Resilience, Coping Strategies and Posttraumatic Growth in the Workplace Following COVID-19: A Narrative Review on the Positive Aspects of Trauma
Abstract
:1. Introduction
2. Materials and Methods
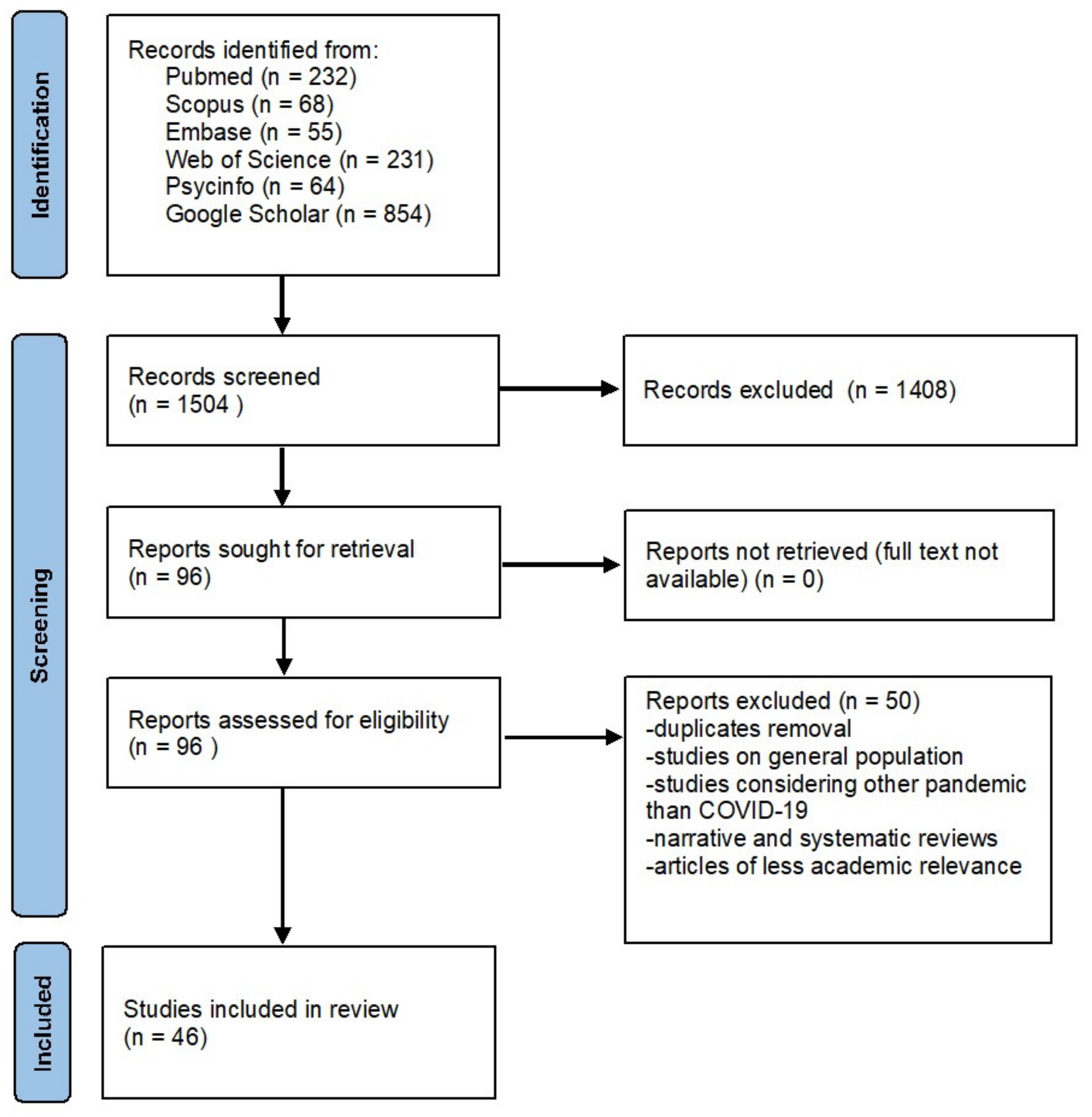
2.1. Literature Research and Data Collection
- Population: Workers from any sector.
- Intervention: The consequences of the COVID-19 pandemic in the workplace.
- Comparison: Not considered.
- Outcome: Resilience, coping strategies, posttraumatic growth, personal growth.
2.2. Inclusion Criteria
2.3. Exclusion Criteria
3. Results
3.1. Resilience
3.2. Coping Strategies
3.3. Posttraumatic Growth (PTG)
4. Discussion
4.1. Strengths and Limitations
4.2. Practical Implications
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19. 11 March 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed on 11 March 2020).
- Skegg, D.; Gluckman, P.; Boulton, G.; Hackmann, H.; Karim, S.S.A.; Piot, P.; Woopen, C. Future Scenarios for the COVID-19 Pandemic. Lancet 2021, 397, 777–778. [Google Scholar] [CrossRef]
- Heath, C.; Sommerfield, A.; von Ungern-Sternberg, B.S. Resilience Strategies to Manage Psychological Distress among Healthcare Workers during the COVID-19 Pandemic: A Narrative Review. Anaesthesia 2020, 75, 1364–1371. [Google Scholar] [CrossRef]
- Batra, K.; Singh, T.P.; Sharma, M.; Batra, R.; Schvaneveldt, N. Investigating the Psychological Impact of COVID-19 among Healthcare Workers: A Meta-Analysis. Int. J. Environ. Res. Public Health 2020, 17, 9096. [Google Scholar] [CrossRef]
- Schwartz, R.; Sinskey, J.L.; Anand, U.; Margolis, R.D. Addressing Postpandemic Clinician Mental Health: A Narrative Review and Conceptual Framework. Ann. Intern. Med. 2020, 173, 981–988. [Google Scholar] [CrossRef]
- Temsah, M.-H.; Al-Sohime, F.; Alamro, N.; Al-Eyadhy, A.; Al-Hasan, K.; Jamal, A.; Al-Maglouth, I.; Aljamaan, F.; Al Amri, M.; Barry, M.; et al. The Psychological Impact of COVID-19 Pandemic on Health Care Workers in a MERS-CoV Endemic Country. J. Infect. Public Health 2020, 13, 877–882. [Google Scholar] [CrossRef]
- Maunder, R.; Lancee, W.; Balderson, K.; Bennett, J.; Borgundvaag, B.; Evans, S.; Fernandes, C.; Goldbloom, D.; Gupta, M.; Hunter, J.; et al. Long-Term Psychological and Occupational Effects of Providing Hospital Healthcare during SARS Outbreak. Emerg. Infect. Dis. 2006, 12, 1924–1932. [Google Scholar] [CrossRef]
- Giorgi, G.; Lecca, L.I.; Alessio, F.; Finstad, G.L.; Bondanini, G.; Lulli, L.G.; Arcangeli, G.; Mucci, N. COVID-19-Related Mental Health Effects in the Workplace: A Narrative Review. Int. J. Environ. Res. Public Health 2020, 17, 7857. [Google Scholar] [CrossRef]
- Pappa, S.; Ntella, V.; Giannakas, T.; Giannakoulis, V.G.; Papoutsi, E.; Katsaounou, P. Prevalence of Depression, Anxiety, and Insomnia among Healthcare Workers during the COVID-19 Pandemic: A Systematic Review and Meta-Analysis. Brain Behav. Immun. 2020, 88, 901–907. [Google Scholar] [CrossRef] [PubMed]
- Horesh, D.; Brown, A.D. Traumatic Stress in the Age of COVID-19: A Call to Close Critical Gaps and Adapt to New Realities. Psychol. Trauma Theory Res. Pract. Policy 2020, 12, 331–335. [Google Scholar] [CrossRef]
- Brooks, S.; Amlôt, R.; Rubin, G.J.; Greenberg, N. Psychological Resilience and Post-Traumatic Growth in Disaster-Exposed Organisations: Overview of the Literature. BMJ Mil. Health 2020, 166, 52–56. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bonanno, G.A. Loss, Trauma, and Human Resilience: Have We Underestimated the Human Capacity to Thrive After Extremely Aversive Events? Am. Psychol. 2004, 59, 20–28. [Google Scholar] [CrossRef] [Green Version]
- Tedeschi, R.G.; Calhoun, L.G. The Posttraumatic Growth Inventory: Measuring the Positive Legacy of Trauma. J. Traum. Stress 1996, 9, 455–471. [Google Scholar] [CrossRef]
- Tedeschi, R.G.; Calhoun, L.G. TARGET ARTICLE: “Posttraumatic Growth: Conceptual Foundations and Empirical Evidence”. Psychol. Inq. 2004, 15, 1–18. [Google Scholar] [CrossRef]
- Maitlis, S. Posttraumatic Growth at Work. Annu. Rev. Organ. Psychol. Organ. Behav. 2020, 7, 395–419. [Google Scholar] [CrossRef] [Green Version]
- Ramos, C.; Leal, I. Posttraumatic Growth in the Aftermath of Trauma: A Literature Review About Related Factors and Application Contexts. Psychol. Commun. Health 2013, 2, 43–54. [Google Scholar] [CrossRef] [Green Version]
- Hyun, H.S.; Kim, M.J.; Lee, J.H. Factors Associated With Post-Traumatic Growth Among Healthcare Workers Who Experienced the Outbreak of MERS Virus in South Korea: A Mixed-Method Study. Front. Psychol. 2021, 12, 541510. [Google Scholar] [CrossRef]
- Blanc, J.; Briggs, A.Q.; Seixas, A.A.; Reid, M.; Jean-Louis, G.; Pandi-Perumal, S.R. Addressing Psychological Resilience during the Coronavirus Disease 2019 Pandemic: A Rapid Review. Curr. Opin. Psychiatry 2021, 34, 29–35. [Google Scholar] [CrossRef]
- Littleton, H.; Horsley, S.; John, S.; Nelson, D.V. Trauma Coping Strategies and Psychological Distress: A Meta-Analysis. J. Traum. Stress 2007, 20, 977–988. [Google Scholar] [CrossRef] [PubMed]
- Hartmann, S.; Weiss, M.; Newman, A.; Hoegl, M. Resilience in the Workplace: A Multilevel Review and Synthesis. Appl. Psychol. 2020, 69, 913–959. [Google Scholar] [CrossRef]
