Assessment of Force Production in Parkinson’s Disease Subtypes
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Pääsuke, M.; Ereline, J.; Gapeyeva, H.; Joost, K.; Mõttus, K.; Taba, P. Leg-extension strength and chair-rise performance in elderly women with Parkinson’s disease. J. Aging Phys. Act. 2004, 12, 511–524. [Google Scholar] [CrossRef]
- Park, J.H.; Stelmach, G.E. Force development during target-directed isometric force production in Parkinson’s disease. Neurosci. Lett. 2007, 412, 173–178. [Google Scholar] [CrossRef] [Green Version]
- Cano-de-la-Cuerda, R.; Pérez-de-Heredia, M.; Miangolarra-Page, J.C.; Muñoz-Hellín, E.; Fernández-de-Las-Peñas, C. Is there muscular weakness in Parkinson’s disease? Am. J. Phys. Med. Rehabil. 2010, 89, 70–76. [Google Scholar] [CrossRef]
- Milner-Brown, H.S.; Fisher, M.A.; Weiner, W.J. Electrical properties of motor units in Parkinsonism and a possible relationship with bradykinesia. J. Neurol. Neurosurg. Psychiatry 1979, 42, 35–41. [Google Scholar] [CrossRef] [Green Version]
- Stevens-Lapsley, J.; Kluger, B.M.; Schenkman, M. Quadriceps muscle weakness, activation deficits, and fatigue with Parkinson disease. Neurorehabil. Neural Repair 2012, 26, 533–541. [Google Scholar] [CrossRef]
- Mak, M.K.; Pang, M.Y.; Mok, V. Gait difficulty, postural instability, and muscle weakness are associated with fear of falling in people with Parkinson’s disease. Parkinsons Dis. 2012, 901721. [Google Scholar] [CrossRef] [Green Version]
- Marsh, A.P.; Rejeski, W.J.; Espeland, M.A.; Miller, M.E.; Church, T.S.; Fielding, R.A.; Gill, T.M.; Guralnik, J.M.; Newman, A.B.; Pahor, M. Muscle strength and BMI as predictors of major mobility disability in the Lifestyle Interventions and Independence for Elders pilot (LIFE-P). J. Gerontol. A Biol. Sci. Med. Sci. 2011, 66, 1376–1383. [Google Scholar] [CrossRef]
- Hortobágyi, T.; Rider, P.; Gruber, A.H.; DeVita, P. Age and muscle strength mediate the age-related biomechanical plasticity of gait. Eur. J. Appl. Physiol. 2016, 116, 805–814. [Google Scholar] [CrossRef]
