Evaluation of the Complementary Health Provision of the Podiatric Foot Care Program for Diabetic Patients in Catalonia (Spain)
Abstract
1. Introduction
2. Materials and Methods
2.1. Study
2.2. Participants
2.3. Procedure
2.4. Statistical Analysis
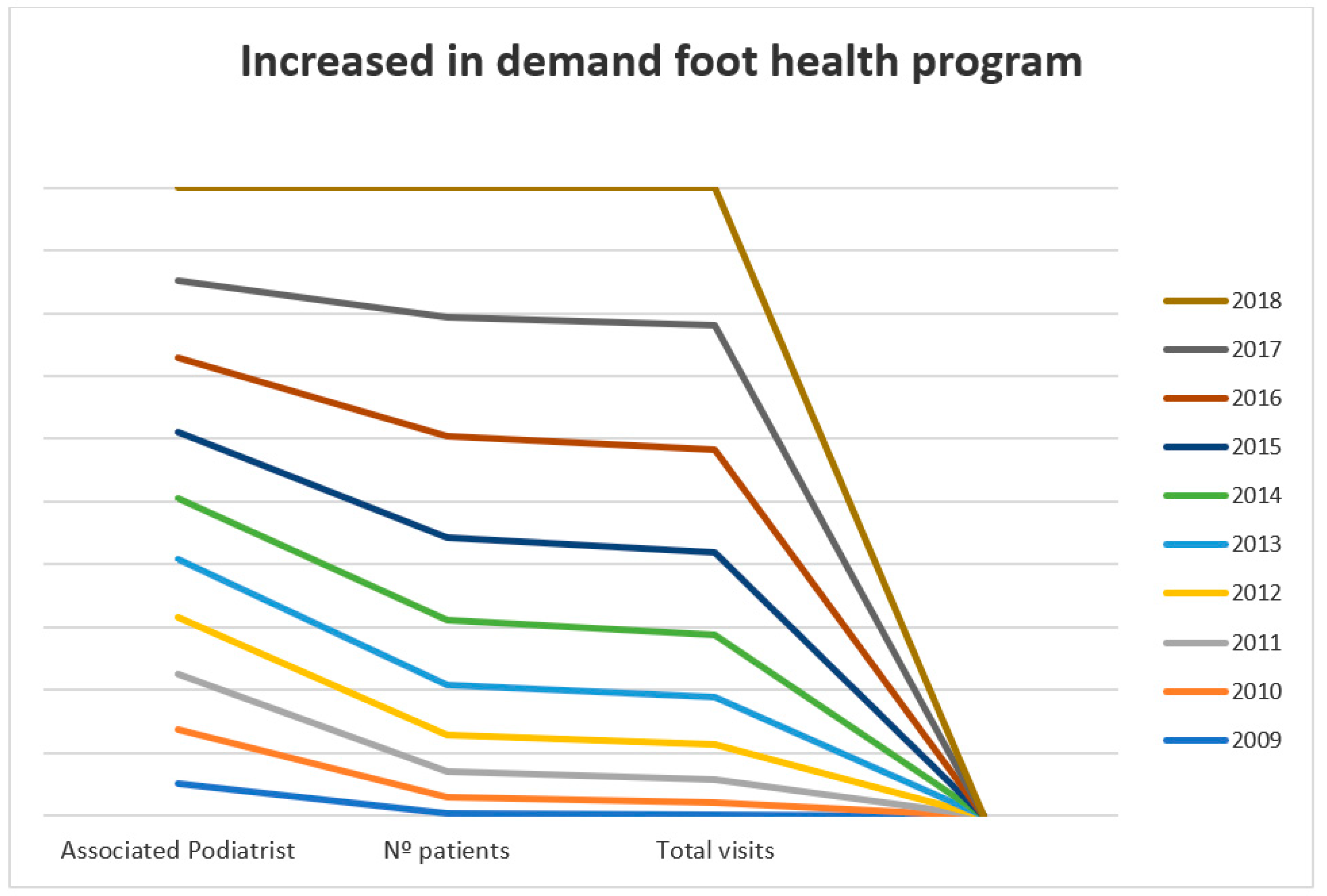
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- International Diabetes Federation (IDF). 2015. Available online: https://www.diabetesatlas.org/upload/resources/material/20200302_133352_2406-IDF-ATLAS-SPAN-BOOK.pdf (accessed on 15 March 2021).