- Kunzler, A.M.; Helmreich, I.; König, J.; Chmitorz, A.; Wessa, M.; Binder, H.; Lieb, K. Psychological Interventions to Foster Resilience in Healthcare Students. Cochrane Database Syst. Rev. 2020. [Google Scholar] [CrossRef]
- Morse, J.M.; Kent-Marvick, J.; Barry, L.A.; Harvey, J.; Okang, E.N.; Rudd, E.A.; Wang, C.-Y.; Williams, M.R. Developing the Resilience Framework for Nursing and Healthcare. Glob. Qual. Nurs. Res. 2021, 8, 233339362110054. [Google Scholar] [CrossRef]
- Kang, X.; Fang, Y.; Li, S.; Liu, Y.; Zhao, D.; Feng, X.; Wang, Y.; Li, P. The Benefits of Indirect Exposure to Trauma: The Relationships among Vicarious Posttraumatic Growth, Social Support, and Resilience in Ambulance Personnel in China. Psychiatry Investig. 2018, 15, 452–459. [Google Scholar] [CrossRef] [Green Version]
- Thompson, N.J.; Fiorillo, D.; Rothbaum, B.O.; Ressler, K.J.; Michopoulos, V. Coping Strategies as Mediators in Relation to Resilience and Posttraumatic Stress Disorder. J. Affect. Disord. 2018, 225, 153–159. [Google Scholar] [CrossRef]
- Rajandram, R.K.; Jenewein, J.; McGrath, C.; Zwahlen, R.A. Coping Processes Relevant to Posttraumatic Growth: An Evidence-Based Review. Support Care Cancer 2011, 19, 583–589. [Google Scholar] [CrossRef] [Green Version]
- Bonanno, G.A.; Galea, S.; Bucciarelli, A.; Vlahov, D. Psychological Resilience After Disaster: New York City in the Aftermath of the September 11th Terrorist Attack. Psychol. Sci. 2006, 17, 181–186. [Google Scholar] [CrossRef] [PubMed]
- Galea, S.; Ahern, J.; Resnick, H.; Kilpatrick, D.; Bucuvalas, M.; Gold, J.; Vlahov, D. Psychological Sequelae of the September 11 Terrorist Attacks in New York City. N. Engl. J. Med. 2002, 346, 982–987. [Google Scholar] [CrossRef]
- Joseph, S.; Murphy, D.; Regel, S. An Affective-Cognitive Processing Model of Post-Traumatic Growth: An Affective-Cognitive Processing Model of Post-Traumatic Growth. Clin. Psychol. Psychother. 2012, 19, 316–325. [Google Scholar] [CrossRef]
- Manning-Jones, S.; de Terte, I.; Stephens, C. Vicarious Posttraumatic Growth: A Systematic Literature Review. Int. J. Wellbeing 2015, 5, 125–139. [Google Scholar] [CrossRef]
- Pan Cui, P.; pan Wang, P.; Wang, K.; Ping, Z.; Wang, P.; Chen, C. Post-Traumatic Growth and Influencing Factors among Frontline Nurses Fighting against COVID-19. Occup. Environ. Med. 2021, 78, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Nowicki, G.J.; Ślusarska, B.; Tucholska, K.; Naylor, K.; Chrzan-Rodak, A.; Niedorys, B. The Severity of Traumatic Stress Associated with COVID-19 Pandemic, Perception of Support, Sense of Security, and Sense of Meaning in Life among Nurses: Research Protocol and Preliminary Results from Poland. Int. J. Environ. Res. Public Health 2020, 17, 6491. [Google Scholar] [CrossRef] [PubMed]
- Lee, N.; Lee, H.-J. South Korean Nurses’ Experiences with Patient Care at a COVID-19-Designated Hospital: Growth after the Frontline Battle against an Infectious Disease Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 9015. [Google Scholar] [CrossRef] [PubMed]
- Kalaitzaki, A.; Rovithis, M. Secondary Traumatic Stress and Vicarious Posttraumatic Growth in Healthcare Workers during the First COVID-19 Lockdown in Greece: The Role of Resilience and Coping Strategies. Psychiatriki 2021. [Google Scholar] [CrossRef]
- Kowalski, R.M.; Carroll, H.; Britt, J. Finding the Silver Lining in the COVID-19 Crisis. J. Health Psychol. 2021, 135910532199908. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Ju, X.; Liu, X. The Relationship between Resilience and Intent to Stay among Chinese Nurses to Support Wuhan in Managing COVID-19: The Serial Mediation Effect of Post-traumatic Growth and Perceived Professional Benefits. Nurs. Open 2021, 8, 2866–2876. [Google Scholar] [CrossRef]
- Chen, R.; Sun, C.; Chen, J.; Jen, H.; Kang, X.L.; Kao, C.; Chou, K. A Large-Scale Survey on Trauma, Burnout, and Posttraumatic Growth among Nurses during the COVID-19 Pandemic. Int. J. Ment. Health Nurs. 2021, 30, 102–116. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Jiménez, J.E.; Blanco-Donoso, L.M.; Demerouti, E.; Belda Hofheinz, S.; Chico-Fernández, M.; Moreno-Jiménez, B.; Garrosa, E. The Role of Healthcare Professionals’ Passion in Predicting Secondary Traumatic Stress and Posttraumatic Growth in the Face of COVID-19: A Longitudinal Approach. Int. J. Environ. Res. Public Health 2021, 18, 4453. [Google Scholar] [CrossRef]
- Babore, A.; Lombardi, L.; Viceconti, M.L.; Pignataro, S.; Marino, V.; Crudele, M.; Candelori, C.; Bramanti, S.M.; Trumello, C. Psychological Effects of the COVID-2019 Pandemic: Perceived Stress and Coping Strategies among Healthcare Professionals. Psychiatry Res. 2020, 293, 113366. [Google Scholar] [CrossRef]
- Hines, S.E.; Chin, K.H.; Glick, D.R.; Wickwire, E.M. Trends in Moral Injury, Distress, and Resilience Factors among Healthcare Workers at the Beginning of the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 488. [Google Scholar] [CrossRef]
- Serrão, C.; Duarte, I.; Castro, L.; Teixeira, A. Burnout and Depression in Portuguese Healthcare Workers during the COVID-19 Pandemic—The Mediating Role of Psychological Resilience. Int. J. Environ. Res. Public Health 2021, 18, 636. [Google Scholar] [CrossRef]
