Sociodemographic Predictors of Health Risk Perception, Attitude and Behavior Practices Associated with Health-Emergency Disaster Risk Management for Biological Hazards: The Case of COVID-19 Pandemic in Hong Kong, SAR China
Abstract
1. Introduction
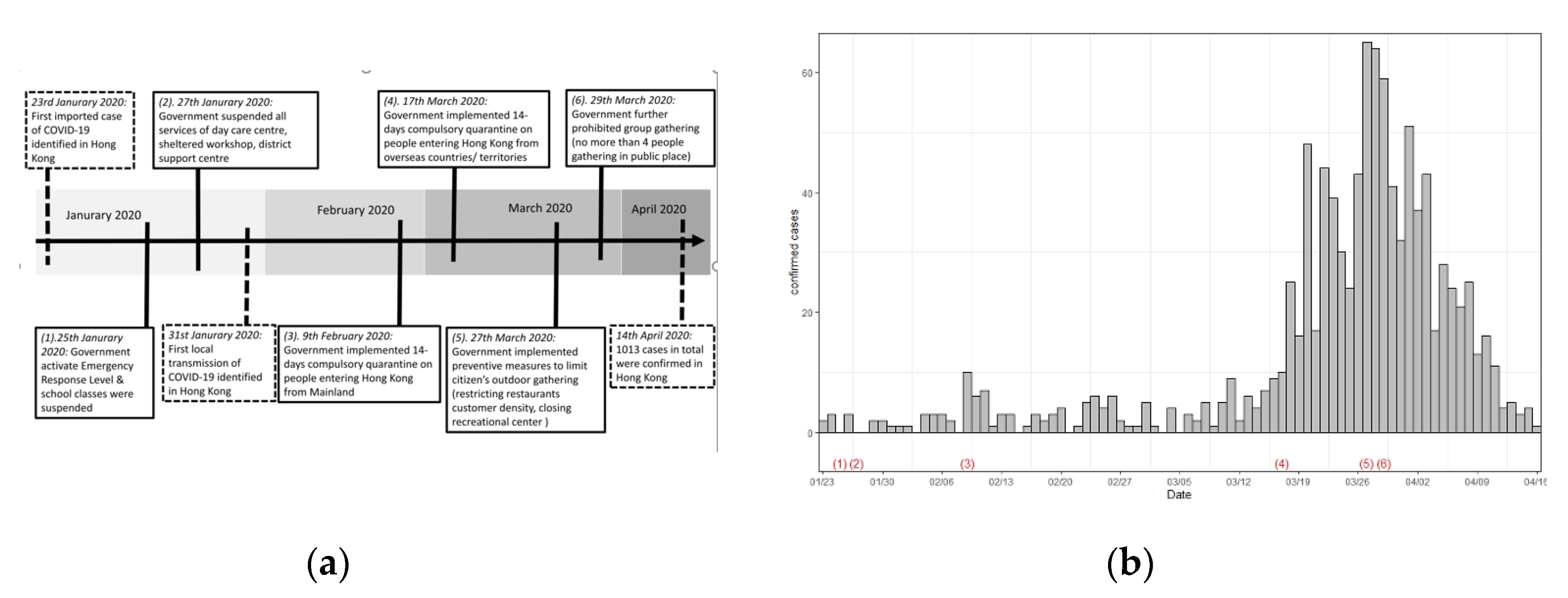
The Situation in Hong Kong and Past Experiences of Similar Pandemics
2. Materials and Methods
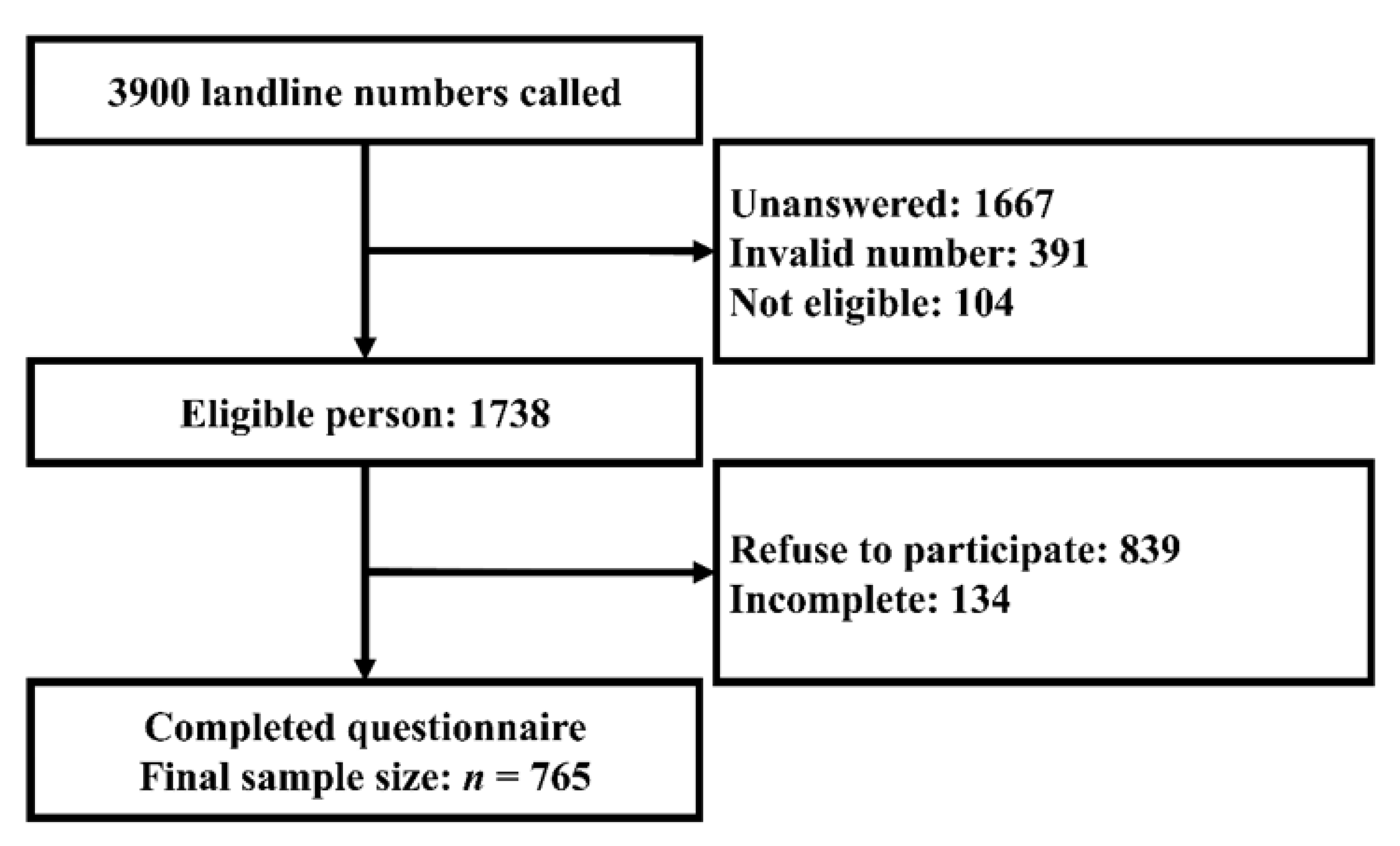
2.1. Study Design and Study Population
2.2. Data Collection
2.3. Study Instrument
- Sociodemographic information was collected for age, gender, district of residence, household income, household size, marital status, education, size of housing, occupation and employment status.
- Knowledge about COVID-19, including the transmission route, and the comparison between COVID-19 and other respiratory diseases.
- Risk perception of Health-EDRM behavior associated with COVID-19, including the perceived impacts (e.g., physical, mental, social, financial and the whole impact), perceived sufficient knowledge to manage COVID-19, perceived severity and infectivity. Five-point Likert scales were used to measure the level of agreement or disagreement for the questions (from 1 to 5, 1 = strongly disagree, 2 = disagree, 3 = neutral, 4 = agree, 5 = strongly agree). The 6-item short form of the State-Trait Anxiety Inventory (STAI) was used for measuring their current anxiety level concerning the outbreak [32]. A binary question of whether the respondent was worried about getting infected with COVID-19 was asked.
