Epidemiological Study on Burnout in Spanish Dentists: Underlying Psychological Factors
Abstract
1. Introduction
2. Materials and Methods
3. Results
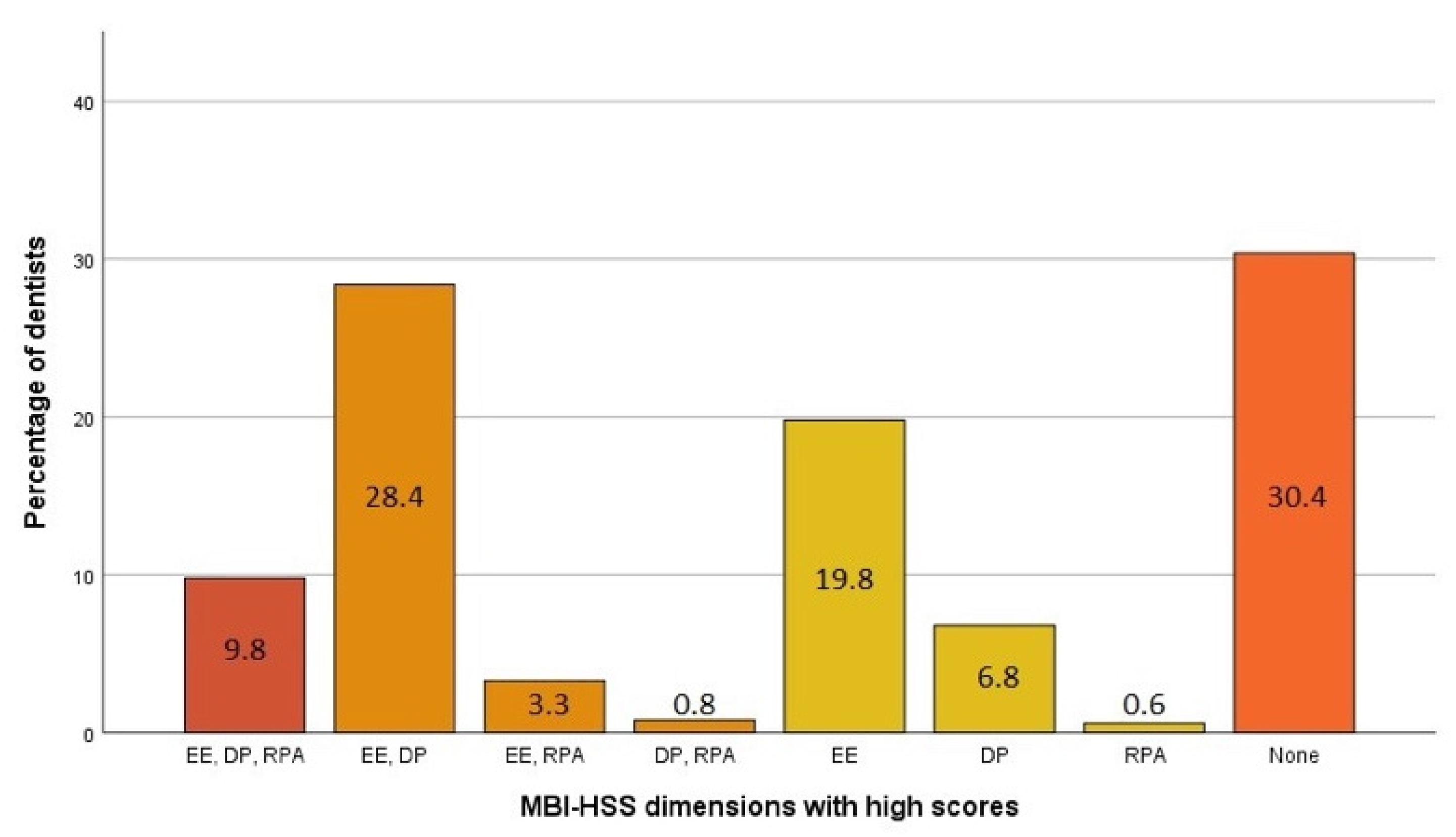
3.1. Prevalence of Burnout, Descriptive Analysis, and Typology of Dentists According to Their Degree of Burnout
3.2. Personality Differences between Groups
- Neuroticism (p < 0.001), with a large effect size (d = 1.00) [48]. Mean scores differed from each other, with the burnout group being the highest, with high burnout scores in at least one of the three dimensions.
