New Intraoral Scanner-Based Chairside Measurement Method to Investigate the Internal Fit of Crowns: A Clinical Trial
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pimenta, M.A.; Frasca, L.C.; Lopes, R.; Rivaldo, E. Evaluation of marginal and internal fit of ceramic and metallic crown copings using x-ray microtomography (micro-CT) technology. J. Prosthet. Dent. 2015, 114, 223–228. [Google Scholar] [CrossRef]
- Neves, F.D.; Prado, C.J.; Prudente, M.S.; Carneiro, T.A.; Zancope, K.; Davi, L.R.; Mendonca, G.; Cooper, L.F.; Soares, C.J. Micro-computed tomography evaluation of marginal fit of lithium disilicate crowns fabricated by using chairside CAD/CAM systems or the heat-pressing technique. J. Prosthet. Dent. 2014, 112, 1134–1140. [Google Scholar] [CrossRef] [PubMed]
- Joda, T.; Ferrari, M.; Gallucci, G.O.; Wittneben, J.G.; Bragger, U. Digital technology in fixed implant prosthodontics. Periodontol 2000 2017, 73, 178–192. [Google Scholar] [CrossRef] [PubMed]
- Boitelle, P.; Mawussi, B.; Tapie, L.; Fromentin, O. A systematic review of CAD/CAM fit restoration evaluations. J. Oral Rehabil. 2014, 41, 853–874. [Google Scholar] [CrossRef]
- Nakamura, T.; Dei, N.; Kojima, T.; Wakabayashi, K. Marginal and internal fit of Cerec 3 CAD/CAM all-ceramic crowns. Int. J. Prosthodont. 2003, 16, 244–248. [Google Scholar]
- Rezende, C.E.; Borges, A.F.; Gonzaga, C.C.; Duan, Y.; Rubo, J.H.; Griggs, J.A. Effect of cement space on stress distribution in Y-TZP based crowns. Dent. Mater. 2017, 33, 144–151. [Google Scholar] [CrossRef]
- Lee, D.H. Digital approach to assessing the 3-dimensional misfit of fixed dental prostheses. J. Prosthet. Dent. 2016, 116, 836–839. [Google Scholar] [CrossRef]
- Keshvad, A.; Hooshmand, T.; Asefzadeh, F.; Khalilinejad, F.; Alihemmati, M.; Van Noort, R. Marginal gap, internal fit, and fracture load of leucite-reinforced ceramic inlays fabricated by CEREC inLab and hot-pressed techniques. J. Prosthodont. Implant Esthet. Reconstr. Dent. 2011, 20, 535–540. [Google Scholar] [CrossRef]
