Particulate Matter 10 (PM10) Is Associated with Epistaxis in Children and Adults
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Statistical Analysis
3. Results
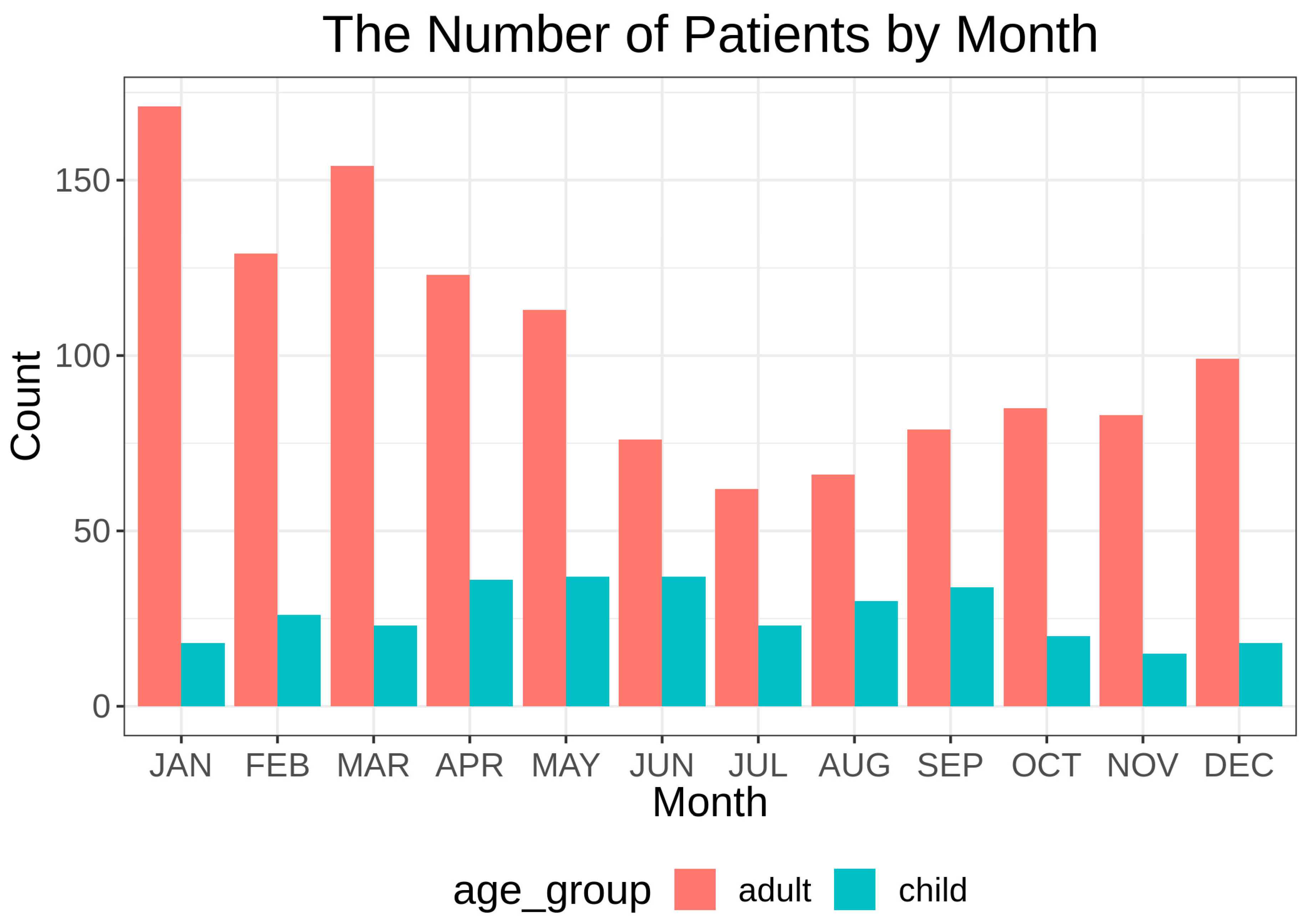
3.1. Characteristics of the Enrolled Subjects
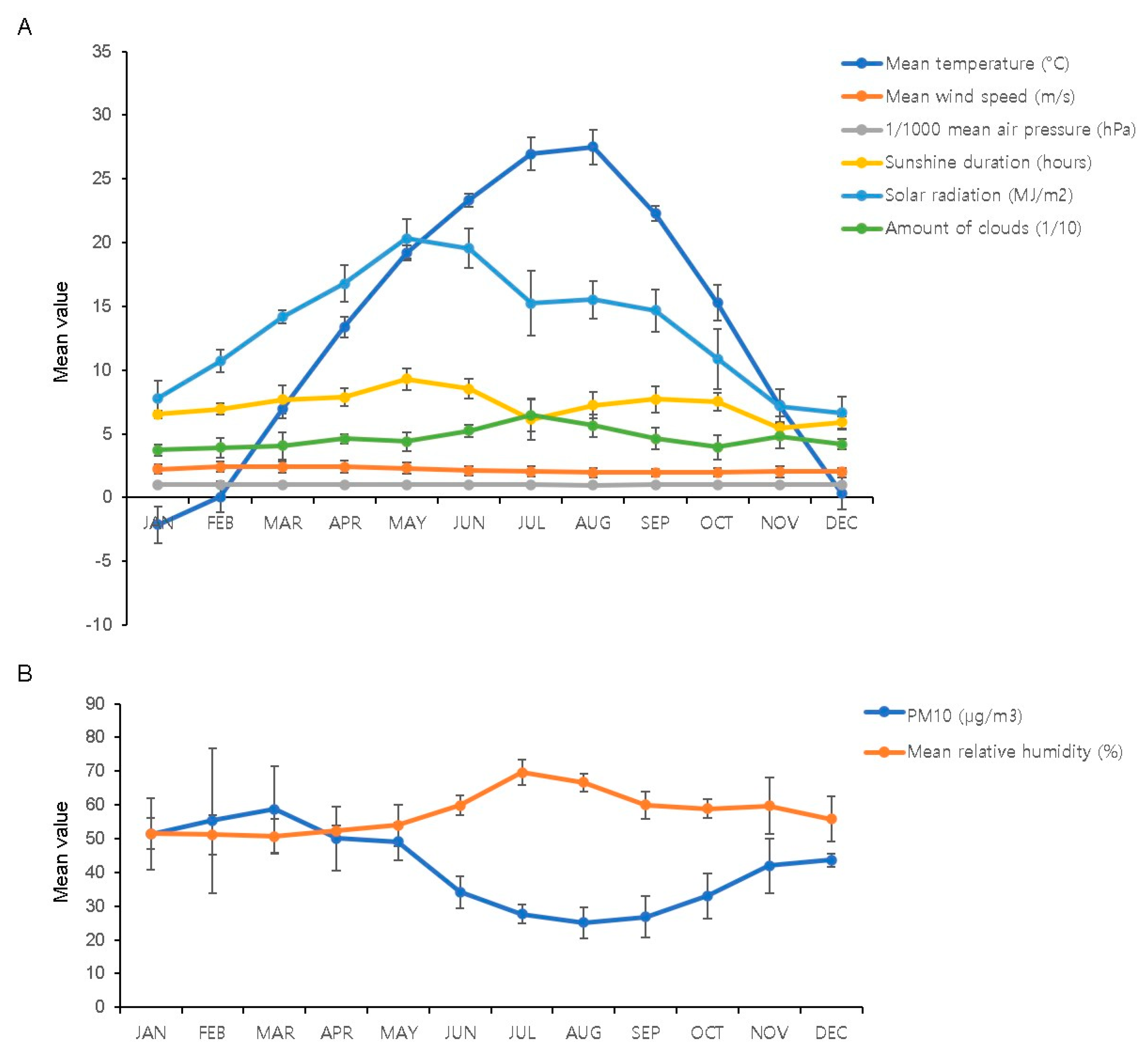
3.2. Monthly Distribution of Meteorological Factors and PM10 Concentration
3.3. Factors Associated with the Incidence of Epistaxis Presentation in Hospital per Day among Children and Adults
3.4. Factors Associated with the Number of Epistaxis Presentations in Hospital per Day among Children and Adults
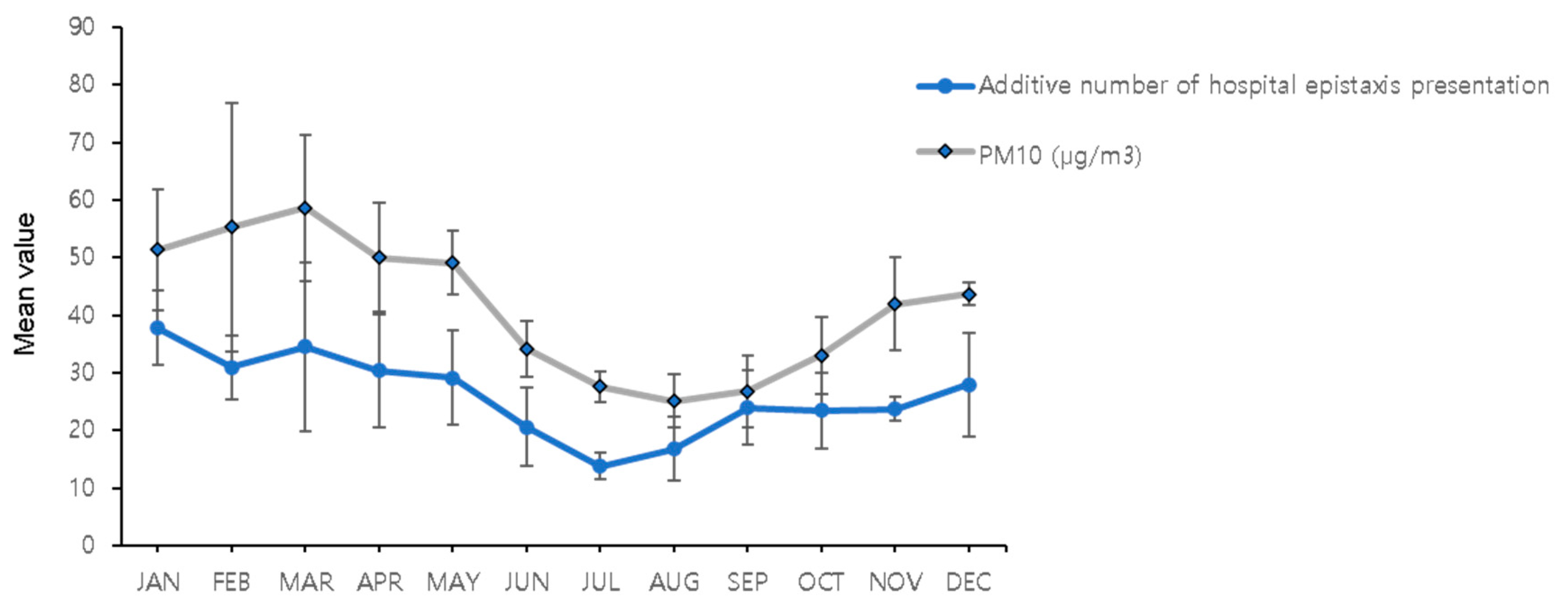
3.5. Additive Effect of PM10 Concentration on Epistaxis Presentation in Hospital
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Petruson, B. Epistaxis in childhood. Rhinology 1979, 17, 83–90. [Google Scholar]
