Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments
Abstract
1. Introduction
2. Materials and Methods
3. Parameter Constraints
3.1. Particle Size
3.2. Particle Emissions and Vocalization
3.3. Viral Load
3.4. Virus Lifetime in Aerosol
3.5. Particle Deposition Probability
3.6. Face Mask Efficiency
3.7. Infective Dose D50
4. Results
4.1. Office Environment
4.2. Classroom Environment
4.3. Choir Practice
4.4. Reception
4.5. Cluster Infections
5. Discussion
5.1. Uncertainties
5.2. Reducing Infection Risk
5.3. Infectiousness and Superspreading
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Cai, J.; Sun, W.; Huang, J.; Gamber, M.; Wu, J.; He, G. Indirect Virus Transmission in Cluster of COVID-19 Cases, Wenzhou, China. Emerg. Infect. Dis. 2020, 26, 1343. [Google Scholar] [CrossRef]
- Jayaweera, M.; Perera, H.; Gunawardana, B.; Manatunge, J. Transmission of COVID-19 virus by droplets and aerosols: A critical review on the unresolved dichotomy. Environ. Res. 2020, 188, 109819. [Google Scholar] [CrossRef] [PubMed]
- European Centre for Disease Prevention and Control. Available online: https://www.ecdc.europa.eu/en/covid-19/latest-evidence/transmission (accessed on 18 October 2020).
- Lloyd-Smith, J.O.; Schreiber, S.J.; Kopp, P.E.; Getz, W.M. Superspreading and the effect of individual variation on disease emergence. Nature 2005, 438, 355–359. [Google Scholar] [CrossRef] [PubMed]
- Tellier, R.; Li, Y.; Cowling, B.J.; Tang, J.W. Recognition of aerosol transmission of infectious agents: A commentary. BMC Infect. Dis. 2019, 19, 101. [Google Scholar] [CrossRef] [PubMed]
- Nishiura, H.; Oshitani, H.; Kobayashi, T.; Saito, T.; Sunagawa, T.; Matsui, T.; Wakita, T.; Suzuki, M.; MHLW COVID-19 Response Team. Closed environments facilitate secondary transmission of coronavirus disease 2019 (COVID-19). medRxiv 2020. Available online: https://www.medrxiv.org/content/10.1101/2020.02.28.20029272v2 (accessed on 14 October 2020).
- Morawska, L.; Milton, D.K. It is time to address airborne transmission of COVID-19. Clin. Infect. Dis. 2020, 6, ciaa939. [Google Scholar] [CrossRef]
- Zhang, R.; Li, Y.; Zhang, A.L.; Wang, Y.; Molina, M.J. Identifying airborne transmission as the dominant route for the spread of COVID-19. Proc. Natl. Acad. Sci. USA 2020, 117, 14857–14863. [Google Scholar] [CrossRef]
- Auger, K.A.; Shah, S.S.; Richardson, T.; Hartley, D.; Hall, M.; Warniment, A.; Timmons, K.; Bosse, D.; Ferris, S.A.; Brady, P.W.; et al. Association between statewide school closure and COVID-19 incidence and mortality. JAMA 2020, 324, 859–870. [Google Scholar] [CrossRef]
- Wölfel, R.; Corman, V.M.; Guggemos, W.; Seilmaier, M.; Zange, S.; Müller, M.A.; Niemeyer, D.; Jones, T.C.; Vollma, P.; Rothe, C.; et al. Virological assessment of hospitalized patients with COVID-2019. Nature 2020, 581, 465–469. [Google Scholar] [CrossRef]
- Jones, T.C.; Mühlemann, B.; Veith, T.; Zuchowski, M.; Hofmann, J.; Stein, A.; Edelmann, A.; Corman, V.M.; Drosten, C. An analysis of SARS-CoV-2 viral load by patient age. medRxiv 2020. [Google Scholar] [CrossRef]
- Jacot, D.; Greub, G.; Jaton, K.; Opota, O. Viral load of SARS-1 CoV-2 across patients and compared to other respiratory viruses. Microbes Infect. 2020. [Google Scholar] [CrossRef] [PubMed]
- Davies, N.G.; Klepac, P.; Liu, Y.; Prem, K.; Jit, M.; Eggo, R.M.; CMMID COVID-19 Working Group. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat. Med. 2020, 26, 1205–1211. [Google Scholar] [CrossRef] [PubMed]
- Mizumoto, K.; Omori, R.; Nishiura, H. Age specificity of cases and attack rate of novel coronavirus disease (COVID-19). medRxiv 2020. Available online: https://www.medrxiv.org/content/10.1101/2020.03.09.20033142v1 (accessed on 14 October 2020).