- Zadok-Gurman, T.; Jakobovich, R.; Dvash, E.; Zafrani, K.; Rolnik, B.; Ganz, A.B.; Lev-Ari, S. Effect of Inquiry-Based Stress Reduction (IBSR) Intervention on Well-Being, Resilience and Burnout of Teachers during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 3689. [Google Scholar] [CrossRef]
- Lorente, L.; Vera, M.; Peiró, T. Nurses´ Stressors and Psychological Distress during the COVID-19 Pandemic: The Mediating Role of Coping and Resilience. J. Adv. Nurs. 2021, 77, 1335–1344. [Google Scholar] [CrossRef] [PubMed]
- Munawar, K.; Choudhry, F.R. Exploring Stress Coping Strategies of Frontline Emergency Health Workers Dealing Covid-19 in Pakistan: A Qualitative Inquiry. Am. J. Infect. Control 2021, 49, 286–292. [Google Scholar] [CrossRef] [PubMed]
- Hong, Y.; Lee, J.; Lee, H.J.; Kim, K.; Cho, I.-K.; Ahn, M.H.; Shin, Y.-W.; Park, J.; Chung, S. Resilience and Work-Related Stress May Affect Depressive Symptoms in Nursing Professionals during the COVID-19 Pandemic Era. Psychiatry Investig. 2021, 18, 357–363. [Google Scholar] [CrossRef] [PubMed]
- Afshari, D.; Nourollahi-darabad, M.; Chinisaz, N. Demographic Predictors of Resilience among Nurses during the COVID-19 Pandemic. Work 2021, 68, 297–303. [Google Scholar] [CrossRef] [PubMed]
- Mosheva, M.; Hertz-Palmor, N.; Dorman Ilan, S.; Matalon, N.; Pessach, I.M.; Afek, A.; Ziv, A.; Kreiss, Y.; Gross, R.; Gothelf, D. Anxiety, Pandemic-related Stress and Resilience among Physicians during the COVID-19 Pandemic. Depress. Anxiety 2020, 37, 965–971. [Google Scholar] [CrossRef]
- Shechter, A.; Diaz, F.; Moise, N.; Anstey, D.E.; Ye, S.; Agarwal, S.; Birk, J.L.; Brodie, D.; Cannone, D.E.; Chang, B.; et al. Psychological Distress, Coping Behaviors, and Preferences for Support among New York Healthcare Workers during the COVID-19 Pandemic. Gen. Hosp. Psychiatry 2020, 66, 1–8. [Google Scholar] [CrossRef]
- Huang, L.; Lei, W.; Xu, F.; Liu, H.; Yu, L. Emotional Responses and Coping Strategies in Nurses and Nursing Students during Covid-19 Outbreak: A Comparative Study. PLoS ONE 2020, 15, e0237303. [Google Scholar] [CrossRef]
- Vagni, M.; Maiorano, T.; Giostra, V.; Pajardi, D. Coping With COVID-19: Emergency Stress, Secondary Trauma and Self-Efficacy in Healthcare and Emergency Workers in Italy. Front. Psychol. 2020, 11, 566912. [Google Scholar] [CrossRef] [PubMed]
- Tahara, M.; Mashizume, Y.; Takahashi, K. Coping Mechanisms: Exploring Strategies Utilized by Japanese Healthcare Workers to Reduce Stress and Improve Mental Health during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 18, 131. [Google Scholar] [CrossRef]
- Prazeres, F.; Passos, L.; Simões, J.A.; Simões, P.; Martins, C.; Teixeira, A. COVID-19-Related Fear and Anxiety: Spiritual-Religious Coping in Healthcare Workers in Portugal. Int. J. Environ. Res. Public Health 2020, 18, 220. [Google Scholar] [CrossRef]
- Bozdağ, F.; Ergün, N. Psychological Resilience of Healthcare Professionals During COVID-19 Pandemic. Psychol. Rep. 2020, 003329412096547. [Google Scholar] [CrossRef]
- Lyu, Y.; Yu, Y.; Chen, S.; Lu, S.; Ni, S. Positive Functioning at Work during COVID-19: Posttraumatic Growth, Resilience, and Emotional Exhaustion in Chinese Frontline Healthcare Workers. Appl. Psychol. Health Well-Being 2021. [Google Scholar] [CrossRef]
- Huffman, E.M.; Athanasiadis, D.I.; Anton, N.E.; Haskett, L.A.; Doster, D.L.; Stefanidis, D.; Lee, N.K. How Resilient Is Your Team? Exploring Healthcare Providers’ Well-Being during the COVID-19 Pandemic. Am. J. Surg. 2021, 221, 277–284. [Google Scholar] [CrossRef] [PubMed]
- Ojo, A.O.; Fawehinmi, O.; Yusliza, M.Y. Examining the Predictors of Resilience and Work Engagement during the COVID-19 Pandemic. Sustainability 2021, 13, 2902. [Google Scholar] [CrossRef]
- MacIntyre, P.D.; Gregersen, T.; Mercer, S. Language Teachers’ Coping Strategies during the Covid-19 Conversion to Online Teaching: Correlations with Stress, Wellbeing and Negative Emotions. System 2020, 94, 102352. [Google Scholar] [CrossRef]
- Vagni, M.; Maiorano, T.; Giostra, V.; Pajardi, D. Hardiness, Stress and Secondary Trauma in Italian Healthcare and Emergency Workers during the COVID-19 Pandemic. Sustainability 2020, 12, 5592. [Google Scholar] [CrossRef]
- Li, L.; Mao, M.; Wang, S.; Yin, R.; Yan, H.; Jin, Y.; Cheng, Y. Posttraumatic Growth in Chinese Nurses and General Public during the COVID-19 Outbreak. Psychol. Health Med. 2021, 1–11. [Google Scholar] [CrossRef]
- Luu, T.T. Worker Resilience during the COVID-19 Crisis: The Role of Core Beliefs Challenge, Emotion Regulation, and Family Strain. Personal. Individ. Differ. 2021, 179, 110784. [Google Scholar] [CrossRef]
- Fino, E.; Bonfrate, I.; Fino, V.; Bocus, P.; Russo, P.M.; Mazzetti, M. Harnessing Distress to Boost Growth in Frontline Healthcare Workers during COVID-19 Pandemic: The Protective Role of Resilience, Emotion Regulation and Social Support. Psychol. Med. 2021, 1–3. [Google Scholar] [CrossRef]
- Li, X.; Zhou, Y.; Xu, X. Factors Associated with the Psychological Well-being among Front-line Nurses Exposed to COVID-2019 in China: A Predictive Study. J. Nurs. Manag. 2021, 29, 240–249. [Google Scholar] [CrossRef]
