A Swiss Health Care Professionals’ Perspective on the Meaning of Interprofessional Collaboration in Health Care of People with MS—A Focus Group Study
Abstract
1. Introduction
- (a)
- What is the perspective of health care professionals regarding the meaning of IPC in comprehensive health care of PwMS?
- (b)
- How does experience with PwMS affect the health care professional’s IPC?
2. Materials and Methods
2.1. Study Design
2.2. Sampling and Participants
2.3. Data Collection
2.4. Data Analysis
2.5. Quality Assurance
3. Results
3.1. Sampling and Participants
3.2. Data Analysis
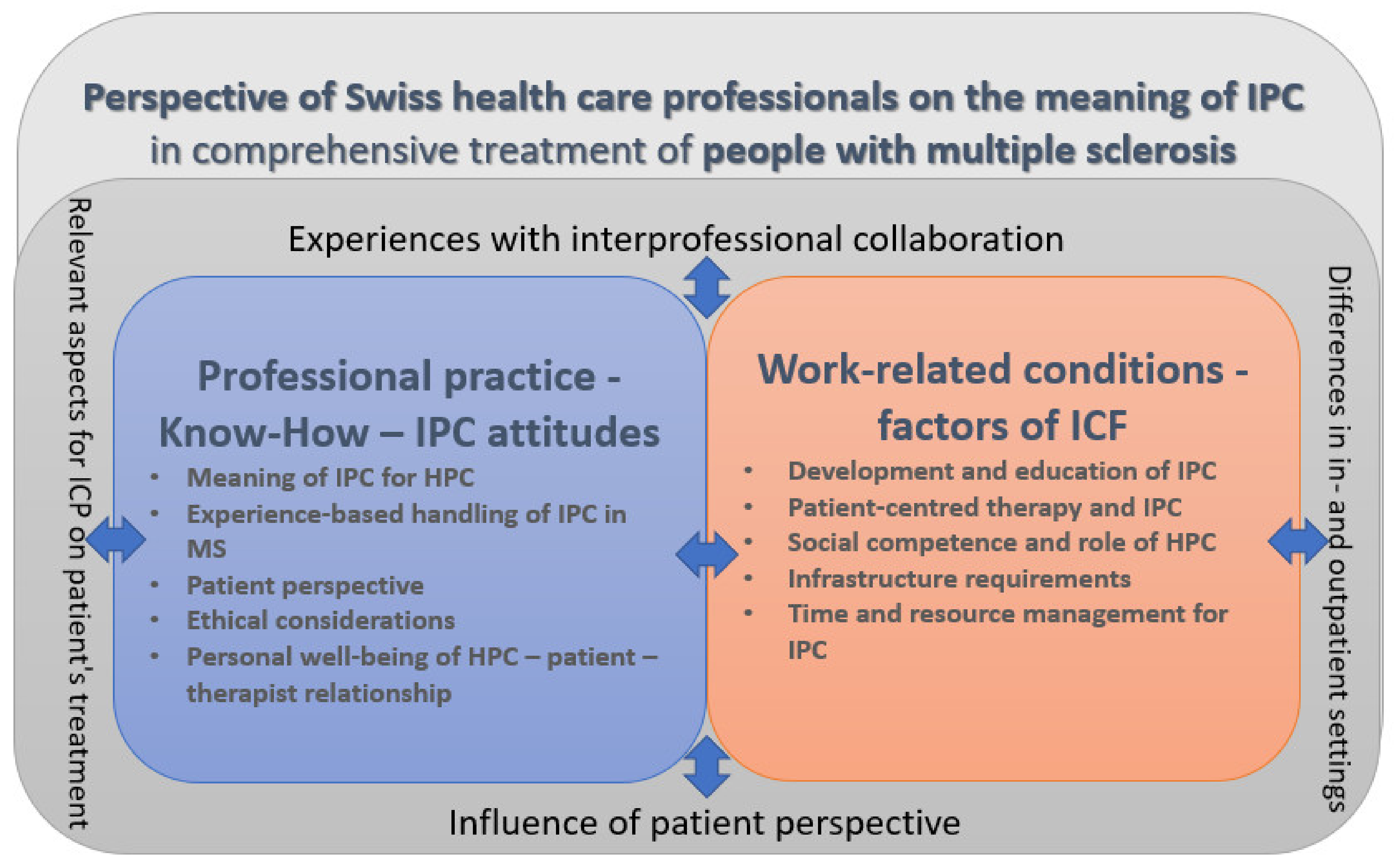
3.2.1. Professional Practice—Know-How—IPC Attitudes
Meaning of IPC for Health Care Professionals
«For me, interprofessional means pulling together on the same rope and if possible, being able to do inpatient work on the same goals in a discipline-specific way (--) and not sinking into parallel worlds where everyone works in a different direction». (FG03; 118)
«But the goal or the patient should actually be in the center. And the goal should be defined as realistically as possible. And, of course, we also need to talk to each other. But that’s what I understand by the definition of interprofessional cooperation». (FG01; 114)
«You also know who works a lot with PwMS, who can I ask, if this is not my subject. For example, if someone has breathing problems, I can ask this therapist». (FG01; 94)
«But we also have a holistic picture of our patients, it is not simply enough just to check out our own professional area. We are also always in contact with the physiotherapy, how far they can go. Because this also has a direct impact on patients’ leisure time and independence and daily routine». (FG02; 21)
Experience and Handling of IPC in MS
«I think it makes it a lot easier. IPC is important to look and see, maybe I have forgotten something. There are cognitive problems for example, and there are also other problems. And that’s where I see the importance of working together in addition to my own work». (FG03; 120)
«That you can only really work at its optimum if you work interprofessionally. And this fundamental attitude that I believe you have to learn to live». (FG01; 47).
«You have to be clear about what you say, so that the patients understand. That they can understand when you do a lot of therapy for three weeks, but no progress shows up». (FG02; 54)
«Then you quickly reach limits of what you can do in the conversation with the patient, for example, how can I tell him that now? These are special challenges. So, the topic of conversation somehow, how can I justify myself? ». (FG01; 74)
Patient Perspective
«Yes, patients see their own future». (FG02; 94) «That is another condition to live clearly in the context I am getting worse and worse, I have a chronic illness, what awaits me, even young people with family». (FG01;67)
«For example, during the first stay, if the therapist recommends a foot lifter splint, they say no and generally reject everything. And over time, during the second or third stay, they see that other PwMS are better off with the same aids and then they accept it. They profit very much from each other». (FG02;71)
«For example, we have a patient who drives her wheelchair with a self-made mouth stick when her hand gets tired». (FG02; 66)
«Yes, they have surprising coping skills, also to some extent self-destructive. How they deal with their problems». (FG02; 62)
