The Use of Added Salt and Sugar in the Diet of Polish and Austrian Toddlers. Associated Factors and Dietary Patterns, Feeding and Maternal Practices
Abstract
1. Introduction
2. Materials and Methods
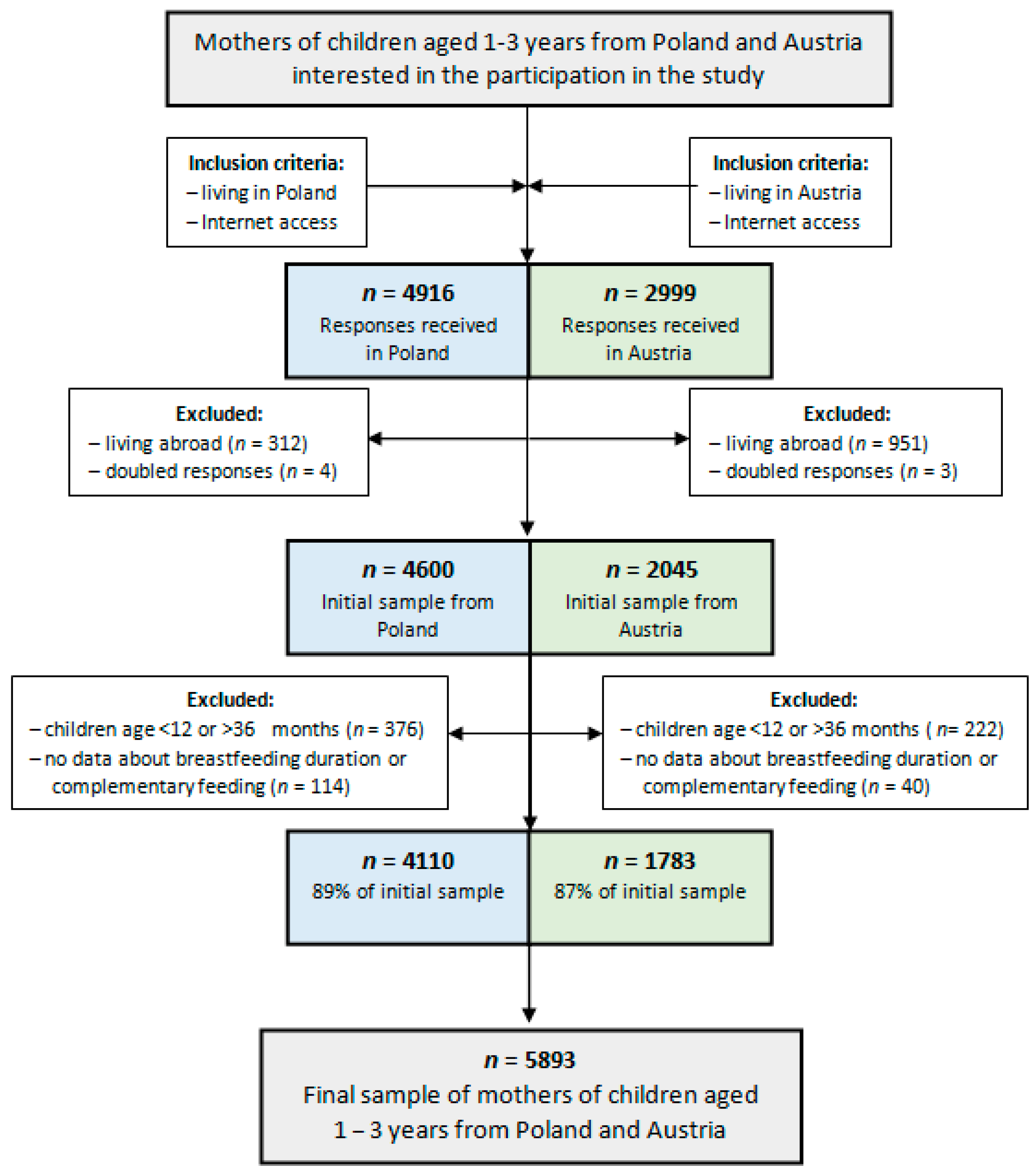
2.1. Study Design and Participants
2.2. Questionnaire
2.2.1. Demographic Data
2.2.2. Early Feeding Practices
2.2.3. Toddlers’ Dietary Habits
2.3. Statistical Analysis
3. Results
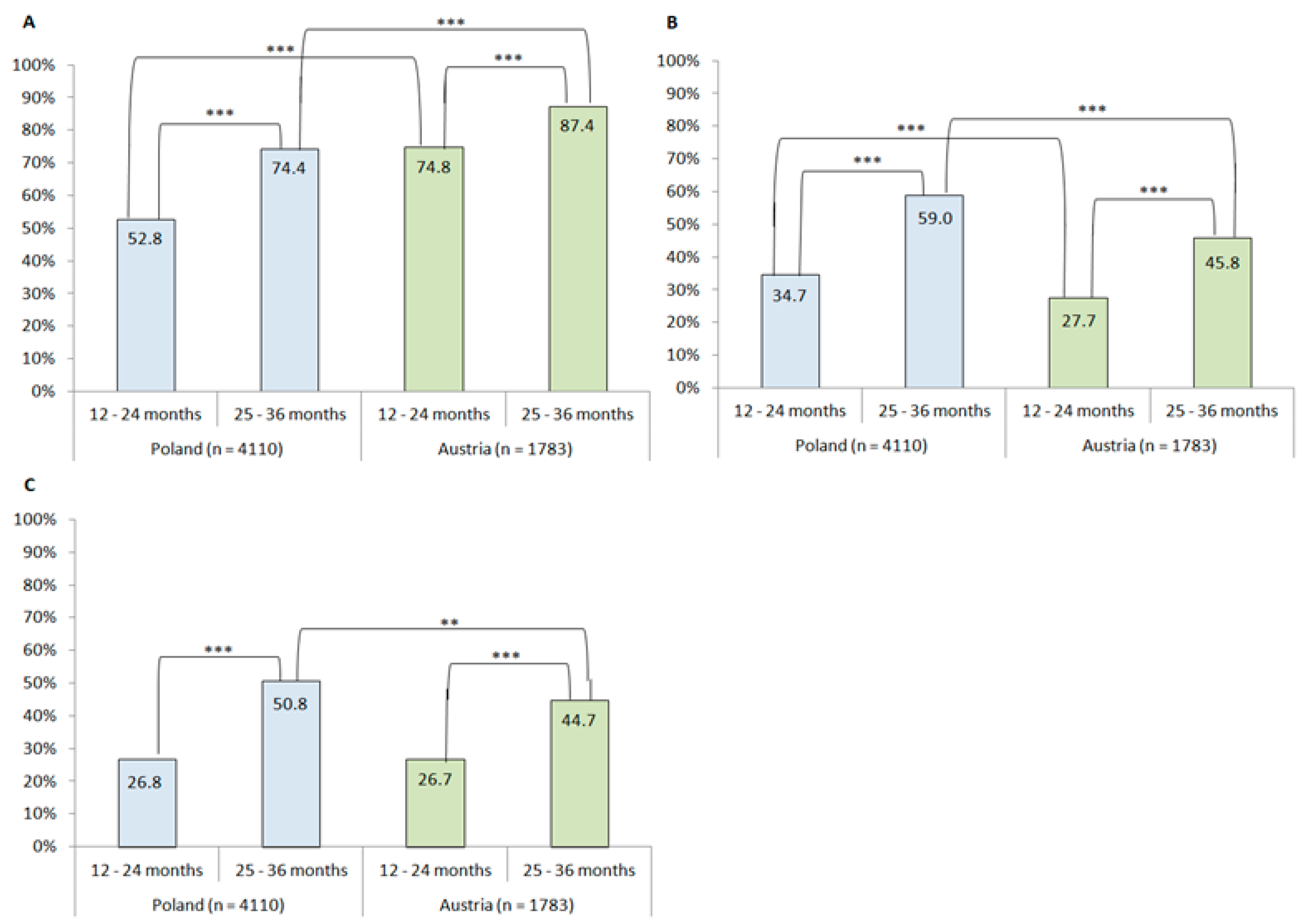
3.1. Use of Added Salt, Sugar and Both Salt and Sugar
3.2. Factors Associated with the Use of Added Salt, Sugar and Both Salt and Sugar in Toddlers’ Diets
3.2.1. Sociodemographic Factors
3.2.2. Early Feeding Factors
3.3. Current Toddlers’ Dietary Habits, Maternal Concerns and Feeding Practices According to the Use of Added Salt, Sugar and Both Salt and Sugar
3.4. Sources of Knowledge about Children’s Feeding According to the Use of Added Salt, Sugar and Both Salt and Sugar
4. Discussion
4.1. Prevalence of the Use of Added Salt and Sugar in the Toddlers’ Diets
4.2. Sociodemographic Factors Associated with the Use of Added Salt and Sugar in the Toddlers’ Diets
4.3. Early Feeding Factors Associated with the Use of Added Salt and Sugar in the Toddlers’ Diet
4.4. The Use of Added Salt and Sugar and Toddlers’ Dietary Habits and Maternal Concerns About Eating
4.5. Sources of Knowledge About Children’s Feeding
4.6. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| aOR | Adjusted odds ratio |
| AS | Added salt |
| AS&Su | Added salt and sugar |
| ASu | Added sugar |
| BF | Breastfeeding |
| BLW | Baby led weaning |
| CF | Complementary foods |
| CFI | Complementary feeding introduction |
| CI | Confidence interval |
| DOHaD | Developmental Origins of Health and Disease hypothesis |
| EBF | Exclusive breastfeeding |
| EFSA | European Food Safety Authority |
| GDP | Gross domestic product |
| OR | Odds ratio |
| TSF | Traditional spoon-feeding |
References
- Baird, J.; Jacob, C.; Barker, M.; Fall, C.H.D.; Hanson, M.; Harvey, N.C.; Inskip, H.M.; Kumaran, K.; Cooper, C. Developmental origins of health and disease: A lifecourse approach to the prevention of non-communicable diseases. Healthcare 2017, 5, 14. [Google Scholar] [CrossRef] [PubMed]
- De Cosmi, V.; Scaglioni, S.; Agostoni, C. Early taste experiences and later food choices. Nutrients 2017, 9, 107. [Google Scholar] [CrossRef] [PubMed]
- Reidy, K.C.; Deming, D.M.; Briefel, R.R.; Fox, M.K.; Saavedra, J.M.; Eldridge, A.L. Early development of dietary patterns: Transitions in the contribution of food groups to total energy—Feeding Infants and Toddlers Study, 2008. BMC Nutr. 2017, 3, 5. [Google Scholar] [CrossRef]
- Daniels, L.A. Feeding practices and parenting: A pathway to child health and family happiness. Ann. Nutr. Metab. 2019, 74, 29–42. [Google Scholar] [CrossRef]
- Venditti, C.; Musa-Veloso, K.; Lee, H.Y.; Poon, T.; Mak, A.; Darch, M.; Juana, J.; Fronda, D.; Noori, D.; Pateman, E.; et al. Determinants of sweetness preference: A scoping review of human studies. Nutrients 2020, 12, 718. [Google Scholar] [CrossRef]
- Liem, D.G. Infants’ and children’s salt taste perception and liking: A review. Nutrients 2017, 9, 1011. [Google Scholar] [CrossRef]
- Gidding, S.S.; Dennison, B.A.; Birch, L.L.; Daniels, S.R.; Gilman, M.W.; Lichtenstein, A.H.; Rattay, K.T.; Steinberger, J.; Stettler, N.; Van Horn, L. Dietary recommendations for children and adolescents: A guide for practitioners: Consensus statement from the American Heart Association. Circulation 2005, 112, 2061–2075. [Google Scholar] [CrossRef]
- Fewtrell, M.; Bronsky, J.; Campoy, C.; Domellöf, M.; Embleton, N.; Mis, N.F.; Hojsak, I.; Hulst, J.M.; Indrio, F.; Lapillonne, A.; et al. Complementary feeding: A position paper by the European Society for Paediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) committee on nutrition. J. Pediatr. Gastroenterol. Nutr. 2017, 64, 119–132. [Google Scholar] [CrossRef]
- Fidler Mis, N.; Braegger, C.; Bronsky, J.; Campoy, C.; Domellöf, M.; Embleton, N.D.; Hojsak, I.; Hulst, J.; Indrio, F.; Lapillonne, A.; et al. Sugar in infants, children and adolescents: A position paper of the European Society for Paediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition. J. Pediatr. Gastroenterol. Nutr. 2017, 65, 681–696. [Google Scholar] [CrossRef]
- WHO. Commercial Foods for Infants and Young Children in the WHO European Region. A Study of the Availability, Composition and Marketing of Baby Foods in Four European Countries; World Health Organization: Geneva, Switzerland, 2019. [Google Scholar]
- Leyvraz, M.; Chatelan, A.; da Costa, B.R.; Taffé, P.; Paradis, G.; Bovet, P.; Bochud, M.; Chiolero, A. Sodium intake and blood pressure in children and adolescents: A systematic review and meta-analysis of experimental and observational studies. Int. J. Epidemiol. 2018, 47, 1796–1810. [Google Scholar] [CrossRef]
- Vos, M.B.; Kaar, J.L.; Welsh, J.A.; Van Horn, L.V.; Feig, D.I.; Anderson, C.A.M.; Patel, M.J.; Cruz Munos, J.; Krebs, N.F.; Xanthakos, S.A.; et al. Added sugars and cardiovascular disease risk in children: A scientific statement from the American Heart Association. Circulation 2017, 135, e1017–e1034. [Google Scholar] [CrossRef] [PubMed]
