Preventing Multimorbidity with Lifestyle Interventions in Sub-Saharan Africa: A New Challenge for Public Health in Low and Middle-Income Countries
Abstract
1. Background and Objectives
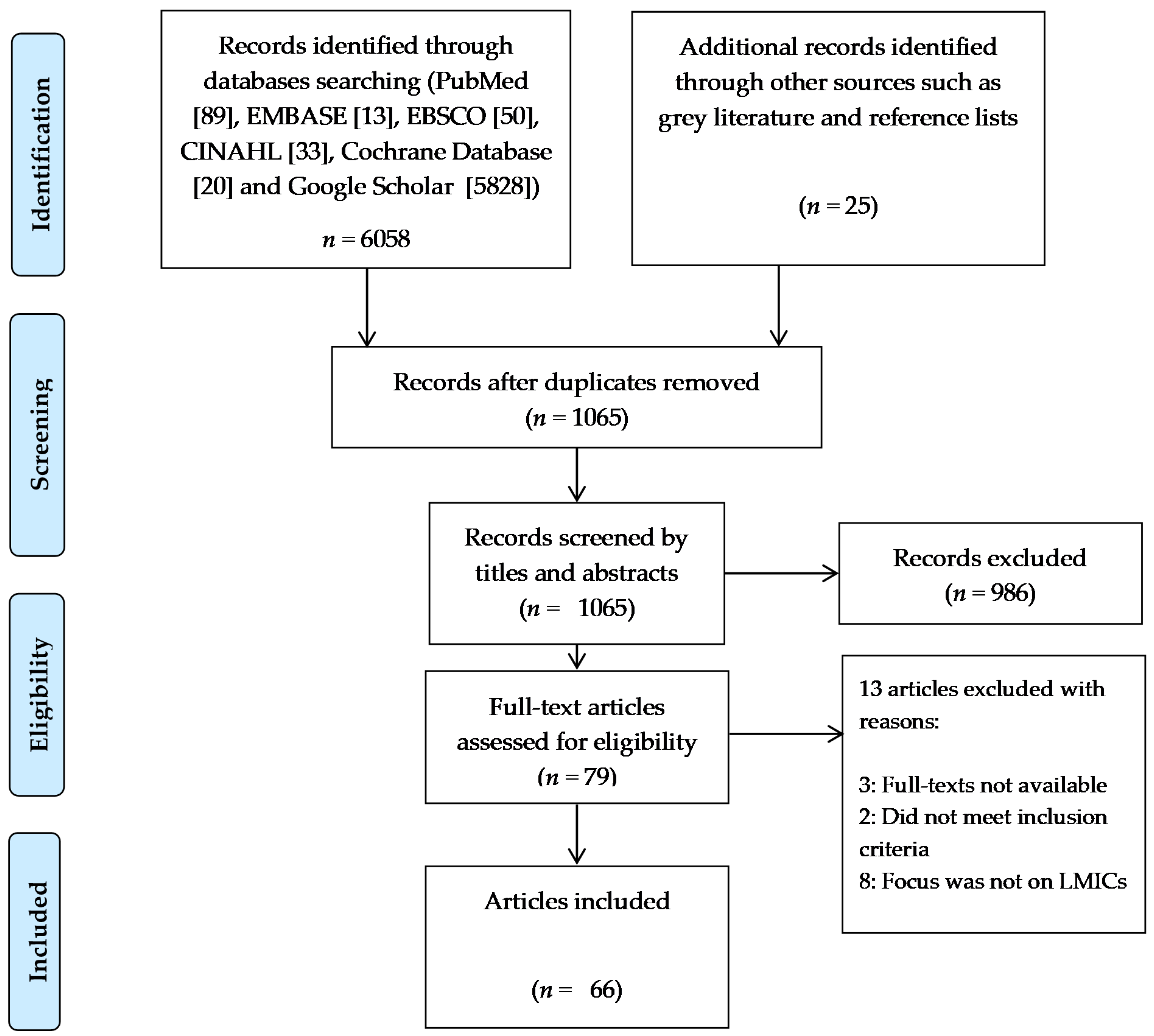
2. Methodology
3. Determinants of Multimorbidity and Its Increased Burden in LMICs
3.1. Age
3.2. Hypertension
3.3. Environmental Factors and Rural Living
3.3.1. Environmental Factors
3.3.2. Rural Living
3.4. Lifestyle Factors
| Study Type and Region | MM Prevalence | Chronic Conditions Included (Forming MM) | Determinants of MM |
|---|---|---|---|
| Cross-sectional survey among older adults, Bangladesh [26] | Overall MM prevalence (56.5%). | MM: Cumulative Illness Rating Scale (domains of disease, hypertension, ear-nose and throat, upper and lower GI, respiratory, cardiovascular, musculoskeleta) | Age: High prevalence in 60–69 y.o. (78.2% with two NCDs, 73.6% with three NCDs and 92.95 with four or more NCDs. Female sex: (prevalence of 64.2%). Hypertension: Higher MM among hypertensive (95.7%). |
| Systematic review of 70 community-based surveys, 31 LMICs and 18 HICs [28] | Pooled MM prevalence in LMICs (43.5%) | MM: 4 to 40 diseases with hypertension, diabetes, arthritis and stroke | Female sex: 21 studies showed higher MM prevalence in women than men (e.g., in South Africa 74% vs. 26%), 4 studies showing the reverse. Age: MM positively associate with age (e.g., 88.1% in women and 76.3% in men prevalence in > 85 y.o). |
| Nationwide WHO Stepwise survey for NCDs risk factors in Uganda [18,44] | Overall prevalence of Hypertension was 26.4%, was concurrent with obesity, and 2% impaired fasting glucose (1.2 diabetes). 56 · 4% had at least two risk factors (mainly high blood pressure and BMI) | MM: Hypertension, diabetes and obesity | Age: Hypertension was high among ≥ 50 y.o (PRR = 3.57). BMI: Hypertension prevalence was highest (PRR = 1.67) among obese (BMI ≥ 30 kg/m2). Rurality, Sex: Lower hypertension in rural than urban (25.8% vs. 28.2% N.S.). Higher hypertension in men vs. women (28.3% vs. 25.2% N.S.). |
| Review on global hypertension burden [32] | Higher overall prevalence of hypertension in LMICs (31.5%, 1.04 billion people) than in HICs (28.5%, 349 million people), and was concurrent with obesity | MM: Hypertension and obesity | Lifestyle factors: high sodium intake, low potassium intake, alcohol consumption, physical inactivity and unhealthy diet. Obesity: increases risk of hypertension. Socioeconomic status: increases risk of hypertension. |
