Preventative Intervention for Social, Emotional and Behavioural Difficulties in Toddlers and Their Families: A Pilot Study
Abstract
1. Introduction
1.1. The Delivery of Behavioural Parent Training Interventions
1.2. The Effectiveness of Behavioural Parent Training Interventions
1.3. The Present Study
2. Method
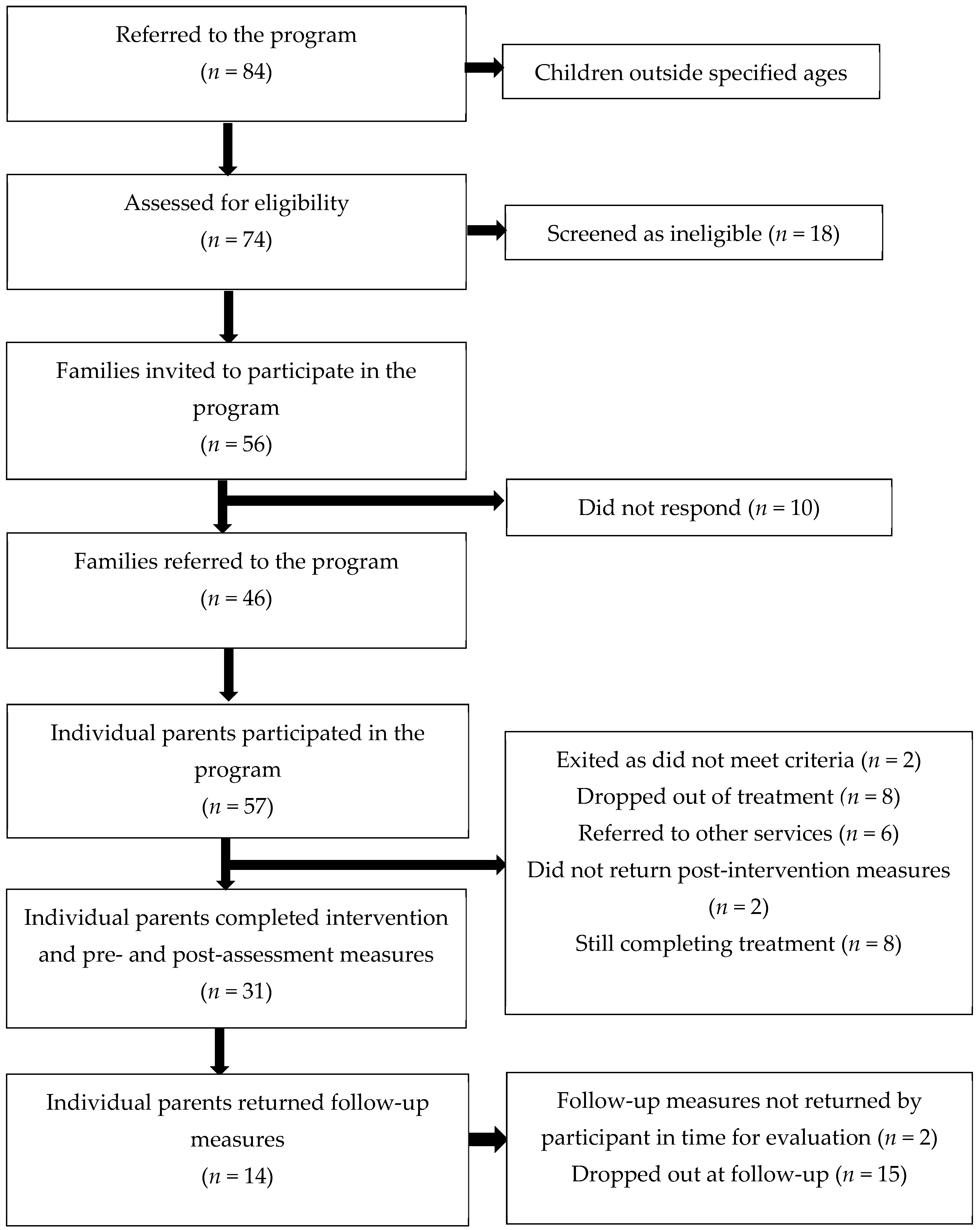
2.1. Participants and Screening
2.2. Design
2.3. Materials
2.3.1. The Child Behaviour Checklist for Ages 1½ to 5
2.3.2. The Parental Stress Index, Short Form
2.3.3. The Depression, Anxiety, and Stress Scales, Short Version
2.4. Ethical Approval
3. Results
3.1. Treatment Effects
3.2. Post Intervention Effects
3.3. Clinical Significance of Change in Emotional and Behavioural Functioning
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lawrence, D.; Johnson, S.; Hafekost, J.; Boterhoven De Haan, K.; Sawyer, M.; Ainley, J.; Zubrick, S.R. The Mental Health of Children and Adolescents; Report on the Second Australian Child and Adolescent Survey of Mental Health and Wellbeing; Department of Health: Canberra, Australia, 2015. [Google Scholar]
- Bayer, J.K.; Hiscock, H.; Ukoumunne, O.C.; Price, A.; Wake, M. Early childhood aetiology of mental health problems: A longitudinal population-based study. J. Child Psychol. Psychiatry 2008, 49, 1166–1174. [Google Scholar] [CrossRef] [PubMed]
- Bayer, J.K.; Sanson, A.V.; Hemphill, S.A. Early childhood aetiology of internalising difficulties: A longitudinal community study. Int. J. Ment. Health Promot. 2010, 12, 16–28. [Google Scholar] [CrossRef]
- Bilancia, S.D.; Resclora, L. Stability of Behavioral and Emotional Problems Over 6 Years in Children Ages 4 to 5 or 6 to 7 at Time 1. J. Emot. Behav. Disord. 2010, 18, 149–161. [Google Scholar] [CrossRef]
- Mesman, J.; Bongers, I.L.; Koot, H.M. Preschool Developmental Pathways to Preadolescent Internalizing and Externalizing Problems. J. Child Psychol. Psychiatry 2001, 42, 679–689. [Google Scholar] [CrossRef] [PubMed]
- Biederman, J.; Faraone, S.V.; Milberger, S.; Jetton, J.G.; Chen, L.; Mick, E.; Russell, R.L. Is childhood oppositional defiant disorder a precursor to adolescent conduct disorder? Findings from a four-year follow-up study of children with ADHD. J. Am. Acad. Child Adolesc. Psychiatry 1996, 35, 1193–1204. [Google Scholar] [CrossRef] [PubMed]
- Briggs-Gowan, M.J.; Carter, A.S. Social-emotional screening status in early childhood predicts elementary school outcomes. Pediatrics 2008, 121, 957–962. [Google Scholar] [CrossRef] [PubMed]
- Bornstein, M.H.; Hahn, C.; Haynes, O.M. Social competence, externalizing and internalizing behavioral adjustment from early childhood through early adolescence: Developmental cascades. Dev. Psychopathol. 2010, 22, 717–735. [Google Scholar] [CrossRef] [PubMed]
- Burke, J.D.; Hipwell, A.E.; Loeber, R. Dimensions of oppositional defiant disorder as predictors of depression and conduct disorder in preadolescent girls. J. Am. Acad. Child Adolesc. Psychiatry 2010, 49, 484–492. [Google Scholar] [PubMed]
- Campbell, S.B.; Spieker, S.; Burchinal, M.; Poe, M.D. Trajectories of aggression from toddlerhood to age 9 predict academic and social functioning through age 12. J. Child Psychol. Psychiatry 2006, 47, 791–800. [Google Scholar] [CrossRef]
- Denham, S.A.; Blair, K.; Schmidt, M.; DeMulder, E. Compromised emotional competence: Seeds of violence sown early? Am. J. Orthopsychiatry 2002, 72, 70–82. [Google Scholar] [CrossRef]
- Fergusson, D.M.; Horwood, L.J.; Ridder, E.M. Show me the child at seven: The consequences of conduct problems in childhood for psychosocial functioning in adulthood. J. Child Psychol. Psychiatry 2005, 46, 837–849. [Google Scholar] [CrossRef] [PubMed]