- Moosavian, S.P.; Haghighatdoost, F.; Surkan, P.J.; Azadbakht, L. Salt and obesity: A systematic review and meta-analysis of observational studies. Int. J. Food Sci. Nutr. 2017, 68, 265–277. [Google Scholar] [CrossRef] [PubMed]
- Poorolajal, J.; Sahraei, F.; Mohamdadi, Y.; Doosti-Irani, A.; Moradi, L. Behavioral factors influencing childhood obesity: A systematic review and meta-analysis. Obes. Res. Clin. Pract. 2020, 14, 109–118. [Google Scholar] [CrossRef] [PubMed]
- Peres, M.A.; Sheiham, A.; Liu, P.; Demarco, F.F.; Silva, A.E.R.; Assunção, M.C.; Menezes, A.M.; Barros, F.C.; Peres, K.G. Sugar consumption and changes in dental caries from childhood to adolescence. J. Dent. Res. 2016, 95, 388–394. [Google Scholar] [CrossRef] [PubMed]
- Noble, E.E.; Hsu, T.M.; Jones, R.B.; Fodor, A.A.; Goran, M.I.; Kanoski, S.E. Early-life sugar consumption affects the rat microbiome independently of obesity. J. Nutr. 2017, 147, 20–28. [Google Scholar] [CrossRef]
- Rinninella, E.; Cintoni, M.; Raoul, P.; Lopetuso, L.R.; Scaldaferri, F.; Pulcini, G.; Miggiano, G.A.D.; Gasbarrini, A.; Mele, M.C. Food components and dietary habits: Keys for a healthy gut microbiota composition. Nutrients 2019, 11, 2393. [Google Scholar] [CrossRef]
- Stiemsma, L.T.; Michels, K.B. The Role of the microbiome in the developmental origins of health and disease. Pediatrics 2018, 141. [Google Scholar] [CrossRef]
- Nehring, I.; Kostka, T.; von Kries, R.; Rehfuess, E.A. Impacts of in utero and early infant taste experiences on later taste acceptance: A systematic review. J. Nutr. 2015, 145, 1271–1279. [Google Scholar] [CrossRef]
- Stein, L.J.; Cowart, B.J.; Beauchamp, G.K. The development of salty taste acceptance is related to dietary experience in human infants: A prospective study. Am. J. Clin. Nutr. 2012, 94, 123–129. [Google Scholar] [CrossRef]
- Brown, I.J.; Tzoulaki, I.; Candeias, V.; Elliott, P. Salt intakes around the world: Implications for public health. Int. J. Epidemiol. 2009, 38, 791–813. [Google Scholar] [CrossRef]
- Foterek, K.; Buyken, A.E.; Bolzenius, K.; Hilbig, A.; Nöthlings, U.; Alexy, U. Commercial complementary food consumption is prospectively associated with added sugar intake in childhood. Br. J. Nutr. 2016, 115, 2067–2074. [Google Scholar] [CrossRef]
- Kyttälä, P.; Erkkola, M.; Kronberg-Kippilä, C.; Tapanainen, H.; Veijola, R.; Simell, O.; Knip, M.; Virtanen, S.M. Food consumption and nutrient intake in Finnish 1–6-year-old children. Public Health Nutr. 2010, 13, 947–956. [Google Scholar] [CrossRef] [PubMed]
- Grimes, C.A.; Campbell, K.J.; Riddell, L.J.; Nowson, C.A. Sources of sodium in Australian children’s diets and the effect of the application of sodium targets to food products to reduce sodium intake. Br. J. Nutr. 2011, 105, 468–477. [Google Scholar] [CrossRef] [PubMed]
- Campbell, K.J.; Hendrie, G.; Nowson, C.; Grimes, C.A.; Riley, M.; Lioret, S.; McNaughton, S.A. Sources and correlates of sodium consumption in the first 2 years of life. J. Acad. Nutr. Diet. 2014, 114, 1525–1532. [Google Scholar] [CrossRef]
- Cribb, V.L.; Warren, J.M.; Emmett, P.M. Contribution of inappropriate complementary foods to the salt intake of 8-month-old infants. Eur. J. Clin. Nutr. 2012, 66, 104–110. [Google Scholar] [CrossRef]
- Bournez, M.; Ksiazek, E.; Charles, M.A.; Lioret, S.; Brindisi, M.C.; De Lauzon-Guillain, B.; Nicklaus, S. Frequency of use of added sugar, salt, and fat in infant foods up to 10 months in the nationwide ELFE cohort study: Associated infant feeding and caregiving practices. Nutrients 2019, 11, 733. [Google Scholar] [CrossRef] [PubMed]
- Verduci, E.; Banderali, G.; Montanari, C.; Canani, R.B.; Caserta, L.C.; Corsello, G.; Mosca, F.; Piazzolla, R.; Rescigno, M.; Terracciano, L.; et al. Childhood dietary intake in Italy: The epidemiological “MY FOOD DIARY” survey. Nutrients 2019, 11, 1129. [Google Scholar] [CrossRef] [PubMed]
- Pietrobelli, A.; Agosti, M.; Palmer, C.; Pereira-Da-Silva, L.; Rego, C.; Rolland-Cacherà, M.F.; Zuccotti, G. Nutrition in the first 1000 days: Ten practices to minimize obesity emerging from published science. Int. J. Environ. Res. Public Health 2017, 14, 1491. [Google Scholar] [CrossRef]
- Song, P.; Zhang, Y.; Yu, J.; Zha, M.; Zhu, Y.; Rahimi, K.; Rudan, I. Global prevalence of hypertension in children: A systematic review and meta-analysis. JAMA Pediatr. 2019, 173, 1154–1163. [Google Scholar] [CrossRef]
- Zielinska, M.A.; Rust, P.; Masztalerz-Kozubek, D.; Bichler, J.; Hamulka, J. Factors Influencing the Age of Complementary Feeding—A Cross-Sectional Study from Two European Countries. Int. J. Environ. Res. Public Health 2019, 16, 3799. [Google Scholar] [CrossRef]
- Eurostat. GDP at Regional Level. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php/GDP_at_regional_level#Regional_GDP_per_capita (accessed on 27 May 2020).
- WHO. The World Health Organization’s Infant Feeding Recommendation. Available online: https://www.who.int/nutrition/topics/infantfeeding_recommendation/en/ (accessed on 26 May 2020).
- Fein, S.B.; Labiner-Wolfe, J.; Scanlon, K.S.; Grummer-Strawn, L.M. Selected complementary feeding practices and their association with maternal education. Pediatrics 2008, 122, S91–S97. [Google Scholar] [CrossRef]