| WHO STEPwise and GSHS surveys report in 33 countries in the WHO African Region [19] | 31 surveys indicated obesity median prevalence of 11% (ranged 2% in Madagascar to 25% in Seychelles). Hypertension median prevalence of 31% (17% to 40%). Diabetes indicated (fasting blood glucose ≥ 6.1 mmol/L), prevalence was 8% (3% in Togo and Benin to 23% in Niger). | MM: Obesity, hypertension, diabetes | Sex: Females are three times more likely to be obese than males (median prevalence of 15% and 5% respectively). Adult males are more likely to be hypertensive than adult females (median 29%). Lifestyle: Tobacco use, unhealthy diet, insufficient physical activity and the harmful use of alcohol associated with higher NCDs risk. |
| A cross-sectional analysis of Demographic and Health Surveys in 33 countries in Sub-Saharan Africa region [33] | Hypertension was highest in women in Lesotho (17.3%) and lowest in women in Burundi (1.0%). Anemia was most prevalent in Gabon (60.6%) and obesity was most prominent in Lesotho (19.9%), Gabon (18.9%) and Ghana (15.6%). | MM: Hypertension and Obesity. Anaemia was also prevelant concurrently with those MM | BMI: Associated with hypertension and anaemia. Lifestyle factors: Smoking, fruits, vegetables and alcohol, exercise were modifiable factors associated with hypertension. Non-modifiable factors (Age, residence, religion, education, wealth index, marital status, employment and number of children ever born) associated with hypertension and anaemia. |
| A population based survey in China and Korea [42] | 31% in China had MM, higher proportions in cities. 24% had MM in Korea | MM: Hypertension, diabetes, arthritis and stroke | Rurality: Associated with reduced risk of MM Socioeconomic status: disparity of MM in rural vs. urban China. |
| A cross-sectional survey in Southern (18,137 middle aged and elderly), China [46] | 20.8% had MM. Most common MM pair was hypertension and diabetes (4.6%). Hypertension was 27.9%. | MM: Hypertension, diabetes | Health-related Quality of Life: Physical, mental, emotional, and social functioning. |
| Cross-sectional (16,000 clinic visits), Kenya [41] | 12.7%and 9% (M and F) Bronchitis; 10.8% and 11.2% (M and F), acute respiratory infection; virosis 12.7% (both M and F). | MM: Acute respiratory infections, bronchitis, virosis | Environmental conditions: Air pollution reduction, drinking water provision, and waste management in slums can have an influence on health status. Air pollution: Cause and aggravating factor of respiratory diseases (chronic obstructive pulmonary disease, asthma, pharyngitis). |
