Sudden Changes and Their Associations with Quality of Life during COVID-19 Lockdown: A Cross-Sectional Study in the French-Speaking Part of Switzerland
Abstract
1. Introduction
2. Materials and Methods
2.1. Context, Study Design, and Population Recruited
2.2. Measures
- -
- They had any novel sickness, any major illnesses they already had, a major illness affecting a family member close to them, an accident or injury, or if they had started caring for/helping a relative or friend;
- -
- they had broken up with a close relative (their lover, family, friends) or had conflicts with neighbours;
- -
- they had major financial difficulties;
- -
- someone in their close circle died (spouse or partner, one of their children, their father or mother, a sibling, another relative or close friend) or if they had lost their house pet;
- -
- they moved out: a voluntary move, a forced relocation, or the loss of their home; or
- -
- none of the above events.
- -
- workload (more, enough, or less than preferred),
- -
- accomplish fewer things (always, often, sometimes, rarely, never),
- -
- hang out more or less frequently than preferred (yes or no), and
- -
- do physical activity more or less than preferred (yes or no).
2.3. Statistical Analysis
3. Results
3.1. Representativeness of the Studied Population
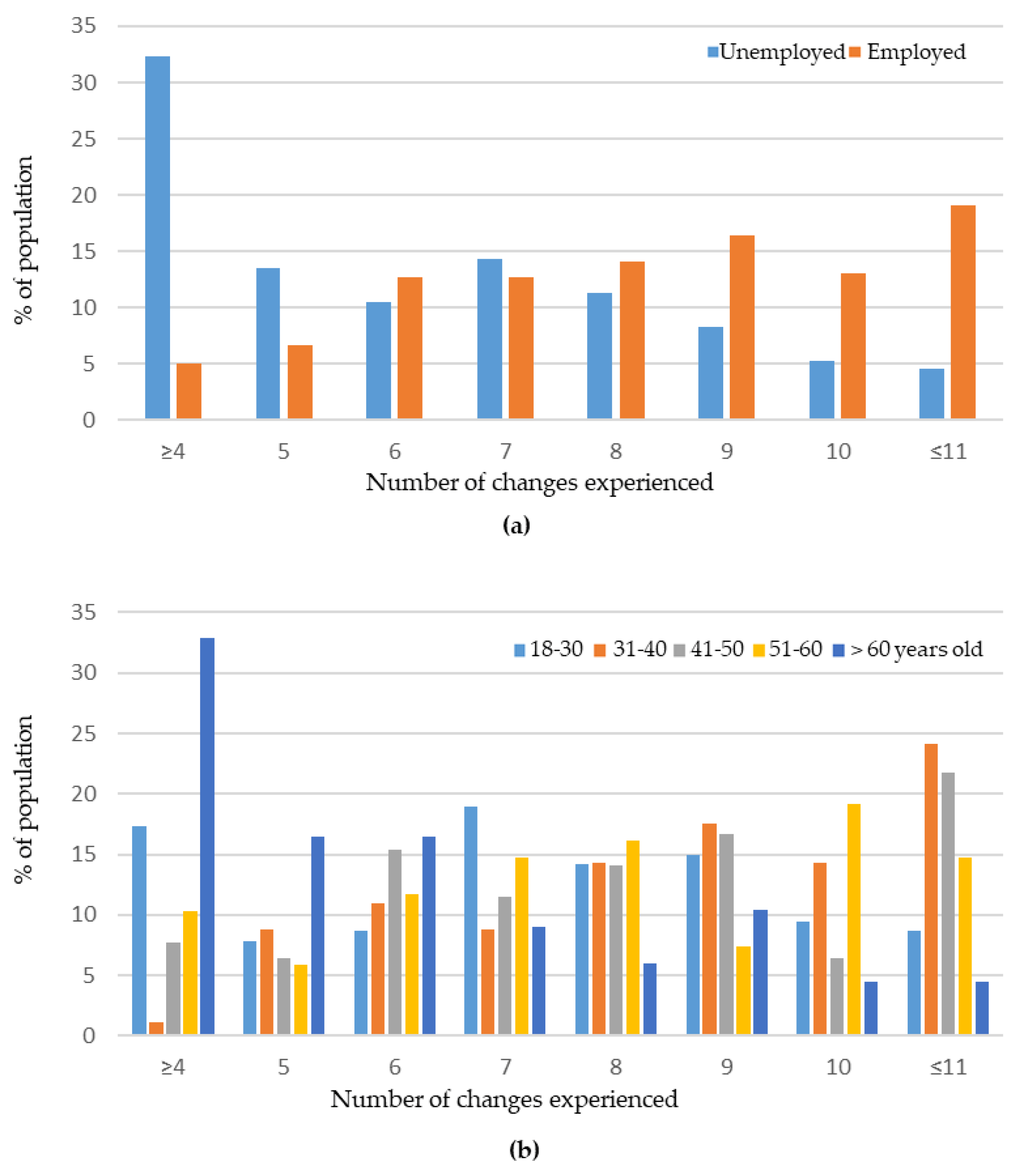
3.2. Changes in Everyday Life during the Lockdown
3.3. Risk Perception of COVID-19
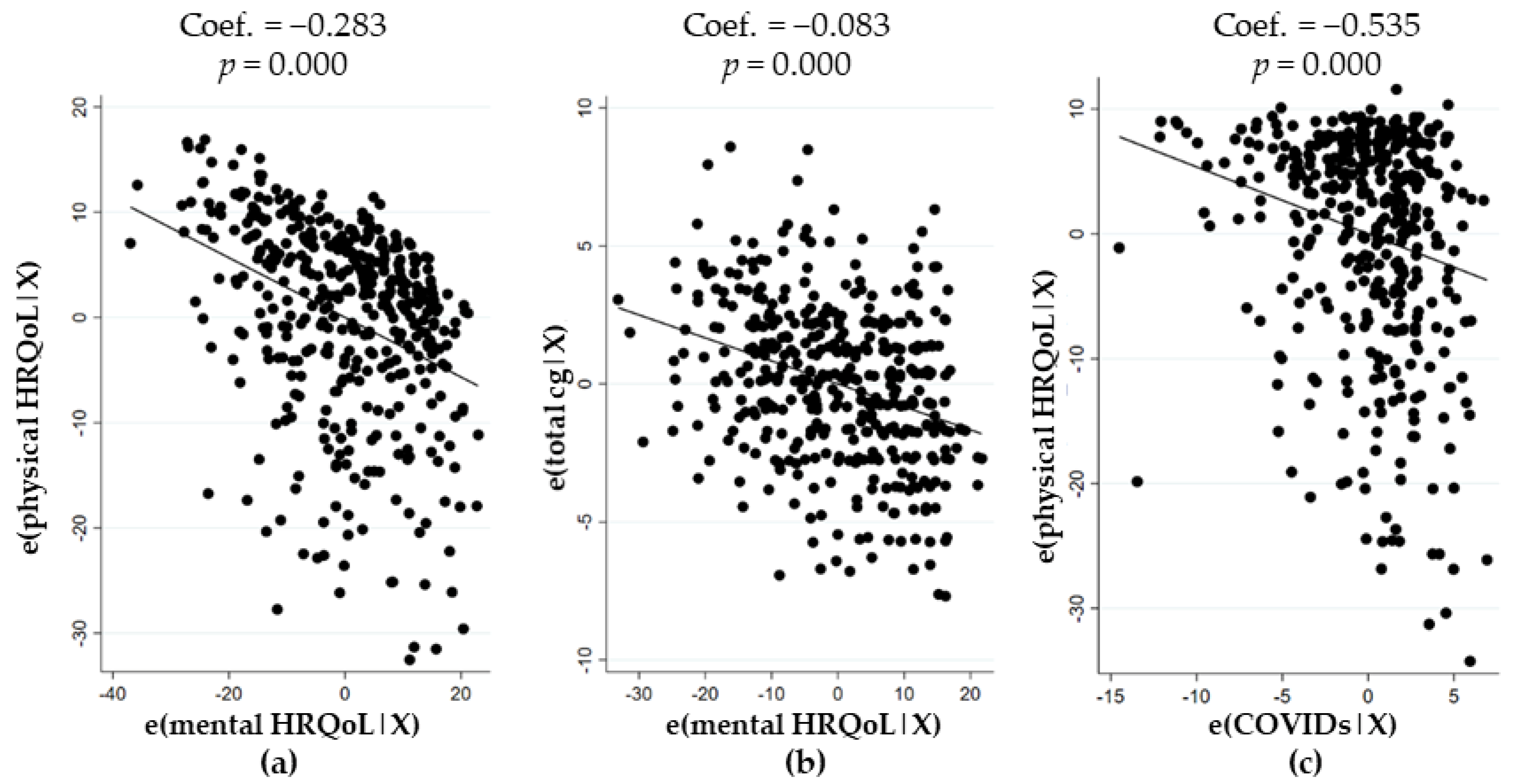
3.4. Association of Changes Experienced with Mental or Physical HRQoL Scores
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Brammer, L.M. Coping with life transitions. Int. J. Advancement Counsel. 1992, 15, 239–253. [Google Scholar] [CrossRef]
- Peschanski, D. «Tu crois qu’on s’en souviendra ?» Mémoire collective du Covid-19. Revue Neuropsychol. 2020, 12, 128–131. [Google Scholar]
