Load Transference with the Gain of Excessive Body Mass: A Two-Year Longitudinal Study
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Equipment and Procedure
2.3. Data Processing and Statistical Analysis
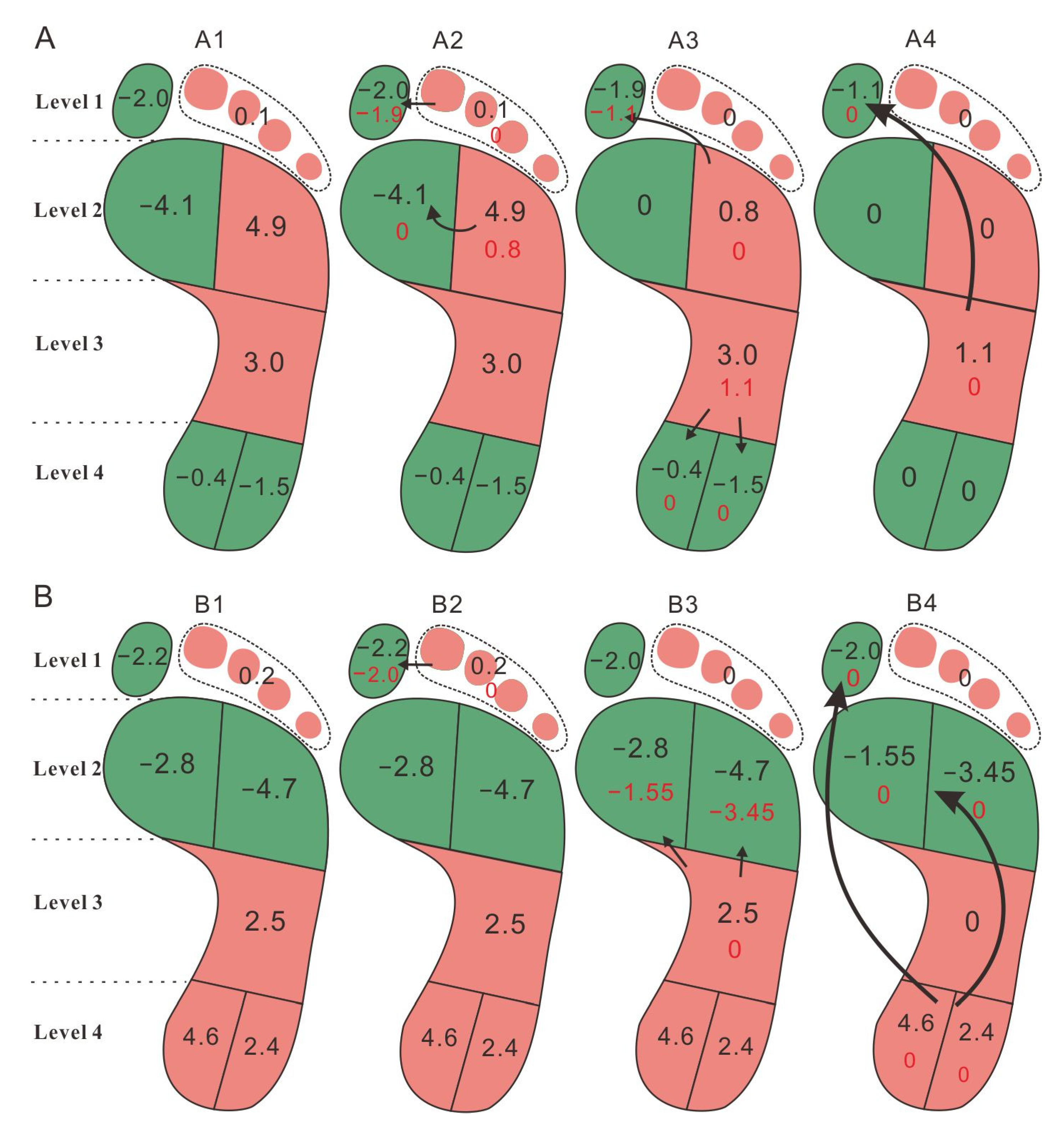
2.4. Load Transfer Method
3. Results
3.1. Participant Characteristics
3.2. Arch Index
3.3. FTI
3.4. Load Transfer
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Steinberg, N.; Nemet, D.; Pantanowitz, M.; Eliakim, A. Gait Pattern, Impact to the skeleton and postural balance in overweight and obese children: A review. Sports 2018, 6, 75. [Google Scholar] [CrossRef]
- Mignardot, J.-B.; Olivier, I.; Promayon, E.; Nougier, V. Obesity impact on the attentional cost for controlling posture. PLoS ONE 2010, 5, 12. [Google Scholar] [CrossRef]
- Anandacoomarasamy, A.; Caterson, I.; Sambrook, P.; Fransen, M.; March, L. The impact of obesity on the musculoskeletal system. Int. J. Obes. 2008, 32, 211–222. [Google Scholar] [CrossRef] [PubMed]
- Gil Madrona, P.; Romero Martinez, S.J.; Saez-Gallego, N.M.; Ordonez Camacho, X.G. Psychomotor limitations of overweight and obese five-year-old children: Influence of body mass indices on motor, perceptual, and social-emotional skills. Int. J. Environ. Res. Public Health 2019, 16, 427. [Google Scholar] [CrossRef] [PubMed]
- Mesquita, P.R.; Neri SG, R.; Lima, R.M.; Carpes, F.P.; de David, A.C. Childhood obesity is associated with altered plantar pressure distribution during running. Gait Posture 2018, 62, 202–205. [Google Scholar] [CrossRef] [PubMed]
- Song-Hua, Y.; Lu, W.; Kuan, Z. Effects of different movement modes on plantar pressure distribution patterns in obese and non-obese Chinese children. Gait Posture 2017, 57, 28–34. [Google Scholar] [CrossRef] [PubMed]
- Steele, J.R.; Riddiford-Harland, D.L.; Mickle, K.J. Excessive weight bearing compromises foot structure and function across the lifespan. Mechanobiol. Obes. Relat. Dis. 2015, 16, 149–179. [Google Scholar]
- Wyszynska, J.; Leszczak, J.; Podgorska-Bednarz, J.; Czenczek-Lewandowska, E.; Rachwal, M.; Deren, K.; Baran, J.; Drzal-Grabiec, J. Body fat and muscle mass in association with foot structure in adolescents: A cross-sectional study. Int. J. Environ. Res. Public Health 2020, 17, 811. [Google Scholar] [CrossRef]
