Physical Activity of Children and Adolescents during the COVID-19 Pandemic—A Scoping Review
Abstract
:1. Introduction
2. Materials and Methods
3. Results
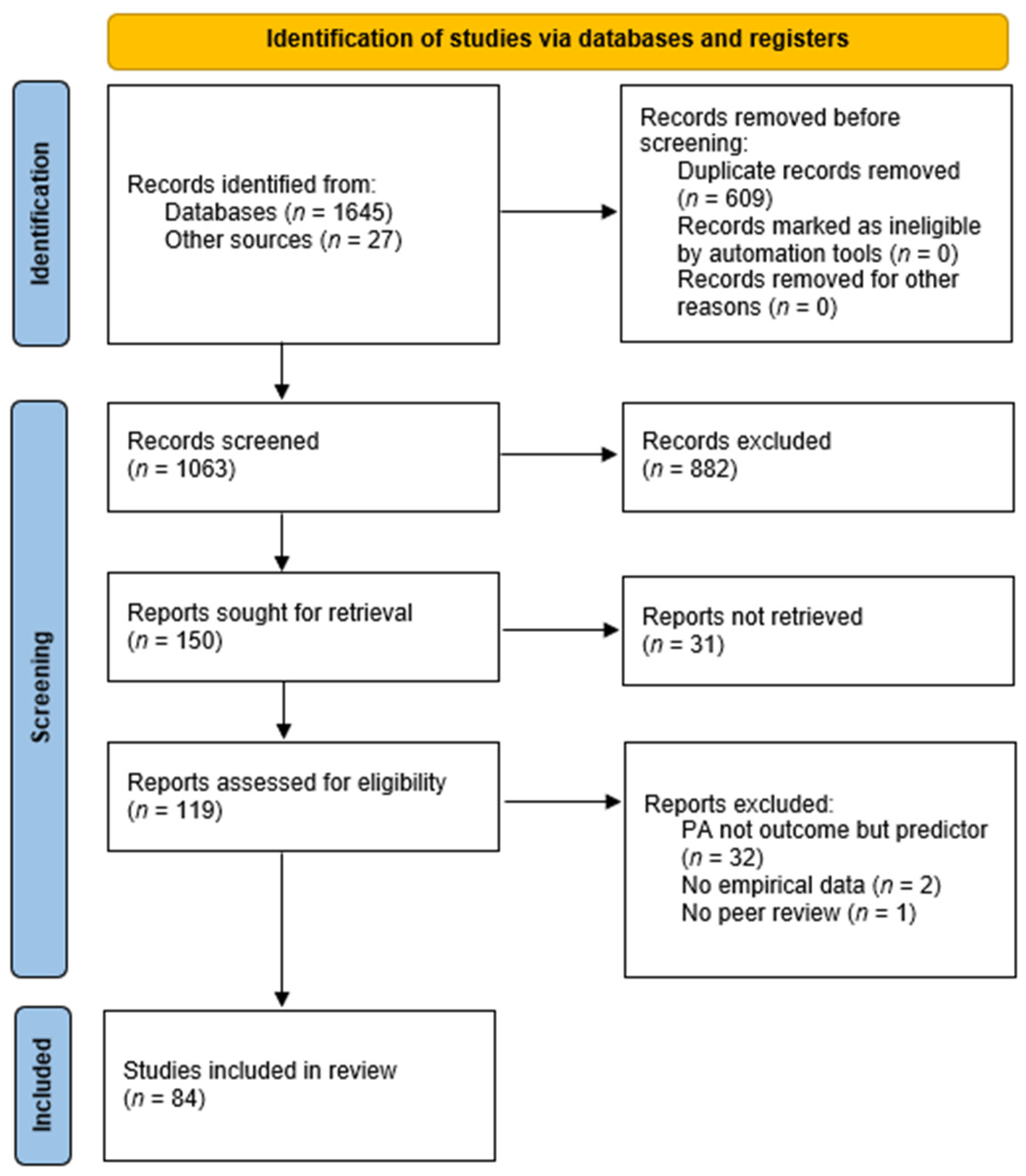
3.1. Study Selection
3.2. Study Characteristics
3.3. Change of Physical Activity Behavior
3.4. Determinants of Physical Activity Behavior
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| No. | Author, Year (Ref) | Country | Research Paradigm | Study Design | Sample (Age Incl.) | Method | Change of PA | Risk of Bias |
|---|---|---|---|---|---|---|---|---|
| Americas | ||||||||
| 1 | Aguilar-Farias et al., 2020 [33] | Chile | QUAN | Cross-sectional | n = 3157 (1–5 years) | Online survey | Decrease | Fair |
| 2 | Bazett-Jones et al., 2020 [61] | USA | QUAN | Cross-sectional | n = 287 (9–19 years) | Online survey | Decrease | Fair |
| 3 | Beck et al., 2021 [62] | USA | QUAN | Cross-sectional | n = 145 (4–12 years) | Survey | Decrease | Fair |
| 4 | Dayton et al., 2020 [63] | USA | QUAN | Retrospective case-control | n = 20 (mean: 15.2 years) | Cardiopulmonary stress testing | Decrease | Fair |
| 5 | Gama de Matos et al., 2020 [64] | Brazil | QUAN | Cross-sectional | n = 426 (children, adolescents, adults, elders) | Online survey | Decrease | Fair |
| 6 | Dos Santos Cardoso de Sá, 2020 [65] | Brazil | QUAN | Cross-sectional | n = 816 (<12 years) | Online survey | Decrease | Poor |
| 7 | Dunton et al., 2020 [66] | USA | QUAN | Cross-sectional | n = 211 (5–13 years) | Online survey | Decrease | Fair |
| 8 | Eyler et al., 2021 [67] | USA | QUAN | Cross-sectional | n = 245 (5–12 years) | Online survey | Decrease | Fair |
| 9 | Garcia et al., 2020 [68] | USA | QUAN | Longitudinal | n = 9 (14–19 years) | Online survey | Decrease | Fair |
| 10 | Guerrero et al., 2020 [35] | Canada | QUAN | Cross-sectional | n = 1472 (5–17 years) | Online survey, decision tree | - | Fair |
| 11 | Hemphill et al., 2020 [69] | Canada | QUAN | Longitudinal | n = 109 (9–16 years) | Step count via Fitbit-Tracker | Decrease | Fair |
| 12 | Kracht et al., 2021 [58] | USA | QUAN | Cross-sectional | n = 1836 (3–6 years) | Online survey | Decrease | Fair |
| 13 | Lafave et al., 2021 [15] | Canada | QUAL | Cross-sectional | n = 17 (2–5 years) | Semi-structured interviews | Increase | Poor |
| 14 | Malta et al., 2021 [70] | Brazil | QUAN | Cross-sectional | n = 6470 (12–17 years) | Online survey | Decrease | Poor |
| 15 | McCormack et al., 2020 [25] | Canada | QUAN | Cross-sectional | n = 328 (school-aged) | Online survey | PA at home: increase PA outdoors: decrease | Fair |
| 16 | Mitra et al., 2020 [46] | Canada | QUAN | Cross-sectional | n = 1472 (5–17 years) | Online survey | Decrease | Fair |
| 17 | Moore et al., 2020 [47] | Canada | QUAN | Cross-sectional | n = 1472 (5–17 years) | Online survey | Decrease | Fair |
| 18 | Pavlovic et al., 2021 [71] | USA | QUAN | Cross-sectional | n = 2440 (PE teachers, school and district administrators, nurses, others) | Online survey | Decrease | Poor |
| 19 | Pelletier et al., 2021 [26] | Canada | QUAL | Cross-sectional | n = 21 (7–12 years) | Semi-structured interview | Increase in unstructured activity; decrease in structured activity | Poor |
| 20 | Perez et al., 2021 [48] | USA | QUAL | Cross-sectional | n = 321 (mean: 7.8 years) | Open-ended survey | Decrease | Poor |
| 21 | Riazi et al., 2021 [16] | Canada | QUAL | Cross-sectional | n = 29 (5–11 years) | Semi-structured interviews | Decrease | Poor |
| 22 | Shepherd et al., 2021 [27] | Canada | QUAL | Cross-sectional | n = 20 (high-school student-athletes) | Semi-structured interviews | Variations | Poor |
| 23 | Siegle et al., 2020 [50] | Brazil | QUAN | Cross-sectional | n = 816 (<13 years) | Online survey | Decrease | Fair |
| 24 | Tulchin-Francis et al., 2021 [52] | USA | QUAN | Cross-sectional | n = 1310 (3–18 years) | Online survey | Decrease | Fair |
| 25 | Wahl-Alexander and Camic, 2021 [72] | USA | QUAN | Longitudinal | n = 264 (mean: 9.6 years) | In-person testing (BMI, fitness assessment) | Decrease | Poor |
| Europe | ||||||||
| 26 | Androutsos et al., 2021 [73] | Greece | QUAN | Cross-sectional | n = 397 (2–18 years) | Online survey | Decrease | Fair |