- Extraversion (p < 0.001), with a medium effect size (d = − 0.64) [48]. The highest mean score corresponded to the members of the group without burnout who presented no signs of burnout.
- Agreeableness (p < 0.001), with a medium effect size (d = − 0.54) [48]. The highest mean score in this dimension again corresponded to the members of the group without burnout.
- Conscientiousness (p < 0.001), with a small effect size (d = − 0.31) [48]. The highest mean score was that of the members of the group without burnout.
3.3. Differences in Coping Strategies between the Groups
- Problem-focused coping, with a small effect size (d = −0.18) [48]. The mean score was higher for members of the group without burnout.
- Emotion-focused coping, with a small effect size (d = −0.19) [48]. This was the same as in the previous dimension: the highest mean score was that of the members of the group without burnout.
- Avoidant coping (p < 0.001), with a medium effect size (d = 0.54) [48]. In this case, the highest mean score was that of the members of the group with burnout.
3.4. Correlation Coefficients between the Five Personality Dimensions (NEO FFI), the Three Coping Styles (Brief COPE-28) and Age, and the Three Dimensions of Burnout Syndrome (MBI-HSS)
3.5. Logistic Regression Model for Estimating Burnout
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Maslach, C. Burnout. Hum. Behav. 1976, 9, 16–22. [Google Scholar]
- Rotenstein, L.S.; Torre, M.; Ramos, M.A.; Rosales, R.C.; Guille, C.; Sen, S.; Mata, D.A. Prevalence of Burnout Among Physicians: A Systematic Review. JAMA 2018, 320, 1131–1150. [Google Scholar] [CrossRef] [PubMed]
- Yates, S.W. Physician Stress and Burnout. Am. J. Med. 2020, 133, 160–164. [Google Scholar] [CrossRef] [PubMed]
- Cherniss, C. Staff Burnout: Job Stress in the Human Services; Sage Publications: Beverly Hills, CA, USA, 1980. [Google Scholar]
- Von Onciul, J. ABC of Work Related Disorders: Stress at Work. BMJ 1996, 313, 745–748. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Huri, M.; Bağiş, N.; Eren, H.; Başibüyük, O.; Şahin, S.; Umaroğlu, M.; Orhan, K. Burnout and occupational participation among dentists with teaching responsibilities in universities. Psychol. Health Med. 2017, 22, 693–700. [Google Scholar] [CrossRef] [PubMed]
- Marian, M.; Borza, A.; Filimon, L.; Marginean, I. Psychosocial determinants of burnout syndrome: Metaanalitic study. JPER 2011, 19, 78–93. [Google Scholar]
- Bakker, A.B.; Demerouti, E. Job demands-resources theory. In Work and Wellbeing: A Complete Reference Guide; Chen, P.Y., Cooper, C.L., Eds.; John Wiley & Sons: New York, NY, USA, 2014; pp. 1–28. [Google Scholar] [CrossRef]
- Zarei, E.; Khakzad, N.; Reniers, G.; Akbari, R. On the relationship between safety climate and occupational burnout in healthcare organizations. Saf. Sci. 2016, 89, 1–10. [Google Scholar] [CrossRef]
- Maslach, C. Finding solutions to the problem of burnout. Consult. Psychol. J. Prac. Res. 2017, 69, 143–152. [Google Scholar] [CrossRef]
- West, C.P.; Dyrbye, L.N.; Shanafelt, T.D. Physician burnout: Contributors, consequences and solutions. J. Intern. Med. 2018, 283, 516–529. [Google Scholar] [CrossRef] [PubMed]
- Lacy, B.E.; Chan, J.L. Physician Burnout: The Hidden Health Care Crisis. Clin. Gastroenterol. Hepatol. 2018, 16, 311–317. [Google Scholar] [CrossRef]