- May, L.G.; Kelly, J.R.; Bottino, M.A.; Hill, T. Effects of cement thickness and bonding on the failure loads of CAD/CAM ceramic crowns: Multi-physics FEA modeling and monotonic testing. Dent. Mater. 2012, 28, e99–e109. [Google Scholar] [CrossRef]
- Choi, S.; Yoon, H.I.; Park, E.J. Load-bearing capacity of various CAD/CAM monolithic molar crowns under recommended occlusal thickness and reduced occlusal thickness conditions. J. Adv. Prosthodont. 2017, 9, 423–431. [Google Scholar] [CrossRef] [Green Version]
- Spitznagel, F.A.; Boldt, J.; Gierthmuehlen, P.C. CAD/CAM Ceramic Restorative Materials for Natural Teeth. J. Dent. Res. 2018, 97, 1082–1091. [Google Scholar] [CrossRef] [PubMed]
- Klur, T.; Hasan, I.; Ottersbach, K.; Stark, H.; Fichte, M.; Dirk, C.; Bourauel, C. PEKK-made indirect temporary crowns and bridges: A clinical pilot study. Clin. Oral Investig. 2019, 23, 771–777. [Google Scholar] [CrossRef] [PubMed]
- Son, K.; Lee, S.; Kang, S.H.; Park, J.; Lee, K.B.; Jeon, M.; Yun, B.J. A Comparison Study of Marginal and Internal Fit Assessment Methods for Fixed Dental Prostheses. J. Clin. Med. 2019, 8, 785. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wostmann, B.; Blosser, T.; Gouentenoudis, M.; Balkenhol, M.; Ferger, P. Influence of margin design on the fit of high-precious alloy restorations in patients. J. Dent. 2005, 33, 611–618. [Google Scholar] [CrossRef]
- Biscaro, L.; Bonfiglioli, R.; Soattin, M.; Vigolo, P. An in vivo evaluation of fit of zirconium-oxide based ceramic single crowns, generated with two CAD/CAM systems, in comparison to metal ceramic single crowns. J. Prosthodont. Implant Esthet. Reconstr. Dent. 2013, 22, 36–41. [Google Scholar] [CrossRef] [PubMed]
- Coli, P. Fit of a New Pressure-Sintered Zirconium Dioxide Coping. Int. J. Prosthodont. 2004, 17, 59–64. [Google Scholar]
- Kauling, A.E.C.; Keul, C.; Erdelt, K.; Kuhnisch, J.; Guth, J.F. Can lithium disilicate ceramic crowns be fabricated on the basis of CBCT data? Clin. Oral Investig. 2019, 23, 3739–3748. [Google Scholar] [CrossRef]