- Bandara, T.; Hettiarachchi, M.; Liyanage, C.; Amarasena, S. Current infant feeding practices and impact on growth in babies during the second half of infancy. J. Hum. Nutr. Diet. 2015, 28, 366–374. [Google Scholar] [CrossRef]
- EFSA. Dietary Salt/Sodium. Available online: https://ec.europa.eu/jrc/en/health-knowledge-gateway/promotion-prevention/nutrition/salt (accessed on 27 May 2020).
- Herrick, K.A.; Fryar, C.D.; Hamner, H.C.; Park, S.; Ogden, C.L. Added sugars intake among US infants and toddlers. J. Acad. Nutr. Diet. 2019, 120, 23–32. [Google Scholar] [CrossRef]
- Erickson, L.W.; Taylor, R.W.; Haszard, J.J.; Fleming, E.A.; Daniels, L.; Morison, B.J.; Leong, C.; Fangupo, L.J.; Wheeler, B.J.; Taylor, B.J.; et al. Impact of a modified version of baby-led weaning on infant food and nutrient intakes: The BLISS randomized controlled trial. Nutrients 2018, 10, 740. [Google Scholar] [CrossRef]
- Wang, Y.; Guglielmo, D.; Welsh, J.A. Consumption of sugars, saturated fat, and sodium among US children from infancy through preschool age, NHANES 2009-2014. Am. J. Clin. Nutr. 2018, 108, 868–877. [Google Scholar] [CrossRef]
- Marinho, A.R.; Severo, M.; Correia, D.; Lobato, L.; Vilela, S.; Oliveira, A.; Ramos, E.; Torres, D.; Lopes, C. Total, added and free sugar intakes, dietary sources and determinants of consumption in Portugal: The National Food, Nutrition and Physical Activity Survey (IAN-AF 2015-2016). Public Health Nutr. 2019, 23, 869–881. [Google Scholar] [CrossRef]
- Perrar, I.; Schmitting, S.; Della Corte, K.W.; Buyken, A.E.; Alexy, U. Age and time trends in sugar intake among children and adolescents: Results from the DONALD study. Eur. J. Nutr. 2019, 59, 1043–1054. [Google Scholar] [CrossRef]
- Brion, M.J.; Ness, A.R.; Davey Smith, G.; Emmett, P.; Rogers, I.; Whincup, P.; Lawlor, D.A. Sodium intake in infancy and blood pressure at 7 years: Findings from the Avon longitudinal study of parents and children. Eur. J. Clin. Nutr. 2008, 62, 1162–1169. [Google Scholar] [CrossRef]
- Weker, H.; Brudnicka, E.; Barańska, M.; Rowicka, G.; Strucińska, M.; Więch, M.; Dyląg, H.; Klemarczyk, W.; Socha, P.; Mazur, J. Dietary patterns of children aged 1–3 years in Poland in two population studies. Ann. Nutr. Metab. 2019, 75, 66–76. [Google Scholar] [CrossRef] [PubMed]
- Bailey, R.L.; Fulgoni, V.L.; Cowan, A.E.; Gaine, P.C. Sources of added sugars in young children, adolescents, and adults with low and high intakes of added sugars. Nutrients 2018, 10, 102. [Google Scholar] [CrossRef]
- Amoutzopoulos, B.; Steer, T.; Roberts, C.; Collins, D.; Page, P. Free and added sugar consumption and adherence to guidelines: The UK national diet and nutrition survey (2014/15–2015/16). Nutrients 2020, 12, 393. [Google Scholar] [CrossRef]
- Quader, Z.S.; Gillespie, C.; Sliwa, S.A.; Ahuja, J.K.C.; Burdg, J.P.; Moshfegh, A.; Pehrsson, P.R.; Gunn, J.P.; Mugavero, K.; Cogswell, M.E. Sodium Intake among US School-Aged Children: National Health and Nutrition Examination Survey, 2011–2012. J. Acad. Nutr. Diet. 2017, 176, 139–148. [Google Scholar] [CrossRef]
- Yuan, W.L.; Nicklaus, S.; Lioret, S.; Lange, C.; Forhan, A.; Heude, B.; Charles, M.A.; De Lauzon-Guillain, B. Early factors related to carbohydrate and fat intake at 8 and 12 months: Results from the EDEN mother-child cohort. Eur. J. Clin. Nutr. 2017, 71, 219–226. [Google Scholar] [CrossRef] [PubMed]
- Morinaga, Y.; Tsuchihashi, T.; Ohta, Y.; Matsumura, K. Salt intake in 3-year-old Japanese children. Hypertens. Res. 2011, 34, 836–839. [Google Scholar] [CrossRef]
- Synnott, K.; Bogue, J.; Edwards, C.A.; Scott, J.A.; Higgins, S.; Norin, E.; Frias, D.; Amarri, S.; Adam, R. Parental perceptions of feeding practices in five European countries: An exploratory study. Eur. J. Clin. Nutr. 2007, 61, 946–956. [Google Scholar] [CrossRef] [PubMed]
- Tromp, I.I.M.; Briedé, S.; Kiefte-de Jong, J.C.; Renders, C.M.; Jaddoe, V.W.V.; Franco, O.H.; Hofman, A.; Raat, H.; Moll, H.A. Factors associated with the timing of introduction of complementary feeding: The Generation R Study. Eur. J. Clin. Nutr. 2013, 67, 625–630. [Google Scholar] [CrossRef]
- Klingberg, S.; Ludvigsson, J.; Brekke, H.K. Introduction of complementary foods in Sweden and impact of maternal education on feeding practices. Public Health Nutr. 2017, 20, 1054–1062. [Google Scholar] [CrossRef] [PubMed]
- Gerritsen, S.; Wall, C.R.; Grant, C.C.; Teixeira, J.A.; Marchioni, D.M.; Pillai, A.; Morton, S.M.B.; de Castro, T.G. Inequalities in infant feeding practices among the growing up in New Zealand cohort. Proceedings 2019, 8, 54. [Google Scholar] [CrossRef]
- Maciel, B.L.L.; Moraes, M.L.; Soares, A.M.; Cruz, I.F.S.; De Andrade, M.I.R.; Filho, J.Q.; Junior, F.S.; Costa, P.N.; Abreu, C.B.; Ambikapathi, R.; et al. Infant feeding practices and determinant variables for early complementary feeding in the first 8 months of life: Results from the Brazilian MAL-ED cohort site. Public Health Nutr. 2018, 21, 2462–2470. [Google Scholar] [CrossRef]
