Prevalence and Predictors of Insulin Resistance in Non-Obese Healthy Young Females in Qatar
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Anthropometric and Biochemical Measurements
2.3. Statistical Analysis
3. Results
3.1. General Characteristics and Prevalence of Insulin Resistance in Age-Matched Individuals with Different BMI Groups
3.2. Multivariate Analysis of Mediators of the Metabolic Syndrome
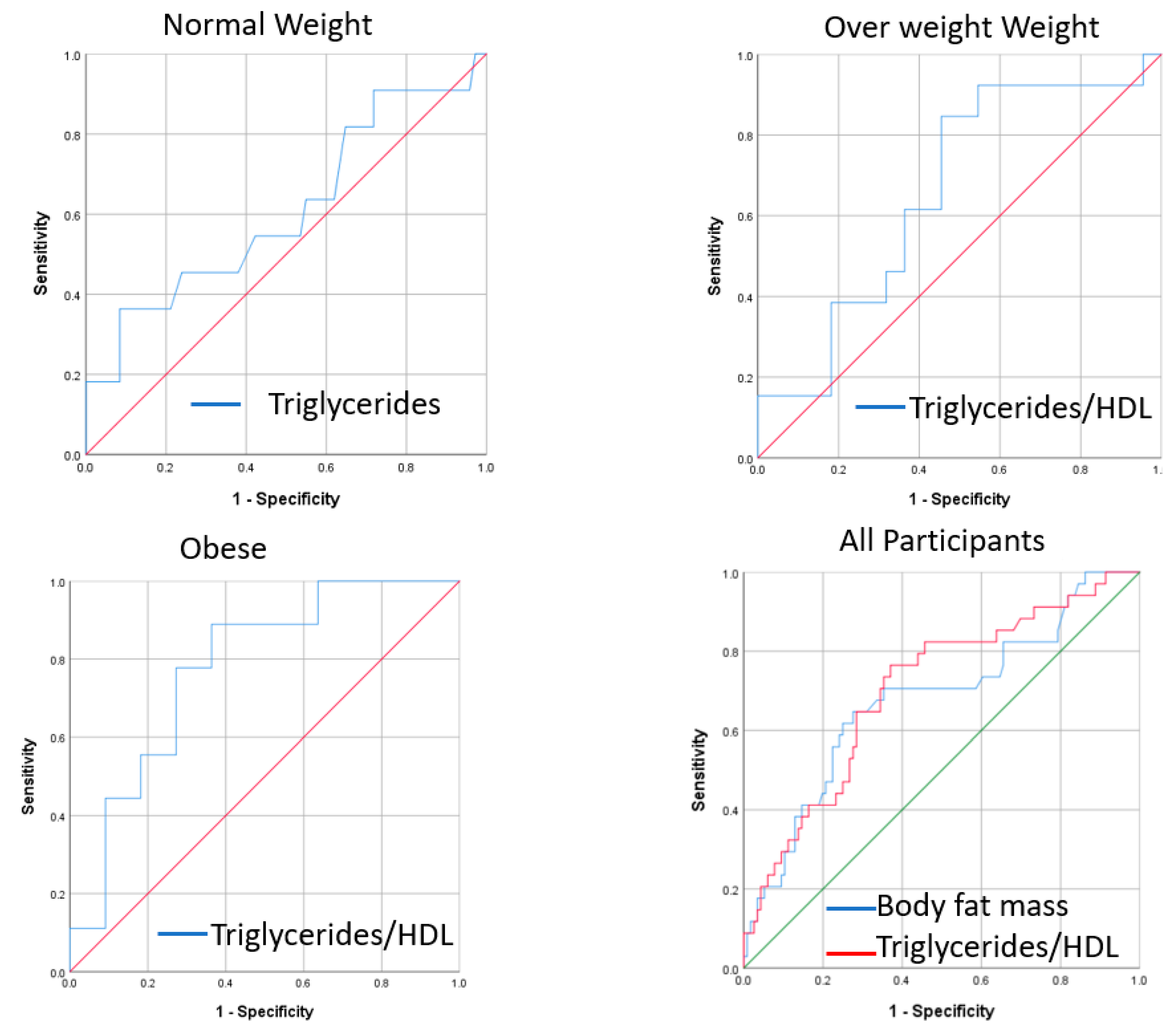
3.3. Mediators of Insulin Resistance
4. Discussion
Study Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Grundy, S.M.; Brewer, H.B., Jr.; Cleeman, J.I.; Smith, S.C., Jr.; Lenfant, C.; National Heart, Lung, and Blood Institute, American Heart Association. Definition of metabolic syndrome: Report of the National Heart, Lung, and Blood Institute/American Heart Association conference on scientific issues related to definition. Circulation 2004, 109, 433–438. [Google Scholar] [CrossRef] [PubMed]
- Gayoso-Diz, P.; Otero-Gonzalez, A.; Rodriguez-Alvarez, M.X.; Gude, F.; Garcia, F.; de Francisco, A.; Quintela, A.G. Insulin resistance (HOMA-IR) cut-off values and the metabolic syndrome in a general adult population: Effect of gender and age: EPIRCE cross-sectional study. BMC Endocr. Disord. 2013, 13, 47. [Google Scholar] [CrossRef] [PubMed]
- Barry, E.; Roberts, S.; Oke, J.; Vijayaraghavan, S.; Normansell, R.; Greenhalgh, T. Efficacy and effectiveness of screen and treat policies in prevention of type 2 diabetes: Systematic review and meta-analysis of screening tests and interventions. BMJ 2017, 356, i6538. [Google Scholar] [CrossRef] [PubMed]
- Bansal, N. Prediabetes diagnosis and treatment: A review. World J. Diabetes 2015, 6, 296–303. [Google Scholar] [CrossRef]
- Tabak, A.G.; Herder, C.; Rathmann, W.; Brunner, E.J.; Kivimaki, M. Prediabetes: A high-risk state for diabetes development. Lancet 2012, 379, 2279–2290. [Google Scholar] [CrossRef]
- Konig, D.; Hormann, J.; Predel, H.G.; Berg, A. A 12-Month Lifestyle Intervention Program Improves Body Composition and Reduces the Prevalence of Prediabetes in Obese Patients. Obes. Facts 2018, 11, 393–399. [Google Scholar] [CrossRef]
- Misra, A.; Gopalan, H.; Jayawardena, R.; Hills, A.P.; Soares, M.; Reza-Albarran, A.A.; Ramaiya, K.L. Diabetes in developing countries. J. Diabetes 2019, 11, 522–539. [Google Scholar] [CrossRef]
