Barriers, Facilitating Factors, and Intersectoral Collaboration for Promoting Active Mobility for Healthy Aging—A Qualitative Study within Local Government in Germany
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Area and Sample
2.3. Data Collection and Analysis
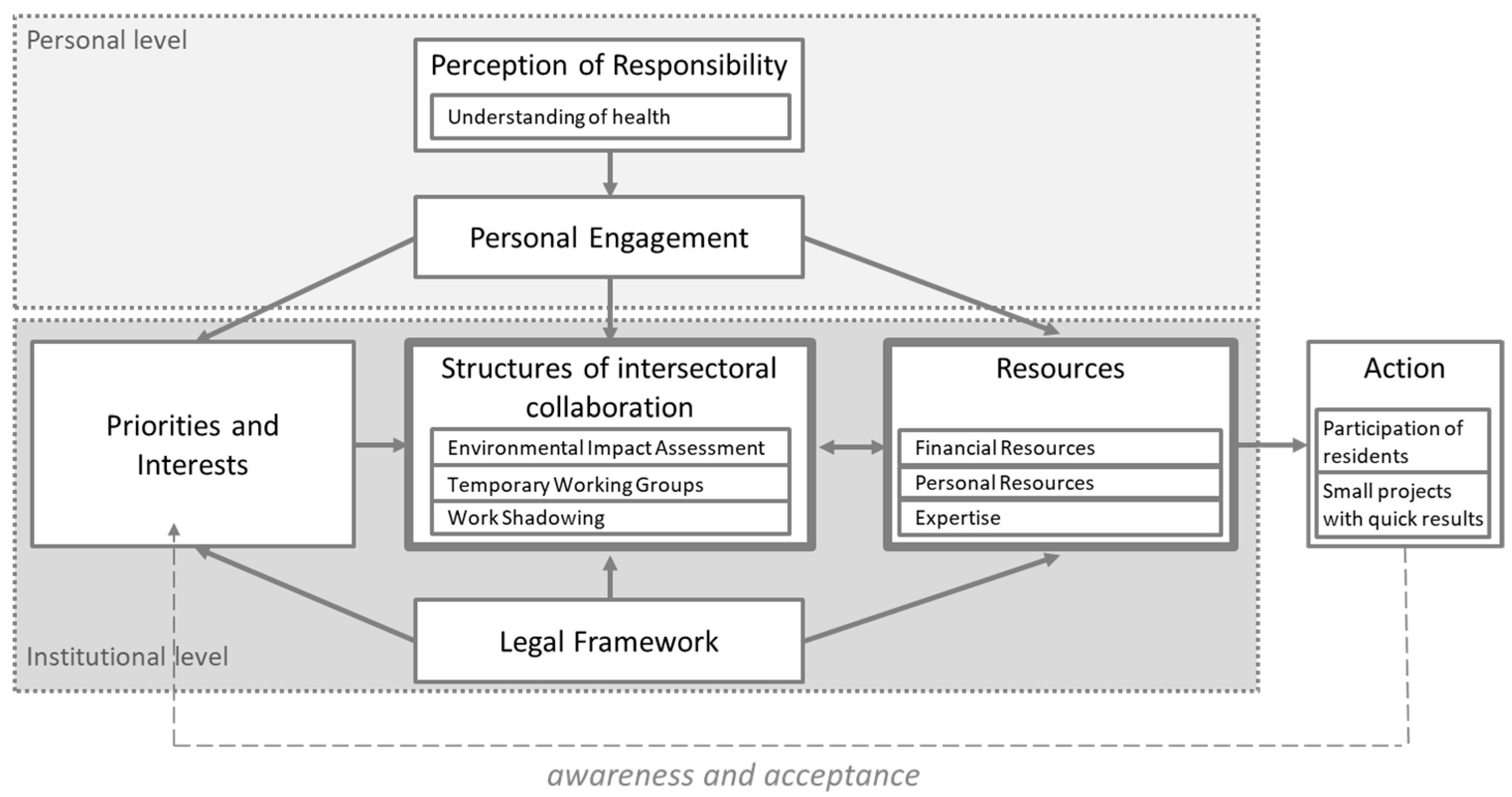
3. Results
3.1. Institutional Level
3.1.1. Legal Framework
3.1.2. Priorities and Interests
3.1.3. Structures of Intersectoral Collaboration
3.1.4. Resources
3.2. Personal Level
3.2.1. Perception of Responsibility
3.2.2. Personal Engagement
3.3. Action
4. Discussion
Strengths and Limitations
5. Implications for Research and Practice
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Current situation |
| How would you describe the situation for cyclists and pedestrians in your city/rural district? |
| ● Do you take into account the needs of special groups, e.g., older people? |
| ● Are there any spatial differences? |
| ● What kind of required action do you see from your own position? |
| ● In which context do your work on this topic? Does physical activity matter? |
| Points of contact in one’s own work |
| Are there any points of contact between health and spatial planning? Alternatively, what could you imagine? |
| ● Do you deal with prevention by environmental change? |
| ● Are there any interventions on active mobility promotion? |
| ● What about addressing health issues in the planning department? |
| Intersectoral collaboration |
| How and when do the health department and the planning department work together? What experiences do you have? |
| ● If none, why? |
| ● What experiences do you have with health impact assessment and environmental impact assessment? |
| ● Are there any committees in which you work together? What is your experience? What goals did you achieve together? |
| Question about a special project or concept in the city/rural district |
| Please tell us about this project/concept. How did it start and who is involved? |
| ● Who determined the content alignment? Who is the leader of the project/concept? |
| ● How are the needs of older people addressed in the project/concept? |
| ● How is the promotion of physical activity addressed in the project/concept? |
| ● In what way did the health department participate in the development of the project? |
| ● Are there any other projects on physical activity promotion where the health department is involved? |
| Outlook |
| The topic of health promotion is now supported by the new law of prevention, also in the community setting. What chances do you see to better integrate the topic into your daily routine by this law? What conditions need to be complied with? |
