Measuring the Level of Medical-Emergency-Related Knowledge among Senior Dental Students and Clinical Trainers
Abstract
1. Advances in Knowledge
2. Application to Patient Care
3. Introduction
4. Materials and Methods
5. Statistical Analysis
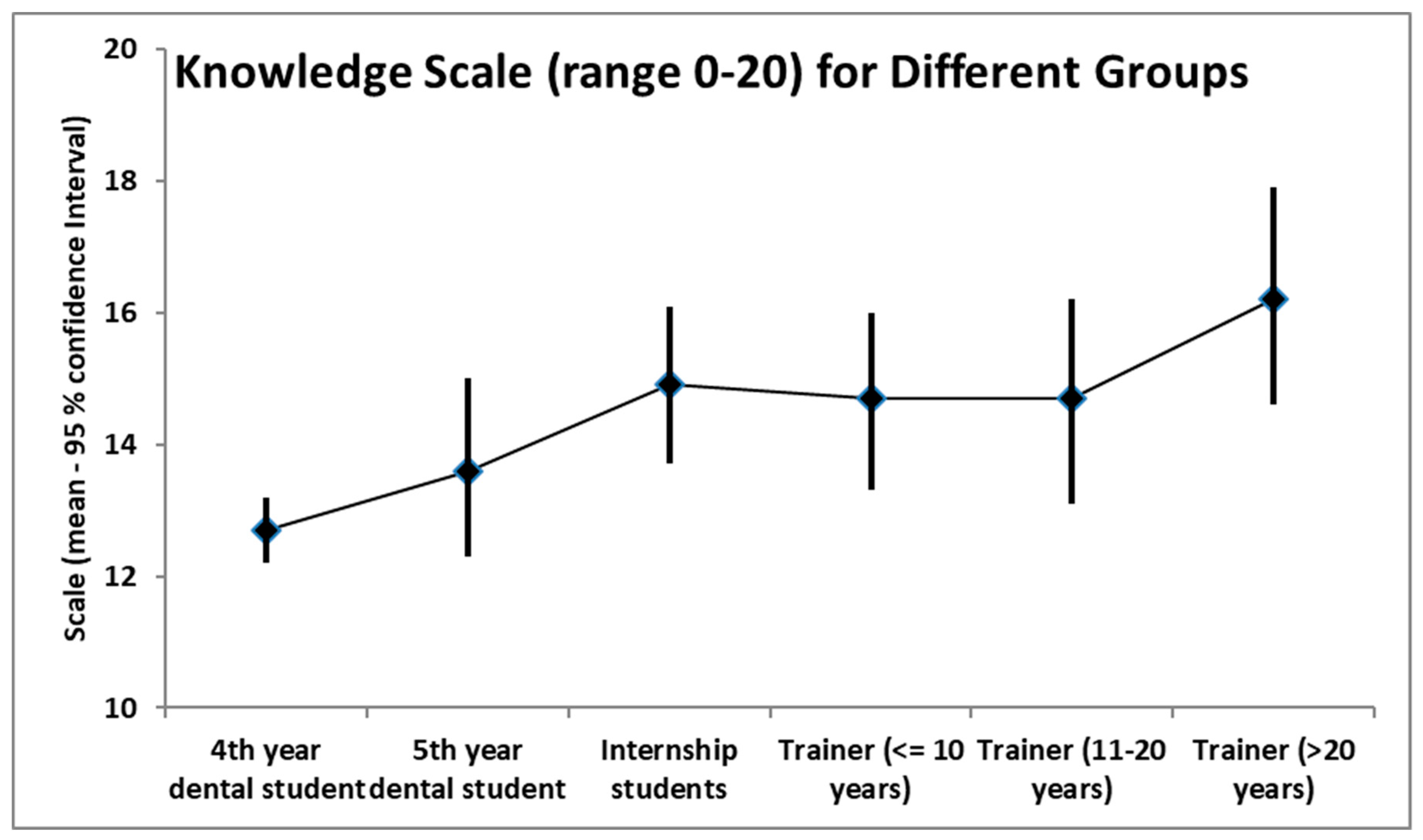
6. Results
7. Discussion
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wilson, M.H.; McArdle, N.S.; Fitzpatrick, J.J.; Stassen, L.F. Medical emergencies in dental practice. J. Ir. Dent. Assoc. 2009, 5, 134–143. [Google Scholar]
- Paquette, D.W.; Bell, K.P.; Phillips, C.; Offenbacher, S.; Wilder, R.S. Dentists’ knowledge and opinions of oral-systemic disease relationships: Relevance to patient care and education. J. Dent. Educ. 2015, 79, 626–635. [Google Scholar] [CrossRef] [PubMed]
- Al-Shamiri, H.M.; Al-Maweri, S.A.; Shugaa-Addin, B.; Alaizari, N.A.; Hunaish, A. Awareness of basic life support among Saudi dental students and interns. Eur. J. Dent. 2017, 11, 521–525. [Google Scholar] [CrossRef][Green Version]
- Jodalli, P.S.; Ankola, A.V. Evaluation of knowledge, experience and perceptions about medical emergencies amongst dental graduates (Interns) of Belgaum City, India. J. Clin. Exp. Dent. 2012, 4, e14–e18. [Google Scholar] [CrossRef]
- de Bedout, T.; Kramer, K.; Blanchard, S.; Hamada, Y.; Eckert, G.J.; Maupome, G.; John, V. Assessing the Medical Emergency Preparedness of Dental Faculty, Residents, and Practicing Periodontists: An Exploratory Study. J. Dent. Educ. 2018, 82, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Coulthard, P.; Bridgman, C.M.; Larkin, A.; Worthington, H.V. Appropriateness of a Resuscitation Council (UK) advanced life support course for primary care dentists. Br. Dent. J. 2000, 188, 507–512. [Google Scholar] [CrossRef]
- Saquib, S.A.; Al-Harthi, H.M.; Khoshhal, A.A.; Shaher, A.A.; Al-Shammari, A.B.; Khan, A.; Al-Qahtani, T.A.; Khalid, I. Knowledge and Attitude about Basic Life Support and Emergency Medical Services amongst Healthcare Interns in University Hospitals: A Cross-Sectional Study. Emerg. Med. Int. 2019, 3, 9342892. [Google Scholar] [CrossRef]
- Coulthard, P.; Horner, K.; Sloan, P.; Theaker, E.D. Master Dentistry: Oral and Maxillofacial Surgery, Radiology, Pathology and Oral Medicine, 3rd ed.; Churchill Livingstone: London, UK, 2013. [Google Scholar]
- Al-Samadani, K.H.; Gazal, G. Effectiveness of benzocaine in reducing deep cavity restoration and post-extraction stress in dental patients. Saudi Med. J. 2015, 36, 1342–1347. [Google Scholar] [CrossRef] [PubMed]
- Gazal, G. Is prilocaine safe and potent enough for use in the oral surgery of medically compromised patients. Saudi Med. J. 2019, 40, 97–100. [Google Scholar] [CrossRef]
- Dym, H.; Barzani, G.; Mohan, N. Emergency Drugs for the Dental Office. Dent. Clin. N. Am. 2016, 60, 287–294. [Google Scholar] [CrossRef] [PubMed]
