Quality of Life in Orthodontic Cancer Survivor Patients—A Prospective Case–Control Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Study Protocol
2.3. Statistical Analysis
3. Results
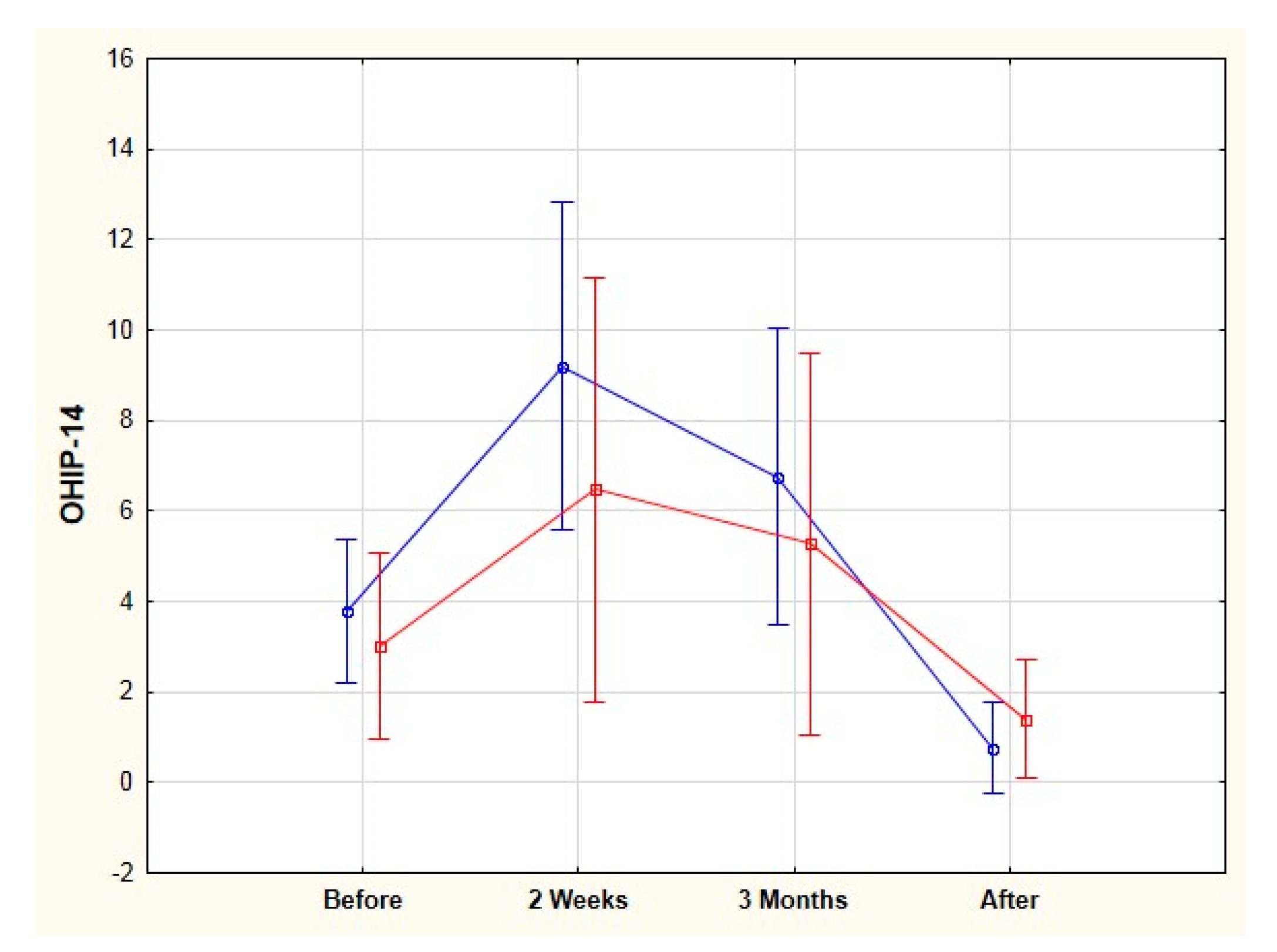
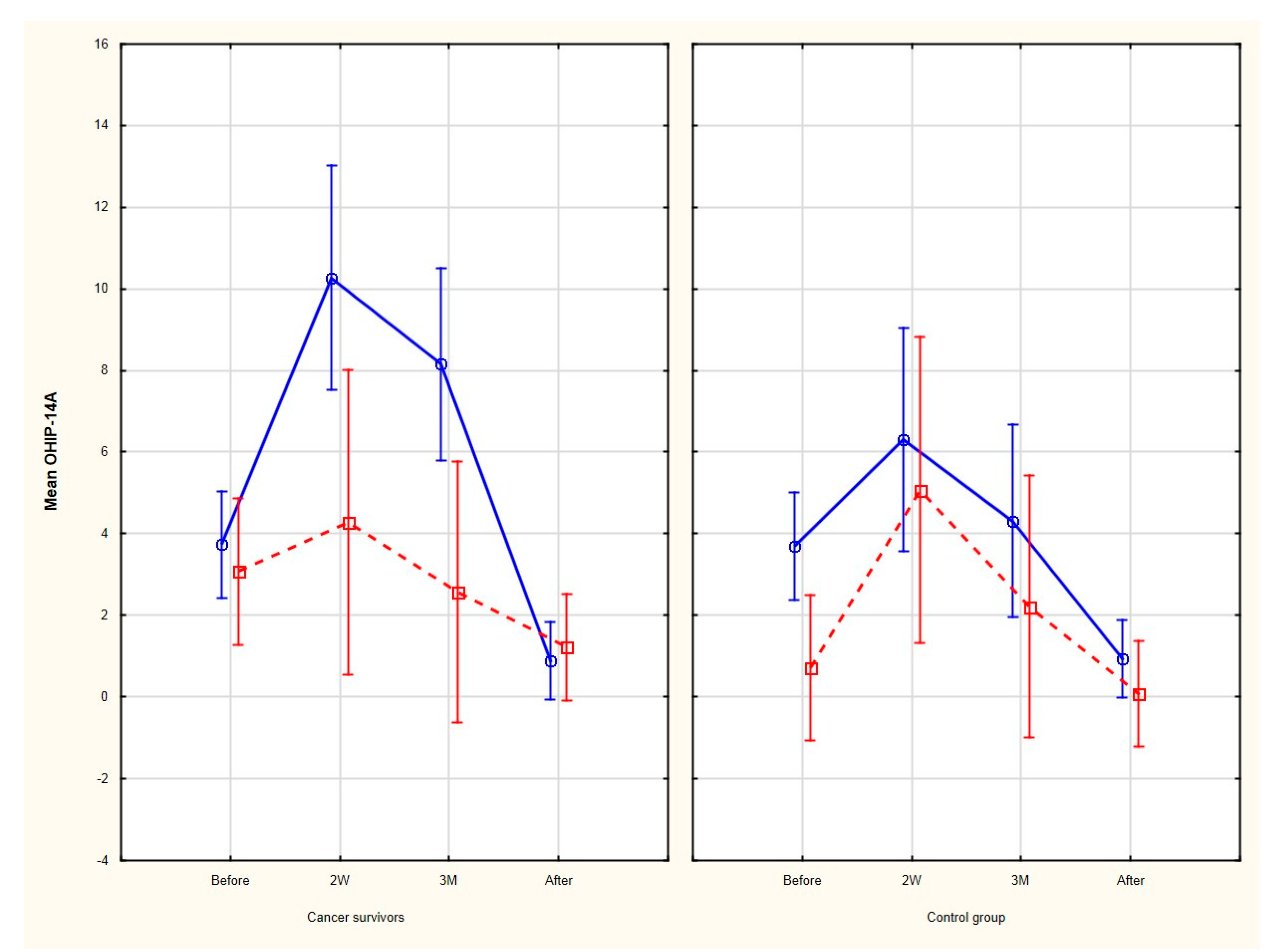
3.1. OHIP-14 Total Score
3.2. OHIP-14 Simple Count
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Steliarova-Foucher, E.; Colombet, M.; Ries, L.A.G.; Moreno, F.; Dolya, A.; Bray, F.; Heeseling, P.; Shin, H.Y.; Stiller, C.A.; Bouzbid, S.; et al. International incidence of childhood cancer, 2001–2010: A population-based registry study [published correction appears in Lancet Oncol. 2017 Jun; 18: e301]. Lancet. Oncol. 2017, 18, 719–731. [Google Scholar] [CrossRef]
- Filbin, M.; Monje, M. Developmental origins and emerging therapeutic opportunities for childhood cancer. Nat. Med. 2019, 25, 367–376. [Google Scholar] [CrossRef] [PubMed]
