Assessment of Lead and Mercury Exposure Levels in the General Population of Korea Using Integrated National Biomonitoring Data
Abstract
1. Introduction
2. Materials and Methods
2.1. Data
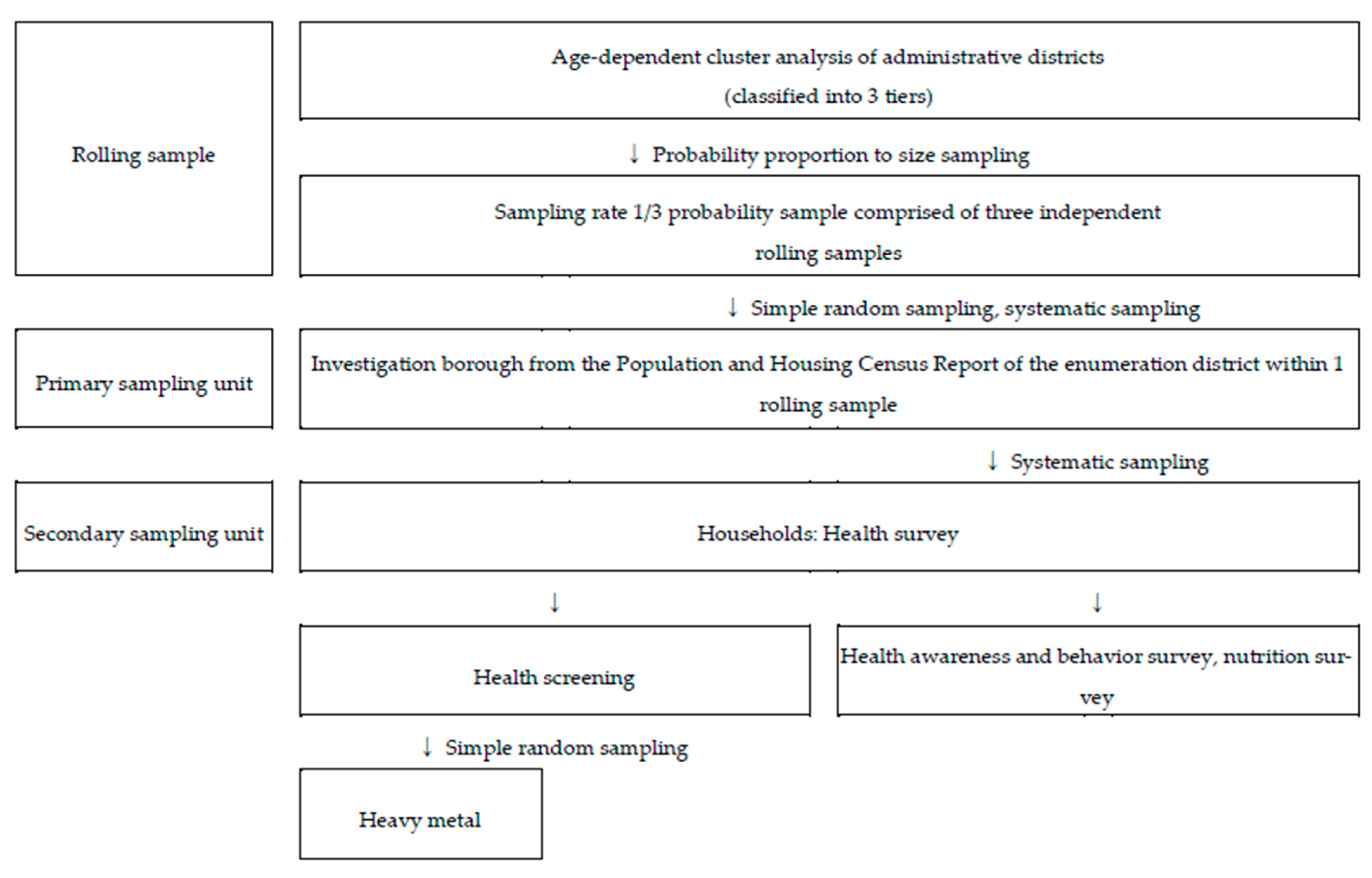
2.1.1. KNEHS
2.1.2. KNHAENS
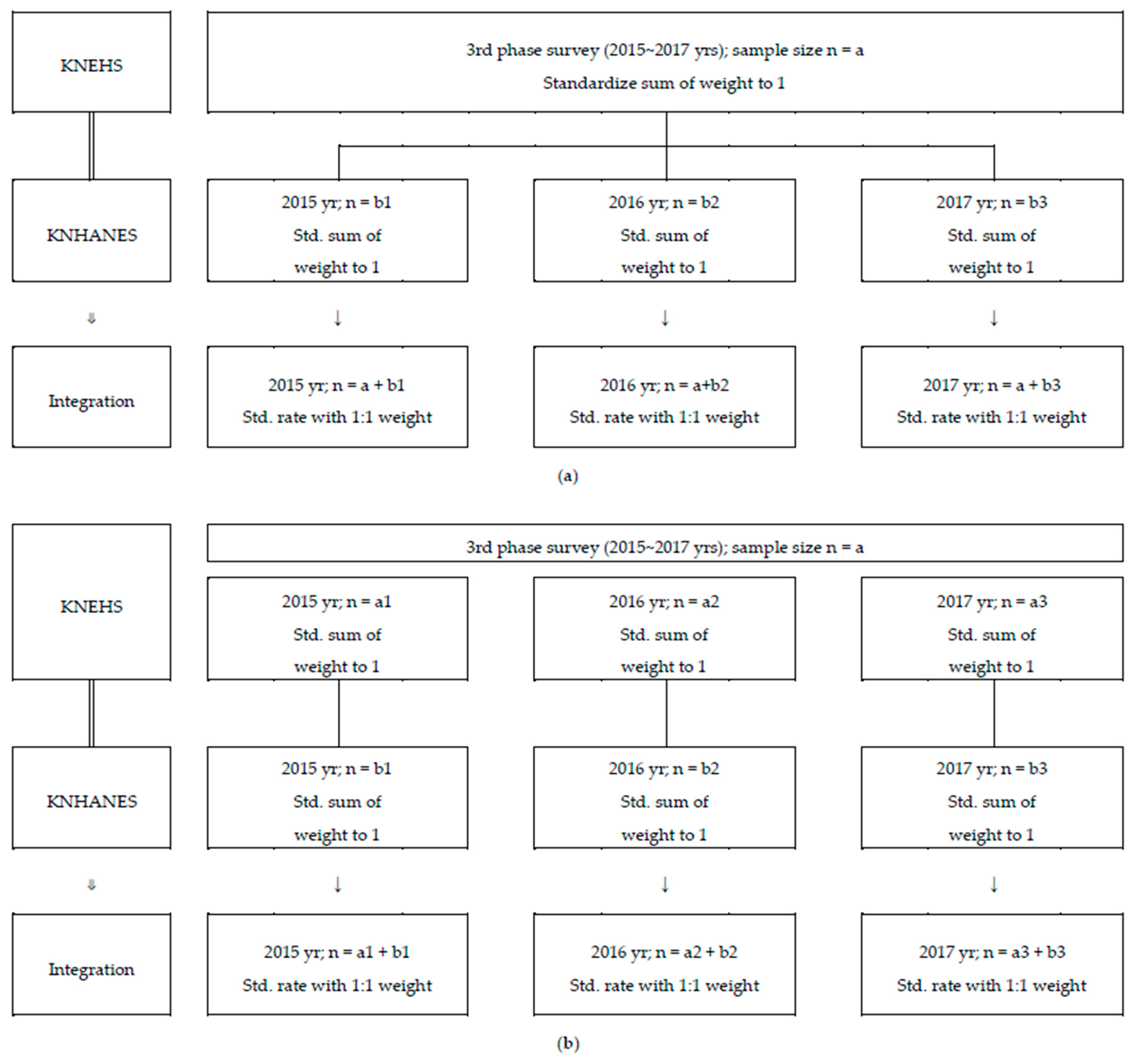
2.1.3. Data Integration