- Gorter, R.C. Burnout among dentists: A question of coping. Ned. Tijdschr. Tandheelkd. 2001, 108, 458–461. [Google Scholar] [PubMed]
- Song, K.-W.; Choi, W.-S.; Jee, H.-J.; Yuh, C.-S.; Kim, Y.-K.; Kim, L.; Lee, H.-J.; Cho, C.-H. Correlation of occupational stress with depression, anxiety, and sleep in Korean dentists: Cross-sectional study. BMC Psychiatry 2017, 17, 398. [Google Scholar] [CrossRef] [PubMed]
- Hakanen, J.J.; Bakker, A.; Demerouti, E. How dentists cope with their job demands and stay engaged: The moderating role of job resources. Eur. J. Oral Sci. 2005, 113, 479–487. [Google Scholar] [CrossRef] [PubMed]
- Te Brake, H.; Bloemendal, E.; Hoogstraten, J. Gender differences in burnout among Dutch dentists. Community Dent. Oral Epidemiol. 2003, 31, 321–327. [Google Scholar] [CrossRef] [PubMed]
- Rios-Santos, J.V.; Reyes-Torres, M.; Lopez-Jimenez, A.; Morillo-Velazquez, J.M.; Bullon, P. Burnout and depression among Spanish periodontology practitioners. Med. Oral Patol. Oral Cir. Bucal. 2010, 15, e813–e819. [Google Scholar] [CrossRef][Green Version]
- Gorter, R.C.; Freeman, R. Burnout and engagement in relation with job demands and resources among dental staff in Northern Ireland. Community Dent. Oral Epidemiol. 2011, 39, 87–95. [Google Scholar] [CrossRef]
- Molina-Hernández, J.; Fernández-Estevan, L.; Montero, J.; González-García, L. Work environment, job satisfaction and burnout among Spanish dentists: A cross-sectional study. BMC Oral Health 2021, 21, 156. [Google Scholar] [CrossRef]
- Puriene, A.; Aleksejuniene, J.; Petrauskiene, J.; Balciuniene, I.; Janulyte, V. Self-perceived mental health and job satisfaction among Lithuanian dentists. Ind. Health 2008, 46, 247–252. [Google Scholar] [CrossRef] [PubMed]
- Denton, D.A.; Newton, J.T.; Bower, E.J. Occupational burnout and work engagement: A national survey of dentists in the United Kingdom. Br. Dent. J. 2008, 205, E13. [Google Scholar] [CrossRef]
- Singh, P.; Aulak, D.S.; Mangat, S.S. Systematic review: Factors contributing to burnout in dentistry. Occup. Med. 2015, 66, 27–31. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W.B.; Bakker, A.B. Job demands, job resources, and their relationship with burnout and engagement: A multi-sample study. J. Organ. Behav. 2004, 25, 293–315. [Google Scholar] [CrossRef]
- Pulcrano, M.; Evans, S.R.T.; Sosin, M. Quality of Life and Burnout Rates Across Surgical Specialties: A Systematic Review. JAMA Surg. 2016, 151, 970–978. [Google Scholar] [CrossRef] [PubMed]
- Golonka, K.; Mojsa-Kaja, J.; Blukacz, M.; Gawłowska, M.; Marek, T. Occupational burnout and its overlapping effect with depression and anxiety. Int. J. Occup. Med. Environ. Health 2019, 32, 229–244. [Google Scholar] [CrossRef] [PubMed]
- Mojsa-Kaja, J.; Golonka, K.; Marek, T. Job burnout and engagement among teachers – Worklife areas and personality traits as predictors of relationships with work. Int. J. Occup. Med. Environ. Health 2015, 28, 102–119. [Google Scholar] [CrossRef]
- Pérez-Fuentes, M.D.C.; Jurado, M.D.M.M.; Linares, J.J.G.; Ruiz, N.F.O. The Role of Emotional Intelligence in Engagement in Nurses. Int. J. Environ. Res. Public Health 2018, 15, 1915. [Google Scholar] [CrossRef]