- Pedrosa, A.L.; Bitencourt, L.; Fróes, A.C.F.; Cazumbá, M.L.B.; Campos, R.G.B.; de Brito, S.; Simões, E.S.A.C. Emotional, Behavioral, and Psychological Impact of the COVID-19 Pandemic. Front. Psychol. 2020, 11, 566212. [Google Scholar] [CrossRef]
- Marks, S.R. Durkheim’s Theory of Anomie. Am. J. Sociol. 1974, 80, 329–363. [Google Scholar] [CrossRef]
- Confédération Suisse Le Conseil fédéral Renforce les Mesures Contre le Coronavirus Pour Protéger la santé de la Population et Soutient les Secteurs Touchés. Available online: https://www.bag.admin.ch/bag/fr/home/das-bag/aktuell/medienmitteilungen.msg-id-78437.html (accessed on 25 March 2021).
- Federal Statistical Office Look for Statistics. Available online: https://www.bfs.admin.ch/bfs/en/home/statistics.html (accessed on 25 June 2020).
- Lambert, A.; Cayouette-Remblière, J.; Guéraut, É.; Le Roux, G.; Bonvalet, C.; Girard, V.; Langlois, L. How the COVID-19 epidemic changed working conditions in France. Popul. Societ. 2020, 579, 1–4. [Google Scholar]
- Bao, Y.; Sun, Y.; Meng, S.; Shi, J.; Lu, L. 2019-nCoV epidemic: Address mental health care to empower society. Lancet 2020, 395, e37–e38. [Google Scholar] [CrossRef]
- Rodríguez-Rey, R.; Garrido-Hernansaiz, H.; Collado, S. Psychological Impact and Associated Factors During the Initial Stage of the Coronavirus (COVID-19) Pandemic Among the General Population in Spain. Front. Psychol. 2020, 11, 1540. [Google Scholar]
- Xiang, Y.T.; Yang, Y.; Li, W.; Zhang, L.; Zhang, Q.; Cheung, T.; Ng, C.H. Timely mental health care for the 2019 novel coronavirus outbreak is urgently needed. Lancet Psychiatry 2020, 7, 228–229. [Google Scholar] [CrossRef]
- Al Najjar, N.S.; Attar, L.M.; Farahat, F.M.; Al Thaqafi, A. Psychobehavioural responses to the 2014 Middle East respiratory syndrome-novel corona virus [MERS CoV] among adults in two shopping malls in Jeddah, Western Saudi Arabia. East. Mediterr. Health J. 2016, 221, 817–823. [Google Scholar] [CrossRef]