- McKeown, R.E. The Epidemiologic Transition: Changing Patterns of Mortality and Population Dynamics. Am. J. Lifestyle Med. 2009, 3, 19S–26S. [Google Scholar] [CrossRef]
- DeFronzo, R.A.; Tobin, J.D.; Andres, R. Glucose clamp technique: A method for quantifying insulin secretion and resistance. Am. J. Physiol. 1979, 237, E214–E223. [Google Scholar] [CrossRef]
- Hompesch, M.; Rave, K. An analysis of how to measure glucose during glucose clamps: Are glucose meters ready for research? J. Diabetes Sci. Technol. 2008, 2, 896–898. [Google Scholar] [CrossRef]
- Matsuda, M. 75-g oral glucose tolerance test, insulin tolerance test, homeostasis model assessment IR (insulin resistance), and Matsuda index. Nihon Rinsho 2012, 70, 475–480. [Google Scholar] [PubMed]
- Matthews, D.R.; Hosker, J.P.; Rudenski, A.S.; Naylor, B.A.; Treacher, D.F.; Turner, R.C. Homeostasis model assessment: Insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985, 28, 412–419. [Google Scholar] [CrossRef] [PubMed]
- Stern, S.E.; Williams, K.; Ferrannini, E.; DeFronzo, R.A.; Bogardus, C.; Stern, M.P. Identification of individuals with insulin resistance using routine clinical measurements. Diabetes 2005, 54, 333–339. [Google Scholar] [CrossRef] [PubMed]
- DeFronzo, R.A.; Tripathy, D. Skeletal muscle insulin resistance is the primary defect in type 2 diabetes. Diabetes Care 2009, 32, S157–S163. [Google Scholar] [CrossRef]
- Calori, G.; Lattuada, G.; Piemonti, L.; Garancini, M.P.; Ragogna, F.; Villa, M.; Mannino, S.; Crosignani, P.; Bosi, E.; Luzi, L.; et al. Prevalence, metabolic features, and prognosis of metabolically healthy obese Italian individuals: The Cremona Study. Diabetes Care 2011, 34, 210–215. [Google Scholar] [CrossRef]
- McLaughlin, T.; Allison, G.; Abbasi, F.; Lamendola, C.; Reaven, G. Prevalence of insulin resistance and associated cardiovascular disease risk factors among normal weight, overweight, and obese individuals. Metabolism 2004, 53, 495–499. [Google Scholar] [CrossRef]
- St-Onge, M.P.; Janssen, I.; Heymsfield, S.B. Metabolic syndrome in normal-weight Americans: New definition of the metabolically obese, normal-weight individual. Diabetes Care 2004, 27, 2222–2228. [Google Scholar] [CrossRef]
- Owei, I.; Umekwe, N.; Provo, C.; Wan, J.; Dagogo-Jack, S. Insulin-sensitive and insulin-resistant obese and non-obese phenotypes: Role in prediction of incident pre-diabetes in a longitudinal biracial cohort. BMJ Open Diabetes Res. Care 2017, 5, e000415. [Google Scholar] [CrossRef]
