Fruit and Vegetable Intake and All-Cause Mortality in a Chinese Population: The China Health and Nutrition Survey
Abstract
1. Introduction
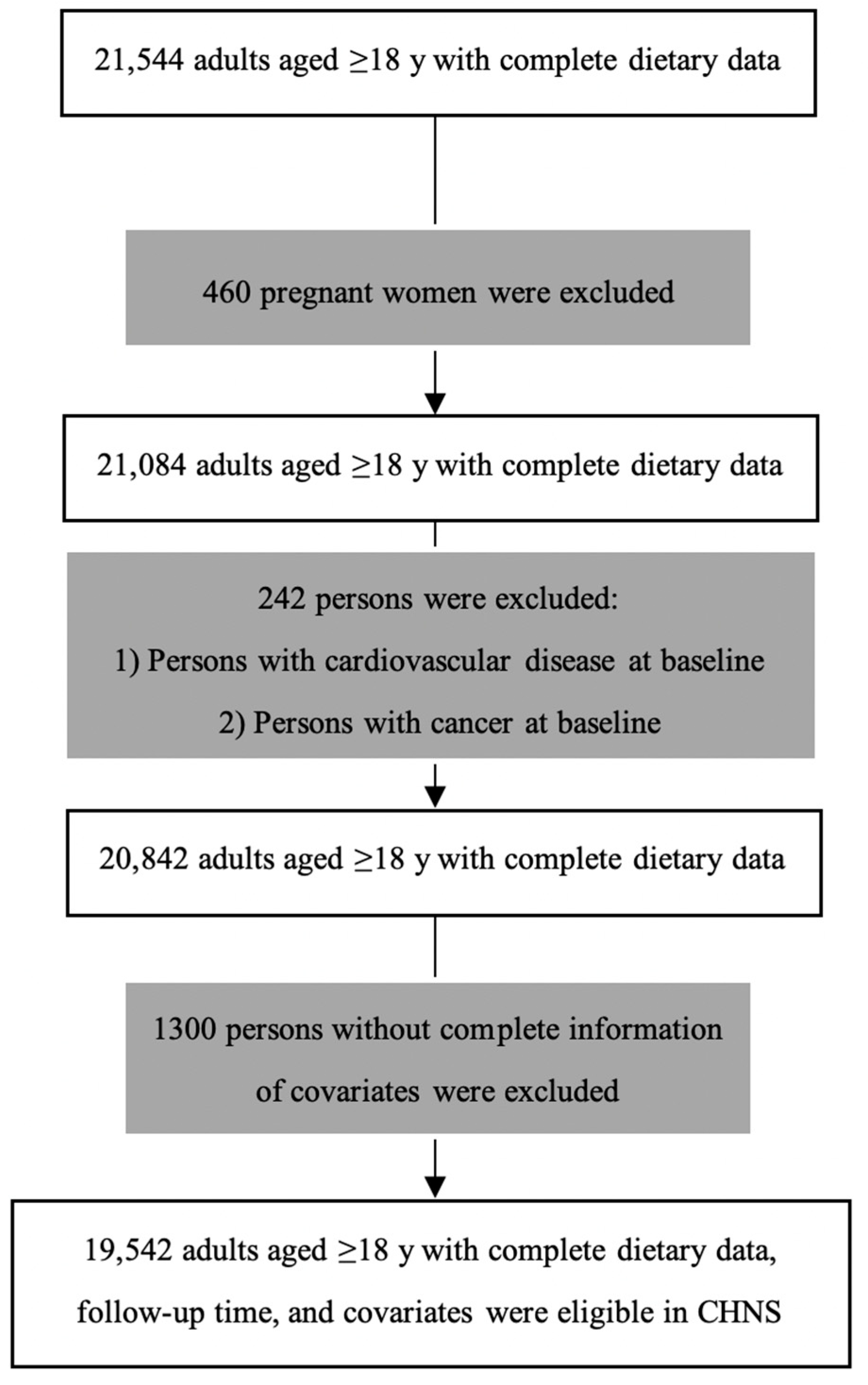
2. Methods
2.1. Data Source
2.2. Measurement
2.2.1. Exposure
2.2.2. Outcome
2.2.3. Covariates
2.3. Statistical Analysis
3. Results
3.1. Participants’ Characteristics
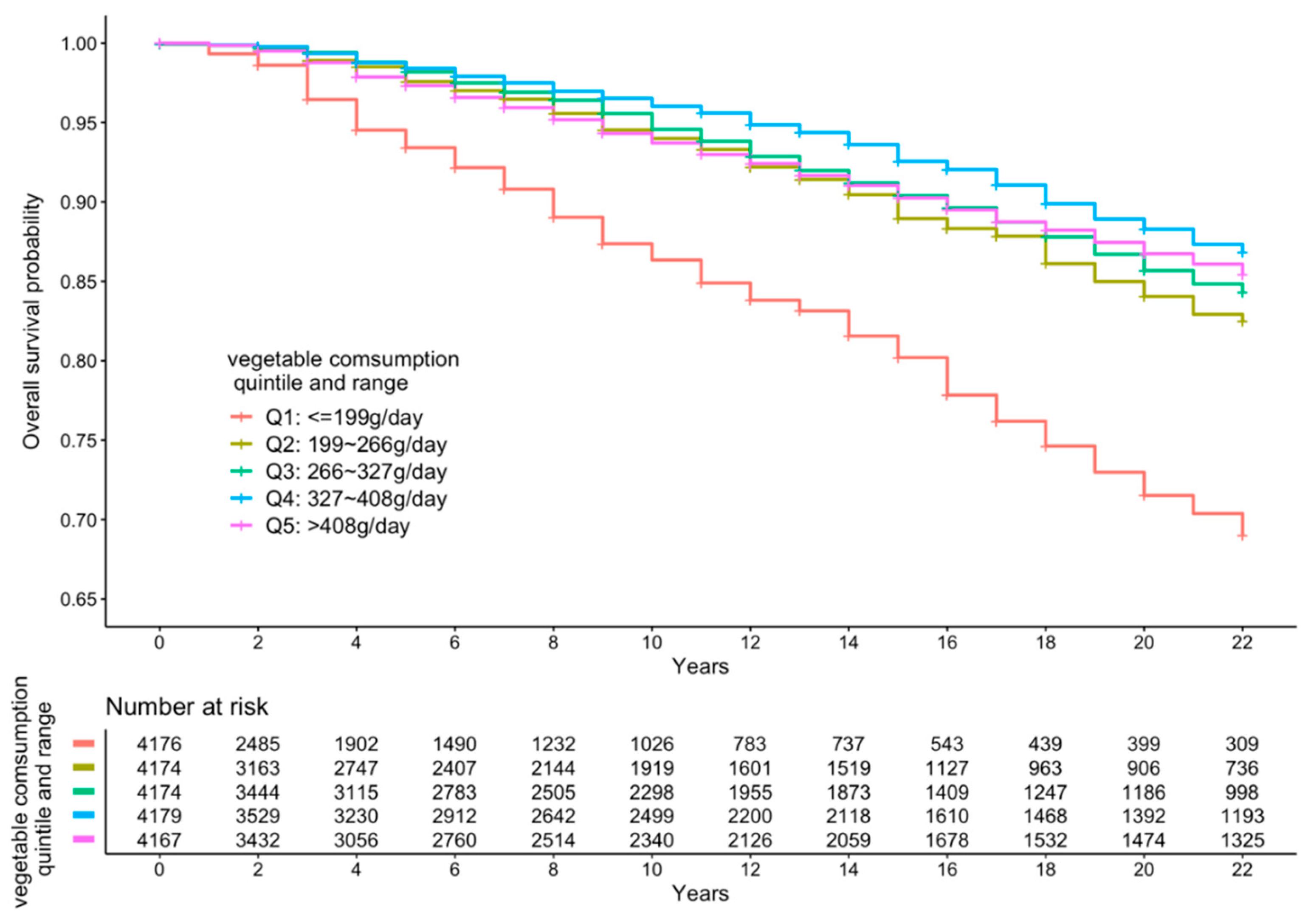
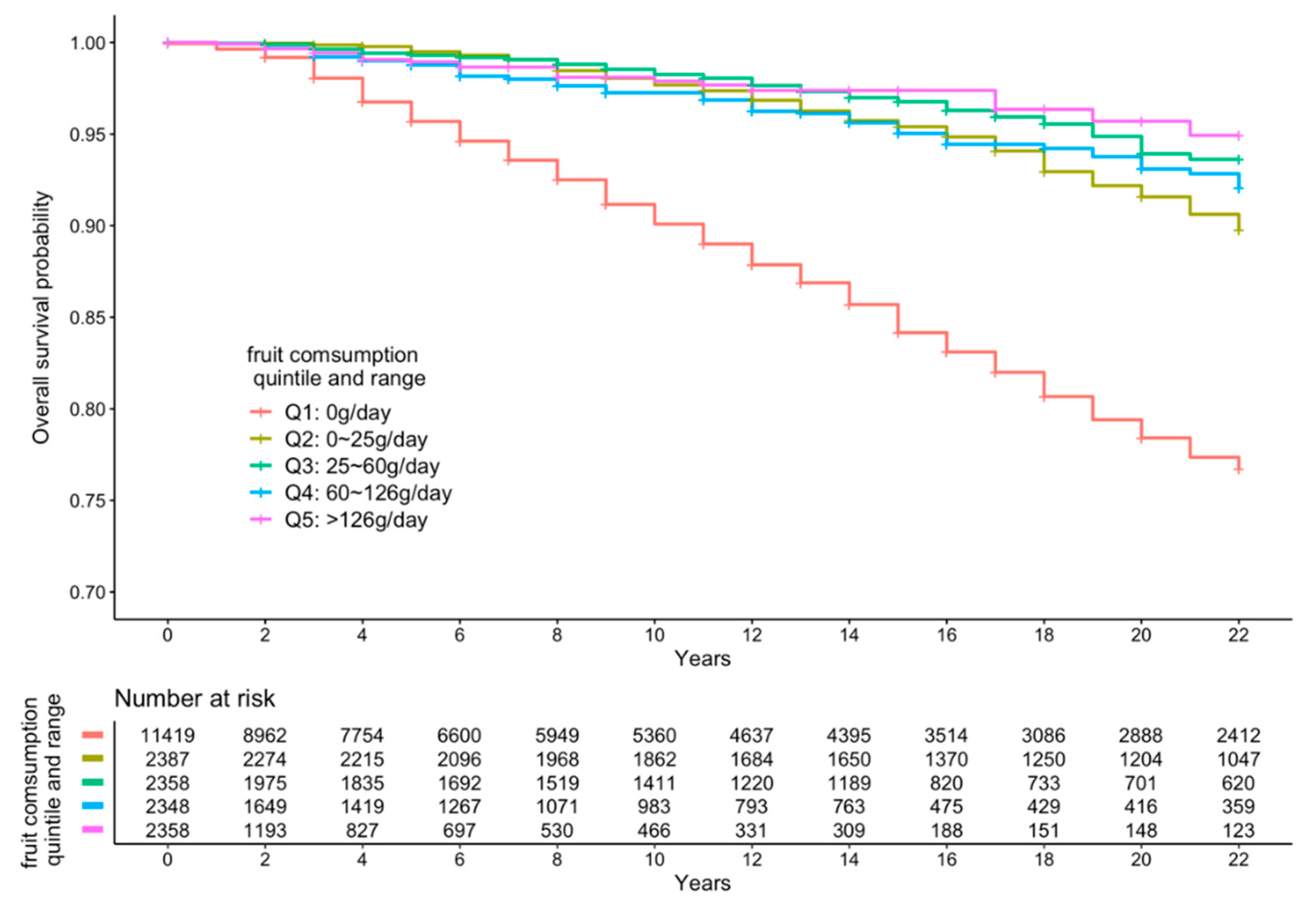
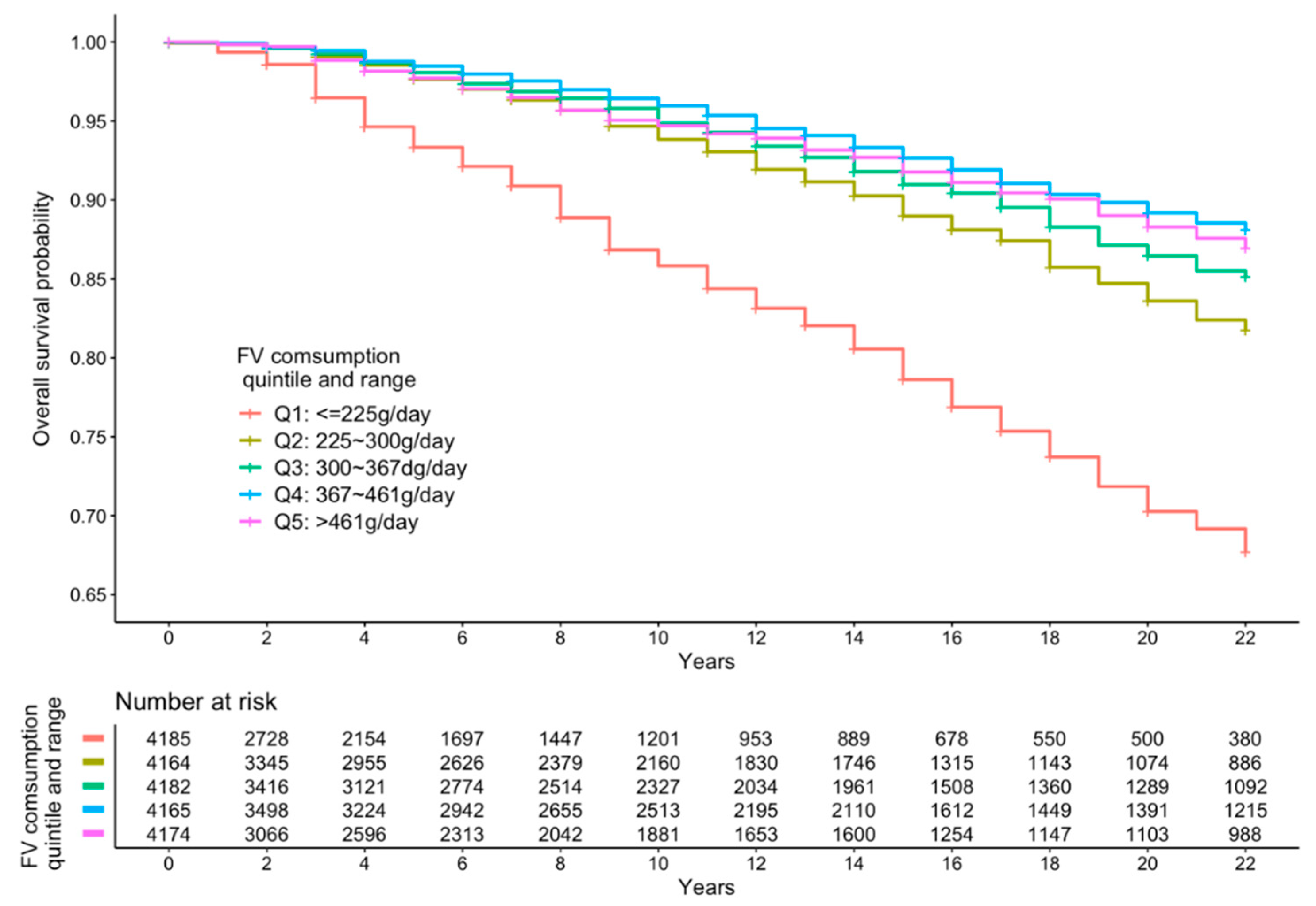
3.2. FV Intake and All-Cause Mortality