- Nallegowda, M.; Singh, U.; Handa, G.; Khanna, M.; Wadhwa, S.; Yadav, S.L.; Kumar, G.; Behari, M. Role of sensory input and muscle strength in maintenance of balance, gait, and posture in Parkinson’s disease: A pilot study. Am. J. Phys. Med. Rehabil. 2004, 83, 898–908. [Google Scholar] [CrossRef]
- Duchowny, K. Do Nationally Representative Cutpoints for Clinical Muscle Weakness Predict Mortality? Results From 9 Years of Follow-up in the Health and Retirement Study. J. Gerontol. A Biol. Sci. Med. Sci. 2019, 74, 1070–1075. [Google Scholar] [CrossRef] [PubMed]
- Aagaard, P.; Simonsen, E.B.; Andersen, J.L.; Magnusson, P.; Dyhre-Poulsen, P. Increased rate of force development and neural drive of human skeletal muscle following resistance training. J. Appl. Physiol. 2002, 93, 1318–1326. [Google Scholar] [CrossRef] [PubMed]
- Maffiuletti, N.A.; Bizzini, M.; Widler, K.; Munzinger, U. Asymmetry in quadriceps rate of force development as a functional outcome measure in TKA. Clin. Orthop. Relat. Res. 2010, 468, 191–198. [Google Scholar] [CrossRef] [Green Version]
- Peñailillo, L.; Blazevich, A.; Numazawa, H.; Nosaka, K. Rate of force development as a measure of muscle damage. Scand. J. Med. Sci. Sports 2015, 25, 417–427. [Google Scholar] [CrossRef] [PubMed]
- Hammond, K.G.; Pfeiffer, R.F.; LeDoux, M.S.; Schilling, B.K. Neuromuscular rate of force development deficit in Parkinson disease. Clin. Biomech. (Bristol, Avon) 2017, 45, 14–18. [Google Scholar] [CrossRef]
- Caetano, M.J.D.; Lord, S.R.; Allen, N.E.; Song, J.; Paul, S.S.; Canning, C.G.; Menant, J.C.C. Executive Functioning, Muscle Power and Reactive Balance Are Major Contributors to Gait Adaptability in People With Parkinson’s Disease. Front. Aging Neurosci. 2019, 11, 154. [Google Scholar] [CrossRef]
- Allen, N.E.; Sherrington, C.; Canning, C.G.; Fung, V.S. Reduced muscle power is associated with slower walking velocity and falls in people with Parkinson’s disease. Parkinsonism Relat. Disord. 2010, 16, 261–264. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.; Hinder, M.R.; Gandevia, S.C.; Carroll, T.J. The ipsilateral motor cortex contributes to cross-limb transfer of performance gains after ballistic motor practice. J. Physiol. 2010, 588, 201–212. [Google Scholar] [CrossRef] [PubMed]