- Self-reported perceived usefulness and actual Health-EDRM behavioral practice of nine personal or household health emergency disaster risks management related behaviors and practices of COVID-19 prevention behavior. These include: (1) washing hands before meals and after toileting, (2) washing hands with soaps, (3) avoiding dining or gathering together, (4) using serving utensils, (5) ordering takeaways more often, (6) bringing one’s own utensil when dining out, (7) wearing a mask when going out, (8) avoiding going to public places or using public transport, and (9) avoiding going to COVID-19-confirmed regions outside Hong Kong. The four-point Likert scale was used to ascertain the level of the practices (from 1 to 4, 1 = always, 2 = usually, 3 = sometimes, 4 = never).
- Current and preferred channels of information acquisition, the information they were interested in and the awareness of COVID-19.
- Questions about home quarantine and caregiving to non-suspected family members during the COVID-19 outbreak were also asked.
2.4. Statistical Analysis
3. Results
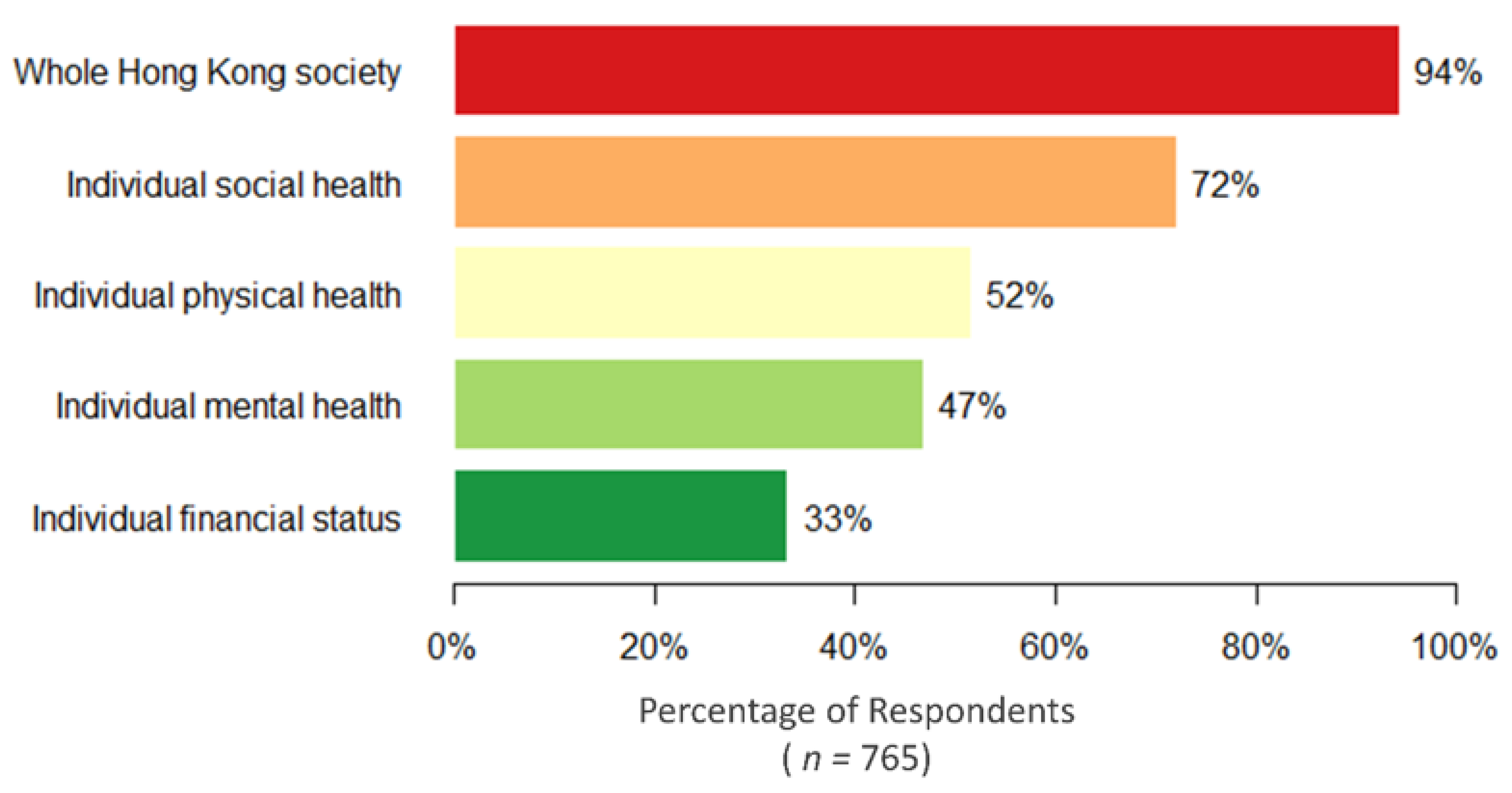
3.1. Perception of Various Health and Economic Impacts of COVID-19
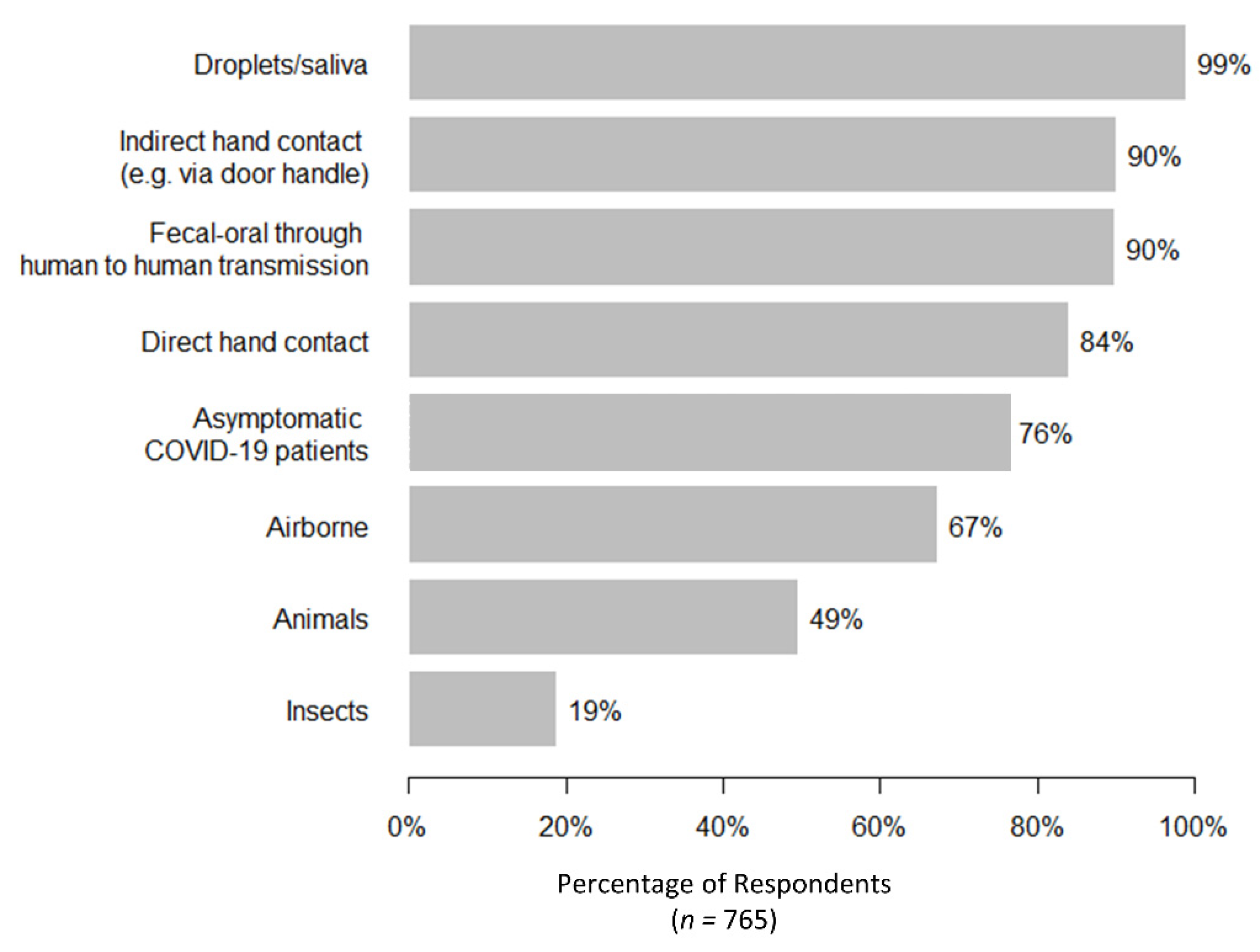
3.2. Knowledge and Risk Perception of COVID-19
3.3. Attitude and Uptake of Health-EDRM Behavior Practice towards COVID-19
3.4. Sociodemographic Factors Affecting Anxiety around Getting COVID-19
3.5. Other Related Behavioral Experiences: Home Quarantine and Caregiving to Non-Infected Family Members during COVID-19