- WHO. Report on Cancer: Setting Priorities, Investing Wisely and Providing Care for All; World Health Organization: Geneva, Switzerland, 2020; Licence: CC BY-NC-SA 3.0 IGO. [Google Scholar]
- Seth, R.; Singh, A. Leukemias in Children. Indian J. Pediatr. 2015, 82, 817–824. [Google Scholar] [CrossRef] [PubMed]
- Howard, S.C.; Zaidi, A.; Cao, X.; Weil, O.; Bey, P.; Patte, C.; Samudio, A.; Haddad, L.; Lam, C.G.; Moreira, C.; et al. The My Child Matters programme: Effect of public-private partnerships on paediatric cancer care in low-income and middle-income countries. Lancet Oncol. 2018, 19, e252–e266. [Google Scholar] [CrossRef]
- Fung, A.; Horton, S.; Zabih, V.; Denburg, A.; Gupta, S. Cost and cost-effectiveness of childhood cancer treatment in low-income and middle-income countries: A systematic review. BMJ Glob. Health. 2019, 4, e001825. [Google Scholar] [CrossRef]
- Saletta, F.; Seng, M.S.; Lau, L. Advances in paediatric cancer treatment. Transl. Pediatr. 2014, 3, 156–182. [Google Scholar]
- Gawade, P.L.; Hudson, M.M.; Kaste, S.C.; Neglia, J.O.; Constine, L.S.; Robison, L.L.; Ness, K.K. A Systematic Review of Dental Late Effects in Survivors of Childhood Cancer. Pediatr. Blood Cancer 2014, 61, 407–416. [Google Scholar] [CrossRef]
- Mishra, S. Orthodontic Therapy for Paediatric Cancer Survivors: A Review. J. Clin. Diagn. Res. 2017, 11, ZE01–CZE04. [Google Scholar] [CrossRef]
- Mituś-Kenig, M.; Łoboda, M.; Marcinkowska-Mituś, A.; Durka-Zajac, M.; Pawłowska, E. Orthodontic treatment in oncological patients. Przegl. Lek. 2015, 72, 243–245. [Google Scholar]
- American Academy of Pediatric Dentistry (AAPD). Guideline on dental management of paediatric patients receiving chemotherapy, hematopoietic cell transplantation, and/or radiation. Pediatr. Dent. 2016, 6, 380–388. [Google Scholar]
- Dental Management of Pediatric Patients Receiving Chemotherapy, Hematopoietic Cell Transplantation, and/or Radiation Therapy. Pediatr. Dent. 2017, 39, 380–388.