| 27 | Bronikowska et al., 2021 [28] | Poland | QUAN | Longitudinal | n = 127 (mean: 15.4 years) | Online survey | Increase in previously inactive, decrease in previously active | Fair |
| 28 | Chambonniere et al., 2021 [51] | France | QUAN | Cross-sectional | n = 6491 (6–17 years) | Online survey | Decrease | Poor |
| 29 | Chen et al., 2021 [74] | Sweden | QUAN | Longitudinal | n = 1316 (mean: 13.6 years at baseline) | Online survey | Decrease | Poor |
| 30 | Dauty et al., 2020 [75] | France | QUAN | Longitudinal | n = 19 (13–15 years) | Pre- and post-confinement Yo-Yo Test | Decrease | Fair |
| 31 | Delisle Nyström et al., 2020 [17] | Sweden | QUAN | Longitudinal | n = 100 (3–5 years) | Phone interview, accelerometer | Increase | Good |
| 32 | Di Renzo et al., 2020 [19] | Italy | QUAN | Cross-sectional | n = 3533 (≥12 years) | Online survey | No difference | Fair |
| 33 | Dragun et al., 2020 [20] | Croatia | QUAN | Longitudinal | n = 1326 (adolescents, medical students) | Pre-COVID: in-person survey During COVID: online survey | No difference | Fair |
| 34 | Fillon et al., 2021 [76] | France | QUAN | Longitudinal | n/a | Expert panel | Decrease | Poor |
| 35 | Francisco et al., 2020 [77] | Italy, Spain, Portugal | QUAN | Cross-sectional | n = 1480 (3–18 years) | Online survey | Decrease | Poor |
| 36 | Gallucio et al., 2021 [21] | Italy | QUAN | Cross-sectional | n = 91 (15–17 years) | Online survey | No difference | Fair |
| 37 | Gilic et al., 2020 [36] | Bosnia and Herzegovina | QUAN | Longitudinal | n = 688 (15–18 years) | Online survey | Decrease | Fair |
| 38 | Jurak et al., 2021 [78] | Slovenia | QUAN | Longitudinal | n = 20,000 (6–14 years) | SLOfit barometer, fitness measurements | Decrease | Poor |
| 39 | Kolota and Glabska, 2021 [22] | Poland | QUAN | Cross-sectional | n = 1334 (10–16 years) | Online survey | No difference | Fair |
| 40 | Kovacs et al., 2021 [38] | 10 Euro-pean countries | QUAN | Cross-sectional | n = 8395 (6–18 years) | Online survey | Decrease | Poor |
| 41 | López-Bueno et al., 2020 [79] | Spain | QUAN | Cross-sectional | n = 860 (3–16 years) | Online survey | Decrease | Fair |
| 42 | Medrano et al., 2020 [34] | Spain | QUAN | Longitudinal | n = 290 (8–16 years) | Online survey | Decrease | Good |
| 43 | Ng et al., 2020 [40] | Ireland | QUAN | Cross-sectional | n = 1214 (12–18 years) | Online survey | Decrease | Fair |
| 44 | O’Kane et al., 2021 [23] | Ireland | MIXED | Longitudinal | n = 281 (12–14 years) | Survey, semi-structured interviews | No difference | Fair |
| 45 | Orgilés et al., 2020 [49] | Italy, Spain | QUAN | Cross-sectional | n = 1143 (3–18 years) | Online survey | Decrease | Poor |
| 46 | Pietrobelli et al., 2020 [80] | Italy | QUAN | Longitudinal | n = 41 (6–18 years) | Pre-COVID: in-person interview During COVID: phone interview | Decrease | Fair |
| 47 | Pombo et al., 2020 [45] | Portugal | QUAN | Cross-sectional | n = 2159 (<13 years) | Online survey | - | Fair |
| 48 | Pombo et al., 2021 [81] | Portugal | QUAN | Longitudinal | n = 114 (6–9 years) | Motor competence assessment | Decrease | Good |
| 49 | Pombo et al., 2021 [82] | Portugal | QUAN | Cross-sectional | n = 2159 (<13 years) | Online survey | Decrease | Fair |
| 50 | Poulain et al., 2021 [29] | Germany | QUAN | Longitudinal | n = 285 (1–10 years) | Online survey | Playing outdoors: increase Indoor sports: decrease | Fair |
| 51 | Schmidt et al., 2020 [30] | Germany | QUAN | Longitudinal | n = 1711 (4–17 years) | Pre-COVID: in-person survey During COVID: online survey | Nonorganized PA: increase Organized sports: decrease | Fair |
| 52 | Sekulic et al., 2020 [42] | Croatia | QUAN | Longitudinal | n = 401 (15–18 years) | Online survey | Decrease | Fair |
| 53 | Siachpazidou et al., 2021 [83] | Greece | QUAN | Cross-sectional | n = 482 (4–12 years) | Online survey | Decrease | Poor |
| 54 | Szabó et al., 2020 [84] | Hungary | QUAN | Cross-sectional | n = 840 (<85 years) | Online survey | Decrease | Fair |
| 55 | Ten Velde et al., 2021 [85] | Netherlands | QUAN | Longitudinal | Cohort A: n = 102 Cohort B: n=131 (A: 4–18 years B: 7–12 years) | Cohort A: online survey Cohort B: online survey, accelerometry | Decrease | Fair |
