Predictors of Changes in Physical Activity and Sedentary Behavior during the COVID-19 Pandemic in a Turkish Migrant Cohort in Germany
Abstract
:1. Introduction
2. Materials and Methods
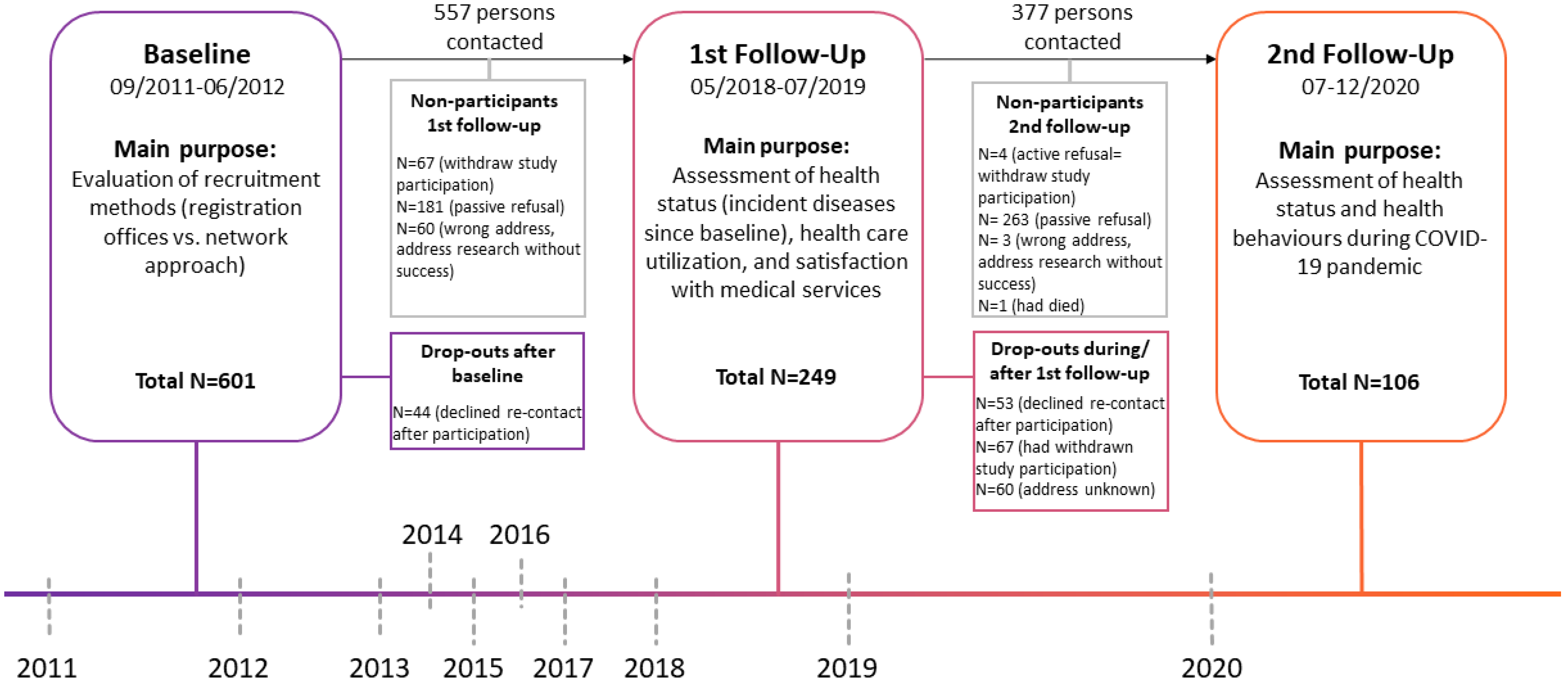
2.1. Study Design
2.2. Participants and Enrollment
2.3. Measures
2.3.1. Changes in Physical Activity (PA) and Sedentary Behavior (SB)—Outcome
2.3.2. Physical Activity as a Covariate
2.3.3. Sociodemographic Variables
2.3.4. Migration-Related Variables
2.3.5. Health-Related Variables
2.3.6. Mental Health Variable
2.4. Statistical Analyses
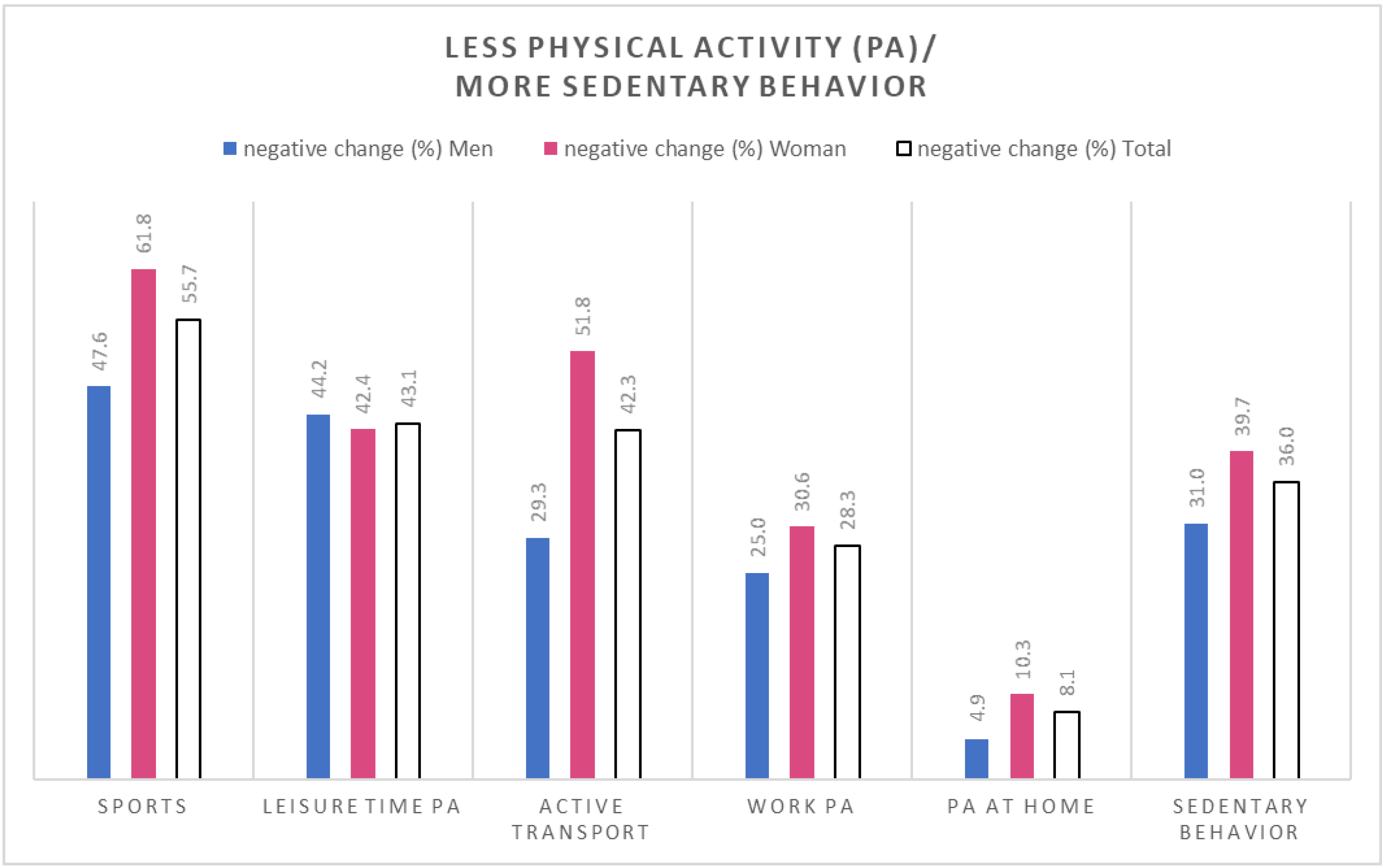
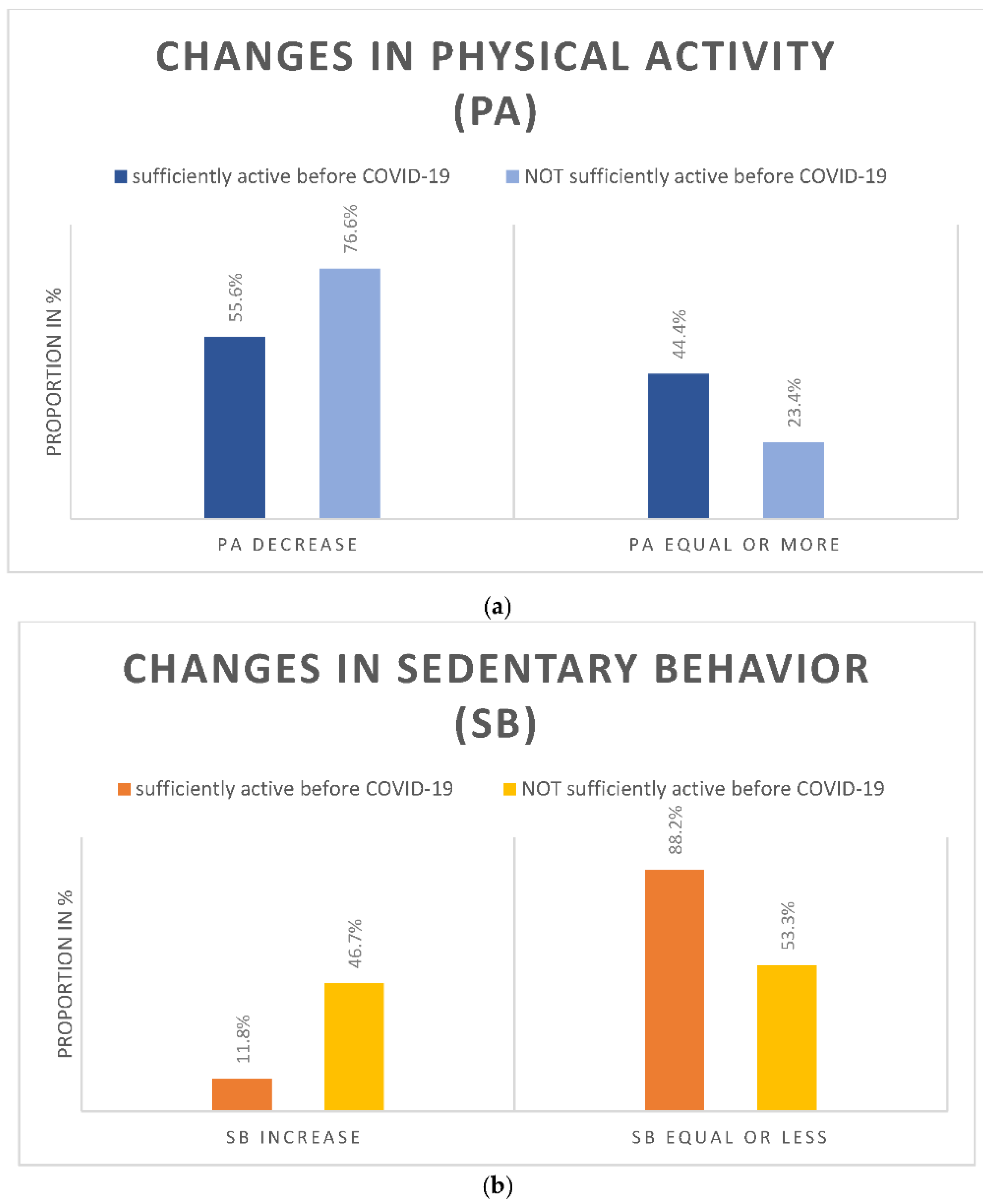
3. Results
Regression Analyses
4. Discussion