- Armstrong, J.; Abraham, E.C.; Squair, M.; Brogan, Y.; Merewood, A. Exclusive breastfeeding, complementary feeding, and food choices in UK infants. J. Hum. Lact. 2014, 30, 201–208. [Google Scholar] [CrossRef]
- de Almeida Fonseca, P.C.; Ribeiro, S.A.V.; Andreoli, C.S.; de Carvalho, C.A.; Pessoa, M.C.; de Novaes, J.F.; Priore, S.E.; Franceschini, S.D.C.C. Association of exclusive breastfeeding duration with consumption of ultra-processed foods, fruit and vegetables in Brazilian children. Eur. J. Nutr. 2019, 58, 2887–2894. [Google Scholar] [CrossRef]
- Kiefte-De Jong, J.C.; De Vries, J.H.; Bleeker, S.E.; Jaddoe, V.W.V.; Hofman, A.; Raat, H.; Moll, H.A. Socio-demographic and lifestyle determinants of “Western-like” and “Health conscious” dietary patterns in toddlers. Br. J. Nutr. 2013, 109, 137–147. [Google Scholar] [CrossRef]
- Fegan, S.; Bassett, E.; Peng, Y.; Steel O’Connor, K. Adherence to complementary feeding recommendations for infants and implications for public health. Public Health Nutr. 2016, 19, 638–649. [Google Scholar] [CrossRef]
- Elliott, C.D.; Conlon, M.J. Packaged baby and toddler foods: Questions of sugar and sodium. Pediatr. Obes. 2015, 10, 149–155. [Google Scholar] [CrossRef] [PubMed]
- Maalouf, J.; Cogswell, M.E.; Bates, M.; Yuan, K.; Scanlon, K.S.; Pehrsson, P.; Gunn, J.P.; Merritt, R.K. Sodium, sugar, and fat content of complementary infant and toddler foods sold in the United States, 2015. Am. J. Clin. Nutr. 2017, 105, 1443–1452. [Google Scholar] [CrossRef] [PubMed]
- Hollis, J.L.; Crozier, S.R.; Inskip, H.M.; Cooper, C.; Godfrey, K.M.; Robinson, S.M. Age at introduction of solid foods and feeding difficulties in childhood: Findings from the Southampton Women’s Survey. Br. J. Nutr. 2016, 116, 743–750. [Google Scholar] [CrossRef]
- Morison, B.J.; Heath, A.L.M.; Haszard, J.J.; Hein, K.; Fleming, E.A.; Daniels, L.; Erickson, E.W.; Fangupo, L.J.; Wheeler, B.J.; Taylor, B.J.; et al. Impact of a modified version of baby-led weaning on dietary variety and food preferences in infants. Nutrients 2018, 10, 1092. [Google Scholar] [CrossRef]
- Morison, B.J.; Taylor, R.W.; Haszard, J.J.; Schramm, C.J.; Erickson, L.W.; Fangupo, L.J.; Fleming, E.A.; Luciano, A.; Heath, A.L.M. How different are baby-led weaning and conventional complementary feeding? A cross-sectional study of infants aged 6-8 months. BMJ Open 2016, 6. [Google Scholar] [CrossRef]
- Rowan, H.; Lee, M.; Brown, A. Differences in dietary composition between infants introduced to complementary foods using Baby-led weaning and traditional spoon feeding. J. Hum. Nutr. Diet. 2019, 32, 11–20. [Google Scholar] [CrossRef]
- Brown, A. Differences in eating behaviour, well-being and personality between mothers following baby-led vs. traditional weaning styles. Matern. Child Nutr. 2016, 12, 826–837. [Google Scholar] [CrossRef]
- Fu, X.; Conlon, C.A.; Haszard, J.J.; Beck, K.L.; von Hurst, P.R.; Taylor, R.W.; Heath, A.L.M. Food fussiness and early feeding characteristics of infants following Baby-Led Weaning and traditional spoon-feeding in New Zealand: An internet survey. Appetite 2018, 130, 110–116. [Google Scholar] [CrossRef]
- Komninou, S.; Halford, J.C.G.; Harrold, J.A. Differences in parental feeding styles and practices and toddler eating behaviour across complementary feeding methods: Managing expectations through consideration of effect size. Appetite 2019, 137, 198–206. [Google Scholar] [CrossRef] [PubMed]
- Grimes, C.A.; Riddell, L.J.; Campbell, K.J.; Nowson, C.A. Dietary salt intake, sugar-sweetened beverage consumption, and obesity risk. Pediatrics 2013, 131, 14–21. [Google Scholar] [CrossRef]
- Marrero, N.M.; He, F.J.; Whincup, P.; MacGregor, G.A. Salt intake of children and adolescents in south london consumption levels and dietary sources. Hypertension 2014, 63, 1026–1032. [Google Scholar] [CrossRef] [PubMed]
- Rios-Leyvraz, M.; Bovet, P.; Bochud, M.; Genin, B.; Russo, M.; Rossier, M.F.; Tabin, R.; Chiolero, A. Estimation of salt intake and excretion in children in one region of Switzerland: A cross-sectional study. Eur. J. Nutr. 2019, 58, 2921–2928. [Google Scholar] [CrossRef] [PubMed]
- Mallan, K.M.; Fildes, A.; Magarey, A.M.; Daniels, L.A. The relationship between number of fruits, vegetables, and noncore foods tried at age 14 months and food preferences, dietary intake patterns, fussy eating behavior, and weight status at age 3.7 years. J. Acad. Nutr. Diet. 2016, 116, 630–637. [Google Scholar] [CrossRef] [PubMed]
- Khokhar, D.; Nowson, C.A.; Margerison, C.; Bolam, B.; Grimes, C.A. Knowledge and attitudes are related to selected salt-specific behaviours among Australian parents. Nutrients 2018, 10, 720. [Google Scholar] [CrossRef] [PubMed]
- Mennella, J.A.; Finkbeiner, S.; Lipchock, S.V.; Hwang, L.-D.; Reed, D.R. Preferences for salty and sweet tastes are elevated and related to each other during childhood. PLoS ONE 2014, 9, e92201. [Google Scholar] [CrossRef] [PubMed]
- Bouhlal, S.; Issanchou, S.; Nicklaus, S. The impact of salt, fat and sugar levels on toddler food intake. Br. J. Nutr. 2011, 105, 645–653. [Google Scholar] [CrossRef]
- Eurostat Individuals—Internet Use. Available online: https://appsso.eurostat.ec.europa.eu/nui/show.do?dataset=isoc_ci_ifp_iu&lang=en (accessed on 25 May 2020).