- Da Rocha, E.S.; Bratz, D.T.; Gubert, L.C.; de David, A.; Carpes, F.P. Obese children experience higher plantar pressure and lower foot sensitivity than non-obese. Clin. Biomech. 2014, 29, 822–827. [Google Scholar] [CrossRef]
- Yan, S.H.; Zhang, K.; Tan, G.Q.; Yang, J.; Liu, Z.C. Effects of obesity on dynamic plantar pressure distribution in Chinese prepubescent children during walking. Gait Posture 2013, 37, 37–42. [Google Scholar] [CrossRef]
- Gijon-Nogueron, G.; Montes-Alguacil, J.; Martinez-Nova, A.; Alfageme-Garcia, P.; Cervera-Marin, J.A.; Morales-Asencio, J.M. Overweight, obesity and foot posture in children: A cross-sectional study. J. Paediatr. Child Health 2017, 53, 33–37. [Google Scholar] [CrossRef] [PubMed]
- Catan, L.; Amaricai, E.; Onofrei, R.R.; Popoiu, C.M.; Iacob, E.R.; Stanciulescu, C.M.; Cerbu, S.; Horhat, D.I.; Suciu, O. The impact of overweight and obesity on plantar pressure in children and adolescents: A systematic review. Int. J. Environ. Res. Public Health 2020, 17, 6600. [Google Scholar] [CrossRef]
- Forriol, F.; Pascual, J. Footprint analysis between 3 and 17 years of age. Foot Ankle 1990, 11, 101–104. [Google Scholar] [CrossRef] [PubMed]
- Volpon, J.B. Footprint analysis during the growth period. J. Pediatric Orthop. 1994, 14, 83–85. [Google Scholar] [CrossRef] [PubMed]
- Bus, S.A.; Ulbrecht, J.S.; Cavanagh, P.R. Pressure relief and load redistribution by custom-made insoles in diabetic patients with neuropathy and foot deformity. Clin. Biomech. 2004, 19, 629–638. [Google Scholar] [CrossRef]
- Bus, S.A.; van Deursen, R.W.; Kanade, R.V.; Wissink, M.; Manning, E.A.; van Baal, J.G.; Harding, K.G. Plantar pressure relief in the diabetic foot using forefoot offloading shoes. Gait Posture 2009, 29, 618–622. [Google Scholar] [CrossRef]
- Bus, S.A.; Waaijman, R.; Arts, M.; Manning, H. The efficacy of a removable vacuum-cushioned cast replacement system in reducing plantar forefoot pressures in diabetic patients. Clin. Biomech. 2009, 24, 459–464. [Google Scholar] [CrossRef]
- Zhao, Y.; Zheng, D.; Yan, S.; Liu, M.; Yang, L. Children with obesity experience different age-related changes in plantar pressure distributions: A follow-up study in china. Int. J. Environ. Res. Public Health 2020, 17, 6602. [Google Scholar] [CrossRef]