- Ministerio de Sanidad, Servicios Sociales e Igualdad. Estrategia en Diabetes del Sistema Nacional de Salud. 2012. Available online: https://www.mscbs.gob.es/organizacion/sns/planCalidadSNS/pdf/excelencia/cuidadospaliativos-diabetes/DIABETES/Estrategia_en_diabetes_del_SNS_Accesible.pdf (accessed on 24 April 2021).
- Official Journal of Catalonia (DOGC). 2009. Available online: https://sid.usal.es/idocs/F3/LYN13831/13831.pdf (accessed on 24 April 2021).
- Costa, B.; Mestre, S.; Barrio, F.; Cabré, J.; Cos, X.; Aguilar, S.; Solé, C.; Castell, C.; Arija, V.; Lindström, J.; et al. Implantación del proyecto DP-TRANSFERS en Cataluña: Un método traslacional para mejorar el cribado y la prevención de la diabetes en atención primaria. PLoS ONE 2018, 13, 3. [Google Scholar]
- Rubeaan, K.; Al Derwish, M.; Ouizi, S.; Amira, Y.; Shazia, S.; Ibrahim, H.; Alamri, B.M. Diabetic Foot Complications and Their Risk Factors from a Large Retrospective Cohort Study. PLoS ONE 2015, 10, 1–17. [Google Scholar] [CrossRef]
- Bakker, K.; Apelqvist, J.; Schaper, N.C. International Working Group on Diabetic Foot Editorial Board. Practical guidelines on the management and prevention of the diabetic foot 2011. Diabetes Metab. Res. Rev. 2012, 28, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Jurado, J.; Zabaleta, E.; Farré, C.; Barcelon, J.; Juvinya, D. Recursos y modelos de atención al pie diabético en Cataluña (España): Estudio descriptivo sobre espacios de mejora. Aten Primaria 2012, 44, 394–401. [Google Scholar] [CrossRef] [PubMed]
- Nadal, J.; Mediavilla, J.; Mata, M.; Mauricio, D.; Asencio, D.; Sarroca, J. Prevalencia y control de la diabetes mellitus tipo 2 entre los médicos de Atención Primaria de España. Estudio PRISMA. Endocrinol. Diabetes Nutr. 2017, 64, 265–271. [Google Scholar] [CrossRef] [PubMed]
- Barshes, N.; Sigireddi, M.; Wrobel, J.; Mahankali, A.; Robbins, J.M.; Kougias, P.; Armstrong, D.G. The system of care for the diabetic foot: Objectives, outcomes, and opportunities. Diabet. Foot Ankle 2013, 4, 1. [Google Scholar] [CrossRef] [PubMed]
- Leone, S.; Pascale, R.; Vitale, M.; Esposito, S. Epidemiology of Diabetic Foot. Infez. Med. 2012, 20, 8–13. Available online: https://www.ncbi.nlm.nih.gov/pubmed/22982692 (accessed on 15 September 2020). [PubMed]
- Amin, N.; Doupis, J. Diabetic foot disease: From the evaluation of the “foot at risk” to the novel diabetic ulcer treatment modalities. World J. Diabetes 2016, 10, 153–164. [Google Scholar] [CrossRef] [PubMed]
- Amstrong, D.; Cohen, K.; Courric, S.; Bharara, M.; Marston, W. Diabetic foot ulcers and vascular insufficiency our population has changed, vu tour methods have not. J. Diabetes Sci. Technol. 2011, 52, 1591–1595. [Google Scholar] [CrossRef] [PubMed]
- Martín, P.; Martínez, M.A.; García, J.M. Documento de posicionamiento sobre la eficiencia de las tecnologías aplicadas al manejo de la diabetes. Av. Diabetol. 2014, 30, 131–149. [Google Scholar] [CrossRef]
- Goicoechea, P.; Cabrera, N.; Artaza, H.; Suárez, M. Need for re-amputation and the clinical characteristics of reamputated diabetic patients. Rev. Cuba. Angiol. Cirugía Vasc. 2013, 14, 1. [Google Scholar]
- García, A.; Alonso, J.; Toledo, N.; Alonso, R.; Pulfer, M.; Cano, J.; García, M. D-005-Pie diabético y amputación: Factores asociados a esta grave complicación. Rev. Clin. Esp. 2020, 220, 129. [Google Scholar]
- Blanchette, V.; Brousseau, M.; Cloutier, L. Effect of contact with podiatry in a team approach context on diabetic foot ulcer and lower extremity amputation: Systematic review and meta-analysis. J. Foot Ankle Res. 2020, 13, 15. [Google Scholar] [CrossRef] [PubMed]
- Khan, Y.; Khan, M.; Raza, M. Diabetic foot ulcers: A review of current management. Int. J. Res. Med. Sci. 2017, 5, 4683–4689. [Google Scholar] [CrossRef]
- Resultats de L’enquesta de Salut de Catalunya (ESCA). Available online: http://salutweb.gencat.cat/ca/el_departament/estadistiques_sanitaries/enquestes/esca/resultats_enquesta_salut_catalunya/ (accessed on 5 March 2021).