- Viner, R.M.; Russell, S.J.; Croker, H.; Packer, J.; Ward, J.; Stansfield, C.; Mytton, O.; Bonell, C.; Booy, R. School closure and management practices during coronavirus outbreaks including COVID-19: A rapid systematic review. Lancet Child Adolesc. Health 2020, 4, 397–404. [Google Scholar] [CrossRef]
- Klompas, M.; Baker, M.A.; Rhee, C. Airborne Transmission of SARS-CoV-2 Theoretical Considerations and Available Evidence. JAMA 2020, 324, 441–442. [Google Scholar] [CrossRef]
- Howard-Reed, C.; Wallace, L.A.; Ott, W.R. The effect of opening windows on air change rates in two homes. J. Air Waste Manag. Assoc. 2011, 52, 147–159. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.; Ma, N.; Witt, C.; Rapp, S.; Wild, P.; Andreae, M.O.; Pöschl, U.; Su, H. Distinct regimes of particle and virus abundance explain face mask efficacy for COVID-19. medRxiv 2020. Available online: https://www.medrxiv.org/content/10.1101/2020.09.10.20190348v1 (accessed on 14 October 2020).
- Johnson, G.R.; Morawska, L.; Ristovski, Z.D.; Hargreaves, M.; Mengersen, K.; Chao, C.Y.H.; Wan, M.P.; Li, Y.; Xie, X.; Katoshevski, D.; et al. Modality of human expired aerosol size distributions. J. Aerosol Sci. 2011, 42, 839–851. [Google Scholar] [CrossRef]
- Yan, J.; Grantham, M.; Pantelic, J.; De Mesquita, P.J.B.; Albert, B.; Liu, F.; Ehrman, S.; Milton, D.K.; EMIT Consortium. Infectious virus in exhaled breath of symptomatic seasonal influenza cases from a college community. Proc. Natl. Acad. Sci. USA 2018, 115, 1081–1086. [Google Scholar] [CrossRef]
- Asadi, S.; Wexler, A.S.; Cappa, C.D.; Santiago Barreda, S.; Bouvier, N.M.; Ristenpart, W.D. Aerosol emission and superemission during human speech increase with voice loudness. Sci. Rep. 2019, 9, 2348. [Google Scholar] [CrossRef]
- Borak, J. Airborne transmission of COVID-19. Occup. Med. 2020, 70, 297–299. [Google Scholar] [CrossRef] [PubMed]
- Vuorinen, V.; Aarnio, M.; Alava, M.; Alopaeus, V.; Atanasova, N.; Auvinen, M.; Balasubramanian, N.; Bordbar, H.; Erasto, P.; Grande, R.; et al. Modelling aerosol transport and virus exposure with numerical simulations in relation to SARS-CoV-2 transmission by inhalation indoors. Saf. Sci. 2020, 130, 104866. [Google Scholar] [CrossRef]
- Morawska, L.; Johnson, G.R.; Ristovski, Z.D.; Hargreaves, M.; Mengersen, K.; Corbett, S.; Chao, C.Y.H.; Li, Y.; Katoshevski, D. Size distribution and sites of origin of droplets expelled from the human respiratory tract during expiratory activities. J. Aerosol Sci. 2009, 40, 256–269. [Google Scholar] [CrossRef]
- Gregson, F.K.A.; Watson, N.A.; Orton, C.M.; Haddrell, A.E.; McCarthy, L.P.; Finnie, T.J.R.; Gent, N.; Donaldson, G.C.; Shah, P.L.; Calder, J.D.; et al. Comparing the Respirable Aerosol Concentrations and Particle Size Distributions Generated by Singing, Speaking and Breathing. ChemRxiv 2020. [Google Scholar] [CrossRef]
- Asadi, S.; Wexler, A.S.; Cappa, C.D.; Barreda, S.; Bouvier, N.M.; Ristenpart, W.D. Effect of voicing and articulation manner on aerosol particle emission during human speech. PLoS ONE 2020, 15, e0227699. [Google Scholar] [CrossRef]
- Mürbe, D.; Fleischer, M.; Lange, J.; Rotheudt, H.; Kriegel, M. Aerosol emission is increased in professional singing. Preprint 2020. [Google Scholar] [CrossRef]
- Riediker, M.; Tsai, D.-H. Estimation of viral aerosol emissions from simulated individuals with asymptomatic to moderate Coronavirus disease 2019. JAMA Netw. Open 2020, 3, e2013807. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, M.O.; Thomas, R.J.; Garton, N.J.; Hudson, A.; Haddrell, A.; Reid, J.R. Assessing the airborne survival of bacteria in populations of 10 aerosol droplets with a novel technology. J. Roy. Soc. Int. 2019, 16, 20180779. [Google Scholar] [CrossRef]