- Rubin, G.J.; Potts, H.W.; Michie, S. The impact of communications about swine flu (influenza A H1N1v) on public responses to the outbreak: Results from 36 national telephone surveys in the UK. Health Technol. Assess. 2010, 14, 183–266. [Google Scholar] [CrossRef] [PubMed]
- Van Bortel, T.; Basnayake, A.; Wurie, F.; Jambai, M.; Koroma, A.S.; Muana, A.T.; Hann, K.; Eaton, J.; Martin, S.; Nellums, L.B. Psychosocial effects of an Ebola outbreak at individual, community and international levels. Bull. World Health Organ. 2016, 94, 210–214. [Google Scholar] [CrossRef]
- Orben, A.; Tomova, L.; Blakemore, S.-J. The effects of social deprivation on adolescent development and mental health. Lancet Child Adolesc. Health 2020, 4, 634–640. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodlan, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Fetzer, T.; Witte, M.; Hensel, L.; Jachimowicz, J.; Haushofer, J.; Ivchenko, A.; Caria, S.; Reutskaja, E.; Roth, C.; Fiorin, S.; et al. Perceptions of an Insufficient Government Response at the Onset of the COVID-19 Pandemic are Associated with Lower Mental Well-Being. PsyArXiv 2020. [Google Scholar] [CrossRef]
- Choi, E.P.H.; Hui, B.P.H.; Wan, E.Y.F.; Kwok, J.Y.Y.; Tam, T.H.L.; Wu, C. COVID-19 and Health-Related Quality of Life: A Community-Based Online Survey in Hong Kong. Int. J. Environ. Res. Public Health 2021, 18, 3228. [Google Scholar] [CrossRef]
- WHO. Policy Brief: COVID-19 and the Need for Action on Mental Health; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Taha, S.; Matheson, K.; Cronin, T.; Anisman, H. Intolerance of uncertainty, appraisals, coping, and anxiety: The case of the 2009 H1N1 pandemic. Br. J. Health Psychol. 2014, 19, 592–605. [Google Scholar] [CrossRef] [PubMed]
- Rettie, H.; Daniels, J. Coping and tolerance of uncertainty: Predictors and mediators of mental health during the COVID-19 pandemic. Am. Psychol. 2020. [Google Scholar] [CrossRef]
- Zheng, Z.; Han, W.; Li, Y.; Wang, D.; Gu, S.; Wang, F. The Mediating Effect of Coping Style in the Relationship Between Depression and Disordered Eating Among Chinese Female Undergraduates. Front. Psychol. 2020, 10. [Google Scholar] [CrossRef]