4.1. Strengths and Limitations
4.2. Implications
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. Timeline of WHO’s Response to COVID-19. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/interactive-timeline?gclid=Cj0KCQjw7pKFBhDUARIsAFUoMDYDCfU8DVtIe_CyR22LqO1_Qur5octqIBn-eSePRKZGQVOFovOCR1QaAiXxEALw_wcB#! (accessed on 19 May 2021).
- WHO. WHO COVID-19 Explorer. Available online: https://worldhealthorg.shinyapps.io/covid/ (accessed on 18 May 2021).
- British Broadcasting Corporation Coronavirus: The World in Lockdown in Maps and Charts—BBC News. Available online: https://www.bbc.com/news/world-52103747 (accessed on 18 May 2021).
- Federal Ministry of Health Chronik Zum Coronavirus SARS-CoV-2. Maßnahmen. Available online: https://www.bundesgesundheitsministerium.de/coronavirus/chronik-coronavirus.html (accessed on 19 May 2021).
- German Federal Government Besprechung der Bundeskanzlerin mit den Regierungschefinnen und Regierungschefs der Länder vom 22.03.2020. Available online: https://www.bundesregierung.de/breg-de/themen/coronavirus/besprechung-der-bundeskanzlerin-mit-den-regierungschefinnen-und-regierungschefs-der-laender-vom-22-03-2020-1733248 (accessed on 19 May 2021).
- German Federal Government Beratung der Kanzlerin mit den Ministerpräsidenten. Available online: https://www.bundesregierung.de/breg-de/aktuelles/bund-laender-beschluss-1811744 (accessed on 19 May 2021).