- Kemal, O.; Sen, E. Does the weather really affect epistaxis? B-ENT 2014, 10, 199–202. [Google Scholar]
- Nunez, D.A.; McClymont, L.G.; Evans, R.A. Epistaxis: A study of the relationship with weather. Clin. Otolaryngol. Allied Sci. 1990, 15, 49–51. [Google Scholar] [CrossRef] [PubMed]
- Purkey, M.R.; Seeskin, Z.; Chandra, R. Seasonal variation and predictors of epistaxis. Laryngoscope 2014, 124, 2028–2033. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Bertisch, S.M.; Mostofsky, E.; Buettner, C.; Mittleman, M.A. Weather, ambient air pollution, and risk of migraine headache onset among patients with migraine. Environ. Int. 2019, 132, 105100. [Google Scholar] [CrossRef] [PubMed]
- Song, W.M.; Liu, Y.; Liu, J.Y.; Tao, N.N.; Li, Y.F.; Liu, Y.; Wang, L.X.; Li, H.C. The burden of air pollution and weather condition on daily respiratory deaths among older adults in China, Jinan from 2011 to 2017. Medicine (Baltimore) 2019, 98, e14694. [Google Scholar] [CrossRef]
- Reddy, V.M.; Judd, O.; Khalil, H. Investigation of the influence of ambient temperature, atmospheric pressure and water vapour pressure on epistaxis admission rate. Rhinology 2010, 48, 348–351. [Google Scholar] [CrossRef] [PubMed]
- Qureishi, A.; Burton, M.J. Interventions for recurrent idiopathic epistaxis (nosebleeds) in children. Cochrane Database Syst. Rev. 2012, 9, CD004461. [Google Scholar] [CrossRef] [PubMed]
- Kubba, H. Childhood epistaxis. Clin. Otolaryngol. 2006, 31, 212–213. [Google Scholar] [CrossRef] [PubMed]
- World Bank. Pm2.5 Air Pollution, Mean Annual Exposure (Micrograms Per Cubic Meter). Available online: https://data.worldbank.org/indicator/EN.ATM.PM25.MC.M3 (accessed on 28 January 2020).