2.2. Statistics Analysis
3. Results
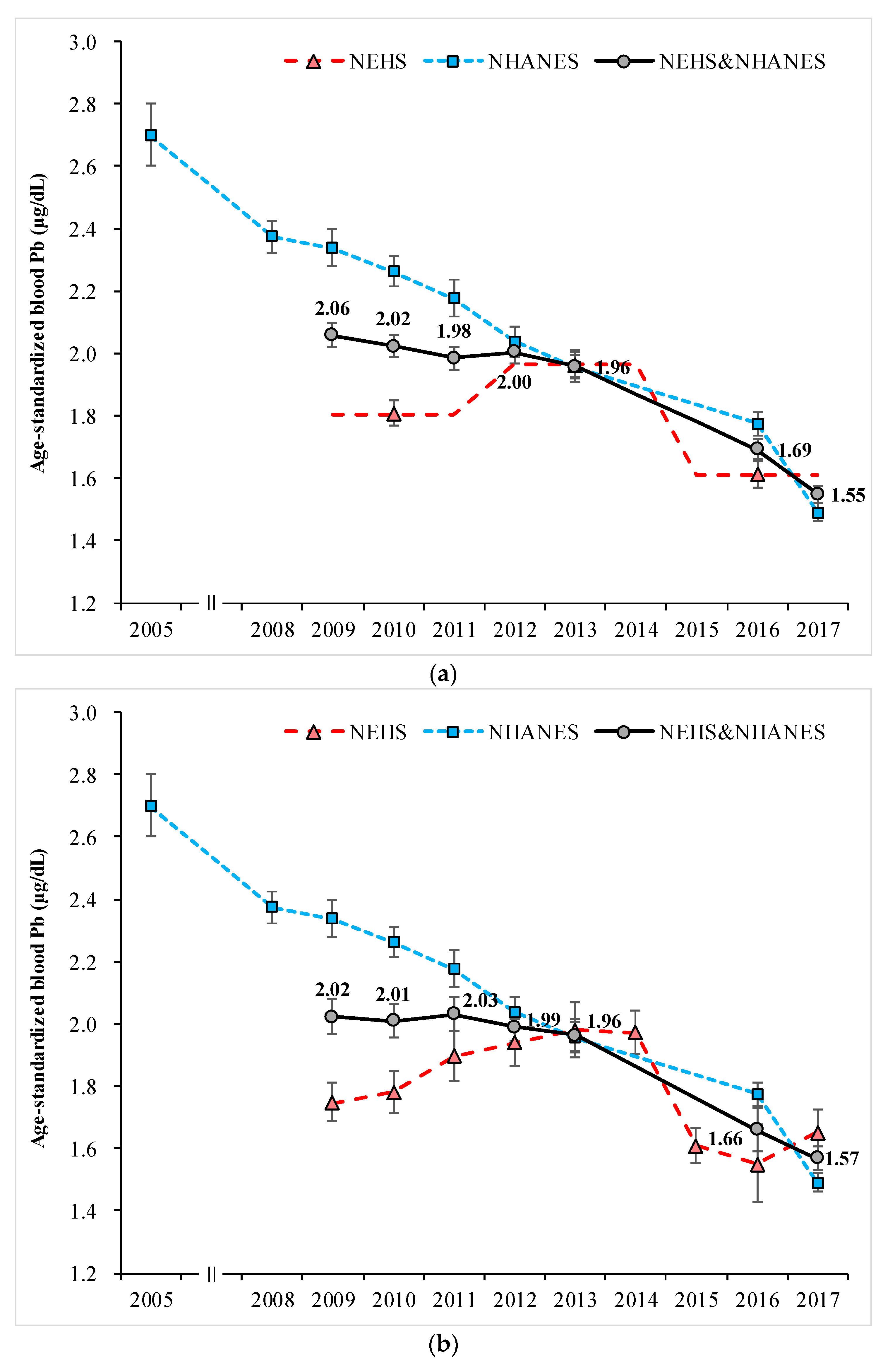
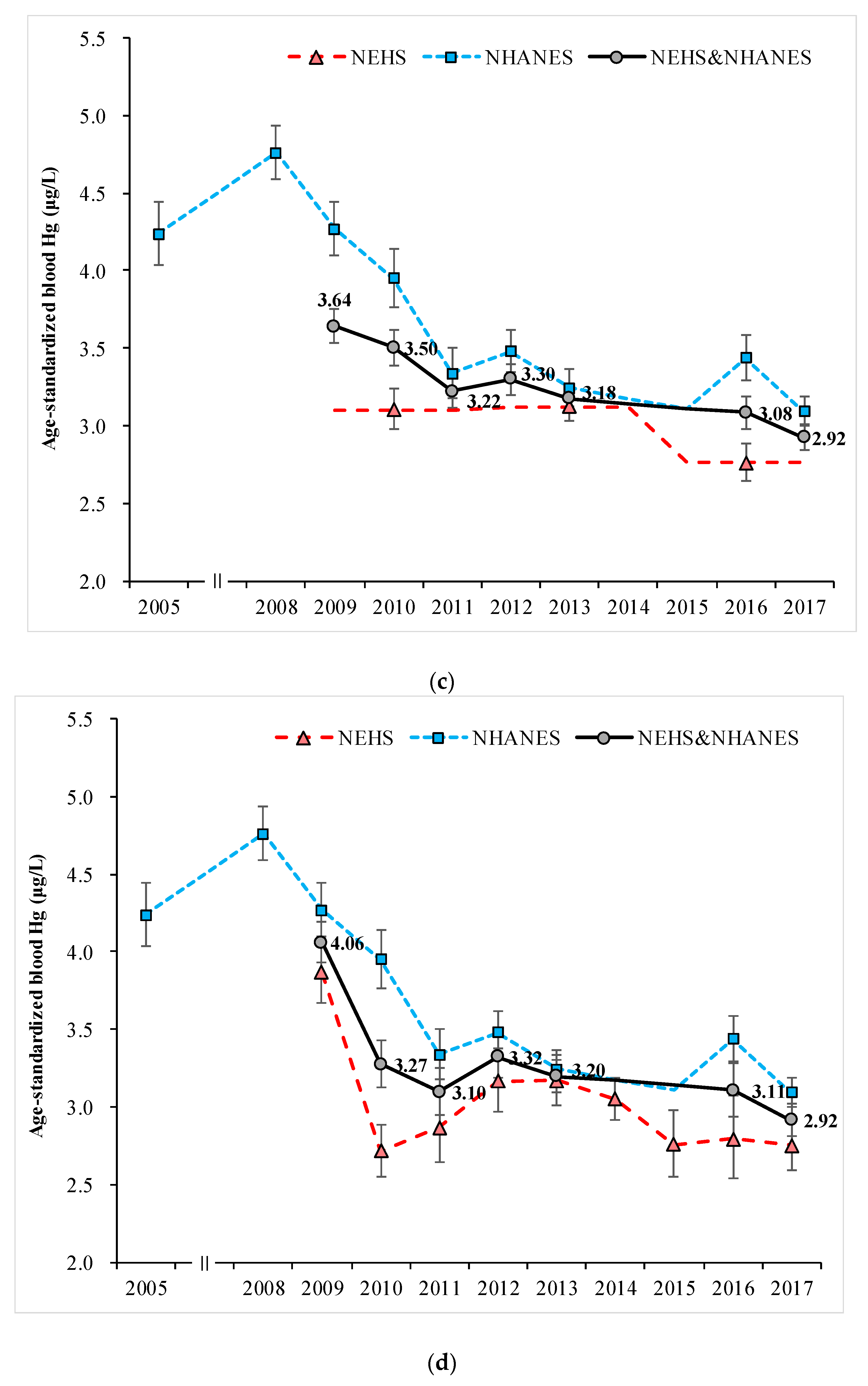
3.1. Combined Exposure Level of Blood Pb and Hg
3.2. Blood Pb and Hg Concentrations According to Demographic Characteristics
3.3. Exceedance of Reference Values for Blood Pb and Hg According to Demographic Characteristics
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- ATSDR(Agency for Toxic Substances and Disease Registry). Support Document to the 2019 Substance Priority List (Candidates for Toxicological Profiles); Agency for Toxic Substances and Disease Registry: Atlanta, GA, USA, 2020.
