Menthol Smoking and Nicotine Dependence among Black/African American Women Smokers Living in Low-Resource, Rural Communities
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Setting
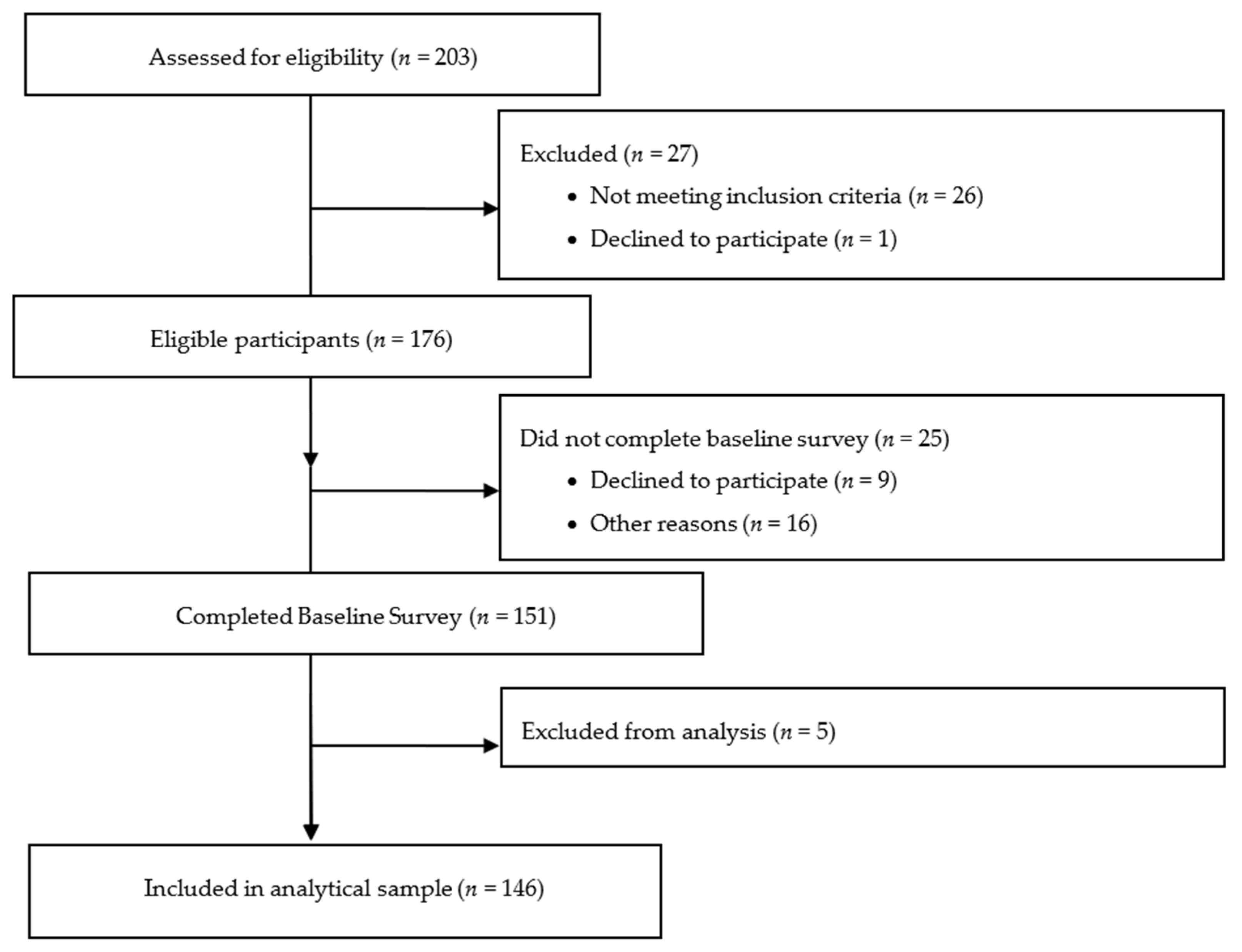
2.2. Sampling, Eligibility, and Recruitment
2.3. Procedures for Survey Administration
2.4. Measures
2.4.1. Sociodemographic Characteristics
2.4.2. Tobacco Use Characteristics
Menthol Cigarette Smoking Status
Cigarette Smoker Characteristics
Menthol LCC Smoking Status
LCC Smoker Characteristics
Composite of Any Current/Past 30-Day Menthol Smoking Status
2.4.3. Other Substance Use Characteristics
2.4.4. Socioeconomic Deprivation Measures
2.4.5. Outcome Variables
Nicotine Dependence
Quitting Behaviors
2.5. Sample and Analysis
3. Results
3.1. Menthol Cigarette Use among Black/African American Women Who Currently Smoke Cigarettes and/or LCCs
3.2. Sociodemographic Characteristics of Black/African American Women Smokers by Menthol Smoking Status
3.3. Tobacco and Other Substance Use Characteristics
3.4. Multivariable Linear and Logistic Regression Predicting Time to First Tobacco Product Use, FTND Score, and Ever Attempting to Quit Cigarettes from Menthol Smoking Status
3.5. Socioeconomic Deprivation by Time to First Tobacco Product Use, Time to First Cigarette Use, and FTND Score
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- DeSantis, C.E.; Miller, K.D.; Goding Sauer, A.; Jemal, A.; Siegel, R.L. Cancer statistics for African Americans, 2019. CA Cancer J. Clin. 2019, 69, 211–233. [Google Scholar] [CrossRef]
- National Cancer Institute. State Cancer Profiles. Available online: https://statecancerprofiles.cancer.gov/index.html (accessed on 23 April 2021).
- Arkansas Department of Public Health, Chronic Disease Epidemiology Section, Epidemiology Branch, Center for Public Health Practice, Tobacco Prevention and Cessation Program, Center for Health Advancement. Tobacco Data Deck. 2018. Available online: https://www.healthy.arkansas.gov/images/uploads/pdf/Tobacco_Data_Deck_June_2018.pdf (accessed on 25 April 2021).
