3.1. Overview of the Samples
A total of 200 respondents participated in the survey in Italy, while 296 respondents participated in Australia. As shown in
Table 1, the caregivers participating in the study were mostly between the ages of 40 and 49 in both Italy (53.0%) and Australia (54.8%). The mean age of the participants’ children was 10.7 and 10.1, in Italy and Australia, respectively, with the majority of the children male in both Italy (81.5%) and Australia (65.9%). In Australia, a higher percentage of caregivers had higher education compared to Italy (68.8% vs. 19.5%).
Table 2 provides an overview of the NDD groups. In Italy, the most common NDDs were Tourette’s syndrome (TS) (54.5%), Autism Spectrum Disorder (ASD) (51.0%) and Intellectual or Learning Disorder (ILD) (37.5%). In Australia, the most common NDDs were ASD (61.3%), ADHD (40.7%) and Anxiety Disorder (33.7%). Parents were also asked whether there were any symptomatic changes in their children during the pandemic. Although significant differences in the symptomatic changes were observed between Italy and Australia across all NDD groups, at least half of the respondents in both Italy and Australia experienced worsening of the symptoms in children with ADHD (50.0% vs. 58.7%), Anxiety Disorder (50.0% vs. 68.0%), OCD (51.4% vs. 51.6%) and TS (52.3% vs. 64.3%). In Australia, children with ASD were perceived to have increased symptoms (58.0%) compared to children in Italy (37.3%). Less than half of the respondents in both Italy and Australia experienced worsening of the symptoms in children with ILD (42.7% vs. 37.5%).
The K6 scores of the parents are presented in
Table 3. On average, parents in Italy showed significantly higher distress levels compared to parents in Australia. For example, 36.0% of the respondents reported being nervous most or all of the time in Italy, whereas only 20.3% felt the same way in Australia. Similarly, 26.0% of parents in Italy reported that most or all of the time they felt so depressed that nothing could cheer them, while only 9.1% felt the same way in Australia. However, when asked “how often did you feel that everything was an effort?”, a greater percentage felt that way most or all the time in Australia, 25.7%, compared to only 20.0% of parents in Italy.
The following results can be found in the
Supplementary Materials. More than half of the participants in both Italy and Australia somewhat or strongly agreed that their child’s overall health and wellbeing had been impacted by the pandemic with 58.5% and 69.4%, respectively. However, just under half (45.5%) believed the pandemic had worsened preexisting health conditions for their child in Italy, with half of the respondents feeling the same way in Australia.
With regards to support networks, caregivers in Australia were impacted more than those in Italy. For example, 77.4% of respondents felt their support networks had decreased compared to 53.0% in Italy. Similarly, 71.8% felt that the pandemic had disrupted caregivers’ support and services in Australia, whereas only 44.89% felt the same way in Italy. Almost three-quarters of the respondents in Italy and Australia, 74.3% and 72.2%, respectively, felt that the pandemic has significantly disrupted the allied health services their child accessed. Most of the respondents in Australia (97.1%) stated that their children took more medication than normal. In Italy, a smaller proportion (29.2%) of caregivers felt that their child’s ability to access specialists had been significantly impacted by the pandemic compared to a much larger proportion of caregivers in Australia (70.5%).
With regards to contributors to overall family health, caregivers in Australia were more impacted than those in Italy with 92.9% stating that COVID had significantly disrupted their child’s routines compared to 69.0% in Italy. Similarly, 75.5% indicated that during the past two weeks, COVID restrictions had been stressful for their child compared to 47.0% in Italy. Moreover, when asked about balancing work with childcare and family responsibilities, the majority (80.9%) of caregivers in Australia reported it had been difficult, whereas less than half (40.0%), felt the same way in Italy. Nearly all the respondents in Italy were optimistic the COVID crisis would end soon (94.5%) with just under three-quarters (73.2%) feeling the same in Australia.
The pandemic had a significant impact on the children’s education in both Italy and Australia, with respondents stating that COVID-19 had prevented their child from attending school with 90.3% and 91.1%, respectively. Although most of the respondents had adequate access to online resources, fewer than half in both Italy (47.5%) and Australia (44.4%) felt their child had adequate capacity to engage in home-based learning. Interestingly, the majority of caregivers in Italy (79.9%) felt that they had adequate capacity to support their child’s educational needs, whereas less than half (46.4%) felt the same way in Australia.