- Akdogan, M.V.; Hizal, E.; Semiz, M.; Topal, Ö.; Akkaş, H.; Kabataş, A.; Erbek, S.S. The role of meteorologic factors and air pollution on the frequency of pediatric epistaxis. Ear Nose Throat J. 2018, 97, E1–E5. [Google Scholar] [CrossRef]
- Zhang, Y.; Cui, L.; Xu, D.; He, M.Z.; Zhou, J.; Han, L.; Li, X.; Li, T. The association of ambient PM2.5 with school absence and symptoms in schoolchildren: A panel study. Pediatr. Res. 2018, 84, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Dominici, F.; Peng, R.D.; Bell, M.L.; Pham, L.; McDermott, A.; Zeger, S.L.; Samet, J.M. Fine particulate air pollution and hospital admission for cardiovascular and respiratory diseases. JAMA 2006, 295, 1127–1134. [Google Scholar] [CrossRef] [PubMed]
- Kang, D.; Jung, I.B.; Lee, S.Y.; Park, S.J.; Kwon, S.J.; Park, D.H.; Son, J.W. Particulate matter less than 10 μm (PM10) activates cancer related genes in lung epithelial cells. Inhal. Toxicol. 2020, 32, 487–493. [Google Scholar] [CrossRef]
- Patel, M.M.; Chillrud, S.N.; Correa, J.C.; Hazi, Y.; Feinberg, M.; Kc, D.; Prakash, S.; Ross, J.M.; Levy, D.; Kinney, P.L. Traffic-related particulate matter and acute respiratory symptoms among New York City area adolescents. Environ. Health Perspect 2010, 118, 1338–1343. [Google Scholar] [CrossRef] [PubMed]
- Mazhar, A.; Rehman, A.; Sheikh, M.A.; Naeem, M.M.; Qaisar, I.; Mazhar, M. Neonates--a neglected paediatric age group. J. Pak. Med. Assoc. 2011, 61, 625–628. [Google Scholar]
- Yu, G.; Fu, Y.; Dong, C.; Duan, H.; Li, H. Is the occurrence of pediatric epistaxis related to climate variables? Int. J. Pediatr. Otorhinolaryngol. 2018, 113, 182–187. [Google Scholar] [CrossRef]
- Comelli, I.; Vincenti, V.; Benatti, M.; Macri, G.F.; Comelli, D.; Lippi, G.; Cervellin, G. Influence of air temperature variations on incidence of epistaxis. Am. J. Rhinol. Allergy 2015, 29, e175–e181. [Google Scholar] [CrossRef]
- Park, S.Y.; Byun, E.J.; Lee, J.D.; Kim, S.; Kim, H.S. Air pollution, autophagy, and skin aging: Impact of particulate matter (PM10) on human dermal fibroblasts. Int. J. Mol. Sci. 2018, 19, 2727. [Google Scholar] [CrossRef]
- Kang, I.G.; Ju, Y.H.; Jung, J.H.; Ko, K.P.; Oh, D.K.; Kim, J.H.; Lim, D.H.; Kim, Y.H.; Jang, T.Y.; Kim, S.T. The effect of PM10 on allergy symptoms in allergic rhinitis patients during spring season. Int. J. Environ. Res. Public Health 2015, 12, 735–745. [Google Scholar] [CrossRef]
- Choi, B.G.; Lee, J.; Kim, S.W.; Lee, M.W.; Baek, M.J.; Ryu, Y.G.; Choi, S.Y.; Byun, J.K.; Mashaly, A.; Park, Y.; et al. The association of chronic air pollutants with coronary artery spasm, vasospastic angina, and endothelial dysfunction. Coron. Artery Dis. 2018, 29, 336–343. [Google Scholar] [CrossRef]
- Jung, M.; Cho, D.; Shin, K. The impact of particulate matter on outdoor activity and mental health: A matching approach. Int. J. Environ. Res. Public Health 2019, 16, 2983. [Google Scholar] [CrossRef] [PubMed]