- Bemanian, M.; Mæland, S.; Blomhoff, R.; Rabben, Å.K.; Arnesen, E.K.; Skogen, J.C.; Fadnes, L.T. Emotional Eating in Relation to Worries and Psychological Distress Amid the COVID-19 Pandemic: A Population-Based Survey on Adults in Norway. Int. J. Environ. Res. Public Health 2021, 18, 130. [Google Scholar] [CrossRef]
- Savitsky, B.; Findling, Y.; Ereli, A.; Hendel, T. Anxiety and coping strategies among nursing students during the COVID-19 pandemic. Nurse. Educ. Pract. 2020, 46, 102809. [Google Scholar] [CrossRef]
- Godinic, D.; Obrenovic, B. Hudaykulov, A. Effects of Economic Uncertainty on Mental Health in the COVID-19 Pandemic Context: Social Identity Disturbance, Job Uncertainty and Psychological Well-Being Model. Int. J. Innov. Econ. Dev. 2020, 6, 61–74. [Google Scholar] [CrossRef]
- Knell, G.; Robertson, M.C.; Dooley, E.E.; Burford, K.; Mendez, K.S. Health Behavior Changes During COVID-19 Pandemic and Subsequent “Stay-at-Home” Orders. Int. J. Environ. Res. Public Health 2020, 17, 6268. [Google Scholar] [CrossRef]
- Tanaka, K.; Tahara, M.; Mashizume, Y.; Takahashi, K. Effects of Lifestyle Changes on the Mental Health of Healthcare Workers with Different Sense of Coherence Levels in the Era of COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 2801. [Google Scholar] [CrossRef] [PubMed]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attinà, A.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; Scerbo, F.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Trans. Med. 2020, 18, 229. [Google Scholar] [CrossRef] [PubMed]
- Huber, B.C.; Steffen, J.; Schlichtiger, J.; Graupe, T.; Deuster, E.; Strouvelle, V.P.; Fischer, M.R.; Massberg, S.; Brunner, S. Alteration of physical activity during COVID-19 pandemic lockdown in young adults. J. Trans. Med. 2020, 18, 410. [Google Scholar] [CrossRef] [PubMed]