- Hu, M.; Zhou, N.; Xu, B.; Chen, W.; Wu, J.; Zhou, J. The mechanism of force transference in feet of children ages two to six. Gait Posture 2017, 54, 15–19. [Google Scholar] [CrossRef] [PubMed]
- Group of China Obesity Task Force. Body mass index reference norm for screening overweight and obesity in Chinese children and adolescents. Chin. J. Epidemiol. 2004, 25, 97–102. [Google Scholar]
- Meyersrice, B.; Sugars, L.; McPoil, T.; Cornwall, M.W. Comparison of 3 methods for obtaining plantar pressures in nonpathologic subjects. J. Am. Podiatr. Med Assoc. 1994, 84, 499–504. [Google Scholar] [CrossRef]
- Menz, H.B. Two feet, or one person? Problems associated with statistical analysis of paired data in foot and ankle medicine. Foot 2004, 14, 2–5. [Google Scholar] [CrossRef]
- Gerych, D.; Tvrznik, A.; Prokesova EV, A.; Nemeckova, Z.; Jelen, K. Analysis of Peak Pressure, Maximal Force, And Contact Area Changes during Walking and Running with Conventional and Shock-Absorbing Insoles In the Combat Boots Of the Czech Army. J. Mech. Med. Biol. 2013, 13, 1350042. [Google Scholar] [CrossRef]
- Cavanagh, P.R.; Rodgers, M.M. The arch index—A useful measure from footprints. J. Biomech. 1987, 20, 547–551. [Google Scholar] [CrossRef]
- Bosch, K.; Gerss, J.; Rosenbaum, D. Development of healthy children’s feet--nine-year results of a longitudinal investigation of plantar loading patterns. Gait Posture 2010, 32, 564–571. [Google Scholar] [CrossRef]
- Martínez-Nova, A.; Gijón-Noguerón, G.; Alfageme-García, P.; Montes-Alguacil, J.; Evans, A.M. Foot posture development in children aged 5 to11 years: A three-year prospective study. Gait Posture 2018, 62, 280–284. [Google Scholar] [CrossRef] [PubMed]
- Ker, R.F.; Bennett, M.B.; Bibby, S.R.; Kester, R.C.; Alexander, R.M. The spring in the arch of the human foot. Nature 1987, 325, 147–149. [Google Scholar] [CrossRef]
- Riddiford-Harland, D.L.; Steele, J.R.; Baur, L.A. Are the feet of obese children fat or flat? Revisiting the debate. Int. J. Obes. 2011, 35, 115–120. [Google Scholar] [CrossRef] [PubMed]
