Grappling with Gulf War Illness: Perspectives of Gulf War Providers
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Setting
2.3. Data Collection
2.4. Data Analysis
3. Results
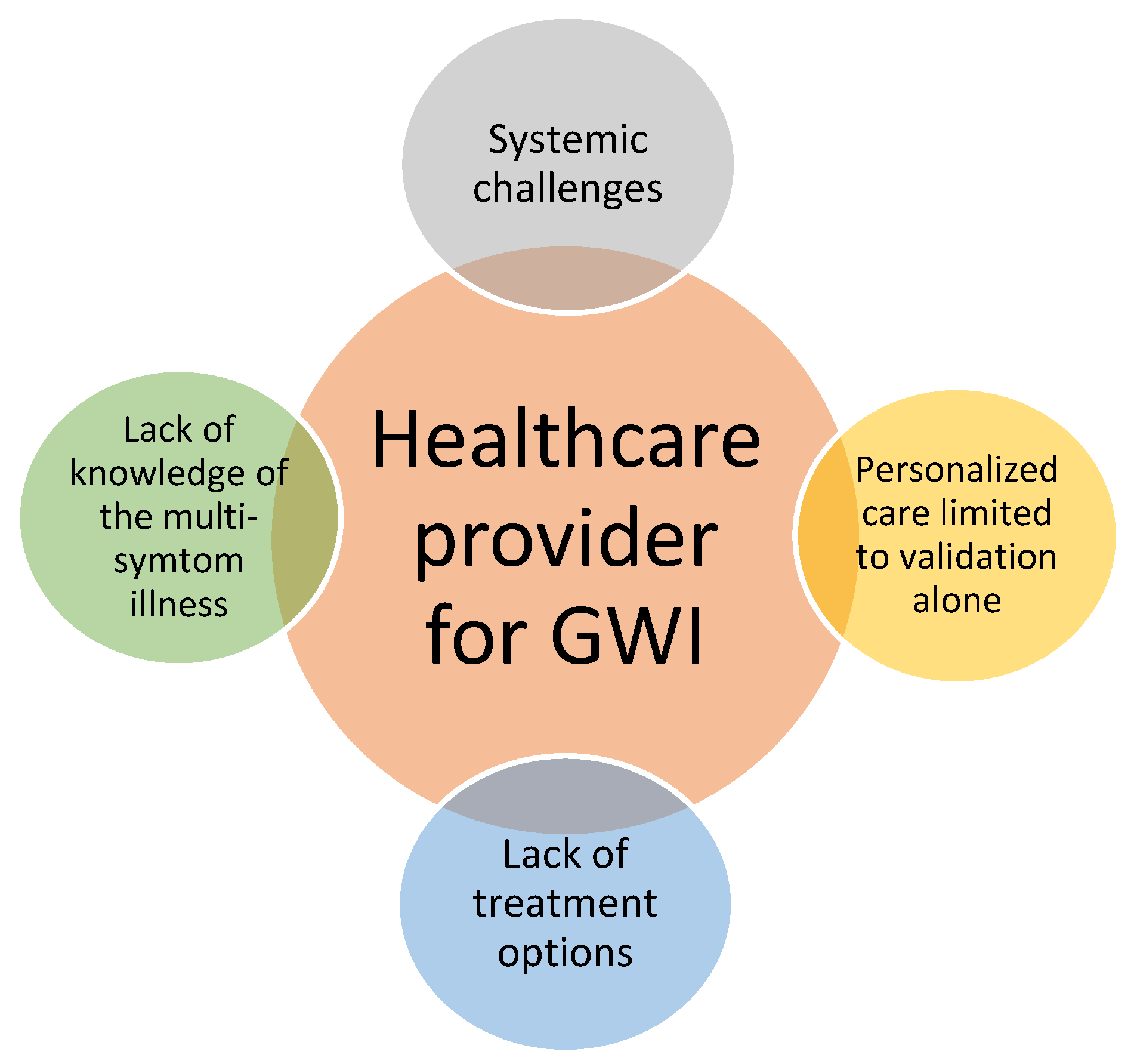
3.1. Gaps in Knowledge of the Multisymptom Illness
“There is a kind of general sense that it might have something to do with toxic exposures, that many of these soldiers, many of these active duty service members were exposed to burning oil wells and burning pits and they may have inhaled something toxic.” (White, male, physician)
“It’s hard to look at, you know… a syndrome when no one is like, you know saying, this is the cause. You know? You know it’s still even hard now to talk about what it is, and what is it going to turn into.” (White, female, psychologist)
“We have no way of knowing, ah, whether there’s a causal relationship with these exposures.” (White, male, physician)
“Most people don’t know for sure [about the exposures]. And a small number of people when they say yes, you know, they really are not aware of what they are saying.” (Asian, female, physician)
“Most healthcare providers do not know. It’s less understood than it was. The information that we know is not getting down to the clinicians.” (White, female, pharmacologist)
“Sometimes it’s difficult to sift out what are the symptoms, like mood symptoms are related to trauma or they are related to toxic exposure, or does the toxic exposure put somebody at higher risk to be susceptible to trauma, you know, it’s really hard to disentangle and understand all these things.” (White, female, psychologist)
3.2. Limited Treatment Options
“There are no Food and Drug Administration (FDA)-approved treatments for Gulf War illness. So even if they were identified, right now you’re just kind of piecemeal treating the symptoms. So maybe you’re treating the mood symptoms, maybe you’re treating the chronic pain, maybe you’re treating the skin rashes, so that’s [a] barrier to care that we don’t have any FDA-approved treatments.” (White, female, psychologist)
“I think that they are being treated… not holistically, but they’ll go in and say, hey, you know I’ve got stomach problems, and they’re just addressing that, they’re not looking at their overall whole-body condition.” (White, female, social worker)
“We kind of approach things symptomatically. As far as I know that’s kind of the approach people take. You know, if they have pain, you try to give medications that are good for chronic pain. If they have problems concentrating, you can give them kind of medication that boosts their concentration.” (White, male, physician)
“When I was doing my acupuncture points, I treated the whole organ. Not just anti-inflammatory, and analgesic, not just that. I treated the whole organ.” (Asian, female, nurse and acupuncturist)
“Right now, it’s a confusing process for the acupuncturists to get compensated and a lot of the VAs don’t even tell people that they can be compensated, so it’s really a payment thing.” (White, female, sociologist)
3.3. Challenges in Personalizing Care
“There’s going to be genetic differences in susceptibility. So, some people may be more susceptible to the toxins they were exposed to, to present certain symptoms, as opposed to others.” (White, female, pharmacologist)