| ● What role could the health and planning departments take up, respectively, in projects of healthy city development? |
| ● Which other actors would be relevant? |
References
- EU. Ageing Europe—Looking at the Lives of Older People in the EU; Publications Office of the European Union: Luxembourg, 2019. [Google Scholar]
- Kemperman, A.; van den Berg, P.; Weijs-Perrée, M.; Uijtdewillegen, K. Loneliness of Older Adults: Social Network and the Living Environment. Int. J. Environ. Res. Public Health 2019, 16, 406. [Google Scholar] [CrossRef] [PubMed]
- Kelly, P.; Kahlmeier, S.; Götschi, T.; Orsini, N.; Richards, J.; Roberts, N.; Scarborough, P.; Foster, C. Systematic review and meta-analysis of reduction in all-cause mortality from walking and cycling and shape of dose response relationship. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 132. [Google Scholar] [CrossRef] [PubMed]
- Carr, K.; Weir, P.L.; Azar, D.; Azar, N.R. Universal Design: A Step toward Successful Aging. J. Aging Res. 2013, 2013, 8. [Google Scholar] [CrossRef] [PubMed]
- Moran, M.; van Cauwenberg, J.; Hercky-Linnewiel, R.; Cerin, E.; Deforche, B.; Plaut, P. Understanding the relationships between the physical environment and physical activity in older adults: A systematic review of qualitative studies. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 79. [Google Scholar] [CrossRef] [PubMed]
- Brüchert, T.; Baumgart, S.; Bolte, G. Social determinants of older adults’ urban design preference: A cross-sectional study. Cities Health 2021, in press. [Google Scholar] [CrossRef]
- Brüchert, T.; Hasselder, P.; Quentin, P.; Bolte, G. Walking for Transport among Older Adults: A Cross-Sectional Study on the Role of the Built Environment in Less Densely Populated Areas in Northern Germany. Int. J. Environ. Res. Public Health 2020, 17, 9479. [Google Scholar] [CrossRef] [PubMed]
- Van Cauwenberg, J.; Clarys, P.; de Bourdeaudhuij, I.; van Holle, V.; Verte, D.; de Witte, N.; de Donder, L.; Buffel, T.; Dury, S.; Deforche, B. Physical environmental factors related to walking and cycling in older adults: The Belgian aging studies. BMC Public Health 2012, 12, 142. [Google Scholar] [CrossRef]
- Cohen, J.M.; Boniface, S.; Watkins, S. Health implications of transport planning, development and operations. J. Transp. Health 2014, 1, 63–72. [Google Scholar] [CrossRef]
- WHO. Our Cities, Our Health, Our Future. Acting on Social Determinants for Health Equity in Urban Settings; World Health Organization Centre for Health Development: Kobe, Japan, 2008. [Google Scholar]
- GBD. Global, regional, and national age-sex-specific mortality and life expectancy, 1950-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1684–1735. [Google Scholar] [CrossRef]