- Fergusson, D.M.; Horwood, L.J.; Ridder, E.M. Conduct and attentional problems in childhood and adolescence and later substance use, abuse and dependence: Results of a 25-year longitudinal study. Drug Alcohol Depend. 2007, 88, 14–26. [Google Scholar] [CrossRef] [PubMed]
- Jones, D.E.; Greenberg, M.; Crowley, M. Early social-emotional functioning and public health: The relationship between kindergarten social competence and future wellness. Am. J. Public Health 2015, 105, 2283–2290. [Google Scholar] [CrossRef] [PubMed]
- Miles, S.; Stipek, D. Contemporaneous and longitudinal associations between social behavior and literacy achievement in a sample of low-income elementary school children. Child Dev. 2006, 77, 103–117. [Google Scholar] [CrossRef] [PubMed]
- Pardini, D.A.; Fite, P.J. Symptoms of Conduct Disorder, Oppositional Defiant Disorder, Attention-Deficit/Hyperactivity Disorder, and Callous-Unemotional Traits as Unique Predictors of Psychosocial Maladjustment in Boys: Advancing an Evidence Base for DSM-V. J. Am. Acad. Child Adolesc. Psychiatry 2010, 49, 1134–1144. [Google Scholar] [CrossRef] [PubMed]
- Webster-Stratton, C.; Taylor, T. Nipping early risk factors in the bud: Preventing substance abuse, delinquency, and violence in adolescence through interventions targeted at young children (0–8 years). Prev. Sci. 2001, 2, 165–192. [Google Scholar] [CrossRef] [PubMed]
- Hembree-Kigin, T.L.; McNeil, C. Parent—Child Interaction Therapy; Springer: New York, NY, USA, 2013. [Google Scholar]
- Ollendick, T.H.; Greene, R.W.; Austin, K.E.; Fraire, M.G.; Halldorsdottir, T.; Allen, K.B.; Jarrett, M.A.; Lewis, K.M.; Whitmore Smith, M.; Cunningham, N.R.; et al. Parent Management Training and Collaborative & Proactive Solutions: A Randomized Control Trial for Oppositional Youth. J. Clin. Child Adolesc. Psychol. 2016, 45, 591–604. [Google Scholar] [PubMed]
- Eyberg, S.M.; Boggs, S.R.; Rodrigues, C.M. Relationships between maternal parenting stress and child disruptive behaviour. Child Fam. Behav. Ther. 1992, 14, 1–9. [Google Scholar] [CrossRef]
- Kashdan, T.B.; Jacob, R.G.; Pelham, W.E.; Lang, A.R.; Hoza, B.; Blumenthal, J.D.; Gnagy, E.M. Depression and Anxiety in Parents of Children with ADHD and Varying Levels of Oppositional Defiant Behaviors: Modeling Relationships with Family Functioning. J. Clin. Child Adolesc. Psychol. 2004, 33, 169–181. [Google Scholar] [CrossRef]
- Ross, C.M.; Blanc, H.M.; McNeil, C.B.; Eyberg, S.M.; Hembree-Kigin, T.L. Parenting stress in mothers of young children with oppositional defiant disorder and other severe behavior problems. Child Study J. 1998, 28, 93–110. [Google Scholar]
- Mash, E.J.; Johnston, C. Determinants of parenting stress: Illustrations from families of hyperactive children and families of physically abused children. J. Clin. Child Psychol. 1990, 19, 303–328. [Google Scholar] [CrossRef]
- Sanders, M.R.; Wooley, M.L. The relationship between maternal self-efficacy and parenting practices: Implications for parent training. Child Care Health Dev. 2005, 31, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Briggs-Gowan, M.J.; Carter, A.S.; Skuban, E.M.; Horwitz, S.M. Prevalence of social emotional and behavioral problems in a community sample of 1- and 2-year-old children. J. Am. Acad. Child Adolesc. Psychiatry 2001, 40, 811–819. [Google Scholar] [CrossRef] [PubMed]
- Hastings, R.P.; Daley, D.; Burns, C.; Beck, A. Maternal distress and expressed emotion: Cross-sectional and longitudinal relationships with behavior problems of children with intellectual disabilities. Am. J. Ment. Retard. 2006, 111, 48–61. [Google Scholar] [CrossRef]