- Zaninotto, L.; Rossi, G.; Danieli, A.; Frasson, A.; Meneghetti, L.; Zordan, M.; Tito, P.; Salvetti, B.; Conca, A.; Ferranti, R.; et al. Exploring the relationships among personality traits, burnout dimensions and stigma in a sample of mental health professionals. Psychiatry Res. 2018, 264, 327–333. [Google Scholar] [CrossRef]
- Maslach, C.; Schaufeli, W.B.; Leiter, M.P. Job Burnout. Annu. Rev. Psychol. 2001, 52, 397–422. [Google Scholar] [CrossRef]
- Kim, H.J.; Shin, K.H.; Umbreit, W.T. Hotel job burnout: The role of personality characteristics. Int. J. Hosp. Manag. 2007, 26, 421–434. [Google Scholar] [CrossRef]
- Bakker, A.B.; Van Der Zee, K.I.; Lewig, K.A.; Dollard, M.F. The Relationship between the Big Five Personality Factors and Burnout: A Study Among Volunteer Counselors. J. Soc. Psychol. 2006, 146, 31–50. [Google Scholar] [CrossRef] [PubMed]
- Allport, G. Personality: A Psychological Interpretation; Henry Holt and Company: New York, NY, USA, 1937. [Google Scholar]
- Costa, P.T.; McCrae, R.R. Personality in Adulthood. A Five-Factor Theory Perspective; Guilford Press: New York, NY, USA, 1990. [Google Scholar]
- Funder, D.C. Personality. Annu. Rev. Psychol. 2001, 52, 197–221. [Google Scholar] [CrossRef] [PubMed]
- John, O.; Srivastava, S. Handbook of Personality: Theory and Research: The Big Five Trait Taxonomy: History, Measurement, and Theoretical Perspectives; Guilford Press: New York, NY, USA, 1999. [Google Scholar]
- Widiger, T.A. Five factor model of personality disorder: Integrating science and practice. J. Res. Pers. 2005, 39, 67–83. [Google Scholar] [CrossRef]
- Lazarus, R.; Folkman, S. Coping Modes Scale. Stress, evaluation and coping. J. Health Soc. Behav. 1984, 45, 150–170. [Google Scholar]
- Costa, P.; McCrae, R. The Revised NEO Personality Inventory (NEO-PI-R) and NEO-Five-Factor Inventory (NEO-FFI) Professional Manual; Psychological Assessment Resources: Odessa, Ukraine, 1992. [Google Scholar]
- Cordero, A.; Pamos, A.; Seisdedos, N. Inventario de Personalidad Neo Revisado (NEO-PI-R). Inventario Neo Reducido de Cinco Factores (NEO-FFI); TEA Ediciones: Madrid, Spain, 1999. [Google Scholar]
- Carver, C.S. You want to measure coping but your protocol’s too long: Consider the Brief COPE. Int. J. Behav. Med. 1997, 4, 92–100. [Google Scholar] [CrossRef]
- Crespo, M.; Cruzado, J.A. La evaluación del afrontamiento: Adaptación española del cuestionario COPE con una muestra de estudiantes universitarios. Anál. Modif. Conducta 1997, 23, 797–830. [Google Scholar] [CrossRef][Green Version]
- Perczek, R.; Carver, C.S.; Price, A.A.; Pozo-Kaderman, C. Coping, Mood, and Aspects of Personality in Spanish Translation and Evidence of Convergence with English Versions. J. Pers. Assess. 2000, 74, 63–87. [Google Scholar] [CrossRef] [PubMed]
- Carver, C.S.; Scheier, M.F.; Weintraub, J.K. Assessing coping strategies: A theoretically based approach. J. Pers. Soc. Psychol. 1989, 56, 267–283. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S.E. Maslach Burnout Inventory-Human Services Survey (MBI-HSS); Consulting Psychologist Press: Palo Alto, CA, USA, 1996. [Google Scholar]
- Seisdedos, N. MBI Inventario “Burnout” de Maslach; TEA Ediciones: Madrid, Spain, 1997. [Google Scholar]