- WHO. WHO Global Report on Falls Prevention in Older Age; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- Faller, I.; Holz-Rau, C.; Scheiner, J. Traffic Accident Risks for the Population of Lower Saxony. ZES Z. Verkehrssicherheit. 2020, 1, 7–20. [Google Scholar]
- Giles-Corti, B.; Foster, S.; Shilton, T.; Falconer, R. The co-benefits for health of investing in active transportation. Nsw Public Health Bull. 2010, 21, 122–127. [Google Scholar] [CrossRef]
- Stahl, T.; Wismar, M.; Ollila, E.; Lahtinen, E.; Leppo, K. Health in All Policies. Prospects and Potentials; Ministry of Social Affairs and Health: Helsinki, Finland, 2006. [Google Scholar]
- Giles-Corti, B.; Vernez-Moudon, A.; Reis, R.; Turrell, G.; Dannenberg, A.L.; Badland, H.; Foster, S.; Lowe, M.; Sallis, J.F.; Stevenson, M.; et al. City planning and population health: A global challenge. Lancet 2016, 388, 2912–2924. [Google Scholar] [CrossRef]
- Leppo, K.; Tangcharoensathien, V. The Health Sector’s Role in HiAP. In Health in All Policies: Seizing Opportunities, Implementing Policies; Cook, S., Leppo, K., Ollila, E., Pena, S., Wismar, M., Eds.; Ministry of Social Affairs and Health: Helsinki, Finland, 2013; pp. 309–324. [Google Scholar]
- WHO. Health in All Policies (HiAP) Framework for Country Action; World Health Organization: Geneva, Switzerland, 2014. [Google Scholar]
- ÖGDG NRW. § 8 Mitwirkung an Planungen [§ 8 Participation in planning]; Ministry of the Interior Northrhine-Westfalia: Düsseldorf, Germany, 1997. [Google Scholar]
- WHO. Towards More Physical Activity in Cities Transforming Public Spaces to Promote Physical Activity—A Key Contributor to Achieving the Sustainable Development Goals in Europe; World Health Organization Regional Office for Europe: Copenhagen, Denmark, 2017. [Google Scholar]
- Exworthy, M.; Hunter, D.J. The Challenge of Joined-Up Government in Tackling Health Inequalities. Int. J. Public Adm. 2011, 34, 201–212. [Google Scholar] [CrossRef]
- Oliver, K.; Cairney, P. The dos and don’ts of influencing policy: A systematic review of advice to academics. Palgrave Commun. 2019, 5, 21. [Google Scholar] [CrossRef]
- Forberger, S.; Bammann, K.; Bauer, J.; Boll, S.; Bolte, G.; Brand, T.; Hein, A.; Koppelin, F.; Lippke, S.; Meyer, J.; et al. How to Tackle Key Challenges in the Promotion of Physical Activity among Older Adults (65+): The AEQUIPA Network Approach. Int. J. Environ. Res. Public Health 2017, 14, 379. [Google Scholar] [CrossRef]
- Brüchert, T.; Quentin, P.; Baumgart, S.; Bolte, G. Intersectoral collaboration of public health and urban planning for promotion of mobility and healthy ageing: Protocol of the AFOOT project. Cities Health 2017, 1, 83–88. [Google Scholar] [CrossRef]