- Christos, P.J.; Chemaitelly, H.; Abu-Raddad, L.J.; Zirie, M.A.; Deleu, D.; Mushlin, A.I. Prevention of type II diabetes mellitus in Qatar: Who is at risk? Qatar Med. J. 2014, 2014, 70–81. [Google Scholar] [CrossRef][Green Version]
- Huang, Y.; Cai, X.; Mai, W.; Li, M.; Hu, Y. Association between prediabetes and risk of cardiovascular disease and all cause mortality: Systematic review and meta-analysis. BMJ 2016, 355, i5953. [Google Scholar] [CrossRef]
- Gonzalez-Cantero, J.; Martin-Rodriguez, J.L.; Gonzalez-Cantero, A.; Arrebola, J.P.; Gonzalez-Calvin, J.L. Insulin resistance in lean and overweight non-diabetic Caucasian adults: Study of its relationship with liver triglyceride content, waist circumference and BMI. PLoS ONE 2018, 13, e0192663. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Chen, S.; Deng, A.; Liu, X.; Liang, Y.; Shao, X.; Sun, M.; Zou, H. Association between lipid ratios and insulin resistance in a Chinese population. PLoS ONE 2015, 10, e0116110. [Google Scholar] [CrossRef] [PubMed]
- Chiang, J.K.; Lai, N.S.; Chang, J.K.; Koo, M. Predicting insulin resistance using the triglyceride-to-high-density lipoprotein cholesterol ratio in Taiwanese adults. Cardiovasc. Diabetol. 2011, 10, 93. [Google Scholar] [CrossRef] [PubMed]
- Hadaegh, F.; Khalili, D.; Ghasemi, A.; Tohidi, M.; Sheikholeslami, F.; Azizi, F. Triglyceride/HDL-cholesterol ratio is an independent predictor for coronary heart disease in a population of Iranian men. Nutr. Metab. Cardiovasc. Dis. 2009, 19, 401–408. [Google Scholar] [CrossRef] [PubMed]
- Savage, D.B.; Petersen, K.F.; Shulman, G.I. Disordered lipid metabolism and the pathogenesis of insulin resistance. Physiol. Rev. 2007, 87, 507–520. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Ambrosi, J.; Silva, C.; Galofre, J.C.; Escalada, J.; Santos, S.; Gil, M.J.; Valenti, V.; Rotellar, F.; Ramirez, B.; Salvador, J.; et al. Body adiposity and type 2 diabetes: Increased risk with a high body fat percentage even having a normal BMI. Obesity (Silver Spring) 2011, 19, 1439–1444. [Google Scholar] [CrossRef]
- Wedin, W.K.; Diaz-Gimenez, L.; Convit, A.J. Prediction of insulin resistance with anthropometric measures: Lessons from a large adolescent population. Diabetes Metab. Syndr. Obes. 2012, 5, 219–225. [Google Scholar]