- Maslach, C.; Jackson, S.E. The measurement of experienced burnout. J. Organ. Behav. 1981, 2, 99–113. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S. Maslasch Burnout Inventory Manual; Consulting Psychologist Press: Palo Alto, CA, USA, 1986. [Google Scholar]
- Andrade, C. Understanding Relative Risk, Odds Ratio, and Related Terms: As Simple as It Can Get. J. Clin. Psychiatry 2015, 76, e857–e861. [Google Scholar] [CrossRef]
- Sawilowsky, S.S. New Effect Size Rules of Thumb. J. Mod. Appl. Stat. Methods 2009, 8, 597–599. [Google Scholar] [CrossRef]
- Hosmer, D.W.; Lemeshow, S. Applied Logistic Regression; Wiley-Interscience: Hoboken, NJ, USA, 2000. [Google Scholar]
- Molavynejad, S.; Babazadeh, M.; Bereihi, F.; Cheraghian, B. Relationship between personality traits and burnout in oncology nurses. J. Fam. Med. Prim. Care 2019, 8, 2898–2902. [Google Scholar] [CrossRef]
- Chen, H.; Cohen, P.; Chen, S. How Big is a Big Odds Ratio? Interpreting the Magnitudes of Odds Ratios in Epidemiological Studies. Commun. Stat.-Simul. Comput. 2010, 39, 860–864. [Google Scholar] [CrossRef]
- Cordes, C.L.; Dougherty, T.W. A Review and an Integration of Research on Job Burnout. Acad. Manag. Rev. 1993, 18, 621–656. [Google Scholar] [CrossRef]
- Swider, B.W.; Zimmerman, R.D. Born to burnout: A meta-analytic path model of personality, job burnout, and work outcomes. J. Vocat. Behav. 2010, 76, 487–506. [Google Scholar] [CrossRef]
- Fornés-Vives, J.; Frias-Navarro, D.; García-Banda, G.; Pascual-Soler, M. The Role of Neuroticism in Predicting Psychological Harassment in Nursing: A Longitudinal Study. Int. J. Environ. Res. Public Health 2019, 16, 889. [Google Scholar] [CrossRef] [PubMed]
- Burisch, M. A longitudinal study of burnout: The relative importance of dispositions and experiences. Work. Stress 2002, 16, 1–17. [Google Scholar] [CrossRef]
- Hudek-Knežević, J.; Kalebić, B.; Krapić, N. Personality organizational stress and attitudes toward work as prospective predictors of professional burnout in hospital nurses. Croat. Med. J. 2011, 52, 538–549. [Google Scholar] [CrossRef] [PubMed]
- Seltzer, J.; Numerof, R.E. Supervisory Leadership and Subordinate Burnout. Acad. Manag. J. 1988, 31, 439–446. [Google Scholar]
- Ahola, K.; Honkonen, T.; Isometsä, E.; Kalimo, R.; Nykyri, E.; Koskinen, S.; Aromaa, A.; Lönnqvist, J. Burnout in the general population. Results from the Finnish Health 2000 Study. Soc. Psychiatry Psychiatr. Epidemiol. 2006, 41, 11–17. [Google Scholar] [CrossRef]
- Maslach, C.; Leiter, M.P.; Schaufeli, W. Measuring Burnout. In The Oxford handbook of Organizational Well-Being; Cooper, C.L., Cartwright, S., Eds.; Oxford University Press: New York, NY, USA, 2009; pp. 86–108. [Google Scholar]
- Losa Iglesias, M.E.; Becerro de Bengoa Vallejo, R.; Salvadores Fuentes, P. The relationship between experiential avoidance and burnout syndrome in critical care nurses: A cross-sectional questionnaire survey. Int. J. Nurs. Stud. 2010, 47, 30–37. [Google Scholar] [CrossRef] [PubMed]
- Hamama, L. Differences between children’s social workers and adult’s social workers on sense of Burnout, work conditions and organisational social support. Br. J. Soc. Work 2012, 42, 1333–1353. [Google Scholar] [CrossRef]
- Rada, R.E.; Johnson-Leong, C. Stress, burnout, anxiety and depression among dentists. J. Am. Dent. Assoc. 2004, 135, 788–794. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W.B.; Enzmann, D. The Burnout Companion to Study and Practice: A Critical Analysis; Taylor & Francis: London, UK, 1998. [Google Scholar]
