Movement Behaviors and Perceived Loneliness and Sadness within Alaskan Adolescents
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Instrumentation
2.3. Procedure
2.4. Statistical Analysis
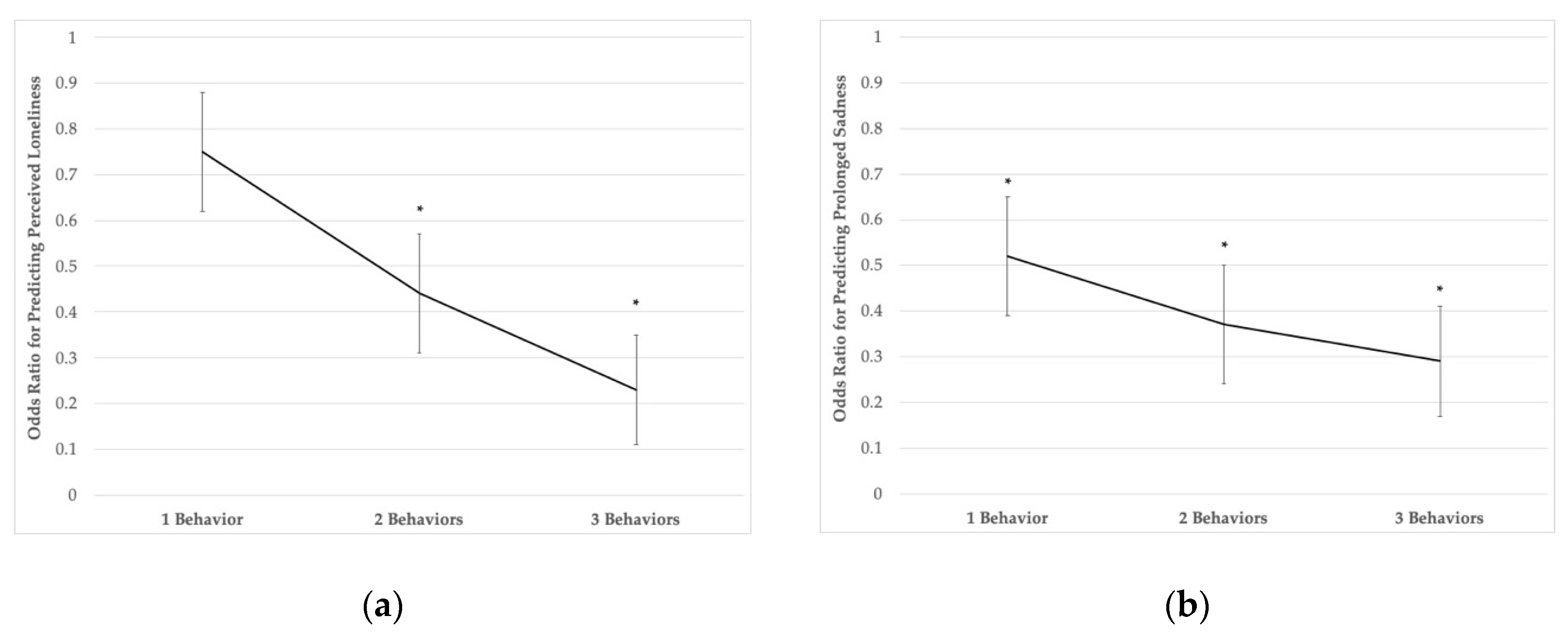
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Tremblay, M.S.; Carson, V.; Chaput, J.-P.; Gorber, S.C.; Dinh, T.; Duggan, M.; Faulkner, G.; Gray, C.E.; Gruber, R.; Janson, K.; et al. Canadian 24-hour movement guidelines for children and youth: An integration of physical activity, sedentary behavior, and sleep. Appl. Physiol. Nutr. Metab. 2016, 41, S311–S327. [Google Scholar] [CrossRef]
- Saunders, T.J.; Gray, C.E.; Poitras, V.J.; Chaput, J.-P.; Janssen, I.; Katzmarzyk, P.T.; Olds, T.; Gorber, S.C.; Kho, M.E.; Sampson, M.; et al. Combinations of physical activity, sedentary behavior and sleep: Relationships with health indicators in school-aged children and youth. Appl. Physiol. Nutr. Metab. 2016, 41, S283–S293. [Google Scholar] [CrossRef]
- Cabanas-Sanchez, V.; Martinez-Gomez, D.; Izquierdo-Gomez, R.; Segura-Jimenez, V.; Castro-Pinero, J.; Veiga, O.L. Association between clustering of lifestyle behaviors and health-related physical fitness in youth: The UP&DOWN Study. J. Pediatr. 2018, 199, 41–48. [Google Scholar] [CrossRef] [PubMed]
- Parker, K.E.; Salmon, J.; Costigan, S.A.; Villanueva, K.; Brown, H.L.; Timperio, A. Activity-related behavior typologies in youth: A systematic review. Int. J. Behav. Nutr. Phys. Act. 2019, 16, 44. [Google Scholar] [CrossRef] [PubMed]
- Dumuid, D.; Pedisic, Z.; Stanford, T.E.; Martin-Fernandez, J.-A.; Hron, K.; Maher, C.A.; Lewis, L.K.; Olds, T. The compositional isotemporal substitution model: A method for estimating changes in a health outcome for reallocation of time between sleep, physical activity and sedentary behaviour. Stat. Methods Med. Res. 2019, 28, 846–857. [Google Scholar] [CrossRef] [PubMed]
- Fairclough, S.J.; Dumuid, D.; Mackintosh, K.A.; Mackintosh, K.A.; Stone, G.; Dagger, R.; Stratton, G.; Davies, I.; Boddy, L.M. Adiposity, fitness, health-related quality of life and the reallocation of time between children’s school day activity behaviors: A compositional data analysis. Prev. Med. Rep. 2018, 11, 254–261. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Burns, R.D.; Lee, D.-C.; Welk, G.J. Associations of movement behaviors and body mass index: Comparison between a report-based and monitor-based method using compositional data analysis. Int. J. Obes. (Lond.) 2020. [Google Scholar] [CrossRef]
- Wilson, R.; Dumuid, D.; Olds, T.; Evans, J.R. Lifestyle clusters and academic achievement in Australian Indigenous children: Empirical findings and discussion of ecological levers for closing the gap. SSM Popul. Health 2020, 10, 100535. [Google Scholar] [CrossRef] [PubMed]
- Goosby, B.J.; Bellatorre, A.; Walsemann, K.M.; Cheadle, J.E. Adolescent loneliness and health in early adulthood. Sociol. Inq. 2013, 83. [Google Scholar] [CrossRef]
- Stickley, A.; Koyanagi, A.; Koposov, R.; Blatny, M.; Hrdlicka, M.; Schwab-Stone, M.; Ruchkin, V. Loneliness and its association with psychological and somatic health problems among Czech, Russian, and US adolescents. BMC Psychiatry 2016, 16, 128. [Google Scholar] [CrossRef]