- KNIER(Korea National Institute of Environmental Research). Manual of Analysis of Environmentally Hazardous Substances on Biological Samples; The Korea National Institute of Environmental Research: Incheon, Korea, 2018.
- KNIER(Korea National Institute of Environmental Research). KNEHS’s Guide to Biological Sample Management(Revised); The Korea National Institute of Environmental Research: Incheon, Korea, 2019.
- KCDC (The Korea Centers for Disease Control and Prevention). Clinical Laboratory Test for the Korea National Health and Nutrition Examination Survey (III–VII); The Korea Centers for Disease Control and Prevention: Osong, Korea, 2008–2013, 2015, 2016, 2017.
- CDC(Centers for Disease Control and Prevention). Fourth National Report on Human Exposure to Environmental Chemicals, Updated Tables, January 2019; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2019.
- Haines, D.A.; Saravanabhavan, G.; Werry, K.; Khoury, C. An overview of human biomonitoring of environmental chemicals in the Canadian Health Measures Survey: 2007–2019. Int. J. Hyg. Environ. Health 2017, 220, 13–28. [Google Scholar] [CrossRef]
- Health Canada. Fifth Report on Human Biomonitoring of Environmental Chemicals in Canada; Minister of Health: Ottawa, ON, Canada, 2019.
- Schulz, C.; Conrad, A.; Becker, K.; Kolossa-Gehring, M.; Seiwert, M.; Seifert, B. Twenty years of the German Environmental Survey (GerES): Human biomonitoring–Temporal and spatial (West Germany/East Germany) differences in population exposure. Int. J. Hyg. Environ. Health 2007, 210, 271–297. [Google Scholar] [CrossRef]
- Bierkens, J.; Smolders, R.; Van Holderbeke, M.; Cornelis, C. Predicting blood lead levels from current and past environmental data in Europe. Sci. Total Environ. 2011, 409, 5101–5110. [Google Scholar] [CrossRef]
- McKelvey, W.; Gwynn, R.C.; Jeffery, N.; Kass, D.; Thorpe, L.E.; Garg, R.K.; Palmer, C.D.; Parsons, P.J. A biomonitoring study of lead, cadmium, and mercury in the blood of New York city adults. Environ. Health Perspect. 2007, 115, 1435–1441. [Google Scholar] [CrossRef]
- Tsoi, M.-F.; Cheung, C.-L.; Cheung, T.T.; Cheung, B.M.Y. Continual Decrease in Blood Lead Level in Americans: United States National Health Nutrition and Examination Survey 1999-2014. Am. J. Med. 2016, 129, 1213–1218. [Google Scholar] [CrossRef] [PubMed]
- Kalcher, K.; Kern, W.; Pietsch, R. Cadmium and lead in the smoke of a filter cigarette. Sci. Total Environ. 1993, 128, 21–35. [Google Scholar] [CrossRef]
- Pocock, S.; Shaper, A.; Walker, M.; Wale, C.; Clayton, B.; Delves, T.; Lacey, R.; Packham, R.; Powell, P. Effects of tap water lead, water hardness, alcohol, and cigarettes on blood lead concentrations. J. Epidemiol. Community Health 1983, 37, 1–7. [Google Scholar] [CrossRef]
- Symanski, E.; Hertz-Picciotto, I. Blood lead levels in relation to menopause, smoking, and pregnancy history. Am. J. Epidemiol. 1995, 141, 1047–1058. [Google Scholar] [CrossRef]
- Tola, S.; Nordman, C.H. Smoking and blood lead concentrations in lead-exposed workers and an unexposed population. Environ. Res. 1977, 13, 250–255. [Google Scholar] [CrossRef]
- Rhainds, M.; Levallois, P. Effects of maternal cigarette smoking and alcohol consumption on blood lead levels of newborns. Am. J. Epidemiol. 1997, 145, 250–257. [Google Scholar] [CrossRef][Green Version]
- Schuhmacher, M.; Domingo, J.; Llobet, J.; Corbella, J. Variability of blood lead levels in an urban population in relation to drinking and smoking habits. Sci. Total Environ. 1993, 138, 23–29. [Google Scholar] [CrossRef]
- National Toxicology Program. NTP Monograph: Health Effects of Low-Level Lead; National Toxicology Program: Durham, NC, USA, 2012.