- Witzel, A. The Problem-centered Interview. Forum Qual. Soz. Forum Qual. Soc. Res. 2000, 1. [Google Scholar] [CrossRef]
- Freie Hansestadt Bremen. Sustainable Urban Mobility Plan Bremen 2025; Senate Department for Environment, Construction and Transport: Bremen, Germany, 2014. [Google Scholar]
- Brüchert, T.; Quentin, P.; Bolte, G. The relationship between perceived built environment and cycling or e-biking for transport among older adults—A cross-sectional study. BMC Public Health 2021. under review. [Google Scholar]
- Helfferich, C. Die Qualität Qualitativer Daten: Manual für die Durchführung Qualitativer Interviews [The Quality of Qualitative Data: Manual for Conducting Qualitative Interviews]; VS Verlag für Sozialwissenschaften/Springer Fachmedien Wiesbaden GmbH: Wiesbaden, Germany, 2011. [Google Scholar]
- Kuckartz, U. Qualitative Inhaltsanalyse: Methoden, Praxis, Computerunterstützung [Qualitative Content Analysis: Methods, Practice, Computer Support]; Beltz Juventa: Weinheim, Germany, 2016. [Google Scholar]
- Hopf, C.; Schmidt, C. Zum Verhältnis von Innerfamilialen Sozialen Erfahrungen, Persönlichkeitsentwicklung und Politischen Orientierungen: Dokumentation und Erörterung des Methodischen Vorgehens in einer Studie zu Diesem Thema [On the Relationship between Intra-Family Social Experiences, Personality Development and Political Orientations: Documentation and Discussion of the Methodological Approach in a Study on this Topic]; SSOAR: Hildesheim, Germany, 1993. [Google Scholar]
- Meuser, M.; Nagel, U. Expertinneninterviews-vielfach erprobt, wenig bedacht. Ein Beitrag zur qualitativen Methodendiskussion [Expert interviews—tried and tested many times, often thoughtless. A contribution to the qualitative method discussion]. In Das Experteninterview: Theorie, Methode, Anwendung; Bogner, A., Littig, B., Menz, W., Eds.; VS, Verlag für Sozialwissenschaften: Wiesbaden, Germany, 2005; pp. 71–94. [Google Scholar]
- Tong, A.; Sainsbury, P.; Craig, J. Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 2007, 19, 349–357. [Google Scholar] [CrossRef] [PubMed]
- de Leeuw, E.; Clavier, C.; Breton, E. Health policy—Why research it and how: Health political science. Health Res. Policy Syst. Biomed. Cent. 2014, 12, 55. [Google Scholar] [CrossRef] [PubMed]
- Parkhurst, J.O. Appeals to evidence for the resolution of wicked problems: The origins and mechanisms of evidentiary bias. Policy Sci. 2016, 49, 373–393. [Google Scholar] [CrossRef]
- Exworthy, M. Policy to tackle the social determinants of health: Using conceptual models to understand the policy process. Health Policy Plan 2008, 23, 318–327. [Google Scholar] [CrossRef] [PubMed]