3.6. Information Channel and Type of Information of Health Information Seeking for COVID-19
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Demographics | Risk Perception | Knowledge | |||||
|---|---|---|---|---|---|---|---|
| Large Impact on Mental Health | Large Impact on Social Health | Large Impact on Financial Status | Large Impact on Hong Kong | Can be Prevented at Government Level | Can Be Spread by Insect | Can Be Spread by Asymptomatic Patient | |
| Education | |||||||
| Primary | 1.10 (0.51–2.38) | 0.15 (0.04–0.51) * | 2.89 (1.35–6.18) * | 0.45 (0.21–0.96) * | |||
| Secondary | 1.81 (1.22–2.69) * | 0.51 (0.21–1.23) | 1.40 (0.87–2.26) | 0.50 (0.32–0.78) * | |||
| Post-secondary | 1 | 1 | 1 | 1 | |||
| Gender | |||||||
| Male | 1 | 1 | |||||
| Female | 1.41 (1.02–1.95) * | 1.60 (1.10–2.33) * | |||||
| Age | |||||||
| 18–24 | 2.00 (0.77–5.18) | 6.12 (1.78–21.54) * | 7.93 (2.76–22.76) * | 3.06 (0.88–10.61) | |||
| 25–44 | 2.21 (1.19–4.12) * | 4.03 (1.99–8.15) * | 7.05 (3.35–14.81) * | 2.12 (1.10–40.9) * | |||
| 45–64 | 1.26 (0.73–2.19) | 2.98 (1.60–5.55) * | 4.32 (2.22–8.42) * | 0.96 (0.55–1.69) | |||
| 65+ | 1 | 1 | 1 | 1 | |||
| Household income | |||||||
| <2000–7999 | 1 | ||||||
| 8000–19,999 | 0.43 (0.20–0.92) * | ||||||
| 20,000–39,999 | 0.33 (0.16–0.72) * | ||||||
| 40,000 or more | 0.25 (0.12–0.54) * | ||||||
| Occupation | |||||||
| White collar | 1 | ||||||
| Blue collar | 1.70 (0.99–2.93) | ||||||
| Housewife | 1.95 (0.98–3.90) | ||||||
| Student | 1.35 (0.36–5.05) | ||||||