- Mogensen, H.; Möller, J.; Hultin, H.; Mittendorfer-Rutz, E. Death of a close relative and the risk of suicide in sweden—A large scale register-based case-crossover study. PLoS ONE 2016, 11, e0164274. [Google Scholar] [CrossRef] [PubMed]
- Hennekam, S.; Bennett, D. Involuntary career transition and identity within the artist population. Person. Rev. 2016, 45, 1114–1131. [Google Scholar] [CrossRef]
- Mosca, I.; Barrett, A. The Impact of Voluntary and Involuntary Retirement on Mental Health: Evidence from Older Irish Adults. J. Ment. Health Policy Econ. 2016, 19, 33–44. [Google Scholar]
- Pressman, S.D.; Matthews, K.A.; Cohen, S.; Martire, L.M.; Scheier, M.; Baum, A.; Schulz, R. Association of enjoyable leisure activities with psychological and physical well-being. Psychosomatic. Med. 2009, 71, 725–732. [Google Scholar] [CrossRef]
- Achdut, N.; Refaeli, T. Unemployment and Psychological Distress among Young People during the COVID-19 Pandemic: Psychological Resources and Risk Factors. Int. J. Environ. Res. Public Health 2020, 17, 7163. [Google Scholar] [CrossRef]
- Wu, P.; Liu, X.; Fang, Y.; Fan, B.; Fuller, C.J.; Guan, Z.; Yao, Z.; Kong, J.; Lu, J.; Litvak, I.J. Alcohol abuse/dependence symptoms among hospital employees exposed to a SARS outbreak. Alcohol. Alcohol. 2008, 43, 706–712. [Google Scholar] [CrossRef] [PubMed]
- Krysinska, K.; Lester, D. Post-traumatic stress disorder and suicide risk: A systematic review. Arch.Suicide Res. 2010, 14, 1–23. [Google Scholar] [CrossRef] [PubMed]
- Cori, L.; Bianchi, F.; Cadum, E.; Anthonj, C. Risk Perception and COVID-19. Int. J. Environ. Res. Public Health 2020, 17, 3114. [Google Scholar] [CrossRef]
- Gralinski, L.E.; Menachery, V.D. Return of the Coronavirus: 2019-nCoV. Viruses 2020, 12, 135. [Google Scholar] [CrossRef] [PubMed]
- Confédération Suisse Communiqués du Conseil fédéral. Available online: https://www.admin.ch/gov/fr/accueil/documentation/communiques/communiques-conseil-federal.html?dyn_startDate=25.02.2020&dyn_endDate=21.03.2020&dyn_topic=0 (accessed on 5 July 2020).
