Spatial Accessibility of Primary Health Care in Rural Areas in Poland
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Area
2.2. PHC Facilities
2.3. Localities
2.4. Population
2.5. Road Network
2.6. Research Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dej, M. Transport publiczny w wiejskich obszarach peryferyjnych polski i jego dostosowanie do potrzeb lokalnych rynków pracy. Pr. Geogr. 2010, 124, 111–130. [Google Scholar]
- Komorowski, Ł.; Stanny, M. Public Transport in Rural Areas—Studies Conclusions. Ann. Pol. Assoc. Agric. Agribus. Econ. 2017, XIX, 129–136. [Google Scholar] [CrossRef][Green Version]
- Aday, L.A.; Andersen, R. A framework for the study of access to medical care. Health Serv. Res. 1974, 9, 208–220. [Google Scholar] [PubMed]
- Ucieklak-Jeż, P.; Bem, A. Dostępność opieki zdrowotnej na obszarach wiejskich w Polsce. Probl. Drob. Gospod. Rol. Probl. Small Agric. Hold. 2017, 4, 117–131. [Google Scholar]
- Kanownik, G. Patient Safety and Accessibility to Health Services. Zesz. Nauk. Uniw. Szczecińskiego Finans. Rynk. Finans. Ubezpieczenia 2017, 1, 609–620. [Google Scholar] [CrossRef][Green Version]
- Guagliardo, M.F. Spatial accessibility of primary care: Concepts, methods and challenges. Int. J. Health Geogr. 2004, 3, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Daly, M.R.; Mellor, J.M.; Millones, M. Do Avoidable Hospitalization Rates among Older Adults Differ by Geographic Access to Primary Care Physicians? Health Serv. Res. 2018, 53, 3245–3264. [Google Scholar] [CrossRef]
- Chen, T.; Pan, J. The effect of spatial access to primary care on potentially avoidable hospitalizations of the elderly: Evidence from Chishui City, China. Soc. Indic. Res. 2020, 1–21. [Google Scholar] [CrossRef]
- Eurostat. Old-Age Dependency Ratio Increasing in the EU. Available online: https://ec.europa.eu/eurostat/en/web/products-eurostat-news/-/DDN-20200713-1 (accessed on 10 August 2021).
- Journal of Laws. Act of 8 March 1990 on Municipal Authorities, Dz.U. 2021 poz. 1372; Law Office of the Polish Parliament: Warsaw, Poland, 2021.
- Regulation of the Ministry of Health. Regulation of the Minister of Health of 10 October 2001 on the Principles and Conditions to Be Fulfilled by the Minimum Security Plan for Outpatient Health Care; Dz.U. 2001 nr 121 poz. 1315; Ministry of Health: Warsaw, Poland, 2001. [Google Scholar]
- Journal of Laws. Act of 27 October 2017 on Primary Healthcare, Dz.U. 2021 poz. 1050; Law Office of the Polish Parliament: Warsaw, Poland, 2021.
- Windak, A.; Niżankowski, R.; Lukas, W.; Tomasik, T.; Panasiuk, L.; Florek-Łuszczki, M.; Paprzycki, P.; Jankowska-Zduńczyk, A.; Jakubiak, A.; Łuczak, J.; et al. Raport "Podstawowa Opieka Zdrowotna w Polsce—Diagnoza i Projekty Zmian"; Instytut Medycyny Wsi im. Witolda Chodźki w Lublinie: Lublin, Poland, 2019. [Google Scholar]
- Living in the EU. Available online: https://europa.eu/european-union/about-eu/figures/living_en?fbclid=IwAR0k5o5HJ7_0bHnj8PhEN3q8D1S34tf904VDXcCO8S2lLG-erVzPx_Jwuds (accessed on 20 August 2021).
- Regional Demography: Demographic Indicators by Rural/Urban Typology, Country Level. Available online: https://stats.oecd.org/index.aspx?queryid=67050&fbclid=IwAR3i8npZCZcBoIOJ3obpR0fIAq4wQuAkOjQqOs9mTAXtikkx-xe8Pa4jy-M# (accessed on 20 August 2021).