- Gross, H.E.; Shaw, D.S.; Moilanen, K.L. Reciprocal associations between boys’ externalizing problems and mothers’ depressive symptoms. J. Abnorm. Child Psychol. 2008, 36, 693–709. [Google Scholar] [CrossRef] [PubMed]
- Pelham, W.E.; Lang, A.R.; Atkeson, B.; Murphy, D.A.; Gnagy, E.M.; Greiner, A.R.; Vodde-Hamilton, M.; Greenslade, K.E. Effects of deviant child behavior on parental alcohol consumption: Stress-induced drinking in parents of ADHD children. Am. J. Addict. 1998, 7, 103–114. [Google Scholar] [CrossRef] [PubMed]
- Eisenhower, A.S.; Baker, B.L.; Blacher, J. Children’s delayed development and behavior problems: Impact on mothers’ perceived physical health across early childhood. Soc. Sci. Med. 2009, 68, 89–99. [Google Scholar] [CrossRef]
- Hutchison, L.; Feder, M.; Abar, B.; Winsler, A. Relations between Parenting Stress, Parenting Style, and Child Executive Functioning for Children with ADHD or Autism. J. Child Fam. Stud. 2016, 25, 3644–3656. [Google Scholar] [CrossRef]
- Webster-Stratton, C. Stress: A Potential Disruptor of Parent Perceptions and Family Interactions. J. Clin. Child Psychol. 1990, 4, 302–312. [Google Scholar] [CrossRef]
- Xu, Y.; Farver, J.A.M.; Zhang, Z.; Zeng, Q.; Yu, L.; Cai, B. Mainland Chinese parenting styles and parent–child interaction. Int. J. Behav. Dev. 2005, 29, 524–531. [Google Scholar]
- Holden, E.W.; Banez, G.A. Child abuse potential and parenting stress within maltreating parents. J. Fam. Violence 1996, 1, 1–12. [Google Scholar] [CrossRef]
- Rodriguez, C.M.; Green, A.J. Parenting stress and anger expression as predictors of child abuse potential. Child Abus. Negl. 1997, 21, 367–377. [Google Scholar] [CrossRef]
- Neece, C.L.; Green, S.A.; Baker, B.L. Parenting Stress and Child Behavior Problems: A Transactional Relationship across Time. Am. J. Intellect. Dev. Disabil. 2012, 117, 48–66. [Google Scholar] [CrossRef] [PubMed]
- Patterson, G.R. The early development of coercive family process. In Antisocial Behavior in Children and Adolescents: Developmental Analysis and Model for Intervention; Reid, J.B., Patterson, G.R., Snyder, J., Eds.; American Psychological Association: Washington, DC, USA, 2002; pp. 25–44. [Google Scholar]
- Baker, B.L.; McIntyre, L.L.; Blacher, J.; Crnic, K.; Eelbrock, C.; Low, C. Pre-school children with and without developmental delay: Behaviour problems and parenting stress over time. J. Intellect. Disabil. Res. 2003, 47, 217–230. [Google Scholar] [CrossRef] [PubMed]
- Johnston, C.; Mash, E.J. Families of children with attention-deficit/hyperactivity disorder: Review and recommendations for future research. Clin. Child Fam. Psychol. Rev. 2001, 4, 183–207. [Google Scholar] [CrossRef] [PubMed]
- Sanders, M.R.; Dadds, M.R.; Bor, W. Contextual analysis of child oppositional and maternal aversive behaviors in families of conduct-disordered and nonproblem children. J. Clin. Child Psychol. 1989, 18, 72–83. [Google Scholar] [CrossRef]
- Podolski, C.; Nigg, J.T. Parent stress and coping in relation to child ADHD severity and associated child disruptive behavior problems. J. Clin. Child Psychol. 2001, 30, 503–513. [Google Scholar] [CrossRef]
- Sanders, M.R.; Mazzucchelli, T.G. The promotion of self-regulation through parenting interventions. Clin. Child Fam. Psychol. Rev. 2013, 16, 1–17. [Google Scholar] [CrossRef]
- Eyberg, S.M.; Nelson, M.M.; Boggs, S.R. Evidence-based psychosocial treatments for child and adolescents with disruptive behaviours. J. Clin. Child Adolesc. Psychol. 2008, 37, 215–237. [Google Scholar] [CrossRef]