- Park, S.Y.; Cho, Y.R.; Kim, H.J.; Hong, E.G.; Higashimori, T.; Lee, S.J.; Goldberg, I.J.; Shulman, G.I.; Najjar, S.M.; Kim, J.K. Mechanism of glucose intolerance in mice with dominant negative mutation of CEACAM1. Am. J. Physiol. Endocrinol. Metab. 2006, 291, E517–E524. [Google Scholar] [CrossRef]

| Groups | Combined | Under Weight | Normal Weight | Overweight | Obese | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (116 IS and 34 IR) | (13 IS and 1 IR) | (71 IS and 11 IR) | (22 IS and 13 IR) | (11 IS and 9 IR) | |||||||||||
| Characteristics | (IR Prevalence 22.7%) | (IR Prevalence 7.1%) | (IR Prevalence 13.4%) | (IR Prevalence 37.1%) | (IR Prevalence 45%) | ||||||||||
| Mean | SD | p Value | Mean | SD | Mean | SD | p Value | Mean | SD | p Value | Mean | SD | p Value | ||
| Age (years) | IS | 22.5 | 4.9 | 0.449 | 21.4 | 1.7 | 22.4 | 5.1 | 0.938 | 23.4 | 5.6 | 0.551 | 23.1 | 4.8 | 0.237 |
| IR | 21.8 | 3.6 | 18 | N/A | 22.3 | 5.3 | 22.4 | 3.5 | 21.1 | 1.4 | |||||
| BMI (Kg/m2) | IS | 23.5 | 4.6 | <0.001 | 17.3 | 0.9 | 21.9 | 2 | 0.946 | 27.1 | 1.3 | 0.424 | 33.2 | 3.2 | 0.184 |
| IR | 28 | 5.8 | 18 | N/A | 21.8 | 1.5 | 27.5 | 1.6 | 35.2 | 3.3 | |||||
| Body fat mass | IS | 21.5 | 8.8 | <0.001 | 10.3 | 2.5 | 18.6 | 4.2 | 0.998 | 27.8 | 4.1 | 0.628 | 40 | 6 | 0.391 |
| IR | 29.5 | 11.1 | 12.1 | N/A | 18.6 | 4.9 | 28.4 | 3.8 | 42.7 | 8.1 | |||||
| WC (cm) | IS | 81.6 | 10 | <0.001 | 70.3 | 6.3 | 78.8 | 7.2 | 0.694 | 89.4 | 7.1 | 0.491 | 95.9 | 7.3 | 0.013 |
| IR | 90.6 | 13 | 87 | N/A | 77.8 | 8.9 | 87.9 | 4 | 106.3 | 9.5 | |||||
| Total body water | IS | 28.8 | 5.6 | 0.366 | 24.7 | 2 | 28.5 | 6.5 | 0.048 | 30.4 | 2.9 | 0.171 | 31.9 | 3 | 0.163 |
| IR | 29.7 | 4.1 | 27.7 | N/A | 26.3 | 1.8 | 29 | 2.8 | 34.1 | 3.9 | |||||
| Free fat mass | IS | 20.7 | 3.1 | 0.037 | 17.8 | 1.7 | 20.1 | 2.8 | 0.309 | 22.6 | 2.4 | 0.216 | 23.7 | 2.4 | 0.149 |
| IR | 22 | 3.4 | 20.2 | N/A | 19.1 | 1.5 | 21.5 | 2.2 | 25.5 | 3.2 | |||||
| % body fat | IS | 34.6 | 7.8 | <0.001 | 23.2 | 4.1 | 32.9 | 5.3 | 0.713 | 39.9 | 4.2 | 0.236 | 47.8 | 2.8 | 0.696 |
| IR | 41 | 7.6 | 24.2 | N/A | 33.7 | 4.8 | 41.7 | 4.1 | 48.4 | 4.2 | |||||
| WHtR | IS | 0.5 | 0.1 | <0.001 | 0.4 | 0 | 0.5 | 0.1 | 0.811 | 0.6 | 0 | 0.866 | 0.6 | 0 | 0.029 |
| IR | 0.6 | 0.1 | 0.5 | N/A | 0.5 | 0.1 | 0.6 | 0 | 0.7 | 0.1 | |||||