“Yea, I think women in the military who have GWI is more complicated because of the hormone balance. Hormones have a big thing to do with a lot of their symptoms. It aggravates them. You know men have this androgen and estrogen issues thing too, but I think it’s easier for men.” (Asian, female, nurse and acupuncturist)
“We are running into a lot of osteoarthritis. That’s probably the main thing in the pain study. A lot of people are running into a lot of cognitive problems and it’s hard to say if its due to aging or if you know, it’s accelerated the aging process, um, so yeah.” (White, male, physician)
“No one’s been there to listen to them about all these problems that they’re facing, you know they kind of go to a separate doctor for each ailment that they have and that’s really problematic.” (White, female, psychologist)
“Some kind of standard way of validating you know, ‘even if there is nothing we can do for you, we acknowledge that this happened. And, um, that you are struggling with symptoms.’ I think that would go a long way. I think the impulse is to say, well I don’t know what to do so let’s not talk about it. Um, and so… some kind of psychological approach to what is going on may be helpful in the absence of being able to kind of attack the root causes of the biological problems.” (White, male, physician)
3.4. Systemic Issues
“I’m not sure that I would say that it’s real, because I don’t think we really know what it is. And I think there are some people who are pretty skeptical of it… no specific pathology has been proven.” (White, male, physician)
“I think because of the early beginnings of skepticism, an awful lot of VA providers still don’t believe it or don’t have the education to know that it’s real or even know what it is.” (White, female, pharmacologist)
“I just feel like there’s, you know, it’s been so limited in the ability to, you know, to have people, even be willing to open up to the idea that this exists. And so, for me anyway, we’ve, you know, I’ve been to meetings where people have basically said to me, ‘oh you’re lying, ok move on’.” (White, female, psychologist)
“So, in the VA we use a computerized patient record system or CPRS and it lists the problems that the patient has, it lists the diagnoses. I can’t recall seeing on a list of diagnoses Gulf War illness.” (White, male, physician)
“So, and it’s not clear to me what the benefits for the patient are to have a Gulf War designation, though maybe it changes their service connection which could be helpful to a patient, but I don’t actually know that… it doesn’t do anything for the patient in terms of entitlement and it doesn’t do anything for the patient in terms of treatment.” (White, male, physician)
“The information we know is not getting down to the clinicians. There’s some lack of communication between what’s happening in congress and what filters down to the VA and what filters down to the healthcare system versus the benefits system, because benefits are separate than the healthcare system. There’s a roadblock.” (White, female, pharmacologist)
“We have research, but it’s just getting it out to people… There is also a lack of consistency across VAs, that everybody talks about. The best analogy I’ve heard is that they’re like little fiefdoms, which they are; they have different policies and different things going on within each of them… and so some more shared systems across VAs would make it easier to have quality programs.” (White, female, sociologist)