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dhandevi, P.; Jeewon, R. Fruit and vegetable intake: Benefits and progress of nutrition education interventions-narrative review article. Iran. J. Public Health 2015, 44, 1309. [Google Scholar]
- Li, X.-T.; Liao, W.; Yu, H.-J.; Liu, M.-W.; Yuan, S.; Tang, B.-W.; Yang, X.-H.; Song, Y.; Huang, Y.; Cheng, S.-L.; et al. Combined effects of fruit and vegetables intake and physical activity on the risk of metabolic syndrome among Chinese adults. PLoS ONE 2017, 12, e0188533. [Google Scholar] [CrossRef] [PubMed]
- Xiao, H.-J.; Liang, H.; Wang, J.-B.; Huang, C.-Y.; Wei, W.-Q.; Boniol, M.; Qiao, Y.-L.; Boffetta, P. Attributable causes of cancer in China: Fruit and vegetable. Chin. J. Cancer Res. 2011, 23, 171–176. [Google Scholar] [CrossRef][Green Version]
- Yang, Y. Expert Interpretation-New Dietary Guidelines (3) Eat More Fruits and Vegetables, Milk, Soybeans. Available online: http://dg.cnsoc.org/article/04/8a2389fd575f695101577a3abfdd02d7.html (accessed on 10 August 2019).