- Bui, J.; Hodge, A.; Shackelford, A.; Acsell, J. Factors contributing to burnout among perfusionists in the United States. Perfusion 2011, 26, 461–466. [Google Scholar] [CrossRef] [PubMed]
- Jefferson, L.; Bloor, K.; Maynard, A. Women in medicine: Historical perspectives and recent trends. Br. Med Bull. 2015, 114, 5–15. [Google Scholar] [CrossRef] [PubMed]
- Purvanova, R.K.; Muros, J.P. Gender differences in burnout: A meta-analysis. J. Vocat. Behav. 2010, 77, 168–185. [Google Scholar] [CrossRef]
- Iwanicki, E.; Schwab, L. Who are our burned out teachers? Educ. Res. Q. 1982, 7, 5–16. [Google Scholar]
- Gómez-Baya, D.; Lucia-Casademunt, A.M.; Salinas-Pérez, J.A. Gender Differences in Psychological Well-Being and Health Problems among European Health Professionals: Analysis of Psychological Basic Needs and Job Satisfaction. Int. J. Environ. Res. Public Health 2018, 15, 1474. [Google Scholar] [CrossRef]
- Piedmont, R.L. A Longitudinal Analysis of Burnout in the Health Care Setting: The Role of Personal Dispositions. J. Pers. Assess. 1993, 61, 457–473. [Google Scholar] [CrossRef]
- Hochwälder, J. Burnout among Torgersen’s eight personality types. Soc. Behav. Pers. Int. J. 2009, 37, 467–480. [Google Scholar] [CrossRef]
- Divinakumar, K.J.; Bhat, P.S.; Prakash, J.; Srivastava, K. Personality traits and its correlation to burnout in female nurses. Ind. Psychiatry J. 2019, 28, 24–28. [Google Scholar] [CrossRef]
- Prins, D.J.; Van Vendeloo, S.N.; Brand, P.L.P.; Van Der Velpen, I.; de Jong, K.; van den Heijkant, F.; Van Der Heijden, F.M.M.A.; Prins, J.T. The relationship between burnout, personality traits, and medical specialty. A national study among Dutch residents. Med. Teach. 2018, 41, 584–590. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W.B.; Buunk, B.P. Burnout: An Overview of 25 Years of Research and Theorizing. In The Handbook of Work and Health Psychology; Wiley: Hoboken, NJ, USA, 2003; Volume 2, pp. 282–424. [Google Scholar]
- Diestel, S.; Schmidt, K.-H. Direct and interaction effects among the dimensions of the Maslach Burnout Inventory: Results from two German longitudinal samples. Int. J. Stress Manag. 2010, 17, 159–180. [Google Scholar] [CrossRef]
- Rudman, A.; Gustavsom, J.P. Early career burnout among new graduate nurses: A prospective observational study of intra-individual change trajectories. Int. J. Nurs. Stud. 2011, 48, 292–306. [Google Scholar] [CrossRef] [PubMed]
- Taris, T.W.; Le Blanc, P.M.; Schaufeli, W.; Schreurs, P.J.G. Are there causal relationships between the dimensions of the Maslach Burnout Inventory? A review and two longitudinal tests. Work. Stress 2005, 19, 238–255. [Google Scholar] [CrossRef]
- Halbesleben, J.; Buckley, M.R. Burnout in Organizational Life. J. Manag. 2004, 30, 859–879. [Google Scholar] [CrossRef]
- Westman, M.; Hobfoll, S.E.; Chen, S.; Davidson, O.B.; Laski, S. Organizational stress through the lens of Conservation of Resources (COR) theory. In Exploring Interpersonal Dynamics; Perrewe, P.L., Ganster, D.C., Eds.; Emerald Group Publishing Limited: Location, 2004; pp. 167–220. [Google Scholar]