- Guglielmin, M.; Muntaner, C.; O’Campo, P.; Shankardass, K. A scoping review of the implementation of health in all policies at the local level. Health Policy 2018, 122, 284–292. [Google Scholar] [CrossRef]
- Riley, R.; Nazelle, A. Barriers and Enablers of Integrating Health Evidence into Transport and Urban Planning and Decision Making: A Framework. In Integrating Human Health into Urban and Transport Planning; Nieuwenhuijsen, M., Khries, H., Eds.; Springer: Cham, Switzerland, 2019; pp. 641–654. [Google Scholar]
- Nieuwenhuijsen, M.J.; Khreis, H.; Verlinghieri, E.; Mueller, N.; Rojas-Rueda, D. Participatory quantitative health impact assessment of urban and transport planning in cities: A review and research needs. Environ. Int. 2017, 103, 61–72. [Google Scholar] [CrossRef]
- Molnar, A.; Renahy, E.; O’Campo, P.; Muntaner, C.; Freiler, A.; Shankardass, K. Using Win-Win Strategies to Implement Health in All Policies: A Cross-Case Analysis. PLoS ONE 2016, 11, e0147003. [Google Scholar] [CrossRef]
- van Eyk, H.; Harris, E.; Baum, F.; Delany-Crowe, T.; Lawless, A.; MacDougall, C. Health in All Policies in South Australia-Did It Promote and Enact an Equity Perspective? Int. J. Environ. Res. Public Health 2017, 14, 1288. [Google Scholar] [CrossRef]
- Lake, A.A.; Henderson, E.J.; Townshend, T.G. Exploring planners’ and public health practitioners’ views on addressing obesity: Lessons from local government in England. Cities Health 2017, 1, 185–193. [Google Scholar] [CrossRef]
- Jansson, E.; Fosse, E.; Tillgren, P. National public health policy in a local context--implementation in two Swedish municipalities. Health Policy 2011, 103, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Mulgan, G. Health is not just the absence of illness: Health in All Policies and ‘all in health policies’. In Implementing Health in All Policies; Kickbusch, I., Buckett, K., Eds.; Department of Health, Government of South Australia Adelaide: Adelaide, Australia, 2010; pp. 39–48. [Google Scholar]
- Rudolph, L.; Caplan, J.; Ben-Moshe, K.; Dillon, L. Health in All Policies. Guide for State and Local Governments; American Public Health Association and Public Health Institute: Washington, DC, USA; Oakland, CA, USA, 2013. [Google Scholar]
- Marmot, M.; Allen, J.; Boyce, T.; Goldblatt, P.; Morrison, J. Health Equity in England: The Marmot Review 10 Years on; Institute of Health Equity: London, UK, 2020. [Google Scholar]
- Hallal, P.C.; Andersen, L.B.; Bull, F.C.; Guthold, R.; Haskell, W.; Ekelund, U. Global physical activity levels: Surveillance progress, pitfalls, and prospects. Lancet 2012, 380, 247–257. [Google Scholar] [CrossRef]
- Government of South Australia. Health in All Policies: The South Australian Approach; Government of South Australia: Adelaide, Australia, 2011.