- Stockwell, S.; Trott, M.; Tully, M.; Shin, J.; Barnett, Y.; Butler, L.; McDermott, D.; Schuch, F.; Smith, L. Changes in physical activity and sedentary behaviours from before to during the COVID-19 pandemic lockdown: A systematic review. BMJ Open Sport Exerc. Med. 2021, 7, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Caputo, E.L.; Reichert, F.F. Studies of Physical Activity and COVID-19 during the Pandemic: A Scoping Review. J. Phys. Act. Health 2020, 17, 1275–1284. [Google Scholar] [CrossRef] [PubMed]
- Pareja-Galeano, H.; Garatachea, N.; Lucia, A. Exercise as a Polypill for Chronic Diseases. In Progress in Molecular Biology and Translational Science; Elsevier Inc.: Amsterdam, The Netherlands, 2015; pp. 497–526. ISBN 9780128039915. [Google Scholar]
- Schuch, F.B.; Stubbs, B.; Meyer, J.; Heissel, A.; Zech, P.; Vancampfort, D.; Rosenbaum, S.; Deenik, J.; Firth, J.; Ward, P.B.; et al. Physical activity protects from incident anxiety: A meta-analysis of prospective cohort studies. Depress. Anxiety 2019, 36, 846–858. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Saltin, B. Exercise as medicine—Evidence for prescribing exercise as therapy in 26 different chronic diseases. Scand. J. Med. Sci. Sport. 2015, 25, 1–72. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brailovskaia, J.; Cosci, F.; Mansueto, G.; Miragall, M.; Herrero, R.; Baños, R.M.; Krasavtseva, Y.; Kochetkov, Y.; Margraf, J. The association between depression symptoms, psychological burden caused by Covid-19 and physical activity: An investigation in Germany, Italy, Russia, and Spain. Psychiatry Res. 2021, 295, 113596. [Google Scholar] [CrossRef]
- Violant-Holz, V.; Gallego-Jiménez, M.G.; González-González, C.S.; Muñoz-Violant, S.; Rodríguez, M.J.; Sansano-Nadal, O.; Guerra-Balic, M. Psychological health and physical activity levels during the covid-19 pandemic: A systematic review. Int. J. Environ. Res. Public Health 2020, 17, 9419. [Google Scholar] [CrossRef]
- Peters, A.; Rospleszcz, S.; Greiser, K.H.; Dallavalle, M.; Berger, K. The Impact of the COVID-19 Pandemic on Self-Reported Health. Dtsch. Arztebl. Int. 2020, 117, 861–867. [Google Scholar] [CrossRef]
- Silva, F.M.; Duarte-Mendes, P.; Rusenhack, M.C.; Furmann, M.; Nobre, P.R.; Fachada, M.Â.; Soares, C.M.; Teixeira, A.; Ferreira, J.P. Objectively measured sedentary behavior and physical fitness in adults: A systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2020, 17, 8660. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Lee, J.; Ahn, J.; Lee, D.-W.; Kim, H.-R.; Kang, M.-Y. Association of Sedentary Work with Colon and Rectal Cancer: Systematic Review and Meta-Analysis. Occup Environ Med. 2021. [Google Scholar] [CrossRef] [PubMed]
- Ramsey, K.A.; Rojer, A.G.M.; D’Andrea, L.; Otten, R.H.J.; Heymans, M.W.; Trappenburg, M.C.; Verlaan, S.; Whittaker, A.C.; Meskers, C.G.M.; Maier, A.B. The association of objectively measured physical activity and sedentary behavior with skeletal muscle strength and muscle power in older adults: A systematic review and meta-analysis. Ageing Res. Rev. 2021, 67, 101266. [Google Scholar] [CrossRef]
- Maertl, T.; De Bock, F.; Huebl, L.; Oberhauser, C.; Coenen, M.; Jung-Sievers, C. Physical activity during COVID-19 in German adults: Analyses in the covid-19 snapshot monitoring study (cosmo). Int. J. Environ. Res. Public Health 2021, 18, 507. [Google Scholar] [CrossRef] [PubMed]
- Wilke, J.; Mohr, L.; Tenforde, A.S.; Edouard, P.; Fossati, C.; González-Gross, M.; Ramírez, C.S.; Laiño, F.; Tan, B.; Pillay, J.D.; et al. A pandemic within the pandemic? Physical activity levels substantially decreased in countries affected by covid-19. Int. J. Environ. Res. Public Health 2021, 18, 2235. [Google Scholar] [CrossRef]
- Huber, B.C.; Schlichtiger, J.; Drey, M.; Steffen, J.; Brunner, S. Change of the Physical Activity Scale for the Elderly (PASE) Score after COVID-19 Outbreak. J. Sports Med. Phys. Fitness 2021. [Google Scholar] [CrossRef]
- Mutz, M.; Gerke, M. Sport and exercise in times of self-quarantine: How Germans changed their behaviour at the beginning of the Covid-19 pandemic. Int. Rev. Sociol. Sport 2020, 56, 305–316. [Google Scholar] [CrossRef]
- Zajacova, A.; Jehn, A.; Stackhouse, M.; Denice, P.; Ramos, H. Changes in health behaviours during early COVID-19 and socio-demographic disparities: A cross-sectional analysis. Can. J. Public Health 2020, 111, 953–962. [Google Scholar] [CrossRef] [PubMed]
- Krist, L.; Dornquast, C.; Reinhold, T.; Becher, H.; Icke, K.; Danquah, I.; Willich, S.N.; Keil, T. Physical activity trajectories among persons of Turkish descent living in Germany—A cohort study. Int. J. Environ. Res. Public Health 2020, 17, 6349. [Google Scholar] [CrossRef] [PubMed]
- Statistisches Bundesamt (Destatis). Bevölkerung und Erwerbstätigkeit: Bevölkerung mit Migrationshintergrund—Ergebnisse des Mikrozensus 2019; Statistisches Bundesamt (Destatis): Wiesbaden, Germany, 2020. [Google Scholar]
- Reiss, K.; Dragano, N.; Ellert, U.; Fricke, J.; Greiser, K.H.; Keil, T.; Krist, L.; Moebus, S.; Pundt, N.; Schlaud, M.; et al. Comparing sampling strategies to recruit migrants for an epidemiological study. Results from a German feasibility study. Eur. J. Public Health 2014, 24, 721–726. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Krist, L.; Dornquast, C.; Reinhold, T.; Solak, S.; Durak, M.; Keil, T. Strategies to enhance follow-up response in a cohort study with Berliners of Turkish descent. Eur. J. Public Health 2019, 29, 400–401. [Google Scholar] [CrossRef]
- WHO. WHO Global Recommendations on Physical Activity. Available online: http://www.who.int/dietphysicalactivity/pa/en/index.htm (accessed on 20 February 2019).