- Dowling, A.M.; Steele, J.R.; Baur, L.A. Does obesity influence foot structure and plantar pressure patterns in prepubescent children? Int. J. Obes. 2001, 25, 845–852. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Ormeno, E.; Aguado, X.; Delgado-Abellan, L.; Mecerreyes, L.; Alegre, L.M. Foot morphology in normal-weight, overweight, and obese schoolchildren. Eur. J. Pediatrics 2013, 172, 645–652. [Google Scholar] [CrossRef] [PubMed]
- Hills, A.P.; Hennig, E.M.; Byrne, N.M.; Steele, J.R. The biomechanics of adiposity—Structural and functional limitations of obesity and implications for movement. Obes. Rev. Off. J. Int. Assoc. Study Obes. 2002, 3, 35–43. [Google Scholar] [CrossRef] [PubMed]
| Age | Male | Female | ||
|---|---|---|---|---|
| Overweight | Obese | Overweight | Obese | |
| 7 | 17.4 | 19.2 | 17.2 | 18.9 |
| 8 | 18.1 | 20.3 | 18.1 | 19.9 |
| 9 | 18.9 | 21.4 | 19.0 | 21.0 |
| 10 | 19.6 | 22.5 | 20.0 | 22.1 |
| 11 | 20.3 | 23.6 | 21.1 | 23.3 |
| Group | Baseline | Follow-Up | Mean Difference (95% CI) | p | |
|---|---|---|---|---|---|
| Number | Group 0 | 15 | 15 | - | - |
| Group 1 | 15 | 15 | - | - | |
| Age (years) | Group 0 | 7.7 ± 0.5 | 9.7 ± 0.5 | 2 | - |
| Group 1 | 7.7 ± 0.5 | 9.7 ± 0.5 | 2 | - | |
| Height (cm) | Group 0 | 130.3 ± 4.1 | 141.2 ± 4.8 | 11.0 (9.9 to 12.0) | 0.000 |
| Group 1 | 129.9 ± 4.3 | 141.1 ± 4.7 | 11.3 (10.3 to 12.2) | 0.000 | |
| Weight (kg) | Group 0 | 25.4 ± 2.6 | 33.3 ± 4.9 | 7.8 (6.5 to 9.2) | 0.000 |
| Group 1 | 28.0 ± 2.3 | 40.4 ± 3.8 | 12.4 (11.0 to 13.8) | 0.000 | |
| BMI (kg·m−2) | Group 0 | 15.0 ± 1.3 | 16.6 ± 2.0 | 1.7 (1.2 to 2.2) | 0.011 |
| Group 1 | 16.6 ± 0.8 | 20.3 ± 0.9 | 3.6 (3.1 to 4.2) | 0.000 | |
| AI | Group 0 | 0.27 ± 0.07 | 0.16 ± 0.07 | −0.11 (−0.08 to −0.13) | 0.000 |
| Group 1 | 0.27 ± 0.06 | 0.19 ± 0.06 | −0.08 (−0.06 to −0.10) | 0.002 |
| Regions | Group 0 | Group 1 | ||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | Follow up | Mean Difference (95% CI) | p | Baseline | Follow up | Mean Difference (95% CI) | p | |
| BT | 6.7 ± 3.0 | 16.2 ± 8.9 | 9.5 (5.0 to 14.0) | 0.001 | 6.0 ± 4.6 | 16.9 ± 10.4 | 10.9 (6.4 to 15.5) | 0.001 |
| T2–5 | 2.2 ± 1.7 | 3.3 ± 2.1 | 1.0 (-0.4 to 2.5) | 0.163 | 1.8 ± 1.5 | 3.4 ± 3.1 | 1.6 (−0.2 to 3.4) | 0.082 |
| MM | 27.4 ± 9.2 | 60.0 ± 22.0 | 34.4 (21.6 to 47.2) | 0.000 | 24.4 ± 15.4 | 55.2 ± 25.2 | 30.8 (14.9 to 46.6) | 0.000 |