- American Lung Association. Tobacco Use in Racial and Ethnic Populations. Available online: https://www.lung.org/quit-smoking/smoking-facts/impact-of-tobacco-use/tobacco-use-racial-and-ethnic (accessed on 25 April 2021).
- Truth Initiative. Tobacco Nation: An Ongoing Crisis—Examining the Health and Policy Disparities of U.S. States with the Highest Smoking Rates. Available online: https://truthinitiative.org/sites/default/files/media/files/2019/06/Tobacco-Nation-An-Ongoing-Crisis.pdf (accessed on 25 April 2021).
- Institute for Women’s Policy Research. Status of Women in the States-Arkansas. Available online: https://statusofwomendata.org/explore-the-data/state-data/arkansas/ (accessed on 25 April 2021).
- Cornelius, M.E.; Wang, T.W.; Jamal, A.; Loretan, C.G.; Neff, L.J. Tobacco Product Use Among Adults—United States, 2019. Morb. Mortal. Wkly. Rep. 2020, 69, 1736–1742. [Google Scholar] [CrossRef]
- Barbeau, E.M.; Krieger, N.; Soobader, M.J. Working class matters: Socioeconomic disadvantage, race/ethnicity, gender, and smoking in NHIS 2000. Am. J. Public Health 2004, 94, 269–278. [Google Scholar] [CrossRef]
- Singh, G.K.; Jemal, A. Socioeconomic and Racial/Ethnic Disparities in Cancer Mortality, Incidence, and Survival in the United States, 1950–2014: Over Six Decades of Changing Patterns and Widening Inequalities. J. Environ. Public Health 2017, 2017, 2819372. [Google Scholar] [CrossRef]
- Lawrence, D.; Rose, A.; Fagan, P.; Moolchan, E.T.; Gibson, J.T.; Backinger, C.L. National patterns and correlates of mentholated cigarette use in the United States. Addiction 2010, 105, 13–31. [Google Scholar] [CrossRef] [PubMed]
- Substance Abuse and Mental Health Services Administration. Substance Abuse and Mental Health Services Administration (SAMHSA)’s Public Online Data Analysis System (PDAS) National Survey on Drug Use and Health. 2019. Available online: https://pdas.samhsa.gov/#/survey/NSDUH-2019-DS0001 (accessed on 5 September 2021).