| 56 | Versloot et al., 2020 [86] | Netherlands | QUAN | Longitudinal | n = 82 (6–49 years) | Phone interview | Decrease | Poor |
| 57 | Vukovic et al., 2021 [43] | Serbia | QUAN | Cross-sectional | n = 450 | Online survey | Decrease | Fair |
| 58 | Wunsch et al., 2021 [44] | Germany | QUAN | Longitudinal | n = 1711 (4–17 years) | Pre-COVID: in-person survey During COVID: online survey | Increase | Fair |
| 59 | Zorcec et al., 2020 [87] | Macedonia | QUAN | Cross-sectional | n = 72 (mean: 7.3 years) | Online survey | Decrease | Poor |
| Asia | ||||||||
| 60 | Constantini et al., 2021 [39] | Israel | QUAN | Cross-sectional | n = 473 (16–18 years) | Online survey | - | Fair |
| 61 | Elnaggar et al., 2020 [57] | Saudi Arabia | QUAN | Longitudinal | n = 63 (14–18 years) | Online survey | Decrease | Poor |
| 62 | Guo et al., 2021 [88] | China | QUAN | Cross-sectional | n = 10,416 (10–16 years) | Online survey | Decrease | Poor |
| 63 | Jia et al., 2020 [89] | China | QUAN | Cross-sectional | n = 10,082 (high school, college, graduate school students) | Online survey | Decrease | Poor |
| 64 | Xiang et al., 2020 [90] | China | QUAN | Longitudinal | n = 2426 (6–17 years) | Online survey | Decrease | Poor |
| 65 | Xiao et al., 2021 [37] | China | QUAN | Cross-sectional | n = 1680 | Online survey | - | Poor |
| 66 | Yang et al., 2020 [91] | China | QUAN | Cross-sectional | n = 10,082 (mean: 19.8 years) | Online survey | Decrease | Poor |
| 67 | Zenic et al., 2020 [59] | Croatia | QUAN | Longitudinal | n = 823 (mean: 16.5 years) | Online survey | Decrease | Fair |
| 68 | Zhang et al., 2020 [56] | China | QUAN | Cross-sectional | n = 9979 (9–14 years) | Online survey | Decrease | Fair |
| 69 | Zhou et al., 2021 [92] | China | QUAN | Cross-sectional | n = 8115 (15–33 years) | Online survey | Decrease | Fair |
| 70 | Zhu et al., 2021 [18] | Hong Kong | QUAN | Cross-sectional | n = 2863 (9–17 years) | In-person survey | Increase | Fair |
| Africa | ||||||||
| 71 | Abid et al., 2021 [93] | Tunisia | QUAN | Cross-sectional | n = 100 (5–12 years) | Online survey | Decrease | Fair |
| 72 | Dixon et al., 2020 [53] | Kenya | QUAL | Cross-sectional | n = 16 (14–18 years) | Case study (observations, participant journals) | Decrease | Poor |
| Oceania | ||||||||
| 73 | Elliott et al., 2021 [94] | Australia | QUAL | Cross-sectional | n = 18 (15–17 years) | Online interviews, focus groups | Decrease | Poor |
| 74 | Masi et al., 2020 [95] | Australia | QUAN | Cross-sectional | n = 302 (2–17 years) | Online survey | Decrease | Poor |
| 75 | Munasinghe et al., 2020 [96] | Australia | QUAN | Longitudinal | n = 582 (13–19 years) | App survey, EMA, smartphone sensors | Decrease | Fair |
| 76 | Nathan et al., 2021 [31] | Australia | QUAN | Longitudinal | n = 157 (5–9 years) | Online survey | Unorganized PA: increase Organized PA: decrease | Fair |
| 77 | Parker et al., 2021 [41] | Australia | QUAN | Cross-sectional | n = 963 (13–17 years) | Online survey | - | Fair |
| 78 | Reece et al., 2020 [97] | Australia | QUAN | Cross-sectional | n = 16,177 (4–18 years) | Online survey | Decrease | Poor |
| 79 | Sciberras et al., 2020 [54] | Australia | QUAN | Longitudinal | n = 213 (5–17 years) | Online survey | Decrease | Fair |
| Cross-continental | ||||||||
| 80 | Guan et al., 2020 [98] | 15 countries | QUAN | Cross-sectional | n/a | Community mobility data (Google) | Decrease | Poor |
| 81 | López-Aymes et al., 2021 [55] | Spain, Latin America | MIXED | Cross-sectional | n = 234 (≥18 years) | Online survey, discourse analysis | - | Poor |
| 82 | López-Gil et al., 2021 [99] | Brazil, Spain | QUAN | Cross-sectional | n = 1099 (3–17 years) | Online survey | Decrease | Fair |
| 83 | Okely et al., 2021 [24] | 14 countries | QUAN | Longitudinal | n = 948 (3–5 years) | Survey | No difference | Fair |
| 84 | Ruíz-Roso et al., 2020 [32] | Brazil, Chile, Colombia, Spain, Italy | QUAN | Cross-sectional | n = 726 (10–19 years) | Online survey | Decrease overall (increase in Italy, Spain, Colombia) | Fair |
References
- World Health Organization (WHO). WHO Interactive Timeline: WHO’s COVID-19 Response. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/interactive-timeline (accessed on 22 July 2021).