- Li, R.; Scanlon, K.S.; Serdula, M.K. The validity and reliability of maternal recall of breastfeeding practice. Nutr. Rev. 2005, 63, 103–110. [Google Scholar] [CrossRef]
- Herrmann, D.; Suling, M.; Reisch, L.; Siani, A.; De Bourdeaudhuij, I.; Maes, L.; Santaliestra-Pasías, A.M.; Veidebaum, T.; Molnár, D.; Pala, V.; et al. Repeatability of maternal report on prenatal, perinatal and early postnatal factors: Findings from the IDEFICS parental questionnaire. Int. J. Obes. 2011, 35, 52–60. [Google Scholar] [CrossRef] [PubMed]
- Natland, S.T.; Andersen, L.F.; Nilsen, T.I.L.; Forsmo, S.; Jacobsen, G.W. Maternal recall of breastfeeding duration twenty years after delivery. BMC Med. Res. Methodol. 2012, 12, 179. [Google Scholar] [CrossRef] [PubMed]
- Van Zyl, Z.; Maslin, K.; Dean, T.; Blaauw, R.; Venter, C. The accuracy of dietary recall of infant feeding and food allergen data. J. Hum. Nutr. Diet. 2016, 29, 777–785. [Google Scholar] [CrossRef] [PubMed]
| Variables | Poland (n = 4110)% | Austria (n = 1783)% | ||||
|---|---|---|---|---|---|---|
| 12–24 Months (n = 2680) | 25–36 Months (n = 1430) | p-Value | 12–24 Months (n = 941) | 25–36 Months (n = 842) | p-Value | |
| Maternal age: | ≤0.001 | ≤0.001 | ||||
| <25 years | 5.3 | 3.4 | 6.4 | 2.7 | ||
| 25–29 years | 36.5 | 24.8 | 28.4 | 23.3 | ||
| 30–34 years | 44.7 | 53.4 | 39.4 | 40.1 | ||
| 35–39 years | 12.2 | 16.4 | 22.4 | 27.2 | ||
| ≥40 years | 1.3 | 2 | 3.4 | 6.7 | ||
| Maternal education: | 0.294 | 0.557 | ||||
| Primary and vocational | 1.1 | 0.7 | 27.2 | 25.1 | ||
| High school | 12 | 11 | 3.4 | 3.8 | ||
| University | 86.9 | 88.3 | 69.4 | 71.1 | ||
| Household size: | ≤0.001 | ≤0.001 | ||||
| 2 persons | 2 | 2 | 1.5 | 3 | ||
| 3 persons | 66.8 | 52.1 | 55.5 | 36.2 | ||
| 4 persons | 23.6 | 38.3 | 30.9 | 46.3 | ||
| 5 persons | 5.5 | 5.7 | 8.5 | 10.1 | ||
| ≥6 persons | 2.1 | 1.9 | 3.6 | 4.4 | ||
| Parity: | ≤0.001 | ≤0.001 | ||||
| Primiparas | 73.3 | 55.8 | 57.1 | 38.2 | ||
| Multiparas | 26.7 | 44.2 | 42.9 | 61.8 | ||
| Living area: | 0.601 | 0.839 | ||||
| Rural | 17.5 | 16.9 | 56.5 | 56.1 | ||
| Urban | 82.5 | 83.1 | 43.5 | 43.9 | ||
| Living macroeconomic region (GDP EU-28 average): | 0.339 | 0.495 | ||||
| 47–50% | 14.4 | 12.7 | - | - | ||
| 51–100% | 62.3 | 63.2 | 5.7 | 5.3 | ||
| 101–110% | 23.3 | 24.1 | 43.6 | 40.3 | ||
| 111–130% | - | - | 25.8 | 26.7 | ||
| 131–150% | - | - | 9.3 | 11.3 | ||
| >150% | - | - | 15.6 | 16.4 | ||
| Average monthly income per capita 1: | 0.468 | 0.008 | ||||
| 1st category | 1.5 | 1.5 | 8.3 | 8.7 | ||
| 2nd category | 15 | 13.5 | 20.6 | 21 | ||
| 3rd category | 32.7 | 32.8 | 33.5 | 29.3 | ||
| 4th category | 17.7 | 16.6 | 27.5 | 25.1 | ||
| 5th category | 11.6 | 13.3 | 8.5 | 12.9 | ||
| 6th category | 21.5 | 22.3 | 1.6 | 3 | ||
| Infant gender: | 0.628 | 0.211 | ||||
| Girl | 48.1 | 47.3 | 51.5 | 48.6 | ||
| Boy | 51.9 | 52.7 | 48.5 | 51.4 | ||
| Timing of CFI: | ≤0.001 | 0.878 | ||||
| <4 months | 2 | 3.4 | 4.3 | 4.5 | ||
| 4–6 months | 59.4 | 62.6 | 74.9 | 75.5 | ||
| ≥7 months | 38.6 | 34 | 20.8 | 20 | ||
| Complementary feeding method: | 0.004 | 0.076 | ||||
| TSF | 26.9 | 30.2 | 38.9 | 33.7 | ||
| mixed | 56.6 | 51.1 | 47.7 | 51.4 | ||
| BLW | 16.5 | 18.7 | 13.4 | 14.9 | ||
| Types of CF: | 0.228 | 0.733 | ||||
| Ready-to-eat foods | 22 | 21.7 | 22.7 | 24 | ||
| Homemade foods | 48.5 | 46.2 | 51.5 | 51.4 | ||
| Family foods | 29.5 | 32 | 25.8 | 24.6 | ||
| Currently BF: | ≤0.001 | ≤0.001 | ||||
| No | 38.8 | 72 | 62.4 | 81 | ||
| Yes | 61.2 | 28 | 37.6 | 19 | ||
| EBF duration: | ≤0.001 | 0.506 | ||||
| Never BF | 5.3 | 5.5 | 8.1 | 9.5 | ||
| Never EBF | 50 | 51.4 | 32.1 | 28.3 | ||
| 1–3 months | 1.9 | 2.4 | 6.3 | 7.5 | ||
| 4–5 months | 7.8 | 11.3 | 25.5 | 25.7 | ||
| 6–7 months | 34.7 | 28.6 | 25.5 | 26.7 | ||
| >7 months | 0.3 | 0.8 | 2.5 | 2.6 | ||
| Factors | Variable | 12–24 Months | 25–36 Months | ||||
|---|---|---|---|---|---|---|---|
| (n = 2680) | (n = 1430) | ||||||
| AS aOR (95% CI) | ASu aOR (95% CI) | AS&Su aOR (95% CI) | AS aOR (95% CI) | ASu aOR (95% CI) | AS&Su aOR (95% CI) | ||
| Sociodemographic Factors | Toddler age: | 1.18 (1.15–1.21) *** | 1.14 (1.11–1.17) *** | 1.16 (1.13–1.19) *** | 1.01 (0.98–1.05) | 1.02 (0.99–1.05) | 1.01 (0.98–1.04) |
| Maternal age: | |||||||
| < 25 years | 0.91 (0.61–1.38) | 1.34 (0.89–2.02) | 1.09 (0.70–1.70) | 1.07 (0.48–2.38) | 2.72 (1.31–5.65) ** | 2.22 (1.12–4.37) * | |
| 25–29 years | 1.01 (0.84–1.22) | 1.11 (0.91–1.34) | 1.11 (0.91–1.37) | 1.23 (0.90–1.69) | 1.49 (1.13–1.96) ** | 1.43 (1.09–1.87) ** | |
| 30–34 years | 1 | 1 | 1 | 1 | 1 | 1 | |
| 35–39 years | 0.98 (0.75–1.28) | 0.79 (0.60–1.05) | 0.80 (0.59–1.08) | 1.36 (0.95–1.94) | 0.92 (0.68–1.25) | 1.11 (0.82–1.50) | |