- Lauer, S.A.; Grantz, K.H.; Bin, Q.; Jones, F.K.; Zheng, Q.; Meredith, H.R.; Azman, A.S.; Reich, N.G.; Lessler, J. The Incubation Period of Coronavirus Disease 2019 (COVID-19) from publicly reported confirmed cases: Estimation and application. Ann. Intern. Med. 2020, 172, 577–582. [Google Scholar] [CrossRef]
- Arons, M.M.; Hatfield, K.M.; Reddy, S.C.; Kimball, A.; James, A.; Jacobs, J.R.; Taylor, J.; Spicer, K.; Bardossy, A.C.; Oakley, L.P.; et al. For the Public Health–Seattle and King County and CDC COVID-19 Investigation Team 2020. Presymptomatic SARS-CoV-2 infections and transmission in a skilled nursing facility. N. Engl. J. Med. 2020, 382, 2081–2090. [Google Scholar] [CrossRef]
- Argyropoulos, K.V.; Serrano, A.; Hu, J.; Black, M.; Feng, X.; Shen, G.; Call, M.; Kim, M.J.; Lytle, A.; Belovarac, B.; et al. Association of initial viral load in severe acute respiratory syndrome Coronavirus 2 (SARS-CoV-2) patients with outcome and symptoms. Am. J. Pathol. 2020, 190, 1881–1887. [Google Scholar] [CrossRef]
- Buitrago-Garcia, D.; Egli-Gany, D.; Counotte, M.J.; Hossmann, S.; Imeri, H.; Ipekci, M.A.; Salanti, G.; Low, N. Asymptomatic SARS-CoV-2 infections: A living systematic review and meta-analysis. medRxiv 2020. [Google Scholar] [CrossRef]
- Pan, Y.; Zhang, D.; Yang, P.; Poon, L.L.M.; Wang, Q. Viral load of SARS-CoV-2 in clinical samples. Lancet Infect. Dis. 2020, 20, 411–412. [Google Scholar] [CrossRef]
- Pujadas, E.; Chaudhry, F.; McBride, R.; Richter, F.; Zhao, S.; Wajnberg, A.; Nadkarni, G.; Glicksberg, B.S.; Houldsworth, J.; Cordon-Card, C. SARS-CoV-2 viral load predicts COVID-19 mortality. Lancet Respir. Med. 2020, 8. [Google Scholar] [CrossRef]
- To, K.K.-W.; Tsang, O.T.-Y.; Leung, W.-S.; Tam, A.R.; Wu, T.-C.; Lung, D.C.; Yip, C.C.-Y.; Cai, J.-P.; Chan, J.M.-C.; Chik, T.S.-H.; et al. Temporal profiles of viral load in posterior oropharyngeal saliva samples and serum antibody responses during infection by SARS-CoV-2: An observational cohort study. Lancet Infect. Dis. 2020, 20, 565–574. [Google Scholar] [CrossRef]
- Yu, X.; Sun, S.; Shi, Y.; Wang, H.; Zhao, R.; Sheng, J. SARS-CoV-2 viral load in sputum correlates with risk of COVID-19 progression. Crit. Care 2020, 24, 170. [Google Scholar] [CrossRef]
- He, X.; Lau, E.H.Y.; Wu, P.; Deng, X.; Wang, J.; Hao, X.; Lau, Y.C.; Wong, J.Y.; Guan, Y.; Tan, X.; et al. Temporal dynamics in viral shedding and transmissibility of COVID-19. Nat. Med. 2020, 26, 672–675. [Google Scholar] [CrossRef]
- Hamner, L.; Dubbel, P.; Capron, I.; Ross, A.; Jordan, A.; Lee, J.; Lynn, J.; Ball, A.; Narwal, S.; Russell, S.; et al. High SARS-CoV-2 Attack Rate Following Exposure at a Choir Practice—Skagit County, Washington, March 2020. MMWR 2020, 69, 606–610. [Google Scholar] [CrossRef]
- Miller, S.L.; Nazaroff, W.W.; Jimenez, J.L.; Boerstra, A.; Buonanno, G.; Dancer, S.J.; Kurnitski, J.; Marr, L.C.; Morawska, L.; Noakes, C. Transmission of SARS-CoV-2 by inhalation of respiratory aerosol in the Skagit Valley Chorale superspreading event. medRxiv 2020. [Google Scholar] [CrossRef]
- Van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I.; et al. Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. N. Engl. J. Med. 2020, 382, 1564–1567. [Google Scholar] [CrossRef]
- Smither, S.J.; Eastaugh, L.S.; Findlay, J.S.; Lever, M.S. Experimental aerosol survival of SARS-CoV-2 in artificial saliva and tissue culture media at medium and high humidity. Emerg. Microbes Infect. 2020, 9. [Google Scholar] [CrossRef]
- Pyankov, O.V.; Bodnev, S.A.; Pyankova, O.; Agranovski, I.E. Survival of aerosolized coronavirus in the ambient air. Aerosol Sci. Technol. 2018, 115, 158–163. [Google Scholar] [CrossRef]
- Casanova, L.M.; Jeon, S.; Rutala, W.A.; Weber, D.J.; Sobsey, M.D. Effects of air temperature and relative humidity on coronavirus survival on surfaces. Appl. Environ. Microbiol. 2010, 76, 2712–2717. [Google Scholar] [CrossRef]