«And there they come up with their own ideas and you reflect and think together. You can’t get such knowledge out of textbooks and reference books. For me, that has actually a lot of value as a therapist». (FG02; 66)
Ethical Considerations
«And with PwMS, it’s often the case that you don’t want to take anything away from them. So, you know, it’s probably already dangerous if he eats the peanuts now. But he loves them more than anything else and that would be a big incision for him now, if I said that he shouldn’t eat them anymore. And then what does this neuropsychological clarification mean? That would mean in three quarters of the cases that they can no longer drive». (FG01; 71-83)
«...but if you are not that aware of the cognitive limitations, you often ask the patient and think the patient does not want that. But often the patient can’t really estimate». (FG01; 79)
Personal Well-Being of Health Care Professionals/Patient–Therapist Relationship
«And then you feel very stupid. And I like to think I’m over 30 years old and he insults me like a little girl. I know how to react to it. I also see him as a patient who has a terrible illness, who can’t deal with it. His illness changes him, we just treat him, but yes. Maybe he will be nice someday». (FG02; 80)
«I am overwhelmed when a patient approaches me very negatively or very impudently. That is difficult for me. There I am.... I already have a few strategies, but if all this is useless to me, if I am only loaded, then I know that my therapy has absolutely no effect at that moment. And then I also take the liberty to stop it. Yes, I have to explain that to my colleagues afterwards». (FG02; 77)
3.2.2. Work-Related Conditions—Factors of IPC
Development and Education of IPC
«I can really see that in MS these are the pioneers of interprofessional cooperation». (FG01; 25)
«It has improved more and more over the last 10 to 15 years. It already starts with recording reports. All professions are present together and they are checking among each other what is the focus of this clinic stay. The therapy package will be put together accordingly. In the last two, three years, collaborations have become better, since we have a common team room.... On the other hand, when aids are needed or when positioning is required for the more severely affected patients, intensive collaboration is required. Or you make splints and we do the positioning together». (FG02; 18)
«For me, insights into job descriptions of the individual professionals are important. Because in recent years we have been able to gain insights from time to time. For example, we had a detailed explanation of how to swallow and how important that is. And if I have a good insight, I can put myself better into it. We had gotten further training; and mutually I know more about occupational therapy and speech therapy than if I didn’t work here. (FG02; 38)
Patient-Centered Therapy in IPC
«But I think the goal should be that the patient’s view of what he wants always comes first». That’s how you should put it. And then perhaps a therapeutic goal can result from it». (FG01; 123) (FG01; 123)
«The fact that the patient is also a component of this interprofessional team includes him as a partner». (FG01; 106)
«But it’s just like doing a balancing act to say that is what the patient wants to do, but that is what I want to work towards now, something different». (FG01; 128)
«These people also usually come into therapy with a very precise idea of what to do now, what the next step could be and what they need. And picking them up, what they imagine and at the same time being able to bring in the therapeutic expertise is a bit of a balancing act». (FG01;64)