“The overwhelming thing is they have been ignored by the system.” (White, male, physician)
“[Gulf War veterans] are kind of like the invisible veterans.” (White, female, social worker)
“I think that… the biggest problem early on was that no one believed them. And, that it was harder and harder to find people that looked at it as a global disorder, right?” (White, female, pharmacologist)
“I know, these vets had a lot of trouble even getting recognized as a syndrome and then, the history of the military is a history of not wanting to, once something is labelled you have to do something about it.” (White, female, sociologist)
“I’d like to know more about treatment. What has been considered successful. I know they are doing a study up there in Waco to see if maybe there’s certain medications that might help some of the symptoms. So, I would like to know more about medical treatment for it.” (White, female, social worker)
“So, from a curiosity standpoint and from future tracking and studies, it would be helpful I think if they came in with DEET exposure or uranium exposure or oil field exposure or whatever else that would be helpful for tracking and for my own curiosity, but not necessary, not necessary for a good acupuncture physician.” (White, male, acupuncturist)
“It would be nice if the ones who have to deal with the veteran care, if they know a little bit more. It would be, I mean not little bit, as much as they can.” (Asian, female, physician)
“I think that a lot the education for providers needs to be about you know kind of slowing down and trying to figure out if this could be more of an overarching diagnosis that’s missing in their clinical picture. And then, you know, how to explain that to them like that they’ve been living with this for however many years and it’s just recognized now.” (Asian, female, psychologist)
“Oh definitely online… I guess some sort of forums, yeah, or training protocols, education forums to share more further ideas, case study you know stuff like that. (White, male, acupuncturist)
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Semi-Structured Interview Protocol
- ○
- Could you tell us about yourself and your experiences treating veterans with Gulf War illness?
- ○
- What would you say are the clinical features of Gulf War illness?
- ○
- What are some symptoms you see in patients?
- ○
- Have these symptoms changed over time?
- ○
- What (if any) clinical difference have you seen in patient symptoms based on age, gender, race/ethnicity, and type of exposure?
- ○
- How do you think Gulf War illness affects patients’ relationships with peers, friends, and family members?
- ○
- How do you think Gulf War illness affects patients’ ability to work?
- ○
- What kind of medical care do veterans with Gulf War illness receive?
- ○
- What kinds of specialized treatments are available for veterans with Gulf War illness?
- ○
- What has been your experience with insurance companies and other healthcare providers serving patients with Gulf War illness?
- ○
- Are there any barriers to care that you feel are unique to the population with Gulf War illness?
- ○
- Are there any opportunities for care that you feel are unique to the population with Gulf War illness?
- ○
- What type of access to information do you have about the latest treatments and clinical trials for Gulf War illness?
- ○
- What kinds of support and resources do you have at present to serve veterans with Gulf War illness?