- Christiansen, B.; Reeder, K.; Hill, M.; Baker, T.B.; Fiore, M.C. Barriers to Effective Tobacco-Dependence Treatment for the Very Poor. J. Stud. Alcohol Drugs 2012, 73, 874–884. [Google Scholar] [CrossRef] [PubMed]
- Tobacco Products Scientific Advisory Committee. Menthol Cigarettes and Public Health: Review of the Scientific Evidence and Recommendations; U.S. Department of Health and Human Services, Food and Drug Administration: Rockville, MD, USA, 2011. [Google Scholar]
- Muscat, J.E.; Liu, H.-P.; Stellman, S.D.; Richie, J.P., Jr. Menthol smoking in relation to time to first cigarette and cotinine: Results from a community-based study. Regul. Toxicol. Pharmacol. 2012, 63, 166–170. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. Menthol and Other Flavors in Tobacco Products. Available online: https://www.fda.gov/tobacco-products/products-ingredients-components/menthol-and-other-flavors-tobacco-products (accessed on 5 September 2021).
- Kuiper, N.M.; Gammon, D.; Loomis, B.; Falvey, K.; Wang, T.W.; King, B.A.; Rogers, T. Trends in Sales of Flavored and Menthol Tobacco Products in the United States During 2011–2015. Nicotine Tob. Res. 2018, 20, 698–706. [Google Scholar] [CrossRef]
- Mattingly, D.T.; Hirschtick, J.L.; Meza, R.; Fleischer, N.L. Trends in prevalence and sociodemographic and geographic patterns of current menthol cigarette use among U.S. adults, 2005–2015. Prev. Med. Rep. 2020, 20, 101227. [Google Scholar] [CrossRef] [PubMed]
- U.S. Food and Drug Administration. Preliminary Scientific Evaluation of the Possible Public Health Effects of Menthol versus Nonmenthol Cigarettes. Available online: https://www.fda.gov/media/86497/download (accessed on 24 April 2021).
- Ahijevych, K.; Wewers, M.E. Factors associated with nicotine dependence among African American women cigarette smokers. Res. Nurs. Health 1993, 16, 283–292. [Google Scholar] [CrossRef]
- Rosenbloom, J.; Rees, V.W.; Reid, K.; Wong, J.; Kinnunen, T. A cross-sectional study on tobacco use and dependence among women: Does menthol matter? Tob. Induc. Dis. 2012, 10, 19. [Google Scholar] [CrossRef] [PubMed]
- Sterling, K.; Fryer, C.; Pagano, I.; Jones, D.; Fagan, P. Association between menthol-flavoured cigarette smoking and flavoured little cigar and cigarillo use among African-American, Hispanic, and white young and middle-aged adult smokers. Tob. Control. 2016, 25, ii21–ii31. [Google Scholar] [CrossRef] [PubMed]
- Sterling, K.; Berg, C.J.; Thomas, A.N.; Glantz, S.A.; Ahluwalia, J.S. Factors Associated with Small Cigar Use Among College Students. Am. J. Health Behav. 2013, 37, 325–333. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sterling, K.L.; Fryer, C.S.; Pagano, I.; Fagan, P. Little Cigars and Cigarillos Use Among Young Adult Cigarette Smokers in the United States: Understanding Risk of Concomitant Use Subtypes. Nicotine Tob. Res. 2016, 18, 2234–2242. [Google Scholar] [CrossRef]
- Cohn, A.; Cobb, C.O.; Niaura, R.S.; Richardson, A. The Other Combustible Products: Prevalence and Correlates of Little Cigar/Cigarillo Use Among Cigarette Smokers. Nicotine Tob. Res. 2015, 17, 1473–1481. [Google Scholar] [CrossRef]
- Spears, C.A.; Jones, D.M.; Pechacek, T.F.; Ashley, D.L. Use of other combustible tobacco products among priority populations of smokers: Implications for U.S. tobacco regulatory policy. Addict. Behav. 2019, 93, 194–197. [Google Scholar] [CrossRef]
- Baker, F.; Ainsworth, S.R.; Dye, J.T.; Crammer, C.; Thun, M.J.; Hoffmann, D.; Repace, J.L.; Henningfield, J.E.; Slade, J.; Pinney, J.; et al. Health risks associated with cigar smoking. JAMA 2000, 284, 735–740. [Google Scholar] [CrossRef]
- National Cancer Institute. Cigars: Health Effects and Trends Smoking; U.S. Department of Health and Human Services, National Institutes of Health, National Cancer Institute: Bethesda, MD, USA, 1998. [Google Scholar]
- County Health Rankings: Arkansas. Available online: https://www.countyhealthrankings.org/app/arkansas/2021/rankings/outcomes/overall (accessed on 24 April 2021).
