 | 6 | 468.72 (272.63, 664.80) |
| 180 | 3 | 3 | 345.88 (163.05, 525.72) | 4 | 5 | 290.68 (190.39, 390.98) |
| 360 | 3 | 3 | 177.18 (122.16, 232.21) | 4 | 5 | 227.37 (177.18, 277.56) ** |
| Days after Onset | Number of Studies (n) | Data Point (n) | Pooled Mean IgA Antibody Response to CTB (95% CI), ELISA Units | Number of Studies (n) | Data Point (n) | * Pooled Mean IgA Antibody Response to CTB (95% CI), ELISA Units * |
|---|---|---|---|---|---|---|
| 2 | 6 | 7 | 5.32 (4.23, 6.41) | 7 | 9 | 5.81 (4.70, 6.93) |
| 7 | 4 | 5 | 49.07 (41.15, 56.99) | 5 | 7 | 55.54 (46.51, 64.57) |
| 30 | 6 | 7 | 20.88 (16.46, 25.30) | 7 | 9 | 19.82 (15.63, 24.01) |
| 90 | 6 | 7 | 9.86 (8.45, 11.27) | 7 | 9 | 9.71 (7.83, 11.58) |
| 180 | 5 | 6 | 8.30 (6.69, 9.91) | 6 | 8 | 8.04 (6.12, 9.96) |
| 360 | 3 | 3 | 6.40 (5.01, 7.78) | 4 | 4 | 7.83 (5.05, 10.61) ** |
| Days after Onset | Number of Studies (n) | Data Point (n) | Pooled Mean IgG Antibody Response to CTB (95% CI), ELISA Units | Number of Studies (n) | Data Point (n) | Pooled Mean IgG Antibody Response to CTB (95% CI), ELISA Units * |
|---|---|---|---|---|---|---|
| 2 | 6 | 7 | 17.66 (14.84, 20.48) | 7 | 9 | 18.71 (16.02, 21.40) |
| 7 | 4 | 5 | 64.64 (57.54, 71.75) | 5 | 7 | 71.17 (62.41, 79.94) |
| 30 | 6 | 7 | 68.62 (64.91, 72.32) | 7 | 9 | 70.69 (66.81, 74.57) |
| 90 | 6 | 7 | 42.18 (38.93, 45.42) | 7 | 9 | 42.94 (40.03, 45.86) |
| 180 | 5 | 6 | 29.27 (26.02, 32.51) | 6 | 8 | 29.46 (26.75, 32.17) |
| 360 | 3 | 3 | 23.52 (20.91, 26.14) | 4 | 4 | 23.91 (22.77, 25.04) ** |
| Days after Onset | Number of Studies (n) | Data Point (n) | Pooled Mean IgA Antibody Response to LPS (95% CI), ELISA Units | Number of Studies (n) | Data Point (n) | Pooled Mean IgA Antibody Response to LPS (95% CI), ELISA Units * |
|---|---|---|---|---|---|---|
| 2 | 5 | 6 | 9.43 (8.27, 10.58) | 6 | 8 | 9.58 (8.86, 10.31) |
| 7 | 3 | 4 | 124.46 (90.38, 158.54) | 3 | 3 | 134.71 (91.74, 177.68) |
| 30 | 5 | 6 | 43.94 (33.25, 54.63) | 6 | 8 | 41.22 (29.47, 52.97) |
| 90 | 5 | 6 | 17.40 (13.60, 21.19) | 6 | 8 | 17.40 (14.72, 20.08) |
| 180 | 5 | 6 | 12.74 (10.97, 14.51) | 6 | 8 | 13.45 (11.55, 15.35) |
| 360 | 3 | 3 | 10.22 (8.84, 11.60) | 4 | 4 | 12.53 (11.37, 13.69) ** |
| Days after Onset | Number of Studies (n) | Data Point (n) | Pooled Mean IgG Antibody Response to LPS (95% CI), ELISA Units | Number of Studies (n) | Data Point (n) | Pooled Mean IgG Antibody Response to LPS (95% CI), ELISA Units * |
|---|---|---|---|---|---|---|
| 2 | 5 | 6 | 35.24 (32.88, 37.59) | 6 | 8 | 35.88 (33.57, 38.18) |
| 7 | 3 | 4 | 93.81 (80.47, 107.15) | 3 | 3 | 101.75 (72.74, 130.76) |
| 30 | 5 | 6 | 84.53 (76.24, 92.83) | 6 | 8 | 86.29 (77.42, 95.16) |
| 90 | 5 | 6 | 51.33 (37.44, 65.22) | 6 | 8 | 53.57 (42.86, 64.28) |
| 180 | 5 | 6 | 46.58 (35.54, 57.61) | 6 | 8 | 48.40 (39.79, 57.00) |
| 360 | 3 | 3 | 32.11 (25.04, 39.19) | 4 | 4 | 34.34 (28.24, 40.43) ** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muzembo, B.A.; Kitahara, K.; Mitra, D.; Ohno, A.; Miyoshi, S.-I. Long-Term Kinetics of Serological Antibodies against Vibrio cholerae Following a Clinical Cholera Case: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2022, 19, 7141. https://doi.org/10.3390/ijerph19127141
Muzembo BA, Kitahara K, Mitra D, Ohno A, Miyoshi S-I. Long-Term Kinetics of Serological Antibodies against Vibrio cholerae Following a Clinical Cholera Case: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health. 2022; 19(12):7141. https://doi.org/10.3390/ijerph19127141
Chicago/Turabian StyleMuzembo, Basilua Andre, Kei Kitahara, Debmalya Mitra, Ayumu Ohno, and Shin-Ichi Miyoshi. 2022. "Long-Term Kinetics of Serological Antibodies against Vibrio cholerae Following a Clinical Cholera Case: A Systematic Review and Meta-Analysis" International Journal of Environmental Research and Public Health 19, no. 12: 7141. https://doi.org/10.3390/ijerph19127141
APA StyleMuzembo, B. A., Kitahara, K., Mitra, D., Ohno, A., & Miyoshi, S.-I. (2022). Long-Term Kinetics of Serological Antibodies against Vibrio cholerae Following a Clinical Cholera Case: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 19(12), 7141. https://doi.org/10.3390/ijerph19127141