| LM | 25.2 ± 19.6 | 31.4 ± 18.0 | 6.2 (−4.4 to 16.8) | 0.379 | 17.9 ± 10.6 | 44.7 ± 23.0 | 26.8 (14.2 to 39.3) | 0.001 |
| MF | 13.7 ± 13.3 | 15.9 ± 13.6 | 2.2 (−1.9 to 6.3) | 0.663 | 17.3 ± 15.7 | 23.4 ± 16.9 | 7.3 (−3.0 to 17.6) | 0.320 |
| HM | 17.0 ± 8.7 | 30.6 ± 13.1 | 13.6 (4.9 to 22.2) | 0.003 | 23.1 ± 18.3 | 33.1 ± 14.5 | 9.9 (−1.0 to 20.9) | 0.110 |
| HL | 14.0 ± 6.9 | 28.1 ± 13.4 | 14.0 (6.4 to 21.6) | 0.002 | 19.0 ± 11.1 | 31.0 ± 12.3 | 12.0 (4.1 to 19.9) | 0.009 |
| Regions | Group 0 | Group 1 | ||||
|---|---|---|---|---|---|---|
| Baseline | Follow up | Transfer Value | Baseline | Follow up | Transfer Value | |
| BT | 6.6 | 8.6 | −2.0 | 6.2 | 8.4 | −2.2 |
| T2–5 | 1.9 | 1.8 | 0.1 | 1.9 | 1.7 | 0.2 |
| MM | 29.1 | 33.2 | −4.1 | 24.0 | 26.8 | −2.8 |
| LM | 21.6 | 16.7 | 4.9 | 16.5 | 21.2 | −4.7 |
| MF | 11.0 | 8.0 | 3.0 | 13.3 | 10.8 | 2.5 |
| HM | 16.1 | 16.5 | −0.4 | 20.4 | 15.8 | 4.6 |
| HL | 13.6 | 15.1 | −1.5 | 17.6 | 15.2 | 2.4 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, R.; Liu, Q.; Chen, X.; Yan, S.; Zhao, Y.; Zhang, L.; Badurova, J.; Yang, L.; Fan, H. Load Transference with the Gain of Excessive Body Mass: A Two-Year Longitudinal Study. Int. J. Environ. Res. Public Health 2021, 18, 2879. https://doi.org/10.3390/ijerph18062879
Li R, Liu Q, Chen X, Yan S, Zhao Y, Zhang L, Badurova J, Yang L, Fan H. Load Transference with the Gain of Excessive Body Mass: A Two-Year Longitudinal Study. International Journal of Environmental Research and Public Health. 2021; 18(6):2879. https://doi.org/10.3390/ijerph18062879
Chicago/Turabian StyleLi, Ruoyi, Qingyun Liu, Xuecan Chen, Shiyang Yan, Yihong Zhao, Linshan Zhang, Jitka Badurova, Luming Yang, and Haojun Fan. 2021. "Load Transference with the Gain of Excessive Body Mass: A Two-Year Longitudinal Study" International Journal of Environmental Research and Public Health 18, no. 6: 2879. https://doi.org/10.3390/ijerph18062879
APA StyleLi, R., Liu, Q., Chen, X., Yan, S., Zhao, Y., Zhang, L., Badurova, J., Yang, L., & Fan, H. (2021). Load Transference with the Gain of Excessive Body Mass: A Two-Year Longitudinal Study. International Journal of Environmental Research and Public Health, 18(6), 2879. https://doi.org/10.3390/ijerph18062879