Social Competence and the Role of the Health Care Professionals
«The one who sees a need addresses it». (FG03; 41) and «Communication is everything». (FG02; 107)
«...Should I do it now or will the SLTs do it? Regarding aids with communication devices, who does what? So simply that it does not run twice or that it will not get forgotten. There are both possibilities here». (FG01; 49).
«To make arrangements and to be able to withdraw. If necessary, to be able to withdraw and remember that I may not be the main person (therapeutic discipline) who has to contribute something». (FG01; 155)
« I also think that one can ask easily and admit oneself, when I need help». (FG01; 94)
«That you can also say, yes I step back now because the patient does not want my therapy. That you are also flexible with structures and hierarchies. That you have a level where you can really communicate with your team». (FG01; 118)
«I think this is very important, the emancipation from these old structures where the doctor was the leader who always knew everything. Which may be partly true, but often not, because it’s actually not possible to know everything in such complex settings». (FG01; 119)
«I think similarly, one must have an interest. I wonder what patients do in speech therapy, what their cognitive abilities are and what they do in physiotherapy. I need to have an interest. It always takes self-initiative» (FG02; 42)
«...and we read each other’s reports or then just go and ask or discuss when we have a concern». (FG03; 30)
Infrastructure Requirements
«What makes it easier is our process in the “Phoenix” system. We have made it very professional and now we have a sheet where all disciplines note their current state of therapy». (FG02; 92)
«Our infrastructure makes it easier to reach our destinations. Plus, that new ideas are implemented relatively quickly here. We therapists work door-to-door with each other, there is a lot of exchange». (FG02; 94)
«Or when we walk through a therapy room and see the colleagues from the physiotherapy treating the patient right now and we have a few minutes, then we observe briefly or can then use time for a brief exchange». (FG02; 22)
«Because the case with us in the outpatient clinic is that I have to consider whether I can find time for a phone call. I cannot charge this time as physiotherapy. And a lot of things that you normally wanted to contribute to quality just will be dropped and left away». (FG01; 110)
«You might be a bit more in your chamber and working on your own thing if you do it on external outpatient care. It rarely happens that I consult the responsible doctor for an outpatient patient». (FG03; 137; FG03; 158)
Time and Resource Management for IPC
«Yes, and I think the big difference for me is that there are also structures provided for this exchange in the inpatient sector». (FG03; 139)
«In the day clinic they take place every week, but each time different patients are discussed. Then one has 10 to 20 min time, where one discusses the patient with the interprofessional goals, agrees on these and names the main problems». (FG01; 45)
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Multiple Sclerosis. Who Gets MS? Multiple Sclerosis (MS) Better Questions Lead to Better Answers. 2021. Available online: https://www.multiplesclerosis.com/global/about_ms.php (accessed on 24 May 2021).