- Wang, B.; Wu, H.; Wan, X.-F. Transport and fate of human expiratory droplets—A modeling approach. Phys. Fluids 2020, 32, 083307. [Google Scholar] [CrossRef]
- Spena, A.; Palombi, L.; Corcione, M.; Carestia, M.; Spena, V.A. On the optimal indoor air conditions for SARS-CoV-2 Inactivation. An enthalpy-based approach. Int. J. Environ. Res. Publ. Health 2020, 17, 6083. [Google Scholar] [CrossRef]
- Liu, L.; Wei, J.; Li, Y.; Ooi, A. Evaporation and dispersion of respiratory droplets from coughing. Indoor Air 2017, 27, 179–190. [Google Scholar] [CrossRef]
- De Gabory, L.; Alharbia, A.; Kérimiana, M.; Lafonc, M.-E. The influenza virus, SARS-CoV-2, and the airways: Clarification for the otorhinolaryngologist. Eur. Ann. Otorhinolaryngol. Head Neck Dis. 2020, 137, 291–296. [Google Scholar] [CrossRef]
- Inthavong, K.; Ge, Q.J.; Li, X.D.; Tu, J.T. Detailed predictions of particle aspiration affected by respiratory inhalation and airflow. Atmos. Environ. 2012, 62, 107–117. [Google Scholar] [CrossRef]
- Dong, J.; Shang, Y.; Tian, L.; Inthavong, K.; Qiu, D.; Tu, J. Ultrafine particle deposition in a realistic human airway at multiple inhalation scenarios. Int. J Numer. Methods Biomed. Eng. 2019, 35, e3215. [Google Scholar] [CrossRef] [PubMed]
- Stahlhofen, W.; Rudolf, G.; James, A.C. Intercomparison of experimental regional aerosol deposition data. J. Aerosol Med. 1989, 2, 285–308. [Google Scholar] [CrossRef]
- Asgharian, B.; Hofmann, W.; Bergmann, R. Particle deposition in a multiple-path model of the human lung. Aer. Sci. Technol. 2010, 34, 332–339. [Google Scholar] [CrossRef]
- Heyder, J. Deposition of inhaled particles in the human respiratory tract and consequences for regional targeting in respiratory drug delivery. Proc. Am. Thorac. Soc. 2004, 1, 315–320. [Google Scholar] [CrossRef]
- Tsuda, A.; Henry, F.S.; Butler, J.P. Particle transport and deposition: Basic physics of particle kinetics. Compr. Physiol. 2015, 3, 1437–1471. [Google Scholar]
- Montoya, L.D.; Lawrence, J.; Krishna Murthy, G.G.; Sarnat, J.A.; Godleski, J.J.; Koutrakis, P. Continuous measurements of ambient particle deposition in human subjects. Aerosol Sci. Technol. 2004, 38, 980–990. [Google Scholar] [CrossRef]
- Hsiao, T.-C.; Chuang, H.-C.; Griffith, S.M.; Chen, S.-J.; Young, L.H. COVID-19: An aerosol’s point of view from expiration to transmission to viral-mechanism. Aerosol Air Qual. Res. 2020, 20, 905–910. [Google Scholar] [CrossRef]
- Lukassen, S.; Chua, R.L.; Trefzer, T.; Kahn, N.C.; Schneider, M.A.; Muley, T.; Winter, H.; Meister, M.; Veith, C.; Boots, A.W.; et al. SARS-CoV-2 receptor ACE2 and TMPRSS2 are primarily expressed in bronchial transient secretory cells. EMBO J. 2020, 39, e105114. [Google Scholar] [CrossRef]
- Chu, D.K.; Akl, E.A.; Duda, S.; Solo, K.; Yaacoub, S.; Schünemann, H.J.; On Behalf of the COVID-19 Systematic Urgent Review Group Effort (SURGE) Study Authors. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: A systematic review and meta-analysis. Lancet 2020, 395, 1973–1987. [Google Scholar] [CrossRef]
- Esposito, S.; Principi, N.; Leung, C.C.; Migliori, G.B. Universal use of face masks for success against COVID-19: Evidence and implications for prevention policies. Eur. Respir. J. 2020, 55, 2001260. [Google Scholar] [CrossRef]
- Fischer, E.P.; Fischer, M.C.; Grass, D.; Henrion, I.; Warren, W.S.; Westman, E. Low-cost measurement of facemask efficacy for filtering expelled droplets during speech. Sci. Adv. 2020, 6, eabd3083. [Google Scholar] [CrossRef]
- Howard, J.; Huang, A.; Li, Z.; Tufekci, Z.; Zdimal, V.; Van der Westhuizen, H.; Von Delft, A.; Price, A.; Fridman, L.; Tang, L.; et al. Face Masks Against COVID-19: An Evidence Review. Preprints 2020, 2020040203. Available online: https://www.preprints.org/manuscript/202004.0203/v1 (accessed on 14 October 2020).