- Keul, C.; Stawarczyk, B.; Erdelt, K.J.; Beuer, F.; Edelhoff, D.; Guth, J.F. Fit of 4-unit FDPs made of zirconia and CoCr-alloy after chairside and labside digitalization--a laboratory study. Dent. Mater. 2014, 30, 400–407. [Google Scholar] [CrossRef]
- Pradies, G.; Zarauz, C.; Valverde, A.; Ferreiroa, A.; Martinez-Rus, F. Clinical evaluation comparing the fit of all-ceramic crowns obtained from silicone and digital intraoral impressions based on wavefront sampling technology. J. Dent. 2015, 43, 201–208. [Google Scholar] [CrossRef] [Green Version]
- Ueda, K.; Beuer, F.; Stimmelmayr, M.; Erdelt, K.; Keul, C.; Guth, J.F. Fit of 4-unit FDPs from CoCr and zirconia after conventional and digital impressions. Clin. Oral Investig. 2016, 20, 283–289. [Google Scholar] [CrossRef]
- Boitelle, P.; Tapie, L.; Mawussi, B.; Fromentin, O. Evaluation of the marginal fit of CAD-CAM zirconia copings: Comparison of 2D and 3D measurement methods. J. Prosthet. Dent. 2018, 119, 75–81. [Google Scholar] [CrossRef]
- Kim, K.B.; Kim, J.H.; Kim, W.C.; Kim, J.H. Three-dimensional evaluation of gaps associated with fixed dental prostheses fabricated with new technologies. J. Prosthet. Dent. 2014, 112, 1432–1436. [Google Scholar] [CrossRef]
- Luthardt, R.G.; Bornemann, G.; Lemelson, S.; Walter, M.H.; Huls, A. An innovative method for evaluation of the 3-D internal fit of CAD/CAM crowns fabricated after direct optical versus indirect laser scan digitizing. Int. J. Prosthodont. 2004, 17, 680–685. [Google Scholar]
- Tsitrou, E.A.; Northeast, S.E.; van Noort, R. Evaluation of the marginal fit of three margin designs of resin composite crowns using CAD/CAM. J. Dent. 2007, 35, 68–73. [Google Scholar] [CrossRef] [Green Version]
- Mostafa, N.Z.; Ruse, N.D.; Ford, N.L.; Carvalho, R.M.; Wyatt, C.C.L. Marginal Fit of Lithium Disilicate Crowns Fabricated Using Conventional and Digital Methodology: A Three-Dimensional Analysis. J. Prosthodont. 2018, 27, 145–152. [Google Scholar] [CrossRef]
- Mai, H.N.; Lee, K.E.; Lee, K.B.; Jeong, S.M.; Lee, S.J.; Lee, C.H.; An, S.Y.; Lee, D.H. Verification of a computer-aided replica technique for evaluating prosthesis adaptation using statistical agreement analysis. J. Adv. Prosthodont. 2017, 9, 358–363. [Google Scholar] [CrossRef] [Green Version]