- Multiple Sklerose. Vorkommen. Schweizerische Multiple Sklerose Gesellschaft. 2021. Available online: https://www.multiplesklerose.ch/de/ueber-ms/multiple-sklerose/vorkommen/ (accessed on 24 May 2021).
- Calabresi, P.A. Diagnosis and management of multiple sclerosis. Am. Fam. Phys. 2004, 70, 1935–1944. [Google Scholar]
- Gimigliano, F.; Negrini, S. The World Health Organization “Rehabilitation 2030—A call for action”. Eur. J. Phys. Rehabil. Med. 2017, 53, 155–168. [Google Scholar] [CrossRef]
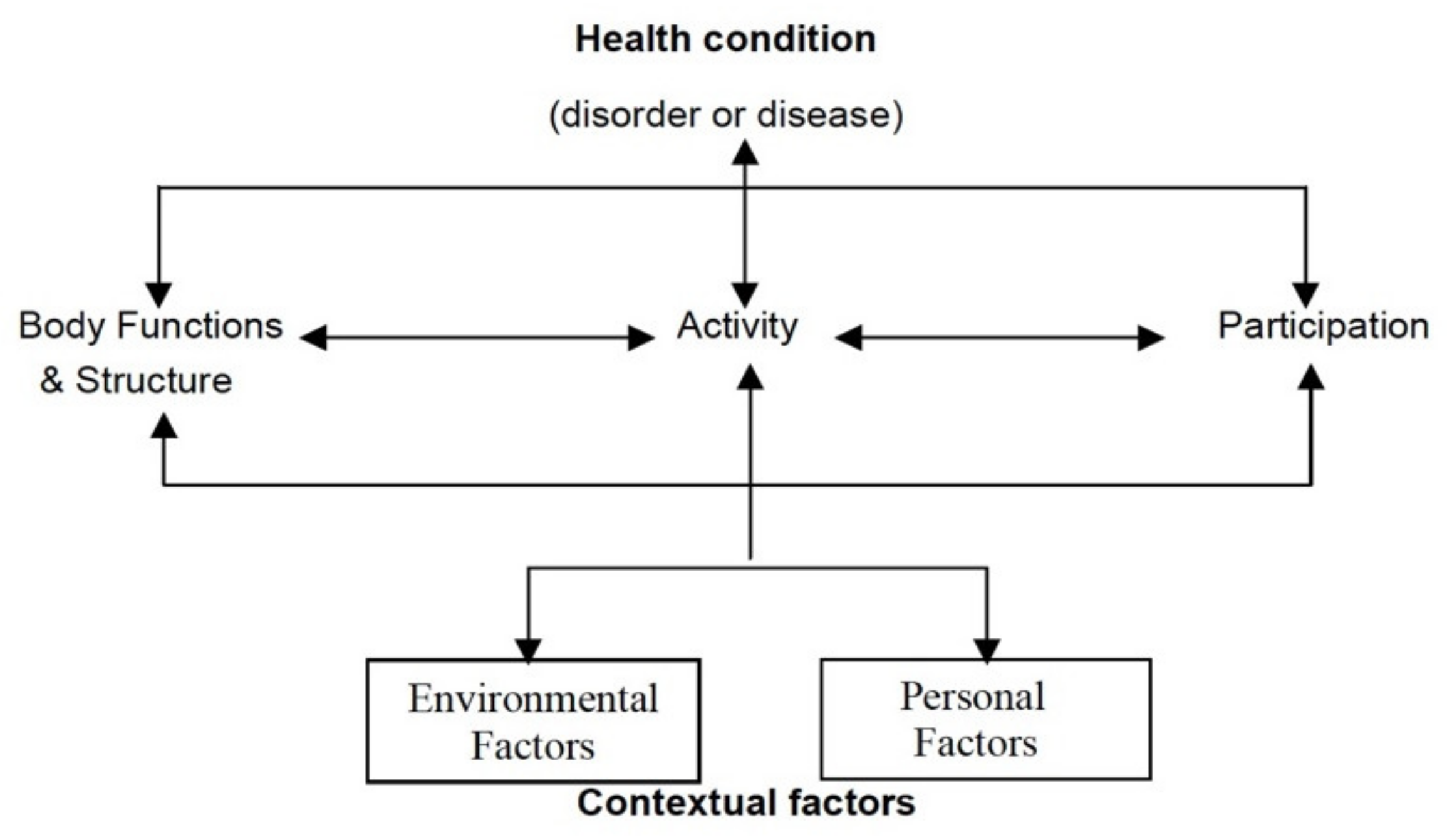
- World Health Towards a Common Language for Functioning, Disability, and Health: ICF. The Organization. International Classification of Functioning, Disability and Health. 2021. Available online: https://www.who.int/classifications/icf/en/ (accessed on 24 May 2021).
- Kostanjsek, N. Use of The International Classification of Functioning, Disability and Health (ICF) as a conceptual framework and common language for disability statistics and health information systems. BMC Public Health 2011, 11 (Suppl. 4), S3. [Google Scholar] [CrossRef] [PubMed]
- Van Bochove, B. Multiple Sclerosis—The Disease with a Thousand Faces. Commer. Ger. 2015, 13, 9. Available online: https://www.amcham.de/publications/commerce-germany/ (accessed on 24 May 2021).
- Reeves, S.; Lewin, S.; Espin, S.; Zwarenstein, M. Interprofessional Teamwork for Health and Social Care; Blackwell-Wiley: London, UK, 2010. [Google Scholar]
- World Health Organization. Interprofessional Collaboration Practice in Primary Health Care: Nursing and Mid-wifery Perspectives. Human Resources for health Observer (13). 2013. Available online: https://www.who.int/hrh/resources/observer13/en/ (accessed on 24 May 2021).