- Collins, W.A.; Maccoby, E.E.; Steinberg, L.; Hetherington, E.M.; Bornstein, M.H. Contemporary research on parenting: The case for nature and nurture. Am. Psychol. 2000, 55, 218–232. [Google Scholar] [CrossRef]
- Bowlby, J. Attachment and Loss, Volume I Attachment; Penguin Books: Harmondsworth, UK, 1969. [Google Scholar]
- Ainsworth, M.D.S. Infant-mother attachment. Am. Psychol. 1979, 34, 932–937. [Google Scholar] [CrossRef] [PubMed]
- Bandura, A. Self-efficacy: Toward a unifying theory of behavioural change. Psychol. Rev. 1977, 84, 191. [Google Scholar] [CrossRef] [PubMed]
- Hanf, C. A two stage program for modifying maternal controlling during mother-child (MC) interaction. Presented at the Western Psychological Association Meeting, Vancouver, BC, Canada, 1969. [Google Scholar]
- Skinner, B.F. The Behavior of Organisms: An Experimental Analysis; Appleton-Century: New York, NY, USA, 1938. [Google Scholar]
- Granic, I.; Patterson, G.R. Toward a comprehensive model of antisocial development: A dynamic systems approach. Psychol. Rev. 2006, 113, 101. [Google Scholar] [CrossRef] [PubMed]
- Patterson, G.R. Coercive Family Process; Castalia: Eugene, OR, USA, 1982. [Google Scholar]
- Davidov, M.; Grusec, J.E. Untangling the links of parental responsiveness to distress and warmth to child outcomes. Child Dev. 2006, 77, 45–48. [Google Scholar] [CrossRef] [PubMed]
- McLeod, B.D.; Wood, J.J.; Weisz, J.R. Examining the association between parenting and childhood anxiety: A meta-analysis. Clin. Psychol. Rev. 2007, 27, 155–172. [Google Scholar] [CrossRef] [PubMed]
- Piko, B.F.; Balazs, M.A. Control or involvement? Relationship between authoritative parenting style and adolescent depressive symptomatology. Eur. Child Adolesc. Psychiatry 2012, 21, 149–155. [Google Scholar] [CrossRef] [PubMed]
- Rapee, R.M. Family factors in the development and management of anxiety disorders. Clin. Child Fam. Psychol. Rev. 2012, 15, 69–80. [Google Scholar] [CrossRef]
- Spinrad, T.L.; Eisenberg, N.; Gaertner, B.; Popp, T.; Smith, C.L.; Kupfer, A.; Greving, K.; Liew, J.; Hofer, C. Relations of maternal socialization and toddlers’ effortful control to children’s adjustment and social competence. Dev. Psychol. 2007, 43, 1170–1186. [Google Scholar] [CrossRef]
- Wood, J.J.; Mcleod, B.D.; Sigman, M.; Hwang, W.; Chu, B.C. Parenting and childhood anxiety: Theory, empirical findings, and future directions. J. Child Psychol. Psychiatry 2003, 44, 134–151. [Google Scholar] [CrossRef]
- Burnstein, M.; Ginsburg, G.S. The effect of parental modelling of anxious behaviors and cognitions in school-aged children: An experimental pilot study. Behav. Res. Theory 2010, 48, 506–515. [Google Scholar] [CrossRef]
- Kazdin, A.E. Parent Management Training Treatment for Oppositional, Aggressive, and Antisocial Behavior in Children and Adolescents; Oxford University Press: New York, NY, USA, 2005. [Google Scholar]
- Sanders, M.R.; Markie-Dadds, T.K.M.T. Practitioner Manual for Standard Triple P, 2nd ed.; Triple P International: Brisbane, Australia, 2012. [Google Scholar]
- Barkley, R.A. Defiant Children; Guilford Press: New York, NY, USA, 1987. [Google Scholar]
- Eyberg, S. Parent–child interaction therapy: Integration of traditional and behavioral concerns. Child Fam. Behav. Therapy 1988, 10, 33–46. [Google Scholar] [CrossRef]
- Ostrander, R.; Herman, K.C. Potential cognitive, parenting, and developmental mediators of the relationship between ADHD and depression. J. Consult. Clin. Psychol. 2006, 74, 89. [Google Scholar] [CrossRef] [PubMed]