- Zhao, L.; Fang, Y.; He, Y.; Yu, D.; Guo, Q.; Yu, W.; Zhao, W. Trends of food intake among Chinese population in 1992–2012. J. Hyg. Res. 2016, 45, 522–526. [Google Scholar]
- Li, Y.C.; Jiang, B.; Zhang, M.; Huang, Z.J.; Qian DE, N.G.; Zhou, M.G.; Wang, L.M. Vegetable and fruit intake among Chinese adults and associated factors: A nationally representative study of 170,847 adults. Biomed. Environ. Sci. 2017, 30, 863–874. [Google Scholar] [PubMed]
- Kaur, H.; Aeri, B.T. Protective Impact of Fruits and Vegetable Intake on Cardiovascular Risk Factors-A Review. J. Clin. Diagn. Res. 2019, 13, 6–9. [Google Scholar]
- Yahia, E.M. The Contribution of Fruit and Vegetable Intake to Human Health. In Fruit and Vegetable Phytochemicals; Wiley: Hoboken, NJ, USA, 2010; pp. 3–51. [Google Scholar]
- Du, H.; Li, L.; Bennett, D.; Yang, L.; Guo, Y.; Key, T.J.; Chen, J. Fresh fruit intake and all-cause and cause-specific mortality: Findings from the China Kadoorie Biobank. Int. J. Epidemiol. 2017, 46, 1444–1455. [Google Scholar] [CrossRef]
- Aune, D.; Giovannucci, E.; Boffetta, P.; Fadnes, L.T.; Keum, N.; Norat, T.; Greenwood, D.C.; Riboli, E.; Vatten, L.J.; Tonstad, S. Fruit and vegetable intake and the risk of cardiovascular disease, total cancer and all-cause mortality—A systematic review and dose-response meta-analysis of prospective studies. Int. J. Epidemiol. 2017, 46, 1029–1056. [Google Scholar] [CrossRef]
- Du, H.; Li, L.; Bennett, D.; Guo, Y.; Key, T.J.; Bian, Z.; Chen, J. Fresh Fruit Intake and Major Cardiovascular Disease in China. N. Eng. J. Med. 2016, 374, 1332–1343. [Google Scholar] [CrossRef]
- Nechuta, S.J.; Shu, X.-O.; Li, H.-L.; Yang, G.; Xiang, Y.-B.; Cai, H.; Chow, W.-H.; Ji, B.; Zhang, X.; Wen, W.; et al. Combined Impact of Lifestyle-Related Factors on Total and Cause-Specific Mortality among Chinese Women: Prospective Cohort Study. PLoS Med. 2010, 7, e1000339. [Google Scholar] [CrossRef]
- Wang, Y.; Yan, R.; Yin, L.; Chen, H.; Li, W. A8560 Fruit, vegetable, and legume intake and mortality risk among China adults. J. Hypertens. 2018, 36, e309. [Google Scholar] [CrossRef]
- Popkin, B.; Du, S.; Zhai, F.; Zhang, B. Cohort Profile: The China Health and Nutrition Survey--monitoring and understanding socio-economic and health change in China, 1989–2011. Int. J. Epidemiol. 2009, 39, 1435–1440. [Google Scholar] [CrossRef]
- Nguyen, B.; Bauman, A.; Gale, J.; Banks, E.; Kritharides, L.; Ding, D. Fruit and vegetable intake and all-cause mortality: Evidence from a large Australian cohort study. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 9. [Google Scholar] [CrossRef]
- Batis, C.; Sotres-Alvarez, D.; Gordon-Larsen, P.; Mendez, M.A.; Adair, L.; Popkin, B. Longitudinal analysis of dietary patterns in Chinese adults from 1991 to 2009. Br. J. Nutr. 2014, 111, 1441–1451. [Google Scholar] [CrossRef]
- Wang, X.; Ouyang, Y.; Liu, J.; Zhu, M.; Zhao, G.; Bao, W.; Hu, F.B. Fruit and vegetable consumption and mortality from all causes, cardiovascular disease, and cancer: Systematic review and dose-response meta-analysis of prospective cohort studies. BMJ 2014, 349, g4490. [Google Scholar] [CrossRef]
- Pan, X.-D.; Wu, P.-G.; Jiang, X.-G. Levels and potential health risk of heavy metals in marketed vegetables in Zhejiang, China. Sci. Rep. 2016, 6, 20317. [Google Scholar] [CrossRef]