- Zhang, X.; Jiang, X.; Ni, P.; Li, H.; Li, C.; Zhou, Q.; Ou, Z.; Guo, Y.; Cao, J. Association between Resilience and Burnout of Front-line Nurses at the Peak of the COVID-19 Pandemic: Positive and Negative Affect as Mediators in Wuhan. Int. J. Ment. Health Nurs. 2021, 30, 939–954. [Google Scholar] [CrossRef]
- Banerjee, D.; Sathyanarayana Rao, T.S.; Kallivayalil, R.A.; Javed, A. Psychosocial Framework of Resilience: Navigating Needs and Adversities during the Pandemic, a Qualitative Exploration in the Indian Frontline Physicians. Front. Psychol. 2021, 12, 622132. [Google Scholar] [CrossRef]
- Coulombe, S.; Pacheco, T.; Cox, E.; Khalil, C.; Doucerain, M.M.; Auger, E.; Meunier, S. Risk and Resilience Factors during the COVID-19 Pandemic: A Snapshot of the Experiences of Canadian Workers Early on in the Crisis. Front. Psychol. 2020, 11, 580702. [Google Scholar] [CrossRef] [PubMed]
- Croghan, I.T.; Chesak, S.S.; Adusumalli, J.; Fischer, K.M.; Beck, E.W.; Patel, S.R.; Ghosh, K.; Schroeder, D.R.; Bhagra, A. Stress, Resilience, and Coping of Healthcare Workers during the COVID-19 Pandemic. J. Prim. Care Community Health 2021, 12, 215013272110084. [Google Scholar] [CrossRef] [PubMed]
- Di Giuseppe, M.; Nepa, G.; Prout, T.A.; Albertini, F.; Marcelli, S.; Orrù, G.; Conversano, C. Stress, Burnout, and Resilience among Healthcare Workers during the COVID-19 Emergency: The Role of Defense Mechanisms. Int. J. Environ. Res. Public Health 2021, 18, 5258. [Google Scholar] [CrossRef] [PubMed]
- Di Trani, M.; Mariani, R.; Ferri, R.; De Berardinis, D.; Frigo, M.G. From Resilience to Burnout in Healthcare Workers During the COVID-19 Emergency: The Role of the Ability to Tolerate Uncertainty. Front. Psychol. 2021, 12, 646435. [Google Scholar] [CrossRef]
- Fleuren, B.P.I.; Poesen, L.T.; Gifford, R.E.; Zijlstra, F.R.H.; Ruwaard, D.; van de Baan, F.C.; Westra, D.D. We’re Not Gonna Fall: Depressive Complaints, Personal Resilience, Team Social Climate, and Worries about Infections among Hospital Workers during a Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 4701. [Google Scholar] [CrossRef]
- Hou, T.; Zhang, T.; Cai, W.; Song, X.; Chen, A.; Deng, G.; Ni, C. Social Support and Mental Health among Health Care Workers during Coronavirus Disease 2019 Outbreak: A Moderated Mediation Model. PLoS ONE 2020, 15, e0233831. [Google Scholar] [CrossRef]
- Jose, S.; Dhandapani, M.; Cyriac, M. Burnout and Resilience among Frontline Nurses during COVID-19 Pandemic: A Cross-Sectional Study in the Emergency Department of a Tertiary Care Center, North India. Indian J. Crit. Care Med. 2020, 24, 1081–1088. [Google Scholar] [CrossRef]
- Lin, J.; Ren, Y.-H.; Gan, H.-J.; Chen, Y.; Huang, Y.-F.; You, X.-M. Factors Associated with Resilience among Non-Local Medical Workers Sent to Wuhan, China during the COVID-19 Outbreak. BMC Psychiatry 2020, 20, 417. [Google Scholar] [CrossRef]
- Maiorano, T.; Vagni, M.; Giostra, V.; Pajardi, D. COVID-19: Risk Factors and Protective Role of Resilience and Coping Strategies for Emergency Stress and Secondary Trauma in Medical Staff and Emergency Workers—An Online-Based Inquiry. Sustainability 2020, 12, 9004. [Google Scholar] [CrossRef]
- McFadden, P.; Ross, J.; Moriarty, J.; Mallett, J.; Schroder, H.; Ravalier, J.; Manthorpe, J.; Currie, D.; Harron, J.; Gillen, P. The Role of Coping in the Wellbeing and Work-Related Quality of Life of UK Health and Social Care Workers during COVID-19. Int. J. Environ. Res. Public Health 2021, 18, 815. [Google Scholar] [CrossRef]
- Roca, J.; Canet-Vélez, O.; Cemeli, T.; Lavedán, A.; Masot, O.; Botigué, T. Experiences, Emotional Responses, and Coping Skills of Nursing Students as Auxiliary Health Workers during the Peak COVID-19 Pandemic: A Qualitative Study. Int. J. Ment. Health Nurs. 2021. [Google Scholar] [CrossRef] [PubMed]
- Zhou, T.; Guan, R.; Sun, L. Perceived Organizational Support and PTSD Symptoms of Frontline Healthcare Workers in the Outbreak of COVID-19 in Wuhan: The Mediating Effects of Self-efficacy and Coping Strategies. Appl. Psychol. Health Well-Being 2021. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. J. Clin. Epidemiol. 2021, 134, 178–189. [Google Scholar] [CrossRef] [PubMed]
- Joseph, S.; Williams, R.; Yule, W. Changes in Outlook Following Disaster: The Preliminary Development of a Measure to Assess Positive and Negative Responses. J. Traum. Stress 1993, 6, 271–279. [Google Scholar] [CrossRef]
- Sigahi, T.F.A.C.; Kawasaki, B.C.; Bolis, I.; Morioka, S.N. A Systematic Review on the Impacts of Covid-19 on Work: Contributions and a Path Forward from the Perspectives of Ergonomics and Psychodynamics of Work. Hum. Factors Man. 2021, 31, 375–388. [Google Scholar] [CrossRef]
- Sanchez-Gomez, M.; Giorgi, G.; Finstad, G.L.; Urbini, F.; Foti, G.; Mucci, N.; Zaffina, S.; León-Perez, J.M. COVID-19 Pandemic as a Traumatic Event and Its Associations with Fear and Mental Health: A Cognitive-Activation Approach. Int. J. Environ. Res. Public Health 2021, 18, 7422. [Google Scholar] [CrossRef]
- World Health Organization COVID-19: Operational Planning Guidelines and COVID-19 Partners Platform to Support Country Preparedness and Response. Available online: https://openwho.org/courses/UNCT-COVID19-preparedness-and-response-EN (accessed on 16 July 2021).