- ○
- What kinds of support and resources would you like to see offered?
- ○
- What do you think are effective ways to educate healthcare providers about Gulf War illness?
- What should we (researchers) look for going forward? Is there anything that we did not ask that you’d like to tell us about?
References
- Maule, A.L.; Janulewicz, P.A.; Sullivan, K.A.; Krengel, M.H.; Yee, M.K.; McClean, M.; White, R.F. Meta-analysis of self-reported health symptoms in 1990–1991 Gulf War and Gulf War-era veterans. BMJ Open 2018, 8, e016086. [Google Scholar] [CrossRef] [PubMed]
- White, R.F.; Steele, L.; O’Callaghan, J.P.; Sullivan, K.; Binns, J.H.; Golomb, B.A.; Bloom, F.E.; Bunker, J.A.; Crawford, F.; Graves, J.C.; et al. Recent research on Gulf War illness and other health problems in veterans of the 1991 Gulf War: Effects of toxicant exposures during deployment. Cortex 2016, 74, 449–475. [Google Scholar] [CrossRef] [PubMed]
- Mawson, A.; Croft, A. Gulf War Illness: Unifying hypothesis for a continuing health problem. Int. J. Environ. Res. Public Health 2019, 16, 111. [Google Scholar] [CrossRef] [PubMed]
- Iversen, A.; Chalder, T.; Wessely, S. Gulf War Illness: Lessons from medically unexplained symptoms. Clin. Psychol. Rev. 2007, 27, 842–854. [Google Scholar] [CrossRef] [PubMed]
- Department of Defense. Gulf War Illness Research Program. 2016. Available online: https://cdmrp.army.mil/gwirp/default (accessed on 7 January 2000).
- Greenberg, L.M.; Litke, D.R.; Ray, K.; Rath, J.F.; Pigeon, W.R.; Helmer, D.A.; Anastasides, N.; McAndrew, L.M. Developing a problem-solving treatment for gulf war illness: Cognitive rehabilitation of veterans with complex post-deployment health concerns. Clin. Soc. Work J. 2018, 46, 100–109. [Google Scholar] [CrossRef]
- United States Government Accountability Office. Gulf War Illness: Improvements Needed for VA to Better Understand, Process, and Communicate Decisions on Claims. 2017. Available online: https://www.gao.gov/assets/690/685562 (accessed on 7 January 2000).
- Kuehn, B.M. Gulf War illness defined. JAMA 2014, 311, 1603. [Google Scholar] [CrossRef]
- Fukuda, K.; Nisenbaum, R.; Stewart, G. Chronic multisymptom illness affecting Air Force veterans of the Gulf War. JAMA 1998, 280, 981–988. [Google Scholar] [CrossRef] [PubMed]
- Steele, L. Prevalence and patterns of Gulf War illness in Kansas veterans: Association of symptoms with characteristics of person, place, and time of military service. Am. J. Epidemiol. 2000, 152, 992–1002. [Google Scholar] [CrossRef] [PubMed]
- Haley, R.W.; Kurt, T.L.; Hom, J. Is there a Gulf War syndrome? Searching for syndromes by factor analysis of symptoms. J. Am. Med. Assoc. 1997, 277, 215–222. [Google Scholar] [CrossRef]
- Kerr, K.J. Gulf War illness: An overview of events, most prevalent health outcomes, exposures, and clues as to pathogenesis. Rev. Environ. Health 2015, 30, 273–286. [Google Scholar] [CrossRef] [PubMed]
- Kilshaw, S. Gulf War Syndrome: A reaction to psychiatry’s invasion of the military? Cult. Med. Psychiatry 2008, 32, 219–237. [Google Scholar] [CrossRef] [PubMed]
- Nettleman, M. Gulf war illness: Challenges persist. Trans. Am. Clin. Climatol. Assoc. 2015, 126, 237. [Google Scholar] [PubMed]
- Research Advisory Committee on Gulf War Veterans’ Illnesses. Gulf War Illness and the Health of Gulf War Veterans. Scientific Findings and Recommendations; U.S. Government Printing Office: Washington, DC, USA, 2008. [Google Scholar]