- Aksit, N. Educational reform in Turkey. Int. J. Educ. Dev. 2007, 27, 129–137. [Google Scholar] [CrossRef] [Green Version]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W. The PHQ-9. Validity of a Brief Depression Severity Measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef] [PubMed]
- Yazici Güleç, M.; Güleç, H.; Şimşek, G.; Turhan, M.; Aydin Sünbül, E. Psychometric properties of the Turkish version of the Patient Health Questionnaire-Somatic, Anxiety, and Depressive Symptoms. Compr. Psychiatry 2012, 53, 623–629. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W.; Löwe, B. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: A systematic review. Gen. Hosp. Psychiatry 2010, 32, 345–359. [Google Scholar] [CrossRef] [PubMed]
- Kriaucioniene, V.; Bagdonaviciene, L.; Rodríguez-Pérez, C.; Petkeviciene, J. Associations between changes in health behaviours and body weight during the covid-19 quarantine in lithuania: The lithuanian covidiet study. Nutrients 2020, 12, 3119. [Google Scholar] [CrossRef] [PubMed]
- Gallè, F.; Sabella, E.A.; Ferracuti, S.; De Giglio, O.; Caggiano, G.; Protano, C.; Valeriani, F.; Parisi, E.A.; Valerio, G.; Liguori, G.; et al. Sedentary behaviors and physical activity of Italian undergraduate students during lockdown at the time of COVID-19 pandemic. Int. J. Environ. Res. Public Health 2020, 17, 6171. [Google Scholar] [CrossRef] [PubMed]
- Schlichtiger, J.; Steffen, J.; Huber, B.C.; Brunner, S. Physical activity during COVID-19 lockdown in older adults. J. Sports Med. Phys. Fit. 2020, 61, 164–166. [Google Scholar] [CrossRef]
- Huber, B.C.; Steffen, J.; Schlichtiger, J.; Graupe, T.; Deuster, E.; Strouvelle, V.P.; Fischer, M.R.; Massberg, S.; Brunner, S. Alteration of physical activity during COVID-19 pandemic lockdown in young adults. J. Transl. Med. 2020, 18, 7–9. [Google Scholar] [CrossRef]
- Wunsch, K.; Nigg, C.; Niessner, C.; Schmidt, S.C.E.; Oriwol, D.; Hanssen-Doose, A.; Burchartz, A.; Eichsteller, A.; Kolb, S.; Worth, A.; et al. The Impact of COVID-19 on the Interrelation of Physical Activity, Screen Time and Health-Related Quality of Life in Children and Adolescents in Germany: Results of the Motorik-Modul Study. Children 2021, 8, 98. [Google Scholar] [CrossRef]
- Meyer, J.; McDowell, C.; Lansing, J.; Brower, C.; Smith, L.; Tully, M.; Herring, M. Changes in physical activity and sedentary behavior in response to covid-19 and their associations with mental health in 3052 us adults. Int. J. Environ. Res. Public Health 2020, 17, 6469. [Google Scholar] [CrossRef]
- Bourdas, D.I.; Zacharakis, E.D. Impact of COVID-19 Lockdown on Physical Activity in a Sample of Greek Adults. Sports 2020, 8, 139. [Google Scholar] [CrossRef] [PubMed]
- Rogers, N.T.; Waterlow, N.R.; Brindle, H.; Enria, L.; Eggo, R.M.; Lees, S.; Roberts, C.h. Behavioral Change Towards Reduced Intensity Physical Activity Is Disproportionately Prevalent Among Adults with Serious Health Issues or Self-Perception of High Risk During the UK COVID-19 Lockdown. Front. Public Health 2020, 8, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Robinson, E.; Boyland, E.; Chisholm, A.; Harrold, J.; Maloney, N.G.; Marty, L.; Mead, B.R.; Noonan, R.; Hardman, C.A. Obesity, eating behavior and physical activity during COVID-19 lockdown: A study of UK adults. Appetite 2020, 156, 104853. [Google Scholar] [CrossRef]
- Knell, G.; Robertson, M.C.; Dooley, E.E.; Burford, K.; Mendez, K.S. Health behavior changes during covid-19 pandemic and subsequent “stay-at-home” orders. Int. J. Environ. Res. Public Health 2020, 17, 6268. [Google Scholar] [CrossRef] [PubMed]