| ≥ 40 years | 0.59 (0.28–1.23) | 0.20 (0.07–0.59) ** | 0.27 (0.09–0.83) * | 1.54 (0.60–3.94) | 0.71 (0.33–1.52) | 0.88 (0.41–1.92) | |
| Maternal education: | |||||||
| Primary and vocational | 2.03 (0.83–4.96) | 1.39 (0.63–3.05) | 2.11 (0.94–4.72) | 2.29 (0.28–19.06) | 1.15 (0.27–4.85) | 1.65 (0.40–6.84) | |
| High school | 1.08 (0.83–1.42) | 1.04 (0.79–1.36) | 1.18 (0.88–1.57) | 1.65 (1.03–2.64) * | 0.86 (0.59–1.26) | 1.00 (0.69–1.45) | |
| University | 1 | 1 | 1 | 1 | 1 | 1 | |
| Parity: | |||||||
| Primiparas | 1 | 1 | 1 | 1 | 1 | 1 | |
| Multiparas | 1.80 (1.47–2.20) *** | 1.37 (1.12–1.67) ** | 1.55 (1.26–1.92) *** | 1.32 (1.01–1.71) * | 1.37 (1.09–1.72) ** | 1.38 (1.10–1.73) ** | |
| Living area: | |||||||
| Rural | 1.02 (0.82–1.27) | 1.12 (0.90–1.40) | 1.10 (0.87–1.39) | 1.08 (0.76–1.52) | 1.17 (0.87–1.58) | 1.15 (0.86–1.54) | |
| Urban | 1 | 1 | 1 | 1 | 1 | 1 | |
| Macroeconomic region (GDP EU-28 average): | |||||||
| 47–50% | 1.07 (0.81–1.42) | 0.83 (0.62–1.11) | 0.79 (0.57–1.07) | 0.86 (0.55–1.34) | 1.05 (0.71–1.55) | 0.95 (0.65–1.39) | |
| 51–100% | 0.99 (0.80–1.21) | 0.93 (0.76–1.15) | 0.86 (0.69–1.07) | 0.98 (0.73–1.33) | 1.13 (0.87–1.47) | 1.11 (0.86–1.44) | |
| 101–110% | 1 | 1 | 1 | 1 | 1 | 1 | |
| Average monthly income per capita (PLN): | |||||||
| <500 | 1.35 (0.64–2.84) | 0.94 (0.45–2.00) | 1.55 (0.71–3.37) | 2.23 (0.61–8.08) | 1.67 (0.57–4.86) | 2.02 (0.74–5.54) | |
| 500–1000 | 1.26 (0.90–1.75) | 1.30 (0.92–1.82) | 1.62 (1.12–2.36) * | 1.16 (0.71–1.89) | 0.85 (0.55–1.32) | 0.94 (0.61–1.44) | |
| 1001–2000 | 1.13 (0.85–1.49) | 1.15 (0.86–1.53) | 1.30 (0.94–1.80) | 1.17 (0.79–1.73) | 0.83 (0.58–1.19) | 0.94 (0.66–1.34) | |
| 2001–2500 | 1.40 (1.03–1.90) * | 1.36 (0.99–1.86) | 1.71 (1.21–2.42) ** | 1.32 (0.84–2.06) | 1.01 (0.67–1.51) | 1.02 (0.69–1.51) | |
| 2501–3000 | 1 | 1 | 1 | 1 | 1 | 1 | |
| ≥3001 | 0.93 (0.69–1.25) | 0.94 (0.69–1.28) | 1.09 (0.77–1.55) | 1.20 (0.79–1.81) | 0.88 (0.61–1.28) | 0.87 (0.60–1.26) | |
| Feeding-Related Factors | Timing of CFI: | ||||||
| <4 months | 1.24 (0.51–1.74) | 1.01 (0.55–1.85) | 0.82 (0.42–1.59) | 1.31 (0.57–2.97) | 0.69 (0.36–1.33) | 0.80 (0.41–1.54) | |
| 4–6 months | 1.09 (0.91–1.32) | 0.94 (0.78–1.14) | 1.04 (0.84–1.28) | 1.14 (0.86–1.52) | 1.10 (0.85–1.43) | 1.20 (0.93–1.54) | |
| ≥7 months | 1 | 1 | 1 | 1 | 1 | 1 | |
| Complementary feeding method: | |||||||
| TSF | 1.28 (1.04–1.58) * | 0.95 (0.77–1.17) | 1.03 (0.82–1.30) | 1.06 (0.77–1.45) | 1.09 (0.83–1.44) | 1.06 (0.81–1.39) | |
| Mixed | 1 | 1 | 1 | 1 | 1 | 1 | |
| BLW | 0.70 (0.55–0.90) ** | 0.95 (0.74–1.22) | 0.81 (0.61–1.08) | 0.69 (0.49–0.98) * | 0.61 (0.44–0.83) ** | 0.63 (0.46–0.87) ** | |
| Types of CF: | |||||||
| Commercial | 1.18 (0.90–1.54) | 0.79 (0.60–1.03) | 0.88 (0.66–1.19) | 0.60 (0.40–1.34) | 0.74 (0.52–1.06) | 0.76 (0.53–1.08) | |
| Homemade | 1.01 (0.82–1.25) | 0.93 (0.75–1.16) | 1.04 (0.82–1.32) | 0.73 (0.53–1.01) | 0.80 (0.60–1.06) | 0.78 (0.59–1.03) | |
| Family | 1 | 1 | 1 | 1 | 1 | 1 | |
| Currently BF: | |||||||
| No | 1.08 (0.89–1.30) | 1.02 (0.84–1.24) | 1.02 (0.83–1.26) | 1.71 (1.27–2.29) *** | 0.96 (0.73–1.27) | 1.15 (0.88–1.51) | |
| Yes | 1 | 1 | 1 | 1 | 1 | 1 | |
| EBF duration: | |||||||
| Never BF | 1.06 (0.70–1.60) | 1.65 (1.10–2.48) * | 1.46 (0.94–2.27) | 3.50 (1.69–7.27) *** | 1.16 (0.65–2.09) | 1.47 (0.83–2.60) | |
| Never EBF | 1.04 (0.87–1.26) | 1.11 (0.91–1.34) | 1.12 (0.91–1.38) | 1.34 (1.01–1.79) * | 1.16 (0.90–1.51) | 1.20 (0.92–1.55) | |
| 1–3 months | 1.77 (0.93–3.36) | 0.92 (0.48–1.76) | 1.28 (0.67–2.48) | 1.35 (0.56–3.26) | 1.05 (0.49–2.23) | 1.33 (0.63–2.81) | |
| 4–5 months | 1.63 (1.15–2.32) ** | 1.86 (1.33–2.60) *** | 1.82 (1.28–2.59) *** | 1.65 (1.01–2.69) * | 1.01 (0.67–1.52) | 1.10 (0.74–1.65) | |
| 6–7 months | 1 | 1 | 1 | 1 | 1 | 1 | |
| >7 months | 0.61 (0.14–2.69) | 0.17 (0.02–1.46) | 0.26 (0.03–2.28) | 0.77 (0.22–2.76) | 0.98 (0.29–3.34) | 1.02 (0.30–3.46) | |
| Factors | Variable | 12–24 Months (n = 941) | 25–36 Months (n = 842) | ||||
|---|---|---|---|---|---|---|---|
| AS aOR (95% CI) | ASu aOR (95% CI) | AS&Su aOR (95% CI) | AS aOR (95% CI) | ASu aOR (95% CI) | AS&Su aOR (95% CI) | ||
| Sociodemographic Factors | Toddler age: | 1.16 (1.11–1.21) *** | 1.13 (1.08–1.18) *** | 1.13 (1.08–1.18) *** | 1.03 (0.97–1.09) | 1.04 (1.00–1.08) | 1.04 (1.00–1.08) * |
| Maternal age: | |||||||
| <25 years | 1.67 (0.78–3.57) | 1.23 (0.64–2.37) | 1.27 (0.66–2.46) | 0.55 (0.16–1.82) | 0.68 (0.28–1.69) | 0.62 (0.24–1.55) | |
| 25–29 years | 1.15 (0.78–1.71) | 1.11 (0.76–1.62) | 1.08 (0.74–1.58) | 0.73 (0.42–1.28) | 0.80 (0.55–1.15) | 0.82 (0.57–1.19) | |
| 30–34 years | 1 | 1 | 1 | 1 | 1 | 1 | |
| 35–39 years | 0.96 (0.63–1.46) | 0.88 (0.58–1.33) | 0.89 (0.58–1.36) | 0.89 (0.52–1.54) | 0.97 (0.68–1.38) | 0.94 (0.66–1.34) | |