- Charkiewicz, A.E.; Backstrand, J.R. Lead Toxicity and Pollution in Poland. Int. J. Environ. Res. Public Health 2020, 17, 4385. [Google Scholar] [CrossRef]
- Wani, A.L.; Ara, A.; Usmani, J.A. Lead toxicity: A review. Interdiscip. Toxicol. 2015, 8, 55–64. [Google Scholar] [CrossRef]
- Rehman, K.; Fatima, F.; Waheed, I.; Akash, M.S.H. Prevalence of exposure of heavy metals and their impact on health consequences. J. Cell. Biochem. 2018, 119, 157–184. [Google Scholar] [CrossRef] [PubMed]
- Apel, P.; Angerer, J.; Wilhelm, M.; Kolossa-Gehring, M. New HBM values for emerging substances, inventory of reference and HBM values in force, and working principles of the German Human Biomonitoring Commission. Int. J. Hyg. Environ. Health 2017, 220, 152–166. [Google Scholar] [CrossRef] [PubMed]
- CDC(Centers for Disease Control and Prevention). Adult Blood Lead Epidemiology and Surveillance (ABLES). Available online: https://www.cdc.gov/niosh/topics/ables/description.html (accessed on 14 March 2021).
- Mortensen, M.E.; Caudill, S.P.; Caldwell, K.L.; Ward, C.D.; Jones, R.L. Total and methyl mercury in whole blood measured for the first time in the U.S. population: NHANES 2011–2012. Environ. Res. 2014, 134, 257–264. [Google Scholar] [CrossRef]
- El-Safty, I.A.; Shouman, A.E.; Amin, N.E. Nephrotoxic effects of mercury exposure and smoking among Egyptian workers in a fluorescent lamp factory. Arch. Med. Res. 2003, 34, 50–55. [Google Scholar] [CrossRef]
- Kowalski, R.; Wierciński, J. Mercury content in smoke and tobacco from selected cigarette brands. Ecol. Chem. Eng. S 2009, 16, 155–162. [Google Scholar]
- Park, H.J.; Kim, K.S. Association of blood mercury concentrations with atopic dermatitis in adults: A population-based study in Korea. Environ. Res. 2011, 111, 573–578. [Google Scholar] [CrossRef]
- Wulf, H.; Kromann, N.; Kousgaard, N.; Hansen, J.; Niebuhr, E.; Albøge, K. Sister chromatid exchange (SCE) in greenlandic eskimos. dose—response relationship between SCE and seal diet, smoking, and blood cadmium and mercury concentrations. Sci. Total Environ. 1986, 48, 81–94. [Google Scholar] [CrossRef]
- Kudsk, F.N. The influence of ethyl alcohol on the absorption of mercury vapour from the lungs in man. Acta Pharm. Toxicol. 1965, 23, 263–274. [Google Scholar] [CrossRef] [PubMed]
- Leppert, B.; Havdahl, A.; Riglin, L.; Jones, H.J.; Zheng, J.; Davey Smith, G.; Tilling, K.; Thapar, A.; Reichborn-Kjennerud, T.; Stergiakouli, E. Association of Maternal Neurodevelopmental Risk Alleles With Early-Life Exposures. JAMA Psychiatry 2019, 76, 834–842. [Google Scholar] [CrossRef]
- Birch, R.J.; Bigler, J.; Rogers, J.W.; Zhuang, Y.; Clickner, R.P. Trends in blood mercury concentrations and fish consumption among US women of reproductive age, NHANES, 1999–2010. Environ. Res. 2014, 133, 431–438. [Google Scholar] [CrossRef] [PubMed]
- Razzaghi, H.; Tinker, S.C.; Crider, K. Blood mercury concentrations in pregnant and nonpregnant women in the United States: National Health and Nutrition Examination Survey 1999-2006. Am. J. Obstet. Gynecol. 2014, 210, e351–e357. [Google Scholar] [CrossRef] [PubMed]
- Franchi, E.; Loprieno, G.; Ballardin, M.; Petrozzi, L.; Migliore, L. Cytogenetic monitoring of fishermen with environmental mercury exposure. Mutat. Res. Genet. Toxicol. 1994, 320, 23–29. [Google Scholar] [CrossRef]
- Hsu, C.S.; Liu, P.L.; Chien, L.C.; Chou, S.Y.; Han, B.C. Mercury concentration and fish consumption in Taiwanese pregnant women. BJOG Int. J. Obstet. Gynaecol. 2007, 114, 81–85. [Google Scholar] [CrossRef]