- Constandt, B.; Thibaut, E.; De Bosscher, V.; Scheerder, J.; Ricour, M.; Willem, A. Exercising in times of lockdown: An analysis of the impact of COVID-19 on levels and patterns of exercise among adults in Belgium. Int. J. Environ. Res. Public Health 2020, 17, 4144. [Google Scholar] [CrossRef] [PubMed]
- Barkley, J.E.; Lepp, A.; Glickman, E.; Farnell, G.; Beiting, J.; Wiet, R.; Dowdell, B. The Acute Effects of the COVID-19 Pandemic on Physical Activity and Sedentary Behavior in University Students and Employees. Int. J. Exerc. Sci. 2020, 13, 1326–1339. [Google Scholar] [PubMed]
- Wang, X.; Lei, S.M.; Le, S.; Yang, Y.; Zhang, B.; Yao, W.; Gao, Z.; Cheng, S. Bidirectional influence of the COVID-19 pandemic lockdowns on health behaviors and quality of life among chinese adults. Int. J. Environ. Res. Public Health 2020, 17, 5575. [Google Scholar] [CrossRef] [PubMed]
- Castañeda-Babarro, A.; Coca, A.; Arbillaga-Etxarri, A.; Gutiérrez-Santamaría, B. Physical activity change during COVID-19 confinement. Int. J. Environ. Res. Public Health 2020, 17, 6878. [Google Scholar] [CrossRef] [PubMed]
- McDowell, C.P.; Herring, M.P.; Lansing, J.; Brower, C.; Meyer, J.D. Working from Home and Job Loss Due to the COVID-19 Pandemic Are Associated with Greater Time in Sedentary Behaviors. Front. Public Health 2020, 8, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Romero-Blanco, C.; Rodríguez-Almagro, J.; Onieva-Zafra, M.D.; Parra-Fernández, M.L.; Prado-Laguna, M.D.C.; Hernández-Martínez, A. Physical activity and sedentary lifestyle in university students: Changes during confinement due to the covid-19 pandemic. Int. J. Environ. Res. Public Health 2020, 17, 6567. [Google Scholar] [CrossRef] [PubMed]
- ZDF Intensivstationen: Warum Corona Minderheiten Härter Trifft—ZDFheute. Available online: https://www.zdf.de/nachrichten/panorama/corona-intensivstation-patienten-migrationshintergrund-100.html (accessed on 1 July 2021).
- Wunsch, K.; Nigg, C.; Niessner, C.; Schmidt, S.C.E.; Oriwol, D.; Hanssen-Doose, A.; Burchartz, A.; Eichsteller, A.; Kolb, S.; Worth, A.; et al. The Impact of COVID-19 on the Interrelation of Physical Activity, Screen Time and Health-Related Quality of Life in Children and Adolescents in Germany: Results of the Motorik-Modul Study—Supplement. Available online: https://www.mdpi.com/2227-9067/8/2/98#supplementary (accessed on 10 September 2021).
- Krug, S.; Jordan, S.; Mensink, G.B.M.; Müters, S.; Finger, J.; Lampert, T. Körperliche Aktivität: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundh.-Gesundh.-Gesundh. 2013, 56, 765–771. [Google Scholar] [CrossRef] [PubMed]
- Löwe, B.; Spitzer, R.L.; Zipfel, S.; Herzog, W.; Patient, P.; Questionnaire, H.; Klinische, A.; Allgemeinmedizin, S. Gesundheitsfragebogen für Patienten (PHQ-D). Manual und Testunterlagen. Pfizer. 2002. Available online: https://www.digotor.info/Downloads/Scores/PHQ-15.pdf?m=1615806367& (accessed on 10 September 2021).
- Bentlage, E.; Ammar, A.; How, D.; Ahmed, M.; Trabelsi, K.; Chtourou, H.; Brach, M. Practical recommendations for maintaining active lifestyle during the covid-19 pandemic: A systematic literature review. Int. J. Environ. Res. Public Health 2020, 17, 6265. [Google Scholar] [CrossRef] [PubMed]
- WHO. #HealthyAtHome—Physical Activity. Available online: https://www.who.int/news-room/campaigns/connecting-the-world-to-combat-coronavirus/healthyathome/healthyathome---physical-activity (accessed on 18 June 2021).
- American Heart Association (AHA). 25 Ways to Get Moving at Home. Available online: https://www.heart.org/en/healthy-living/fitness/getting-active/25-ways-to-get-moving-at-home-infographic (accessed on 18 June 2021).