- Adams, J.G.; Walls, R.M. Supporting the Health Care Workforce During the COVID-19 Global Epidemic. JAMA 2020, 323, 1439. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vinkers, C.H.; van Amelsvoort, T.; Bisson, J.I.; Branchi, I.; Cryan, J.F.; Domschke, K.; Howes, O.D.; Manchia, M.; Pinto, L.; de Quervain, D.; et al. Stress Resilience during the Coronavirus Pandemic. Eur. Neuropsychopharmacol. 2020, 35, 12–16. [Google Scholar] [CrossRef]
- Baldassarre, A.; Giorgi, G.; Alessio, F.; Lulli, L.; Arcangeli, G.; Mucci, N. Stigma and Discrimination (SAD) at the Time of the SARS-CoV-2 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 6341. [Google Scholar] [CrossRef]
- Rangachari, P.; Woods, J.L. Preserving Organizational Resilience, Patient Safety, and Staff Retention during COVID-19 Requires a Holistic Consideration of the Psychological Safety of Healthcare Workers. Int. J. Environ. Res. Public Health 2020, 17, 4267. [Google Scholar] [CrossRef]
- Kreh, A.; Brancaleoni, R.; Magalini, S.C.; Chieffo, D.P.R.; Flad, B.; Ellebrecht, N.; Juen, B. Ethical and Psychosocial Considerations for Hospital Personnel in the Covid-19 Crisis: Moral Injury and Resilience. PLoS ONE 2021, 16, e0249609. [Google Scholar] [CrossRef]
- Rieckert, A.; Schuit, E.; Bleijenberg, N.; ten Cate, D.; de Lange, W.; de Man-van Ginkel, J.M.; Mathijssen, E.; Smit, L.C.; Stalpers, D.; Schoonhoven, L.; et al. How Can We Build and Maintain the Resilience of Our Health Care Professionals during COVID-19? Recommendations Based on a Scoping Review. BMJ Open 2021, 11, e043718. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. COVID-19: Occupational Health and Safety for Health Workers. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-HCW_advice-2021.1 (accessed on 17 July 2021).
- Preti, E.; Di Mattei, V.; Perego, G.; Ferrari, F.; Mazzetti, M.; Taranto, P.; Di Pierro, R.; Madeddu, F.; Calati, R. The Psychological Impact of Epidemic and Pandemic Outbreaks on Healthcare Workers: Rapid Review of the Evidence. Curr. Psychiatry Rep. 2020, 22, 43. [Google Scholar] [CrossRef]
- Cabarkapa, S.; Nadjidai, S.E.; Murgier, J.; Ng, C.H. The Psychological Impact of COVID-19 and Other Viral Epidemics on Frontline Healthcare Workers and Ways to Address It: A Rapid Systematic Review. Brain Behav. Immun. Health 2020, 8, 100144. [Google Scholar] [CrossRef] [PubMed]
- Thoresen, S.; Tønnessen, A.; Lindgaard, C.V.; Andreassen, A.L.; Weisaeth, L. Stressful but Rewarding: Norwegian Personnel Mobilised for the 2004 Tsunami Disaster. Disasters 2009, 33, 353–368. [Google Scholar] [CrossRef] [PubMed]
- Bakhshi, S.; Lynn-Nicholson, R.; Jones, B.; Amlôt, R.; Greenberg, N.; Rubin, G.J. Responding to a Radiological Crisis: Experiences of British Foreign Office Staff in Japan After the Fukushima Nuclear Meltdown. Disaster Med. Public Health Prep. 2014, 8, 397–403. [Google Scholar] [CrossRef] [Green Version]
- Shih, F.-J.; Liao, Y.-C.; Chan, S.-M.; Duh, B.-R.; Gau, M.-L. The Impact of the 9–21 Earthquake Experiences of Taiwanese Nurses as Rescuers. Soc. Sci. Med. 2002, 55, 659–672. [Google Scholar] [CrossRef]
- Yang, Y.-N.; Xiao, L.D.; Cheng, H.-Y.; Zhu, J.-C.; Arbon, P. Chinese Nurses’ Experience in the Wenchuan Earthquake Relief: Nurses’ Experience in the Wenchuan Earthquake. Int. Nurs. Rev. 2010, 57, 217–223. [Google Scholar] [CrossRef]
- Berah, E.F.; Jones, H.J.; Valent, P. The Experience of a Mental Health Team Involved in the Early Phase of a Disaster. Aust. N. Z. J. Psychiatry 1984, 18, 354–358. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.L.; Chan, C.L.W.; Shi, Z.B.; Wang, B. Mental Health Risks in the Local Workforce Engaged in Disaster Relief and Reconstruction. Qual. Health Res. 2013, 23, 207–217. [Google Scholar] [CrossRef] [PubMed]
- Lopez, S.J.; Prosser, E.C.; Edwards, L.M.; Magyar-Moe, J.L.; Neufeld, J.E.; Rasmussen, H.N. Putting positive psychology in a multicultural context. In Handbook of Positive Psychology; Oxford University Press: New York, NY, USA, 2002; pp. 700–714. ISBN 0-19-513533-4. [Google Scholar]
| Reference | Research Design/Sample/Nation | Variables Considered/Main Aims | Brief Summary | Topic |
|---|---|---|---|---|
| Cui et al. [30] | Cross-sectional/167 frontline nurses/China | Post-traumatic growth (PTG) prevalence/rumination/socio-demographic variables. | In the sample of nurses, the level of PTG was medium to high. This was influenced by years of work, self-confidence with respect to frontline work, risk awareness, psychological training and deliberate rumination. | PTG |
| Nowicki et al. [31] | Cross-sectional/325 nurses/Poland | Level of post-traumatic stress/perceived social support/opinions about the positive and negative consequences of the pandemic/sense of security and sense of meaning. | The team of nurses presented with intense post-traumatic symptoms with high avoidance symptoms. The pandemic had induced a reduced sense of security with an intense reflection on issues related to the security of oneself, others and the world. The respondents valued the meaning of life but were less likely to seek it out. In addition, PTG was detected, highlighted by positive changes in the existing situation. | PTG |
| Lee and Lee [32] | Qualitative study/Nurses with at least 1 year of general experience and 2 months of experience in a COVID-19 ward/South Korea | Experience in patient care in a COVID-19 hospital. | Nine themes were identified: pushed onto the battlefield without any preparation, fighting on the front line, altered daily life, low morale, unexpectedly long war, ambivalence towards patients, forces that keep me going, giving meaning to my work and taking another step forward in one’s own growth. Nurses who have interfaced with COVID-19 patients have experienced both negative and positive consequences such as PTG. | PTG |
| Kalaitzaki and Rovithis [33] | Cross-sectional/673 healthcare workers/Greece | The role of resilience and coping strategies in the secondary stress of Greek health workers and PTG following lockdown. Secondary traumatic stress (STS) and vicarious posttraumatic growth (VPTG). | The results suggested that greater resilience corresponded to lower levels of STS and higher levels of VPTG. PTG was associated with the use of positive coping strategies. | PTG, RESILIENCE AND COPING STRATEGIES |
| Kowalski et al. [34] | Brief report/179 Mechanical Turk workers/United States of America (USA) | Benefit seeking, PTG, coping style (positive reframing), optimism/pessimism, gratitude, general well-being, personal satisfaction. | Results showed a decline in satisfaction with work, leisure, fitness, mental health and finances in the midst of the pandemic. Benefit finding in relation to COVID-19 was significantly related to PTG, coping, gratitude and mental health. The most common positive aspects of the pandemic included more time with family and friends, a slower pace of life and improvements in physical health. | PTG AND COPING STRATEGIES |
| Liu et al. [35] | Cross-sectional/200 nurses/China | PTG, perceived job benefits, resilience and intention to stay at work. | The results showed that resilience had the strongest direct effect on intention to stay. Perceived professional benefits were a mediating factor in the association between resilience and intention to stay. The multiple serial mediations of PTG and perceived occupational benefits in the relationship between resilience and intention to stay were statistically significant. | PTG AND RESILIENCE |
| Chen et al. [36] | Cross-sectional/12,596 nurses/Not available (N.A.) | Assessment of trauma, burnout, PTG and influence of associated factors such as age, gender, level of education, assignment, affiliated department and patient care with COVID-19. | Nurses, ICU nurses, nurses working in COVID-19 hospitals and wards involved in treating COVID-19 patients all have worse mental health outcomes. | PTG |
| Moreno-Jiménez et al. [37] | Longitudinal study/172 health professionals/Spain | Workload, fear of infection, lack of staff and personal protective equipment (PPE), harmonious passion, STS and PTG. | Results revealed that in the second survey, workload and fear of contagion were positive predictors for STS, whereas harmonious passion was a negative predictor. Fear of contagion at time 1 and time 2 seemed to positively predict PTG, as did harmonious passion. Lack of staff/PPE, appeared to be a moderator as PTG was greater when workload was high, particularly in those with a high staff/PPE shortages. | PTG |