- Hongxing, L.; List, T.; Nilsson, I.M.; Johansson, A.; Astrøm, A.N. Validity and reliability of OIDP and OHIP-14: A survey of Chinese high school students. BMC Oral Health 2014, 14, 158. [Google Scholar] [CrossRef] [PubMed]
- Sischo, L.; Broder, H.L. Oral health-related quality of life: What, why, how, and future implications. J. Dent. Res. 2011, 90, 1264–1270. [Google Scholar] [CrossRef] [PubMed]
- Andiappana, M.; Gaob, W.; Bernabé, E.; Kandalad, N.B.; Donaldson, A.N. Malocclusion, orthodontic treatment, and the Oral Health Impact Profile (OHIP-14): Systematic review and meta-analysis. Angle Orthod. 2015, 85, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Andrews, L.F. The six keys to normal occlusion. Am. J. Orthod. 1972, 62, 296–309. [Google Scholar] [CrossRef]
- Husain, F.A.; Tatengkeng, F. Oral Health-Related Quality of Life Appraised by OHIP-14 Between Urban and Rural Areas in Kutai Kartanegara Regency, Indonesia: Pilot Pathfinder Survey. Open Dent. J. 2017, 11, 557–564. [Google Scholar] [CrossRef] [PubMed]
- Deboni, A.L.; Giordani, A.J.; Lopes, N.N.; Dias, R.S.; Segreto, R.A.; Jensen, S.B.; Segreto, H.R.C. Long-term oral effects in patients treated with radiochemotherapy for head and neck cancer. Support Care Cancer 2012, 20, 555–568. [Google Scholar] [CrossRef]
- Aguiar, G.P.; Jham, B.C.; Magalhães, C.S.; Sensi, L.G.; Freire, A.R. A review of the biological and clinical aspects of radiation caries. J. Contemp. Dent. Pract. 2009, 10, 83–89. [Google Scholar] [CrossRef]
- Hong, C.H.; Fonseca, M. Consideration in the pediatric population with cancer. Dent. Clin. N. Am. 2008, 52, 155–181. [Google Scholar] [CrossRef]
- Kaste, S.C.; Goodman, P.; Leisenring, W.; Stovall, M.; Hayashi, R.J.; Yeazel, M.; Beiraghi, S.; Hudson, M.W.; Sklar, C.A.; Robison, L.L.; et al. Impact of radiation and chemotherapy on the risk of dental abnormalities. Cancer 2009, 115, 5817–5827. [Google Scholar] [CrossRef]
- Sonis, S.T. Oral mucositis. Anticancer Drugs 2011, 22, 607–612. [Google Scholar] [CrossRef] [PubMed]
- Montero-Martín, J.; Bravo-Pérez, M.; Albaladejo-Martínez, A.; Hernández- Martín, L.A.; Rosel-Gallardo, E.M. Validation the Oral Health Impact Profile (OHIP-14sp) for adults in Spain. J. Clin. Exp. Dent. 2009, 1, e1–e7. [Google Scholar]
- Rourke, M.T.; Stuber, M.L.; Hobbie, W.L.; Kazak, A.E. Posttraumatic stress disorder: Understanding the psychosocial impact of surviving childhood cancer into young adulthood. J. Pediatr. Oncol. Nurs. 1999, 16, 126–135. [Google Scholar] [PubMed]