- American College of Sports Medicine (ACSM). Staying Physically Active during the COVID-19 Pandemic. Available online: https://www.acsm.org/read-research/newsroom/news-releases/news-detail/2020/03/16/staying-physically-active-during-covid-19-pandemic (accessed on 18 June 2021).
- Reimers, A.K.; Brzoska, P.; Niessner, C.; Schmidt, S.C.E.; Worth, A.; Woll, A. Are there disparities in different domains of physical activity between school-aged migrant and non-migrant children and adolescents? Insights from Germany. PLoS ONE 2019, 14, e0214022. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walter, U.; Bisson, S.; Gerken, U.; Machleidt, W.; Krauth, C. Gesundheits- und Präventionsverhalten von Personen mit und ohne Migrationshintergrund. Gesundh. Suppl. 2015, 77, S85–S86. [Google Scholar] [CrossRef] [PubMed]
- Langøien, L.J.; Terragni, L.; Rugseth, G.; Nicolaou, M.; Holdsworth, M.; Stronks, K.; Lien, N.; Roos, G. Systematic mapping review of the factors influencing physical activity and sedentary behaviour in ethnic minority groups in Europe: A DEDIPAC study. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 99. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holdsworth, M.; Nicolaou, M.; Langøien, L.J.; Osei-Kwasi, H.A.; Chastin, S.F.M.; Stok, F.M.; Capranica, L.; Lien, N.; Terragni, L.; Monsivais, P.; et al. Developing a systems-based framework of the factors influencing dietary and physical activity behaviours in ethnic minority populations living in Europe—A DEDIPAC study. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 1–15. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ramchand, R.; Ahluwalia, S.C.; Xenakis, L.; Apaydin, E.; Raaen, L.; Grimm, G. A systematic review of peer-supported interventions for health promotion and disease prevention. Prev. Med. 2017, 101, 156–170. [Google Scholar] [CrossRef] [PubMed]
| Men N = 44 | Women N = 62 | Total N = 106 | |
|---|---|---|---|
| % or mean ± standard deviation | |||
| Sociodemographics | data | ||
| Age in years | 54.8 ± 10.9 | 53.2 ± 12.5 | 53.9 ± 11.8 |
| Educational level 1 | |||
| <10 years | 22.7 | 41.9 | 34.0 |
| 10–12 years | 47.7 | 33.9 | 39.6 |
| >12 years | 27.3 | 16.1 | 20.8 |
| Questionnaire language | |||
| German | 61.4 | 48.1 | 59.4 |
| Turkish | 38.6 | 41.9 | 40.6 |
| Own migration experience 1 | 88.6 | 77.8 | 82.0 |
| Employed (half or full time) | 54.8 | 38.3 | 45.1 |
| Health-related variables | |||
| Body mass index (BMI) 2 | 29.7 ± 4.7 | 29.3 ± 5.3 | 29.5 ± 5.1 |
| Normal weight (18.5 to <25.0 kg/m2) | 9.7 | 23.2 | 18.4 |
| Overweight (25.0 to <30.0 kg/m2) | 41.9 | 33.9 | 36.8 |
| Obesity (≥30.0 kg/m2) | 48.4 | 42.9 | 44.8 |
| Smoking behavior | |||
| Smoker | 34.1 | 30.0 | 31.7 |
| Ex-smoker | 22.7 | 28.3 | 26.0 |
| Never smoker | 43.2 | 41.7 | 42.3 |
| Physical activity before COVID-19 pandemic 2 | |||
| At least 150 min/week of moderate physical activity | 17.6 | 25.0 | 22.0 |
| Health status, self-reported | |||
| Good (including good, very good, excellent) | 86.4 | 71.0 | 77.4 |
| Poor (including less good, poor) | 13.6 | 29.0 | 22.6 |
| Depressive symptoms (≥10 points on PHQ-9 scale 3) | 25.0 | 34.5 | 30.5 |
| Predictors | Less Physical Activity in Transport, Leisure Time, and/or Sports | ||||
|---|---|---|---|---|---|
| Univariable | Multivariable 4 | ||||
| n | OR (95% CI) | p | OR (95% CI) | p | |
| Sociodemographics | |||||
| Age per year | 103 | 1.0 (1.0;1.1) | 0.383 | - | |
| Sex 1 | |||||
| Male vs. female | 103 | 0.5 (0.2;1.1) | 0.096 | 0.3 (0.1;0.9) | 0.032 |
| Educational level 1 | |||||
| <10 years | 100 | Ref | - | - | |
| 10–12 years | 2.0 (0.8;5.2) | 0.141 | - | - | |
| >12 years | 1.8 (0.6;5.5) | 0.300 | - | - | |
| Employed | |||||