- Berardelli, A.; Rothwell, J.C.; Thompson, P.D.; Hallett, M. Pathophysiology of bradykinesia in Parkinson’s disease. Brain 2001, 124, 2131–2146. [Google Scholar] [CrossRef] [Green Version]
- Pfann, K.D.; Buchman, A.S.; Comella, C.L.; Corcos, D.M. Control of movement distance in Parkinson’s disease. Mov. Disord. 2001, 16, 1048–1065. [Google Scholar] [CrossRef]
- Paul, S.S.; Sherrington, C.; Fung, V.S.; Canning, C.G. Motor and cognitive impairments in Parkinson disease: Relationships with specific balance and mobility tasks. Neurorehabil. Neural Repair 2013, 27, 63–71. [Google Scholar] [CrossRef]
- Allen, N.E.; Canning, C.G.; Sherrington, C.; Fung, V.S. Bradykinesia, muscle weakness and reduced muscle power in Parkinson’s disease. Mov. Disord. 2009, 24, 1344–1351. [Google Scholar] [CrossRef]
- Pelicioni, P.H.S.; Brodie, M.A.; Latt, M.D.; Menant, J.C.; Menz, H.B.; Fung, V.S.C.; Lord, S.R. Head and trunk stability during gait before and after levodopa intake in Parkinson’s disease subtypes. Exp. Gerontol. 2018, 111, 78–85. [Google Scholar] [CrossRef]
- Pelicioni, P.H.S.; Menant, J.C.; Latt, M.D.; Lord, S.R. Falls in Parkinson’s Disease Subtypes: Risk Factors, Locations and Circumstances. Int. J. Environ. Res. Public Health 2019, 16, 2216. [Google Scholar] [CrossRef] [Green Version]
- Pelicioni, P.H.S.; Pereira, M.P.; Lahr, J.; Rodrigues, M.M.L.; Gobbi, L.T.B. Biomechanical analysis of sit-to-walk in different Parkinson’s disease subtypes. Clin. Biomech. (Bristol, Avon) 2020, 75, 105010. [Google Scholar] [CrossRef]
- Orcioli-Silva, D.; Vitório, R.; Beretta, V.S.; da Conceição, N.R.; Nóbrega-Sousa, P.; Oliveira, A.S.C.; Gobbi, L.T.B. Is cortical activation during walking different between Parkinson’s disease motor subtypes? J. Gerontol. A Biol. Sci. Med. Sci. 2020. [Google Scholar] [CrossRef]
- Orcioli-Silva, D.; Vitório, R.; Lirani-Silva, E.; Santos, P.C.R.; Beretta, V.S.; Gobbi, L.T.B. Objective measures of unobstructed walking and obstacle avoidance in Parkinson’s disease subtypes. Gait Posture 2018, 62, 405–408. [Google Scholar] [CrossRef] [Green Version]