- Official Journal of Catalonia (DOGC). 2009. Available online: https://catsalut.gencat.cat/web/.content/minisite/catsalut/ciutadania/serveis_atencio_salut/quins_serveis_ofereix_catsalut/prestacions-complementaries/criteris-atencio-podologica.pdf (accessed on 10 January 2017).
- Wu, S.; Driver, V.; Wrobel, J.; Armstrong, D. Foot ulcers in the diabetic patient, prevention and treatment. Vasc. Health Risk Manag. 2007, 3, 65–76. [Google Scholar] [PubMed]
- Blanchette, V.; Hains, S.; Cloutier, L. Establishing a multidisciplinary partnership integrating podiatric care into the Quebec public health-care system to improve diabetic foot outcomes: A retrospective cohort. Foot 2019, 38, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Pérez, A.; Edo, M.; Cañas, E.; Pablos, O.; Rios, J.M.; Verdazco, J.; Santamaria, A. Diagnostic and therapeutic guide of the SEMCPT for diabetic foot complications (1.st part). Rev. Pie Tobillo 2020, 34, 145–158. [Google Scholar]
- Estévez, A.; García, Y.; Licea, M.; Alfonso, A.; Álvarez, H. Identificación de las deformidades podálicas en personas con diabetes mellitus, una estrategia para prevenir amputaciones. Rev. Cubana Endocrinol. 2013, 24, 297–313. [Google Scholar]
- Cardiovascular Disease and Diabetes: Policies for Better Health and Quality of Care @OECD. 2015. Available online: https://www.oecd.org/israel/Cardiovascular-Disease-and-Diabetes-Policies-for-Better-Health-and-Quality-of-Care-Israel.pdf (accessed on 15 March 2021).
- Joret, M.O.; Osman, K.; Dean, A.; Cao, C.; van der Werf, B.; Bhamidipaty, V. Multidisciplinary clinics reduce treatment costs and improve patient outcomes in diabetic foot disease. J. Vasc. Surg. 2019, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Viadé, J. The role of the chiropodist in the care of diabetic foot. Angiología 2015, 67, 483–487. [Google Scholar] [CrossRef]
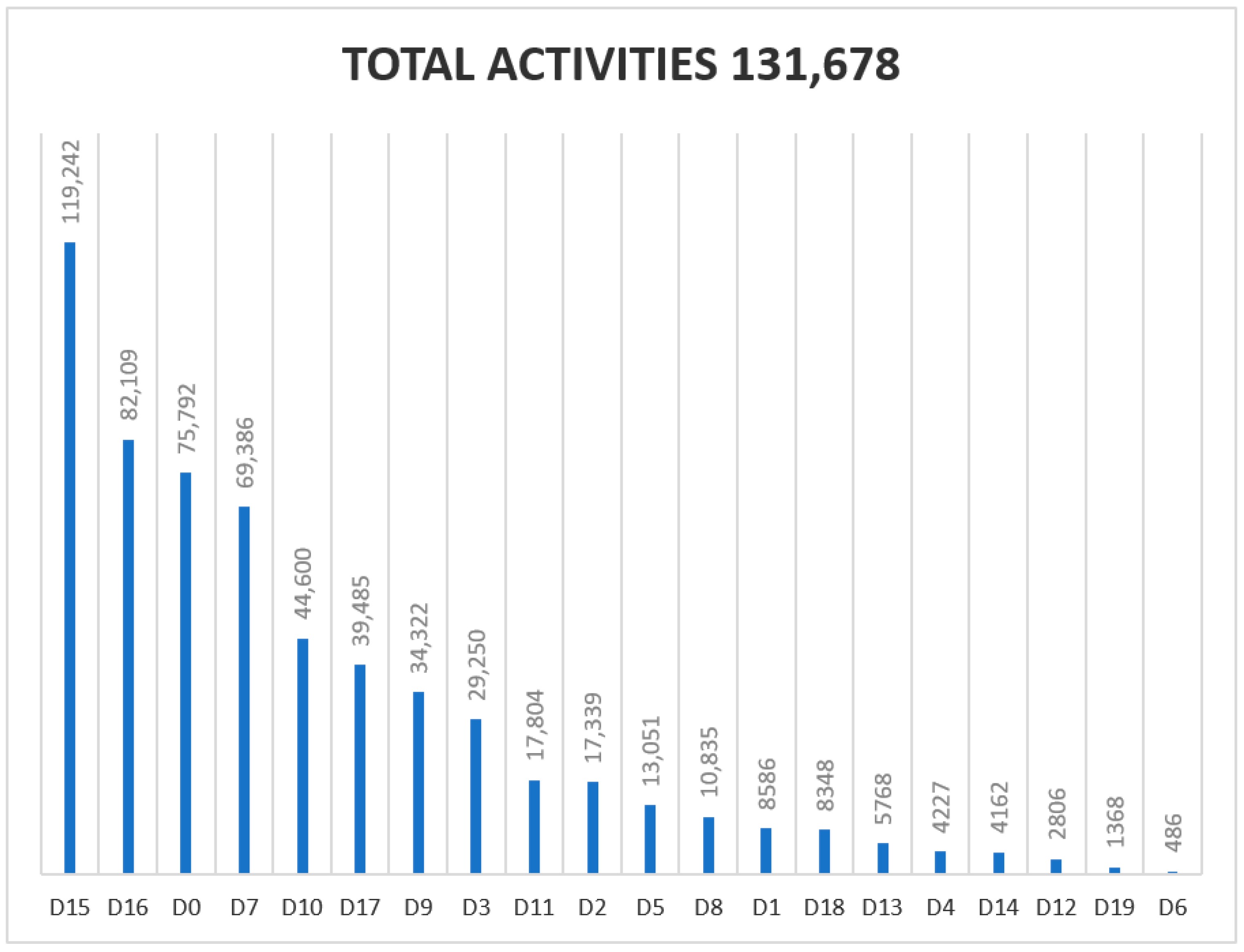