- Al-Imam, H.; Michou, S.; Benetti, A.R.; Gotfredsen, K. Evaluation of marginal and internal fit of acrylic bridges using optical coherence tomography. J. Oral Rehabil. 2019, 46, 274–281. [Google Scholar] [CrossRef]
- Zimmermann, M.; Valcanaia, A.; Neiva, G.; Mehl, A.; Fasbinder, D. Digital evaluation of the fit of zirconia-reinforced lithium silicate crowns with a new three-dimensional approach. Quintessence Int. 2018, 49, 9–15. [Google Scholar]
- Schlenz, M.A.; Vogler, J.A.H.; Schmidt, A.; Rehmann, P.; Wostmann, B. Chairside measurement of the marginal and internal fit of crowns: A new intraoral scan-based approach. Clin. Oral Investig. 2019. [Google Scholar] [CrossRef]
- Praca, L.; Pekam, F.C.; Rego, R.O.; Radermacher, K.; Wolfart, S.; Marotti, J. Accuracy of single crowns fabricated from ultrasound digital impressions. Dent. Mater. 2018, 34, e280–e288. [Google Scholar] [CrossRef]
- Podhorsky, A.; Rehmann, P.; Wostmann, B. Tooth preparation for full-coverage restorations-a literature review. Clin. Oral Investig. 2015, 19, 959–968. [Google Scholar] [CrossRef]
- Wostmann, B.; Rehmann, P.; Balkenhol, M. Influence of different retraction techniques on crevicular fluid flow. Int. J. Prosthodont. 2008, 21, 215–216. [Google Scholar] [PubMed]
- Rehmann, P.; Sichwardt, V.; Wostmann, B. Intraoral Scanning Systems: Need for Maintenance. Int. J. Prosthodont. 2017, 30, 27–29. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muller, P.; Ender, A.; Joda, T.; Katsoulis, J. Impact of digital intraoral scan strategies on the impression accuracy using the TRIOS Pod scanner. Quintessence Int. 2016, 47, 343–349. [Google Scholar]
- Bosniac, P.; Rehmann, P.; Wostmann, B. Comparison of an indirect impression scanning system and two direct intraoral scanning systems in vivo. Clin. Oral Investig. 2019, 23, 2421–2427. [Google Scholar] [CrossRef] [PubMed]