- American Community Survey. Quick Facts Phillips County, Arkansas; Lee County, Arkansas; Arkansas. Available online: https://www.census.gov/quickfacts/fact/table/phillipscountyarkansas,leecountyarkansas,AR# (accessed on 25 April 2021).
- Biddle, J.; Louie, S.; Simmons, L.; Sharma, R.; Al-Mousawi, H.; Smith, M.R.; Porter, A. Red County: County Life Expectancy Profile 2017; Office of Minority Health and Health Disparities, Arkansas Department of Health, Arkansas Minority Health Commission: Little Rock, AR, USA, 2018. [Google Scholar]
- Feeding America. State-By-State Resource: The Impact of Coronavirus on Food Insecurity. Available online: https://feedingamericaaction.org/resources/state-by-state-resource-the-impact-of-coronavirus-on-food-insecurity/ (accessed on 29 April 2021).
- Jager, J.; Putnick, D.L.; Bornstein, M.H., II. More Than Just Convenient: The Scientific Merits of Homogenous Convenience Samples. Monogr. Soc. Res. Child. Dev. 2017, 82, 13–30. [Google Scholar] [CrossRef]
- Bornstein, M.H.; Jager, J.; Putnick, D.L. Sampling in developmental science: Situations, shortcomings, solutions, and standards. Dev. Rev. 2013, 33, 357–370. [Google Scholar] [CrossRef]
- Crosby, R.A.; Salazar, L.F.; Diclemente, R.J.; Lang, D.L. Balancing rigor against the inherent limitations of investigating hard-to-reach populations. Health Educ. Res. 2010, 25, 1–5. [Google Scholar] [CrossRef]
- Bonevski, B.; Randell, M.; Paul, C.; Chapman, K.; Twyman, L.; Bryant, J.; Brozek, I.; Hughes, C. Reaching the hard-to-reach: A systematic review of strategies for improving health and medical research with socially disadvantaged groups. BMC Med. Res. Methodol. 2014, 14, 42. [Google Scholar] [CrossRef]
- Heatherton, T.F.; Kozlowski, L.T.; Frecker, R.C.; Fagerstrom, K.O. The Fagerstrom Test for Nicotine Dependence: A revision of the Fagerstrom Tolerance Questionnaire. Br. J. Addict. 1991, 86, 1119–1127. [Google Scholar] [CrossRef]
- Baker, T.B.; Piper, M.E.; McCarthy, D.E.; Bolt, D.M.; Smith, S.S.; Kim, S.-Y.; Colby, S.; Conti, D.; Giovino, G.A.; Hatsukami, D.; et al. Time to first cigarette in the morning as an index of ability to quit smoking: Implications for nicotine dependence. Nicotine Tob. Res. 2007, 9, S555–S570. [Google Scholar] [CrossRef]
- Ahijevych, K.; Garrett, B.E. The role of menthol in cigarettes as a reinforcer of smoking behavior. Nicotine Tob. Res. 2010, 12, S110–S116. [Google Scholar] [CrossRef]
- Okuyemi, K.S.; Ahluwalia, J.S.; Ebersole-Robinson, M.; Catley, D.; Mayo, M.S.; Resnicow, K. Does menthol attenuate the effect of bupropion among African American smokers? Addiction 2003, 98, 1387–1393. [Google Scholar] [CrossRef]
- Muscat, J.E.; Chen, G.; Knipe, A.; Stellman, S.D.; Lazarus, P.; Richie, J.P. Effects of Menthol on Tobacco Smoke Exposure, Nicotine Dependence, and NNAL Glucuronidation. Cancer Epidemiol. Prev. Biomark. 2009, 18, 35–41. [Google Scholar] [CrossRef]
- Collins, C.C.; Moolchan, E.T. Shorter time to first cigarette of the day in menthol adolescent cigarette smokers. Addict. Behav. 2006, 31, 1460–1464. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.S.; Fiore, M.C.; Baker, T.B. Smoking cessation in smokers who smoke menthol and non-menthol cigarettes. Addiction 2014, 109, 2107–2117. [Google Scholar] [CrossRef] [PubMed]