- Blitz, M.; Britton, K.C. Management of the uncooperative child. Oral Maxillofac. Surg. Clin. N. Am. 2010, 22, 461–469. [Google Scholar] [CrossRef]
- Samaei, H.; Weiland, T.J.; Dilley, S.; Jelinek, G.A. Knowledge and confidence of a convenience sample of Australasian emergency doctors in managing dental emergencies: Results of a survey. Emerg. Med. Int. 2015, 2015, 148384. [Google Scholar] [CrossRef]
- Miller, C.J.; Metz, M.J. Can clinical scenario videos improve dental students’ perceptions of the basic sciences and ability to apply content knowledge? J. Dent. Educ. 2015, 79, 1452–1460. [Google Scholar] [CrossRef] [PubMed]
- Whitney, E.M.; Walton, J.N.; Aleksejuniene, J.; Schönwetter, D.J. Graduating dental students’ views of competency statements: Importance, confidence, and time trends from 2008 to 2012. J. Dent. Educ. 2015, 79, 322–330. [Google Scholar] [CrossRef] [PubMed]
- Goodchild, J.H.; Dickinson, S.C. Anxiolysis in dental practice: A report of three cases. Gen. Dent. 2004, 52, 264–268. [Google Scholar] [PubMed]
- Al-Iryani, G.M.; Ali, F.M.; Alnami, N.H.; Almashhur, S.K.; Adawi, M.A.; Tairy, A.A. Knowledge and preparedness of dental practitioners on management of medical emergencies in Jazan province. Maced. J. Med. Sci. 2018, 6, 402–405. [Google Scholar] [CrossRef] [PubMed]
- McKernon, S.L.; Kaura, L.; Taylor, K.H.; Reid, S.; Balmer, M.C. An Update on current Resuscitation Council (UK) Guidelines. Dent. Update 2017, 44, 341–350. [Google Scholar] [CrossRef] [PubMed]
- Lello, S.; Burke, J.; Taylor, K. A review of the available guidance regarding management of medical emergencies in primary dental care. Dent. Update 2016, 43, 928–932. [Google Scholar] [CrossRef]
- Malamed, S.F. Medical emergencies in the dental surgery. Part 1: Preparation of the office and essential management. J. Ir. Dent. Assoc. 2015, 61, 302–308. [Google Scholar]
- Hashim, R.; Mathew, L.S.; Rustom, S.; Amer, F.; Odeh, R. Emergency medical care in dentistry: A cross sectional analysis of competencies for undergraduate students. Int. J. Crit. Illn. Inj. Sci. 2021, 11, 33–38. [Google Scholar] [CrossRef]
- Al-Sebaei, M.O.; Alkayyal, M.A.; Alsulimani, A.H.; Alsulaimani, O.S.; Habib, W.T. The preparedness of private dental offices and polyclinics for medical emergencies. A survey in western Saudi Arabia. Saudi Med. J. 2015, 36, 335–340. [Google Scholar] [CrossRef] [PubMed]
- Gazal, G. Management of an emergency tooth extraction in diabetic patients on the dental chair. Saudi Dent. J. 2020, 32, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Solanki, C.; Geisinger, M.L.; Luepke, P.G.; Al-Bitar, K.; Palomo, L.; Lee, W.; Blanchard, S.; Shin, D.; Maupome, G.; Eckert, G.J.; et al. Assessing readiness to manage medical emergencies among dental students at four dental schools. J. Dent. Educ. 2021. [Google Scholar] [CrossRef] [PubMed]