- Calderon-Garciduenas, L.; Rodriguez-Alcaraz, A.; Valencia-Salazar, G.; Mora-Tascareño, A.; García, R.; Osnaya, N.; Villarreal-Calderón, A.; Devlin, R.B.; Van Dyke, T. Nasal biopsies of children exposed to air pollutants. Toxicol. Pathol. 2001, 29, 558–564. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Chen, G.; Liu, F.; Mao, S.; Liu, Y.; Liu, S.; Mao, Z.; Lu, Y.; Wang, C.; Guo, Y.; et al. Associations between long-term exposure to air pollution and blood pressure and effect modifications by behavioral factors. Environ. Res. 2020, 182, 109109. [Google Scholar] [CrossRef]
- Send, T.; Bertlich, M.; Eichhorn, K.W.; Ganschow, R.; Schafigh, D.; Horlbeck, F.; Bootz, F.; Jakob, M. Etiology, management, and outcome of pediatric epistaxis. Pediatr. Emerg. Care 2019. online ahead of print. [Google Scholar] [CrossRef] [PubMed]
| N | |
|---|---|
| No. of days | 1704 |
| No. of epistaxis cases | 1557 |
| Age (years) | |
| Total | |
| Mean (SD) | 44.94 (25.34) |
| Range | 1–94 |
| Children to adults | 323:1234 |
| Children | |
| Mean (SD) | 7.59 (4.41) |
| Range | 1–17 |
| Adults | |
| Mean (SD) | 60.00 (18.85) |
| Range | 18–94 |
| Parameter | Univariate | Multivariate | ||
|---|---|---|---|---|
| Odds Ratio (95% CI) | p-Value | Odds Ratio (95% CI) | p-Value | |
| Children | ||||
| Mean temperature (°C) | 1.107 (1.005–1.030) | <0.001 | 1.025 (1.010–1.041) | <0.001 |
| Minimum temperature (°C) | 1.013 (1.001–1.026) | <0.001 | ||
| Maximum temperature (°C) | 1.020 (1.007–1.032) | <0.001 | ||
| Mean air pressure (hPa) | 0.979 (0.963–0.995) | 0.013 | ||
| Maximum wind speed (m/s) | 1.062 (0.991–1.137) | <0.001 | ||
| Mean wind speed (m/s) | 1.364 (1.160–1.601) | <0.001 | 1.385 (1.143–1.674) | <0.001 |
| Minimum relative humidity (%) | 0.991 (0.982–1.000) | <0.001 | ||
| Mean relative humidity (%) | 0.991 (0.982–1.000) | <0.001 | ||
| Sunshine duration (h) | 1.083 (1.045–1.123) | <0.001 | 1.064 (1.022–1.108) | 0.003 |
| Solar radiation amount (MJ/m2) | 1.045 (1.025–1.066) | <0.001 | ||
| Number of clouds (1/10) | 0.943 (0.902–0.985) | <0.001 | ||
| PM10 (μg/m3) | 1.004 (1.000–1.008) | <0.001 | 1.006 (1.001–1.011) | 0.040 |
| Adults | ||||
| Mean temperature (°C) | 0.967 (0.958–0.976) | <0.001 | ||
| Minimum temperature (°C) | 0.965 (0.956–0.974) | <0.001 | 0.970 (0.959–0.982) | <0.001 |
| Maximum temperature (°C) | 0.969 (0.960–0.978) | <0.001 | ||
| Mean air pressure (hPa) | 1.043 (1.030–1.057) | <0.001 | ||
| Maximum wind speed (m/s) | 0.989 (0.937–1.044) | 0.684 | ||
| Mean wind speed (m/s) | 1.076 (0.945–1.225) | 0.271 | ||
| Minimum relative humidity (%) | 0.987 (0.980–0.993) | <0.001 | ||
| Mean relative humidity (%) | 0.986 (0.979–0.993) | <0.001 | 0.987 (0.977–0.997) | 0.013 |
| Sunshine duration (h) | 0.987 | 0.329 | ||
| Solar radiation amount (MJ/m2) | 0.978 | 0.003 | ||
| Number of clouds (1/10) | 0.990 (0.958–1.023) | 0.554 | 1.085 (1.035–1.139) | <0.001 |