| Babore et al. [38] | Cross-sectional/595 healthcare professionals/Italy | Protective and risk factors for stress with reference to: socio-demographic variables, direct exposure to COVID-19 and coping strategies | The results suggested that a positive attitude towards the stressful situation was the main protective factor. Social support seeking, avoidance strategies and working with COVID-19 patients were risk factors. | COPING STRATEGIES |
| Hines et al. [39] | Longitudinal study/96 healthcare workers/USA | Moral injury and distress scores are expected to be higher during the first three months of the COVID-19 pandemic and should be affected by resilience factors such as job type, social support and sleep problems. | Moral injury scores remained stable for three months, while distress decreased. A favourable work environment is associated with lower moral impairment, whereas a stressful and less favourable environment is associated with increased moral impairment. Distress was not influenced by any occupational or resilience factors at baseline, except for poor sleep. | RESILIENCE |
| Serrão et al. [40] | Cross-sectional/2008 healthcare workers/Portugal | Analysis of the mediating role of resilience in the relationship between depression and burnout (personal, work-related and patient-related). | Psychological resilience partly mediated the relationship between depression and all three dimensions of burnout. | RESILIENCE |
| Zadok-Gurman et al. [41] | Prospective controlled trial with an intervention group (N = 35) and a comparison control group (N = 32)/67 teachers/Israel | Evaluation of the effect of IBSR on resilience, burnout, mindfulness and stress among teachers during the COVID-19 pandemic. | Mixed IBSR intervention improved teacher resilience and psychological and subjective well-being. At the same time, the control group experienced higher levels of burnout and a reduction in well-being. | RESILIENCE |
| Lorente et al. [42] | Cross-sectional/421 nurses/Spain | Evaluation of the impact of stressors (work overload, insufficient preparation to cope with job demands, lack of support, death and fear of infection) during the peak of the COVID-19 pandemic on the psychological distress of nurses. In addition, the mediating role of problem-focused and emotion-focused coping strategies and resilience is analysed. | All stressors have a significant, direct and negative relationship with nurses’ psychological distress; emotion-focused strategies are negatively related to nurses’ psychological distress directly and indirectly through resilience; problem-focused strategies are positively related to nurses’ psychological distress and negatively and indirectly through emotion-focused strategies. | RESILIENCE AND COPING STRATEGIES |
| Munawar and Choudhry [43] | Qualitative study/15 frontline emergency HWCs/Pakistan | Coping strategies and COVID-19 psychological impact. | The most frequently used coping strategies were religious coping and a passion to serve humanity and the country. | COPING STRATEGIES |
| Hong et al. [44] | Cross-sectional/824 nurses/South Korea | The effect of resilience on mental health, work-related stress and anxiety in relation to the COVID-19 pandemic. | A high level of general anxiety, work-related stress during viral epidemics and a low level of resilience were predictors of depression in healthcare workers. | RESILIENCE |
| Afshari et al. [45] | Cross-sectional/387 nurses/Iran | Resilience score and demographic predictive factors among nurses working in hospitals involved in addressing COVID-19. | The results of this study showed that age, work experience and education level had a significant positive correlation with nurses’ resilience score. The nurses’ resilience score was low. Multiple regression analysis indicated that work experience and level of education were predictors of resilience. | RESILIENCE |
| Mosheva et al. [46] | Cross-sectional/1106 doctors/Israel | Association between pandemic-related stressors (PRSF) and anxiety and assessment of the potential effect of resilience on anxiety. | The results show a negative association between resilience and anxiety. Four salient PRSFs (mental exhaustion, anxiety about being infected, anxiety about infecting family members and sleep difficulties) were positively associated with anxiety scores. | RESILIENCE |
| Shechter et al. [47] | Cross-sectional/657 healthcare professionals/USA | Distress, coping and preferences for support | 61% of participants reported a greater sense of meaning/purpose from the COVID-19 outbreak. Physical activity/exercise was the most common coping strategy (59%) and access to an individual therapist with self-guided online counselling (33%) was of greatest interest. | COPING STRATEGIES |
| Huang et al. [48] | Comparative study/802 in total: 374 nurses and 430 nursing students/China | Comparison of emotional responses and coping strategies between nurses and students. | For the group of professional nurses, anxiety, fear, sadness and anger were significantly higher than for college students. More nurses used problem-focused coping strategies than students did. | COPING STRATEGIES |
| Vagni et al. [49] | Cross-sectional/210 in total: 121 healthcare workers and 89 emergency workers/Italy | Investigation of the relationship between coping strategies used by healthcare professionals and emergency workers to manage emergency-related stressors COVID-19. | The results suggested that the healthcare worker group had higher levels of stress and arousal and used more problem-focused coping strategies than the emergency worker group. | COPING STRATEGIES |
| Tahara et al. [50] | Cross-sectional/661 healthcare workers/Japan | Analysis of risk and coping factors associated with the mental state of healthcare workers. | The results suggest that female gender, low levels of communication with friends and high anxiety were associated with poorer mental health. Conversely, good health, high job satisfaction and high satisfaction with new activities were associated with a reduction in mental health problems. Most participants chose an avoidance strategy, and participants with poorer mental health were more likely to adopt social support seeking as their coping strategy. | COPING STRATEGIES |
| Prazeres et al. [51] | Cross-sectional/222 healthcare workers/Portugal | The role of religious-spiritual coping in relation to COVID-19 fear and anxiety in health care workers. | Participants with higher levels on the hope/optimism dimension of the spirituality scale showed less anxiety related to COVID-19. | COPING STRATEGIES |
| Bozdag and Ergu [52] | Cross-sectional/214 healthcare workers/Turkey | Assessment of the psychological resilience of healthcare workers taking into account individual and environmental variables. | Psychological resilience was significantly and positively correlated with life satisfaction, positive affect, perceived social support subscales, age, adoption of personal COVID-19 precautions, diet and quality of sleep while was negatively correlated with negative affect, feeling personally at risk as a healthcare professional and worried about being infected. | RESILIENCE |
| Lyu et al. [53] | longitudinal study 1—cross-sectional study 2/134 frontline healthcare workers in the first phase and 401 frontline healthcare workers in the second phase/China | The study explores the longitudinal relationship between resilience, PTG and the role of burnout. | Cross-lagged analysis showed that resilience at Time 1 positively predicted PTG at Time 2, which in turn positively predicted resilience at Time 3. PTG at Time 1 also positively predicted resilience at Time 2 (Study 1). Job burnout was negatively related to both resilience and PTG; in particular, emotional exhaustion moderated the link between PTG and resilience (Study 2). | PTG AND RESILIENCE |