| Medical Emergency Scenario | Proposed Management |
|---|---|
| Lay flat +/− give oxygen→expect prompt recovery |
| Ask patient to re-breath from cupped hands or reservoir bag |
| Lay flat, give oxygen, and sit up very slowly |
| Give glucose with a little water or glucose oral gel |
| 1 mg Glucagon injection |
| Place the patient in recovery position and check airway after convulsive movements have subsided |
| Lay flat + give oxygen + 200 mg hydrocortisone IV |
| Sit up + give oxygen + salbutamol |
| 1 mL adrenaline (1 mg/mL) for IM |
| Reverse of conscious sedation by giving 0.2 mg Flumazenil IV over 15 s |
| Reassure the patient and transfer to hospital |
| Transfer to hospital |
| 400 mcg nitroglycerin spray + 300 mg aspirin chewable tablets + 50% oxygen with 50% nitrous oxide |
| Give oxygen and allow home if mild and rapidly recovered |
| Hospital for giving: IV diamorphine + thrombolytic therapy (heparin) |
| Immediate cardiopulmonary resuscitation (CPR) |
| After 30 chest compression, give 2 breaths (the 30:2 cycle of CPR) |
| Arrangement for a coagulation screen and liver function tests prior to surgery |
| Check if patient has eaten and give him some glucose |
| Dental extraction must be done the day following dialysis because there is no active heparin in circulation |
| Characteristics of Participants | Students (n = 202) | Trainers (n = 41) | |
|---|---|---|---|
| Gender | Female | 56.4% (114) | 70.7% (29) |
| Male | 43.6% (88) | 29.3% (12) | |
| Nationality | Saudi | 100% (202) | 22% (9) |
| Non-Saudi | 0% (0) | 78% (32) | |
| Year of study (Students) | 4th year | 70.8% (143) | - |
| 5th year | 17.3% (35) | - | |
| Internship | 11.9% (24) | - | |
| Experience (Trainers) | Trainer <= 10 years | - | 22%(9) |
| Trainer 11–20 years | - | 43.9% (18) | |
| Trainer > 20 years | - | 34.1% (14) | |
| Qualification (Trainers) | Bachelor | - | 2.4% (1) |
| MSc | - | 12.2% (5) | |
| Board | - | 14.6% (6) | |
| PhD | - | 70.7% (29) | |
| Mean ± SD | Mean (SD) | ||
| Age | 22.9 ± 1.3 | 43.8 ± 8.2 | |
| Clinical experience in years (Trainers) | - | 18.8 ± 8.7 | |
| Medical Emergency Scenario | 4th Year (N = 143) % (95% CI) | 5th Year (N = 35) % (95% CI) | Internship (24) % (95% CI) | Trainer (41) % (95% CI) | p |
|---|---|---|---|---|---|
| Fainting patient in dental chair | 72.7% (64.7–79.8%) | 60% (42.1–76.1%) | 83.3% (62.6–95.3%) | 92.7% (80.1–98.5%) | 0.01 * |
| Patient with hyperventilation | 65.7% (57.3–73.5%) | 62.9% (44.9–78.5%) | 91.7% (73–99%) | 70.7% (54.5–83.9%) | 0.17 |
| Patient with postural hypotension | 65.7% (57.3–73.5%) | 74.3% (56.7–87.5%) | 79.2% (57.8–92.9%) | 90.2% (76.9–97.3%) | 0.001 * |