- Santos-Eggimann, B.; Karmaniola, A.; Seematter-Bagnoud, L.; Spagnoli, J.; Büla, C.; Cornuz, J.; Rodondi, N.; Vollenweider, P.; Waeber, G.; Pécoud, A. The Lausanne cohort Lc65+: A population-based prospective study of the manifestations, determinants and outcomes of frailty. BMC Geriatr. 2008, 8, 20. [Google Scholar] [CrossRef]
- Ware, J.; Kosinki, M.; Keller, S. SF-12: How to Score the SF-12 Physical and Mental Health Summary Scales, 2nd ed.; The Health Institute, New England Medical Center: Boston, MA, USA, 1995. [Google Scholar]
- Voeten, H. Standard Questionnaire on Risk Perception of An Infectious Disease Outbreak. Effective Communication in Outbreak Management for Europe; Municipal Public Health Service Rotterdam-Rijnmond (GGD): Rotterdam, The Netherlands, 2015; pp. 1–10. [Google Scholar]
- Drivsholm, T.; Eplov, L.F.; Davidsen, M.; Jørgensen, T.; Ibsen, H.; Hollnagel, H.; Borch-Johnsen, K. Representativeness in population-based studies: A detailed description of non-response in a Danish cohort study. Scand. J. Public Health 2006, 34, 623–631. [Google Scholar] [CrossRef]
- Bonvin, J.-M.; Lovey, M.; Rosenstein, E.; Kempeneers, P. La Population en Grande Précarité en Période de COVID-19 à Genéve: Conditions de vie et Stratégies de Résilience. Rapport Final de L’étude Sollicitée par la Fondation Colis du Cœur; Université de Genève: Gevena, Switzerland, 2020. [Google Scholar]
- Edwards, Z.; Howes, S.; Reedy, J.; Sefton, T. Poverty in the Pandemic: An Update on the Impact of Coronavirus on Low-Income Families and Children; Child Poverty Action Group, The Church of England: London, UK, 2020. [Google Scholar]
- Prime, H.; Wade, M.; Browne, D.T. Risk and resilience in family well-being during the COVID-19 pandemic. Am. Psychol. 2020, 75, 631–643. [Google Scholar] [CrossRef]
- Traber, D.; Jauffret-Roustide, M.; Roumian, J.; Morgiève, M.; Vellut, N.; Briffault, X.; Clot, C. L’impact du confinement sur la santé mentale, l’importance des signaux faibles et des indicateurs fins. Résultats préliminaires de l’enquête Covadapt. L’informat. Psychiatr. 2020, 96, 632–638. [Google Scholar]
- Pieh, C.; Budimir, S.; Probst, T. The effect of age, gender, income, work, and physical activity on mental health during coronavirus disease (COVID-19) lockdown in Austria. J. Psychosom. Res. 2020, 136, 110186. [Google Scholar] [CrossRef]
- Arora, T.; Grey, I. Health behaviour changes during COVID-19 and the potential consequences: A mini-review. J. Health Psychol. 2020, 25, 1155–1163. [Google Scholar] [CrossRef]
- Rubin, O.; Nikolaeva, A.; Nello-Deakin, S.; te Brommelstroet, M. What can we learn from the COVID-19 pandemic about how people experience working from home and commuting? CUS, University of Amsterdam, 2020; pp. 1–9. Available online: https://urbanstudies.uva.nl/content/blog-series/covid-19-pandemic-working-from-home-and-commuting.html (accessed on 25 March 2021).
- Baert, S.; Lippens, L.; Moens, E.; Weytjens, J.; Sterkens, P. The Covid-19 Crisis and Telework: A Research Survey on Experiences, Expectations and Hopes; IZA Institute of Labor Economics: Bonn, Germany, 2020; pp. 1–37. [Google Scholar]
- Kawohl, W.; Nordt, C. COVID-19, unemployment, and suicide. Lancet 2020, 7, 389–390. [Google Scholar] [CrossRef]
- Brzezinski, A.; Deiana, G.; Kecht, V.; Van Dijcke, D. The COVID-19 Pandemic: Government vs. Community Action Across the United States; Institute for New Economic Thinking at the Oxford Martin School: Oxford, UK, 2020. [Google Scholar]
- Bruine de Bruin, W. Age Differences in COVID-19 Risk Perceptions and Mental Health: Evidence From a National U.S. Survey Conducted in March 2020. J. Gerontol. Series B 2020, 76, e24–e29. [Google Scholar] [CrossRef]
- Karasneh, R.; Al-Azzam, S.; Muflih, S.; Soudah, O.; Hawamdeh, S.; Khader, Y. Media’s effect on shaping knowledge, awareness risk perceptions and communication practices of pandemic COVID-19 among pharmacists. Res. Soc. Adm. Pharm 2020, 17, 1897–1902. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Cho, S.I. Middle East respiratory syndrome risk perception among students at a university in South Korea, 2015. Am. J. Infect. Control 2017, 45, e53–e60. [Google Scholar] [CrossRef]
- World Health Organization Risk Communication and Community Engagement Readiness and Response to Coronavirus Disease (COVID-19): Interim Guidance; World Health Organization: Geneva, Switzerland, 2020; pp. 1–5.