- Shirom, A. Job-related Burnout: A revision. In Handbook of Occupational Health Psychology; Quick, J.C., Tetrick, L.E., Eds.; American Psychological Association: Washington, DC, USA, 2003; pp. 245–265. [Google Scholar]
- Ben-Zur, H.; Michael, K. Burnout, Social Support, and Coping at Work Among Social Workers, Psychologists, and Nurses: The role of challenge/control appraisals. Soc. Work. Health Care 2007, 45, 63–82. [Google Scholar] [CrossRef] [PubMed]
- Shinan-Altman, S.; Werner, P.; Cohen, M. The connection between illness representations of Alzheimer’s disease and burnout among social workers and nurses in nursing homes and hospitals: A mixed-methods investigation. Aging Ment. Health 2016, 20, 352–361. [Google Scholar] [CrossRef]
- Anderson, D.G. Coping strategies and burnout among veteran child protection workers. Child Abus. Negl. 2000, 24, 839–848. [Google Scholar] [CrossRef]
- Burke, R.J.; Greenglass, E.R. Hospital Restructuring and Nursing Staff Well-Being: The Role of Coping. Int. J. Stress Manag. 2000, 7, 49–59. [Google Scholar] [CrossRef]
- Van Den Broeck, U.; D’Hooghe, T.; Enzlin, P.; Demyttenaere, K. Predictors of psychological distress in patients starting IVF treatment: Infertility-specific versus general psychological characteristics. Hum. Reprod. 2010, 25, 1471–1480. [Google Scholar] [CrossRef]
- Yansane, A.; Tokede, O.; Walji, M.; Obadan-Udoh, E.; Riedy, C.; White, J.; Kalenderian, E. Burnout, Engagement, and Dental Errors Among U.S. Dentists. J. Patient Saf. 2020, in press. [Google Scholar] [CrossRef]
- Roth, S.F.; Heo, G.; Varnhagen, C.; Glover, K.E.; Major, P.W. Job satisfaction among Canadian orthodontists. Am. J. Orthod. Dentofac. Orthop. 2003, 123, 695–700. [Google Scholar] [CrossRef]
- Günüşen, N.P.; Üstün, B. An RCT of coping and support groups to reduce burnout among nurses. Int. Nurs. Rev. 2010, 57, 485–492. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Rey, R.; Palacios, A.; Alonso-Tapia, J.; Pérez, E.; Álvarez, E.; Coca, A.; Mencía, S.; Marcos, A.; Mayordomo-Colunga, J.; Fernández, F.; et al. Burnout and posttraumatic stress in paediatric critical care personnel: Prediction from resilience and coping styles. Aust. Crit. Care 2019, 32, 46–53. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.-F.; Kuo, C.-C.; Chien, T.-W.; Wang, Y.-R. A Meta-Analysis of the Effects of Coping Strategies on Reducing Nurse Burnout. Appl. Nurs. Res. 2016, 31, 100–110. [Google Scholar] [CrossRef] [PubMed]
| Prevalence | Number of Dentists | Percentage (%) |
|---|---|---|
| No Burnout | 395 | 30.5% |
| Initial Burnout | 353 | 27.2%% |
| Moderate Burnout | 423 | 32.5% |
| Severe Burnout | 127 | 9.8% |
| Mean | SD | Minimum | Maximum | |
|---|---|---|---|---|
| Age | 41.8 | 11.5 | 22 | 74 |
| NEO FFI | ||||
| Neuroticism | 33.8 | 9.2 | 12 | 60 |
| Extraversion | 40.2 | 7.3 | 15 | 60 |
| Openness to experience | 40.1 | 6.8 | 20 | 60 |
| Agreeableness | 42.1 | 5.9 | 15 | 60 |
| Conscientiousness | 45.9 | 6.0 | 27 | 60 |
| COPE-28 | ||||
| Problem-focused coping | 70.9 | 10.4 | 25.0 | 100.0 |
| Emotion-focused coping | 56.2 | 8.9 | 25.0 | 87.5 |
| Avoidant coping | 48.8 | 7.5 | 25.0 | 77.1 |
| MBI-HSS | ||||
| Emotional exhaustion | 30.8 | 10.9 | 9 | 54 |
| Depersonalization | 10.3 | 4.7 | 5 | 28 |
| Reduced personal accomplishment | 39.8 | 5.9 | 8 | 48 |