- Boeddinghaus, M.; Breloer, E.S.; Rehmann, P.; Wostmann, B. Accuracy of single-tooth restorations based on intraoral digital and conventional impressions in patients. Clin. Oral Investig. 2015, 19, 2027–2034. [Google Scholar] [CrossRef] [PubMed]
- Zimmermann, M.; Valcanaia, A.; Neiva, G.; Mehl, A.; Fasbinder, D. Three-Dimensional Digital Evaluation of the Fit of Endocrowns Fabricated from Different CAD/CAM Materials. J. Prosthodont. 2019, 28, e504–e509. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- El Ghoul, W.A.; Ozcan, M.; Ounsi, H.; Tohme, H.; Salameh, Z. Effect of different CAD-CAM materials on the marginal and internal adaptation of endocrown restorations: An in vitro study. J. Prosthet. Dent. 2020, 123, 128–134. [Google Scholar] [CrossRef] [Green Version]
- Huang, Z.; Zhang, L.; Zhu, J.; Zhao, Y.; Zhang, X. Clinical Marginal and Internal Fit of Crowns Fabricated Using Different CAD/CAM Technologies. J. Prosthodont. 2015, 24, 291–295. [Google Scholar] [CrossRef]
- Rodiger, M.; Schneider, L.; Rinke, S. Influence of Material Selection on the Marginal Accuracy of CAD/CAM-Fabricated Metal- and All-Ceramic Single Crown Copings. BioMed Res. Int. 2018, 2018, 2143906. [Google Scholar] [CrossRef]
- Hasanzade, M.; Moharrami, M.; Alikhasi, M. Evaluation of Marginal and Internal Adaptation of Endocrowns Fabricated from Three Different CAD/CAM Materials. Eur. J. Prosthodont. Restor. Dent. 2019, 27, 164–171. [Google Scholar] [CrossRef]
- Gressler May, L.; Kelly, J.R.; Bottino, M.A.; Hill, T. Influence of the resin cement thickness on the fatigue failure loads of CAD/CAM feldspathic crowns. Dent. Mater. 2015, 31, 895–900. [Google Scholar]
- Shim, J.S.; Lee, J.S.; Lee, J.Y.; Choi, Y.J.; Shin, S.W.; Ryu, J.J. Effect of software version and parameter settings on the marginal and internal adaptation of crowns fabricated with the CAD/CAM system. J. Appl. Oral Sci. 2015, 23, 515–522. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mennito, A.S.; Evans, Z.P.; Nash, J.; Bocklet, C.; Lauer Kelly, A.; Bacro, T.; Cayouette, M.; Ludlow, M.; Renne, W.G. Evaluation of the trueness and precision of complete arch digital impressions on a human maxilla using seven different intraoral digital impression systems and a laboratory scanner. J. Esthet. Restor. Dent. 2019, 31, 369–377. [Google Scholar] [CrossRef] [PubMed]