4. Future Scope for Multimorbidity Prevention through Lifestyle Interventions in LMICs
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| BMI | Body Mass Index |
| CDs | Communicable Diseases |
| DHS | Demographic Health Survey |
| HIC, HICs | High Income Countries |
| LMIC, LMICs | Low and Middle Income Countries |
| MM | Multimorbidity |
| NCDs | Non-communicable Diseases |
| CVD | Cardiovascular disease |
References
- World Health Organisation. Non-Communicable Diseases Key Facts. Available online: https://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases (accessed on 7 July 2020).
- Gouda, H.N.; Charlson, F.; Sorsdahl, K.; Ahmadzada, S.; Ferrari, A.J.; Erskine, H.; Leung, J.; Santamauro, D.; Lund, C.; Aminde, L.N.; et al. Burden of non-communicable diseases in sub-Saharan Africa, 1990–2017: Results from the Global Burden of Disease Study 2017. Lancet Glob. Health 2019, 7, e1375–e1387. [Google Scholar] [CrossRef]
- Dalal, S.; Beunza, J.J.; Volmink, J.; Adebamowo, C.; Bajunirwe, F.; Njelekela, M.; Mozaffarian, D.; Fawzi, W.; Willett, W.; Adami, H.-O.; et al. Non-communicable diseases in sub-Saharan Africa: What we know now. Int. J. Epidemiol. 2011, 40, 885–901. [Google Scholar] [CrossRef]
- Naghavi, M.; Forouzanfar, M.H. Burden of non-communicable diseases in sub-Saharan Africa in 1990 and 2010: Global Burden of Diseases, Injuries, and Risk Factors Study 2010. Lancet 2013, 381, S95. [Google Scholar] [CrossRef]
- Murray, C.J.L.; Vos, T.; Lozano, R.; Naghavi, M.; Flaxman, A.D.; Michaud, C.; Ezzati, M.; Shibuya, K.; Salomon, J.A.; Abdalla, S.; et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2013, 380, 2197–2223. [Google Scholar] [CrossRef]
- Hall, V.; Thomsen, R.W.; Henriksen, O.; Lohse, N. Diabetes in Sub Saharan Africa 1999–2011: Epidemiology and public health implications. A systematic review. BMC Public Health 2011, 11, 564. [Google Scholar] [CrossRef]
- Rokas, N.; Vesna-Kerstin, P.; Andrea, F.; Martin, S. Multimorbidity: What do we know? What should we do? J. Comorbidity 2016, 6, 4–11. [Google Scholar]
- World Health Organisation. Multimorbidity: Technical Series on Safer Primary Care. Geneva: World Health Organization. Available online: https://apps.who.int/iris/bitstream/handle/10665/252275/9789241511650-eng.pdf?sequence=1 (accessed on 7 July 2020).