- Jones, P.B. Adult mental health disorders and their age at onset. Br. J. Psychiatry Suppl. 2013, 54, s5–s10. [Google Scholar] [CrossRef] [PubMed]
- Henrikson, C.A.; Stein, M.B.; Afifi, T.O.; Enns, M.W.; Lix, L.M.; Sareen, J. Identifying factors that predict longitudinal outcomes of untreated common mental disorders. Psychiatr. Serv. 2015, 66, 163–170. [Google Scholar] [CrossRef] [PubMed]
- Owens, M.; Stevenson, J.; Hadwin, J.A. Anxiety and depression in academic performance: An exploration of the mediating factors of worry and working memory. Sch. Psychol. Int. 2012, 33, 433–449. [Google Scholar] [CrossRef]
- Orri, M.; Scardera, S.; Perret, L.C.; Bolanis, D.; Temcheff, C.; Seguin, J.R.; Boivin, M.; Turecki, G.; Tremblay, R.E.; Côté, S.M.; et al. Mental health problems and risk of suicidal ideation and attempts in adolescents. Pediatrics 2020, 146, 300–310. [Google Scholar] [CrossRef] [PubMed]
- Nock, M.K.; Green, J.G.; Hwang, I.; McLaughlin, K.A.; Sampson, N.A.; Zaslavsky, A.M.; Kessler, R.C. Prevalence, correlates, and treatment of lifetime suicidal behavior among adolescents: Results from the National Comorbidity Survey Replication Adolescent Supplement. JAMA Psychiatry 2013, 70, 300–310. [Google Scholar] [CrossRef]
- Pfledderer, C.D.; Burns, R.D.; Brusseau, T.A. School environment, physical activity, and sleep as predictors of suicidal ideation in adolescents: Evidence from a national survey. J. Adolesc. 2019, 74, 83–90. [Google Scholar] [CrossRef]
- Kim, S.; Favotto, L.; Halladay, J.; Wang, L.; Boyle, M.H.; Georgiades, K. Differential associations between passive and active forms of screen time and adolescent mood and anxiety disorders. Soc. Psychiatry Psychiatr. Epidemiol. 2020. [Google Scholar] [CrossRef]
- Boers, E.; Afzali, M.H.; Newton, N.; Conrod, P. Association of screen time and depression in adolescence. JAMA Pediatr. 2019, 173, 853–859. [Google Scholar] [CrossRef]
- Zhu, X.; Haegele, J.A.; Healy, S. Movement and mental health: Behavioral correlates of anxiety and depression among children of 6–17 years old in the US. Ment. Health Phys. Act. 2019, 16, 60–65. [Google Scholar] [CrossRef]
- Ogawa, S.; Kitagawa, Y.; Fukushima, M.; Yonehara, H.; Nishida, A.; Togo, F.; Sasaki, T. Interactive effect of sleep duration and physical activity on anxiety/depression in adolescents. Psychiatry Res. 2019, 273, 456–460. [Google Scholar] [CrossRef]
- Blackdeer, A.A.; Patterson Silver Wolf, D.A. Evidence mapping: Interventions for American Indian and Alaska Native youth mental health. J. Evid. Base. Soc. Work. 2020, 17, 49–62. [Google Scholar] [CrossRef]
- Markon, C.J.; Trainor, S.F.; Chapin, F.S., III. The United States National Climate Assessment-Alaska Technical Regional Report; US Geological Survey: Reston, VA, USA, 2012; pp. 1–148.
- Alaska Youth Risk Behavior Survey (YRBS). Alaska Department of Health and Social Services Division of Public Health website. Available online: http://dhss.alaska.gov/dph/Chronic/Pages/yrbs/default.aspxr (accessed on 23 July 2020).