| PM10 (μg/m3) | 1.013 (1.008–1.018) | <0.001 | 1.008 (1.003–1.014) | 0.003 |
| Parameter | Univariate | Multivariate | ||
|---|---|---|---|---|
| Odds Ratio (95% CI) | p-Value | Odds Ratio (95% CI) | p-Value | |
| Children | ||||
| Mean temperature (°C) | 1.018 (1.005–1.030) | 0.005 | 1.005 (1.010–1.041) | <0.001 |
| Minimum temperature (°C) | 1.014 (1.002–1.026) | 0.025 | ||
| Maximum temperature (°C) | 1.020 (1.008–1.033) | 0.001 | ||
| Mean air pressure (hPa) | 0.978 (0.978–0.978) | <0.001 | ||
| Maximum wind speed (m/s) | 1.061 (0.990–1.135) | 0.088 | ||
| Mean wind speed (m/s) | 1.357 (1.155–1.591) | <0.001 | 1.385 (1.143–1.672) | <0.001 |
| Minimum relative humidity (%) | 0.991 (0.982–1.000) | 0.058 | ||
| Mean relative humidity (%) | 0.991 (0.982–1.000) | 0.061 | ||
| Sunshine duration (h) | 1.081 (1.044–1.122) | <0.001 | 1.063 (1.022–1.107) | 0.003 |
| Solar radiation amount (MJ/m2) | 1.044 (1.025–1.066) | <0.001 | ||
| Number of clouds (1/10) | 0.944 (0.904–0.986) | <0.001 | ||
| PM10 (μg/m3) | 1.004 (1.000–1.008) | 0.058 | 1.005 (1.001–1.010) | 0.019 |
| Adults | ||||
| Mean temperature (°C) | 0.965 (0.956–0.973) | <0.001 | ||
| Minimum temperature (°C) | 0.963 (0.955–0.971) | <0.001 | ||
| Maximum temperature (°C) | 0.967 (0.959–0.976) | <0.001 | 0.970(0.960–0.980) | <0.001 |
| Mean air pressure (hPa) | 1.045 (1.0453–1.0455) | <0.001 | ||
| Maximum wind speed (m/s) | 0.973 (0.925–1.023) | 0.289 | 0.915(0.862–0.971) | 0.003 |
| Mean wind speed (m/s) | 1.068 (0.955–1.207) | 0.295 | ||
| Minimum relative humidity (%) | 0.985 (0.978–0.991) | <0.001 | ||
| Mean relative humidity (%) | 0.984 (0.977–0.990) | <0.001 | 0.991(0.984–0.999) | 0.031 |
| Sunshine duration (h) | 0.993 (0.970–1.017) | 0.563 | ||
| Solar radiation amount (MJ/m2) | 0.977 (0.963–0.991) | 0.001 | ||
| Number of clouds (1/10) | 0.981 (0.951–1.012) | 0.222 | ||
| PM10 (μg/m3) | 1.010 (1.007–1.014) | <0.001 | 1.008(1.004–1.013) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, K.; Kwak, I.-Y.; Min, H. Particulate Matter 10 (PM10) Is Associated with Epistaxis in Children and Adults. Int. J. Environ. Res. Public Health 2021, 18, 4809. https://doi.org/10.3390/ijerph18094809
Kim K, Kwak I-Y, Min H. Particulate Matter 10 (PM10) Is Associated with Epistaxis in Children and Adults. International Journal of Environmental Research and Public Health. 2021; 18(9):4809. https://doi.org/10.3390/ijerph18094809
Chicago/Turabian StyleKim, Kyungsoo, Il-Youp Kwak, and Hyunjin Min. 2021. "Particulate Matter 10 (PM10) Is Associated with Epistaxis in Children and Adults" International Journal of Environmental Research and Public Health 18, no. 9: 4809. https://doi.org/10.3390/ijerph18094809
APA StyleKim, K., Kwak, I.-Y., & Min, H. (2021). Particulate Matter 10 (PM10) Is Associated with Epistaxis in Children and Adults. International Journal of Environmental Research and Public Health, 18(9), 4809. https://doi.org/10.3390/ijerph18094809