- Carey, G.; Crammond, B. Action on the social determinants of health: Views from inside the policy process. Soc. Sci. Med. 2015, 128, 134–141. [Google Scholar] [CrossRef]
- Kingdon, J.W.; Thurber, J.A. Agendas, Alternatives, and Public Policies, Updated Edition; Longman Classics in Political Science, 2nd ed.; Longman: Boston, MA, USA, 2011. [Google Scholar]
- Hasselback, J.; Fuller, D.; Schwandt, M. Choosing tools for building healthy spaces: An overview of guidance toolkits available from North America and Australia. Cities Health 2017, 1, 31–37. [Google Scholar] [CrossRef]
- AFOOT-project team. Promoting Active Mobility among the Older Population. Guidelines for Cooperation between Municipal Planning and Building Authorities and Public Health Services in Small and Medium-Sized Towns in Germany; Bremen and Dortmund: Dortmund, Germany, 2018. [Google Scholar]
- Dragano, N.; Gerhardus, A.; Kurth, B.M.; Kurth, T.; Razum, O.; Stang, A.; Teichert, U.; Wieler, L.H.; Wildner, M.; Zeeb, H. Public Health: Setting Goals, Establishing Structures and Improving Health for All. Gesundheitswesen 2016, 78, 686–688. [Google Scholar] [CrossRef] [PubMed]
- Wildner, M.; Wieler, L.H.; Zeeb, H. Germany’s expanding role in global health. Lancet 2018, 391, 657. [Google Scholar] [CrossRef]
- Luederitz, C.; Schäpke, N.; Wiek, A.; Lang, D.J.; Bergmann, M.; Bos, J.J.; Burch, S.; Davies, A.; Evans, J.; König, A.; et al. Learning through evaluation—A tentative evaluative scheme for sustainability transition experiments. J. Clean. Prod. 2017, 169, 61–76. [Google Scholar] [CrossRef]
- de Leeuw, E. Engagement of Sectors Other than Health in Integrated Health Governance, Policy, and Action. Annu. Rev. Public Health 2017, 38, 329–349. [Google Scholar] [CrossRef] [PubMed]
- Kickbusch, I.; Gleicher, D. Governance for Health in the 21st Century; World Health Organization Regional Office for Europe: Copenhagen, Denmark, 2012. [Google Scholar]
- Pinto, A.D.; Molnar, A.; Shankardass, K.; O’Campo, P.J.; Bayoumi, A.M. Economic considerations and health in all policies initiatives: Evidence from interviews with key informants in Sweden, Quebec and South Australia. BMC Public Health 2015, 15, 171. [Google Scholar] [CrossRef]
| N | Sex/Gender | ||
|---|---|---|---|
| Female | Male | ||
| No. of interviewees * | 24 | 4 | 20 |
| Single Interviews | 3 | 0 | 3 ** |
| Double Interviews | 5 | 0 | 5 ** |
| Group Interviews (≥3 Interviewees) | 3 | 3 ** | 3 ** |
| Institutional age *** | |||
| median (min,max) | 8 (1–34) | 8 (1–21) | 12 (1–34) |
| Position | |||
| Head of Public Health Department | 8 | 0 | 8 |
| Head of Planning/Transport Department | 8 | 1 | 7 |
| Administrative staff—Planning/Transport | 4 | 1 | 3 |
| Administrative staff—Health | 0 | 0 | 0 |
| Administrative staff—Seniors/Demography | 3 | 2 | 1 |
| Head of regional development department | 1 | 0 | 1 |
| Administrative Level | |||
| No. of interviews in city administrations | 4 | 0 | 4 ** |
| No. of interviews in district administrations | 7 | 3 ** | 7 ** |
| Legal framework | |
|---|---|
| Quote 1 | “It is easier to protect an owl couple from [traffic noise] than an older couple living there.” (Public Health, City 3, 74) |
| Priorities and interests | |
| Quote 2 | “So, we always try to underpin and strengthen our positions, but with health, we have a relatively poor position and often lose out when it comes to conflicting goals.” (Public Health, City 3, 74) |
| Quote 3 | “It’s not law, but it exerts pressure if there are demands. What the Advisory Council says, that also has a political character.” (Public Health, City 3, 74). |
| Quote 4 | “So, there are EXTREME resistances [of the population] against it and that also leads to the fact that the local authorities are sometimes torn between two positions. On the one hand, they have to keep an eye on the interests of their residents; on the other hand, they know very well that they also need to give space to these alternative energy sources.” (Planning, District 1, 10) |
| Quote 5 | “Such politicians, who are willing to give up their careers for a long-term meaningful strategy—there are very few.” (Public Health, District 3, 138) |
| Structures of intersectoral collaboration | |