- Choate, M.L.; Pincus, D.B.; Eyberg, S.M.; Barlow, D.H. Parent-Child Interaction therapy for treatment of separation anxiety disorder in young children: A pilot study. Cogn. Behav. Pract. 2005, 12, 126–135. [Google Scholar] [CrossRef]
- Kaminski, J.W.; Valle, L.A.; Filene, J.H.; Boyle, C.L. A Meta-Analytic Review of Components Associated with Parent Training Program Effectiveness. J. Abnorm. Child Psychol. 2008, 36, 567–589. [Google Scholar] [CrossRef] [PubMed]
- McNeil, C.; Norman, M.; Wallace, N. Parent-Child Interaction Therapy. e-J. Aust. Clin. Psychol. Assoc. 2013, 7, 9–12. [Google Scholar]
- Hautmann, C.; Hoijtink, H.; Eichelberger, I.; Hanisch, C.; Pluck, J.; Walter, D.; Dopfner, M. One-Year Follow-up of a Parent Management Training for Children with Externalizing Behaviour Problems in the Real World. Behav. Cogn. Psychother. 2009, 37, 379–396. [Google Scholar] [CrossRef] [PubMed]
- Maughan, D.R.; Christiansen, E.; Jenson, W.R.; Olympia, D.; Clark, E. Behavioral parent training as a treatment for externalizing behaviors and disruptive behavior disorders: A meta-analysis. Sch. Psychol. Rev. 2005, 34, 267. [Google Scholar]
- Fernandez, M.A.; Eyberg, S.M. Predicting Treatment and Follow-up Attrition in Parent–Child Interaction Therapy. J. Abnorm. Child Psychol. 2009, 37, 431–444. [Google Scholar] [CrossRef] [PubMed]
- Friars, P.M.; Mellor, D.J. Drop Out from Behavioral Management Training Programs for ADHD: A Prospective Study. J. Child Fam. Stud. 2007, 16, 427–441. [Google Scholar] [CrossRef]
- Nock, M.K.; Kazdin, A.E. Parent expectancies for child therapy: Assessment and relation to participation in treatment. J. Child Fam. Stud. 2001, 10, 155–180. [Google Scholar] [CrossRef]
- Dretzke, J.; Davenport, C.; Frew, E.; Barlow, J.; Stewart-Brown, S.; Bayliss, S.; Taylor, R.; Sandercock, J.; Hyde, C. The clinical effectiveness of different parenting programs for children with conduct problems: A systematic review of randomized controlled trials. Child Adolesc. Psychiatry Ment. Health 2009, 3, 589–590. [Google Scholar] [CrossRef] [PubMed]
- Bayer, J.K.; Rapee, R.M.; Hiscock, H.; Ukoumunne, O.C.; Mihalopoulos, C.; Clifford, S.; Wake, M. The Cool Little Kids randomised controlled trial: Population-level early prevention for anxiety disorders. BMC Public Health 2011, 11, 11. [Google Scholar] [CrossRef] [PubMed]
- Brestan, E.V.; Eyberg, S.M. Effective psychosocial treatments of conduct-disordered children and adolescents: 29 years, 82 studies, and 5272 kids. J. Clin. Child Psychol. 1998, 27, 180–189. [Google Scholar] [CrossRef] [PubMed]
- Colalillo, S.; Johnston, C. Parenting Cognition and Affective Outcomes Following Parent Management Training: A Systematic Review. Clin. Child Fam. Psychol. Rev. 2016, 19, 216–235. [Google Scholar] [CrossRef] [PubMed]
- Cooley, M.E.; Veldorale-Griffin, A.; Petren, R.E.; Mullis, A.K. Parent–Child Interaction Therapy: A Meta-Analysis of Child Behavior Outcomes and Parent Stress. J. Fam. Soc. Work 2014, 17, 191–208. [Google Scholar] [CrossRef]
- Eckshtain, D.; Kuppens, S.; Weisz, J.R. Amelioration of Child Depression Through Behavioral Parent Training: A Preliminary Study. J. Clin. Child Adolesc. Psychol. 2017, 46, 611–618. [Google Scholar] [CrossRef] [PubMed]
- Lundahl, B.; Risser, H.J.; Lovejoy, M.C. A meta-analysis of parent training: Moderators and follow-up effects. Clin. Psychol. Rev. 2006, 26, 86–104. [Google Scholar] [CrossRef]
- Michelson, D.; Davenport, C.; Dretzke, J.; Barlow, J.; Day, C. Do Evidence-Based Interventions Work When Tested in the ‘‘Real World?’’ A Systematic Review and Meta-analysis of Parent Management Training for the Treatment of Child Disruptive Behavior. Clin. Child Fam. Psychol. Rev. 2013, 16, 18–34. [Google Scholar] [CrossRef]