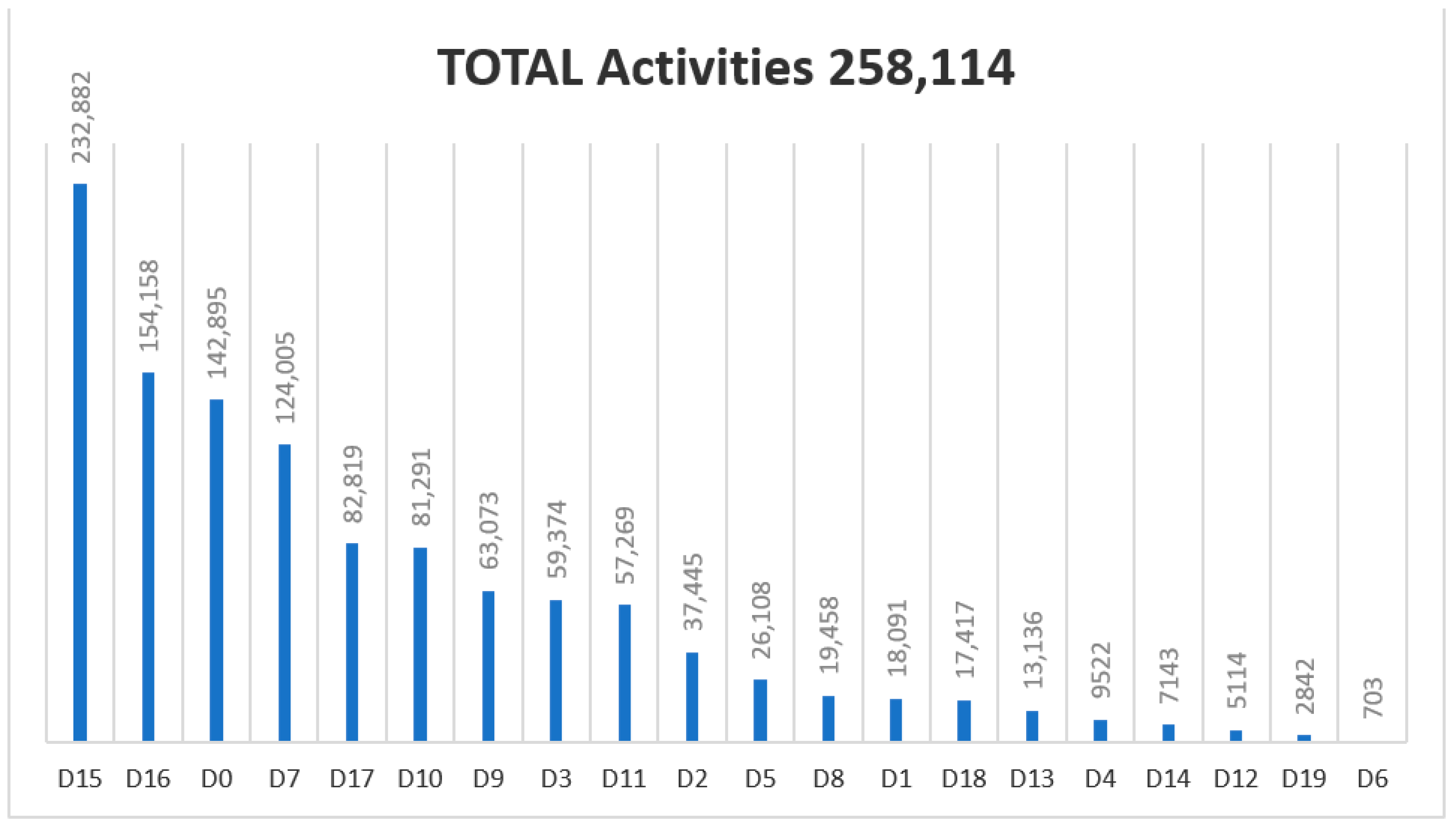

| List of Diagnosis Codes |
|---|
| 1—Diagnosis (Assessment of structural alterations in the foot) |
| D0_ No sensory alterations |
| D1_Flat foot |
| D2_ Foot dig |
| D3_ Digital deformity |
| D4_ Hindfoot alterations |
| D5_ Biomechanical alteration |
| 2—Control and treatment of keratotic and nail lesions |
| D6—Wart |
| D7—Keratopathies |
| D8—Fang infections |
| D9—Onychocryptosis |
| D10—Onychogryphosis |
| D11—Sensory alteration |
| 3—Control and treatment of grade 1 lesions (superficial) ITB index> 0.7 |
| D12—Presence and healing of ulcer |
| D13—Heel cracks |
| D14—Erosions and vesicles |
| D15—Without sensory alteration |
| 4.Diabetic foot assessment (neuropathic and vascular) |
| D16—Grade 0: Without neuropathic, vascular or structural and biomechanical alteration of the foot |
| D17—Grade 1: One present alteration (neuropathic, vascular or structural of the foot) |