- Hwang, T.-J.; Rabheru, K.; Peisah, C.; Reichman, W.; Ikeda, M. Loneliness and social isolation during the COVID-19 pandemic. Int. Psychogeriatr. 2020, 32, 1217–1220. [Google Scholar] [CrossRef]
- Stockwell, S.; Trott, M.; Tully, M.; Shin, J.; Barnett, Y.; Butler, L.; McDermott, D.; Schuch, F.; Smith, L. Changes in physical activity and sedentary behaviours from before to during the COVID-19 pandemic lockdown: A systematic review. BMJ Open Sport Exerc. Med. 2021, 7, e000960. [Google Scholar] [CrossRef] [PubMed]
- Polero, P.; Rebollo-Seco, C.; Adsuar, J.C.; Pérez-Gómez, J.; Rojo-Ramos, J.; Manzano-Redondo, F.; Garcia-Gordillo, M.; Carlos-Vivas, J. Physical Activity Recommendations during COVID-19: Narrative Review. Int. J. Environ. Res. Public Health 2020, 18, 65. [Google Scholar] [CrossRef]
- Kang, S.-J.; Jung, S.I. Age-Related Morbidity and Mortality among Patients with COVID-19. Infect. Chemother. 2020, 52, 154–164. [Google Scholar] [CrossRef]
- Konstabel, K.; Verbestel, V.; Veidebaum, T.; Moreno, L.A.; Bammann, K.; Tornaritis, M.; Eiben, G.; Molnár, D.; Siani, A.; Sprengeler, O.; et al. Objectively measured physical activity in European children: The IDEFICS study. Int. J. Obes. 2014, 38, S135–S143. [Google Scholar] [CrossRef] [Green Version]
- Scheerder, J.; Thomis, M.; Vanreusel, B.; Lefevre, J.; Renson, R.; Eynde, B.V.; Beunen, G.P. Sports Participation Among Females from Adolescence to Adulthood. Int. Rev. Sociol. Sport 2006, 41, 413–430. [Google Scholar] [CrossRef]
- Rodriguez-Ayllon, M.; Cadenas-Sánchez, C.; Estévez-López, F.; Muñoz, N.E.; Mora-Gonzalez, J.; Migueles, J.H.; Molina-Garcia, P.; Henriksson, H.; Mena-Molina, A.; Martínez-Vizcaíno, V.; et al. Role of Physical Activity and Sedentary Behavior in the Mental Health of Preschoolers, Children and Adolescents: A Systematic Review and Meta-Analysis. Sports Med. 2019, 49, 1383–1410. [Google Scholar] [CrossRef]
- García-Hermoso, A.; Ramírez-Campillo, R.; Izquierdo, M. Is Muscular Fitness Associated with Future Health Benefits in Children and Adolescents? A Systematic Review and Meta-Analysis of Longitudinal Studies. Sports Med. 2019, 49, 1079–1094. [Google Scholar] [CrossRef] [PubMed]
- López-Valenciano, A.; Suárez-Iglesias, D.; Sanchez-Lastra, M.A.; Ayán, C. Impact of COVID-19 Pandemic on University Students’ Physical Activity Levels: An Early Systematic Review. Front. Psychol. 2021, 11, 624567. [Google Scholar] [CrossRef]
- Violant-Holz, V.; Gallego-Jiménez, M.G.; González-González, C.S.; Muñoz-Violant, S.; Rodríguez, M.J.; Sansano-Nadal, O.; Guerra-Balic, M. Psychological Health and Physical Activity Levels during the COVID-19 Pandemic: A Systematic Review. Int. J. Environ. Res. Public Health 2020, 17, 9419. [Google Scholar] [CrossRef]
- Downs, S.H.; Black, N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J. Epidemiol. Community Health 1998, 52, 377–384. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mani-Babu, S.; Morrissey, D.; Waugh, C.; Screen, H.; Barton, C. The Effectiveness of Extracorporeal Shock Wave Therapy in Lower Limb Tendinopathy. Am. J. Sports Med. 2014, 43, 752–761. [Google Scholar] [CrossRef] [PubMed]
- Williams, C.Y.K.; Townson, A.T.; Kapur, M.; Ferreira, A.F.; Nunn, R.; Galante, J.; Phillips, V.; Gentry, S.; Usher-Smith, J.A. Interventions to reduce social isolation and loneliness during COVID-19 physical distancing measures: A rapid systematic review. PLoS ONE 2021, 16, e0247139. [Google Scholar] [CrossRef] [PubMed]
- Lafave, L.; Webster, A.D.; McConnell, C. Impact of COVID-19 on Early Childhood Educator’s Perspectives and Practices in Nutrition and Physical Activity: A Qualitative Study. J. Fam. Econ. Issues 2021, 49, 935–945. [Google Scholar] [CrossRef]
- Riazi, N.; Wunderlich, K.; Gierc, M.; Brussoni, M.; Moore, S.; Tremblay, M.; Faulkner, G. “You Can’t Go to the Park, You Can’t Go Here, You Can’t Go There”: Exploring Parental Experiences of COVID-19 and Its Impact on Their Children’s Movement Behaviours. Children 2021, 8, 219. [Google Scholar] [CrossRef]
- Nyström, C.D.; Alexandrou, C.; Henström, M.; Nilsson, E.; Okely, A.; Wehbe El Masri, S.; Löf, M. International Study of Movement Behaviors in the Early Years (SUNRISE): Results from SUNRISE Sweden’s Pilot and COVID-19 Study. Int. J. Environ. Res. Public Health 2020, 17, 8491. [Google Scholar] [CrossRef]
- Zhu, S.; Zhuang, Y.; Ip, P. Impacts on Children and Adolescents’ Lifestyle, Social Support and Their Association with Negative Impacts of the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 4780. [Google Scholar] [CrossRef]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attinà, A.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; Scerbo, F.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Transl. Med. 2020, 18, 229. [Google Scholar] [CrossRef] [PubMed]
- Dragun, R.; Veček, N.; Marendić, M.; Pribisalić, A.; Đivić, G.; Cena, H.; Polašek, O.; Kolčić, I. Have Lifestyle Habits and Psychological Well-Being Changed among Adolescents and Medical Students Due to COVID-19 Lockdown in Croatia? Nutrients 2020, 13, 97. [Google Scholar] [CrossRef]
- Galluccio, A.; Caparello, G.; Avolio, E.; Manes, E.; Ferraro, S.; Giordano, C.; Sisci, D.; Bonofiglio, D. Self-Perceived Physical Activity and Adherence to the Mediterranean Diet in Healthy Adolescents during COVID-19: Findings from the DIMENU Pilot Study. Healthcare 2021, 9, 622. [Google Scholar] [CrossRef]
- Kołota, A.; Głąbska, D. COVID-19 Pandemic and Remote Education Contributes to Improved Nutritional Behaviors and Increased Screen Time in a Polish Population-Based Sample of Primary School Adolescents: Diet and Activity of Youth during COVID-19 (DAY-19) Study. Nutrients 2021, 13, 1596. [Google Scholar] [CrossRef]
- O’Kane, S.M.; Lahart, I.M.; Gallagher, A.M.; Carlin, A.; Faulkner, M.; Jago, R.; Murphy, M.H. Changes in Physical Activity, Sleep, Mental Health, and Social Media Use During COVID-19 Lockdown Among Adolescent Girls: A Mixed-Methods Study. J. Phys. Act. Health 2021, 18, 677–685. [Google Scholar] [CrossRef] [PubMed]