- Izati, D.W.; Tualeka, A.R.; Singga, S.; Rahmawati, P.; Russeng, S.S.; Wahyu, A. Safe Concentration of Mercury (Hg) Exposure in Fish Consumed by the Residents of Bulawa Subdistrict, Bone Bolango District, Gorontalo Province, Indonesia. Indian J. Public Health Res. Dev. 2019, 10, 1665–1669. [Google Scholar] [CrossRef]
- Jo, E.M.; Kim, B.G.; Kim, Y.M.; Yu, S.D.; You, C.H.; Kim, J.Y.; Hong, Y.S. Blood mercury concentration and related factors in an urban coastal area in Korea. J. Prev. Med. Public Health 2010, 43, 377–386. [Google Scholar] [CrossRef]
- Kim, K.W.; Sreeja, S.R.; Kwon, M.; Yu, Y.L.; Kim, M.K. Association of Blood Mercury Level with the Risk of Depression According to Fish Intake Level in the General Korean Population: Findings from the Korean National Health and Nutrition Examination Survey (KNHANES) 2008–2013. Nutrients 2020, 12, 189. [Google Scholar] [CrossRef]
- Mahaffey, K.R.; Clickner, R.P.; Jeffries, R.A. Adult women’s blood mercury concentrations vary regionally in the United States: Association with patterns of fish consumption (NHANES 1999–2004). Environ. Health Perspect. 2009, 117, 47–53. [Google Scholar] [CrossRef]
- You, C.H.; Kim, B.G.; Kim, J.M.; Yu, S.D.; Kim, Y.M.; Kim, R.B.; Hong, Y.S. Relationship between blood mercury concentration and waist-to-hip ratio in elderly Korean individuals living in coastal areas. J. Prev. Med. Public Health 2011, 44, 218. [Google Scholar] [CrossRef] [PubMed]
- Hightower, J.M.; O’Hare, A.; Hernandez, G.T. Blood mercury reporting in NHANES: Identifying Asian, Pacific Islander, Native American, and multiracial groups. Environ. Health Perspect. 2006, 114, 173–175. [Google Scholar] [CrossRef] [PubMed]
- Guillen, J.; Natale, F.; Carvalho, N.; Casey, J.; Hofherr, J.; Druon, J.-N.; Fiore, G.; Gibin, M.; Zanzi, A.; Martinsohn, J.T. Global seafood consumption footprint. Ambio 2019, 48, 111–122. [Google Scholar] [CrossRef] [PubMed]
- Joint Research Centre. How Much Fish Do We Consume? First Global Seafood Consumption Footprint Published. Available online: https://ec.europa.eu/jrc/en/news/how-much-fish-do-we-consume-first-global-seafood-consumption-footprint-published (accessed on 28 April 2021).
| Heavy Metal | Survey Data | Weighted GM (Stderr) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| KNEHS Phase | 1st | 2nd | 3rd | ||||||||||
| KNHANES Phase | 3rd | 4th | 5th | 6th | 7th | ||||||||
| Year | 2005 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | ||
| Blood Pb (μg/dL) | Phase | KNEHS | 1.768 (0.023) | 1.940 (0.024) | 1.603 (0.023) | ||||||||
| KNHANES | 2.611 (0.050) | 2.306 (0.019) | 2.119 (0.015) | 1.935 (0.026) | 1.617 (0.016) | ||||||||
| Year | KNEHS | 1.725 (0.040) | 1.748 (0.037) | 1.836 (0.044) | 1.920 (0.042) | 1.934 (0.043) | 1.963 (0.040) | 1.591 (0.031) | 1.554 (0.062) | 1.647 (0.042) | |||
| KNHANES | 2.611 (0.050) | 2.320 (0.026) | 2.293 (0.030) | 2.215 (0.025) | 2.142 (0.032) | 2.005 (0.026) | 1.935 (0.026) | 1.764 (0.022) | 1.482 (0.017) | ||||
| Integration by method 1 | 1.989 (0.032) | 1.967 (0.028) | 1.984 (0.030) | 1.962 (0.026) | 1.935 (0.025) | 1.656 (0.036) | 1.562 (0.022) | ||||||
| Integration by method 2 | 2.014 (0.021) | 1.979 (0.020) | 1.947 (0.021) | 1.972 (0.018) | 1.938 (0.018) | 1.682 (0.017) | 1.541 (0.014) | ||||||
| Blood Hg (μg/L) | Phase | KNEHS | 3.083 (0.066) | 3.113 (0.050) | 2.752 (0.066) | ||||||||
| KNHANES | 4.188 (0.100) | 4.481 (0.060) | 3.557 (0.048) | 3.268(0.063) | 3.253 (0.044) | ||||||||