| Conscious patient with hypoglycemia | 96.5% (92–98.9%) | 100% (90–100%) | 100% (85.8–100%) | 92.7% (80.1–98.5%) | 0.49 |
| Unconscious patient with hypoglycemia | 75.5% (67.6–82.3%) | 65.7% (47.8–80.9%) | 75% (53.3–90.2%) | 63.4% (46.9–77.9%) | 0.16 |
| Epileptic seizure | 73.4% (65.4–80.5%) | 80% (63.1–91.6%) | 87.5% (67.6–97.3%) | 85.4% (70.8–94.4%) | 0.05 * |
| Crisis of hypoadrenalism | 30.1% (22.7–38.3%) | 45.7% (28.8–63.4%) | 50% (29.1–70.9%) | 61% (44.5–75.8%) | <0.001 * |
| Acute asthmatic attack | 68.5% (60.2–76%) | 85.7% (69.7–95.2%) | 91.7% (73–99%) | 90.2% (76.9–97.3%) | 0.001 * |
| Anaphylactic shock | 50.3% (41.9–58.8%) | 71.4% (53.7–85.4%) | 79.2% (57.8–92.9%) | 70.7% (54.5–83.9%) | 0.002 * |
| Deeply sedated with benzodiazepine overdose | 24.5% (17.7–32.4%) | 54.3% (36.6–71.2%) | 41.7% (22.1–63.4%) | 34.1% (20.1–50.6%) | 0.08 |
| Sudden onset of brain stroke | 67.1% (58.8–74.8%) | 68.6% (50.7–83.1%) | 70.8% (48.9–87.4%) | 68.3% (51.9–81.9%) | 0.8 |
| Psychiatric patient | 60.8% (52.3–68.9%) | 65.7% (47.8–80.9%) | 62.5% (40.6–81.2%) | 56.1% (39.7–71.5%) | 0.69 |
| Crushed chest pain | 47.6% (39.1–56.1%) | 37.1% (21.5–55.1%) | 70.8% (48.9–87.4%) | 78% (62.4–89.4%) | <0.001 * |
| Episode of chest pain relieved by rest and nitrates | 50.3% (41.9–58.8%) | 51.4% (34–68.6%) | 50% (29.1–70.9%) | 73.2% (57.1–85.8%) | 0.03 * |
| Severe chest pain not relieved by rest and nitrates | 51.7% (43.2–60.2%) | 37.1% (21.5–55.1%) | 54.2% (32.8–74.4%) | 68.3% (51.9–81.9%) | 0.11 |
| Sudden heart arrest | 81.8% (74.5–87.8%) | 74.3% (56.7–87.5%) | 87.5% (67.6–97.3%) | 97.6% (87.1–99.9%) | 0.02 * |
| Cardiopulmonary resuscitation steps | 71.3% (63.2–78.6%) | 82.9% (66.4–93.4%) | 70.8% (48.9–87.4%) | 85.4% (70.8–94.4%) | 0.1 |
| Chronic liver disease needs dental extraction | 69.2% (61–76.7%) | 74.3% (56.7–87.5%) | 91.7% (73–99%) | 85.4% (70.8–94.4%) | 0.008 |
| Known diabetes who becomes sweaty, with nausea and tachycardia | 73.4% (65.4–80.5%) | 91.4% (76.9–98.2%) | 75% (53.3–90.2%) | 85.4% (70.8–94.4%) | 0.11 |
| Renal failure needs dental extraction | 71.3% (63.2–78.6%) | 80% (63.1–91.6%) | 79.2% (57.8–92.9%) | 70.7% (54.5–83.9%) | 0.79 |
| 4th Year Dental Student (143) | 5th Year Dental Student (35) | Internship Dental Student (24) | Trainer <=10 Years (9) | Trainer 11–20 Years (18) | Trainer >20 Years (14) | p | |
|---|---|---|---|---|---|---|---|
| Received training in the management of medical emergencies during Undergraduate dental program | 53.8% (77) | 71.4% (25) | 58.3% (14) | 88.9% (8) | 94.4% (17) | 64.3% (9) | 0.004 * |
| Quality of training | - | - | - | - | - | - | 0.07 |
| Poor | 15.6% (12) | 4% (1) | 14.3% (2) | 0% (0) | 11.8% (2) | 0% (0) | |