- Galushko, M.; Golla, H.; Strupp, J.; Karbach, U.; Kaiser, C.; Ernstmann, N.; Pfaff, H.; Ostgathe, C.; Voltz, R. Unmet Needs of Patients Feeling Severely Affected by Multiple Sclerosis in Germany: A Qualitative Study. J. Palliat. Med. 2014, 17, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Hepworth, M.; Harrison, J.; James, N. Information needs of people with multiple sclerosis and the implications for information provision based on a national UK survey. Aslib Proc. 2003, 55, 290–303. [Google Scholar] [CrossRef]
- Kantor, D.; Bright, J.R.; Burtchell, J. Perspectives from the Patient and the Healthcare Professional in Multiple Sclerosis: Social Media and Participatory Medicine. Neurol. Ther. 2018, 7, 37–49. [Google Scholar] [CrossRef]
- Kirk, S.; Hinton, D. “I’m not what I used to be”: A qualitative study exploring how young people experience being diagnosed with a chronic illness. Child Care Health Dev. 2019, 45, 216–226. [Google Scholar] [CrossRef]
- Somerset, M.; Campbell, R.; Sharp, D.J.; Peters, T. What do people with MS want and expect from health-care services? Health Expect. 2001, 4, 29–37. [Google Scholar] [CrossRef]
- Bainbridge, L.; Nasmith, L.; Orchard, C.; Wood, V. Competencies for Interprofessional Collaboration. J. Phys. Ther. Educ. 2010, 24, 6–11. [Google Scholar] [CrossRef]
- Delva, D.; Jamieson, M.; Lemieux, M. Team effectiveness in academic primary health care teams. J. Interprof. Care 2008, 22, 598–611. [Google Scholar] [CrossRef]
- Cameron, E.; Rog, D.; McDonnell, G.; Overell, J.; Pearson, O.; French, D.P. Factors influencing multiple sclerosis disease-modifying treatment prescribing decisions in the United Kingdom: A qualitative interview study. Mult. Scler. Relat. Disord. 2019, 27, 378–382. [Google Scholar] [CrossRef]
- Smith, C.M.; Hale, L.A.; Olson, K.; Baxter, G.D.; Schneiders, A.G. Healthcare provider beliefs about exercise and fatigue in people with multiple sclerosis. J. Rehabil. Res. Dev. 2013, 50, 733. [Google Scholar] [CrossRef]
- Turner, A.P.; Martin, C.; Williams, R.M.; Goudreau, K.; Bowen, J.D.; Hatzakis, M., Jr.; Whitham, R.H.; Bourdette, D.N.; Walker, L.; Haselkorn, J.K. Exploring educational needs of multiple sclerosis care providers: Results of a care-provider sur-vey. J. Rehabil. Res. Dev. 2006, 43, 25–34. [Google Scholar] [CrossRef]