| Huffman et al. [54] | Cross-sectional/785 healthcare providers, medical trainees and administrators/USA | The impact of the COVID-19 pandemic on the psychological well-being of healthcare workers, medical trainees and administrators and identify sources of stress. | Greater resilience was associated with less stress, anxiety, fatigue and sleep problems. Additionally, increased resilience and grit were protective factors in managing personal and systemic stressors at the height of the COVID-19 pandemic. | RESILIENCE |
| Oluwaseyi Ojo et al. [55] | Cross-sectional/259 employees/Malaysia | Based on the conservation of resources theory, the study investigates the work, social and personal resources underlying employee resilience and the impact of resilience in stimulating work engagement during the COVID-19 pandemic. | The results of the path modelling analysis showed a significant impact of self-efficacy, facilitating conditions and support from family and friends on employee resilience. Furthermore, resilience was significantly associated with engagement. | RESILIENCE |
| MacIntyre et al. [56] | Cross-sectional/600 language teachers/Several countries from Europe, North America, South America, Asia, Middle East | The survey measured stressors and 14 coping strategies grouped into two types, ‘approach’ and ‘avoidant’. | Correlations suggested that positive psychological outcomes (well-being, health, happiness, resilience and growth during trauma) were positively correlated with coping and negatively correlated with avoidance. Avoidant coping increased as stress increased, demonstrating a possible cost of using avoidant coping strategies. | COPING STRATEGIES |
| Vagni et al. [57] | Cross-sectional/236 in total: 140 healthcare workers and 96 emergency workers/Italy | The aim was to assess which stressors caused secondary trauma and to assess the protective role of the hardiness construct. | Healthcare workers had higher levels of stress and arousal than the emergency worker group, and those involved in COVID-19 treatment were exposed to a high degree of stress and were at high risk of developing secondary trauma. Commitment was associated with high levels of stress, arousal and intrusion, while control showed a protective function. Stress and hardiness accounted for 37% and 17% of the variance in arousal and intrusion, respectively. | COPING STRATEGIES |
| Li et al. [58] | Comparative study/455 nurses and 424 general population/China | Evaluation of PTG of Chinese nurses and the general population during the COVID-19 pandemic. | The results highlighted some differences in the PTGI score between nurses and the GP, both in the total score and in the 3 dimensions of new possibilities, personal strength and spiritual change. There were also differences between first-line nurses (FLN) and non-first-line nurses (nFLN). Psychological counselling from the WeChat network and self-relaxation were valid coping strategies for relieving nurses’ stress. | PTG |
| Tuan [59] | Cross-sectional/672 employees in the tourism sector/Vietnam | Study of the role of core beliefs challenge in promoting workers’ resilience. | The results revealed a positive association between workers’ core beliefs challenge and their resilience. Cognitive reappraisal was found to be a mediator in the relationship between core beliefs challenge and resilience, whereas no evidence was found regarding the mediating role of expressive suppression. Family strain negatively moderated the relationship between core beliefs challenge and both emotion regulation strategies. | RESILIENCE |
| Fino et al. [60]. | Cross-sectional/202 healthcare workers/Italy | Analysis of the relationship between post-traumatic stress and PTG, the moderating role of resilience, emotion regulation and social support. Hypothesis: A high level of distress would be associated with PTG in health workers with high resilience, high emotion regulation skills and high social support. | The moderating role of resilience was significant, as indicated by the model and the PTSD-by-resilience interaction. Greater positive reappraisal of events was associated with high levels of post-traumatic growth at normal and above normal levels, but not with low levels of PTSD. | PTG AND RESILIENCE |
| Li et al. [61] | Predictive study/356 front-line nurses/China | Assessment of psychological well-being and factors associated with PTSD before and after nurses worked in COVID-19 wards. | The level of stress and the prevalence of PTSD increased significantly after working in COVID-19 units. Work experience of less than 2 years was significantly associated with a high risk of developing PTSD. Nurses working in COVID-19 wards were significantly more likely to suffer from PTSD than those working in other COVID-19-related units. Resilience was negatively associated with PTSD. | RESILIENCE |
| Zhang et al. [62] | Cross-sectional/180 front-line nurses/China | Analysis of the mediating roles of positive and negative affect in the relationship between resilience and burnout in Wuhan hospital nurses at the peak of the COVID-19 pandemic. | Resilience showed significant negative correlations with burnout and emotional exhaustion, depersonalization, reduced personal accomplishment. Resilience correlates positively with positive affect. The excellent preparation to resilience of frontline nurses and the associated positive effect can reduce the risk of burnout. | RESILIENCE |
| Debanjan et al. [63] | Cross-sectional/172 Physicians working at COVID-19 Hospitals/India | Understanding adversity and defining the resilience framework of doctors in COVID-19 hospitals, through a qualitative approach. | The resilience “framework” of these workers is a process that has emerged as doctors have faced fears of infection, uncertainty, stigma, guilt and social isolation. Unmet needs were flexible work policies, administrative measures for better medical protection, media sensitivity to the image of HCWs, effective risk communication for their health and social inclusion. Resilience consisted of three facets: forming a “resilient identity”, managing resilience and working through socio-occupational distress. | RESILIENCE AND COPING STRATEGIES |
| Coulombe et al. [64] | Cross-sectional/1122 workers from different sectors/Canada | The study aims to explore associations of potential resilience factors at multiple ecological levels (i.e., trait resilience, family functioning, social support from friends, social participation and trust in health care institutions) with mental health and well-being outcomes and their role as moderators against the negative effects of the pandemic. | Meaning of life was positively associated with trait resilience, better family functioning, greater social support from friends, social participation and trust in healthcare institutions. Lower stress was associated with better family functioning, trust in healthcare institutions and greater trait resilience. | RESILIENCE |
| Croghan et al. [65] | Cross-sectional/302 healthcare workers/USA | The purpose of the study was to assess the level of stress, resilience and ability to cope among HCWs during the initial stages of the pandemic and to determine inter-professional differences. | HCWs reported moderate-high stress scores, and normal levels of resilience and coping, the MD/NP/PA group had the highest resilience, while nurses had the lowest. Nurses also had higher stress levels compared to the MD/PA/NP group; older age was associated with higher resilience. | RESILIENCE |
| Di Giuseppe et al. [66] | Cross-sectional/233 healthcare workers/Italy | This study aimed to identify protective factors against perceived stress and burnout and factors that can improve resilience among health workers. | Mature defences were positively associated with resilience and personal accomplishment, while they have negative influences on stress and burnout. Neurotic and immature defences followed the opposite trend. Lower age, female gender, higher exposure to COVID-19, lower resilience and less adaptive defensive functioning were the best predictors of perceived stress and emotional exhaustion among healthcare professionals. | COPING STRATEGIES |