- Fagan, P.; Moolchan, E.T.; Hart, A., Jr.; Rose, A.; Lawrence, D.; Shavers, V.L.; Gibson, J.T. Nicotine dependence and quitting behaviors among menthol and non-menthol smokers with similar consumptive patterns. Addiction 2010, 105, 55–74. [Google Scholar] [CrossRef] [PubMed]
- St. Helen, G.; Benowitz, N.L.; Ahluwalia, J.S.; Tyndale, R.F.; Addo, N.; Gregorich, S.E.; Pérez-Stable, E.J.; Lisa Sanderson, C. Black Light Smokers: How Nicotine Intake and Carcinogen Exposure Differ Across Various Biobehavioral Factors. J. Natl. Med. Assoc. 2019, 111, 509–520. [Google Scholar] [CrossRef] [PubMed]
- Chen, A.; Machiorlatti, M.; Krebs, N.M.; Muscat, J.E. Socioeconomic differences in nicotine exposure and dependence in adult daily smokers. BMC Public Health 2019, 19, 375. [Google Scholar] [CrossRef]
- Siahpush, M. Socioeconomic variations in nicotine dependence, self-efficacy, and intention to quit across four countries: Findings from the International Tobacco Control (ITC) Four Country Survey. Tob. Control. 2006, 15, iii71–iii75. [Google Scholar] [CrossRef] [PubMed]
- Branstetter, S.A.; Mercincavage, M.; Muscat, J.E. Predictors of the Nicotine Dependence Behavior Time to the First Cigarette in a Multiracial Cohort. Nicotine Tob. Res. 2015, 17, 819–824. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Leeman, R.F.; O’Malley, S.S.; White, M.A.; McKee, S.A. Nicotine and food deprivation decrease the ability to resist smoking. Psychopharmacology 2010, 212, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Adams, G.B. An Empirical Analysis of the Association Between Cigarette Smoking and Participation in the Supplemental Nutrition Assistance Program. Am. J. Health Promot. 2016, 32, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Lund, M. Social Inequality in Cigarette Consumption, Cigarette Dependence, and Intention to Quit among Norwegian Smokers. BioMed Res. Int. 2015, 2015, 835080. [Google Scholar] [CrossRef][Green Version]
- Rath, J.M.; Villanti, A.C.; Williams, V.F.; Richardson, A.; Pearson, J.L.; Vallone, D.M. Correlates of current menthol cigarette and flavored other tobacco product use among U.S. young adults. Addict. Behav. 2016, 62, 35–41. [Google Scholar] [CrossRef]
- Glasser, A.M.; Johnson, A.L.; Rose, S.W.; Ganz, O.; Cantrell, J.; Delnevo, C.; Villanti, A.C. Correlates of Cigar Use by Type and Flavor among US Young Adults: 2011–2015. Tob. Regul. Sci. 2017, 3, 59–71. [Google Scholar] [CrossRef]
- Villanti, A.C.; Mowery, P.D.; Delnevo, C.D.; Niaura, R.S.; Abrams, D.B.; Giovino, G.A. Changes in the prevalence and correlates of menthol cigarette use in the USA, 2004–2014. Tob. Control. 2016, 25, ii14. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. FDA Commits to Evidence-Based Actions Aimed at Saving Lives and Preventing Future Generations of Smokers. Available online: https://www.fda.gov/news-events/press-announcements/fda-commits-evidence-based-actions-aimed-saving-lives-and-preventing-future-generations-smokers (accessed on 29 April 2021).