- Xu, X.; Li, L.; Huang, X.; Lin, H.; Liu, G.; Xu, D.; Jiang, J. Survey of Four Groups of Cumulative Pesticide Residues in 12 Vegetables in 15 Provinces in China. J. Food Prot. 2018, 81, 377–385. [Google Scholar] [CrossRef]
- Engwa, G.A.; Ferdinand, P.U.; Nwalo, F.N.; Unachukwu, M.N. Mechanism and Health Effects of Heavy Metal Toxicity in Humans. In Poisoning in the Modern World–New Tricks for an Old Dog? IntechOpen: London, UK, 2019. [Google Scholar]
- Kim, K.-H.; Kabir, E.; Jahan, S.A. Exposure to pesticides and the associated human health effects. Sci. Total. Environ. 2017, 575, 525–535. [Google Scholar] [CrossRef]
- Okuda, N.; Miura, K.; Okayama, A.; Okamura, T.; Abbott, R.D.; Nishi, N.; Fujiyoshi, A.; Kita, Y.; Nakamura, Y.; Miyagawa, N.; et al. Fruit and vegetable intake and mortality from cardiovascular disease in Japan: A 24-year follow-up of the NIPPON DATA80 Study. Eur. J. Clin. Nutr. 2015, 69, 482–488. [Google Scholar] [CrossRef]
- Choi, Y.; Lee, J.E.; Bae, J.-M.; Li, Z.-M.; Kim, D.-H.; Lee, M.-S.; Ahn, Y.-O.; Shin, M.-H. Vegetable Intake, but Not Fruit Intake, Is Associated with a Reduction in the Risk of Cancer Incidence and Mortality in Middle-Aged Korean Men. J. Nutr. 2015, 145, 1249–1255. [Google Scholar] [CrossRef]
- Oyebode, O.; Gordondseagu, V.L.Z.; Walker, A.; Mindell, J.S. Fruit and vegetable consumption and all-cause, cancer and CVD mortality: Analysis of Health Survey for England data. J. Epidemiol. Community Health 2014, 68, 856–862. [Google Scholar] [CrossRef]
- Leenders, M.; Sluijs, I.; Ros, M.M.; Boshuizen, H.C.; Siersema, P.D.; Ferrari, P.; Clavel-Chapelon, F. Fruit and Vegetable Intake and Mortality European Prospective Investigation into Cancer and Nutrition. Am. J. Epidemiol. 2013, 178, 590–602. [Google Scholar] [CrossRef]
- Bellavia, A.; Larsson, S.C.; Bottai, M.; Wolk, A.; Orsini, N. Fruit and vegetable intake and all-cause mortality: A dose-response analysis. Am. J. Clin. Nutr. 2013, 98, 454–459. [Google Scholar] [CrossRef]
- Zhang, X.; Shu, X.O.; Xiang, Y.B.; Yang, G.; Li, H.; Gao, J.; Zheng, W. Cruciferous vegetable intake is associated with a reduced risk of total and cardiovascular disease mortality. Am. J. Clin. Nutr. 2011, 94, 240–246. [Google Scholar] [CrossRef]
- Nakamura, K.; Nagata, C.; Oba, S.; Takatsuka, N.; Shimizu, H. Fruit and Vegetable Intake and Mortality from Cardiovascular Disease Are Inversely Associated in Japanese Women but Not in Men. J. Nutr. 2008, 138, 1129–1134. [Google Scholar] [CrossRef]
| Variable | Overall | Quintiles of Fruit Intake | Quintiles of Vegetable Intake | Quintiles of Combined FV Intake | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Q1 | Q2 | Q3 | Q4 | Q5 | Q1 | Q2 | Q3 | Q4 | Q5 | Q1 | Q2 | Q3 | Q4 | Q5 | ||
| Number of subjects | 19,542 | 10,444 | 2332 | 2251 | 2245 | 2270 | 3840 | 3891 | 3924 | 3957 | 3930 | 3800 | 3885 | 3934 | 3944 | 3979 |
| Age (mean (SD)) | 41.04 (15.37) | 40.87 (16.03) | 40.15 (14.00) | 40.15 (14.56) | 41.61 (14.60) | 43.09 (14.94) | 44.23 (17.27) | 41.79 (15.61) | 40.68 (14.76) | 39.39 (14.29) | 39.22 (14.21) | 44.00 (17.46) | 41.69 (15.66) | 40.06 (14.67) | 39.35 (13.93) | 40.25 (14.52) |
| Age group (%) | ||||||||||||||||
| 18–24 | 2895 (14.8) | 1815 (17.4) | 283 (12.1) | 300 (13.3) | 252 (11.2) | 245 (10.8) | 546 (14.2) | 529 (13.6) | 556 (14.2) | 612 (15.5) | 652 (16.6) | 579 (15.2) | 548 (14.1) | 578 (14.7) | 574 (14.6) | 616 (15.5) |