A proportion of caregivers in Italy reported a reduction in sleep quality in their children (18.7%) compared to almost half (46.9%) of caregivers in Australia. In both Italy and Australia, more than half of the respondents reported that their child had become more easily annoyed since the start of the pandemic (Italy: 60.6% vs. Australia 65.2%). Moreover, the majority of the parents reported that their children spent more screen time and played significantly more video games since the outbreak (Italy: 58.7% vs. Australia 65.4%).
3.2. Impact of Diagnoses of Children on Parental Distress
The results from the linear regression analysis in Australia (
Table 4) show the diagnosis of ILD in children is significantly positively correlated with parental distress after adjusting for the other NDDs, the child’s age, the caregivers’ age and education level. Interestingly, parents with children diagnosed with TS were significantly inversely correlated with parental distress levels during the pandemic after adjusting for the same confounders. Although there were no significant associations between NDDs and parental distress in Italy, children with ASD showed a positive correlation with parental distress. When merging the two datasets together, it became apparent that ILD could be a major contributor to parental distress during the pandemic (
B = −1.2654,
p = 0.038). However, children diagnosed with TS were inversely correlated with parental distress (
B = 2.7612,
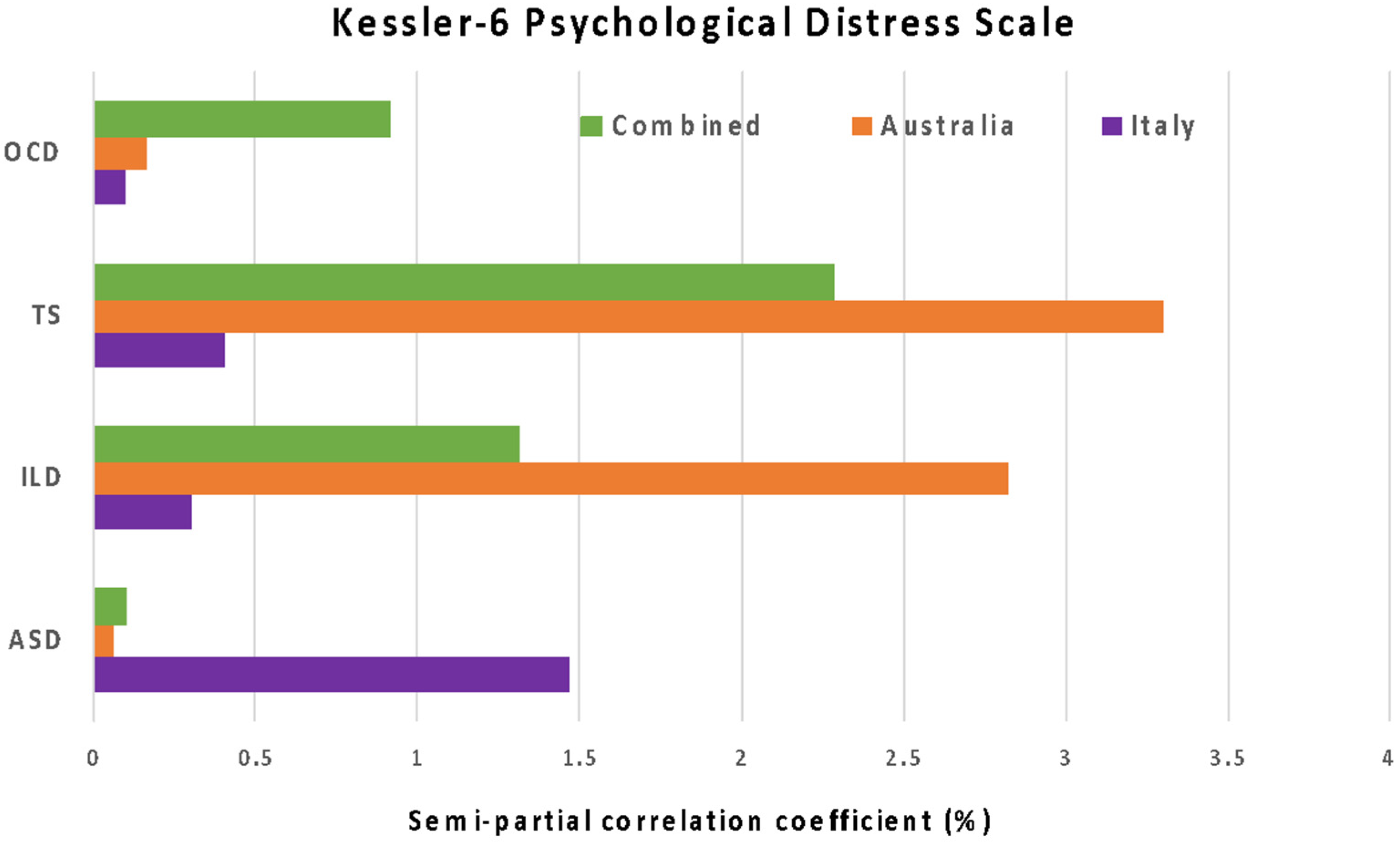
p < 0.005). The proportion in the K6 score explained by each diagnosis of the child in each country is shown in
Figure 1. The results indicate that, among all diagnoses, the largest contributor to parental stress in Australia was TS, while the largest contributor to parental stress in Italy was ASD.