| ≥40 years | 0.77 (0.32–1.85) | 0.85 (0.36–2.01) | 0.92 (0.39–2.19) | 0.64 (0.28–1.50) | 1.20 (0.66–2.16) | 1.15 (0.64–2.08) | |
| Maternal education: | |||||||
| Primary and vocational | 1.07 (0.73–1.59) | 1.08 (0.76–1.54) | 1.11 (0.77–1.59) | 0.85 (0.50–1.43) | 1.08 (0.76–1.53) | 1.03 (0.73–1.47) | |
| High school | 0.43 (0.19–1.05) | 0.65 (0.26–1.61) | 0.56 (0.22–1.46) | 1.58 (0.34–7.28) | 1.56 (0.73–3.35) | 1.44 (0.67–3.08) | |
| University | 1 | 1 | 1 | 1 | 1 | 1 | |
| Parity: | |||||||
| Primiparias | 1 | 1 | 1 | 1 | 1 | 1 | |
| Multiparias | 1.61 (1.14–2.28) ** | 1.84 (1.34–2.54) *** | 1.85 (1.34–2.55) *** | 0.82 (0.52–1.30) | 1.09 (0.80–1.47) | 1.11 (0.82–1.50) | |
| Living area: | |||||||
| Rural | 1.23 (0.85–1.78) | 1.57 (1.09–2.27)* | 1.54 (1.06–2.24)* | 0.96 (0.58–1.59) | 1.13 (0.81–1.58) | 1.08 (0.77–1.51) | |
| Urban | 1 | 1 | 1 | 1 | 1 | 1 | |
| Macroeconomic region (GDP EU-28 average): | |||||||
| 47–50% | - | - | - | - | - | - | |
| 51–100% | 1.17 (0.55–2.48) | 1.43 (0.75–2.73) | 1.52 (0.79–2.91) | 3.97 (0.89–17.66) | 0.36 (0.18–0.72) ** | 0.38 (0.19–0.76) ** | |
| 101–110% | 1 | 1 | 1 | 1 | 1 | 1 | |
| 111–130% | 0.85 (0.58–1.26) | 1.35 (0.93–1.96) | 1.31 (0.89–1.91) | 1.16 (0.69–1.94) | 0.81 (0.57–1.15) | 0.78 (0.55–1.10) | |
| 131–150% | 1.16 (0.64–2.12) | 0.69 (0.37–1.27) | 0.67 (0.36–1.25) | 2.06 (0.86–4.94) | 0.63 (0.38–1.02) | 0.62 (0.38–1.01) | |
| >150% | 0.82 (0.50–1.34) | 1.31 (0.78–2.21) | 1.25 (0.74–2.11) | 0.95 (0.49–1.85) | 0.61 (0.38–0.98) * | 0.58 (0.36–0.93) * | |
| Average monthly income per capita (EUR): | |||||||
| <1000 | 0.80 (0.37–1.70) | 1.00 (0.46–2.17) | 1.27 (0.57–2.82) | 1.53 (0.65–3.62) | 0.95 (0.51–1.78) | 0.89 (0.47–1.66) | |
| 1000–1500 | 1.05 (0.55–2.02) | 1.56 (0.82–2.97) | 1.78 (0.91–3.48) | 2.45 (1.16–5.18) * | 1.22 (0.74–2.02) | 1.21 (0.73–2.01) | |
| 1501–2000 | 1.15 (0.63–2.10) | 0.99 (0.54–1.82) | 1.26 (0.66–2.38) | 1.55 (0.81–2.97) | 1.14 (0.71–1.83) | 1.15 (0.71–1.85) | |
| 2001–3000 | 1.04 (0.56–1.92) | 1.21 (0.65–2.24) | 1.46 (0.76–2.78) | 1.60 (0.82–3.15) | 1.10 (0.68–1.80) | 1.10 (0.68–1.79) | |
| 3001–5000 | 1 | 1 | 1 | 1 | 1 | 1 | |
| ≥5001 | 0.84 (0.22–3.17) | 1.59 (0.44–5.75) | 1.95 (0.53–7.10) | 1.58 (0.41–6.06) | 1.41 (0.57–3.47) | 1.22 (0.50–3.01) | |
| Feeding-Related Factors | Timing of CFI: | ||||||
| <4 months | 1.04 (0.42–2.55) | 0.57 (0.24–1.36) | 0.55 (0.22–1.34) | 1.75 (0.51–5.97) | 0.93 (0.43–2.02) | 0.80 (0.37–1.75) | |
| 4–6 months | 1.14 (0.74–1.76) | 0.91 (0.59–1.40) | 0.91 (0.58–1.40) | 1.66 (0.93–2.96) | 0.90 (0.60–1.35) | 0.89 (0.59–1.34) | |
| ≥7 months | 1 | 1 | 1 | 1 | 1 | 1 | |
| Complementary feeding method: | |||||||
| TSF | 0.87 (0.60–1.26) | 1.19 (0.83–1.70) | 1.13 (0.79–1.62) | 1.26 (0.75–2.10) | 0.97 (0.70–1.34) | 0.92 (0.66–1.27) | |
| Mixed | 1 | 1 | 1 | 1 | 1 | 1 | |
| BLW | 0.61 (0.35–1.05) | 0.70 (0.39–1.25) | 0.69 (0.38–1.24) | 0.74 (0.39–1.40) | 0.89 (0.56–1.43) | 0.81 (0.51–1.31) | |
| Types of CF: | |||||||
| Commercial | 1.15 (0.65–2.04) | 0.82 (0.48–1.38) | 0.94 (0.55–1.59) | 1.39 (0.66–2.95) | 0.78 (0.48–1.26) | 0.84 (0.52–1.35) | |
| Homemade | 0.82 (0.51–1.33) | 0.73 (0.46–1.14) | 0.81 (0.51–1.27) | 0.79 (0.44–1.40) | 0.81 (0.54–1.21) | 0.81 (0.54–1.21) | |
| Family | 1 | 1 | 1 | 1 | 1 | 1 | |
| Currently BF: | |||||||
| No | 1.51 (1.01–2.25) * | 1.56 (1.03–2.37) * | 1.63 (1.07–2.49) * | 1.52 (0.78–2.94) | 1.24 (0.74–2.09) | 1.36 (0.80–2.29) | |
| Yes | 1 | 1 | 1 | 1 | 1 | 1 | |
| EBF duration: | |||||||
| Never BF | 0.92 (0.46–1.82) | 1.52 (0.75–3.09) | 1.52 (0.74–3.09) | 1.92 (0.62–5.93) | 2.39 (1.16–4.95) * | 2.30 (1.11–4.79) * | |
| Never EBF | 1.47 (0.93–2.34) | 1.46 (0.94–2.26) | 1.31 (0.84–2.04) | 0.76 (0.41–1.39) | 1.53 (1.01–2.32) * | 1.42 (0.94–2.16) | |
| 1–3 months | 0.44 (0.21–0.88) * | 0.87 (0.42–1.78) | 0.63 (0.30–1.34) | 0.62 (0.25–1.55) | 1.66 (0.90–3.06) | 1.42 (0.77–2.63) | |
| 4–5 months | 0.92 (0.57–1.47) | 1.00 (0.62–1.61) | 0.93 (0.58–1.50) | 0.79 (0.41–1.50) | 1.53 (1.00–2.35) * | 1.45 (0.94–2.22) | |
| 6–7 months | 1 | 1 | 1 | 1 | 1 | 1 | |
| >7 months | 1.81 (0.60–5.47) | 1.67 (0.62–4.51) | 1.78 (0.66–4.83) | 0.62 (0.20–1.86) | 1.47 (0.57–3.75) | 1.51 (0.59–3.87) | |
| Variables | 12–24 Months (n = 2680) | 25–36 Months (n = 1430) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| AS | ASu | AS&Su | AS | ASu | AS&Su | |||||||
| Yes 52.8% | No 47.2% | Yes 34.7% | No 65.3% | Yes 26.8% | No 73.2% | Yes 74.4% | No 25.6% | Yes 59.0% | No 41.0% | Yes 50.8% | No 49.2% | |
| Dietary pattern: | ||||||||||||
| →Pro-health | 35.1 | 54.6 *** | 37 | 48.1 *** | 31.6 | 48.9 *** | 28.9 | 44.8 *** | 32.6 | 40.9 *** | 26.6 | 39.5 *** |