| Quote 6 | “I believe that we also have to change structurally […] on these issues. That’s one of those great things I expected in the law of public health services, that they think about STRUCTURES. BUT, I actually realized they’re going on like they used to. And that is wrong. We can have so many great ideas, but we will fail at the smallest trivialities.” (Public Health, District 1, 261) |
| Quote 7 | “[…] that is our biggest common problem, to get things into the heads in a forward-looking way, that we are ready to accept changes to which we haven’t been ready for years.” (Planning, District 1, 267) |
| Resources | |
| Quote 8 | “In the end, it’s personnel resources ... I do not have to ask for [project] money, but I have to have the opportunity to take care of those [additional topics].” (Public Health, City 1, 111) |
| Quote 9 | “We have neither the expertise nor the time, we have to read, we have to deal with it, we have to talk more often about such issues. That’s just not possible, that’s not possible.” (Public Health, District 3, 61) |
| Perception of responsibility | |
| Quote 10 | “Here in the department, we work risk-oriented. We look at the risks that affect people in the city, and we are always concerned with minimizing those risks ... so when I talk about noise action planning, I’m talking about noise. I’m also talking about quiet zones, but I do not have the focus on physical activity in quiet areas or whatever else I can do because it’s all about minimizing that stressor noise, that’s our point of view, in that direction we argue.” (Public Health, City 3, 17, and 21) |
| Quote 11 | “The more I think about the topic, promoting physical activity in old age is a quite complex topic which has many facets. Spontaneously I wouldn’t know where to start.” (Public Health, District 6, 55) |
| Personal Engagement | |
| Quote 12 | “Work is not done by itself and sometimes, if the mountain will not come to Muhammad, choose the opposite way and just go to the people and say: ‘I have this vision, let’s get together and discuss how we can achieve that.’” (Public Health, District 5, 110) |
| Quote 13 | “[...] it has to be a severe issue, that I’ll rack my brain over things that are not at all part of my routine.” (Public Health, District 3, 83) |
| Action | |
| Quote 14 | “[...] that is the plea for very simple solutions that may not be the pure science and may not be particularly rewarded in planners circles especially [...], but in that case, it is a clarity that goes along with the fact that [...] the people […] just do it that way.” (Planning, City 2, 57) |
| Quote 15 | “[...] So, if you want to bring such a topic into implementation, then you have to make it a topic again [...] so invite people and inspire them, ‘That’s a topic!’. And when they jump on it and are enthusiastic about the matter, then you can let go, then they march off. But that is difficult enough.” (Planning, District 6, 58–59) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brüchert, T.; Quentin, P.; Baumgart, S.; Bolte, G. Barriers, Facilitating Factors, and Intersectoral Collaboration for Promoting Active Mobility for Healthy Aging—A Qualitative Study within Local Government in Germany. Int. J. Environ. Res. Public Health 2021, 18, 3807. https://doi.org/10.3390/ijerph18073807
Brüchert T, Quentin P, Baumgart S, Bolte G. Barriers, Facilitating Factors, and Intersectoral Collaboration for Promoting Active Mobility for Healthy Aging—A Qualitative Study within Local Government in Germany. International Journal of Environmental Research and Public Health. 2021; 18(7):3807. https://doi.org/10.3390/ijerph18073807
Chicago/Turabian StyleBrüchert, Tanja, Paula Quentin, Sabine Baumgart, and Gabriele Bolte. 2021. "Barriers, Facilitating Factors, and Intersectoral Collaboration for Promoting Active Mobility for Healthy Aging—A Qualitative Study within Local Government in Germany" International Journal of Environmental Research and Public Health 18, no. 7: 3807. https://doi.org/10.3390/ijerph18073807
APA StyleBrüchert, T., Quentin, P., Baumgart, S., & Bolte, G. (2021). Barriers, Facilitating Factors, and Intersectoral Collaboration for Promoting Active Mobility for Healthy Aging—A Qualitative Study within Local Government in Germany. International Journal of Environmental Research and Public Health, 18(7), 3807. https://doi.org/10.3390/ijerph18073807