- Leung, N.H.L.; Chu, D.K.W.; Shiu, E.Y.C.; Chan, K.-H.; McDevitt, J.J.; Hau, B.J.P.; Yen, H.-L.; Li, Y.; Ip, D.K.M.; Peiris, J.S.M.; et al. Respiratory virus shedding in exhaled breath and efficacy of face masks. Nat. Med. 2020, 26, 676–680. [Google Scholar] [CrossRef]
- MacIntyre, C.R.; Chughtai, A.A. A rapid systematic review of the efficacy of face masks and respirators against coronaviruses and other respiratory transmissible viruses for the community, healthcare workers and sick patients. Int. J. Nurs. Stud. 2020, 108, 103629. [Google Scholar] [CrossRef]
- Worby, C.J.; Chang, H.-H. Face mask use in the general population and optimal resource allocation during the COVID-19 pandemic. Nat. Commun. 2020, 11, 4049. [Google Scholar] [CrossRef]
- Mueller, A.V.; Eden, M.J.; Oakes, J.M.; Bell, C.; Fernandez, L.A. Quantitative method for comparative assessment of particle filtration efficiency of fabric masks as alternatives to standard surgical masks for PPE. medRxiv 2020. Available online: https://www.medrxiv.org/content/10.1101/2020.04.17.20069567v4 (accessed on 14 October 2020).
- Verma, S.; Dhanak, M.; Frankenfield, J. Visualizing the effectiveness of face masks in obstructing respiratory jets. Phys. Fluids 2020, 32, 061708. [Google Scholar] [CrossRef] [PubMed]
- Drewnick, F.; Pikmann, J.; Fachinger, F.; Moormann, L.; Sprang, F.; Borrmann, S. Aerosol filtration efficiency of household materials for homemade face masks: Influence of material properties, particle size, particle electrical charge, face velocity, and leaks. Aerosol Sci. Technol. 2020. [Google Scholar] [CrossRef]
- Davies, A.; Thompson, K.-A.; Giri, K.; Kafatos, G.; Walker, J.; Bennett, A. Testing the efficacy of homemade masks: Would they protect in an influenza pandemic? Disaster Med. Public Health Prep. 2013, 7, 413–418. [Google Scholar] [CrossRef] [PubMed]
- Shakya, K.M.; Noyes, A.; Kallin, R.; Peltie, R.E. Evaluating the efficacy of cloth facemasks in reducing particulate matter exposure. J. Expo. Sci. 2017, 27, 352–357. [Google Scholar] [CrossRef]
- Kai, D.; Goldstein, G.-P.; Morgunov, A.; Nangalia, V.; Rotkirch, A. Universal masking is urgent in the COVID-19 pandemic: SEIR and agent based models, empirical validation, policy recommendations. arXiv 2020, arXiv:2004.13553. Available online: https://arxiv.org/abs/2004.13553 (accessed on 14 October 2020).
- Watanabe, T.; Bartrand, T.A.; Weir, M.H.; Omura, T.; Haas, C.N. Development of a dose-response model for SARS Coronavirus. Risk Anal. 2010, 30, 1129–1138. [Google Scholar] [CrossRef]
- Schröder, I. COVID-19: A risk assessment perspective. Chem. Health Saf. 2020. [Google Scholar] [CrossRef]
- Karimzadeh, S.; Bhopal, R.; Huy, N.T. Review of viral dynamics, exposure, infective dose, and outcome of COVID-19 caused by the SARS-COV-2 virus: Comparison with other respiratory viruses. Preprints 2020. Available online: https://www.preprints.org/manuscript/202007.0613/v1 (accessed on 14 October 2020).
- Salomoni, S.; Van den Hoorn, W.; Hodges, P. Breathing and Singing: Objective characterization of breathing patterns in classical singers. PLoS ONE 2016, 11, e0155084. [Google Scholar] [CrossRef]
- Buonanno, G.; Stabile, L.; Morawska, L. Estimation of airborne viral emission: Quanta emission rate of SARS-CoV-2 for infection risk assessment. Environ. Int. 2020, 141, 105794. [Google Scholar] [CrossRef]
- Hao, X.; Cheng, S.; Wu, D.; Lin, X.; Wang, C. Reconstruction of the full transmission dynamics of COVID-19 in Wuhan. Nature 2020, 583, 420–424. [Google Scholar] [CrossRef]
- Morawska, L.; Cao, J. Airborne transmission of SARS-CoV-2: The world should face the reality. Environ. Int. 2020, 139, 105730. [Google Scholar] [CrossRef] [PubMed]
- Fisk, W.J. The ventilation problem in schools: Literature review. Indoor Air. 2017, 27, 1039–1051. [Google Scholar] [CrossRef]
- Liu, J.; Ning, Z.; Chen, Y.; Guo, M.; Liu, Y.; Kumar Gali, N.; Sun, L.; Duan, Y.; Cai, J.; Westerdahl, D.; et al. Aerodynamic analysis of SARS-CoV-2 in two Wuhan hospitals. Nature 2020, 582, 557–560. [Google Scholar] [CrossRef]
- Christopherson, D.A.; Yao, W.C.; Lu, M.; Vijayakumar, R.; Sedaghat, A.R. High-efficiency particulate air filters in the era of COVID-19: Function and efficacy. Am. Acad. Otolaryngol. 2020. [Google Scholar] [CrossRef]
- Mousavi, E.S.; Kananizadeh, N.; Martinello, R.A.; Sherman, J.D. COVID-19 Outbreak and hospital air quality: A systematic review of evidence on air filtration and recirculation. Environ. Sci. Technol. 2020. [Google Scholar] [CrossRef]
- Kähler, C.J.; Fuchs, T.; Hain, R. Können Mobile Raumluftreiniger eine Indirekte SARS-CoV-2 Infektionsgefahr Durch Aerosole Wirksam Reduzieren? 2020. Available online: https://www.unibw.de/lrt7/raumluftreiniger.pdf (accessed on 14 October 2020).