| Di Trani et al. [67] | Cross-sectional/267 healthcare workers/Italy | The general aim of this study was to explore the burnout dimensions among Italian HCWs during the COVID-19 emergency and to evaluate their relationships with some psychological features (resilience and intolerance to uncertainty). | HCWs at high risk of burnout showed significantly lower levels of resilience and higher levels of uncertainty intolerance. Levels of resilience and the ability to tolerate uncertainty were significant factors in determining the impact of the COVID-19 emergency on HCWs. The use of emotional strategies that allow individuals to remain in a critical situation without the need to control it seems to protect against burnout in these circumstances. | RESILIENCE |
| Fleuren et al. [68] | Cross-sectional/1126 healthcare workers/The Netherlands | The study aims to investigate the relationships between resilience, team social climate and depressive complaints, specifically focusing on infection-related fears as a relevant explanatory mechanism. | This model shows that personal resilience is negatively associated with depressive complaints and concerns about infections, which in turn are positively related to depressive symptoms. Team social climate is associated with a lower effect of worries about being infected and infecting others on depressive complaints. Resilience can be an important individual resource in preventing depressive complaints. | RESILIENCE |
| Hou et al. [69] | Cross-sectional/1472 healthcare workers/China | The study examined the effect of social support on the mental health of healthcare workers and its underlying mechanisms regarding the mediating role of resilience and the moderating role of age during the epidemic. | The results highlighted the protective role of social support in mental health among healthcare professionals. Resilience could be one of the pathways through which social support contributes to mental health. The effect of social support on mental health through resilience is attenuated in middle-aged healthcare workers compared to younger ones. | RESILIENCE |
| Sinu et al. [70] | Cross-sectional/120 frontline healthcare workers/India | This study aims to determine burnout and resilience levels and associated factors among frontline nurses caring for COVID-19 patients. | Resilience showed a significant negative relationship with emotional exhaustion and reduced professional efficacy. Emotional exhaustion and reduced personal accomplishments are significantly negatively correlated with total resilience, but there is no significant relationship between depersonalization and resilience. Increasing resilience among nurses will help mitigate the symptoms of burnout. | RESILIENCE |
| Lin et al. [71] | Cross-sectional/114 healthcare workers/China | Investigation of the resilience of non-local healthcare workers sent to support local healthcare workers in treating the COVID-19 outbreak. | Resilience correlated negatively with anxiety and depression but positively with active coping styles. Active coping, depression, anxiety and training/support provided by the respondent’s permanent hospital were significantly associated with resilience. | RESILIENCE AND COPING STRATEGIES |
| Maiorano et al. [72] | Cross-sectional/140 healthcare workers and 100 emergency workers/Italy | The study aims to investigate the direct and mediated effects of coping strategies and hardiness on secondary trauma among Italian medical staff and emergency workers involved in the first phase of the COVID-19 pandemic. | Physicians, nurses and rescuers were exposed to similar levels of organizational, cognitive, social and emotional stress. The use of cognitive and emotional avoidance strategies, especially in an initial emergency phase seems to allow these workers to limit their sense of helplessness and inability, favoring resilience and the activation of proactive attitudes. Stopping negative emotions seems to reduce stress levels and arousal and intrusive aspects of the trauma. Older workers showed a greater tendency to adopt avoidance strategies toward negative thoughts and emotions, but exhibited higher levels of arousal. Age seems to allow health and emergency workers to stop the intrusive aspects of the trauma, thus making them more committed to the intervention and less influenced by the consequences. | COPING STRATEGIES |
| McFadden et al. [73] | Cross-sectional/3425 healthcare workers and social workers/United Kingdom (UK) | This study examines the relationship between coping strategies and wellbeing and quality of working life in nurses, midwives, allied health professionals, social care workers and social workers who worked in health and social care in the UK during its first wave of COVID-19. | Positive coping strategies, such as active coping and seeking help, have been associated with higher well-being and a better quality of working life. Negative coping strategies showed an opposite trend. The most frequently used coping strategy was acceptance. Avoidance coping was associated with lower well-being. Among the more adaptive coping strategies, active coping and seeking help were found to help be protective factors. Active coping, help seeking, religion, humour, work-family segmentation, working to improve skills, recreation and relaxation and exercise were all coping strategies employed by workers (personal job resources) that protected them from low wellbeing. | COPING STRATEGIES |
| Roca et al. [74] | Qualitative study/22 nursing students/Spain | The study aimed to qualitatively explore the experiences and emotional responses of senior nursing students who volunteered to provide health assistance at the peak of the COVID-19 pandemic and to identify coping measures taken to deal with the situation. | The coping strategies used in the work context were teamwork, psychological assistance by the healthcare institution, seeking information on COVID-19 care and peer support, primarily through social networks. Other personal strategies included receiving support from family and friends, recreational activities, self-reliance, humour and religion. | COPING STRATEGIES |
| Zhou et al. [75] | Longitudinal study/107 healthcare workers/China | The study aims to examine the effects of perceived organizational support, self-efficacy and two types of coping strategies on the PTSD symptoms of frontline healthcare workers fighting against COVID-19 in Wuhan. | Perceived organizational support reduced PTSD symptoms through the mediating effect of problem-focused coping and the sequential mediating effect of self-efficacy and problem-focused coping strategies. Emotion-focused coping is less likely to be used and is not effective for reducing PTSD symptoms. Self-efficacy predicted reduction of PTSD symptoms by the mediating effect of problem-focused coping. | COPING STRATEGIES |
| Topic | Overall Findings | Implications |
|---|---|---|
| Resilience |
|
|
| Coping Strategies |
|
|
| Posttraumatic growth |
|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Finstad, G.L.; Giorgi, G.; Lulli, L.G.; Pandolfi, C.; Foti, G.; León-Perez, J.M.; Cantero-Sánchez, F.J.; Mucci, N. Resilience, Coping Strategies and Posttraumatic Growth in the Workplace Following COVID-19: A Narrative Review on the Positive Aspects of Trauma. Int. J. Environ. Res. Public Health 2021, 18, 9453. https://doi.org/10.3390/ijerph18189453
Finstad GL, Giorgi G, Lulli LG, Pandolfi C, Foti G, León-Perez JM, Cantero-Sánchez FJ, Mucci N. Resilience, Coping Strategies and Posttraumatic Growth in the Workplace Following COVID-19: A Narrative Review on the Positive Aspects of Trauma. International Journal of Environmental Research and Public Health. 2021; 18(18):9453. https://doi.org/10.3390/ijerph18189453
Chicago/Turabian StyleFinstad, Georgia Libera, Gabriele Giorgi, Lucrezia Ginevra Lulli, Caterina Pandolfi, Giulia Foti, José M. León-Perez, Francisco J. Cantero-Sánchez, and Nicola Mucci. 2021. "Resilience, Coping Strategies and Posttraumatic Growth in the Workplace Following COVID-19: A Narrative Review on the Positive Aspects of Trauma" International Journal of Environmental Research and Public Health 18, no. 18: 9453. https://doi.org/10.3390/ijerph18189453
APA StyleFinstad, G. L., Giorgi, G., Lulli, L. G., Pandolfi, C., Foti, G., León-Perez, J. M., Cantero-Sánchez, F. J., & Mucci, N. (2021). Resilience, Coping Strategies and Posttraumatic Growth in the Workplace Following COVID-19: A Narrative Review on the Positive Aspects of Trauma. International Journal of Environmental Research and Public Health, 18(18), 9453. https://doi.org/10.3390/ijerph18189453