- O’Toole, S.; Osnes, C.; Bartlett, D.; Keeling, A. Investigation into the accuracy and measurement methods of sequential 3D dental scan alignment. Dent. Mater. 2019, 35, 495–500. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, A.; Klussmann, L.; Wostmann, B.; Schlenz, M.A. Accuracy of Digital and Conventional Full-Arch Impressions in Patients: An Update. J. Clin. Med. 2020, 9, 688. [Google Scholar] [CrossRef] [Green Version]
- Keul, C.; Guth, J.F. Accuracy of full-arch digital impressions: An in vitro and in vivo comparison. Clin. Oral Investig. 2020, 24, 735–745. [Google Scholar] [CrossRef]
- Rudolph, H.; Ostertag, S.; Ostertag, M.; Walter, M.H.; Luthardt, R.G.; Kuhn, K. Reliability of light microscopy and a computer-assisted replica measurement technique for evaluating the fit of dental copings. J. Appl. Oral Sci. 2018, 26, e20160590. [Google Scholar] [CrossRef] [Green Version]
- Zimmermann, M.; Valcanaia, A.; Neiva, G.; Mehl, A.; Fasbinder, D. Influence of Different CAM Strategies on the Fit of Partial Crown Restorations: A Digital Three-dimensional Evaluation. Oper. Dent. 2018, 43, 530–538. [Google Scholar] [CrossRef]

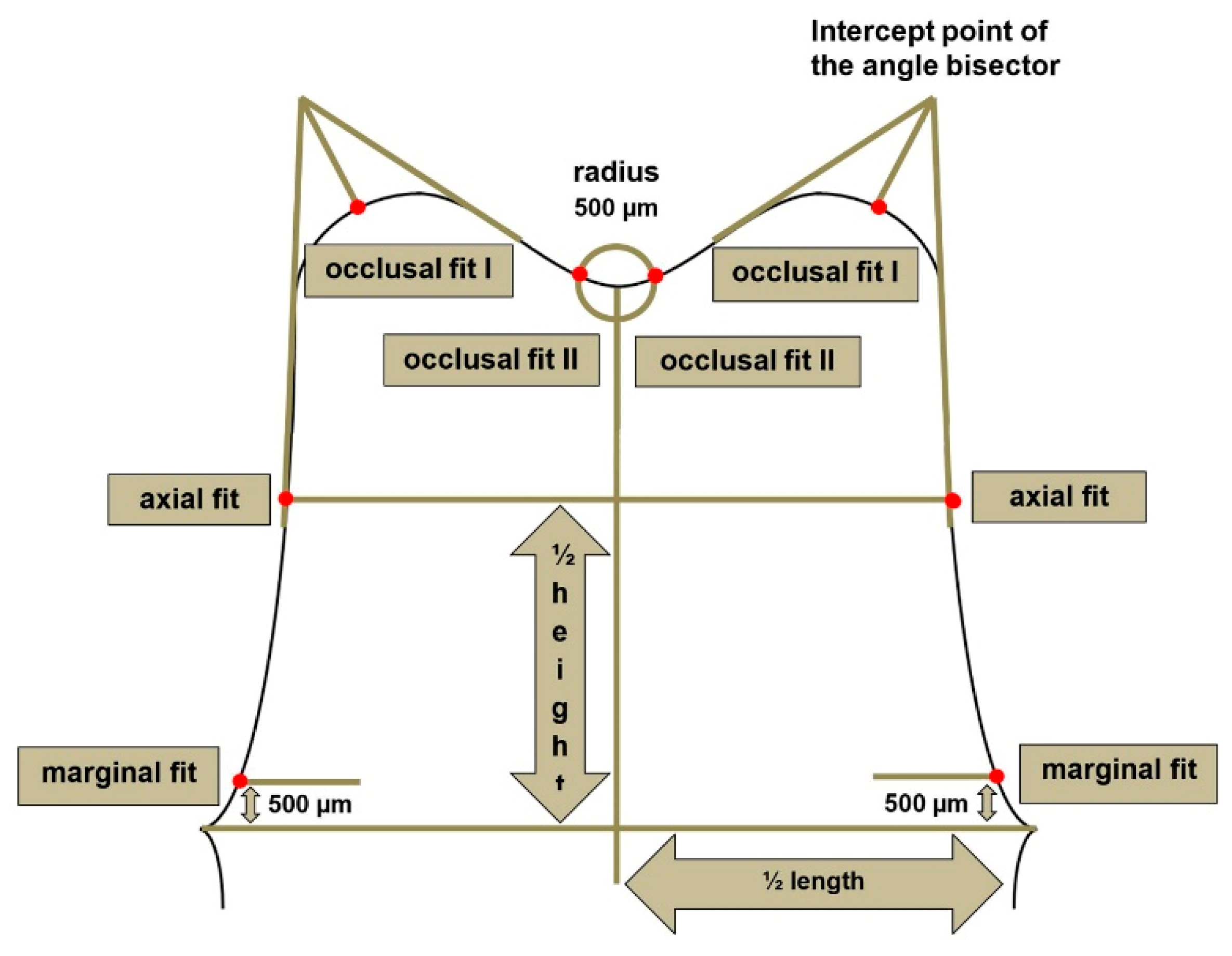
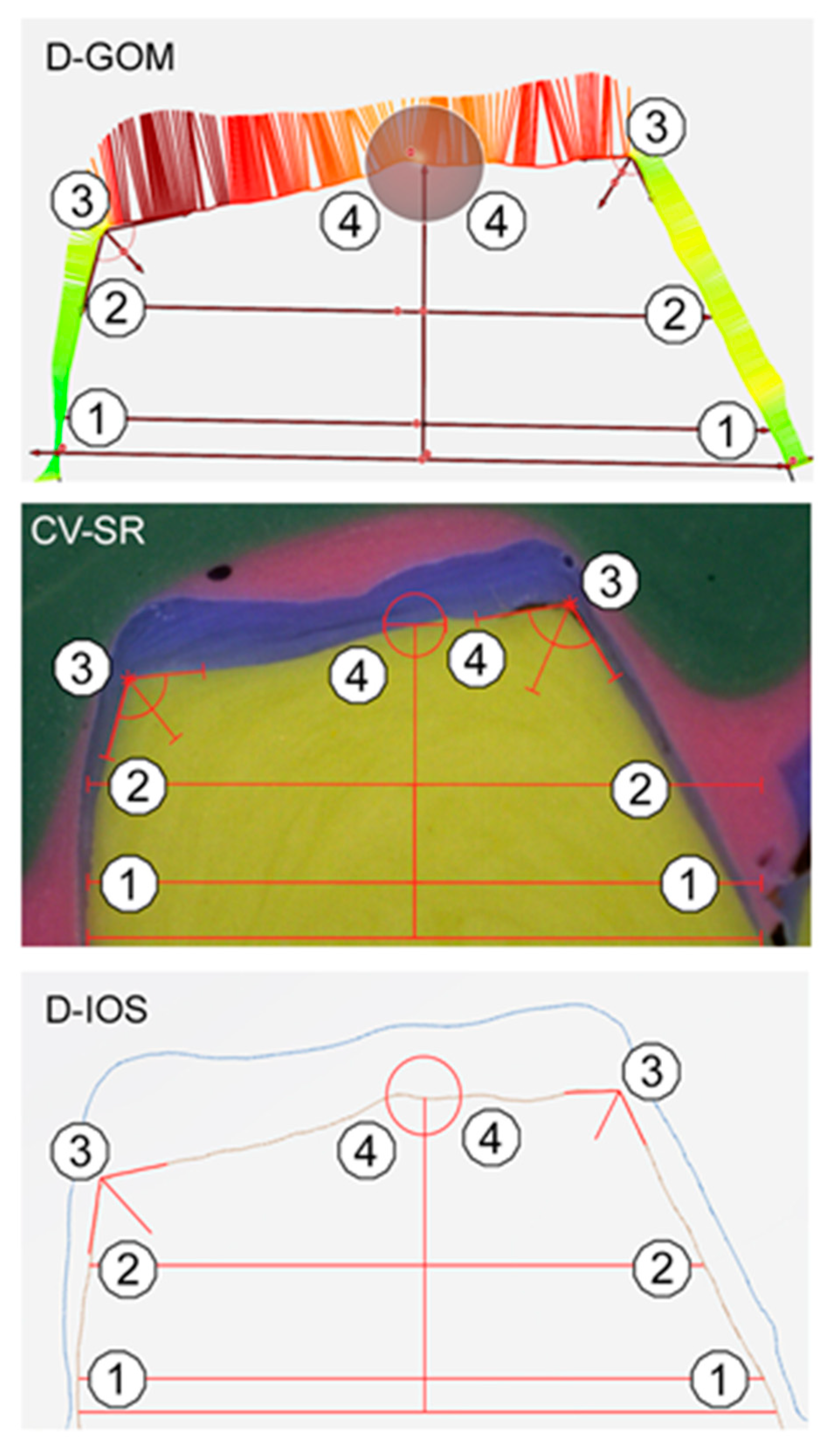
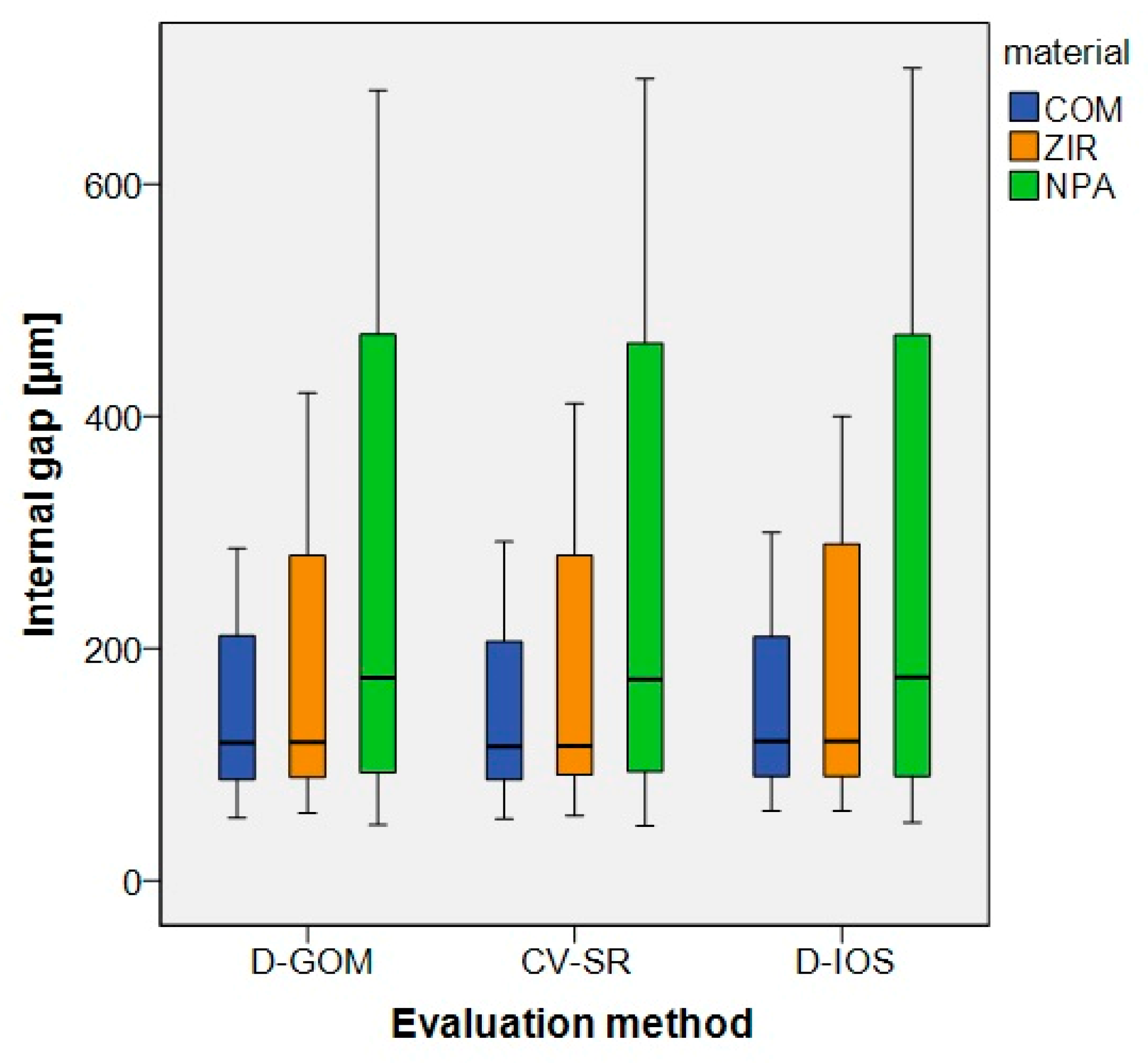
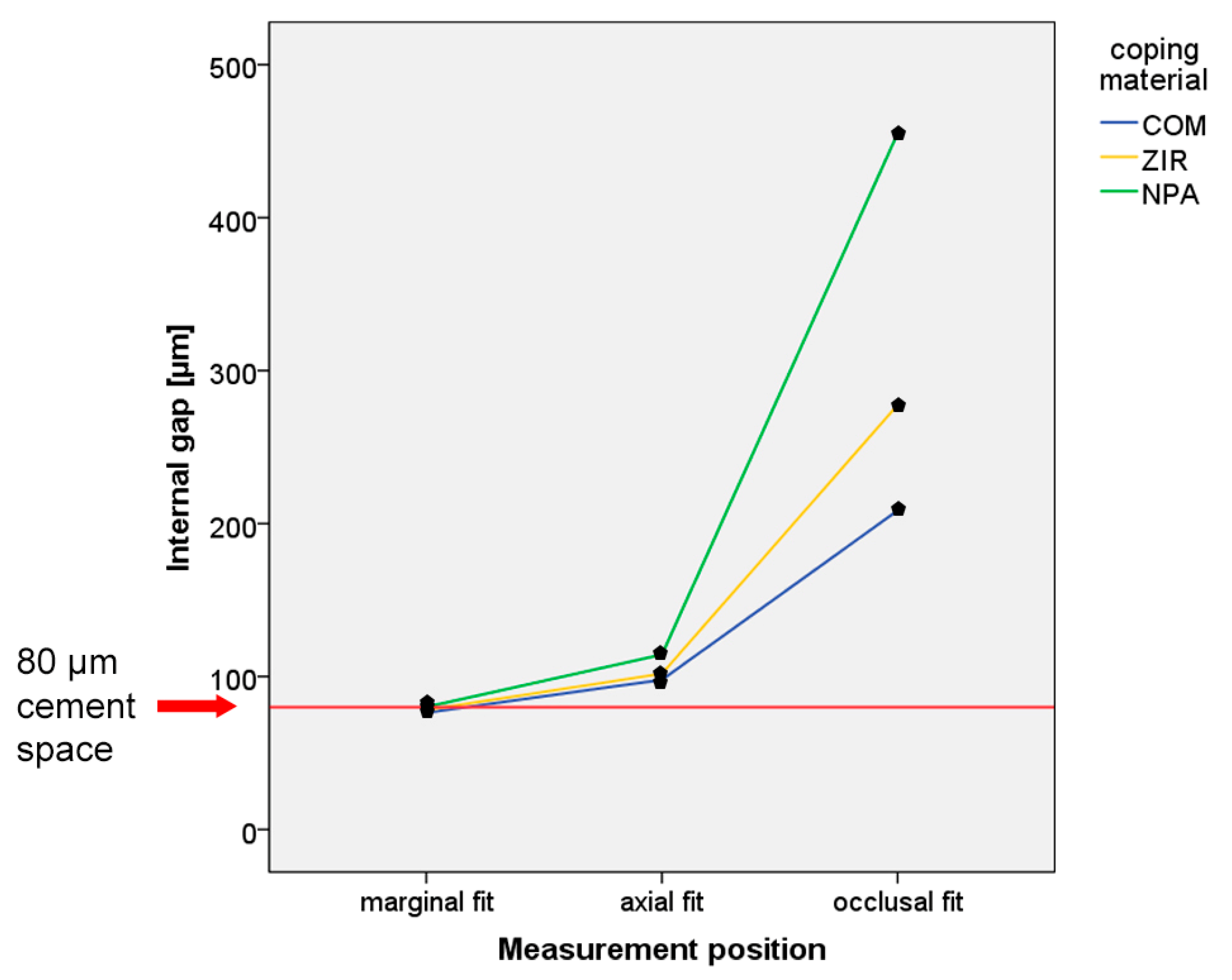
| Material | Product Name (Batch No.) | Manufacturer |
|---|---|---|
| Powder spray | CEREC Optispray (S50868) | Dentsply Sirona (Bensheim, Germany) |
| Low-viscosity addition-curing silicone | Fit Test C&B (1841465) | Voco (Cuxhaven, Germany) |
| Low-viscosity vinyl polyether silicone | EXA’lence Extra Light Body (1806261) | GC (Tokyo, Japan) |
| Low-viscosity vinyl polyether silicone | EXA’lence Light Body (1806221) | |
| High-viscosity vinyl polyether silicone | EXA’lence Putty (1711091) | |
| Resin composite block | LuxaCam Composite (784249) | DMG (Hamburg, Germany) |