- Max Planck Institute for Chemistry. Algorithm to Estimate COVID-19 Infection Risks by Aerosol Transmission in Indoor Environments. Available online: https://www.mpic.de/4747065/risk-calculation (accessed on 14 October 2020).
| Parameters | Standard | Range | Units |
|---|---|---|---|
| Infectious episode (exposure) | 2 | 0.08–5 | Days |
| Wet aerosol diameter | 5 | 2–10 | µm |
| Virus lifetime in aerosol | 1.7 | 0.6–2.6 | Hours |
| Concentration from breathing | 0.1 | 0.06–1.0 | cm−3 |
| Concentration from speaking (singing) | 1.1 | 0.06–6.0 | cm−3 |
| Speaking/breathing ratio | 0.10 | 0–1 | - |
| Respiratory rate | 10 | 5–20 | L/min |
| Viral load “highly infectious” | 5 × 108 | 108–109 | RNA Copies/cm3 |
| Viral load “super infectious” | 5 × 109 | 109–1010 | RNA copies/cm3 |
| Deposition probability in lungs | 0.5 | 0.2–0.8 | - |
| Infective dose (D50) | 316 | 100–1000 | RNA copies |
| Room area | 60 | 40–100 | m2 |
| Room height | 3 | 3–4 | m |
| Subjects in room | 25 | 4–100 | Persons |
| Passive ventilation rate | 0.35 | 0–1 | Hour−1 |
| Active ventilation rate (with outside air) | 2 | 2–9 | Hour−1 |
| Face mask filter efficiency from inhalation plus exhalation | 0.7 | 0–0.95 | - |
| Indoor Environment | Room Size (m2) | Room Height (m) | Subjects Present | Exposure Duration (Hours) |
|---|---|---|---|---|
| 1. Office | 40 | 3 | 4 | 16 |
| 2. Classroom | 60 | 3 | 25 | 12 |
| 3. Choir practice | 100 | 4 | 25 | 3 |
| 4. Reception | 100 | 4 | 100 | 3 |
| Scenario | VR 0.35 hr−1 | VR 2 hr−1 | Masks, 70% Efficiency | Masks, 95% Efficiency | High-Vol VR 9 hr−1 |
|---|---|---|---|---|---|