- Mushtaq, R.; Shoib, S.; Shah, T.; Mushtaq, S. Relationship between loneliness, psychiatric disorders and physical health? A review on the psychological aspects of loneliness. J. Clin. Diag. Res. 2014, 8, WE01–WE04. [Google Scholar] [CrossRef] [PubMed]
- Tebeka, S.; Pignon, B.; Amad, A.; Le Strat, Y.; Brichant-Petitjean, C.; Thomas, P.; Vaiva, G.; Roelandt, J.-L.; Benradia, I.; Etain, B.; et al. A study in the general population about sadness to disentangle the continuum from well-being to depressive disorders. J. Affect. Disord. 2018, 226, 66–71. [Google Scholar] [CrossRef]
- Sivertsen, B.; Harvey, A.; Pallesen, S.; Hysing, M. Mental health problems in adolescents with delayed sleep phase: Results from a large population-based study in Norway. J. Sleep Res. 2014, 24, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Paksarian, D.; Lamers, F.; Hickie, I.B.; He, J.; Merikanges, K.R. Sleep patterns and mental health correlates in US adolescents. J. Pediatr. 2017, 182, 137–143. [Google Scholar] [CrossRef]
- Daly, B.P.; Jameson, J.P.; Patterson, F.; McCurdy, M.; Kirk, A.; Michael, K.D. Sleep duration, mental health, and substance use among rural adolescents: Developmental correlates. J. Rural Ment. Health 2015, 39, 108–122. [Google Scholar] [CrossRef]
- Baddam, S.K.R.; Canaparti, C.A.; van Noordt, S.J.R.; Crowley, M.J. Sleep disturbances in child and adolescent mental health disorders: A review of the variability of objective sleep markers. Med. Sci. 2018, 6, 46. [Google Scholar] [CrossRef]
- Forbes, E.E.; Bertocci, M.A.; Gregory, A.M.; Ryan, N.D.; Axelson, D.A.; Birmaher, B.; Dahl, R.E. Objective sleep in pediatric anxiety disorders and major depressive disorder. J. Am. Acad. Child Adolesc. Psychiatry 2008, 47, 148–155. [Google Scholar] [CrossRef]
- Alfano, C.A.; Reynolds, K.; Scott, N.; Dahl, R.E.; Mellman, T.A. Polysomnographic sleep patterns of non-depressed, non-medicated children with generalized anxiety disorder. J. Affect. Disord. 2013, 147, 379–384. [Google Scholar] [CrossRef]
- Forbes, E.E.; Williamson, D.E.; Ryan, N.D.; Birmaher, B.; Axelson, D.A.; Dahl, R.E. Peri-sleep-onset cortisol levels in children and adolescents with affective disorders. Biol. Psychiatry 2006, 59, 24–30. [Google Scholar] [CrossRef] [PubMed]
- Loades, M.E.; Chatburn, E.; Higson-Sweeney, N.; Reynolds, S.; Shafran, R.; Brigden, A.; Linney, C.; McManus, M.N.; Borwick, C.; Crawley, E. Rapid systematic review: The impact of social isolation and loneliness on the mental health of children and adolescents in the context of COVID-19. J. Am. Acad. Child. Adolesc. Psychiatry 2020. [Google Scholar] [CrossRef] [PubMed]
- Chaplin, T.M. Anger, happiness, and sadness: Associations with depressive symptoms in late adolescence. J. Youth Adolesc. 2006, 35, 977–986. [Google Scholar] [CrossRef]
- Bell, S.L.; Audrey, S.; Gunnell, D.; Cooper, A.; Campbell, R. The relationship between physical activity, mental wellbeing and symptoms of mental health disorder in adolescents: A cohort study. Int. J. Behav. Nutr. Phys. Act. 2019, 16, 138. [Google Scholar] [CrossRef] [PubMed]
- Biddle, S.J.; Ciaccioni, S.; Thomas, G.; Vergeer, I. Physical activity and mental health in children and adolescents: An updated review of reviews and an analysis of causality. Psychol. Sport Exerc. 2019, 42, 146–155. [Google Scholar] [CrossRef]