- Cadham, C.J.; Sanchez-Romero, L.M.; Fleischer, N.L.; Mistry, R.; Hirschtick, J.L.; Meza, R.; Levy, D.T. The actual and anticipated effects of a menthol cigarette ban: A scoping review. BMC Public Health 2020, 20, 1055. [Google Scholar] [CrossRef] [PubMed]
- Winickoff, J.P.; McMillen, R.C.; Vallone, D.M.; Pearson, J.L.; Tanski, S.E.; Dempsey, J.H.; Cheryl, H.; Klein, J.D.; David, A. US Attitudes About Banning Menthol in Cigarettes: Results from a Nationally Representative Survey. Am. J. Public Health 2011, 101, 1234–1236. [Google Scholar] [CrossRef] [PubMed]
- Wackowski, O.A.; Delnevo, C.D.; Pearson, J.L. Switching to E-Cigarettes in the Event of a Menthol Cigarette Ban. Nicotine Tob. Res. 2015, 17, 1286–1287. [Google Scholar] [CrossRef] [PubMed]
- Pacek, L.R.; Oliver, J.A.; Sweitzer, M.M.; McClernon, F.J. Young adult dual combusted cigarette and e-cigarette users’ anticipated responses to a nicotine reduction policy and menthol ban in combusted cigarettes. Drug Alcohol Depend. 2019, 194, 40–44. [Google Scholar] [CrossRef] [PubMed]
- Rose, S.W.P.; Ganz, O.D.M.; Zhou, Y.M.S.; Carnegie, B.E.M.P.H.; Villanti, A.C.P.; Rath, J.P.; Hair, E.C.P. Longitudinal Response to Restrictions on Menthol Cigarettes Among Young Adult US Menthol Smokers, 2011–2016. Am. J. Public Health 2019, 109, 1400–1403. [Google Scholar] [CrossRef]
| Sociodemographic Characteristics | Overall Sample % (n) or M (SD) | Current Menthol Smoking Status (Cigarette or LCC) % (n) or M (SD) | |
|---|---|---|---|
| Any Menthol | Non-menthol | ||
| 69.2 (101) | 30.8 (45) | ||
| Age | 33.3 (8.7) | 34.3 (8.1) | 31.2 (9.7) |
| Race | |||
| Black/African American only | 94.4 (136) | 94.0 (94) | 95.5 (42) |
| Biracial/Multiracial | 5.6 (8) | 6.0 (6) | 4.6 (2) |
| Sexual Orientation | |||
| Heterosexual/Straight | 73.6 (106) | 71.7 (71) | 77.8 (35) |
| Gay/Lesbian/Bisexual/Other | 26.4 (38) | 28.3 (28) | 22.2 (10) |
| Body Mass Index (BMI) | 32.2 (9.6) | 31.9 (10.3) | 32.7 (7.7) |
| Marital Status | |||
| Married | 25.0 (36) | 29.3 (29) | 15.6 (7) |
| Living with partner | 15.3 (22) | 17.2 (17) | 11.1 (5) |
| Other | 15.3 (22) | 15.2 (15) | 15.6 (7) |
| Never married | 44.4 (64) | 38.4 (38) | 57.8 (26) |
| Employment Status | |||
| Full-time | 20.7 (30) | 19.0 (19) | 24.4 (11) |
| Part-time | 16.6 (24) | 13.0 (13) | 24.4 (11) |
| Do not currently work for pay | 62.8 (91) | 68.0 (68) | 51.1 (23) |
| Insurance Status | |||
| Insured | 81.1 (116) | 78.6 (77) | 86.7 (39) |
| Uninsured | 18.9 (27) | 21.4 (21) | 13.3 (6) |
| Enrolled in Degree Program | |||
| Yes | 15.9 (23) | 13.0 (13) | 22.2 (10) |
| No | 84.1 (122) | 87.0 (87) | 77.8 (35) |
| Education * | |||
| Less than high school | 26.9 (39) | 31.0 (31) | 17.8 (8) |