| Dimension | Burnout (n = 903) Mean (SD) | No Burnout (n = 395) Mean (SD) | T Test | p | Cohen’s d (CI95%) |
|---|---|---|---|---|---|
| Neuroticism | 36.6 (8.6) | 27.5 (7.0) | 18.652 | <0.001 | 1.00 (0.89; 1.10) |
| Extraversion | 38.8 (7.4) | 43.5 (6.1) | −11.128 | <0.001 | −0.64 (−0.75; −0.53) |
| Openness to experience | 39.9 (7.0) | 40.4 (6.3) | −1.220 | 0.223 | −0.07 (−0.19; 0.04) |
| Agreeableness | 41.1 (5.9) | 44.3 (5.2) | −9.328 | <0.001 | −0.54 (−0.66; −0.43) |
| Conscientiousness | 45.3 (6.1) | 47.2 (5.8) | −5.242 | <0.001 | −0.31 (−0.43; −0.20) |
| Dimension | Burnout (n = 903) Mean (SD | No Burnout (n = 395) Mean (SD) | T Test | p | Cohen’s d (CI95%) |
|---|---|---|---|---|---|
| Problem-focused coping | 70.4 (10.7) | 72.2 (9.7) | 8.733 | 0.003 | −0.18 (−0.30; −0.06) |
| Emotion-focused coping | 55.7 (9.0) | 57.4 (8.6) | 9.826 | 0.002 | −0.19 (−0.31; −0.07) |
| Avoidant coping | 50.0 (7.7) | 45.9 (6.3) | 87.034 | <0.001 | 0.54 (0.43; 0.66) |
| Pearson’s Correlation Coefficients | |||
|---|---|---|---|
| Emotional Exhaustion | Depersonalization | Reduced Personal Accomplishment | |
| Age | −0.140 ** | −0.131 ** | 0.080 ** |
| NEO FFI | |||
| Neuroticism | 0.633 ** | 0.381 ** | −0.508 ** |
| Extraversion | −0.395 ** | −0.309 ** | 0.471 ** |
| Openness to experience | −0.038 | −0.043 | 0.190 ** |
| Agreeableness | −0.267 ** | −0.355 ** | 0.267 ** |
| Conscientiousness | −0.189 ** | −0.144 ** | 0.322 ** |
| COPE-28 | |||
| Problem-focused coping | −0.086 ** | −0.060 * | 0.309 ** |
| Emotion-focused coping | −0.085 ** | −0.053 | 0.281 ** |
| Avoidant coping | 0.340 ** | 0.327 ** | −0.146 ** |
| B | DE(B) | Wald | p | OR | CI 95% OR | |
|---|---|---|---|---|---|---|
| Neuroticism | 0.115 | 0.011 | 102.793 | <0.001 | 1.122 | 1.098–1.148 |
| Extraversion | −0.066 | 0.012 | 28.268 | <0.001 | 0.936 | 0.914–0.959 |
| Agreeableness | −0.047 | 0.014 | 11.744 | 0.001 | 0.954 | 0.928–0.980 |
| Avoidant coping | 0.043 | 0.011 | 14.808 | <0.001 | 1.044 | 1.022–1.068 |
| Conscientiousness | 0.035 | 0.013 | 6.580 | 0.010 | 1.035 | 1.008–1.063 |
| Age | −0.020 | 0.006 | 10.026 | 0.002 | 0.980 | 0.968–0.992 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gómez-Polo, C.; Martín Casado, A.M.; Castaño, A.; Montero, J. Epidemiological Study on Burnout in Spanish Dentists: Underlying Psychological Factors. Int. J. Environ. Res. Public Health 2021, 18, 13418. https://doi.org/10.3390/ijerph182413418
Gómez-Polo C, Martín Casado AM, Castaño A, Montero J. Epidemiological Study on Burnout in Spanish Dentists: Underlying Psychological Factors. International Journal of Environmental Research and Public Health. 2021; 18(24):13418. https://doi.org/10.3390/ijerph182413418
Chicago/Turabian StyleGómez-Polo, Cristina, Ana María Martín Casado, Antonio Castaño, and Javier Montero. 2021. "Epidemiological Study on Burnout in Spanish Dentists: Underlying Psychological Factors" International Journal of Environmental Research and Public Health 18, no. 24: 13418. https://doi.org/10.3390/ijerph182413418
APA StyleGómez-Polo, C., Martín Casado, A. M., Castaño, A., & Montero, J. (2021). Epidemiological Study on Burnout in Spanish Dentists: Underlying Psychological Factors. International Journal of Environmental Research and Public Health, 18(24), 13418. https://doi.org/10.3390/ijerph182413418