- Akker, M.V.D.; Buntinx, F.; Knottnerus, J.A. Comorbidity or multimorbidity. Eur. J. Gen. Pr. 1996, 2, 65–70. [Google Scholar] [CrossRef]
- Starfield, B.; Kinder, K. Multimorbidity and its measurement. Health Policy 2011, 103, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Ioakeim-Skoufa, I.; Poblador-Plou, B.; Carmona-Pírez, J.; Díez-Manglano, J.; Navickas, R.; Gimeno-Feliu, L.A.; González-Rubio, F.; Jureviciene, E.; Dambrauskas, L.; Prados-Torres, A.; et al. Multimorbidity Patterns in the General Population: Results from the EpiChron Cohort Study. Int. J. Environ. Res. Public Health 2020, 17, 4242. [Google Scholar] [CrossRef]
- Smith, S.M.; Wallace, E.; O’Dowd, T.; Fortin, M. Interventions for improving outcomes in patients with multimorbidity in primary care and community settings. Cochrane Database Syst. Rev. 2021, 2021, CD006560. [Google Scholar] [CrossRef] [PubMed]
- Garin, N.; Koyanagi, A.; Chatterji, S.; Tyrovolas, S.; Olaya, B.; Leonardi, M.; Lara, E.; Koskinen, S.; Tobiasz-Adamczyk, B.; Ayuso-Mateos, J.L.; et al. Global Multimorbidity Patterns: A Cross-Sectional, Population-Based, Multi-Country Study. J. Gerontol. A Biol. Sci. Med. Sci. 2016, 71, 205–214. [Google Scholar] [CrossRef] [PubMed]
- Aarts, S.; Akker, M.V.D.; Bosma, H.; Tan, F.; Verhey, F.; Metsemakers, J.; van Boxtel, M. The effect of multimorbidity on health related functioning: Temporary or persistent? Results from a longitudinal cohort study. J. Psychosom. Res. 2012, 73, 211–217. [Google Scholar] [CrossRef] [PubMed]
- Glynn, L.G.; Valderas, J.M.; Healy, P.; Burke, E.; Newell, J.; Gillespie, P.; Murphy, A. The prevalence of multimorbidity in primary care and its effect on health care utilization and cost. Fam. Pr. 2011, 28, 516–523. [Google Scholar] [CrossRef]
- Pullar, J.; Allen, L.; Townsend, N.; Williams, J.; Foster, C.; Roberts, N.; Rayner, M.; Mikkelsen, B.; Branca, F.; Wickramasinghe, K. The impact of poverty reduction and development interventions on non-communicable diseases and their behavioural risk factors in low and lower-middle income countries: A systematic review. PLoS ONE 2018, 13, e0193378. [Google Scholar] [CrossRef]
- Eyowas, F.A.; Schneider, M.; Yirdaw, B.A.; Getahun, F.A. Multimorbidity of chronic non-communicable diseases and its models of care in low- and middle-income countries: A scoping review protocol. BMJ Open 2019, 9, e033320. [Google Scholar] [CrossRef]
- Guwatudde, D.; Mutungi, G.; Wesonga, R.; Kajjura, R.; Kasule, H.; Muwonge, J.; Ssenono, V.; Bahendeka, S.K. The Epidemiology of Hypertension in Uganda: Findings from the National Non-Communicable Diseases Risk Factor Survey. PLoS ONE 2015, 10, e0138991. [Google Scholar]
- World Health Organisation. Report on the Status of Major Risk Factors for Non-Communicable Diseases-WHO African Region. Available online: https://www.afro.who.int/sites/default/files/2017-06/15264_who_afr-situation-ncds-15-12-2016-for-web_0.pdf (accessed on 7 July 2020).
- World Health Organisation. Global Status Report on Noncommunicable Diseases. Available online: https://www.who.int/nmh/publications/ncd_report2010/en/ (accessed on 7 July 2020).