- Bruce, M. A systematic and conceptual review of posttraumatic stress in childhood cancer survivors and their parents. Clin. Psychol. Rev. 2006, 26, 233–256. [Google Scholar] [CrossRef] [PubMed]
- Johal, A.; Alyaqoobi, I.; Patel, R.; Cox, S. The impact of orthodontic treatment on quality of life and self-esteem in adult patients. Eur. J. Orthod. 2015, 37, 233–237. [Google Scholar] [CrossRef]
- Feu, D.; Miguel, J.A.; Celeste, R.K.; Oliveira, B.H. Effect of orthodontic treatment on oral health-related quality of life. Angle Orthod. 2013, 83, 892–898. [Google Scholar] [CrossRef]
- Javidi, H.; Benson, P. The impact of malocclusion and its treatment on the oral health related quality of life of adults, assessed using the Oral Health Impact Profile (OHIP-14). Evid. Based Dent. 2015, 16, 57–58. [Google Scholar] [CrossRef]
- Ni, J.; Song, S.; Zhou, N. Impact of surgical orthodontic treatment on quality of life in Chinese young adults with class III malocclusion: A longitudinal study. BMC Oral Health 2019, 19, 109. [Google Scholar] [CrossRef]
- Rezaei, F.; Masalehi, H.; Golshah, A.; Imani, M.M. Oral health related quality of life of patients with class III skeletal malocclusion before and after orthognathic surgery. BMC Oral Health 2019, 19, 289. [Google Scholar] [CrossRef]
- Zheng, D.H.; Wang, X.X.; Su, Y.R.; Zhao, S.Y.; Xu, C.; Kong, C.; Zhang, J. Assessing changes in quality of life using the Oral Health Impact Profile (OHIP) in patients with different classifications of malocclusion during comprehensive orthodontic treatment. BMC Oral Health 2015, 15, 148. [Google Scholar] [CrossRef]
- Demirovic, K.; Habibovic, J.; Dzemidzic, V.; Tiro, A.; Nakas, E. Comparison of Oral Health-Related Quality of Life in Treated and Non-Treated Orthodontic Patients. Med. Arch. 2019, 73, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Jamilian, A.; Kiaee, B.; Sanayei, S.; Khosravi, S.; Perillo, L. Orthodontic Treatment of Malocclusion and its Impact on Oral Health-Related Quality of Life. Open Dent. J. 2016, 10, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.M.; Kang, K.H. Effect of malocclusion or orthodontic treatment on oral health-related quality of life in adults. Korean J. Orthod. 2014, 44, 304–311. [Google Scholar] [CrossRef] [PubMed]
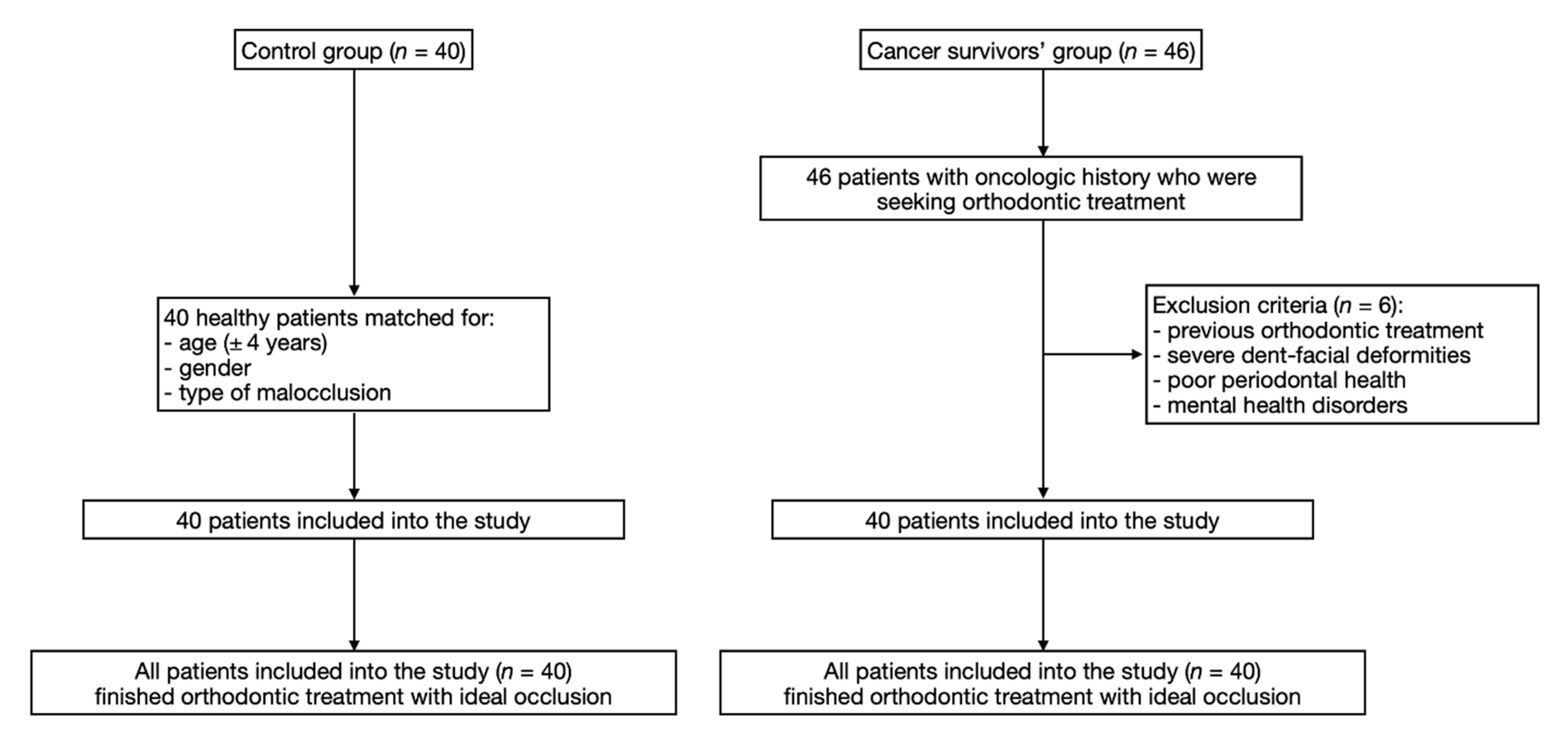
| Factor | Cancer Survivors’ Group | Control Group | p-Value a |
|---|---|---|---|
| Number of patients (n) (female/male ratio) | 40 (26/14) | 40 (26/14) | 1.000 |
| Median age (range) (years) | 19.4 (14–28) | 19.2 (14–28) | 0.889 |