- Pels, F.; Kleinert, J. Loneliness and physical activity: A systematic review. Int. Rev. Sport Exerc. Psychol. 2016, 9, 231–260. [Google Scholar] [CrossRef]
- Buchan, M.C.; Carson, V.; Faulkner, G.; Qian, W.; Leatherdale, S.T. Factors associated with students meeting components of Canada’s new 24-hour movement guidelines over time in the COMPASS Study. Int. J. Environ. Res. Public Health 2020, 17, 5326. [Google Scholar] [CrossRef]
- Survey reveals Alaska children are playing less during the pandemic, which is concerning for their physical and mental health/Play Every Day blog. Alaska Department of Health and Social Services Division of Public Health Website. Available online: http://dhss.alaska.gov/dph/Epi/id/Pages/COVID-19/blog/20200513.aspx (accessed on 12 September 2020).
- Twenge, J.M.; Campbell, W.K. Associations between screen tie and lower psychological well-being among children and adolescents: Evidence from a population-based study. Prev. Med. Rep. 2018, 12, 271–283. [Google Scholar] [CrossRef]
- Vancampfort, D.; Ashdown-Franks, G.; Smith, L.; Firth, J.; Van Damme, T.; Christiaansen, L.; Stubbs, B.; Koyanagi, A. Leisure-time sedentary behavior and loneliness among 148,045 adolescents aged 12–15 years from 52 low-and middle-income countries. J. Affect Disord. 2019, 251, 149–155. [Google Scholar] [CrossRef]
- Pearson, N.; Sherar, L.B.; Hamer, M. Prevalence and correlates of meeting sleep, screen-time, and physical activity guidelines among adolescents in the United Kingdom. JAMA Pediatr. 2019, 173, 993–994. [Google Scholar] [CrossRef]
- Maes, M.; Nelemans, S.A.; Danneel, S.; Fernández-Castilla, B.; Van den Noortgate, W.; Goossens, L.; Vanhalst, J. Loneliness and social anxiety across childhood and adolescence: Multilevel meta-analyses of cross-sectional and longitudinal associations. Dev. Psychol. 2019, 55, 1548–1565. [Google Scholar] [CrossRef] [PubMed]
- McClelland, H.; Evans, J.J.; Nowland, R.; Ferguson, E.; O’Connor, R.C. Loneliness as a predictor of suicidal ideation and behaviour: A systematic review and meta-analysis of prospective studies. J. Affect Dis. 2020, 274, 880–896. [Google Scholar] [CrossRef] [PubMed]
- James, S.; Reddy, S.P.; Ellahebokus, A.; Sewpaul, R.; Naidoo, P. The association between adolescent risk behaviours and feelings of sadness or hopelessness: A cross-sectional survey of south African secondary school learners. Psychol. Health Med. 2017, 22, 778–789. [Google Scholar] [CrossRef] [PubMed]
- Crowley, S.J.; Acebo, C.; Carskadon, M.A. Sleep, circadian rhythms, and delayed phase in adolescence. Sleep Med. 2007, 86, 602–612. [Google Scholar] [CrossRef] [PubMed]
- Watson, N.F.; Martin, J.L.; Wise, M.S.; Carden, K.A.; Kirsch, D.B.; Kristo, D.A.; Malhotra, R.K.; Olson, E.J.; Ramar, K.; Rosen, I.M.; et al. Delaying middle school and high school start times promotes student health and performance: An American Academy of Sleep Medicine position statement. J. Clin. Sleep Med. 2017, 13, 623–625. [Google Scholar] [CrossRef]