- Bavel, J.J.V.; Baicker, K.; Boggio, P.S.; Capraro, V.; Cichocka, A.; Cikara, M.; Crockett, M.J.; Crum, A.J.; Douglas, K.M.; Druckman, J.N.; et al. Using social and behavioural science to support COVID-19 pandemic response. Nat. Hum. Behav. 2020, 4, 460–471. [Google Scholar] [CrossRef] [PubMed]
- Lohiniva, A.L.; Sane, J.; Sibenberg, K.; Puumalainen, T.; Salminen, M. Understanding coronavirus disease (COVID-19) risk perceptions among the public to enhance risk communication efforts: A practical approach for outbreaks, Finland, February 2020. Eurosurveillance 2020, 25, 2000317. [Google Scholar] [CrossRef] [PubMed]
- Korkeila, K.; Suominen, S.; Ahvenainen, J.; Ojanlatva, A.; Rautava, P.; Helenius, H.; Koskenvuo, M. Non-response and related factors in a nation-wide health survey. Eur. J. Epidemiol. 2001, 17, 991–999. [Google Scholar] [CrossRef]
| Variables | N (%) |
|---|---|
| Gender | |
| Female | 291 (67.5) |
| Age | |
| 18–30 | 127 (29.5) |
| 31–40 | 91 (21.1) |
| 41–50 | 78 (18.1) |
| 51–60 | 68 (15.8) |
| ≥61 | 67 (15.6) |
| Citizenship | |
| Swiss | 320 (74.3) |
| dual citizenship | 66 (15.3) |
| other | 45 (10.4) |
| Civil status | |
| single | 171 (39.7) |
| married or cohabiting | 205 (47.6) |
| separated or divorced | 48 (11.1) |
| widow or widower | 7 (1.6) |
| Education level | |
| first level | 14 (3.3) |
| second level | 116 (26.9) |
| third level | 301 (69.8) |
| Average household income (monthly, in CHF) | |
| less than 2500 CHF | 25 (5.8) |
| between CHF 2501 and 5000 | 77 (17.9) |
| between CHF 5001 and 7500 | 104 (24.1) |
| between CHF 7501 and 10,000 | 92 (21.4) |
| between 10,000 and 12,500 CHF | 63 (14.6) |
| ≥12,501 CHF | 70 (16.2) |
| Number of children | |
| none | 232 (53.83) |
| one | 58 (13.46) |
| two | 88 (20.42) |
| ≥three | 53 (12.3) |
| Children at home | |
| yes | 119 (59.8) |
| no | 80 (40.2) |
| Changes for N = 431 | n (%) | Mental HRQoL | Physical HRQoL | R-Squared |
|---|---|---|---|---|
| Coef. | Coef. | |||
| Food intake (frequent or systematic change) | 91 (21.1) | −0.013 *** | −0.008 *** | 0.134 |
| Different frequency in home cleaning | 191 (44.3) | −0.003 | −0.002 | 0.008 |
| Home-schooling of children | 85 (19.7) | 0.000 | −0.002 | 0.004 |
| Stop doing things (frequently or systematically) | 247 (57.3) | −0.009 *** | −0.001 | 0.050 |
| Different leisure activities | 341 (79.1) | 0.004 * | 0.004 | 0.012 |
| Mode of transportation | 231 (53.6) | −0.001 | 0.001 | 0.001 |
| Different frequency in sport practice | 109 (25.3) | −0.005 ** | −0.001 | 0.017 |
| Limitation in social interaction (frequent or systematic) | 240 (55.7) | −0.014*** | −0.005 | 0.100 |
| Conflicts (1 or 2 events) | 69 (16.0) | −0.011 *** | −0.003 | 0.122 |
| Diseases (1 or 2 events) | 108 (25.1) | −0.006 *** | −0.015 *** | 0.104 |
| Financial difficulties | 23 (5.3) | −0.002 ** | −0.001 | 0.016 |
| Relocation | 13 (3.0) | −0.000 | 0.000 | 0.004 |
| Deaths | 26 (6.0) | 0.000 | −0.001 | 0.003 |
| Accomplished less things than wished | 196 (45.5) | −0.015 *** | −0.004 | 0.118 |
| Hanging out less than wished | 325 (75.4) | −0.007 *** | −0.002 | 0.038 |
| Worked more or less than wished | 171 (39.7) | −0.001 | 0.006 * | 0.017 |
| Practiced less physical activities than wished | 229 (53.1) | −0.004 * | 0.000 | 0.012 |