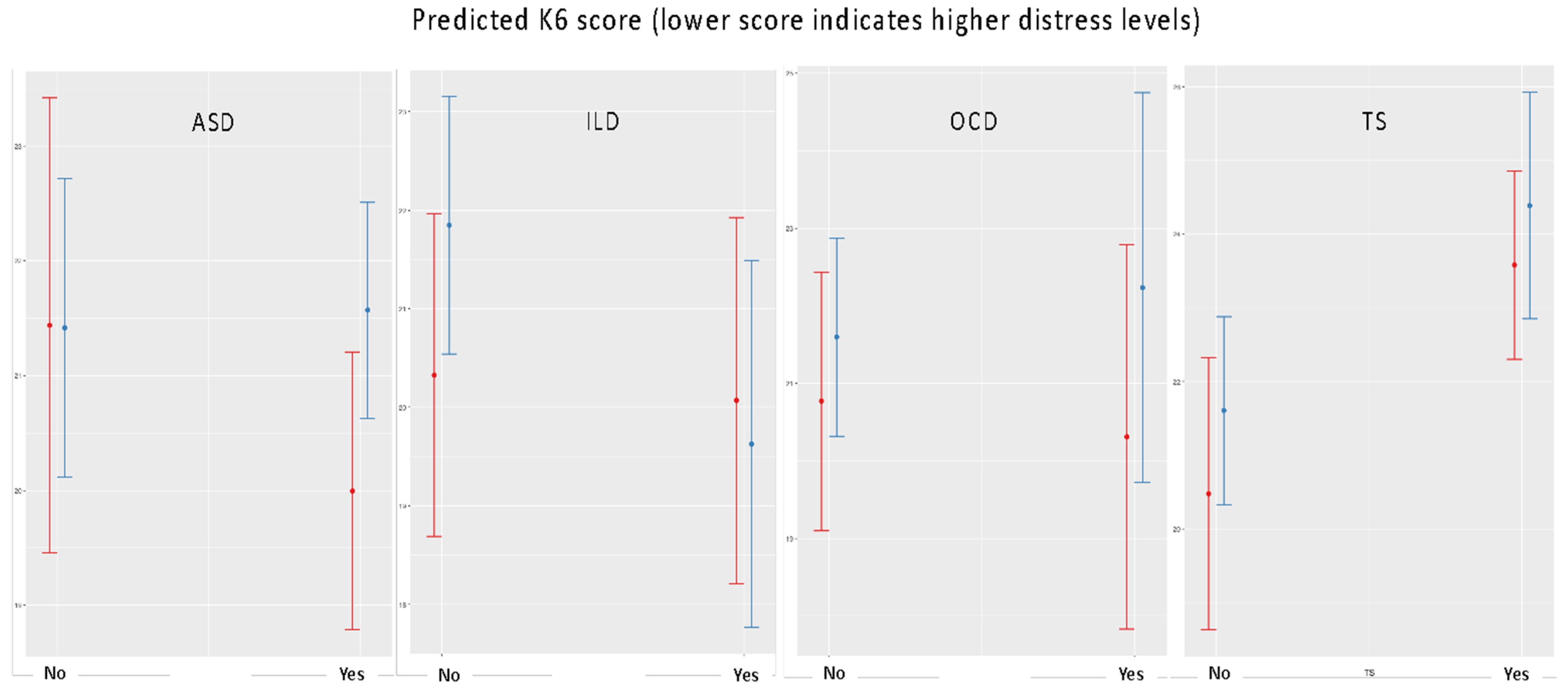
Figure 2 provides an overview of the interaction plots which illustrates how Italian and Australian parents experienced different levels of stress during the pandemic by the following child diagnoses: ASD, TS, ILD and OCD. The results confirm the earlier analyses that children diagnosed with TS showed lower parental distress levels compared to those without the diagnosis. There was no significant difference between Australia and Italy regarding the impact of NDDs on parental distress (
Table 5).