- Kacperczyk, E.; Ciesielska, K.; Korzeniewski, K.; Macioch, B. Area and Population in the Territorial Profile in 2021; GUS: Warsaw, Poland, 2021. [Google Scholar]
- GeoPy’s Documentation. Available online: https://geopy.readthedocs.io/en/stable/#on (accessed on 20 August 2021).
- Page, N.; Langford, M.; Higgs, G. An evaluation of alternative measures of accessibility for investigating potential ‘deprivation amplification’ in service provision. Appl. Geogr. 2018, 95, 19–33. [Google Scholar] [CrossRef]
- Luo, W.; Wang, F. Measures of spatial accessibility to health care in a GIS environment: Synthesis and a case study in the Chicago region. Environ. Plan. B Plan. Des. 2003, 30, 865–884. [Google Scholar] [CrossRef]
- Morrill, R.L.; Kelley, M.B. The Simulation of Hospital Use and the Estimation of Location Efficiency. Geogr. Anal. 1970, 2, 283–300. [Google Scholar] [CrossRef]
- Fyer, G.E.; Drisko, J.; Krugman, R.D.; Vojir, C.P.; Prochazka, A.; Miyoshi, T.J.; Miller, M.E. Multi-method Assessment of Access to Primary Medical Care in Rural Colorado. J. Rural Health 1999, 15, 113–121. [Google Scholar] [CrossRef]
- Fortney, J.; Rost, K.; Warren, J. Comparing alternative methods of measuring geographic access to health services. Health Serv. Outcomes Res. Methodol. 2000, 1, 173–184. [Google Scholar] [CrossRef]
- Higgs, G. A literature review of the use of GIS-based measures of access to health care services. Health Serv. Outcomes Res. Methodol. 2004, 5, 119–139. [Google Scholar] [CrossRef]
- Merwin, E.; Snyder, A.; Katz, E. Differential Access to Quality Rural Healthcare. Fam. Community Health 2006, 29, 186–194. [Google Scholar] [CrossRef]
- Bell, S.; Wilson, K.; Bissonnette, L.; Shah, T. Access to Primary Health Care: Does Neighborhood of Residence Matter? Ann. Assoc. Am. Geogr. 2013, 103, 85–105. [Google Scholar] [CrossRef]