- Hughes, A.J.; Daniel, S.E.; Kilford, L.; Lees, A.J. Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: A clinico-pathological study of 100 cases. J. Neurol. Neurosurg. Psychiatry 1992, 55, 181–184. [Google Scholar] [CrossRef] [Green Version]
- Fahn, S.; Elton, R.L. Unified Parkinson’s Disease Rating Scale. In Recent Developments in Parkinson’s Disease; Fahn, S., Mardsen, C.D., Calne, D., Goldstein, M., Eds.; Macmillan Healthcare Information: Florham Park, NJ, USA, 1987; pp. 153–163. [Google Scholar]
- Jankovic, J.; McDermott, M.; Carter, J.; Gauthier, S.; Goetz, C.; Golbe, L.; Huber, S.; Koller, W.; Olanow, C.; Shoulson, I.; et al. Variable expression of Parkinson’s disease: A base-line analysis of the DATATOP cohort. The Parkinson Study Group. Neurology 1990, 40, 1529–1534. [Google Scholar] [CrossRef]
- Tomlinson, C.L.; Stowe, R.; Patel, S.; Rick, C.; Gray, R.; Clarke, C.E. Systematic review of levodopa dose equivalency reporting in Parkinson’s disease. Mov. Disord. 2010, 25, 2649–2653. [Google Scholar] [CrossRef]
- Pereira, M.P.; Gonçalves, M. Muscular coactivation (CA) around the knee reduces power production in elderly women. Arch. Gerontol. Geriatr. 2011, 52, 317–321. [Google Scholar] [CrossRef]
- Maffiuletti, N.A.; Aagaard, P.; Blazevich, A.J.; Folland, J.; Tillin, N.; Duchateau, J. Rate of force development: Physiological and methodological considerations. Eur. J. Appl. Physiol. 2016, 116, 1091–1116. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sawilowsky, S. New effect size rules of thumb. J. Mod. Appl. Stat. Methods 2009, 8, 467–474. [Google Scholar] [CrossRef]
- Rose, M.H.; Løkkegaard, A.; Sonne-Holm, S.; Jensen, B.R. Tremor irregularity, torque steadiness and rate of force development in Parkinson’s disease. Motor Control 2013, 17, 203–216. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Desmedt, J.E.; Godaux, E. Ballistic contractions in man: Characteristic recruitment pattern of single motor units of the tibialis anterior muscle. J. Physiol. 1977, 264, 673–693. [Google Scholar] [CrossRef] [PubMed]