- Nahmod, N.G.; Lee, S.; Master, L.; Chang, A.M.; Hale, L.; Buxton, O.M. Later high school start times associated with longer actigraphic sleep duration in adolescents. Sleep 2019, 42, zsy212. [Google Scholar] [CrossRef]
- Beets, M.W.; Okely, A.; Weaver, R.G.; Webster, C.; Lubans, D.; Brusseau, T.A.; Carson, R.; Cliff, D.P. The theory of expanded, extended, and enhanced opportunities for youth physical activity promotion. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 120. [Google Scholar] [CrossRef]
- Minges, K.E.; Owen, N.; Salmon, J.; Chao, A.; Dunstan, D.W.; Whittemore, R. Reducing youth screen time: Qualitative meta-synthesis of findings on barriers and facilitators. Health Psychol. 2015, 34, 381–397. [Google Scholar] [CrossRef]
| Variable | Level | n | Unweighted Prevalence (%) | Weighted Prevalence (%) |
|---|---|---|---|---|
| Age | 15 years old or younger | 847 | 45.4% | 38.8% |
| 16 or 17 years old | 800 | 42.9% | 45.2% | |
| 18 years old or older | 220 | 11.8% | 16.0% | |
| Sex | Male | 919 | 49.7% | 51.6% |
| Female | 930 | 50.3% | 48.4% | |
| Race/Ethnicity | White | 921 | 50.6% | 45.5% |
| American Indian or Alaska Native | 434 | 23.9% | 31.4% | |
| Black or African American | 49 | 2.7% | 2.5% | |
| Hispanic or Latino | 157 | 8.6% | 5.4% | |
| Other Races | 185 | 10.2% | 11.4% | |
| Multiple Races | 73 | 4.0% | 3.9% | |
| Weight Status | Healthy Weight | 1164 | 67.0% | 66.9% |
| Overweight/Obese | 572 | 33.0% | 33.1% |
| Variable | Level | n | Unweighted Prevalence (%) | Weighted Prevalence (%) |
|---|---|---|---|---|
| Perceived Loneliness | No Perceived loneliness | 1262 | 70.9% | 72.7% |
| Perceived loneliness | 518 | 29.1% | 27.3% | |
| Prolonged Sadness | No Prolonged Sadness | 1107 | 59.6% | 61.9% |
| Prolonged Sadness | 749 | 40.4% | 38.1% | |
| Physical Activity Only | Recommendations Not Met | 1474 | 81.2% | 82.1% |
| Recommendations Met | 341 | 18.8% | 17.9% | |
| Physical Activity and Muscle Strengthening | Recommendations Not Met | 1521 | 84.4% | 85.5% |
| Recommendations Met | 281 | 15.6% | 14.5% | |
| Television and Computer Screen Use | 2 h or more/Day | 766 | 42.8% | 39.8% |
| Less than 2 h/Day | 1024 | 57.2% | 60.3% | |
| School-Night Sleep Duration | Less than 8 h/Night | 1352 | 75.4% | 74.4% |
| 8 h/Night or More | 441 | 24.6% | 25.6% |
| Variable | Level | Crude OR (95% CI) | Adjusted OR 1 (95% CI) |
|---|---|---|---|
| Physical Activity and Muscle Strengthening | Recommendations Not Met | referent | referent |
| Recommendations Met | 0.66 * (0.45–0.98) | 0.77 (0.52–1.17) | |
| Television and Computer Screen Use | 2 h or more/Day | referent | referent |
| Less than 2 h/Day | 0.74 * (0.56–0.98) | 0.73 (0.52–1.02) | |
| School-Night Sleep Duration | Less than 8 h/Night | referent | referent |
| 8 h/Night or more | 0.47 * (0.28–0.78) | 0.43 * (0.24–0.75) | |
| Age (years) | 0.99 (0.89–1.11) | 1.02 (0.91–1.16) | |
| BMI z-score | 1.16 (0.99–1.37) | 1.20 * (1.00–1.43) | |
| Sex | Male | referent | referent |
| Female | 1.43 * (1.12–1.82) | 1.44 * (1.11–1.85) | |
| Race/Ethnicity | White | referent | referent |
| American Indian or Alaska Native | 1.04 (0.76–1.44) | 1.05 (0.76–1.43) | |