| Unemployment or retired | 3.41 (1.72–6.76) * | ||||||
| Demographics | Wash Hands with Soaps | Avoid Dining or Gathering Together | Use Serving Utensil | Avoid Going to Public Place or Using Public Transport |
|---|---|---|---|---|
| Education | ||||
| Primary | 0.31 (0.12–0.84) * | 0.15 (0.04-0.51) * | ||
| Secondary | 0.68 (0.33–1.42) | 0.51 (0.21–1.23) | ||
| Post-secondary | 1 | 1 | ||
| Gender | ||||
| Male | 1 | 1 | ||
| Female | 2.27 (1.17–4.43) * | 1.82 (1.21–2.74) * | ||
| Age | ||||
| 18–24 | 2.15 (0.39–11.97) | 2.48 (0.93–6.65) | ||
| 25–44 | 4.62 (1.47–14.52) * | 2.08 (1.09–3.98) * | ||
| 45–64 | 2.83 (1.15–6.95) * | 1.37 (0.77–2.44) | ||
| 65+ | 1 | 1 | ||
| Household income | ||||
| <2000–7999 | ||||
| 8000–19,999 | ||||
| 20,000–39,999 | ||||
| 40,000 or more | ||||
| Occupation | ||||
| White collar | 1 | |||
| Blue collar | 0.70 (0.44–1.23) | |||
| Housewife | 3.47 (1.87–6.42) * | |||
| Student | 0.99 (0.37–2.65) | |||
| Unemployment or retired | 2.29 (1.28–4.07) * | |||
References
- Rolling Updates on Coronavirus Disease (COVID-19). Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen (accessed on 23 April 2020).
- Ye, Z.W.; Yuan, S.; Yuen, K.S.; Fung, S.Y.; Chan, C.P.; Jin, D.Y. Zoonotic origins of human coronaviruses. Int. J. Biol. Sci. 2020, 16, 1686. [Google Scholar] [CrossRef]
- Coronavirus Disease 2019 (COVID-19) Situation Report–85. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200414-sitrep-85-covid-19.pdf?sfvrsn=7b8629bb_2 (accessed on 23 April 2020).