- Stępniak, M. Wykorzystanie metody 2SFCA w badaniach dostępności przestrzennej usług medycznych. Przegląd Geogr. 2013, 85, 199–218. [Google Scholar] [CrossRef]
- McLafferty, S.L. GIS and Health Care. Annu. Rev. Public Health 2003, 24, 25–42. [Google Scholar] [CrossRef]
- McGrail, M.R.; Humphreys, J.S. Measuring spatial accessibility to primary care in rural areas: Improving the effectiveness of the two-step floating catchment area method. Appl. Geogr. 2009, 29, 533–541. [Google Scholar] [CrossRef]
- Wyszewiański, L. Access to care: Remembering old lessons. Health Serv. Res. 2002, 37, 1441–1443. [Google Scholar] [CrossRef]
- Dacey, M.F. Analysis of Central Place and Point Patterns by a Nearest Neighbor Method. L. Stud. Geogr. Ser. B 1962, 24, 55–75. [Google Scholar]
- Apparicio, P.; Gelb, J.; Dubé, A.; Kingham, S.; Gauvin, L.; Robitaille, É. The approaches to measuring the potential spatial access to urban health services revisited: Distance types and aggregation-error issues. Int. J. Health Geogr. 2017, 16, 1–24. [Google Scholar] [CrossRef] [PubMed]
- Neutens, T. Accessibility, equity and health care: Review and research directions for transport geographers. J. Transp. Geogr. 2015, 43, 14–27. [Google Scholar] [CrossRef]
- Freiria, S.; Tavares, A.O.; Julião, R.P. The benefits of a link-based assessment of health services accessibility: Unveiling gaps in Central Region of Portugal. Land Use Policy 2019, 87. [Google Scholar] [CrossRef]
- Hawthorne, T.L.; Kwan, M.P. Using GIS and perceived distance to understand the unequal geographies of healthcare in lower-income urban neighbourhoods. Geogr. J. 2012, 178, 18–30. [Google Scholar] [CrossRef] [PubMed]
- Haynes, R.; Lovett, A.; Sünnenberg, G. Potential accessibility, travel time, and consumer choice: Geographical variations in general medical practice registrations in Eastern England. Environ. Plan. A 2003, 35, 1733–1750. [Google Scholar] [CrossRef]
- Drury, P. Some spatial aspects of health service developments. Prog. Hum. Geogr. 1983, 7, 60–77. [Google Scholar] [CrossRef]
