Heat Stress in Indoor Environments of Scandinavian Urban Areas: A Literature Review
Abstract
1. Introduction
- -
- To investigate how severe heat can develop indoors;
- -
- How severe heat can be identified in indoor environments;
- -
- To describe local level actions that have scientific support.
2. Materials and Methods
3. Results and Discussion
3.1. The Relationship between the Outdoor and Indoor Climate
3.2. Risk Groups
3.3. Combination Effects of Heat in Indoor Environments
3.3.1. Heat and Air Quality
3.3.2. Heat and Energy Efficient Housing
3.3.3. Heat and Social Participation
3.4. Identification and Evaluation of Severe Heat in Indoor Environments
3.4.1. The Wet Bulb Globe Temperature (WBGT)
3.4.2. The Predicted Heat Strain (PHS) Model
3.4.3. The Thermal Work Limit (TWL)
3.4.4. The Equivalent Temperature (ET)
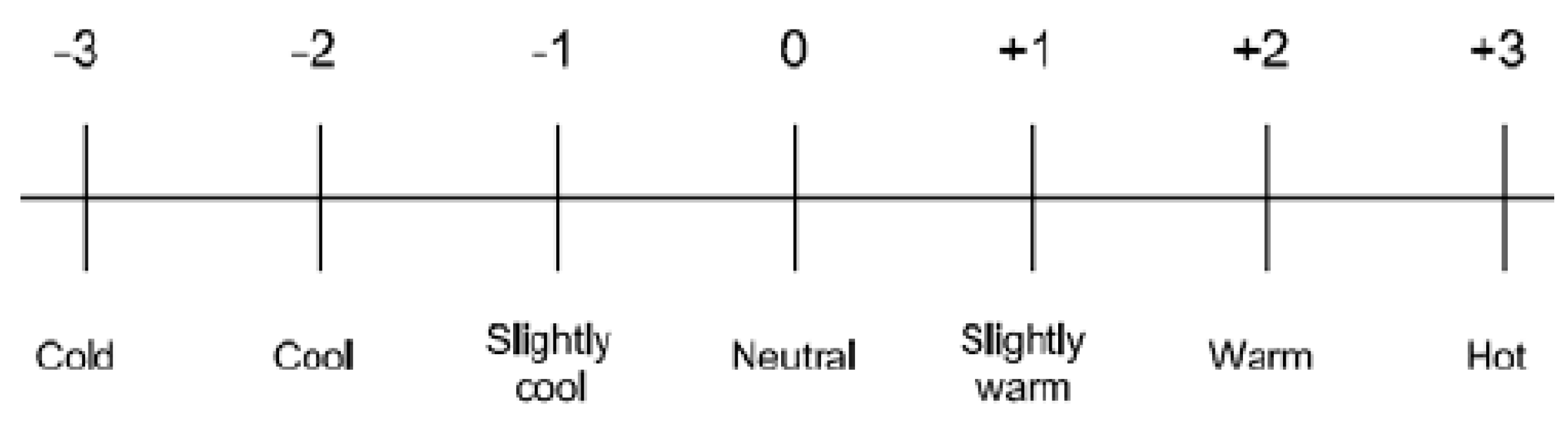
3.4.5. Thermal Comfort Evaluation
- A psychological assessment that sees thermal comfort as a state of mind that expresses satisfaction with the thermal environment [9].
- A thermophysiological assessment focusing on the thermal receptors in the skin and hypothalamus and based on the heat balance equation [9].
- An adaptive assessment based on field studies that look at adaptive comfort, psychology, and behavior. The assessment takes into consideration the local context, for example, the indoor comfort temperature is calculated from the outside temperature using an adaptive algorithm [63].