| Year | KNEHS | 3.808 (0.105) | 2.697 (0.086) | 2.873 (0.124) | 3.167 (0.106) | 3.136 (0.089) | 3.050 (0.074) | 2.729 (0.113) | 2.852 (0.138) | 2.733 (0.084) | |||
| KNHANES | 4.188 (0.100) | 4.729 (0.086) | 4.247 (0.088) | 3.916 (0.099) | 3.324 (0.085) | 3.456 (0.071) | 3.268 (0.063) | 3.427 (0.076) | 3.088 (0.050) | ||||
| Integration by method 1 | 4.022 (0.070) | 3.251 (0.076) | 3.091 (0.079) | 3.309 (0.069) | 3.201 (0.055) | 3.128 (0.088) | 2.907 (0.052) | ||||||
| Integration by method 2 | 3.619 (0.056) | 3.475 (0.060) | 3.202 (0.054) | 3.280 (0.049) | 3.189 (0.040) | 3.073 (0.054) | 2.916 (0.043) | ||||||
| Factor | Level | 3rd Phase KNEHS (‘15~‘17) and 7th Phase KNHANES (‘16~‘17) Integrated Data | ||||
|---|---|---|---|---|---|---|
| n (%) | Weighted GM (95% CI) | |||||
| Blood Pb (μg/dL) | Blood Hg (μg/L) | |||||
| Total | Crude | 8618 (100.0) | 1.61 (1.58–1.64) | 2.99 (2.91–3.07) | ||
| Age standardized | 1.62 (1.59–1.64) | 3.01 (2.93–3.08) | ||||
| Adjusted | 1.61 (1.58–1.63) | 2.98 (2.90–3.06) | ||||
| Survey | KNEHS | 3787 (43.9) | 1.60 (1.56–1.64) | 2.81 (2.68–2.94) | ||
| KNHANES | 4831 (56.1) | 1.62 (1.59–1.64) | 3.18 (3.09–3.27) | |||
| p-value | 0.517 | <.001 | ||||
| Sex | Male | 3797 (44.1) | 1.87 (1.84–1.91) | 3.60 (3.48–3.72) | ||
| age standardized | Female | 4821 (55.9) | 1.40 (1.38–1.42) | 2.51 (2.44–2.58) | ||
| p-value | <0.001 | <0.001 | ||||
| Sex | Male | 3797 (44.1) | 1.78 (1.75–1.82) | 3.41 (3.28–3.55) | ||
| Female | 4821 (55.9) | 1.45 (1.42–1.48) | 2.61 (2.53–2.70) | |||
| p-value | <0.001 | <0.001 | ||||
| Age(yr) | 18–29 | 879 (10.2) | 1.22 (1.17–1.27) | a | 2.08 (1.95–2.23) | a |
| 30–39 | 1384 (16.1) | 1.43 (1.39–1.47) | b | 2.89 (2.77–3.02) | b | |
| 40–49 | 1558 (18.1) | 1.59 (1.56–1.63) | c | 3.22 (3.09–3.35) | cd | |
| 50–59 | 1852 (21.5) | 1.89 (1.84–1.93) | d | 3.45 (3.32–3.59) | cd | |
| 60–69 | 1706 (19.8) | 1.92 (1.87–1.98) | d | 3.52 (3.34–3.70) | d | |
| ≥70 | 1239 (14.4) | 1.88 (1.81–1.96) | d | 3.08 (2.87–3.31) | bc | |
| p-value | <0.001 | <0.001 | ||||
| Smoke | Currently | 1527 (17.9) | 1.82 (1.77–1.87) | a | 3.16 (3.01–3.32) | a |
| Former | 1743 (20.4) | 1.63 (1.59–1.68) | b | 3.13 (2.99–3.27) | a | |
| Never | 5276 (61.7) | 1.53 (1.50–1.56) | c | 2.88 (2.78–2.98) | c | |
| p-value | <0.001 | 0.003 | ||||
| Drink | Currently | 6081 (71.1) | 1.64 (1.61–1.66) | a | 3.05 (2.97–3.14) | a |
| Former | 1187 (13.9) | 1.51 (1.46–1.55) | b | 2.68 (2.57–2.80) | b | |
| Never | 1282 (15.0) | 1.53 (1.48–1.58) | b | 2.85 (2.72–3.00) | b | |
| p-value | <.001 | <.001 | ||||
| House income | Low | 1568 (18.2) | 1.64 (1.59–1.70) | 2.76 (2.62–2.91) | a | |
| Middle low | 2715 (31.6) | 1.63 (1.59–1.68) | 2.86 (2.75–2.98) | ab | ||
| Middle high | 2265 (26.3) | 1.59 (1.55–1.63) | 3.02 (2.92–3.14) | bc | ||
| High | 2055 (23.9) | 1.58 (1.54–1.62) | 3.19 (3.06–3.34) | c | ||
| p-value | 0.135 | <0.001 | ||||
| Education level | Below elementary | 2148 (25.7) | 1.64 (1.59–1.69) | 2.67 (2.54–2.82) | a | |
| Middle | 1625 (19.4) | 1.59 (1.54–1.64) | 2.83 (2.70–2.97) | a | ||
| High | 2355 (28.1) | 1.62 (1.58–1.65) | 3.06 (2.95–3.17) | b | ||
| Above college | 2243 (26.8) | 1.59 (1.55–1.62) | 3.26 (3.14–3.38) | c | ||
| p-value | 0.160 | <0.001 | ||||
| Factor | Level | 3rd Phase KNEHS (‘15~’17) and 7th Phase KNHANES (‘16~’17) Integrated Data | ||||
|---|---|---|---|---|---|---|
| n (%) | Weighted % (95% CI) | |||||
| Blood Pb ≥ 5 μg/dL | Blood Hg ≥ 5 μg/L | |||||
| Total | Crude | 8618 (100.0) | 0.75 (0.51–0.99) | 20.99 (19.65–22.33) | ||
| Age standardized | 0.76 (0.52–1.00) | 21.18 (19.83–22.52) | ||||