| High school or GED | 48.3 (70) | 51.0 (51) | 42.2 (19) |
| Some college or associates degree | 24.8 (36) | 18.0 (18) | 40.0 (18) |
| Annual Household Income | |||
| <$10 K | 65.5 (95) | 64.0 (64) | 68.9 (31) |
| ≥$10 K | 34.5 (50) | 36.0 (36) | 31.1 (14) |
| Received SNAP Benefits in Past Year | |||
| Yes | 81.4 (118) | 84.0 (84) | 75.6 (34) |
| No | 18.6 (27) | 16.0 (16) | 24.4 (11) |
| Tobacco/Other Substance Use Characteristic | Overall Sample % (n) or M (SD) | Any Current Menthol Smoking % (n) or M (SD) | |
|---|---|---|---|
| Menthol 69.2 (101) | Non-Menthol 30.8 (45) | ||
| Age First Smoked Cigarettes Fairly Regularly | 18.6 (5.0) | 18.9 (5.2) | 17.2 (4.1) |
| Age First Smoked LCCs Fairly Regularly | 21.1 (7.4) | 21.6 (7.5) | 20.7 (7.4) |
| Daily Cigarette Smoking (Yes) *** | 61.3 (92) | 81.0 (81) | 24.4 (11) |
| Daily LCC Smoking (Yes) *** | 15.3 (23) | 7.0 (7) | 35.6 (16) |
| Number of Days Smoked Cigarettes in Past 30 Days *** | 20.2 (10.5) | 21.7 (10.2) | 12.9 (9.2) |
| Cigarettes Smoked Per Day (Median (IQR)) ** | 8.0 (10.0) | 10.0 (15.0) | 5.0 (6.0) |
| Number of Days Smoked LCCs In Past 30 Days ** | 12.4 (11.2) | 8.6 (9.6) | 16.1 (11.4) |
| LCCs Smoked Per Day | 6.4 (6.5) | 5.8 (6.1) | 6.9 (7.0) |
| Past 30-day Brand of LCC Smoked | |||
| Black & Mild | 61.0 (36) | 58.6 (17) | 63.3 (19) |
| Swisher Sweets | 28.8 (17) | 34.5 (10) | 23.3 (7) |
| Other | 10.2 (6) | 6.9 (2) | 13.3 (4) |
| Current Other Tobacco Product Use ** (Yes) | 29.7 (43) | 22.0 (22) | 46.7 (21) |
| Current Alcohol Use (Yes) | 37.2 (54) | 34.0 (34) | 44.4 (20) |
| Current Marijuana Use (Yes) | 26.4 (38) | 22.0 (22) | 36.4 (16) |
| Current Blunt (Yes) | 50.6 (40) | 47.7 (21) | 54.3 (19) |
| Current Other Drug Use (Yes) | 2.8 (4) | 2.0 (2) | 4.4 (2) |
| Action Taken if Menthol Cigarettes Were Banned | |||
| Switch to non-menthol cigarette | 18.1 (21) | 18.2 (18) | 17.7 (3) |
| Switch to LCC | 22.4 (26) | 20.2 (20) | 35.3 (6) |
| Quit any cigarette smoking | 25.0 (29) | 25.3 (25) | 23.5 (4) |
| Switch to marijuana | 11.2 (13) | 12.1 (12) | 5.9 (1) |
| None of the above | 23.3 (27) | 24.2 (24) | 17.7 (3) |
| Nicotine Dependence and Quitting Behaviors | |||
| FTND Score * | 4.5 (2.2) | 4.7 (2.0) | 3.4 (2.6) |
| Time to First Cigarette of within 5 min ** | 50.0 (60) | 55.6 (55) | 23.8 (5) |
| Time to First LCC of within 5 min | 32.8 (19) | 39.3 (11) | 26.7 (8) |
| Time to First Tobacco Product Use of within 5 min *** | 48.0 (70) | 57.4 (58) | 36.7 (12) |
| Ever Tried to Quit Cigarettes | 54.2 (64) | 50.5 (49) | 71.4 (15) |
| Tried to Quit Cigarettes in Past 12 Months (yes) | 56.5 (35) | 56.3 (27) | 57.1 (8) |
| Planning to Quit Cigarette Smoking in Next 30 Days (yes) | 19.8 (23) | 18.8 (18) | 25.0 (5) |