- Yin, C.; He, Q.; Liu, Y.; Chen, W.; Gao, Y. Inequality of public health and its role in spatial accessibility to medical facilities in China. Appl. Geogr. 2018, 92, 50–62. [Google Scholar] [CrossRef]
- Martin, D.; Wrigley, H.; Barnett, S.; Roderick, P. Increasing the sophistication of access measurement in a rural healthcare study. Health Place 2002, 8, 3–13. [Google Scholar] [CrossRef]
- Luo, W.; Qi, Y. An enhanced two-step floating catchment area (E2SFCA) method for measuring spatial accessibility to primary care physicians. Health Place 2009, 15, 1100–1107. [Google Scholar] [CrossRef] [PubMed]
- Borowska-Stefańska, M.; Wiśniewski, S.; Mădălina-Teodora, A. The functioning of hospital emergency rooms in the Łódź region in the light of spatial analysis. Mod. Manag. Rev. 2017, XXII, 17–32. [Google Scholar] [CrossRef][Green Version]
- Suchecki, B.; Antczak, E. Ekonometria Przestrzenna II: Modele Zaawansowane; Metody Ilościowe; C. H. Beck: Warszawa, Poland, 2012; ISBN 9788325540159/9788325540166. [Google Scholar]
- Bellu, L.G.; Liberati, P. Describing Income Inequality Theil Index and Entropy Class Indexes. Food Agric. Organ. U. N. FAO 2006, 51, 1–20. [Google Scholar]
- Bellu, L.G.; Liberati, P. Policy Impacts on Inequality: Decomposition of Income Inequality by Income Source. Food Agric. Organ. U. N. FAO 2006, 53, 1–23. [Google Scholar]
- Longley, P.A.; Goodchild, M.F.; Maguire, D.J.; Rhind, D.W. Geographic Information Science & Systems, 4th ed.; Wiley: Hoboken, NJ, USA, 2015. [Google Scholar]
- Scott, L.M.; Janikas, M. V Spatial Statistics in ArcGIS. In Handbook of Applied Spatial Analysis; Fischer, M.M., Getis, A., Eds.; Springer: Berlin/Heidelberg, Germany, 2009. [Google Scholar]
- Anselin, L. Local Indicators of Spatial Association—LISA. Geogr. Anal. 1995, 27, 93–115. [Google Scholar] [CrossRef]