| Black or African American | 1.19 (0.53–2.64) | 0.83 (0.34–1.98) | |
| Hispanic or Latino | 1.34 (0.79–2.27) | 1.21 (0.75–1.96) | |
| Other Races | 1.56 * (1.04–2.34) | 1.36 (0.88–2.11) | |
| Multiple Races | 1.21 (0.68–2.15) | 1.11 (0.61–2.03) |
| Variable | Level | Crude OR (95% CI) | Adjusted OR 1 (95% CI) |
|---|---|---|---|
| Physical Activity and Muscle Strengthening | Recommendations Not Met | referent | referent |
| Recommendations Met | 0.65 * (0.45–0.95) | 0.72 (0.48–1.08) | |
| Television and Computer Screen Use | 2 h or more/Day | referent | referent |
| Less than 2 h/Day | 0.83 (0.63–1.10) | 0.74 (0.54–1.02) | |
| School-Night Sleep Duration | Less than 8 h/Night | referent | referent |
| 8 h/Night or more | 0.54 * (0.36–0.82) | 0.48 * (0.33–0.70) | |
| Age (years) | 0.99 (0.88–1.12) | 1.02 (0.91–1.16) | |
| BMI z-score | 0.92 (0.83–1.03) | 0.91 (0.81–1.03) | |
| Sex | Male | referent | referent |
| Female | 2.36 * (1.75–3.18) | 2.24 * (1.61–3.13) | |
| Race/Ethnicity | White | referent | referent |
| American Indian or Alaska Native | 1.47 * (1.02–2.07) | 1.72 * (1.24–2.49) | |
| Black or African American | 1.02 (0.45–2.33) | 0.96 (0.44–2.10) | |
| Hispanic or Latino | 1.57 * (1.06–2.33) | 1.51 * (1.07–2.14) | |
| Other Races | 1.10 (0.73–1.66) | 1.08 (0.67–1.72) | |
| Multiple Races | 1.50 (0.88–2.56) | 1.56 (0.83–2.94) |
| Outcome Variable | Recommendations Met | Adjusted OR 1 (95% CI) |
|---|---|---|
| Perceived Loneliness | All Behaviors Not Met | referent |
| Screen Use and Sleep | 0.32 * (0.13–0.77) | |
| Physical Activity and Sleep | 0.17 * (0.04–0.71) | |
| Physical Activity and Screen Use | 0.84 (0.42–1.66) | |
| Physical Activity, Screen Use, and Sleep | 0.23 * (0.08–0.64) | |
| Prolonged Sadness | All Behaviors Not Met | referent |
| Screen Use and Sleep | 0.37 * (0.24–0.57) | |
| Physical Activity and Sleep | 0.47 (0.21–1.06) | |
| Physical Activity and Screen Use | 0.56 * (0.33–0.91) | |
| Physical Activity, Screen Use, and Sleep | 0.29 * (0.11–0.77) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Burns, R.D.; Bai, Y.; Pfledderer, C.D.; Brusseau, T.A.; Byun, W. Movement Behaviors and Perceived Loneliness and Sadness within Alaskan Adolescents. Int. J. Environ. Res. Public Health 2020, 17, 6866. https://doi.org/10.3390/ijerph17186866
Burns RD, Bai Y, Pfledderer CD, Brusseau TA, Byun W. Movement Behaviors and Perceived Loneliness and Sadness within Alaskan Adolescents. International Journal of Environmental Research and Public Health. 2020; 17(18):6866. https://doi.org/10.3390/ijerph17186866
Chicago/Turabian StyleBurns, Ryan D., Yang Bai, Christopher D. Pfledderer, Timothy A. Brusseau, and Wonwoo Byun. 2020. "Movement Behaviors and Perceived Loneliness and Sadness within Alaskan Adolescents" International Journal of Environmental Research and Public Health 17, no. 18: 6866. https://doi.org/10.3390/ijerph17186866
APA StyleBurns, R. D., Bai, Y., Pfledderer, C. D., Brusseau, T. A., & Byun, W. (2020). Movement Behaviors and Perceived Loneliness and Sadness within Alaskan Adolescents. International Journal of Environmental Research and Public Health, 17(18), 6866. https://doi.org/10.3390/ijerph17186866