| Outcomes | |||
|---|---|---|---|
| Predictor | Time to First Tobacco Product Use (≤5 min vs. >5 min) AOR (95% CI) | FTND Score B (SE), t, p | Ever Tried to Quit Cigarettes (Yes vs. No) AOR (95% CI) |
| MODEL 1 | |||
| Any menthol product use (yes vs. no) | 4.10 (1.73, 9.70) | - | 0.36 (0.11, 1.12) |
| Menthol cigarette use (yes vs. no) | - | 1.49 (0.56) t = 2.68, p = 0.0085 | - |
| MODEL 2 | |||
| Any menthol product use (yes vs. no) | 5.90 (1.16, 22.33) | 0.45 (0.12, 1.72) | |
| Menthol cigarette use (yes vs. no) | - | 1.16 (0.58), t = 2.01, p = 0.0469 | - |
| Overall N = 146 | Low Education | Low Education and Low Income | Low Education, Low Income, and SNAP Recipient | |
|---|---|---|---|---|
| Cigarette and/or LCC smokers | ||||
| n = 146 | n = 39 | n = 32 | n = 23 | |
| % (n) | % (n) | % (n) | % (n) | |
| Time to First Tobacco Product Use ≤5 min of waking (Yes) | 47.9 (70) | 59.0 (23) | 62.5 (20) | 65.2 (15) |
| Cigarette smokers | ||||
| n = 120 | n = 37 | n = 31 | n = 22 | |
| % (n) or M (SD) | % (n) or M (SD) | % (n) or M (SD) | % (n) or M (SD) | |
| Time to First Cigarette Use ≤5 min of waking (Yes) | 50.0 (60) | 59.5 (22) | 61.3 (19) | 63.6 (14) |
| FTND Score | 4.6 (2.3) | 4.9 (2.5) | 4.9 (2.6) | 4.9 (2.8) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jones, D.M.; Kulik, M.C.; Baezconde-Garbanati, L.; Bullock, S.; Guy, M.C.; Fagan, P. Menthol Smoking and Nicotine Dependence among Black/African American Women Smokers Living in Low-Resource, Rural Communities. Int. J. Environ. Res. Public Health 2021, 18, 10877. https://doi.org/10.3390/ijerph182010877
Jones DM, Kulik MC, Baezconde-Garbanati L, Bullock S, Guy MC, Fagan P. Menthol Smoking and Nicotine Dependence among Black/African American Women Smokers Living in Low-Resource, Rural Communities. International Journal of Environmental Research and Public Health. 2021; 18(20):10877. https://doi.org/10.3390/ijerph182010877
Chicago/Turabian StyleJones, Dina M., Margarete C. Kulik, Lourdes Baezconde-Garbanati, Sandilyn Bullock, Mignonne C. Guy, and Pebbles Fagan. 2021. "Menthol Smoking and Nicotine Dependence among Black/African American Women Smokers Living in Low-Resource, Rural Communities" International Journal of Environmental Research and Public Health 18, no. 20: 10877. https://doi.org/10.3390/ijerph182010877
APA StyleJones, D. M., Kulik, M. C., Baezconde-Garbanati, L., Bullock, S., Guy, M. C., & Fagan, P. (2021). Menthol Smoking and Nicotine Dependence among Black/African American Women Smokers Living in Low-Resource, Rural Communities. International Journal of Environmental Research and Public Health, 18(20), 10877. https://doi.org/10.3390/ijerph182010877