- Freund, H.J.; Büdingen, H.J. The relationship between speed and amplitude of the fastest voluntary contractions of human arm muscles. Exp. Brain Res. 1978, 31, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Dimitrova, D.; Horak, F.B.; Nutt, J.G. Postural muscle responses to multidirectional translations in patients with Parkinson’s disease. J. Neurophysiol. 2004, 91, 489–501. [Google Scholar] [CrossRef] [Green Version]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, M146–M157. [Google Scholar] [CrossRef] [PubMed]
- Lauretani, F.; Maggio, M.; Ticinesi, A.; Tana, C.; Prati, B.; Gionti, L.; Nouvenne, A.; Meschi, T. Muscle weakness, cognitive impairment and their interaction on altered balance in elderly outpatients: Results from the TRIP observational study. Clin. Interv. Aging 2018, 13, 1437–1443. [Google Scholar] [CrossRef] [Green Version]
- Hurley, M.V.; Rees, J.; Newham, D.J. Quadriceps function, proprioceptive acuity and functional performance in healthy young, middle-aged and elderly subjects. Age Ageing 1998, 27, 55–62. [Google Scholar] [CrossRef] [Green Version]
- Pelicioni, P.H.S.; Pereira, M.P.; Lahr, J.; Rodrigues, M.M.L.; de Morais, L.C.; Moraes, R.; Gobbi, L.T.B. Motor adjustments during time-constrained sit-to-walk in people with Parkinson’s disease. Exp. Gerontol. 2019, 124, 110654. [Google Scholar] [CrossRef]
- Santos, P.C.; Gobbi, L.T.; Orcioli-Silva, D.; Simieli, L.; van Dieën, J.H.; Barbieri, F.A. Effects of leg muscle fatigue on gait in patients with Parkinson’s disease and controls with high and low levels of daily physical activity. Gait Posture 2016, 47, 86–91. [Google Scholar] [CrossRef] [Green Version]
- Espay, A.J.; Giuffrida, J.P.; Chen, R.; Payne, M.; Mazzella, F.; Dunn, E.; Vaughan, J.E.; Duker, A.P.; Sahay, A.; Kim, S.J.; et al. Differential response of speed, amplitude, and rhythm to dopaminergic medications in Parkinson’s disease. Mov. Disord. 2011, 26, 2504–2508. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Outcomes | OA (n = 14) | TD (n = 14) | PIGD (n = 10) | p |
|---|---|---|---|---|