- Upton, D.; Taylor, C. What Are the Support Needs of Men with Multiple Sclerosis, and Are They Being Met? Int. J. MS Care 2015, 17, 9–12. [Google Scholar] [CrossRef]
- Tong, A.; Sainsbury, P.; Craig, J. Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 2007, 19, 349–357. [Google Scholar] [CrossRef]
- Malterud, K. Systematic text condensation: A strategy for qualitative analysis. Scand. J. Public Health 2012, 40, 795–805. [Google Scholar] [CrossRef]
- Flick, U.; Kardorff, E.V.; Steinke, I. Qualitative Forschung, 12th ed.; Rowohlt: Reinbek, Germany, 2017. [Google Scholar]
- Robson, C. Real World Research: A Resource for Social Scientists and Practitioner—Researchers, 2nd ed.; Blackwell Publishing: Oxford, UK, 2002. [Google Scholar]
- World Medical Association. World Medical Association Declaration of Helsinki. Ethical principles for medical research involving human subjects. Bull. World Health Organ. 2001, 79, 373–374. [Google Scholar]
- McQuarrie, E.F.; Krueger, R.A. Focus Groups: A Practical Guide for Applied Research. J. Mark. Res. 1989, 26, 371. [Google Scholar] [CrossRef]
- Wechselwirkung auf die Versorgung von Berufszufriedenheit—Akademischer Erstqualifizierung und der Bedarfsentwicklung in der Ergotherapie. Available online: http://bdsl-ev.de/wp-content/uploads/2019/11/probst_bmg_14.11.2018.pdf (accessed on 16 June 2021).
- Merriam, S.B. Qualitative Research and Case Study Applications in Education. Revised and Expanded from “Case Study Research in Education”; Jossey-Bass: San Francisco, CA, USA, 1998. [Google Scholar]
- Dresing, T.; Pehl, T. Praxisbuch Interview, Transkription & Analyse. Anleitungen und Regelsysteme für Qualitativ For-Schende, 8th ed.; Eigenverlag: Marburg, Germany, 2018; Available online: https://www.audiotranskription.de/downloads#praxisbuch (accessed on 24 May 2021).