- Pincus, D.B.; Santucci, L.C.; Ehrenreich, J.T.; Eyberg, S.M. The implementation of modified parent–child interaction therapy for youth with separation anxiety disorder. Cogn. Behav. Pract. 2008, 15, 118–125. [Google Scholar] [CrossRef]
- Sanders, M.R.; Kirby, J.N.; Tellegen, C.L.; Day, J.J. The Triple P-Positive Parenting Program: A systematic review and meta-analysis of a multi-level system of parenting support. Clin. Psychol. Rev. 2014, 34, 337–357. [Google Scholar] [CrossRef]
- Serketich, W.J.; Dumas, J.E. The effectiveness of behavioral parent training to modify antisocial behavior in children: A meta-analysis. Behav. Ther. 1996, 27, 171–186. [Google Scholar] [CrossRef]
- Thomas, R.; Zimmer-Gembeck, M.J. Behavioral outcomes of parent-child interaction therapy and triple p—Positive parenting program: A review and meta-analysis. J. Abnorm. Child Psychol. 2007, 35, 475–495. [Google Scholar] [CrossRef] [PubMed]
- Webster-Stratton, C.; Herman, K.C. The impact of parent behavior-management training on child depressive symptoms. J. Couns. Psychol. 2008, 55, 473–484. [Google Scholar] [CrossRef] [PubMed]
- Hagen, K.A.; Ogden, T.; Bjørnebekk, G. Treatment outcomes and mediators of parent management training: A one-year follow-up of children with conduct problems. J. Clin. Child Adolesc. Psychol. 2011, 40, 165–178. [Google Scholar] [CrossRef] [PubMed]
- Hood, K.K.; Eyberg, S.M. Outcomes of parent-child interaction therapy: Mothers’ reports of maintenance three to six years after treatment. J. Clin. Child Adolesc. Psychol. 2003, 32, 419–429. [Google Scholar] [CrossRef] [PubMed]
- Long, P.; Forehand, R.; Wiserson, M.; Morgan, A. Does parent training with young noncompliant children have long-term effects? Behav. Res. Ther. 1994, 32, 101–107. [Google Scholar] [CrossRef]
- Moreland, D.A.; Felton, J.W.; Hanson, R.F.; Jackson, C.; Dumas, J.E. The Relation Between Parenting Stress, Locus of Control and Child Outcomes: Predictors of Change in a Parenting Intervention. J. Child Fam. Stud. 2016, 25, 2046–2054. [Google Scholar] [CrossRef]
- Wierzbicki, M.; Pekarik, G. A meta-analysis of psychotherapy dropout. Prof. Psychol. Res. Pract. 1993, 24, 190–195. [Google Scholar] [CrossRef]
- Barros, L.; Goes, A.R.; Pereira, A.I. Parental self-regulation, emotional regulation and temperament: Implications for intervention. Estudos Psicol. 2015, 32, 295–306. [Google Scholar] [CrossRef]
- Bowen, M. Family Therapy in Clinical Practice; Jason Aronson: New York, NY, USA; London, UK, 1978. [Google Scholar]
- Kerr, M.; Bowen, M. Family Evaluation: An Approach Based in Brown Theory; Norton: New York, NY, USA, 1988. [Google Scholar]
- Kochanska, G.; Coy, K.C.; Murray, K.T. The development of self-regulation in the first four years of life. Child Dev. 2001, 72, 1091–1111. [Google Scholar] [CrossRef]
- Kochanska, G.; Murray, K.T. Mother–child mutually responsive orientation and conscience development: From toddler to early school age. Child Dev. 2000, 71, 417–431. [Google Scholar] [CrossRef] [PubMed]
- Wadlinger, H.A.; Isaacowitz, D.M. Fixing our focus: Training attention to regulate emotion. Personal. Soc. Psychol. Rev. 2011, 15, 75–102. [Google Scholar] [CrossRef] [PubMed]
- Tully, L.A.; Hunt, C. A randomized controlled trial of a brief versus standard group parenting program for toddler aggression. Aggress. Behav. 2017, 43, 291–303. [Google Scholar] [CrossRef] [PubMed]