| A. Standard (passive ventilation) | + | ||||
| B. Active ventilation | + | ||||
| C. Active ventilation + medium efficient masks | + | + | |||
| D. Active ventilation + highly efficient masks | + | + | |||
| E. High-volume air filtration with HEPA | + |
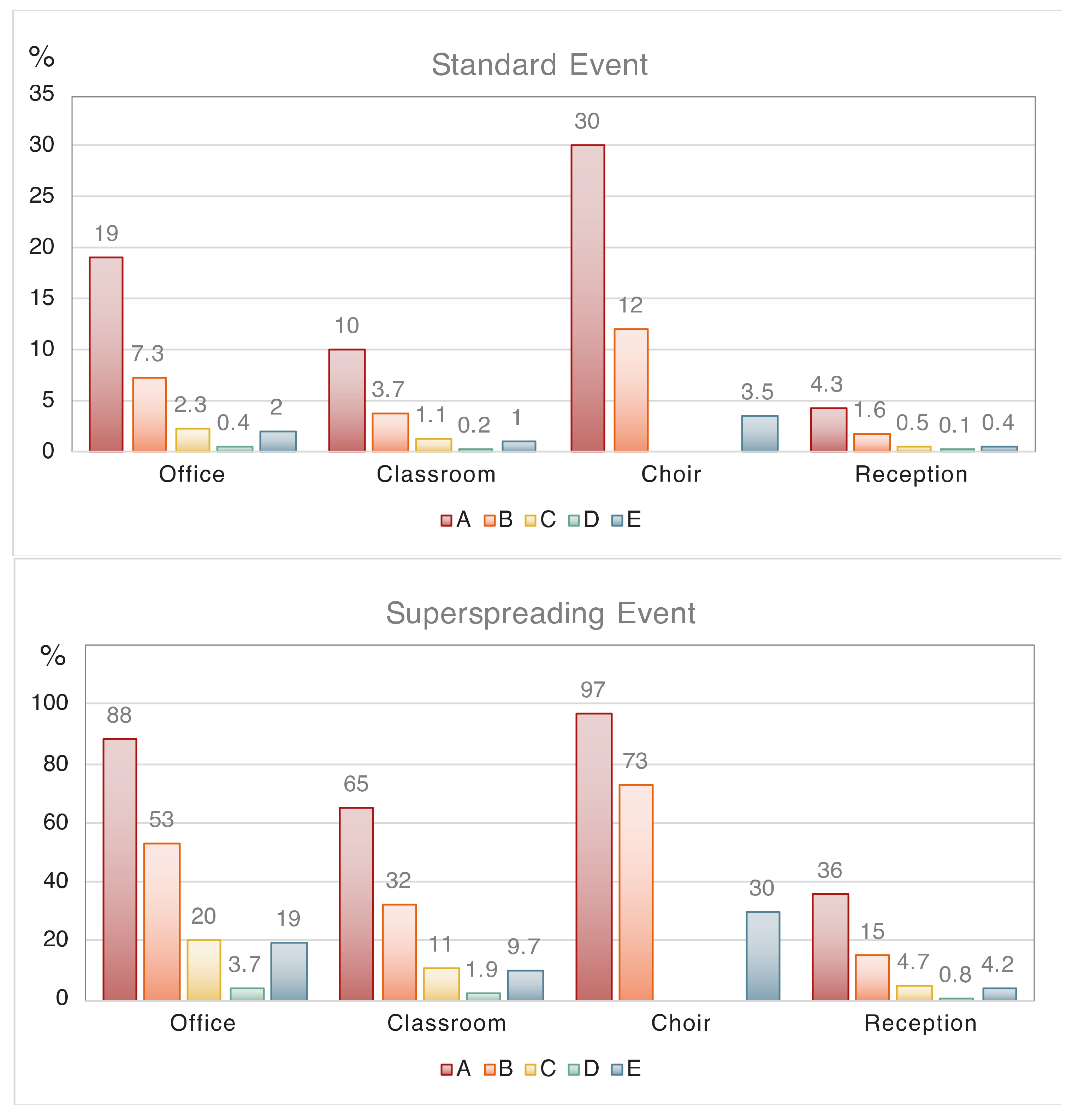
| Environment | Scenario A VR 0.35 hr−1 | Scenario B VR 2 hr−1 | Scenario C Masks, 70% Efficiency | Scenario D Masks, 95% Efficiency | Scenario E High-Vol VR 9 hr−1 |
|---|---|---|---|---|---|
| 1.1. Office individual risk | 19 | 7.3 | 2.3 | 0.4 | 2.0 |
| 1.2. Office group risk | 47 | 20 | 6.6 | 1.1 | 6.0 |
| 2.1. Classroom individual risk (>10 years) | 10 | 3.7 | 1.1 | 0.2 | 1.0 |
| 2.2. Classroom group risk (>10 years) | 92 | 60 | 24 | 4.5 | 22 |
| 2.3. Classroom individual risk (≤10 years) | 1.0 | 0.4 | 0.1 | 0 | 0.1 |
| 2.4. Classroom group risk (≤10 years) | 22 | 8.7 | 2.7 | 0.5 | 2.4 |
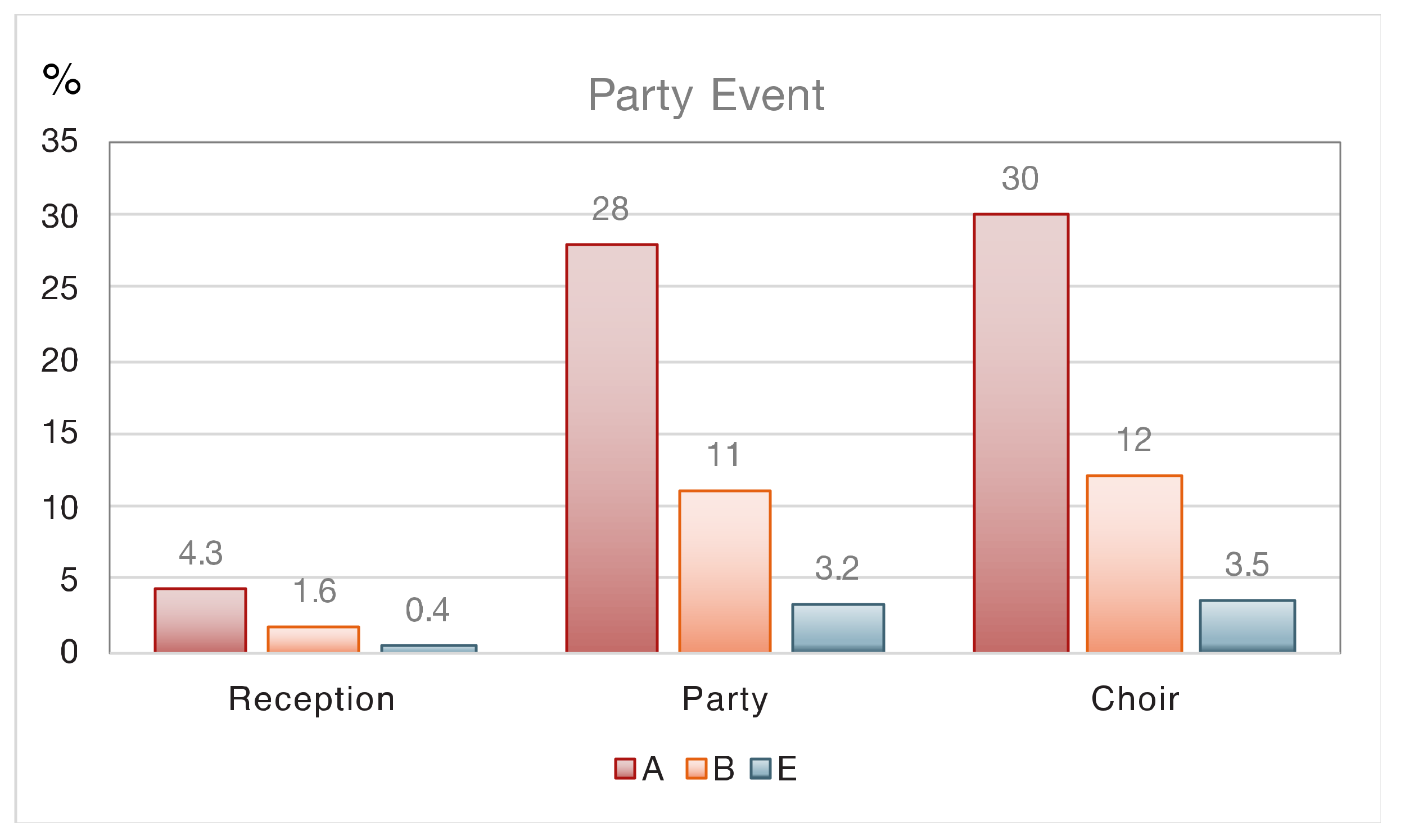
| 3.1. Choir practice individual risk | 30 | 12 | - | - | 3.5 |
| 3.2. Choir practice group risk | 100 | 96 | - | - | 57 |
| 4.1. Reception individual risk | 4.3 | 1.6 | 0.5 | 0.1 | 0.4 |
| 4.2. Reception group risk | 99 | 80 | 38 | 7.6 | 35 |
| 4.3. Party individual risk | 28 | 11 | 3.5 | 0.6 | 3.2 |
| 4.4. Party group risk | 100 | 100 | 97 | 45 | 96 |
| Environment | Scenario A VR 0.35 hr−1 | Scenario B VR 2 hr−1 | Scenario C Masks, 70% Efficiency | Scenario D Masks, 95% Efficiency | Scenario E High-Vol VR 9 hr−1 |
|---|---|---|---|---|---|
| 1.1. Office individual risk | 88 | 53 | 20 | 3.7 | 19 |
| 1.2. Office group risk | 100 | 90 | 50 | 11 | 46 |
| 2.1. Classroom individual risk (>10 years) | 65 | 32 | 11 | 1.9 | 9.7 |