- Golomb, B.A. A Review of the Scientific Literature as it Pertains to Gulf War Illnesses: Volume 2: Pyridostigmine Bromide; RAND Corporation: Santa Monica, CA, USA, 1999. [Google Scholar]
- Steele, L.; Lockridge, O.; Gerkovich, M.M.; Cook, M.R.; Sastre, A. Butyrylcholinesterase genotype and enzyme activity in relation to Gulf War illness: Preliminary evidence of gene-exposure interaction from a case-control study of 1991 Gulf War veterans. Environ. Health 2015, 14, 4. [Google Scholar] [CrossRef] [PubMed]
- Golomb, B.A. Acetylcholinesterase inhibitors and Gulf War illnesses. Proc. Natl. Acad. Sci. USA 2008, 105, 4295–4300. [Google Scholar] [CrossRef]
- Heng, H.H. Challenges and new strategies for gulf war illness research. Environ. Dis. 2016, 1, 118. [Google Scholar] [CrossRef]
- Department of Veterans Affairs. War Related Illness and Injury Study Center. 2018. Available online: https://www.warrelatedillness.va.gov/education/factsheets/gulf-war-illness-for-providers.pdf (accessed on 25 April 2000).
- Department of Veterans Affairs/Department of Defense. VA/DoD Clinical Practice Guidelines for the Management of Chronic Multisymptom Illness. 2014. Available online: https://www.healthquality.va.gov/guidelines/MR/cmi/VADoDCMICPG2014.pdf (accessed on 25 April 2000).
- Conboy, L.; Gerke, T.; Hsu, K.-Y.; St John, M.; Goldstein, M.; Schnyer, R. The effectiveness of individualized acupuncture protocols in the treatment of Gulf War illness: A pragmatic randomized clinical trial. PLoS ONE 2016. [Google Scholar] [CrossRef] [PubMed]
- Golomb, B.A.; Allison, M.; Koperski, S.; Koslik, H.J.; Devaraj, S.; Ritchie, J.B. Coenzyme Q10 benefits symptoms in Gulf War veterans: Results of a randomized double-blind study. Neural Comput. 2014, 26, 2594–2651. [Google Scholar] [CrossRef] [PubMed]
- Department of Defense. The Gulf War Illness Landscape. 2018. Available online: https://cdmrp.army.mil/gwirp/pdfs/GWIRP_Landscape.pdf (accessed on 25 April 2000).
- Minshall, D. Gulf War Syndrome: A review of current knowledge and understanding. J. R. Naval Med. Serv. 2014, 100, 252–258. [Google Scholar]
- Corbin, J.; Strauss, A. Strategies for qualitative data analysis. In Basics of Qualitative Research. Techniques and Procedures for Developing Grounded Theory; Sage: London, UK, 2008; Volume 3. [Google Scholar]
- Kentor, J.; Jorgenson, A.K.; Kick, E. The “new” military and income inequality: A cross national analysis. Soc. Sci. Res. 2012, 41, 514–526. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kaimal, G.; Dieterich-Hartwell, R. Grappling with Gulf War Illness: Perspectives of Gulf War Providers. Int. J. Environ. Res. Public Health 2020, 17, 8574. https://doi.org/10.3390/ijerph17228574
Kaimal G, Dieterich-Hartwell R. Grappling with Gulf War Illness: Perspectives of Gulf War Providers. International Journal of Environmental Research and Public Health. 2020; 17(22):8574. https://doi.org/10.3390/ijerph17228574
Chicago/Turabian StyleKaimal, Girija, and Rebekka Dieterich-Hartwell. 2020. "Grappling with Gulf War Illness: Perspectives of Gulf War Providers" International Journal of Environmental Research and Public Health 17, no. 22: 8574. https://doi.org/10.3390/ijerph17228574
APA StyleKaimal, G., & Dieterich-Hartwell, R. (2020). Grappling with Gulf War Illness: Perspectives of Gulf War Providers. International Journal of Environmental Research and Public Health, 17(22), 8574. https://doi.org/10.3390/ijerph17228574