- Metzler, C.W.; Sanders, M.R.; Rusby, J.C.; Crowley, R.N. Using consumer preference information to increase the reach and impact of media-based parenting interventions in a public health approach to parenting support. Behav. Ther. 2012, 43, 257–270. [Google Scholar] [CrossRef] [PubMed]
- Stolk, M.N.; Mesman, J.; van Zeijl, J.; Alink, L.R.; Bakermans-Kranenburg, M.J.; van IJzendoorn, M.H.; Juffer, F.; Koot, H.M. Early parenting intervention: Family risk and first-time parenting related to intervention effectiveness. J. Child Fam. Stud. 2008, 17, 55. [Google Scholar] [CrossRef]
- Achenbach, T.; Rescorla, L. Manual for the ASEBA Preschool Forms and Profiles; University of Vermont, Research Center for Children, Youth, and Families: Burlington, MA, USA, 2000. [Google Scholar]
- Lovibond, P.F.; Lovibond, S.H. The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav. Res. Ther. 1995, 33, 335–343. [Google Scholar] [CrossRef]
- Abidin, R.R. Parenting Stress Index-Manual, 3rd ed.; Pediatric Psychology Press: Charlottesville, VA, USA, 1990. [Google Scholar]
- Haskett, M.E.; Ahern, L.S.; Ward, C.S.; Allaire, J.C. Factor structure and validity of the parenting stress index-short form. J. Clin. Child Adolesc. Psychol. 2006, 35, 302–312. [Google Scholar] [CrossRef]
- Reitman, D.; Currier, R.O.; Stickle, T.R. A critical evaluation of the Parenting Stress Index-Short Form (PSI-SF) in a head start population. J. Clin. Child Adolesc. Psychol. 2002, 31, 384–392. [Google Scholar] [CrossRef]
- Antony, M.M.; Bieling, P.J.; Cox, B.J.; Enns, M.W.; Swinson, R.P. Psychometric properties of the 42-item and 21-item versions of the Depression Anxiety Stress Scales in clinical groups and a community sample. Psychol. Assess. 1998, 10, 176. [Google Scholar] [CrossRef]
- Brown, T.A.; Chorpita, B.F.; Korotitsch, W.; Barlow, D.H. Psychometric properties of the Depression Anxiety Stress Scales (DASS) in clinical samples. Behav. Res. Ther. 1997, 35, 79–89. [Google Scholar] [CrossRef]
- Cohen, J. Some statistical issues in psychological research. In Handbook of Clinical Psychology; Wolman, B.B., Ed.; McGraw-Hill: New York, NY, USA, 1965; pp. 95–121. [Google Scholar]
- Jacobson, N.S.; Follette, W.C.; Revenstorf, D. Toward a standard definition of clinically significant change. Behav. Ther. 1996, 15, 309–311. [Google Scholar] [CrossRef]
- Jacobson, N.S.; Truax, P. Clinical significance: A statistical approach to defining meaningful change in psychotherapy research. J. Consult. Clin. Psychol. 1991, 59, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Chase, R.M.; Eyberg, S.M. Clinical presentation and treatment outcome for children with comorbid externalizing and internalizing symptoms. J. Anxiety Disord. 2008, 22, 273–282. [Google Scholar] [CrossRef] [PubMed]
- Williford, A.P.; Calkins, S.D.; Keane, S.P. Predicting change in parenting stress across early childhood: Child and maternal factors. J. Abnorm. Child Psychol. 2007, 35, 251–263. [Google Scholar] [CrossRef] [PubMed]
- Eyberg, S.M.; Nelson, M.M.; Ginn, N.C.; Bhuiyan, N.; Boggs, S.R. Dyadic Parent Child Interaction Coding System: Comprehensive Manual for Research and Training; PCIT International: Gainesville, FL, USA, 2013. [Google Scholar]
- Feldman, R. Coding Interactive Behavior Manual; Bar-Ilan University: Ramat Gan, Israel, 1998; Unpublished manual. [Google Scholar]
| Sociodemographic Variables | Mean (SD), Range |
|---|---|
| Child age (months) | 31.5 (9.51), 16 to 47 |
| Parent age (years) | 37.1 (4.84), 27 to 46 |
| n (%) | |
| Parent gender male | 14 (45) |
| Child gender male | 18 (60) |
| Child’s cultural group | |
| Caucasian | 21 (70) |
| South East Asian | 3 (10) |