| 2.2. Classroom group risk (>10 years) | 100 | 100 | 94 | 37 | 91 |
| 3.1. Choir practice individual risk | 97 | 73 | - | - | 30 |
| 3.2. Choir practice group risk | 100 | 100 | - | - | 100 |
| 4.1. Reception individual risk | 36 | 15 | 4.7 | 0.8 | 4.2 |
| 4.2. Reception group risk | 100 | 100 | 99 | 55 | 99 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lelieveld, J.; Helleis, F.; Borrmann, S.; Cheng, Y.; Drewnick, F.; Haug, G.; Klimach, T.; Sciare, J.; Su, H.; Pöschl, U. Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments. Int. J. Environ. Res. Public Health 2020, 17, 8114. https://doi.org/10.3390/ijerph17218114
Lelieveld J, Helleis F, Borrmann S, Cheng Y, Drewnick F, Haug G, Klimach T, Sciare J, Su H, Pöschl U. Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments. International Journal of Environmental Research and Public Health. 2020; 17(21):8114. https://doi.org/10.3390/ijerph17218114
Chicago/Turabian StyleLelieveld, Jos, Frank Helleis, Stephan Borrmann, Yafang Cheng, Frank Drewnick, Gerald Haug, Thomas Klimach, Jean Sciare, Hang Su, and Ulrich Pöschl. 2020. "Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments" International Journal of Environmental Research and Public Health 17, no. 21: 8114. https://doi.org/10.3390/ijerph17218114
APA StyleLelieveld, J., Helleis, F., Borrmann, S., Cheng, Y., Drewnick, F., Haug, G., Klimach, T., Sciare, J., Su, H., & Pöschl, U. (2020). Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments. International Journal of Environmental Research and Public Health, 17(21), 8114. https://doi.org/10.3390/ijerph17218114