| Orthodontic assessment (the same for both groups) | Skeletal class II: 26 patients each group Skeletal class I: 9 patients each group Skeletal class III: 5 patients each group | 1.000 | |
| Diagnosis | No of Cases | Mean Age at Diagnosis | Follow-up Time | Treatment Modality | |
|---|---|---|---|---|---|
| Chemotherapy | Radiotherapy | ||||
| Leukemia | 22 | 3.8 ± 1.3 | 9.5 ± 4.6 | 28 | 0 |
| Neuroblastoma | 3 | 0.7 ± 0.4 | 5.3 ± 1.1 | 4 | 0 |
| Soft tissue sarcoma | 3 | 2.2 ± 1.76 | 7.2 ± 2.0 | 4 | 1 |
| Non-Hodgkin’s lymphoma | 6 | 4.7 ± 2.1 | 8.0 ± 4.2 | 8 | 1 |
| Wilms tumor | 6 | 3.8 ± 2.2 | 6.1 ± 3.3 | 8 | 0 |
| The List of Questions in the OHIP-14 Questionnaire |
|---|
| Functional Limitation |
|
| Physical Pain |
|
| Psychological Discomfort |
|
| Physical Disability |
|
| Psychological Disability |
|
| Social Disability |
|
| Handicap |
|
| Time of Orthodontic Treatment (TX) | Cancer Survivors’ Group | Control Group | p-Value a |
|---|---|---|---|
| (mean ± SD) (Range) | (mean ± SD) (Range) | ||
| Before TX | 3.5 ± 3.9 1,2,3 | 3.7 ± 3.0 4,5,6 | 0.278 |
| (0–14) | (0–9) | ||
| 2 weeks after the onset of TX | 8.2 ± 8.9 1 | 8 ± 5.0 4 | 0.159 |
| (0–32) | (0–20) | ||
| 3 months after the onset of TX | 6.2 ± 7.9 2 | 6.2 ± 3.9 5 | 0.213 |
| (0–28) | (0–15) | ||
| After TX | 1.0 ± 2.5 3 | 0.6 ± 2.3 6 | 0.126 |
| (0–14) | (0–12) |
| OHIP-14 Domains | Functional Limitation | Physical Pain | Psychological Discomfort | Physical Disability | Psychological Disability | Social Disability | Handicap |
|---|---|---|---|---|---|---|---|
| Before (cancer survivors vs. control) | 0.3 ± 0.5 0.3 ± 0.6 | 0.1 ± 0.3 0.1 ± 0.3 | 0.4 ± 0.7 0.2 ± 0.5 | 0.9 ± 0.9 0.6 ± 0.9 | 0.7 ± 1.3 0.5 ± 0.8 | 0.4 ± 0.7 0.3 ± 0.6 | 0.8 ± 1.1 0.6 ± 0.9 |
| 2 weeks (cancer survivors vs. control) | 0.8 ± 0.9 0.9 ± 1.2 | 2.2 ± 2.7 1.6 ± 1.2 | 1.3 ± 2.0 1 0.3 ± 0.6 1 | 1.7 ± 1.6 1.2 ± 1.0 | 1.2 ± 1.6 1.0 ± 1.3 | 0.4 ± 0.8 0.4 ± 0.7 | 0.7 ± 1.3 0.5 ± 0.8 |
| 3 months (cancer survivors vs. control) | 0.4 ± 0.8 0.6 ± 0.9 | 1.6 ± 2.1 0.9 ± 0.9 | 1.0 ± 1.6 2 0.2 ± 0.9 2 | 1.4 ± 1.7 0.8 ± 1.0 | 1.0 ± 1.5 0.7 ± 0.9 | 0.4 ± 0.8 0.2 ± 0.5 | 0.5 ± 1.2 0.4 ± 0.6 |
| After (cancer survivors vs. control) | 0.1 ± 0.3 0.1 ± 1.4 | 0.2 ± 0.5 0.1 ± 0.3 | 0.2 ± 0.6 0.1 ± 0.3 | 0.3 ± 0.6 0.1 ± 0.4 | 0.1 ± 0.5 0.1 ± 0.3 | 0.1 ± 0.4 0.1 ± 0.4 | 0.1 ± 0.3 0.1 ± 0.4 |
| OHIP-14 Domains | Functional Limitation | Physical Pain | Psychological Discomfort | Physical Disability | Psychological Disability | Social Disability | Handicap |