| Glucose (mmol/L) | IS | 5 | 0.4 | 0.581 | 5 | 0.3 | 5 | 0.4 | 0.912 | 5 | 0.4 | 0.059 | 4.9 | 0.5 | 0.259 |
| IR | 5 | 0.6 | 5.1 | N/A | 5.1 | 0.4 | 4.7 | 0.5 | 5.2 | 0.7 | |||||
| Insulin (pmol/L) | IS | 2.8 | 2.2 | <0.001 | 2.4 | 2.5 | 2.4 | 2.1 | <0.001 | 4 | 2.2 | <0.001 | 3.2 | 1.8 | <0.001 |
| IR | 20.3 | 7.8 | 20.9 | N/A | 20.8 | 7.3 | 18.9 | 7.2 | 21.9 | 9.8 | |||||
| HOMA-IR | IS | 0.6 | 0.5 | <0.001 | 0.5 | 0.5 | 0.5 | 0.5 | <0.001 | 0.9 | 0.5 | <0.001 | 0.7 | 0.4 | <0.001 |
| IR | 4.5 | 1.7 | 4.7 | N/A | 4.6 | 1.5 | 4.1 | 1.8 | 4.9 | 2 | |||||
| Groups | Combined | Under Weight | Normal Weight | Overweight | Obese | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Characteristics | Mean | SD | p Value | Mean | SD | Mean | SD | p Value | Mean | SD | p Value | Mean | SD | p Value | |
| LDL (mmol/L) | IS | 2.4 | 0.7 | 0.123 | 2.2 | 0.7 | 2.5 | 0.7 | 0.102 | 2.4 | 0.4 | 0.486 | 2.4 | 0.9 | 0.998 |
| IR | 2.2 | 0.5 | 1.8 | N/A | 2.1 | 0.5 | 2.2 | 0.5 | 2.4 | 0.6 | |||||
| HDL (mmol/L) | IS | 1.4 | 0.3 | 0.049 | 1.6 | 0.4 | 1.5 | 0.4 | 0.867 | 1.3 | 0.3 | 0.581 | 1.2 | 0.2 | 0.427 |
| IR | 1.3 | 0.4 | 1.5 | N/A | 1.4 | 0.3 | 1.2 | 0.4 | 1.1 | 0.2 | |||||
| Triglyceride (mmol/L) | IS | 0.7 | 0.2 | <0.001 | 0.7 | 0.2 | 0.7 | 0.2 | 0.027 | 0.8 | 0.2 | 0.159 | 0.8 | 0.3 | 0.115 |
| IR | 1.0 | 0.4 | 0.7 | N/A | 0.9 | 0.4 | 1.0 | 0.5 | 1.0 | 0.3 | |||||
| Cholesterol (mmol/L) | IS | 4.2 | 0.9 | 0.147 | 4.2 | 1.0 | 4.3 | 0.9 | 0.288 | 4.0 | 0.6 | 0.694 | 3.9 | 1.0 | 0.972 |
| IR | 3.9 | 0.7 | 3.6 | N/A | 4.0 | 0.8 | 3.9 | 0.7 | 3.9 | 0.8 | |||||
| APoA (g/L) | IS | 0.6 | 0.7 | 0.494 | 0.6 | 0.5 | 0.5 | 0.6 | 0.204 | 0.9 | 0.9 | 0.673 | 0.7 | 0.4 | 0.372 |
| IR | 0.7 | 0.7 | 0.4 | N/A | 0.3 | 0.2 | 1.0 | 1.0 | 0.9 | 0.6 | |||||
| LDL oxidase | IS | 21.2 | 4.4 | 0.031 | 20.4 | 3.2 | 21.8 | 4.0 | 0.625 | 20.1 | 6.1 | 0.218 | 20.6 | 3.1 | 0.174 |
| IR | 23.5 | 4.7 | 27.2 | N/A | 22.6 | 3.2 | 22.7 | 3.4 | 25.2 | 7.7 | |||||
| Leptin (ng/mL) | IS | 3.4 | 1.5 | 0.262 | 4.2 | 1.6 | 3.6 | 1.5 | 0.169 | 2.5 | 1.0 | 0.077 | 4.1 | 1.9 | 0.987 |
| IR | 3.8 | 1.4 | 4.8 | N/A | 4.3 | 1.1 | 3.1 | 1.2 | 4.1 | 1.7 | |||||
| Adiponectin (ng/mL) | IS | 21.1 | 7.1 | 0.01 | 23.9 | 6.7 | 22.8 | 7.4 | 0.991 | 20.2 | 7.0 | 0.03 | 17.8 | 6.2 | 0.952 |
| IR | 16.6 | 6.3 | N/A | N/A | 22.7 | 1.0 | 14.8 | 5.6 | 17.6 | 7.0 | |||||
| CRP (mg/L) | IS | 2.4 | 2.7 | 0.077 | 2.1 | 2.6 | 1.7 | 2.3 | 0.744 | 3.4 | 2.7 | 0.957 | 4.5 | 3.9 | 0.726 |