- Okely, A.D.; Kariippanon, K.E.; Guan, H.; Taylor, E.K.; Suesse, T.; Cross, P.L.; Chong, K.H.; Suherman, A.; Turab, A.; Staiano, A.E.; et al. Global effect of COVID-19 pandemic on physical activity, sedentary behaviour and sleep among 3 to 5-year-old children: A longitudinal study of 14 countries. BMC Public Health 2021, 21, 1–15. [Google Scholar] [CrossRef] [PubMed]
- McCormack, G.R.; Doyle-Baker, P.K.; Petersen, J.A.; Ghoneim, D. Parent anxiety and perceptions of their child’s physical activity and sedentary behaviour during the COVID-19 pandemic in Canada. Prev. Med. Rep. 2020, 20, 101275. [Google Scholar] [CrossRef]
- Pelletier, C.; Cornish, K.; Sanders, C. Children’s Independent Mobility and Physical Activity during the COVID-19 Pandemic: A Qualitative Study with Families. Int. J. Environ. Res. Public Health 2021, 18, 4481. [Google Scholar] [CrossRef]
- Shepherd, H.; Evans, T.; Gupta, S.; McDonough, M.; Doyle-Baker, P.; Belton, K.; Karmali, S.; Pawer, S.; Hadly, G.; Pike, I.; et al. The Impact of COVID-19 on High School Student-Athlete Experiences with Physical Activity, Mental Health, and Social Connection. Int. J. Environ. Res. Public Health 2021, 18, 3515. [Google Scholar] [CrossRef]
- Bronikowska, M.; Krzysztoszek, J.; Łopatka, M.; Ludwiczak, M.; Pluta, B. Comparison of Physical Activity Levels in Youths before and during a Pandemic Lockdown. Int. J. Environ. Res. Public Health 2021, 18, 5139. [Google Scholar] [CrossRef]
- Poulain, T.; Meigen, C.; Sobek, C.; Ober, P.; Igel, U.; Körner, A.; Kiess, W.; Vogel, M. Loss of childcare and classroom teaching during the COVID-19-related lockdown in spring 2020: A longitudinal study on consequences on leisure behavior and schoolwork at home. PLoS ONE 2021, 16, e0247949. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, S.C.E.; Anedda, B.; Burchartz, A.; Eichsteller, A.; Kolb, S.; Nigg, C.; Niessner, C.; Oriwol, D.; Worth, A.; Woll, A. Physical activity and screen time of children and adolescents before and during the COVID-19 lockdown in Germany: A natural experiment. Sci. Rep. 2020, 10, 1–12. [Google Scholar] [CrossRef]
- Nathan, A.; George, P.; Ng, M.; Wenden, E.; Bai, P.; Phiri, Z.; Christian, H. Impact of COVID-19 Restrictions on Western Australian Children’s Physical Activity and Screen Time. Int. J. Environ. Res. Public Health 2021, 18, 2583. [Google Scholar] [CrossRef]
- Ruíz-Roso, M.; Padilha, P.D.C.; Matilla-Escalante, D.; Brun, P.; Ulloa, N.; Acevedo-Correa, D.; Peres, W.A.F.; Martorell, M.; Carrilho, T.R.B.; Cardoso, L.D.O.; et al. Changes of Physical Activity and Ultra-Processed Food Consumption in Adolescents from Different Countries during COVID-19 Pandemic: An Observational Study. Nutrients 2020, 12, 2289. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Farias, N.; Toledo-Vargas, M.; Miranda-Marquez, S.; Cortinez-O’Ryan, A.; Cristi-Montero, C.; Rodriguez-Rodriguez, F.; Martino-Fuentealba, P.; Okely, A.; Cruz, B.D.P. Sociodemographic Predictors of Changes in Physical Activity, Screen Time, and Sleep among Toddlers and Preschoolers in Chile during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 18, 176. [Google Scholar] [CrossRef]
- Medrano, M.; Cadenas-Sanchez, C.; Oses, M.; Arenaza, L.; Amasene, M.; Labayen, I. Changes in lifestyle behaviours during the COVID-19 confinement in Spanish children: A longitudinal analysis from the MUGI project. Pediatric Obes. 2020, 16, e12731. [Google Scholar] [CrossRef] [PubMed]
- Guerrero, M.; Vanderloo, L.; Rhodes, R.; Faulkner, G.; Moore, S.; Tremblay, M. Canadian children’s and youth’s adherence to the 24-h movement guidelines during the COVID-19 pandemic: A decision tree analysis. J. Sport Health Sci. 2020, 9, 313–321. [Google Scholar] [CrossRef] [PubMed]
- Gilic, B.; Ostojic, L.; Corluka, M.; Volaric, T.; Sekulic, D. Contextualizing Parental/Familial Influence on Physical Activity in Adolescents before and during COVID-19 Pandemic: A Prospective Analysis. Children 2020, 7, 125. [Google Scholar] [CrossRef] [PubMed]
- Xiao, S.; Yan, Z.; Zhao, L. Physical Activity, Screen Time, and Mood Disturbance Among Chinese Adolescents During COVID-19. J. Psychosoc. Nurs. Ment. Health Serv. 2021, 59, 14–20. [Google Scholar] [CrossRef]
- Kovacs, V.A.; Starc, G.; Brandes, M.; Kaj, M.; Blagus, R.; Leskošek, B.; Suesse, T.; Dinya, E.; Guinhouya, B.C.; Zito, V.; et al. Physical activity, screen time and the COVID-19 school closures in Europe—An observational study in 10 countries. Eur. J. Sport Sci. 2021, 373, 1–10. [Google Scholar] [CrossRef]
- Constantini, K.; Markus, I.; Epel, N.; Jakobovich, R.; Gepner, Y.; Lev-Ari, S. Continued Participation of Israeli Adolescents in Online Sports Programs during the COVID-19 Pandemic Is Associated with Higher Resilience. Int. J. Environ. Res. Public Health 2021, 18, 4386. [Google Scholar] [CrossRef]
- Ng, K.; Cooper, J.; McHale, F.; Clifford, J.; Woods, C. Barriers and facilitators to changes in adolescent physical activity during COVID-19. BMJ Open Sport Exerc. Med. 2020, 6, e000919. [Google Scholar] [CrossRef]
- Parker, K.; Uddin, R.; Ridgers, N.D.; Brown, H.; Veitch, J.; Salmon, J.; Timperio, A.; Sahlqvist, S.; Cassar, S.; Toffoletti, K.; et al. The Use of Digital Platforms for Adults’ and Adolescents’ Physical Activity During the COVID-19 Pandemic (Our Life at Home): Survey Study. J. Med. Internet Res. 2021, 23, e23389. [Google Scholar] [CrossRef]
- Sekulic, D.; Blazevic, M.; Gilic, B.; Kvesic, I.; Zenic, N. Prospective Analysis of Levels and Correlates of Physical Activity during COVID-19 Pandemic and Imposed Rules of Social Distancing; Gender Specific Study among Adolescents from Southern Croatia. Sustainability 2020, 12, 4072. [Google Scholar] [CrossRef]
- Vuković, J.; Matić, R.; Milovanović, I.; Maksimović, N.; Krivokapić, D.; Pišot, S. Children’s Daily Routine Response to COVID-19 Emergency Measures in Serbia. Front. Pediatr. 2021, 9, 154. [Google Scholar] [CrossRef]