- Rajgor, D.D.; Lee, M.H.; Archuleta, S.; Bagdasarian, N.; Quek, S.C. The many estimates of the COVID-19 case fatality rate. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Kim, D.D.; Goel, A. Estimating case fatality rates of COVID-19. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Day, M. Covid-19: Identifying and isolating asymptomatic people helped eliminate virus in Italian village. BMJ 2020, 368, m1165. [Google Scholar] [CrossRef] [PubMed]
- Kimball, A. Asymptomatic and presymptomatic SARS-CoV-2 infections in residents of a long-term care skilled nursing facility—King County, Washington, March 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 377–381. [Google Scholar] [CrossRef]
- Mahase, E. Coronavirus: COVID-19 has killed more people than SARS and MERS combined, despite lower case fatality rate. BMJ 2020, m641. [Google Scholar] [CrossRef]
- Wells, C.R.; Sah, P.; Moghadas, S.M.; Pandey, A.; Shoukat, A.; Wang, Y.; Galvani, A.P. Impact of international travel and border control measures on the global spread of the novel 2019 coronavirus outbreak. Proc. Natl. Acad. Sci. USA 2020, 117, 7504–7509. [Google Scholar] [CrossRef]
- Lewnard, J.A.; Lo, N.C. Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Novel Coronavirus (2019-nCoV) SITUATION REPORT-3 23 JANUARY 2020. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200123-sitrep-3-2019-ncov.pdf?sfvrsn=d6d23643_8 (accessed on 23 April 2020).
- CHP Investigates Two Additional Cases of Novel Coronavirus Infection. Available online: https://www.info.gov.hk/gia/general/202001/31/P2020013100015.htm?fontSize=1 (accessed on 23 April 2020).
- Latest Situation of Cases of COVID-19 (as of 14 April, 2020). Available online: https://www.chp.gov.hk/files/pdf/local_situation_covid19_en.pdf (accessed on 15 April 2020).
- CE Announces Activation of Emergency Response Level in Relation to Novel Coronavirus Infection (with Photo). Available online: https://www.info.gov.hk/gia/general/202001/26/P2020012600087.htm (accessed on 23 April 2020).
- LNY Welfare Services Set. Available online: https://www.news.gov.hk/eng/2020/01/20200127/20200127_233955_845.html (accessed on 23 April 2020).
- Deferral of Class Resumption for All Schools Together, We Fight the Virus. Available online: https://www.edb.gov.hk/attachment/en/sch-admin/admin/about-sch/diseases-prevention/edb_20200331_eng.pdf (accessed on 23 April 2020).
- Compulsory Quarantine Implemented Smoothly. Available online: https://www.info.gov.hk/gia/general/202002/09/P2020020900715.htm?fontSize=1 (accessed on 23 April 2020).
- Quarantine Measures Enhanced. Available online: https://www.news.gov.hk/eng/2020/03/20200317/20200317_202509_713.html (accessed on 23 April 2020).
- Prevention and Control of Disease (Requirement and Directions) (Business and Premises) Regulation Gazette. Available online: https://www.info.gov.hk/gia/general/202003/27/P2020032700878.htm?fontSize=1 (accessed on 23 April 2020).
- Prevention and Control of Disease (Prohibition on Group Gathering) Regulation. Available online: https://www.info.gov.hk/gia/general/202003/28/P2020032800720.htm?fontSize=1 (accessed on 23 April 2020).
- Health Emergency and Disaster Risk Management Framework. Available online: https://www.who.int/hac/techguidance/preparedness/health-emergency-and-disaster-risk-management-framework-eng.pdf?ua=1 (accessed on 23 April 2020).
- Wan, Y.K.P. A comparison of the governance of tourism planning in the two Special Administrative Regions (SARs) of China–Hong Kong and Macao. Tour. Manag. 2013, 36, 164–177. [Google Scholar]
- Kung, N.Y.; Morris, R.S.; Perkins, N.R.; Sims, L.D.; Ellis, T.M.; Bissett, L.; Peiris, M.J. Risk for infection with highly pathogenic influenza A virus (H5N1) in chickens, Hong Kong, 2002. Emerg. Infect. Dis. 2007, 13, 412. [Google Scholar] [CrossRef]
- Cheng, V.C.C.; Lee, W.M.; Sridhar, S.; Ho, P.L.; Yuen, K.Y. Prevention of nosocomial transmission of influenza A (H7N9) in Hong Kong. J. Hosp. Infect. 2015, 90, 355–356. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.T.; Chen, H.; Liu, S.H.; Hsu, E.K.; Luk, K.S.; Lai, C.K.; Tong, A.Y. From SARS to avian influenza preparedness in Hong Kong. Clin. Infect. Dis. 2017, 64 (Suppl. S2), S98–S104. [Google Scholar] [CrossRef] [PubMed]
- Lau, J.T.; Tsui, H.; Lau, M.; Yang, X. SARS transmission, risk factors, and prevention in Hong Kong. Emerg. Infect. Dis. 2004, 10, 587. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.Y.Y.; Cheng, C.K.; Tam, G.; Huang, Z.; Lee, P. Knowledge, attitudes, and practices of Hong Kong population towards human A/H7N9 influenza pandemic preparedness, China, 2014. BMC Public Health 2015, 15, 943. [Google Scholar] [CrossRef] [PubMed]