| 3Y-TZP zirconium dioxide | Lava Plus (4525742) | 3M (St.Paul, MN, USA) |
| Non-precious alloy (>10 wt% cobalt, chrome, 1–10 wt% tungsten, silicon, manganese, iron, 0.1–1 wt% carbon) | Finoframe CoCr (K10627) | Fino (Bad Bocklet, Germany) |
| Evaluation Method | Coping Material | Measurement Position | Internal Gap [µm] | ||||
|---|---|---|---|---|---|---|---|
| Mean | Standard Deviation | Median | Confidence Interval | ||||
| Lower | Upper | ||||||
| CV-SR | COM | marginal fit | 75.8 | 9.9 | 77.0 | 74.0 | 77.6 |
| axial fit | 96.4 | 9.3 | 96.0 | 94.7 | 98.1 | ||
| occlusal fit | 204.9 | 39.5 | 206.0 | 199.9 | 209.9 | ||
| ZIR | marginal fit | 77.8 | 9.2 | 77.0 | 76.2 | 79.5 | |
| axial fit | 100.2 | 9.3 | 100.5 | 98.5 | 101.8 | ||
| occlusal fit | 273.9 | 59.9 | 280.0 | 266.3 | 281.5 | ||
| NPA | marginal fit | 79.8 | 12.6 | 79.0 | 77.5 | 82.1 | |
| axial fit | 112.5 | 21.1 | 106.0 | 108.7 | 116.3 | ||
| occlusal fit | 451.1 | 147.6 | 463.0 | 432.4 | 469.9 | ||
| D-GOM | COM | marginal fit | 76.6 | 9.5 | 77.0 | 74.9 | 78.4 |
| axial fit | 98.0 | 10.8 | 96.5 | 96.0 | 100.0 | ||
| occlusal fit | 208.2 | 38.3 | 211.0 | 203.3 | 213.0 | ||
| ZIR | marginal fit | 77.9 | 8.8 | 78.0 | 76.3 | 79.5 | |
| axial fit | 101.6 | 9.6 | 101.0 | 99.9 | 103.4 | ||
| occlusal fit | 277.3 | 59.0 | 280.0 | 269.8 | 284.8 | ||
| NPA | marginal fit | 80.1 | 11.7 | 80.5 | 78.0 | 82.2 | |
| axial fit | 113.9 | 20.6 | 107.0 | 110.2 | 117.6 | ||
| occlusal fit | 455.2 | 146.9 | 470.5 | 436.6 | 473.9 | ||
| D-IOS | COM | marginal fit | 76.7 | 10.1 | 80.0 | 74.8 | 78.5 |
| axial fit | 99.1 | 10.8 | 100.0 | 97.1 | 101.0 | ||
| occlusal fit | 212.4 | 39.5 | 210.0 | 207.4 | 217.4 | ||
| ZIR | marginal fit | 78.7 | 9.2 | 80.0 | 77.0 | 80.3 | |
| axial fit | 103.8 | 10.2 | 100.0 | 101.9 | 105.6 | ||
| occlusal fit | 281.5 | 59.5 | 290.0 | 274.0 | 289.1 | ||
| NPA | marginal fit | 80.4 | 12.3 | 80.0 | 78.2 | 82.6 | |
| axial fit | 116.4 | 20.6 | 110.0 | 112.7 | 120.1 | ||
| occlusal fit | 458.7 | 147.2 | 470.0 | 440.0 | 477.4 | ||
| Measurement Position | ZIR | NPA | |