| D18—Grade 2: Two alterations (neuropathic, vascular or small structural) |
| D19—Grade 3: Three alterations present (neuropathic, vascular or small structural) |
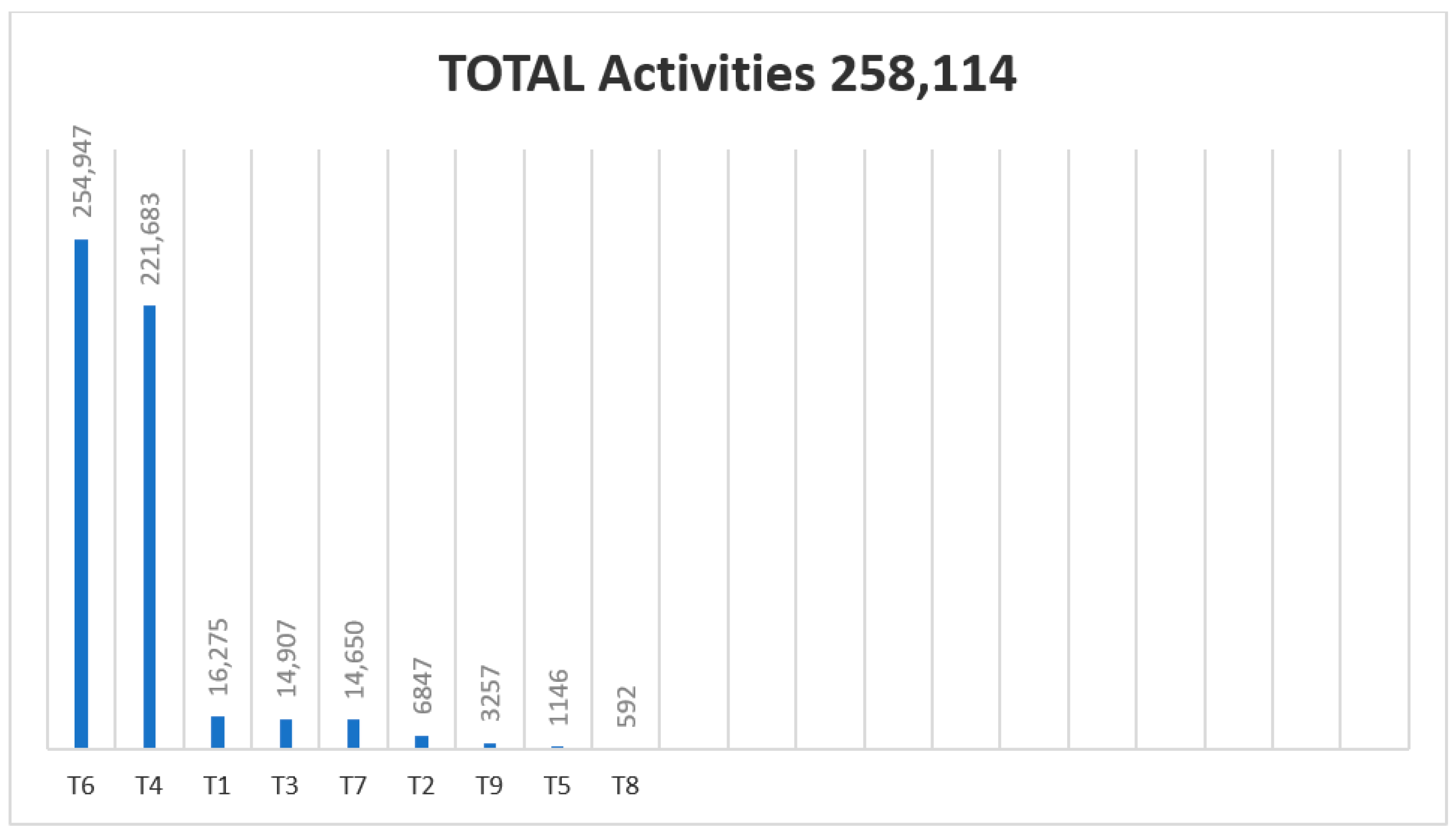
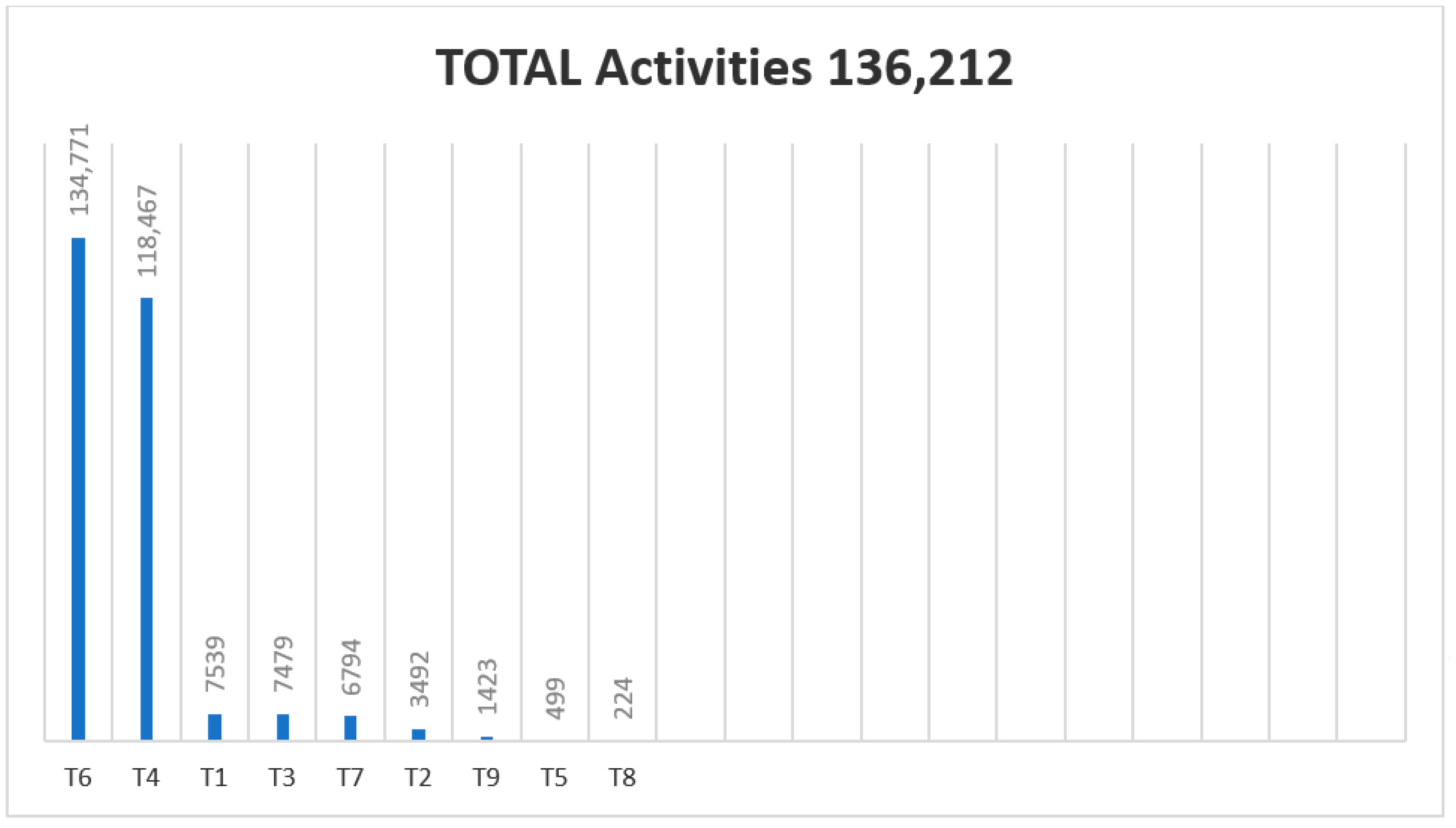
| List of Treatment codes |
| 1.Proposed ortho-podiatric |
| T1—Plantar supports |
| T2—Silicone orthosis |
| T3—Provisional descriptions |
| T4—Without treatment |
| T5—Prosthesis |
| 2.Control and treatment of keratotic and nail lesions |
| T6—Conservative TTO (Podiatry) |
| T7—Pharmacological |
| TTO |
| T8—Surgical TTO |
| T9—Referral to a specialist |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ruiz-Toledo, J.; Zalacain-Vicuña, A.J.; de Planell-Mas, E. Evaluation of the Complementary Health Provision of the Podiatric Foot Care Program for Diabetic Patients in Catalonia (Spain). Int. J. Environ. Res. Public Health 2021, 18, 5093. https://doi.org/10.3390/ijerph18105093
Ruiz-Toledo J, Zalacain-Vicuña AJ, de Planell-Mas E. Evaluation of the Complementary Health Provision of the Podiatric Foot Care Program for Diabetic Patients in Catalonia (Spain). International Journal of Environmental Research and Public Health. 2021; 18(10):5093. https://doi.org/10.3390/ijerph18105093
Chicago/Turabian StyleRuiz-Toledo, Jessica, Antonio J. Zalacain-Vicuña, and Elena de Planell-Mas. 2021. "Evaluation of the Complementary Health Provision of the Podiatric Foot Care Program for Diabetic Patients in Catalonia (Spain)" International Journal of Environmental Research and Public Health 18, no. 10: 5093. https://doi.org/10.3390/ijerph18105093
APA StyleRuiz-Toledo, J., Zalacain-Vicuña, A. J., & de Planell-Mas, E. (2021). Evaluation of the Complementary Health Provision of the Podiatric Foot Care Program for Diabetic Patients in Catalonia (Spain). International Journal of Environmental Research and Public Health, 18(10), 5093. https://doi.org/10.3390/ijerph18105093