- Bhojani, U.; Beerenahalli, T.S.; Devadasan, R.; Munegowda, C.; Devadasan, N.; Criel, B.; Kolsteren, P. No longer diseases of the wealthy: Prevalence and health-seeking for self-reported chronic conditions among urban poor in Southern India. BMC Health Serv. Res. 2013, 13, 306. [Google Scholar] [CrossRef] [PubMed]
- Abad-Díez, J.M.; Calderón-Larrañaga, A.; Poncel-Falcó, A.; Poblador-Plou, B.; Calderón-Meza, J.M.; Sicras-Mainar, A.; Clerencia-Sierra, M.; Prados-Torres, A. Age and gender differences in the prevalence and patterns of multimorbidity in the older population. BMC Geriatr. 2014, 14, 75. [Google Scholar] [CrossRef]
- Violán, C.; Foguet-Boreu, Q.; Flores-Mateo, G.; Salisbury, C.; Blom, J.; Freitag, M.; Glynn, L.; Muth, C.; Valderas, J.M. Prevalence, Determinants and Patterns of Multimorbidity in Primary Care: A Systematic Review of Observational Studies. PLoS ONE 2014, 9, e102149. [Google Scholar] [CrossRef]
- Uijen, A.A.; van de Lisdonk, E.H. Multimorbidity in primary care: Prevalence and trend over the last 20 years. Eur. J. Gen. Pract. 2008, 14 (Suppl. 1), 28–32. [Google Scholar] [CrossRef] [PubMed]
- Afshar, S.; Roderick, P.J.; Kowal, P.; Dimitrov, B.D.; Hill, A.G. Multimorbidity and the inequalities of global ageing: A cross-sectional study of 28 countries using the World Health Surveys. BMC Public Health 2015, 15, 1–10. [Google Scholar] [CrossRef]
- Sara, H.H.; Chowdhury, M.A.B.; Haque, A. Multimorbidity among elderly in Bangladesh. Aging Med. 2018, 1, 267–275. [Google Scholar] [CrossRef]
- Ofori-Asenso, R.; Chin, K.L.; Curtis, A.J.; Zomer, E.; Zoungas, S.; Liew, D. Recent Patterns of Multimorbidity Among Older Adults in High-Income Countries. Popul. Health Manag. 2019, 22, 127–137. [Google Scholar] [CrossRef]
- Nguyen, H.; Manolova, G.; Daskalopoulou, C.; Vitoratou, S.; Prince, M.; Prina, A.M. Prevalence of multimorbidity in community settings: A systematic review and meta-analysis of observational studies. J. Comorbidity 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- United Nations; Department of Economic and Social Affairs; Population Division. World Mortality. Available online: https://www.un.org/en/development/desa/population/publications/pdf/mortality/WMR2019/World_Mortality_2019.pdf (accessed on 7 July 2020).
- Mills, K.T.; Stefanescu, A.; He, J. The global epidemiology of hypertension. Nat. Rev. Nephrol. 2020, 16, 223–237. [Google Scholar] [CrossRef] [PubMed]
- World Health Organisation. Top Ten Causes of Death. Available online: https://www.who.int/en/news-room/fact-sheets/detail/the-top-10-causes-of-death (accessed on 8 July 2020).
- Ataklte, F.; Erqou, S.; Kaptoge, S.; Taye, B.; Echouffo-Tcheugui, J.B.; Kengne, A.P. Burden of undiagnosed hypertension in sub-Saharan Africa: A systematic review and meta-analysis. Hypertension 2015, 65, 291–298. [Google Scholar] [CrossRef]
- Yaya, S.; Ekholuenetale, M.; Bishwajit, G. Differentials in prevalence and correlates of metabolic risk factors of non-communicable diseases among women in sub-Saharan Africa: Evidence from 33 countries. BMC Public Health 2018, 18, 1168. [Google Scholar] [CrossRef]
- Manisalidis, I.; Stavropoulou, E.; Stavropoulos, A.; Bezirtzoglou, E. Environmental and Health Impacts of Air Pollution: A Review. Front. Public Health 2020, 8, 14. [Google Scholar] [CrossRef] [PubMed]
- Jiang, X.-Q.; Mei, X.-D.; Feng, D. Air pollution and chronic airway diseases: What should people know and do? J. Thorac. Dis. 2016, 8, E31–E40. [Google Scholar]
- Eze, I.C.; Schaffner, E.; Fischer, E.; Schikowski, T.; Adam, M.; Imboden, M.; Tsai, M.; Carballo, D.; von Eckardstein, A.; Künzli, N.; et al. Long-term air pollution exposure and diabetes in a population-based Swiss cohort. Environ. Int. 2014, 70, 95–105. [Google Scholar] [CrossRef]
- Mannucci, P.M.; Franchini, M. Health effects of ambient air pollution in developing countries. Int. J. Environ. Res. Public Health 2017, 14, 1048. [Google Scholar] [CrossRef]
- World Health Organisation. Burden of Disease from Ambient and Household Air Pollution. Available online: http://who.int/phe/health_topics/outdoorair/databases/en/ (accessed on 7 July 2020).