|---|---|---|---|
| marginal fit | COM | p = 0.037 | p < 0.001 |
| ZIR | p = 0.040 | ||
| axial fit | COM | p < 0.001 | p < 0.001 |
| ZIR | p < 0.001 | ||
| occlusal fit | COM | p < 0.001 | p < 0.001 |
| ZIR | p < 0.001 |
| Measurement Position | Internal Gap (mean (SD) [µm]) | Internal Gap – Cement Space = Absolute Discrepancy (Mean (SD) [µm]) | ||||
|---|---|---|---|---|---|---|
| COM | ZIR | NPA | COM | ZIR | NPA | |
| marginal fit (n = 120) | 76.4 (0.5) | 78.1 (0.5) | 80.1 (0.6) | −3.6 (0.5) | −1.9 (0.5) | 0.1 (0.6) |
| axial fit (n = 120) | 97.8 (0.6) | 101.8 (0.5) | 114.3 (1.1) | 17.8 (0.6) | 21.8 (0.5) | 34.3 (1.1) |
| occlusal fit (n = 240) | 208.5 (1.5) | 277.6 (2.2) | 455.0 (5.5) | 128.5 (1.5) | 197.6 (2.2) | 375.0 (5.5) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schlenz, M.A.; Vogler, J.; Schmidt, A.; Rehmann, P.; Wöstmann, B. New Intraoral Scanner-Based Chairside Measurement Method to Investigate the Internal Fit of Crowns: A Clinical Trial. Int. J. Environ. Res. Public Health 2020, 17, 2182. https://doi.org/10.3390/ijerph17072182
Schlenz MA, Vogler J, Schmidt A, Rehmann P, Wöstmann B. New Intraoral Scanner-Based Chairside Measurement Method to Investigate the Internal Fit of Crowns: A Clinical Trial. International Journal of Environmental Research and Public Health. 2020; 17(7):2182. https://doi.org/10.3390/ijerph17072182
Chicago/Turabian StyleSchlenz, Maximiliane Amelie, Jonas Vogler, Alexander Schmidt, Peter Rehmann, and Bernd Wöstmann. 2020. "New Intraoral Scanner-Based Chairside Measurement Method to Investigate the Internal Fit of Crowns: A Clinical Trial" International Journal of Environmental Research and Public Health 17, no. 7: 2182. https://doi.org/10.3390/ijerph17072182
APA StyleSchlenz, M. A., Vogler, J., Schmidt, A., Rehmann, P., & Wöstmann, B. (2020). New Intraoral Scanner-Based Chairside Measurement Method to Investigate the Internal Fit of Crowns: A Clinical Trial. International Journal of Environmental Research and Public Health, 17(7), 2182. https://doi.org/10.3390/ijerph17072182