| 25–34 | 5073 (26.0) | 2595 (24.8) | 662 (28.4) | 657 (29.2) | 603 (26.9) | 556 (24.5) | 857 (22.3) | 1015 (26.1) | 1033 (26.3) | 1135 (28.7) | 1033 (26.3) | 846 (22.3) | 984 (25.3) | 1111 (28.2) | 1125 (28.5) | 1007 (25.3) |
| 35–44 | 4182 (21.4) | 2104 (20.1) | 590 (25.3) | 504 (22.4) | 528 (23.5) | 456 (20.1) | 650 (16.9) | 789 (20.3) | 908 (23.1) | 890 (22.5) | 945 (24.0) | 637 (16.8) | 816 (21.0) | 868 (22.1) | 945 (24.0) | 916 (23.0) |
| 45–54 | 3077 (15.7) | 1525 (14.6) | 380 (16.3) | 365 (16.2) | 367 (16.3) | 440 (19.4) | 608 (15.8) | 592 (15.2) | 619 (15.8) | 611 (15.4) | 647 (16.5) | 551 (14.5) | 587 (15.1) | 619 (15.7) | 646 (16.4) | 674 (16.9) |
| 55–64 | 2675 (13.7) | 1420 (13.6) | 274 (11.7) | 284 (12.6) | 319 (14.2) | 378 (16.7) | 620 (16.1) | 612 (15.7) | 534 (13.6) | 474 (12.0) | 435 (11.1) | 625 (16.4) | 590 (15.2) | 502 (12.8) | 442 (11.2) | 516 (13.0) |
| 65+ | 1640 (8.4) | 985 (9.4) | 143 (6.1) | 141 (6.3) | 176 (7.8) | 195 (8.6) | 559 (14.6) | 354 (9.1) | 274 (7.0) | 235 (5.9) | 218 (5.5) | 562 (14.8) | 360 (9.3) | 256 (6.5) | 212 (5.4) | 250 (6.3) |
| Sex = female (%) | 10,532 (53.9) | 5353 (51.3) | 1261 (54.1) | 1251 (55.6) | 1288 (57.4) | 1379 (60.7) | 2296 (59.8) | 2174 (55.9) | 2183 (55.6) | 2057 (52.0) | 1822 (46.4) | 2155 (56.7) | 2188 (56.3) | 2141 (54.4) | 2076 (52.6) | 1972 (49.6) |
| Body mass index (mean (SD)) | 23.09 (3.42) | 22.78 (3.25) | 22.96 (4.18) | 23.42 (3.23) | 23.62 (3.34) | 23.82 (3.38) | 23.35 (3.69) | 23.05 (3.21) | 23.05 (3.21) | 23.06 (3.13) | 22.86 (3.80) | 23.12 (3.57) | 23.03 (3.23) | 23.06 (3.16) | 23.06 (3.16) | 23.17 (3.84) |
| BMI category (%) | ||||||||||||||||
| underweight | 904 (4.6) | 599 (5.7) | 93 (4.0) | 65 (2.9) | 73 (3.3) | 74 (3.3) | 225 (5.9) | 153 (3.9) | 169 (4.3) | 168 (4.2) | 189 (4.8) | 236 (6.2) | 177 (4.6) | 151 (3.8) | 167 (4.2) | 173 (4.3) |
| normal weight | 11,886 (60.8) | 6642 (63.6) | 1491 (63.9) | 1333 (59.2) | 1223 (54.5) | 1197 (52.7) | 2162 (56.3) | 2349 (60.4) | 2400 (61.2) | 2419 (61.1) | 2556 (65.0) | 2213 (58.2) | 2383 (61.3) | 2450 (62.3) | 2428 (61.6) | 2412 (60.6) |
| overweight | 5330 (27.3) | 2546 (24.4) | 614 (26.3) | 672 (29.9) | 732 (32.6) | 766 (33.7) | 1094 (28.5) | 1095 (28.1) | 1079 (27.5) | 1119 (28.3) | 943 (24.0) | 1039 (27.3) | 1052 (27.1) | 1056 (26.8) | 1076 (27.3) | 1107 (27.8) |
| obese | 1422 (7.3) | 657 (6.3) | 134 (5.7) | 181 (8.0) | 217 (9.7) | 233 (10.3) | 359 (9.3) | 294 (7.6) | 276 (7.0) | 251 (6.3) | 242 (6.2) | 312 (8.2) | 273 (7.0) | 277 (7.0) | 273 (6.9) | 287 (7.2) |
| Education (%) | ||||||||||||||||
| Primary or junior high school | 14,235 (72.8) | 8330 (79.8) | 1929 (82.7) | 1598 (71.0) | 1318 (58.7) | 1060 (46.7) | 2429 (63.3) | 2718 (69.9) | 2957 (75.4) | 3001 (75.8) | 3130 (79.6) | 2661 (70.0) | 2907 (74.8) | 2962 (75.3) | 2934 (74.4) | 2771 (69.6) |
| High school or equal | 3823 (19.6) | 1656 (15.9) | 340 (14.6) | 505 (22.4) | 612 (27.3) | 710 (31.3) | 904 (23.5) | 842 (21.6) | 716 (18.2) | 749 (18.9) | 612 (15.6) | 782 (20.6) | 727 (18.7) | 730 (18.6) | 769 (19.5) | 815 (20.5) |
| College and university | 1484 (7.6) | 458 (4.4) | 63 (2.7) | 148 (6.6) | 315 (14.0) | 500 (22.0) | 507 (13.2) | 331 (8.5) | 251 (6.4) | 207 (5.2) | 188 (4.8) | 357 (9.4) | 251 (6.5) | 242 (6.2) | 241 (6.1) | 393 (9.9) |
| Individual average income † | ||||||||||||||||
| Q1 | 4884 (25.0) | 3290 (31.5) | 796 (34.1) | 454 (20.2) | 217 (9.7) | 127 (5.6) | 570 (14.8) | 819 (21.0) | 973 (24.8) | 1149 (29.0) | 1373 (34.9) | 730 (19.2) | 971 (25.0) | 1048 (26.6) | 1128 (28.6) | 1007 (25.3) |