| IR | 3.3 | 3.0 | 1.2 | N/A | 2.0 | 2.8 | 3.4 | 3.0 | 5.1 | 2.9 | |||||
| IL-6 (pg/mL) | IS | 3.0 | 3.5 | 0.758 | 2.9 | 1.7 | 2.7 | 1.9 | 0.167 | 2.7 | 1.0 | 0.147 | 6.2 | 9.8 | 0.359 |
| IR | 2.8 | 1.2 | 4.6 | N/A | 1.9 | 0.7 | 3.3 | 1.3 | 3.1 | 0.9 | |||||
| TNFalpha (pg/mL) | IS | 119.8 | 273.2 | 0.665 | 33.2 | 13.8 | 148.8 | 314.7 | 0.582 | 127.5 | 290.9 | 0.594 | 42.9 | 47.7 | 0.332 |
| IR | 92.3 | 203.9 | N/A | N/A | 22.5 | 5.7 | 76.4 | 199.1 | 129.2 | 238.1 | |||||
| Variables Explaining HOMA-IR | Importance | p Value |
|---|---|---|
| Triglycerides | 0.67 | <0.001 |
| Interleukin-6 | 0.29 | <0.001 |
| Adiponectin | 0.03 | <0.001 |
| HDL | 0.01 | <0.001 |
| TNF-alpha | 0.008 | <0.001 |
| Group | Predictor | Adjusted | Std. Error of the Estimate | p Value | Area Under Curve | (95% CI) |
|---|---|---|---|---|---|---|
| R Square | ||||||
| Normal weight | TG | 0.23 | 1.2 | 0.01 | 0.61 | (0.41–0.81) |
| Overweight | TG/HDL | 0.22 | 1.3 | 0.01 | 0.66 | (0.47–0.85) |
| Obese | TG/HDL | 0.44 | 2 | 0.01 | 0.78 | (0.57–0.99) |
| All groups | TG/HDL | 0.31 | 1.4 | <0.001 | 0.7 | (0.60–0.80) |
| TG/HDL and Free fat mass | 0.37 | 1.4 | 0.02 | 0.68 | (0.57–0.79) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Elrayess, M.A.; Rizk, N.M.; Fadel, A.S.; Kerkadi, A. Prevalence and Predictors of Insulin Resistance in Non-Obese Healthy Young Females in Qatar. Int. J. Environ. Res. Public Health 2020, 17, 5088. https://doi.org/10.3390/ijerph17145088
Elrayess MA, Rizk NM, Fadel AS, Kerkadi A. Prevalence and Predictors of Insulin Resistance in Non-Obese Healthy Young Females in Qatar. International Journal of Environmental Research and Public Health. 2020; 17(14):5088. https://doi.org/10.3390/ijerph17145088
Chicago/Turabian StyleElrayess, Mohamed A., Nasser M. Rizk, Amina S. Fadel, and Abdelhamid Kerkadi. 2020. "Prevalence and Predictors of Insulin Resistance in Non-Obese Healthy Young Females in Qatar" International Journal of Environmental Research and Public Health 17, no. 14: 5088. https://doi.org/10.3390/ijerph17145088
APA StyleElrayess, M. A., Rizk, N. M., Fadel, A. S., & Kerkadi, A. (2020). Prevalence and Predictors of Insulin Resistance in Non-Obese Healthy Young Females in Qatar. International Journal of Environmental Research and Public Health, 17(14), 5088. https://doi.org/10.3390/ijerph17145088