- Wunsch, K.; Nigg, C.; Niessner, C.; Schmidt, S.; Oriwol, D.; Hanssen-Doose, A.; Burchartz, A.; Eichsteller, A.; Kolb, S.; Worth, A.; et al. The Impact of COVID-19 on the Interrelation of Physical Activity, Screen Time and Health-Related Quality of Life in Children and Adolescents in Germany: Results of the Motorik-Modul Study. Children 2021, 8, 98. [Google Scholar] [CrossRef] [PubMed]
- Pombo, A.; Luz, C.; de Sá, C.; Rodrigues, L.; Cordovil, R. Effects of the COVID-19 Lockdown on Portuguese Children’s Motor Competence. Children 2021, 8, 199. [Google Scholar] [CrossRef] [PubMed]
- Mitra, R.; Moore, S.A.; Gillespie, M.; Faulkner, G.; Vanderloo, L.M.; Chulak-Bozzer, T.; Rhodes, R.E.; Brussoni, M.; Tremblay, M.S. Healthy movement behaviours in children and youth during the COVID-19 pandemic: Exploring the role of the neighbourhood environment. Health Place 2020, 65, 102418. [Google Scholar] [CrossRef]
- Moore, S.A.; Faulkner, G.; Rhodes, R.E.; Brussoni, M.; Chulak-Bozzer, T.; Ferguson, L.J.; Mitra, R.; O’Reilly, N.; Spence, J.C.; Vanderloo, L.M.; et al. Impact of the COVID-19 virus outbreak on movement and play behaviours of Canadian children and youth: A national survey. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 1–11. [Google Scholar] [CrossRef]
- Perez, D.; Thalken, J.; Ughelu, N.; Knight, C.; Massey, W. Nowhere to Go: Parents’ Descriptions of Children’s Physical Activity During a Global Pandemic. Front. Public Health 2021, 9, 642932. [Google Scholar] [CrossRef]
- Orgilés, M.; Morales, A.; DelVecchio, E.; Mazzeschi, C.; Espada, J.P. Immediate Psychological Effects of the COVID-19 Quarantine in Youth from Italy and Spain. Front. Psychol. 2020, 11, 579038. [Google Scholar] [CrossRef]
- Siegle, C.B.H.; Pombo, A.; Luz, C.; Rodrigues, L.P.; Cordovil, R.; Sá, C.D.S.C.D. Influences of family and household characteristics on children’s level of physical activity during social distancing due to COVID-19 in brazil. Rev. Paul. de Pediatr. 2021, 39, e2020297. [Google Scholar] [CrossRef]
- Chambonniere, C.; Lambert, C.; Fearnbach, N.; Tardieu, M.; Fillon, A.; Genin, P.; Larras, B.; Melsens, P.; Bois, J.; Pereira, B.; et al. Effect of the COVID-19 lockdown on physical activity and sedentary behaviors in French children and adolescents: New results from the ONAPS national survey. Eur. J. Integr. Med. 2021, 43, 101308. [Google Scholar] [CrossRef]
- Tulchin-Francis, K.; Stevens, W.; Gu, X.; Zhang, T.; Roberts, H.; Keller, J.; Dempsey, D.; Borchard, J.; Jeans, K.; VanPelt, J. The impact of the coronavirus disease 2019 pandemic on physical activity in U.S. children. J. Sport Health Sci. 2021, 10, 323–332. [Google Scholar] [CrossRef]
- Dixon, M.A.; Hardie, A.; Warner, S.M.; Owiro, E.A.; Orek, D. Sport for Development and COVID-19: Responding to Change and Participant Needs. Front. Sports Act. Living 2020, 2, 590151. [Google Scholar] [CrossRef]
- Sciberras, E.; Patel, P.; Stokes, M.A.; Coghill, D.; Middeldorp, C.M.; Bellgrove, M.A.; Becker, S.P.; Efron, D.; Stringaris, A.; Faraone, S.V.; et al. Physical Health, Media Use, and Mental Health in Children and Adolescents with ADHD During the COVID-19 Pandemic in Australia. J. Atten. Disord. 2020. [Google Scholar] [CrossRef]
- López-Aymes, G.; Valadez, M.D.L.D.; Rodríguez-Naveiras, E.; Castellanos-Simons, D.; Aguirre, T.; Borges, A. A Mixed Methods Research Study of Parental Perception of Physical Activity and Quality of Life of Children Under Home Lock Down in the COVID-19 Pandemic. Front. Psychol. 2021, 12, 649481. [Google Scholar] [CrossRef]
- Zhang, X.; Zhu, W.; Kang, S.; Qiu, L.; Lu, Z.; Sun, Y. Association between Physical Activity and Mood States of Children and Adolescents in Social Isolation during the COVID-19 Epidemic. Int. J. Environ. Res. Public Health 2020, 17, 7666. [Google Scholar] [CrossRef]
- Elnaggar, R.K.; Alqahtani, B.A.; Mahmoud, W.S.; ElFakharany, M.S. Physical Activity in Adolescents During the Social Distancing Policies of the COVID-19 Pandemic. Asia Pac. J. Public Health 2020, 32, 491–494. [Google Scholar] [CrossRef] [PubMed]
- Kracht, C.; Katzmarzyk, P.; Staiano, A. Household chaos, family routines, and young child movement behaviors in the US during the COVID-19 outbreak: A cross-sectional study. BMC Public Health 2021, 21, 860. [Google Scholar] [CrossRef] [PubMed]
- Zenic, N.; Taiar, R.; Gilic, B.; Blazevic, M.; Maric, D.; Pojskic, H.; Sekulic, D. Levels and Changes of Physical Activity in Adolescents during the COVID-19 Pandemic: Contextualising Urban vs. Rural Living Environment. Appl. Sci. 2020, 10, 3997. [Google Scholar] [CrossRef]
- Vandermeerschen, H.; Vos, S.; Scheerder, J. Towards level playing fields? A time trend analysis of young people’s participation in club-organised sports. Int. Rev. Sociol. Sport 2014, 51, 468–484. [Google Scholar] [CrossRef]
- Bazett-Jones, D.M.; Garcia, M.C.; Taylor-Haas, J.A.; Long, J.T.; Rauh, M.J.; Paterno, M.V.; Ford, K.R. Impact of COVID-19 Social Distancing Restrictions on Training Habits, Injury, and Care Seeking Behavior in Youth Long-Distance Runners. Front. Sports Act. Living 2020, 2, 586141. [Google Scholar] [CrossRef]
- Beck, A.; Huang, J.; Lendzion, L.; Fernandez, A.; Martinez, S. Impact of the COVID-19 pandemic on parents’ perception of health behaviors in children with overweight and obesity. Acad. Pediatr. 2021, in press. [Google Scholar] [CrossRef]
- Dayton, J.D.; Ford, K.; Carroll, S.J.; Flynn, P.A.; Kourtidou, S.; Holzer, R.J. The Deconditioning Effect of the COVID-19 Pandemic on Unaffected Healthy Children. Pediatr. Cardiol. 2021, 42, 554–559. [Google Scholar] [CrossRef]
- de Matos, D.G.; Aidar, F.J.; de Almeida-Neto, P.F.; Moreira, O.C.; de Souza, R.F.; Marçal, A.C.; Marcucci-Barbosa, L.S.; Júnior, F.d.M.; Lobo, L.F.; Santos, J.L.d.; et al. The Impact of Measures Recommended by the Government to Limit the Spread of Coronavirus (COVID-19) on Physical Activity Levels, Quality of Life, and Mental Health of Brazilians. Sustainability 2020, 12, 9072. [Google Scholar] [CrossRef]