| Q2 | 4901 (25.1) | 2805 (26.9) | 789 (33.8) | 617 (27.4) | 466 (20.8) | 224 (9.9) | 797 (20.8) | 1006 (25.9) | 1086 (27.7) | 1100 (27.8) | 912 (23.2) | 932 (24.5) | 1078 (27.7) | 1109 (28.2) | 1027 (26.0) | 755 (19.0) |
| Q3 | 4757 (24.3) | 2359 (22.6) | 549 (23.5) | 685 (30.4) | 666 (29.7) | 498 (21.9) | 866 (22.6) | 1032 (26.5) | 1085 (27.7) | 959 (24.2) | 815 (20.7) | 901 (23.7) | 981 (25.3) | 1003 (25.5) | 1003 (25.4) | 869 (21.8) |
| Q4 | 5000 (25.6) | 1990 (19.1) | 198 (8.5) | 495 (22.0) | 896 (39.9) | 1421 (62.6) | 1607 (41.8) | 1034 (26.6) | 780 (19.9) | 749 (18.9) | 830 (21.1) | 1237 (32.6) | 855 (22.0) | 774 (19.7) | 786 (19.9) | 1348 (33.9) |
| Marital status = married (%) | 16,416 (84.0) | 8465 (81.1) | 2050 (87.9) | 1982 (88.0) | 1956 (87.1) | 1963 (86.5) | 3074 (80.1) | 3246 (83.4) | 3375 (86.0) | 3416 (86.3) | 3305 (84.1) | 3015 (79.3) | 3250 (83.7) | 3353 (85.2) | 3401 (86.2) | 3397 (85.4) |
| Residence = urban (%) | 11,324 (57.9) | 6910 (66.2) | 1455 (62.4) | 1197 (53.2) | 986 (43.9) | 776 (34.2) | 1953 (50.9) | 2138 (54.9) | 2313 (58.9) | 2425 (61.3) | 2495 (63.5) | 2126 (55.9) | 2314 (59.6) | 2357 (59.9) | 2351 (59.6) | 2176 (54.7) |
| Urban index ‡ (mean (SD)) | 58.59 (22.75) | 53.72 (21.97) | 51.11 (19.11) | 59.86 (21.31) | 68.69 (20.44) | 77.44 (19.25) | 66.95 (21.47) | 61.90 (21.64) | 58.31 (21.63) | 54.61 (21.97) | 51.44 (23.66) | 63.00 (21.55) | 58.56 (21.42) | 56.95 (21.93) | 55.30 (22.40) | 59.30 (25.39) |
| Smoking status | ||||||||||||||||
| Current | 2920 (14.9) | 1537 (14.7) | 201 (8.6) | 337 (15.0) | 405 (18.0) | 440 (19.4) | 684 (17.8) | 610 (15.7) | 507 (12.9) | 537 (13.6) | 582 (14.8) | 674 (17.7) | 543 (14.0) | 517 (13.1) | 515 (13.1) | 671 (16.9) |
| Not current (never, past) | 7565 (38.7) | 3433 (32.9) | 491 (21.1) | 887 (39.4) | 1200 (53.5) | 1554 (68.5) | 1966 (51.2) | 1564 (40.2) | 1454 (37.1) | 1364 (34.5) | 1217 (31.0) | 1672 (44.0) | 1406 (36.2) | 1392 (35.4) | 1404 (35.6) | 1691 (42.5) |
| Not answered | 9057 (46.3) | 5474 (52.4) | 1640 (70.3) | 1027 (45.6) | 640 (28.5) | 276 (12.2) | 1190 (31.0) | 1717 (44.1) | 1963 (50.0) | 2056 (52.0) | 2131 (54.2) | 1454 (38.3) | 1936 (49.8) | 2025 (51.5) | 2025 (51.3) | 1617 (40.6) |
| Alcohol drinking | ||||||||||||||||
| Current | 3603 (18.4) | 1735 (16.6) | 232 (9.9) | 432 (19.2) | 549 (24.5) | 655 (28.9) | 871 (22.7) | 731 (18.8) | 664 (16.9) | 643 (16.2) | 694 (17.7) | 785 (20.7) | 659 (17.0) | 648 (16.5) | 648 (16.4) | 863 (21.7) |
| Not current (never, past) | 6838 (35.0) | 3211 (30.7) | 456 (19.6) | 788 (35.0) | 1052 (46.9) | 1331 (58.6) | 1778 (46.3) | 1429 (36.7) | 1291 (32.9) | 1249 (31.6) | 1091 (27.8) | 1555 (40.9) | 1284 (33.1) | 1251 (31.8) | 1260 (31.9) | 1488 (37.4) |
| Not answered | 9101 (46.6) | 5498 (52.6) | 1644 (70.5) | 1031 (45.8) | 644 (28.7) | 284 (12.5) | 1191 (31.0) | 1731 (44.5) | 1969 (50.2) | 2065 (52.2) | 2145 (54.6) | 1460 (38.4) | 1942 (50.0) | 2035 (51.7) | 2036 (51.6) | 1628 (40.9) |
| Physical activity | ||||||||||||||||
| Light | 10,273 (52.6) | 4623 (44.3) | 1015 (43.5) | 1307 (58.1) | 1563 (69.6) | 1765 (77.8) | 2701 (70.3) | 2374 (61.0) | 2067 (52.7) | 1731 (43.7) | 1400 (35.6) | 2454 (64.6) | 2166 (55.8) | 1955 (49.7) | 1821 (46.2) | 1877 (47.2) |