In Italy, higher parental distress levels were significantly associated with the worsening of the symptomatic changes in children with ILD, OCD and TS—which is also shown in
Table 6. In Australia, only worsening of the symptoms in ASD or ILD was associated with increased parental distress levels, while worsening of symptoms in OCD and TS did not statistically significantly correlate with parental distress levels. These results imply that the impact of symptomatic changes in OCD or TS on parental distress might vary by country during the pandemic. However, none of the interaction effects between the diagnosis-specific symptomatic changes and the country on parental distress reached statistical significance levels (
Table 7).
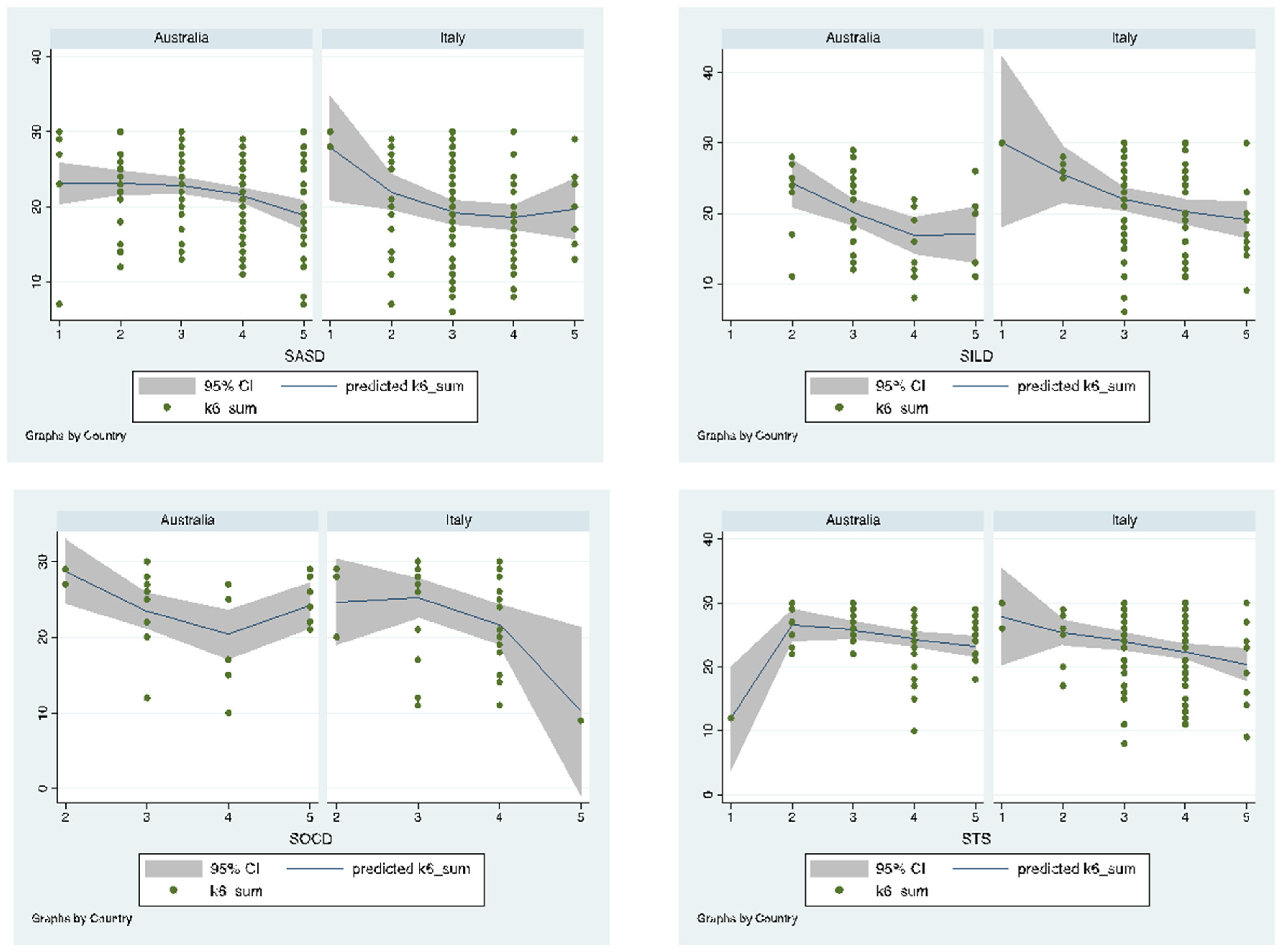
Figure 3 shows the results of the effect of diagnosis-specific symptomatic change and its effect on parental distress.