- Sá, C.D.S.C.D.; Pombo, A.; Luz, C.; Rodrigues, L.P.; Cordovil, R. COVID-19 Social Isolation in Brazil: Effects on the Physical Activity Routine of Families with Children. Rev. Paul. De Pediatr. 2021, 39, e2020159. [Google Scholar] [CrossRef] [PubMed]
- Dunton, G.; Do, B.; Wang, S. Early effects of the COVID-19 pandemic on physical activity and sedentary behavior in children living in the US. BMC Public Health 2020, 20, 1351. [Google Scholar] [CrossRef]
- Eyler, A.A.; Schmidt, L.; Kepper, M.; Mazzucca, S.; Gilbert, A.; Beck, A. Parent Perceptions of Changes in Child Physical Activity During COVID-19 Stay-At-Home Orders. Front. Public Health 2021, 9, 637151. [Google Scholar] [CrossRef]
- Garcia, J.M.; Lawrence, S.; Brazendale, K.; Leahy, N.; Fukuda, D. Brief report: The impact of the COVID-19 pandemic on health behaviors in adolescents with Autism Spectrum Disorder. Disabil. Health J. 2021, 14, 101021. [Google Scholar] [CrossRef]
- Hemphill, N.M.; Kuan, M.T.; Harris, K.C. Reduced Physical Activity During COVID-19 Pandemic in Children with Congenital Heart Disease. Can. J. Cardiol. 2020, 36, 1130–1134. [Google Scholar] [CrossRef]
- Malta, D.C.; Gomes, C.S.; Barros, M.B.D.A.; Lima, M.G.; da Silva, A.G.; Cardoso, L.S.D.M.; Werneck, A.O.; da Silva, D.R.P.; Ferreira, A.P.D.S.; Romero, D.E.; et al. The COVID-19 pandemic and changes in the lifestyles of Brazilian adolescents. Rev. Bras. Epidemiol. 2021, 24, e210012. [Google Scholar] [CrossRef]
- Pavlovic, A.; DeFina, L.F.; Natale, B.L.; Thiele, S.E.; Walker, T.J.; Craig, D.W.; Vint, G.R.; Leonard, D.; Haskell, W.L.; Kohl, H.W. Keeping children healthy during and after COVID-19 pandemic: Meeting youth physical activity needs. BMC Public Health 2021, 21, 1–8. [Google Scholar] [CrossRef]
- Wahl-Alexander, Z.; Camic, C.L. Impact of COVID-19 on School-Aged Male and Female Health-Related Fitness Markers. Pediatr. Exerc. Sci. 2021, 33, 61–64. [Google Scholar] [CrossRef]
- Androutsos, O.; Perperidi, M.; Georgiou, C.; Chouliaras, G. Lifestyle Changes and Determinants of Children’s and Adolescents’ Body Weight Increase during the First COVID-19 Lockdown in Greece: The COV-EAT Study. Nutrients 2021, 13, 930. [Google Scholar] [CrossRef]
- Chen, Y.; Osika, W.; Henriksson, G.; Dahlstrand, J.; Friberg, P. Impact of COVID-19 pandemic on mental health and health behaviors in Swedish adolescents. Scand. J. Public Health 2021. [Google Scholar] [CrossRef]
- Dauty, M.; Menu, P.; Fouasson-Chailloux, A. Effects of the COVID-19 confinement period on physical conditions in young elite soccer players. J. Sports Med. Phys. Fit. 2021, 61, 1252–1257. [Google Scholar] [CrossRef]
- Fillon, A.; Genin, P.; Larras, B.; Vanhelst, J.; Luiggi, M.; Aubert, S.; Verdot, C.; Rey, O.; Lhuisset, L.; Bois, J.; et al. France’s 2020 Report Card on Physical Activity and Sedentary Behaviors in Children and Youth: Results and Progression. J. Phys. Act. Health 2021, 18, 811–817. [Google Scholar] [CrossRef] [PubMed]
- Francisco, R.; Pedro, M.; DelVecchio, E.; Espada, J.P.; Morales, A.; Mazzeschi, C.; Orgilés, M. Psychological Symptoms and Behavioral Changes in Children and Adolescents During the Early Phase of COVID-19 Quarantine in Three European Countries. Front. Psychiatry 2020, 11, 570164. [Google Scholar] [CrossRef] [PubMed]
- Jurak, G.; Morrison, S.A.; Kovač, M.; Leskošek, B.; Sember, V.; Strel, J.; Starc, G. A COVID-19 Crisis in Child Physical Fitness: Creating a Barometric Tool of Public Health Engagement for the Republic of Slovenia. Front. Public Health 2021, 9, 644235. [Google Scholar] [CrossRef] [PubMed]
- López-Bueno, R.; López-Sánchez, G.F.; Casajús, J.A.; Calatayud, J.; Gil-Salmerón, A.; Grabovac, I.; Tully, M.A.; Smith, L. Health-Related Behaviors Among School-Aged Children and Adolescents During the Spanish COVID-19 Confinement. Front. Pediatr. 2020, 8, 573. [Google Scholar] [CrossRef]
- Pietrobelli, A.; Pecoraro, L.; Ferruzzi, A.; Heo, M.; Faith, M.; Zoller, T.; Antoniazzi, F.; Piacentini, G.; Fearnbach, S.N.; Heymsfield, S.B. Effects of COVID-19 Lockdown on Lifestyle Behaviors in Children with Obesity Living in Verona, Italy: A Longitudinal Study. Obesity 2020, 28, 1382–1385. [Google Scholar] [CrossRef] [PubMed]
- Pombo, A.; Luz, C.; Rodrigues, L.P.; Cordovil, R. Effects of COVID-19 Confinement on the Household Routines of Children in Portugal. J. Child Fam. Stud. 2021, 30, 1664–1674. [Google Scholar] [CrossRef]
- Pombo, A.; Luz, C.; Rodrigues, L.; Ferreira, C.; Cordovil, R. Correlates of children’s physical activity during the COVID-19 confinement in Portugal. Public Health 2020, 189, 14–19. [Google Scholar] [CrossRef]
- Siachpazidou, D.; Kotsiou, O.; Chatziparasidis, G.; Papagiannis, D.; Vavougios, G.; Gogou, E.; Stavrou, V.; Gourgoulianis, K. Action and Reaction of Pre-Primary and Primary School-Age Children to Restrictions during COVID-19 Pandemic in Greece. J. Pers. Med. 2021, 11, 451. [Google Scholar] [CrossRef]
- Szabó, T.; Stocker, M.; Ács, P.; Morvay-Sey, K.; Pálvölgyi, A.; Laczkó, T. Impact of COVID-19 on the physical activity and well-being of hungarian athletes and sports professionals. Health Probl. Civiliz. 2020, 14, 165–173. [Google Scholar] [CrossRef]
- ten Velde, G.; Lubrecht, J.; Arayess, L.; van Loo, C.; Hesselink, M.; Reijnders, D.; Vreugdenhil, A. Physical activity behaviour and screen time in Dutch children during the COVID-19 pandemic: Pre-, during- and post-school closures. Pediatr. Obes. 2021, 16, e12779. [Google Scholar] [CrossRef]
- Versloot, O.; van der Net, J.; Fischer, K. Sports participation of patients with haemophilia in the COVID-19 era: The Dutch experience. Haemophilia 2020, 27, e295–e297. [Google Scholar] [CrossRef] [PubMed]
- Zorcec, T.; Jakovska, T.; Micevska, V.; Boskovska, K.; Cholakovska, V.C. Pandemic with COVID-19 and Families with Children with Chronic Respiratory Diseases. PRILOZI 2020, 41, 95–101. [Google Scholar] [CrossRef]
- Guo, Y.-F.; Liao, M.-Q.; Cai, W.-L.; Yu, X.-X.; Li, S.-N.; Ke, X.-Y.; Tan, S.-X.; Luo, Z.-Y.; Cui, Y.-F.; Wang, Q.; et al. Physical activity, screen exposure and sleep among students during the pandemic of COVID-19. Sci. Rep. 2021, 11, 1–11. [Google Scholar] [CrossRef]