| →Western-like | 35.3 | 14.2 | 38.6 | 18.3 | 43.3 | 18.8 | 55.4 | 35.5 | 42.5 | 22.4 | 59.8 | 40.5 |
| →Non-eaters | 29.6 | 31.1 | 24.3 | 33.5 | 25.1 | 32.3 | 15.8 | 19.7 | 24.9 | 36.8 | 13.6 | 20 |
| Eating at least one meal with the family | 97.5 | 97.1 | 98.4 | 96.7 ** | 98.2 | 97.0 | 98.3 | 97.3 | 99.2 | 99.3 ** | 98.6 | 97.4 |
| Eating meals separately | 50.2 | 49.4 | 46.7 | 51.5 * | 47.2 | 50.8 | 51.6 | 44.8 * | 35.2 | 41.5 * | 52.6 | 47.0 * |
| Eating while watching TV 1 | 34.1 | 19.8 *** | 32.9 | 24.4 *** | 37.2 | 23.8 *** | 49.3 | 36.3 *** | 13.4 | 8.5 *** | 51.5 | 40.3 *** |
| Eating during playing | 9.9 | 9.1 | 11.7 | 8.3 ** | 10.9 | 9.0 | 12.3 | 12.6 | 12.7 | 11.9 | 12.3 | 12.5 |
| None concern | 70.8 | 76.8 *** | 70.7 | 75.2 ** | 69.1 | 75.3 *** | 68.4 | 76.2 ** | 67.6 | 74.4 ** | 65.8 | 75.1 *** |
| Toddler eats too little | 17.6 | 13.9 ** | 17.3 | 15.1 | 18.9 | 14.7 ** | 14.8 | 11.5 | 14.6 | 12.9 | 15.8 | 11.9 |
| Toddler eats too much | 7.2 | 6.9 | 7.3 | 6.9 | 7.1 | 7.0 | 4.5 | 4.4 | 4.2 | 4.9 | 4.0 | 5.0 |
| Toddler eats same thing for longer period | 20.2 | 15.7 ** | 20.8 | 16.7 ** | 22.3 | 16.6 *** | 25.8 | 21.9 | 26.1 | 23.0 | 27.4 | 22.2 * |
| Toddler does not eat vegetables | 19.4 | 11.9 *** | 18.6 | 14.4 ** | 20.6 | 14.1 *** | 25.5 | 18.3 *** | 26.0 | 20.3 ** | 27.1 | 20.0 ** |
| Toddler does not eat novel foods | 16.3 | 11.5 *** | 16.0 | 13.0 * | 17.4 | 12.8 ** | 27.6 | 21.6 * | 28.6 | 22.5 ** | 29.9 | 22.2 *** |
| Variables | 12–24 Months (n = 941) | 25–36 Months (n = 842) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| AS | ASu | AS&Su | AS | ASu | AS&Su | |||||||
| Yes 74.8% | No 25.2% | Yes 27.7% | No 72.3% | Yes 26.8% | No 73.2% | Yes 87.4% | No 12.6% | Yes 45.8% | No 54.2% | Yes 44.7% | No 55.3% | |
| Dietary pattern: | ||||||||||||
| →Pro-health | 37.8 | 40.9 *** | 32.6 | 40.9 *** | 33.1 | 40.6 *** | 28.8 | 38.7 | 24.6 | 34.6 *** | 25 | 34.1 *** |
| →Western-like | 32.4 | 14.8 | 42.5 | 22.4 | 42.2 | 22.8 | 54.6 | 42.5 | 60.9 | 46.5 | 60.9 | 46.8 |
| →Non-eaters | 29.8 | 44.3 | 24.9 | 36.8 | 24.7 | 36.7 | 16.6 | 18.9 | 14.5 | 18.9 | 14,1 | 19.1 |
| Eating at least one meal with the family | 99.4 | 98.7 | 99.2 | 99.3 | 99.2 | 99.3 | 99.5 | 0.0 | 99.7 | 99.3 | 99.7 | 99.4 |
| Eating meals separately | 38.2 | 44.3 | 35.2 | 41.5 | 35.5 | 41.3 | 34.2 | 31.1 | 34.5 | 33.3 | 34.6 | 33.3 |
| Eating while watching TV 1 | 9.9 | 9.7 | 13.4 | 8.5 * | 12.7 | 8.8 | 17.8 | 16.0 | 18.9 | 16.4 | 18.6 | 16.7 |
| Eating during playing | 7.5 | 8.4 | 5.7 | 8.5 | 5.6 | 8.6 | 7.1 | 11.3 | 8.0 | 7.2 | 8.0 | 7.3 |
| None concern | 62.8 | 62.9 | 59.4 | 64.1 | 69.6 | 63.6 | 62.9 | 56.6 | 61.7 | 62.5 | 62.2 | 62.0 |
| Toddler eats too little | 17.8 | 16.9 | 20.3 | 16.5 | 19.9 | 16.7 | 19.3 | 17.0 | 20.2 | 18.0 | 18.0 | 20.2 |
| Toddler eats too much | 3.3 | 0.8* | 1.9 | 2.9 | 2.0 | 2.9 | 3.3 | 2.8 | 3.9 | 2.6 | 2.6 | 4.0 |
| Toddler eats same thing for longer period | 14.8 | 15.6 | 16.1 | 14.6 | 15.9 | 14.6 | 16.7 | 13.2 | 16.8 | 15.8 | 16.3 | 16.2 |
| Toddler does not eat vegetables | 11.6 | 11.4 | 12.6 | 11.2 | 12.4 | 11.3 | 14.7 | 10.4 | 16.1 | 12.5 | 12.7 | 16.0 |
| Toddler does not eat novel foods | 8.4 | 7.6 | 10.3 | 7.4 | 10.4 | 7.4 | 15.5 | 9.4 | 16.6 | 13.2 | 13.1 | 16.8 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Masztalerz-Kozubek, D.; Zielinska, M.A.; Rust, P.; Majchrzak, D.; Hamulka, J. The Use of Added Salt and Sugar in the Diet of Polish and Austrian Toddlers. Associated Factors and Dietary Patterns, Feeding and Maternal Practices. Int. J. Environ. Res. Public Health 2020, 17, 5025. https://doi.org/10.3390/ijerph17145025
Masztalerz-Kozubek D, Zielinska MA, Rust P, Majchrzak D, Hamulka J. The Use of Added Salt and Sugar in the Diet of Polish and Austrian Toddlers. Associated Factors and Dietary Patterns, Feeding and Maternal Practices. International Journal of Environmental Research and Public Health. 2020; 17(14):5025. https://doi.org/10.3390/ijerph17145025
Chicago/Turabian StyleMasztalerz-Kozubek, Daria, Monika A. Zielinska, Petra Rust, Dorota Majchrzak, and Jadwiga Hamulka. 2020. "The Use of Added Salt and Sugar in the Diet of Polish and Austrian Toddlers. Associated Factors and Dietary Patterns, Feeding and Maternal Practices" International Journal of Environmental Research and Public Health 17, no. 14: 5025. https://doi.org/10.3390/ijerph17145025
APA StyleMasztalerz-Kozubek, D., Zielinska, M. A., Rust, P., Majchrzak, D., & Hamulka, J. (2020). The Use of Added Salt and Sugar in the Diet of Polish and Austrian Toddlers. Associated Factors and Dietary Patterns, Feeding and Maternal Practices. International Journal of Environmental Research and Public Health, 17(14), 5025. https://doi.org/10.3390/ijerph17145025