- Hashim, D.; Boffetta, P. Occupational and Environmental Exposures and Cancers in Developing Countries. Ann. Glob. Health 2014, 80, 393–411. [Google Scholar] [CrossRef] [PubMed]
- Lelieveld, J.; Klingmüller, K.; Pozzer, A.; Pöschl, U.; Fnais, M.; Daiber, A.; Münzel, T. Cardiovascular disease burden from ambient air pollution in Europe reassessed using novel hazard ratio functions. Eur. Heart J. 2019, 40, 1590–1596. [Google Scholar] [CrossRef] [PubMed]
- Gulis, G.; Mulumba, J.A.A.; Juma, O.; Kakosova, B. Health status of people of slums in Nairobi, Kenya. Environ. Res. 2004, 96, 219–227. [Google Scholar] [CrossRef]
- Yi, J.Y.; Kim, H.; Chi, I. Urban–rural differences in multimorbidity and associated factors in China and Korea: A population-based survey study. Geriatr. Gerontol. Int. 2019, 19, 1157–1164. [Google Scholar] [CrossRef]
- Foguet-Boreu, Q.; Violan, C.; Roso-Llorach, A.; Rodriguez-Blanco, T.; Pons-Vigués, M.; Muñoz-Pérez, A.M.; Pujol-Ribera, E.; Valderas, J.M. Impact of multimorbidity: Acute morbidity, area of residency and use of health services across the life span in a region of south Europe. BMC Fam. Pr. 2014, 15, 55. [Google Scholar] [CrossRef]
- Wesonga, R.; Guwatudde, D.; Bahendeka, S.K.; Mutungi, G.; Nabugoomu, F.; Muwonge, J. Burden of cumulative risk factors associated with non-communicable diseases among adults in Uganda: Evidence from a national baseline survey. Int. J. Equity Health 2016, 15, 195. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Fortin, M.; Haggerty, J.; Almirall, J.; Bouhali, T.; Sasseville, M.; Lemieux, M. Lifestyle factors and multimorbidity: A cross sectional study. BMC Public Health 2014, 14, 686. [Google Scholar] [CrossRef]
- Bao, X.Y.; Xie, Y.X.; Zhang, X.X.; Peng, X.; Huang, J.X.; Du, Q.F.; Wang, P.X. The association between multimorbidity and health-related quality of life: A cross-sectional survey among community middle-aged and elderly residents in southern China. Health Qual. Life Outcomes 2019, 17, 107. [Google Scholar] [CrossRef]
- Tayel, D.I.; El-Sayed, N.A. Dietary pattern and blood pressure levels of adolescents in Sohag, Egypt. J. Egypt. Public Health Assoc. 2013, 88, 97–103. [Google Scholar] [CrossRef]
- Chang, A.Y.; Gómez-Olivé, F.X.; Payne, C.; Rohr, J.K.; Manne-Goehler, J.; Wade, A.N.; Wagner, R.G.; Montana, L.; Tollman, S.; Salomon, A.J. Chronic multimorbidity among older adults in rural South Africa. BMJ Glob. Health 2019, 4, e001386. [Google Scholar] [CrossRef]
- Alaba, O.; Chola, L. The social determinants of multimorbidity in South Africa. Int. J. Equity Health 2013, 12, 63. [Google Scholar] [CrossRef]