- Jia, P.; Zhang, L.; Yu, W.; Yu, B.; Liu, M.; Zhang, D.; Yang, S. Impact of COVID-19 lockdown on activity patterns and weight status among youths in China: The COVID-19 Impact on Lifestyle Change Survey (COINLICS). Int. J. Obes. 2020, 45, 695–699. [Google Scholar] [CrossRef]
- Xiang, M.; Zhang, Z.; Kuwahara, K. Impact of COVID-19 pandemic on children and adolescents’ lifestyle behavior larger than expected. Prog. Cardiovasc. Dis. 2020, 63, 531–532. [Google Scholar] [CrossRef]
- Yang, S.; Guo, B.; Ao, L.; Yang, C.; Zhang, L.; Zhou, J.; Jia, P. Obesity and activity patterns before and during COVID-19 lockdown among youths in China. Clin. Obes. 2020, 10, e12416. [Google Scholar] [CrossRef] [PubMed]
- Zhou, J.; Xie, X.; Guo, B.; Pei, R.; Pei, X.; Yang, S.; Jia, P. Impact of COVID-19 Lockdown on Physical Activity Among the Chinese Youths: The COVID-19 Impact on Lifestyle Change Survey (COINLICS). Front. Public Health 2021, 9, 592795. [Google Scholar] [CrossRef]
- Abid, R.; Ammar, A.; Maaloul, R.; Souissi, N.; Hammouda, O. Effect of COVID-19-Related Home Confinement on Sleep Quality, Screen Time and Physical Activity in Tunisian Boys and Girls: A Survey. Int. J. Environ. Res. Public Health 2021, 18, 3065. [Google Scholar] [CrossRef] [PubMed]
- Elliott, S.; Drummond, M.J.; Prichard, I.; Eime, R.; Drummond, C.; Mason, R. Understanding the impact of COVID-19 on youth sport in Australia and consequences for future participation and retention. BMC Public Health 2021, 21, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Masi, A.; Diaz, A.M.; Tully, L.; Azim, S.I.; Woolfenden, S.; Efron, D.; Eapen, V. Impact of the COVID-19 pandemic on the well-being of children with neurodevelopmental disabilities and their parents. J. Paediatr. Child Health 2021, 57, 631–636. [Google Scholar] [CrossRef]
- Munasinghe, S.; Sperandei, S.; Freebairn, L.; Conroy, E.; Jani, H.; Marjanovic, S.; Page, A. The Impact of Physical Distancing Policies During the COVID-19 Pandemic on Health and Well-Being Among Australian Adolescents. J. Adolesc. Health 2020, 67, 653–661. [Google Scholar] [CrossRef] [PubMed]
- Reece, L.; Owen, K.; Foley, B.; Rose, C.; Bellew, B.; Bauman, A. Understanding the impact of COVID-19 on children’s physical activity levels in NSW, Australia. Health Promot. J. Aust. 2020, 32, 365–366. [Google Scholar] [CrossRef] [PubMed]
- Guan, H.; Okely, A.D.; Aguilar-Farias, N.; Cruz, B.D.P.; Draper, C.E.; Hamdouchi, A.E.; Florindo, A.A.; Jáuregui, A.; Katzmarzyk, P.T.; Kontsevaya, A.; et al. Promoting healthy movement behaviours among children during the COVID-19 pandemic. Lancet Child Adolesc. Health 2020, 4, 416–418. [Google Scholar] [CrossRef]
- López-Gil, J.; Tremblay, M.; Brazo-Sayavera, J. Changes in Healthy Behaviors and Meeting 24-h Movement Guidelines in Spanish and Brazilian Preschoolers, Children and Adolescents during the COVID-19 Lockdown. Children 2021, 8, 83. [Google Scholar] [CrossRef]
| Change of PA Identified | Min | Max | No. of Studies |
|---|---|---|---|
| Decrease | −45 min/day [33] | −91 min/day [34] | 57 |
| Increase | - | +53 min/day [17] | 4 |
| No change | - | - | 6 |
| Mixed results | - | - | 8 |
| Level | Facilitating Factor | No. of Studies |
|---|---|---|
| Individual level | Prior fitness status | 4 |
| Male gender | 3 | |
| Taking part in online PE classes | 3 | |
| Following a daily routine | 2 | |
| Spending time on outdoor PA | 2 | |
| More time available | 1 | |
| No school | 1 | |
| Use of digital platforms | 1 | |
| Health-related quality of life | 1 | |
| Context level | Size of outdoor space available | 4 |
| More than one child | 3 | |
| Parental encouragement and support | 3 | |
| Household income | 2 | |
| Higher parental education | 1 | |
| Perceived parental capability | 1 | |
| Living in a house | 1 | |
| Low dwelling density | 1 | |
| Access to parks | 1 | |
| Parental engagement in PA | 1 | |
| Family dog ownership | 1 | |
| Family coexistence | 1 |
| Level | Constraining Factor | No. of Studies |
|---|---|---|
| Individual level | Child’s age | 6 |
| Feelings of stress | 2 | |
| Feeling comfortable at home | 1 | |
| Having a migration background | 1 | |
| Lower socioeconomic status | 1 | |
| Change to routines | 1 | |
| Pre-COVID sedentary time | 1 | |
| Pre-COVID activity levels | 1 | |
| Mood states | 1 | |
| Context level | Caregiver’s level of education | 3 |
| Family conflict | 2 | |
| Restrictions from COVID-19 | 2 | |
| Urban environment | 2 | |
| Living in an apartment | 1 | |
| Parent’s age | 1 | |
| Parent’s marital status | 1 | |
| Lack of playmates | 1 | |
| No outdoor space available | 1 | |
| Level of parent’s stress | 1 | |
| Lack of supervision | 1 | |
| Proximity to major roads | 1 | |
| Club training cancellation | 1 | |
| Enrolment in an early education center | 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rossi, L.; Behme, N.; Breuer, C. Physical Activity of Children and Adolescents during the COVID-19 Pandemic—A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 11440. https://doi.org/10.3390/ijerph182111440
Rossi L, Behme N, Breuer C. Physical Activity of Children and Adolescents during the COVID-19 Pandemic—A Scoping Review. International Journal of Environmental Research and Public Health. 2021; 18(21):11440. https://doi.org/10.3390/ijerph182111440
Chicago/Turabian StyleRossi, Lea, Nick Behme, and Christoph Breuer. 2021. "Physical Activity of Children and Adolescents during the COVID-19 Pandemic—A Scoping Review" International Journal of Environmental Research and Public Health 18, no. 21: 11440. https://doi.org/10.3390/ijerph182111440
APA StyleRossi, L., Behme, N., & Breuer, C. (2021). Physical Activity of Children and Adolescents during the COVID-19 Pandemic—A Scoping Review. International Journal of Environmental Research and Public Health, 18(21), 11440. https://doi.org/10.3390/ijerph182111440