| Fair | 33.8% (26) | 52% (13) | 50% (7) | 37.5% (3) | 11.8% (2) | 22.2% (2) | |
| Good | 37.7% (29) | 36% (9) | 35.7% (5) | 50% (4) | 41.2% (7) | 77.8% (7) | |
| Very good | 9.1% (7) | 8% (2) | 0% (0) | 12.5% (1) | 29.4% (5) | 0% (0) | |
| Excellent | 3.9% (3) | 0% (0) | 0% (0) | 0% (0) | 5.9% (1) | 0% (0) | |
| Satisfaction level with knowledge about medical emergencies | - | - | - | - | - | - | - |
| Not at all satisfied | 20.3% (29) | 14.3% (5) | 25% (6) | 11.1% (1) | 5.6% (1) | 0% (0) | <0.001 * |
| Slightly satisfied | 40.6% (58) | 42.9% (15) | 45.8% (11) | 11.1% (1) | 5.6% (1) | 7.1% (1) | |
| Moderately satisfied | 30.8% (44) | 42.9% (15) | 25% (6) | 55.6% (5) | 50% (9) | 64.3% (9) | |
| Very satisfied | 7% (10) | 0% (0) | 4.2% (1) | 22.2% (2) | 27.8% (5) | 28.6% (4) | |
| Extremely satisfied | 1.4% (2) | 0% (0) | 0% (0) | 0% (0) | 11.1% (2) | 0% (0) | |
| Self-evaluation of the clinical competency in dealing with medical emergencies | - | - | - | - | - | - | <0.001 * |
| Poor | 18.9% (27) | 22.9% (8) | 25% (6) | 11.1% (1) | 5.6% (1) | 0% (0) | |
| Fair | 44.1% (63) | 45.7% (16) | 50% (12) | 33.3% (3) | 0% (0) | 35.7% (5) | |
| Good | 31.5% (45) | 28.6% (10) | 25% (6) | 33.3% (3) | 55.6% (10) | 35.7% (5) | |
| Very good | 4.9% (7) | 2.9% (1) | 0% (0) | 22.2% (2) | 22.2% (4) | 21.4% (3) | |
| Excellent | 0.7% (1) | 0% (0) | 0% (0) | 0% (0) | 16.7% (3) | 7.1% (1) | |
| Need for further training in the field of medical emergencies | 99.3% (142) | 100% (35) | 100% (24) | 88.9% (8) | 88.9% (16) | 92.9% (13) | 0.002 * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gazal, G.; Aljohani, H.; Al-Samadani, K.H.; Nassani, M.Z. Measuring the Level of Medical-Emergency-Related Knowledge among Senior Dental Students and Clinical Trainers. Int. J. Environ. Res. Public Health 2021, 18, 6889. https://doi.org/10.3390/ijerph18136889
Gazal G, Aljohani H, Al-Samadani KH, Nassani MZ. Measuring the Level of Medical-Emergency-Related Knowledge among Senior Dental Students and Clinical Trainers. International Journal of Environmental Research and Public Health. 2021; 18(13):6889. https://doi.org/10.3390/ijerph18136889
Chicago/Turabian StyleGazal, Giath, Hamzah Aljohani, Khalid H Al-Samadani, and Mohammad Zakaria Nassani. 2021. "Measuring the Level of Medical-Emergency-Related Knowledge among Senior Dental Students and Clinical Trainers" International Journal of Environmental Research and Public Health 18, no. 13: 6889. https://doi.org/10.3390/ijerph18136889
APA StyleGazal, G., Aljohani, H., Al-Samadani, K. H., & Nassani, M. Z. (2021). Measuring the Level of Medical-Emergency-Related Knowledge among Senior Dental Students and Clinical Trainers. International Journal of Environmental Research and Public Health, 18(13), 6889. https://doi.org/10.3390/ijerph18136889