- Beran, D. Difficulties Facing the Provision of Care for Multimorbidity in Low-Income Countries. In Comorbidity of Mental and Physical Disorders; Sartorius, N., Holt, R.I.G., Maj, M., Eds.; Karger Publishers: Basel, Switzerland, 2014; Volume 179, pp. 33–41. [Google Scholar] [CrossRef]
- Ezzati, M. Excess weight and multimorbidity: Putting people’s health experience in risk factor epidemiology. Lancet Public Health 2017, 2, e252–e253. [Google Scholar] [CrossRef]
- Freisling, H.; Viallon, V.; Lennon, H.; Bagnardi, V.; Ricci, C.; Butterworth, A.S.; Sweeting, M.; Muller, D.; Romieu, I.; Bazelle, P.; et al. Lifestyle factors and risk of multimorbidity of cancer and cardiometabolic diseases: A multinational cohort study. BMC Med. 2020, 18, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Dhalwani, N.N.; Zaccardi, F.; O’Donovan, G.; Carter, P.; Hamer, M.; Yates, T.; Davies, M.; Khunti, K. Association Between Lifestyle Factors and the Incidence of Multimorbidity in an Older English Population. J. Gerontol. Ser. A Boil. Sci. Med. Sci. 2016, 72, 528–534. [Google Scholar] [CrossRef] [PubMed]
- Wikström, K.; Lindström, J.; Harald, K.; Peltonen, M.; Laatikainen, T. Clinical and lifestyle-related risk factors for incident multimorbidity: 10-year follow-up of Finnish population-based cohorts 1982–2012. Eur. J. Intern. Med. 2015, 26, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Kivimäki, M.; Kuosma, E.; Ferrie, E.J.; Luukkonen, R.; Nyberg, S.T.; Alfredsson, L.; Batty, G.; Brunner, E.; Fransson, E.; Goldberg, M.; et al. Overweight, obesity, and risk of cardiometabolic multimorbidity: Pooled analysis of individual-level data for 120 813 adults from 16 cohort studies from the USA and Europe. Lancet Public Health 2017, 2, e277–e285. [Google Scholar] [CrossRef]
- Mounce, L.; Campbell, J.; Henley, W.E.; Arreal, M.C.T.; Porter, I.; Valderas, J.M. Predicting Incident Multimorbidity. Ann. Fam. Med. 2018, 16, 322–329. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Mishra, G.D.; Dobson, A.J.; Jones, M. Progression of diabetes, heart disease, and stroke multimorbidity in middle-aged women: A 20-year cohort study. PLoS Med. 2018, 15, e1002516. [Google Scholar] [CrossRef]
- World Health Organisation. Global Action Plan for the Prevention and Control of Noncommunicable Diseases 2013–2020. World Health Organisation. Available online: http://apps.who.int/iris/bitstream/10665/94384/1/9789241506236_eng.pdf?ua=1 (accessed on 7 July 2020).
- World Health Organisation. From Burden to “Best Buys”: Reducing the Economic Impact of NCDs in Low- and Middle-Income Countries. Executive Summary. Available online: http://www.who.int/nmh/publications/best_buys_summary/en/ (accessed on 7 July 2020).