- West, R.; Michie, S.; Rubin, G.J.; Amlôt, R. Applying principles of behaviour change to reduce SARS-CoV-2 transmission. Nat. Hum. Behav. 2020, 4, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.Y.Y.; Shahzada, T.S.; Sham, T.; Dubois, C.; Huang, Z.; Liu, S.; Shaw, R. Non-Pharmaceutical Behavioural Measures for Droplet-Borne Biological Hazards Prevention: Health-EDRM for COVID-19 (SARS-CoV-2) Pandemic. 2020; Manuscript Submitted for Publication. [Google Scholar]
- Chan, E.Y.Y.; Cheng, C.K.Y.; Tam, G.; Huang, Z.; Lee, P. Willingness of future A/H7N9 influenza vaccine uptake: A cross-sectional study of Hong Kong community. Vaccine 2015, 33, 4737–4740. [Google Scholar] [CrossRef] [PubMed]
- Tam, G.; Huang, Z.; Chan, E.Y.Y. Household preparedness and preferred communication channels in public health emergencies: A cross-sectional survey of residents in an Asian developed urban city. Int. J. Environ. Res. Public Health 2018, 15, 1598. [Google Scholar] [CrossRef]
- Marteau, T.M.; Bekker, H. The development of a six-item short-form of the state scale of the Spielberger State-Trait Anxiety Inventory (STAI). Br. J. Clin. Psychol. 1992, 31 Pt 3, 301–306. [Google Scholar] [CrossRef]
- Chan, E.Y.Y.; Wong, C.S. Public health prevention hierarchy in disaster context. In Public Health and Disasters-Health Emergency and Disaster Risk Management in Asia; Chan, E.Y.Y., Shaw, R., Eds.; Springer: Tokyo, Japan, 2020; pp. 7–17. [Google Scholar]
- Chan, E.Y.Y. Building Bottom-up Health and Disaster Risk Reduction Programmes; Oxford University Press: Oxford, UK, 2018. [Google Scholar]
- Chan, E.Y.Y.; Huang, Z.; Mark, C.K.M.; Guo, C. Weather information acquisition and health significance during extreme cold weather in a subtropical city: A cross-sectional survey in Hong Kong. Int. J. Disaster Risk Sci. 2017, 8, 134–144. [Google Scholar] [CrossRef]
- Chan, E.Y.Y.; Huang, Z.; Hung, K.K.C.; Chan, G.K.W.; Lam, H.C.Y.; Lo, E.S.K.; Yeung, M.P.S. Health emergency disaster risk management of public transport systems: A population-based study after the 2017 subway fire in Hong Kong, China. Int. J. Environ. Res. Public Health 2019, 16, 228. [Google Scholar] [CrossRef]
- Hong Kong SAR Census and Statistics Department. Available online: https://www.bycensus2016.gov.hk/en/bc-dp.html (accessed on 23 April 2020).
- Cowling, B.J.; Ali, S.T.; Ng, T.W.; Tsang, T.K.; Li, J.C.; Fong, M.W.; Wu, J.T. Impact assessment of non-pharmaceutical interventions against coronavirus disease 2019 and influenza in Hong Kong: An observational study. Lancet Public Health 2020, 5, e279–e288. [Google Scholar] [CrossRef]
- Leung, G.M.; Lam, T.H.; Ho, L.M.; Ho, S.Y.; Chan, B.H.Y.; Wong, I.O.L.; Hedley, A.J. The impact of community psychological responses on outbreak control for severe acute respiratory syndrome in Hong Kong. J. Epidemiol. Community Health 2003, 57, 857–863. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Zhao, N. Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 epidemic in China: A web-based cross-sectional survey. MedRxiv 2020, 288, 112954. [Google Scholar]
- Kwok, K.O.; Li, K.K.; Chan, H.H.; Yi, Y.Y.; Tang, A.; Wei, W.I.; Wong, S.Y. Community Responses during Early Phase of COVID-19 Epidemic, Hong Kong. Emerg. Infect. Dis. 2020, 26. [Google Scholar] [CrossRef]
- Collinson, S.; Khan, K.; Heffernan, J.M. The effects of media reports on disease spread and important public health measurements. PLoS ONE 2015, 10, e0141423. [Google Scholar] [CrossRef]
- Shahid, Z.; Kalayanamitra, R.; McClafferty, B.; Kepko, D.; Ramgobin, D.; Patel, R.; Jain, R. COVID-19 and older adults: What we know. J. Am. Geriatr. Soc. 2020, 68, 926–929. [Google Scholar] [CrossRef]
- Kalligeros, M.; Shehadeh, F.; Mylona, E.K.; Benitez, G.; Beckwith, C.G.; Chan, P.A.; Mylonakis, E. Association of Obesity with Disease Severity among Patients with COVID-19. Obesity 2020. [Google Scholar] [CrossRef]
- Hussain, A.; Bhowmik, B.; do Vale Moreira, N.C. COVID-19 and diabetes: Knowledge in progress. Diabetes Res. Clin. Pract. 2020, 162, 108142. [Google Scholar] [CrossRef]
- Cook, T.M. The importance of hypertension as a risk factor for severe illness and mortality in COVID-19. Anaesthesia 2020. [Google Scholar] [CrossRef]
- World Health Organization. Modes of Transmission of Virus Causing COVID-19: Implications for IPC Precaution Recommendations: Scientific Brief, 27 March 2020 (No. WHO/2019-nCoV/Sci_Brief/Transmission_modes/2020.1). Available online: https://apps.who.int/iris/bitstream/handle/10665/331601/WHO-2019-nCoV-Sci_Brief-Transmission_modes-2020.1-eng.pdf (accessed on 23 April 2020).