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Clarke, V.; Braun, V. Successful Qualitative Research: A Practical Guide for Beginners; Sage: London, UK, 2013. [Google Scholar]
- Beauchamp, T.; Childress, J. Principles of Biomedical Ethics, 7th ed.; University Press: Oxford, MO, USA, 2001. [Google Scholar] [CrossRef]
- Heesen, C.; Köpke, S.; Richter, T.; Kasper, J. Shared decision making and selfmanagement in multiple sclerosis—A consequence of evidence. J. Neurol. 2007, 254, II116–II121. [Google Scholar] [CrossRef] [PubMed]
- Tractenberg, R.E.; Garver, A.; Ljungberg, I.H.; Schladen, M.M.; Groah, S.L. Maintaining primacy of the patient perspective in the development of patient-centered patient reported outcomes. PLoS ONE 2017, 12, e0171114. [Google Scholar] [CrossRef] [PubMed]
- Cutler, S.; Morecroft, C.; Carey, P.; Kennedy, T. Are interprofessional healthcare teams meeting patient expectations? An exploration of the perceptions of patients and informal caregivers. J. Interprof. Care 2018, 33, 66–75. [Google Scholar] [CrossRef] [PubMed]
- Rothwell, P.M.; McDowell, Z.; Wong, C.K.; Dorman, P.J. Doctors and patients don’t agree: Cross sectional study of patients’ and doctors’ perceptions and assessments of disability in multiple sclerosis. BMJ 1997, 314, 1580. [Google Scholar] [CrossRef]
- James, T.A.; Page, J.S.; Sprague, J. Promoting interprofessional collaboration in oncology through a teamwork skills simulation programme. J. Interprof. Care 2016, 30, 1–3. [Google Scholar] [CrossRef]
- McLoughlin, C.; Patel, K.D.; O’Callaghan, T.; Reeves, S. The use of virtual communities of practice to improve interprofessional collaboration and education: Findings from an integrated review. J. Interprof. Care 2017, 32, 136–142. [Google Scholar] [CrossRef]
- Stakeholders’ Perspectives on Innovative Models of Interprofessional Collaboration in Community-Based Care. Available online: https://www.cnhw.ch/fileadmin/user_upload/Abstract_ID_2.pdf (accessed on 16 June 2021).
- Soklaridis, S.; Romano, N.; Fung, W.L.A.; Martimianakis, M.A.; Sargeant, J.; Chambers, J.; Wiljer, D.; Silver, I.; Fung, A.W.L. Where is the client/patient voice in interprofessional healthcare team assessments? Findings from a one-day forum. J. Interprof. Care 2016, 31, 1–3. [Google Scholar] [CrossRef]
- Howe, A. Can the patient be on our team? An operational approach to patient involvement in interprofessional approaches to safe care. J. Interprof. Care 2006, 20, 527–534. [Google Scholar] [CrossRef]
- Goretti, B.; Portaccio, E.; Zipoli, V.; Hakiki, B.; Siracusa, G.; Sorbi, S.; Amato, M.P. Coping strategies, psychological variables and their relationship with quality of life in multiple sclerosis. Neurol. Sci. 2009, 30, 15–20. [Google Scholar] [CrossRef]
- McCabe, M.P.; McKern, S.; McDonald, E. Coping and psychological adjustment among people with multiple sclerosis. J. Psychosom. Res. 2004, 56, 355–361. [Google Scholar] [CrossRef]
- FOPH. Förderprogramm Interprofessionalität im Gesundheitswesen 2017–2020. 2018. Available online: https://www.bag.admin.ch/bag/de/home/strategie-und-politik/nationale-gesundheitspolitik/foerderprogramme-der-fachkraefteinitiative-plus/foerderprogramme-interprofessionalitaet.html (accessed on 24 May 2021).
- FOPH. Policy Briefs—Findings and Recommendations for Target Group-Specific Implementation. 2021. Available online: https://www.bag.admin.ch/bag/de/home/strategie-und-politik/nationale-gesundheitspolitik/foerderprogramme-der-fachkraefteinitiative-plus/foerderprogramme-interprofessionalitaet/policy-briefs-interprof.html#704340575 (accessed on 24 May 2021).