- Jażdżewska, I. Zmiany gęstości ludności miejskiej w centralnej Polsce. Estymacja rozkładu gęstości zaludnienia z wykorzystaniem nieparametrycznych estymatorów jądrowych (kernel function). Człowiek Sr. 2011, 35, 5–17. [Google Scholar]
- Silverman, B.W. Density Estimation for Statistics and Data Analysis; Chapman and Hall: New York, NY, USA, 1986. [Google Scholar]
- Kłudacz, M.; Walczak, R.; Szustak, A. Analiza dostępności usług ratownictwa medycznego na terenie Województwa Mazowieckiego. Logistyka 2014, 6, 5504–5513. [Google Scholar]
- Krawczyk-Sołtys, A. Dostępność do ambulatoryjnej opieki zdrowotnej na wsi w Polsce. Ujęcie przestrzenno-czasowe. J. Agribus. Rural Dev. 2014, 2, 79–86. [Google Scholar] [CrossRef]
- Stępniak, M.; Wiśniewski, R.; Goliszek, S.; Marcińczak, S. Dostępność Przestrzenna Do Usług Publicznych w Polsce; Instytut Geografii i Przestrzennego Zagospodarowania PAN: Warszawa, Poland, 2017; ISBN 978-83-61590-82-8. [Google Scholar]
- Wisniewski, S. Spatial Accessibility of Hospital Healthcare in Łódź Voivodeship. Quaest. Geogr. 2016, 35, 157–166. [Google Scholar] [CrossRef]
- Jarczewska, D.Ł.; Jarczewski, W. Dostępność geograficzna i rozmieszczenie w przestrzeni ośrodków POZ w Krakowie. Probl. Rozw. Miast 2014, 1, 79–89. [Google Scholar]
- Martin, D.; Roderick, P.; Diamond, I.; Clements, S.; Stone, N. Geographical aspects of the uptake of renal replacement therapy in England. Int. J. Popul. Geogr. 1998, 4, 227–242. [Google Scholar] [CrossRef]
- Śleszyński, P. Oszacowanie rzeczywistej liczby ludności gmin województwa mazowieckiego z wykorzystaniem danych GUS. Studia Demogr. 2011, 160, 35–57. [Google Scholar]



| Road Class in OSM | Length in OSM for Poland after Calculation (km) |
|---|---|
| Motorway | 3889.83 |
| Trunk | 5713.37 |
| Primary | 17,970.81 |
| Secondary | 31,777.92 |
| Tertiary | 90,012.95 |
| Unclassified | 72,519.37 |
| Residential | 147,197.94 |
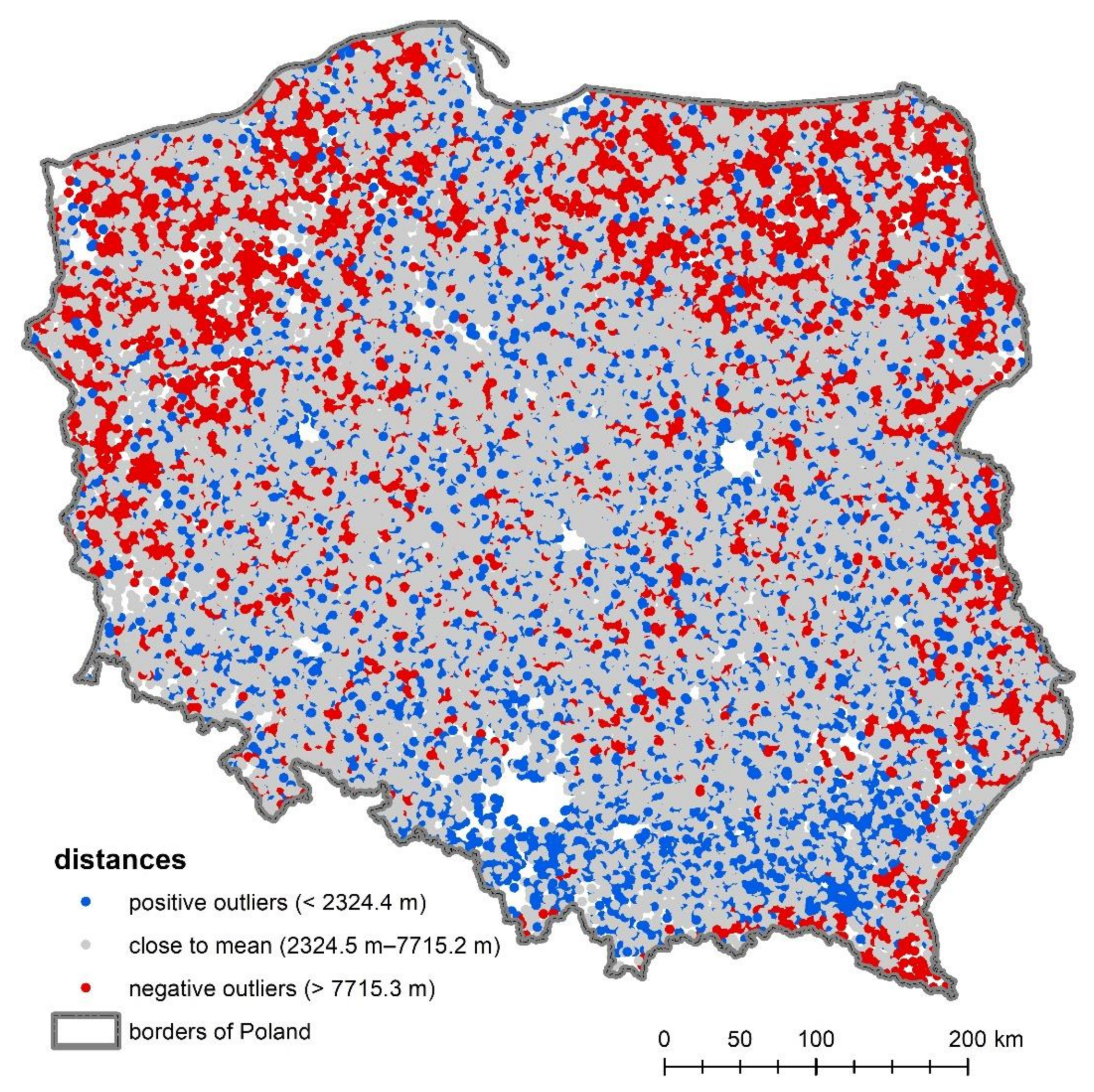