- Abdelhafiz, A.S.; Mohammed, Z.; Ibrahim, M.E.; Ziady, H.H.; Alorabi, M.; Ayyad, M.; Sultan, E.A. Knowledge, Perceptions, and Attitude of Egyptians Towards the Novel Coronavirus Disease (COVID-19). J. Community Health 2020, 1–10. [Google Scholar] [CrossRef]
- Mizumoto, K.; Kagaya, K.; Zarebski, A.; Chowell, G. Estimating the asymptomatic proportion of coronavirus disease 2019 (COVID-19) cases on board the Diamond Princess cruise ship, Yokohama, Japan, 2020. Eurosurveillance 2020, 25, 2000180. [Google Scholar] [CrossRef] [PubMed]
- Coronavirus Disease (COVID-19) in HK. Available online: https://chp-dashboard.geodata.gov.hk/covid-19/en.html (accessed on 23 April 2020).
- Let’s Beat COVID-19 Together. Available online: https://www.cfs.gov.hk/english/whatsnew/whatsnew_fstr/whatsnew_fstr_Beat_COVID-19.html (accessed on 18 May 2020).
- New Regulations to Fight COVID-19. Available online: https://www.news.gov.hk/eng/2020/03/20200327/20200327_202339_445.html (accessed on 18 May 2020).
- Office of the Communications Authority Key Communications Statistics. Available online: https://www.ofca.gov.hk/en/data_statistics/data_statistics/key_stat/ (accessed on 23 April 2020).
- Petrovčič, A.; Vehovar, V.; Dolničar, V. Landline and mobile phone communication in social companionship networks of older adults: An empirical investigation in Slovenia. Technol. Soc. 2016, 45, 91–102. [Google Scholar] [CrossRef]
| Demographics | 2016 Population Census | Study Sample | p-Value d | ||
|---|---|---|---|---|---|
| Age | n | % | n | % | 0.332 |
| 18–24 | 600,726 | 9.50% | 71 | 9.30% | |
| 25–44 | 2,228,566 | 35.26% | 248 | 32.40% | |
| 45–64 | 2,328,430 | 36.84% | 303 | 39.60% | |
| 65 or older | 1,163,153 | 18.40% | 143 | 18.70% | |
| Gender | 0.425 e | ||||
| Male | 2,850,731 | 45.10% | 356 | 46.50% | |
| Female | 3,470,144 | 54.90% | 409 | 53.50% | |
| Marital status | 0.962 e | ||||
| Non-married | 2,523,742 | 39.93% | 304 | 39.80% | |
| Married | 3,797,133 | 60.07% | 459 | 60.20% | |
| Residential district a,b | 0.334 | ||||
| Hong Kong Island | 1,120,143 | 17.2% | 147 | 19.20 | |
| Kowloon | 1,987,380 | 30.6% | 231 | 30.20 | |
| New Territory | 3,397,499 | 52.2% | 387 | 50.60 | |
| Education a | <0.001 | ||||
| Primary level or below | 1,673,431 | 25.7% | 61 | 8.00% | |
| Secondary | 2,841,510 | 43.7% | 330 | 43.30% | |
| Tertiary level | 1,991,189 | 30.6% | 371 | 48.70% | |
| Household Income c | <0.001 | ||||
| <2000–7999 | 378,451 | 15.1 | 66 | 9.3 | |
| 8000–19999 | 649,450 | 25.9 | 101 | 14.1 | |
| 20000–39999 | 699,450 | 27.8 | 191 | 26.6 | |
| 40000 or more | 782,383 | 31.2 | 360 | 50.2 | |
| Control Measures that Can Protect from COVID-19 Infections | Thought It Was Useful for Prevention | Always or Usually Practicing Currently | Attitude vs. Practice a | ||
|---|---|---|---|---|---|
| n | % | n | % | p-Value | |
| Wash hands before meals and after toilet | 749 | 97.9 | 749 | 97.9 | 0.555 b |
| Wash hands with soaps | 740 | 96.7 | 706 | 92.3 | <0.001 |
| Wear mask when going out | 753 | 98.4 | 745 | 97.4 | <0.001 b |
| Use serving utensil | 708 | 92.5 | 568 | 74.2 | 0.174 |
| Bring own utensils when dining out † | 542 | 81.9 | 52 | 7.9 | 0.199 |
| Order takeaway more often | 474 | 62.0 | 262 | 34.4 | <0.001 |
| Avoid dining or gathering together | 742 | 97.0 | 616 | 85.0 | 0.178 |
| Avoid going to public place or using public transport | 713 | 93.4 | 408 | 53.5 | 0.002 |
| Avoid going to COVID-19 confirmed regions outside Hong Kong | 714 | 93.3 | 628 | 88.0 | <0.001 |
| Characteristics | Not Worry or Don’t Know † (n = 252) | Worry (n = 505) | p-Value | AOR (95% CI) | p-Value | |
|---|---|---|---|---|---|---|
| Age | 18–24 | 15 (6.0%) | 55 (10.9%) | 0.037 | 1 | |
| 25–44 | 77 (30.6%) | 169 (33.5%) | 0.567 (0.294–1.095) | 0.091 | ||
| 45–64 | 103 (40.9%) | 198 (39.2%) | 0.606 (0.318–1.153) | 0.127 | ||
| 65 or more | 57 (22.6%) | 83 (16.4%) | 0.493 (0.244–0.995) | 0.048 | ||
| Gender | Male | 132 (52.4%) | 220 (43.6%) | 0.022 | 1 | |
| Female | 120 (47.6%) | 285 (56.4%) | 1.323 (0.956–1.831) | 0.092 | ||
| Chronic disease | No | 206 (81.7%) | 412 (81.6%) | 0.957 | ||
| Yes | 46 (18.3%) | 93 (18.3%) | ||||