| Question Order | Questions of Focus Groups Interview Guide |
|---|---|
| A | What experiences have you had with interprofessional cooperation (IPC) in the treatment of patients (positive and negative)? Possible stimulus question: - What do you understand by interprofessional cooperation? |
| B | What positive and/or negative aspects do you consider relevant from your perspective as a therapist for interprofessional treatment of PwMS? Possible stimulus questions: - What is your experience with patients with MS compared to other patients? - What obstacles/challenges can you describe in terms of comprehensive treatment as a therapist in treating patients with MS? - What aspects do you think facilitate/hinder IPC in your work with patients with MS? - What role do you think the patient perspective plays for IPC? - What are the advantages/disadvantages of IPC in your opinion? - What experience do you have with regard to training in IPC? |
| C | Do you think there are differences in IPC (knowledge and application) in inpatient and outpatient care? Possible stimulus questions: - Are there any professional groups with whom more IPC takes place? - What opportunities and challenges can you see for IPC in the provision of health care for people with MS? - What are you personally doing to achieve better IPC? - In your opinion, is IPC demanded and necessary, or superfluous for MS patients? |
| D | How do your experiences with PwMS influence the IPC of different health professionals? |
| E | Do you have additional aspects which are relevant from your perspective to add to IPC? |
| Phases 1–6: | Tasks of Thematic Analysis of Focus Groups |
|---|---|
| Phase 1: Familiarsing yourself with your data: | At the beginning, all transcripts were read and initial ideas were written down. |
| Phase 2: Generating initial codes: | Text passages were extracted from all three focus groups and provided with codes that were relevant for the research questions. This coding was inductive, and data controlled. Transcripts of all three groups were independently coded by a second researcher (AG) to improve research rigor. Created codes were compared and discussed by the research team (FS and AG). After coding all three focus groups, one researcher (FS) went through all coded transcripts again for reviewing and competition. Ideas and thoughts relating to every code were written down in memos. After a reviewing evaluation all statements were condensed to one code. |
| Phase 3: Searching themes: | Codes were collected to identify potential themes. For this, the written memos were used. |
| Phase 4: Reviewing themes: | The created themes and the associated codes were checked. Memo function was again used to refine definitions of the themes. |
| Phase 5: Defining and naming themes: | Themes were checked again and then divided into sets based on the questions. |
| Phase 6: Producing the report: | The individual sets were assigned to categories. A visual representation was carried out of code, topic, and sets. |
| Demographics | Number of Participants | |
|---|---|---|
| Age | 20–30 years 31–40 years 41–50 years 51–60 years No details | 2 5 4 1 1 |
| Gender | Male Female | 1 12 |
| Profession | Physiotherapy Occupational Therapy Speech and Language Therapy | 6 4 3 |
| Work field | Outpatient setting Inpatient setting both | 1 5 7 |
| Work experience with PwMS | <1 year 1–2 years 5–10 years 10–20 years >20 years | 0 1 7 4 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schmid, F.; Rogan, S.; Glässel, A. A Swiss Health Care Professionals’ Perspective on the Meaning of Interprofessional Collaboration in Health Care of People with MS—A Focus Group Study. Int. J. Environ. Res. Public Health 2021, 18, 6537. https://doi.org/10.3390/ijerph18126537
Schmid F, Rogan S, Glässel A. A Swiss Health Care Professionals’ Perspective on the Meaning of Interprofessional Collaboration in Health Care of People with MS—A Focus Group Study. International Journal of Environmental Research and Public Health. 2021; 18(12):6537. https://doi.org/10.3390/ijerph18126537
Chicago/Turabian StyleSchmid, Fabienne, Slavko Rogan, and Andrea Glässel. 2021. "A Swiss Health Care Professionals’ Perspective on the Meaning of Interprofessional Collaboration in Health Care of People with MS—A Focus Group Study" International Journal of Environmental Research and Public Health 18, no. 12: 6537. https://doi.org/10.3390/ijerph18126537
APA StyleSchmid, F., Rogan, S., & Glässel, A. (2021). A Swiss Health Care Professionals’ Perspective on the Meaning of Interprofessional Collaboration in Health Care of People with MS—A Focus Group Study. International Journal of Environmental Research and Public Health, 18(12), 6537. https://doi.org/10.3390/ijerph18126537