| Mean Distance (m) | Standard Deviation σ | (−1σ; +1σ) | Maximum Value (m) | % Close to Mean | % Positive Outliers (Smaller Distances) | % Negative Outliers (Longer Distances) |
|---|---|---|---|---|---|---|
| 5019.8 | 2695.4 | (2324.5; 7715.2) | 32,552.2 | 71.6 | 13.8 | 14.6 |
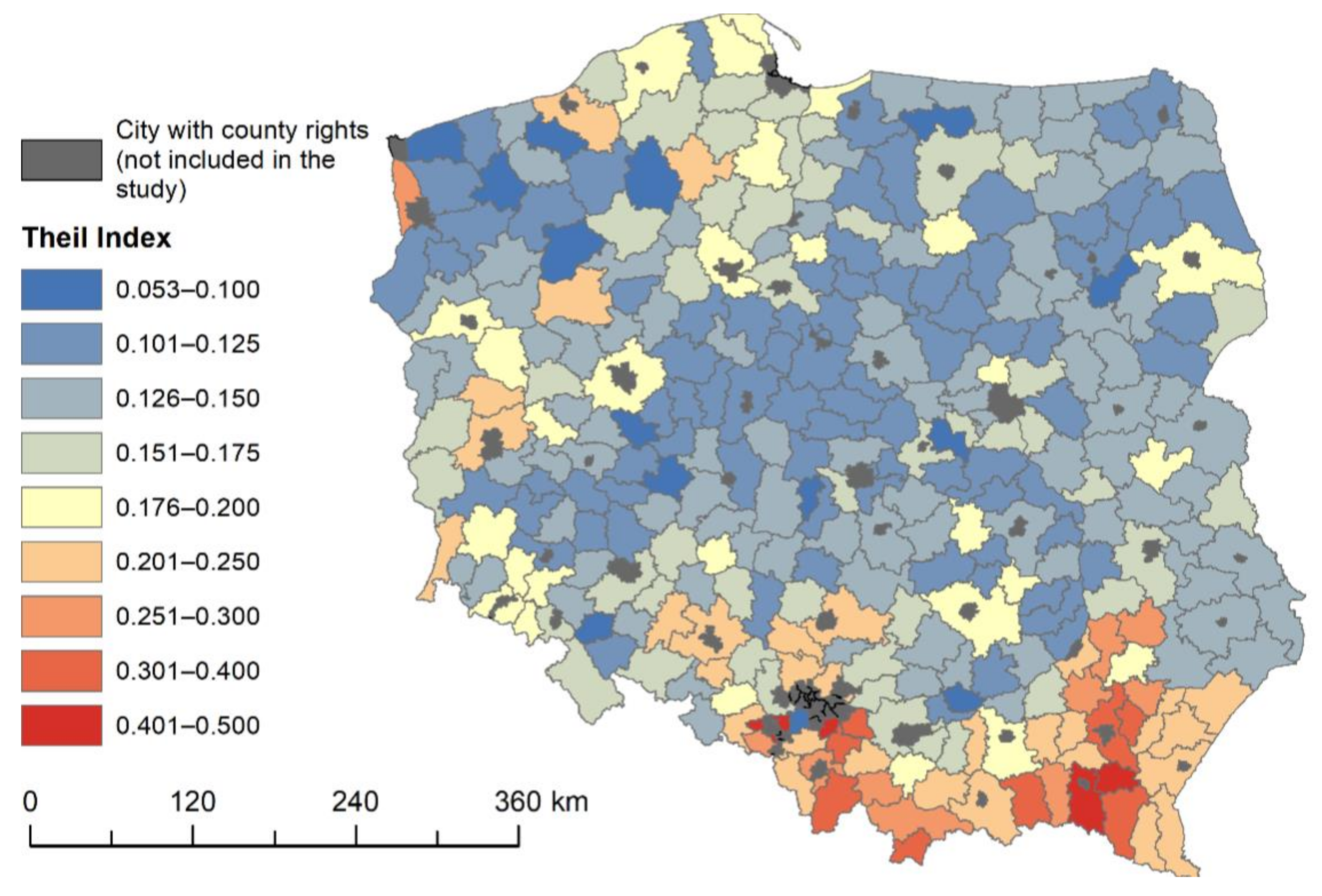
| Ti | Text | Tint |
|---|---|---|
| 0.1668 | 0.0263 | 0.1405 |
| Moran’s Index | z-Score | p-Value | % HH | % HL | % LH | % LL |
|---|---|---|---|---|---|---|
| 0.33 | 209.18 | 0 | 16.48 | 3.86 | 1.60 | 23.96 |
| Voivodeship Name | PHC Percentage Area |
|---|---|
| Lower Silesia | 3.27 |
| Kuyavian-Pomeranian | 3.34 |
| Lublin | 6.19 |
| Lubusz | 2.55 |
| Lodz | 3.08 |
| Lesser Poland | 2.00 |
| Masovian | 7.91 |
| Opole | 1.83 |
| Subcarpathian | 2.50 |
| Podlaskie | 1.67 |
| Pomeranian | 6.00 |
| Silesian | 0.45 |
| Swietokrzyskie | 2.21 |
| Warmian-Masurian | 4.31 |
| Greater Poland | 10.66 |
| Western Pomeranian | 5.75 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lechowski, Ł.; Jasion, A. Spatial Accessibility of Primary Health Care in Rural Areas in Poland. Int. J. Environ. Res. Public Health 2021, 18, 9282. https://doi.org/10.3390/ijerph18179282
Lechowski Ł, Jasion A. Spatial Accessibility of Primary Health Care in Rural Areas in Poland. International Journal of Environmental Research and Public Health. 2021; 18(17):9282. https://doi.org/10.3390/ijerph18179282
Chicago/Turabian StyleLechowski, Łukasz, and Angelika Jasion. 2021. "Spatial Accessibility of Primary Health Care in Rural Areas in Poland" International Journal of Environmental Research and Public Health 18, no. 17: 9282. https://doi.org/10.3390/ijerph18179282
APA StyleLechowski, Ł., & Jasion, A. (2021). Spatial Accessibility of Primary Health Care in Rural Areas in Poland. International Journal of Environmental Research and Public Health, 18(17), 9282. https://doi.org/10.3390/ijerph18179282