- Hyseni, L.; Elliot-Green, A.; Lloyd-Williams, F.; Kypridemos, C.; O’Flaherty, M.; McGill, R.; Orton, L.; Bromley, H.; Cappuccio, F.P.; Capewell, S. Systematic review of dietary salt reduction policies: Evidence for an effectiveness hierarchy? PLoS ONE 2017, 12, e0177535. [Google Scholar] [CrossRef]
- Trieu, K.; McMahon, E.; Santos, J.A.; Bauman, A.; Jolly, K.A.; Bolam, B.; Webster, J. Review of behaviour change interventions to reduce population salt intake. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 17. [Google Scholar] [CrossRef]
- Alkhatib, A. Personalising Exercise and Nutrition Behaviours in Diabetes Lifestyle Prevention. EMJ 2020, 5, 67–77. [Google Scholar]
- BeLue, R.; A Okoror, T.; Iwelunmor, J.; Taylor, K.D.; Degboe, A.N.; Agyemang, C.; Ogedegbe, G. An overview of cardiovascular risk factor burden in sub-Saharan African countries: A socio-cultural perspective. Glob. Health 2009, 5, 10. [Google Scholar] [CrossRef]
- Alkhatib, A.; Tsang, C.; Tiss, A.; Bahorun, T.; Arefanian, H.; Barake, R.; Khadir, A.; Tuomilehto, J. Functional foods and lifestyle approaches for diabetes prevention and management. Nutrients 2017, 9, 1310. [Google Scholar] [CrossRef]
- Alkhatib, A. Antiviral Functional Foods and Exercise Lifestyle Prevention of Coronavirus. Nutrients 2020, 12, 2633. [Google Scholar] [CrossRef] [PubMed]
- Alkhatib, A.; Tuomilehto, J. Lifestyle diabetes prevention. In Encyclopaedia of Endocrine Diseases; Huhtaniemi, I., Ed.; Elsevier: London, UK, 2019; pp. 148–159. [Google Scholar]
- Damasceno, A.; Azevedo, A.; Silva-Matos, C.; Prista, A.; Diogo, D.; Lunet, N. Hypertension prevalence, awareness, treatment, and control in Mozambique: Urban/rural gap during epidemiological transition. Hypertension 2009, 54, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Ngugi, A.K.; Bottomley, C.; Kleinschmidt, I.; Wagner, R.G.; Kakooza-Mwesige, A.; Ae-Ngibise, K.; Owusu-Agyei, S.; Masanja, H.; Kamuyu, G.; Odhiambo, R.; et al. Prevalence of active convulsive epilepsy in sub-Saharan Africa and associated risk factors: Cross-sectional and case-control studies. Lancet Neurol. 2013, 12, 253–263. [Google Scholar] [CrossRef]
- Keezer, M.R.; Sisodiya, S.M.; Sander, J.W. Comorbidities of epilepsy: Current concepts and future perspectives. Lancet Neurol. 2015, 15, 106–115. [Google Scholar] [CrossRef]
- Gururaj, G.; Satishchandra, P.; Amudhan, S. Epilepsy in India II: Impact, burden, and need for a multisectoral public health response. Ann. Indian Acad. Neurol. 2015, 18, 369–381. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alkhatib, A.; Nnyanzi, L.A.; Mujuni, B.; Amanya, G.; Ibingira, C. Preventing Multimorbidity with Lifestyle Interventions in Sub-Saharan Africa: A New Challenge for Public Health in Low and Middle-Income Countries. Int. J. Environ. Res. Public Health 2021, 18, 12449. https://doi.org/10.3390/ijerph182312449
Alkhatib A, Nnyanzi LA, Mujuni B, Amanya G, Ibingira C. Preventing Multimorbidity with Lifestyle Interventions in Sub-Saharan Africa: A New Challenge for Public Health in Low and Middle-Income Countries. International Journal of Environmental Research and Public Health. 2021; 18(23):12449. https://doi.org/10.3390/ijerph182312449
Chicago/Turabian StyleAlkhatib, Ahmad, Lawrence Achilles Nnyanzi, Brian Mujuni, Geofrey Amanya, and Charles Ibingira. 2021. "Preventing Multimorbidity with Lifestyle Interventions in Sub-Saharan Africa: A New Challenge for Public Health in Low and Middle-Income Countries" International Journal of Environmental Research and Public Health 18, no. 23: 12449. https://doi.org/10.3390/ijerph182312449
APA StyleAlkhatib, A., Nnyanzi, L. A., Mujuni, B., Amanya, G., & Ibingira, C. (2021). Preventing Multimorbidity with Lifestyle Interventions in Sub-Saharan Africa: A New Challenge for Public Health in Low and Middle-Income Countries. International Journal of Environmental Research and Public Health, 18(23), 12449. https://doi.org/10.3390/ijerph182312449