| Moderate | 3537 (18.1) | 2038 (19.5) | 519 (22.3) | 395 (17.5) | 325 (14.5) | 260 (11.5) | 577 (15.0) | 716 (18.4) | 760 (19.4) | 788 (19.9) | 696 (17.7) | 652 (17.2) | 762 (19.6) | 766 (19.5) | 713 (18.1) | 644 (16.2) |
| Heavy | 5732 (29.3) | 3783 (36.2) | 798 (34.2) | 549 (24.4) | 357 (15.9) | 245 (10.8) | 562 (14.6) | 801 (20.6) | 1097 (28.0) | 1438 (36.3) | 1834 (46.7) | 694 (18.3) | 957 (24.6) | 1213 (30.8) | 1410 (35.8) | 1458 (36.6) |
| Calorie intake (kcal/day) (mean (SD)) | 2183.09 (1190.61) | 2228.19 (1287.02) | 2229.97 (546.66) | 2129.02 (582.43) | 2071.18 (1356.15) | 2091.75 (1444.66) | 1993.62 (778.84) | 2178.29 (502.93) | 2238.84 (425.09) | 2370.71 (507.87) | 2511.44 (1175.61) | 1925.57 (1147.12) | 2093.93 (616.98) | 2187.04 (619.84) | 2284.93 (597.35) | 2411.24 (2113.77) |
| Quintiles a | P for Trend | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Q1 | Q2 | Q3 | Q4 | Q5 | |||||||
| Vegetable intake | |||||||||||
| Model 1 (crude) | 1 | Reference | 0.52 | (0.44–0.62) | 0.46 | (0.39–0.54) | 0.37 | (0.31–0.44) | 0.46 | (0.39–0.55) | <0.001 |
| Model 2 b (age, sex adjusted) | 1 | Reference | 0.71 | (0.60–0.85) | 0.74 | (0.62–0.87) | 0.66 | (0.55–0.79) | 0.93 | (0.79–1.11) | 0.311 |
| Model 3 c (adjusted) | 1 | Reference | 0.78 | (0.65,0.93) | 0.75 | (0.63,0.89) | 0.63 | (0.53,0.76) | 0.8 | (0.67,0.96) | 0.234 |
| Fruit intake | |||||||||||
| Model 1 (crude) | 1 | Reference | 0.35 | (0.29–0.41) | 0.19 | (0.15–0.25) | 0.24 | (0.18–0.31) | 0.13 | (0.08–0.21) | <0.001 |
| Model 2 b (age, sex adjusted) | 1 | Reference | 0.34 | (0.29–0.41) | 0.23 | (0.18–0.30) | 0.30 | (0.23–0.39) | 0.13 | (0.08–0.21) | <0.001 |
| Model 3 c (adjusted) | 1 | Reference | 0.36 | (0.30–0.43) | 0.28 | (0.22–0.36) | 0.43 | (0.32–0.57) | 0.24 | (0.15–0.40) | <0.001 |
| FV intake | |||||||||||
| Model 1 (crude) | 1 | Reference | 0.48 | (0.41–0.56) | 0.38 | (0.32–0.44) | 0.29 | (0.25–0.35) | 0.34 | (0.28–0.40) | <0.001 |
| Model 2 b (age, sex adjusted) | 1 | Reference | 0.68 | (0.58–0.8) | 0.61 | (0.52–0.72) | 0.56 | (0.47–0.67) | 0.65 | (0.55–0.78) | <0.001 |
| Model 3 c (adjusted) | 1 | Reference | 0.71 | (0.61–0.84) | 0.63 | (0.54–0.75) | 0.59 | (0.49–0.70) | 0.70 | (0.58–0.85) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gu, Y.; He, Y.; Ali, S.H.; Harper, K.; Dong, H.; Gittelsohn, J. Fruit and Vegetable Intake and All-Cause Mortality in a Chinese Population: The China Health and Nutrition Survey. Int. J. Environ. Res. Public Health 2021, 18, 342. https://doi.org/10.3390/ijerph18010342
Gu Y, He Y, Ali SH, Harper K, Dong H, Gittelsohn J. Fruit and Vegetable Intake and All-Cause Mortality in a Chinese Population: The China Health and Nutrition Survey. International Journal of Environmental Research and Public Health. 2021; 18(1):342. https://doi.org/10.3390/ijerph18010342
Chicago/Turabian StyleGu, Yuxuan, Yansu He, Shahmir H. Ali, Kaitlyn Harper, Hengjin Dong, and Joel Gittelsohn. 2021. "Fruit and Vegetable Intake and All-Cause Mortality in a Chinese Population: The China Health and Nutrition Survey" International Journal of Environmental Research and Public Health 18, no. 1: 342. https://doi.org/10.3390/ijerph18010342
APA StyleGu, Y., He, Y., Ali, S. H., Harper, K., Dong, H., & Gittelsohn, J. (2021). Fruit and Vegetable Intake and All-Cause Mortality in a Chinese Population: The China Health and Nutrition Survey. International Journal of Environmental Research and Public Health, 18(1), 342. https://doi.org/10.3390/ijerph18010342