| No vs. yes | 99 | 0.8 (0.4;1.9) | 0.636 | - | - |
| Migration-related variables | |||||
| Questionnaire language | |||||
| Turkish vs. German | 103 | 1.2 (0.5;2.8) | 0.678 | - | - |
| Own migration experience 1 | |||||
| No vs. yes | 87 | 2.7 (0.7;10.2) | 0.143 | - | - |
| Health-related variables | |||||
| Obesity vs. normal/overweight 2 | 85 | 1.3 (0.5;3.2) | 0.616 | 2.0 (0.6;6.9) | 0.254 |
| Never/ex-smokers vs. smokers | 101 | 0.6 (0.2;1.4) | 0.214 | 0.4 (0.1;1.4) | 0.146 |
| <150 min PA per week vs. ≥150 min PA per week (WHO recommendations)—before COVID-19 pandemic 2 | 80 | 2.6 (0.9;7.8) | 0.072 | 6.2 (1.7;22.6) | 0.006 |
| Subjective health status: poor (not so good or poor) vs. good (good, very good, or excellent) | 103 | 0.8 (0.3;2.1) | 0.633 | 0.3 (0.1;1.3) | 0.115 |
| Depressive symptoms (≥10 vs. <10 on PHQ-9 scale 3) | 95 | 1.4 (0.5;3.7) | 0.487 | - | - |
| Predictors | More Sedentary Behavior | ||||
|---|---|---|---|---|---|
| Univariable | Multivariable 4 | ||||
| n | OR (95% CI) | p | OR (95% CI) | p | |
| Sociodemographics | |||||
| Age per year | 100 | 1.0 (1.0;1.0) | 0.467 | - | - |
| Sex 1 | |||||
| Male vs. female | 100 | 0.7 (0.3;1.6) | 0.371 | 0.3 (0.1;0.9) | 0.040 |
| Educational level 1 | |||||
| <10 years | 100 | Ref | - | - | |
| 10–12 years | 1.5 (0.6;4.0) | 0.393 | - | - | |
| >12 years | 1.3 (0.4;4.2) | 0.610 | - | - | |
| Employed | |||||
| No vs. yes | 96 | 1.3 (0.5;3.0) | 0.575 | - | - |
| Migration-related variables | |||||
| Questionnaire language | |||||
| Turkish vs. German | 100 | 1.2 (0.5;2.7) | 0.682 | - | - |
| Own migration experience 1 | |||||
| No vs. yes | 84 | 1.0 (0.3;3.0) | 0.957 | - | - |
| Health-related variables | |||||
| Obesity vs. normal/overweight 2 | 82 | 1.5 (0.6;3.6) | 0.398 | 3.3 (1.0;10.4) | 0.043 |
| Never/ex-smokers vs. smokers | 98 | 1.0 (0.4;2.4) | 0.993 | - | - |
| <150 min PA per week vs. ≥150 min PA per week (WHO recommendations)—before COVID-19 pandemic 2 | 77 | 6.6 (1.4;31.2) | 0.009 | 19.3 (2.2;170.0) | 0.008 |
| Subjective health status: poor (not so good or poor) vs. good (good, very good, or excellent) | 100 | 1.3 (0.5;3.4) | 0.587 | - | - |
| Depressive symptoms (≥10 vs. <10 on PHQ-9 scale 3) | 92 | 2.4 (0.9;5.9) | 0.062 | - | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Krist, L.; Dornquast, C.; Reinhold, T.; Icke, K.; Danquah, I.; Willich, S.N.; Becher, H.; Keil, T. Predictors of Changes in Physical Activity and Sedentary Behavior during the COVID-19 Pandemic in a Turkish Migrant Cohort in Germany. Int. J. Environ. Res. Public Health 2021, 18, 9682. https://doi.org/10.3390/ijerph18189682
Krist L, Dornquast C, Reinhold T, Icke K, Danquah I, Willich SN, Becher H, Keil T. Predictors of Changes in Physical Activity and Sedentary Behavior during the COVID-19 Pandemic in a Turkish Migrant Cohort in Germany. International Journal of Environmental Research and Public Health. 2021; 18(18):9682. https://doi.org/10.3390/ijerph18189682
Chicago/Turabian StyleKrist, Lilian, Christina Dornquast, Thomas Reinhold, Katja Icke, Ina Danquah, Stefan N. Willich, Heiko Becher, and Thomas Keil. 2021. "Predictors of Changes in Physical Activity and Sedentary Behavior during the COVID-19 Pandemic in a Turkish Migrant Cohort in Germany" International Journal of Environmental Research and Public Health 18, no. 18: 9682. https://doi.org/10.3390/ijerph18189682
APA StyleKrist, L., Dornquast, C., Reinhold, T., Icke, K., Danquah, I., Willich, S. N., Becher, H., & Keil, T. (2021). Predictors of Changes in Physical Activity and Sedentary Behavior during the COVID-19 Pandemic in a Turkish Migrant Cohort in Germany. International Journal of Environmental Research and Public Health, 18(18), 9682. https://doi.org/10.3390/ijerph18189682