| Chinese | 2 (7) |
| European | 2 (7) |
| Indigenous Australian | 1 (3) |
| Parent employment | |
| Full time | 16 (53) |
| Part time | 3 (10) |
| Full time parenting | 11 (37) |
| Parent education | |
| Year 12 or less | 1 (3) |
| TAFE college/trade certificate | 1 (3) |
| University degree | 28 (94) |
| Family income | |
| $100,000 to $150,000 | 10 (38) |
| $180,000 to $190,000 | 3 (13) |
| $200,000 to $250,000 | 4 (15) |
| $300,000 to $350,000 | 9 (33) |
| $700,000 | 1 (1) |
| Child attends childcare | |
| 1 day | 6 (20) |
| 2 days | 7 (23) |
| 3 days | 5 (18) |
| 4 days | 4 (13) |
| 5 days | 8 (27) |
| Previous treatment for presenting concerns | 2 (7) |
| Previous diagnosis | 1 (3) |
| Measure | Pre-Intervention | Post-Intervention | Follow-Up | ||||||
|---|---|---|---|---|---|---|---|---|---|
| n | Mean | SD | n | Mean | SD | n | Mean | SD | |
| CBCL | |||||||||
| Affective Problems | 31 | 4.54 | 3.06 | 31 | 1.90 * | 1.65 | 14 | 2.00 ns | 1.88 |
| Anxiety Problems | 31 | 4.14 | 2.59 | 31 | 2.10 ** | 2.91 | 14 | 1.86 ns | 1.66 |
| OD Problems | 31 | 6.3 | 3.08 | 31 | 3.00 ** | 1.96 | 14 | 2.86 ns | 1.35 |
| ADH Problems | 31 | 6.25 | 2.88 | 31 | 3.66 ** | 2.24 | 14 | 3.29 ns | 2.13 |
| DASS-21 | |||||||||
| Depression | 31 | 3.21 | 2.72 | 31 | 2.22 ** | 2.82 | 14 | 2.07 ns | 2.67 |
| Anxiety | 31 | 2.56 | 1.91 | 31 | 1.14 ** | 1.84 | 14 | 1.21 ns | 2.15 |
| Stress | 31 | 7.26 | 2.41 | 31 | 5.30 ** | 2.58 | 14 | 4.71 ns | 2.52 |
| PSI-SF | |||||||||
| DC | 31 | 27.85 | 6.96 | 31 | 16.78 ** | 6.85 | 14 | 15.93 ns | 7.3 |
| PCDI | 31 | 12.69 | 5.35 | 31 | 9.04 * | 4.8 | 14 | 8.86 ns | 5.43 |
| PD | 31 | 18.89 | 5.62 | 31 | 12.78 ** | 6.77 | 12 | 10.58 ns | 7.43 |
| Measure | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
|---|---|---|---|---|---|---|---|---|---|
| 1. CBCL AffP | . | ||||||||
| 2. CBCL AnxP | 0.321 | ||||||||
| 3. CBCL ODP | 569 ** | 0.106 | |||||||
| 4. CBCL ADHP | 0.518 ** | −0.211 | 0.681 ** | ||||||
| 5. DASS-21 Dep | 0.091 | −0.11 | −0.002 | 0.267 | |||||
| 6. DASS-21 Anx | 0.212 | −0.048 | 0.047 | 0.303 | 0.403 * | ||||
| 7. DASS-21 Stress | 0.404 ** | 0.035 | 0.266 | 0.694 ** | 0.02 | 0.269 | |||
| 8. PSI-SF DC | 0.498 ** | 0.33 | 0.641 ** | 0.521 ** | 0.408 * | 0. 075 | 0.256 | ||
| 9. PSI-SF PCDI | 0.354 | 0.258 | 0.042 | −0.078 | 0.047 | 0.179 | 0.017 | 0.405 * | |
| 10. PSI-SF PD | −0.17 | −0.04 | −0.113 | 0.231 | 0.348 | 0.390 * | 0.296 | 0.18 | −0.124 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
McAloon, J.; Lazarou, K.D. Preventative Intervention for Social, Emotional and Behavioural Difficulties in Toddlers and Their Families: A Pilot Study. Int. J. Environ. Res. Public Health 2019, 16, 569. https://doi.org/10.3390/ijerph16040569
McAloon J, Lazarou KD. Preventative Intervention for Social, Emotional and Behavioural Difficulties in Toddlers and Their Families: A Pilot Study. International Journal of Environmental Research and Public Health. 2019; 16(4):569. https://doi.org/10.3390/ijerph16040569
Chicago/Turabian StyleMcAloon, John, and Karina D. Lazarou. 2019. "Preventative Intervention for Social, Emotional and Behavioural Difficulties in Toddlers and Their Families: A Pilot Study" International Journal of Environmental Research and Public Health 16, no. 4: 569. https://doi.org/10.3390/ijerph16040569
APA StyleMcAloon, J., & Lazarou, K. D. (2019). Preventative Intervention for Social, Emotional and Behavioural Difficulties in Toddlers and Their Families: A Pilot Study. International Journal of Environmental Research and Public Health, 16(4), 569. https://doi.org/10.3390/ijerph16040569