| Education level | Primary level or below | 25 (10.0%) | 33 (6.6%) | 0.249 | ||
| Secondary level | 108 (43.0%) | 220 (43.7%) | ||||
| Tertiary level | 118 (47.0%) | 250 (49.7%) | ||||
| Marital status | Non-married | 99 (39.4%) | 201 (39.9%) | 0.908 | ||
| Married | 152 (60.2%) | 303 (60.1%) | ||||
| Residential district | Hong Kong Island | 52 (21.0%) | 93 (18.4%) | 0.207 | ||
| Kowloon | 83 (32.9%) | 145 (28.7%) | ||||
| New Territories | 116 (46.0%) | 267 (52.9%) | ||||
| Families members with chronic disease | No or don’t know | 209 (82.9%) | 393 (77.8%) | 0.100 | ||
| Yes | 43 (17.1%) | 112 (22.2%) | ||||
| Household floor area | 350 ft or below | 53 (21.6%) | 100 (21.1%) | 0.964 | ||
| 351 ft to 800 ft | 157 (64.1%) | 304 (64.0%) | ||||
| 801 ft or above | 35 (14.3%) | 71 (14.9%) | ||||
| Household income | <2000–7999 | 29 (12.1%) | 36 (7.6%) | 0.147 | ||
| 8000–19,999 | 36 (15.0%) | 65 (13.8%) | ||||
| 20,000–39,999 | 66 (27.5%) | 123 (26.1%) | ||||
| 40,000 or more | 109 (45.4%) | 248 (52.5%) | ||||
| Believing COVID-19 had large effect on their physical health | No | 158 (62.9%) | 206 (40.9%) | <0.001 | 1 | |
| Yes | 93 (37.1%) | 298 (59.1%) | 1.583 (1.111–2.256) | 0.011 | ||
| Believing COVID-19 had large effect on their mental health | No | 183 (72.6%) | 219 (43.4%) | <0.001 | 1 | |
| Yes | 69 (27.4%) | 286 (56.6%) | 2.490 (1.719–3.608) | <0.001 | ||
| Believing COVID-19 had large effect on their financial status | No | 181 (71.8%) | 324 (64.2%) | 0.035 | 1 | |
| Yes | 71 (28.2%) | 181 (35.8%) | 0.927 (0.644–1.336) | 0.685 | ||
| Believing COVID-19 had large effect on their social life | No | 104 (41.3%) | 108 (21.4%) | <0.001 | 1 | |
| Yes | 148 (58.7%) | 397 (78.6%) | 1.657 (1.138–2.413) | 0.008 | ||
| Believing COVID-19 had large effect on whole Hong Kong society | No | 22 (8.7%) | 20 (4.0%) | 0.007 | 1 | |
| Yes | 230 (91.3%) | 485 (96.0%) | 1.205 (0.608–2.385) | 0.593 | ||
| Perceived sufficient knowledge to manage COVID-19 | No | 127 (50.4%) | 269 (53.3%) | 0.456 | ||
| Yes | 125 (49.6%) | 236 (43.7%) | ||||
| Perceived COVID-19 infectivity | Very low to medium or don’t know | 16 (6.3%) | 17 (3.4%) | 0.058 | 1 | |
| High or very high | 236 (93.7%) | 488 (96.6%) | 1.290 (0.610–2.728) | 0.505 | ||
| Perceived COVID-19 severity | Very low to medium or don’t know | 58 (23.0%) | 63 (19.0%) | 0.197 | ||
| High or very high | 194 (77.0%) | 409 (81.0%) | ||||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chan, E.Y.Y.; Huang, Z.; Lo, E.S.K.; Hung, K.K.C.; Wong, E.L.Y.; Wong, S.Y.S. Sociodemographic Predictors of Health Risk Perception, Attitude and Behavior Practices Associated with Health-Emergency Disaster Risk Management for Biological Hazards: The Case of COVID-19 Pandemic in Hong Kong, SAR China. Int. J. Environ. Res. Public Health 2020, 17, 3869. https://doi.org/10.3390/ijerph17113869
Chan EYY, Huang Z, Lo ESK, Hung KKC, Wong ELY, Wong SYS. Sociodemographic Predictors of Health Risk Perception, Attitude and Behavior Practices Associated with Health-Emergency Disaster Risk Management for Biological Hazards: The Case of COVID-19 Pandemic in Hong Kong, SAR China. International Journal of Environmental Research and Public Health. 2020; 17(11):3869. https://doi.org/10.3390/ijerph17113869
Chicago/Turabian StyleChan, Emily Ying Yang, Zhe Huang, Eugene Siu Kai Lo, Kevin Kei Ching Hung, Eliza Lai Yi Wong, and Samuel Yeung Shan Wong. 2020. "Sociodemographic Predictors of Health Risk Perception, Attitude and Behavior Practices Associated with Health-Emergency Disaster Risk Management for Biological Hazards: The Case of COVID-19 Pandemic in Hong Kong, SAR China" International Journal of Environmental Research and Public Health 17, no. 11: 3869. https://doi.org/10.3390/ijerph17113869
APA StyleChan, E. Y. Y., Huang, Z., Lo, E. S. K., Hung, K. K. C., Wong, E. L. Y., & Wong, S. Y. S. (2020). Sociodemographic Predictors of Health Risk Perception, Attitude and Behavior Practices Associated with Health-Emergency Disaster Risk Management for Biological Hazards: The Case of COVID-19 Pandemic in Hong Kong, SAR China. International Journal of Environmental Research and Public Health, 17(11), 3869. https://doi.org/10.3390/ijerph17113869