| Work lifestyle | 260 (60.3) | 0.006 ** | 0.011 *** | 0.047 |
| Teleworking | 184 (42.7) | 0.003 | 0.008 ** | 0.022 |
| Consequence on the household income | 108 (25.1) | −0.001 | 0.003 | 0.007 |
| Partial employment | 36 (8.3) | 0.000 | 0.001 | 0.001 |
| Number of imposed changes | 360 (83.5) | −0.012 ** | 0.005 | 0.026 |
| Number of unexpected changes | 184 (42.7) | −0.021 *** | −0.021 *** | 0.120 |
| Number of unwished changes | 392 (90.9) | −0.028 *** | 0.001 | 0.086 |
| Total number of changes | 429 (99.5) | −0.083 *** | −0.01 | 0.111 |
| Mental HRQoL | Physical HRQoL | R-Squared | |
|---|---|---|---|
| Coef. | Coef. | ||
| What do you think the COVID-19 is? (4-point scale on knowledge) | 0.002 | −0.001 | 0.003 |
| How serious do you think the COVID-19 is? (5 point-scale from “not all” to “very serious”) | −0.002 | −0.026 *** | 0.100 |
| In your opinion, should COVID-19 be avoided? (dichotomous outcome) | 0.002 | −0.004 * | 0.035 |
| Do you think you can contract COVID-19 in the coming months if you do not take any preventive measures? (5-point scale from “certainly not” to “most certainly”) | −0.003 | −0.005 | 0.003 |
| How concerned are you about contracting COVID-19? (5-point scale from “certainly not” to “most certainly”) | −0.019 *** | −0.038 *** | 0.114 |
| Do you think the measures taken by the authorities during lockdown are … | |||
| … necessary? (5-point scale from “certainly not” to “most certainly”) | 0.004 | −0.010 * | 0.020 |
| … helping to prevent the spread of the infection? (5-point scale from “certainly not” to “most certainly”) | 0.009 ** | 0.000 | 0.018 |
| ... being respected by the general population? (5-point scale from “never” to “always”) | 0.006 | 0.009 * | 0.015 |
| Are you able to carry out the imposed measures? (5-point scale “never” to “always”) | −0.005 | −0.005 | 0.009 |
| Risk perception of COVID-19 overall score | −0.006 | −0.081 *** | 0.046 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Duay, M.; Morgiève, M.; Niculita-Hirzel, H. Sudden Changes and Their Associations with Quality of Life during COVID-19 Lockdown: A Cross-Sectional Study in the French-Speaking Part of Switzerland. Int. J. Environ. Res. Public Health 2021, 18, 4888. https://doi.org/10.3390/ijerph18094888
Duay M, Morgiève M, Niculita-Hirzel H. Sudden Changes and Their Associations with Quality of Life during COVID-19 Lockdown: A Cross-Sectional Study in the French-Speaking Part of Switzerland. International Journal of Environmental Research and Public Health. 2021; 18(9):4888. https://doi.org/10.3390/ijerph18094888
Chicago/Turabian StyleDuay, Manon, Margot Morgiève, and Hélène Niculita-Hirzel. 2021. "Sudden Changes and Their Associations with Quality of Life during COVID-19 Lockdown: A Cross-Sectional Study in the French-Speaking Part of Switzerland" International Journal of Environmental Research and Public Health 18, no. 9: 4888. https://doi.org/10.3390/ijerph18094888
APA StyleDuay, M., Morgiève, M., & Niculita-Hirzel, H. (2021). Sudden Changes and Their Associations with Quality of Life during COVID-19 Lockdown: A Cross-Sectional Study in the French-Speaking Part of Switzerland. International Journal of Environmental Research and Public Health, 18(9), 4888. https://doi.org/10.3390/ijerph18094888