|---|---|---|---|---|---|---|---|
| Before vs. after | <0.001 <0.001 | <0.001 <0.001 | <0.001 0.652 | <0.001 <0.001 | <0.001 0.004 | 0.156 0.342 | <0.001 <0.001 |
| Before vs. 2 weeks | <0.001 <0.001 | <0.001 <0.001 | <0.001 0.020 | <0.001 0.225 | <0.001 0.025 | 0.656 0.421 | 0.034 0.041 |
| Before vs. 3 months | <0.001 <0.001 | <0.001 <0.001 | <0.001 0.030 | <0.001 0.225 | 0.041 0.287 | 1 0.987 | 0.019 0.012 |
| OHIP-14 DOMAINS | Functional Limitation | Physical Pain | Psychological Discomfort | Physical Disability | Psychological Disability | Social Disability | Handicap |
|---|---|---|---|---|---|---|---|
| Before (cancer survivors vs. control) | 1 3 | 0 0 | 4 1 | 12 10 | 8 6 | 6 2 | 8 7 |
| 2 weeks (cancer survivors vs. control) | 6 11 | 16 17 | 13 1 2 1 | 22 19 | 13 11 | 5 4 | 6 3 |
| 3 months (cancer survivors vs. control) | 2 7 | 14 7 | 11 2 2 2 | 16 12 | 12 6 | 5 3 | 5 3 |
| After (cancer survivors vs. control) | 1 1 | 2 1 | 3 1 | 2 1 | 2 1 | 2 2 | 1 2 |
| Time of Orthodontic Treatment (TX) | Cancer Survivors’ Group | Control Group | p-Value |
|---|---|---|---|
| (Chi-Square Test) | |||
| Before | 6 (15.0%) | 3 (7.5%) | 0.289 |
| 2 weeks | 13 (32.5%) | 11 (27.5%) | 0.716 |
| 3 months | 11 (27.5%) | 6 (15.0%) | 0.172 |
| After the treatment | 2 (5.0%) | 1 (2.5%) | 0.556 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mitus-Kenig, M.; Derwich, M.; Czochrowska, E.; Pawlowska, E. Quality of Life in Orthodontic Cancer Survivor Patients—A Prospective Case–Control Study. Int. J. Environ. Res. Public Health 2020, 17, 5824. https://doi.org/10.3390/ijerph17165824
Mitus-Kenig M, Derwich M, Czochrowska E, Pawlowska E. Quality of Life in Orthodontic Cancer Survivor Patients—A Prospective Case–Control Study. International Journal of Environmental Research and Public Health. 2020; 17(16):5824. https://doi.org/10.3390/ijerph17165824
Chicago/Turabian StyleMitus-Kenig, Maria, Marcin Derwich, Ewa Czochrowska, and Elzbieta Pawlowska. 2020. "Quality of Life in Orthodontic Cancer Survivor Patients—A Prospective Case–Control Study" International Journal of Environmental Research and Public Health 17, no. 16: 5824. https://doi.org/10.3390/ijerph17165824
APA StyleMitus-Kenig, M., Derwich, M., Czochrowska, E., & Pawlowska, E. (2020). Quality of Life in Orthodontic Cancer Survivor Patients—A Prospective Case–Control Study. International Journal of Environmental Research and Public Health, 17(16), 5824. https://doi.org/10.3390/ijerph17165824