| Sex Male (%) | 9 (60) | 11 (79) | 6 (60) | 0.498 |
| Age (years) | 69.7 (5.0) | 72.0 (5.5) | 70.1 (4.2) | 0.436 |
| Weight (kg) | 67.7 (15.1) | 75.1 (9.4) | 64.2 (11.3) | 0.092 |
| Height (cm) | 162.4 (8.0) | 164.3 (5.9) | 159.2 (8.0) | 0.257 |
| Disease duration (years) | - | 5.1 (2.7) | 6.4 (4.6) | 0.452 |
| UPDRS part III (score) | - | 28.5 (9.0) | 29.1 (7.3) | 0.769 |
| HY (stage) | - | 1.9 (0.3) | 2.0 (0.3) | 0.596 |
| LED (mg) | - | 692 (478) | 867 (509) | 0.403 |
| Outcomes | OA (n = 14) | TD (n = 14) | PIGD (n = 10) | p |
|---|---|---|---|---|
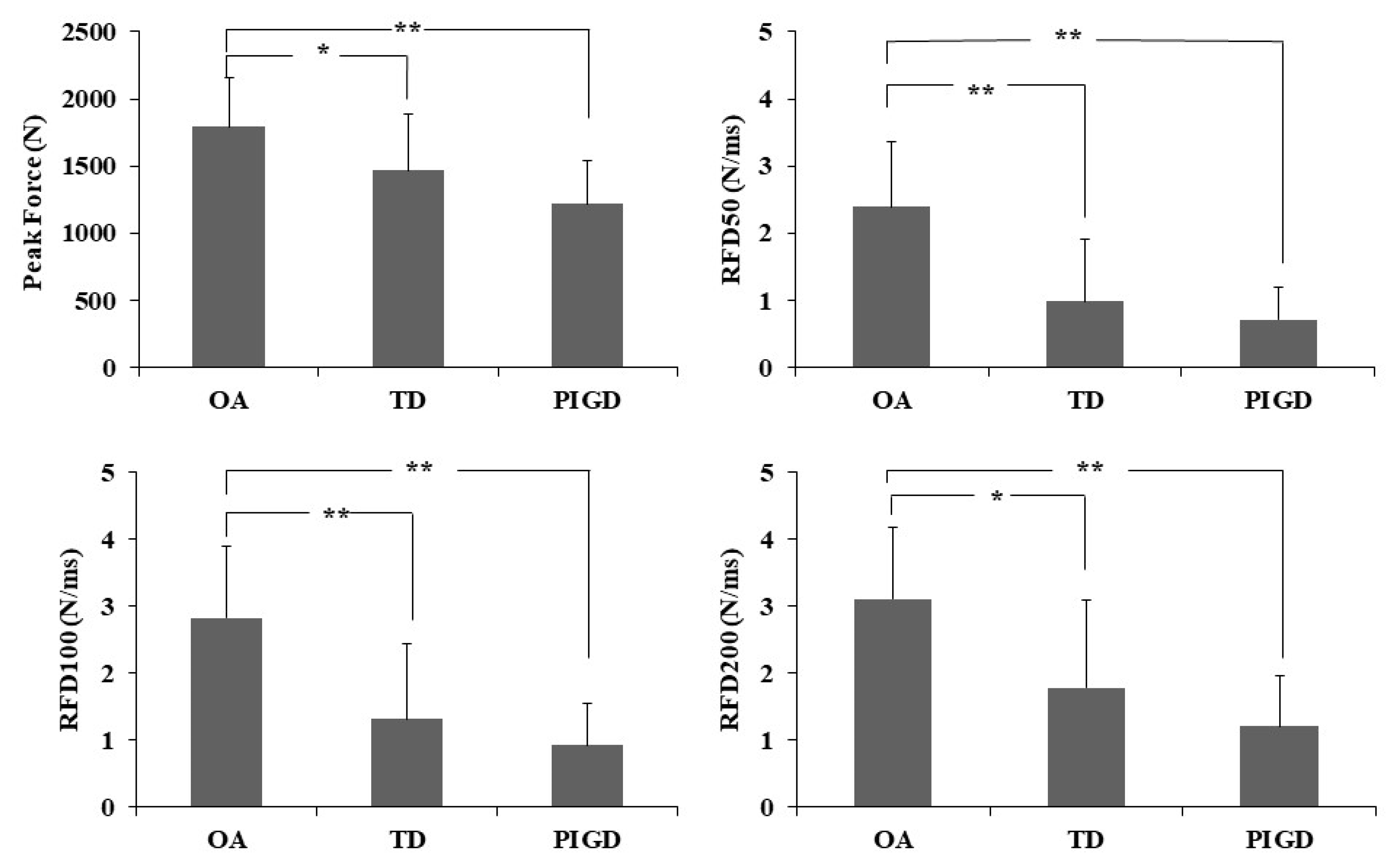
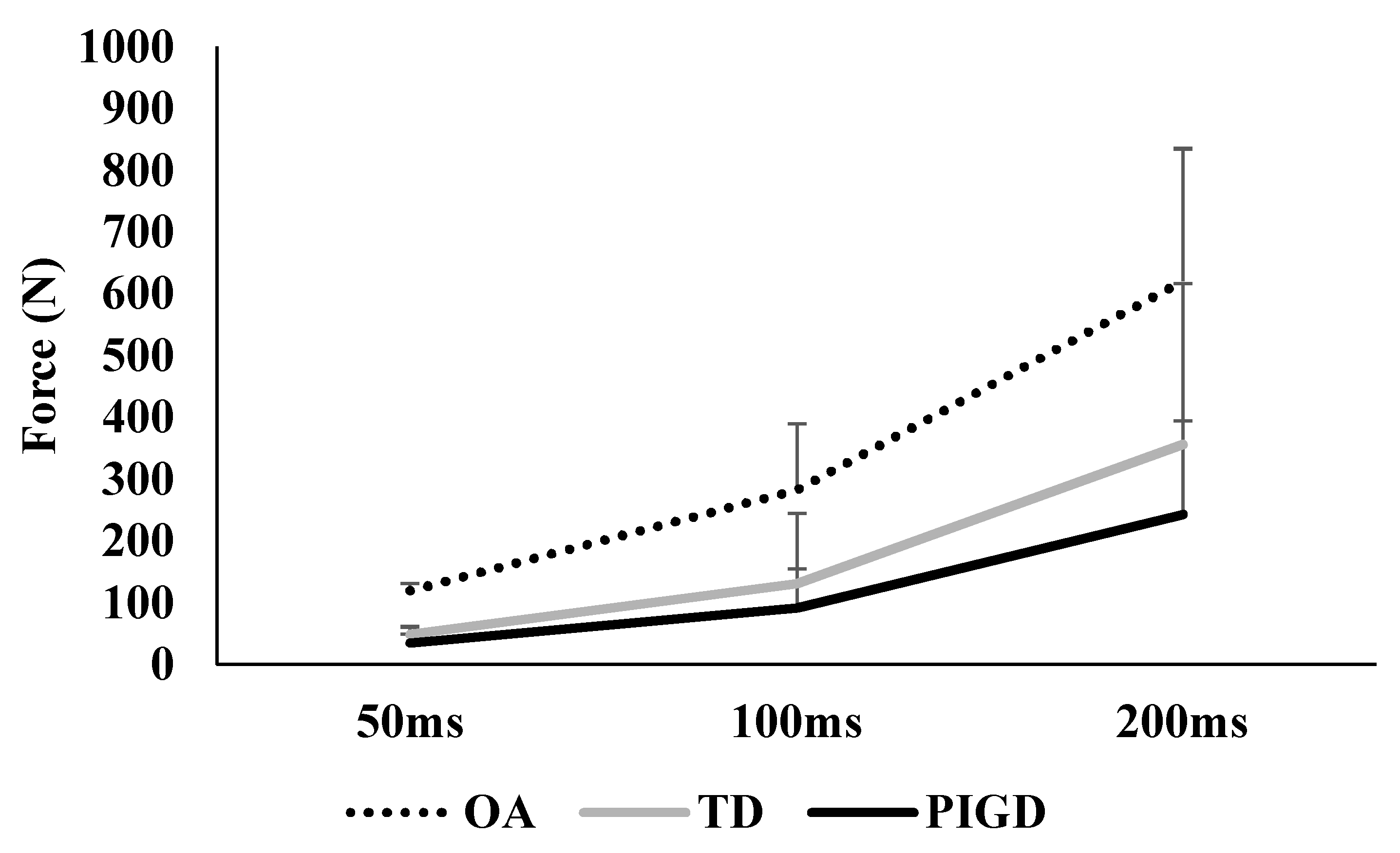
| Peak force (N) | 1791 (367) | 1467 (417) | 1217 (324) | 0.003 a,b,c |
| RFD50 (N/ms) | 2.39 (0.97) | 0.98 (0.93) | 0.71 (0.49) | <0.001 a,b,c |
| RFD100 (N/ms) | 2.82 (1.08) | 1.31 (1.13) | 0.92 (0.63) | <0.001 a,b,c |
| RFD200 (N/ms) | 3.10 (1.07) | 1.78 (1.30) | 1.21 (0.75) | <0.001 a,b,c |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pelicioni, P.H.S.; Pereira, M.P.; Lahr, J.; dos Santos, P.C.R.; Gobbi, L.T.B. Assessment of Force Production in Parkinson’s Disease Subtypes. Int. J. Environ. Res. Public Health 2021, 18, 10044. https://doi.org/10.3390/ijerph181910044
Pelicioni PHS, Pereira MP, Lahr J, dos Santos PCR, Gobbi LTB. Assessment of Force Production in Parkinson’s Disease Subtypes. International Journal of Environmental Research and Public Health. 2021; 18(19):10044. https://doi.org/10.3390/ijerph181910044
Chicago/Turabian StylePelicioni, Paulo Henrique Silva, Marcelo Pinto Pereira, Juliana Lahr, Paulo Cezar Rocha dos Santos, and Lilian Teresa Bucken Gobbi. 2021. "Assessment of Force Production in Parkinson’s Disease Subtypes" International Journal of Environmental Research and Public Health 18, no. 19: 10044. https://doi.org/10.3390/ijerph181910044
APA StylePelicioni, P. H. S., Pereira, M. P., Lahr, J., dos Santos, P. C. R., & Gobbi, L. T. B. (2021). Assessment of Force Production in Parkinson’s Disease Subtypes. International Journal of Environmental Research and Public Health, 18(19), 10044. https://doi.org/10.3390/ijerph181910044