| Adjusted | 0.77 (0.52–1.02) | 20.79 (19.45–22.13) | ||||
| Survey | KNEHS | 3787 (43.9) | 0.98 (0.59–1.36) | 19.11 (16.91–21.32) | ||
| KNHANES | 4831 (56.1) | 0.55 (0.27–0.83) | 22.54 (20.82–24.26) | |||
| p-value | 0.071 | 0.021 | ||||
| Sex | Male | 3797 (44.1) | 1.30 (0.88–1.72) | 30.84 (28.78–32.90) | ||
| Age standardized | Female | 4821 (55.9) | 0.24 (0.09–0.39) | 11.53 (10.22–12.85) | ||
| p-value | <0.001 | <0.001 | ||||
| Sex | Male | 3797 (44.1) | 1.06 (0.72–1.40) | 28.09 (25.84–30.33) | ||
| Female | 4821 (55.9) | 0.49 (0.25–0.73) | 13.64 (12.00–15.27) | |||
| p-value | <0.001 | <0.001 | ||||
| Age (yr) | 18–29 | 879 (10.2) | 0.75 (0.00–1.70) | 5.72 (3.41–8.03) | a | |
| 30–39 | 1384 (16.1) | 0.37 (0.00–0.75) | 17.37 (14.39–20.34) | b | ||
| 40–49 | 1558 (18.1) | 0.42 (0.00–0.91) | 23.63 (20.86–26.39) | c | ||
| 50–59 | 1852 (21.5) | 1.21 (0.57–1.85) | 26.81 (24.31–29.31) | c | ||
| 60–69 | 1706 (19.8) | 0.83 (0.27–1.40) | 29.76 (26.62–32.90) | c | ||
| ≥70 | 1239 (14.4) | 1.26 (0.30–2.21) | 24.24 (20.25–28.23) | bc | ||
| p-value | 0.226 | <0.001 | ||||
| Smoke | Currently | 1527 (17.9) | 1.72 (0.83–2.61) | a | 24.35 (21.21–27.49) | a |
| Former | 1743 (20.4) | 0.79 (0.19–1.40) | ab | 23.17 (20.17–26.18) | ab | |
| Never | 5276 (61.7) | 0.44 (0.21–0.67) | b | 18.80(17.05–20.54) | c | |
| p-value | 0.023 | 0.004 | ||||
| Drink | Currently | 6081 (71.1) | 0.81 (0.53–1.10) | 21.99 (20.51–23.46) | a | |
| Former | 1187 (13.9) | 0.72 (0.24–1.21) | 14.61 (12.11–17.10) | b | ||
| Never | 1282 (15.0) | 0.55 (0.02–1.09) | 19.57 (16.82–22.31) | a | ||
| p-value | 0.703 | <0.001 | ||||
| House income | Low | 1568 (18.2) | 1.06 (0.22–1.91) | 16.30 (13.54–19.07) | a | |
| Middle low | 2715 (31.6) | 1.00 (0.39–1.62) | 18.04 (15.95–20.13) | ab | ||
| Middle high | 2265 (26.3) | 0.60 (0.23–0.98) | 21.23 (19.09–23.38) | bc | ||
| High | 2055 (23.9) | 0.55 (0.16–0.94) | 25.55 (22.90–28.20) | c | ||
| p-value | 0.533 | <0.001 | ||||
| Education level | Below elementary | 2148 (25.7) | 1.06 (0.37–1.76) | 16.87 (14.34–19.41) | a | |
| Middle | 1625 (19.4) | 1.11 (0.27–1.95) | 18.27 (15.80–20.75) | a | ||
| High | 2355 (28.1) | 0.52 (0.17–0.86) | 22.29 (20.09–24.48) | b | ||
| Above college | 2243 (26.8) | 0.58 (0.23–0.93) | 23.84 (21.62–26.06) | b | ||
| p-value | 0.419 | <0.001 | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Seo, J.-W.; Hong, Y.-S.; Kim, B.-G. Assessment of Lead and Mercury Exposure Levels in the General Population of Korea Using Integrated National Biomonitoring Data. Int. J. Environ. Res. Public Health 2021, 18, 6932. https://doi.org/10.3390/ijerph18136932
Seo J-W, Hong Y-S, Kim B-G. Assessment of Lead and Mercury Exposure Levels in the General Population of Korea Using Integrated National Biomonitoring Data. International Journal of Environmental Research and Public Health. 2021; 18(13):6932. https://doi.org/10.3390/ijerph18136932
Chicago/Turabian StyleSeo, Jeong-Wook, Young-Seoub Hong, and Byoung-Gwon Kim. 2021. "Assessment of Lead and Mercury Exposure Levels in the General Population of Korea Using Integrated National Biomonitoring Data" International Journal of Environmental Research and Public Health 18, no. 13: 6932. https://doi.org/10.3390/ijerph18136932
APA StyleSeo, J.-W., Hong, Y.-S., & Kim, B.-G. (2021). Assessment of Lead and Mercury Exposure Levels in the General Population of Korea Using Integrated National Biomonitoring Data. International Journal of Environmental Research and Public Health, 18(13), 6932. https://doi.org/10.3390/ijerph18136932