3.4.6. The Need for the Development of a Heat Index for Indoor Environments
3.5. Solutions to the Development of Severe Heat Stress in Indoor Environments
3.5.1. Microclimate Solutions
3.5.2. Macroclimatic Solutions
4. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- IPCC (Intergovernmental Panel on Climate Change). IPCC Fifth Assessment Report: Climate Change, 2013: The Physical Science Basis; Cambridge University Press: Cambridge, UK, 2013. [Google Scholar]
- Oke, T.R. The energetic basis of the urban heat island. Q. J. R. Meteorol. Soc. 1982, 108, 1–24. [Google Scholar] [CrossRef]
- Półrolniczak, M.; Tomczyk, A.M.; Kolendowicz, L. Thermal Conditions in the City of Poznań (Poland) during Selected Heat Waves. Atmosphere 2018, 9, 11. [Google Scholar] [CrossRef]
- Tomczyk, A.M.; Piotrowski, P.; Bednorz, E. Warm spells in Northern Europe in relation to atmospheric circulation. Theor. Appl. Climatol. 2017, 128, 623–634. [Google Scholar] [CrossRef]
- Nazaroff, W.W. Exploring the consequences of climate change for indoor air quality. Environ. Res. Lett. 2013, 8, 015022. [Google Scholar] [CrossRef]
- WHO (World Health Organization). Improving Public Health Responses to Extreme Weather/Heat-Waves—EuroHEAT: Technical Summary; WHO Regional Office for Europe: Copenhagen, Denmark, 2009; Available online: http://apps.who.int/iris/bitstream/handle/10665/107935/E92474.pdf;jsessionid=837E9E472218EAC8D179B0C4E04774D5?sequence=1 (accessed on 12 February 2018).
- Oudin Åström, D.; Åström, C.; Forsberg, B.; Vicedo-Cabrarera, A.M.; Gasparrini, A.; Oudin, A.; Sundquist, K. Heat wave–related mortality in Sweden: A case-crossover study investigating effect modification by neighbourhood deprivation. Scand. J. Public Health 2018. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, C.S.; Zhang, J.; Sigsgaard, T.; Jantunen, M.; Lioy, P.J.; Samaon, R.; Karol, M.H. Current state of the science: Health effects and indoor environmental quality. Environ. Health Perspect. 2007, 115, 958–964. [Google Scholar] [CrossRef] [PubMed]
- Höppe, P. Different aspects of assessing indoor and outdoor thermal comfort. Energy Build. 2002, 34, 661–665. [Google Scholar] [CrossRef]
- Givoni, B. Comfort, climate analysis and building design guidelines. Energy Build. 1992, 18, 11–23. [Google Scholar] [CrossRef]
- Quinn, A.; Tamerius, J.D.; Perzanowski, M.; Jacobson, J.S.; Goldstein, I.; Acosta, L.; Shaman, J. Predicting indoor heat exposure risk during extreme heat events. Sci. Total Environ. 2014, 490, 686–693. [Google Scholar] [CrossRef]
- Franck, U.; Kruger, M.; Schwarz, N.; Grossmann, K.; Röder, S.; Schlink, U. Heat stress in urban areas: Indoor and outdoor temperatures in different urban structure types and subjectively reported well-being during a heat wave in the city of Leipzig. Meteorol. Z. 2013, 22, 167–177. [Google Scholar] [CrossRef]
- Uejio, C.K.; Tamerius, J.D.; Vredenburg, J.; Asaeda, G.; Isaacs, D.A.; Braun, J.; Quinn, A.; Freese, J.P. Summer indoor heat exposure and respiratory and cardiovascular distress calls in New York City, NY, U.S. Indoor Air 2016, 26, 594–604. [Google Scholar] [CrossRef] [PubMed]
- White-Newsome, J.L.; Sanchez, B.N.; Jolliet, O.; Zhang, Z.; Parker, E.A.; Dvonch, J.T.; O’neill, M.S. Climate change and health: Indoor heat exposure in vulnerable populations. Environ. Res. 2012, 112, 20–27. [Google Scholar] [CrossRef] [PubMed]
- Walikewitz, N.; Jänicke, B.; langner, M.; Endlicher, W. Assessment of indoor heat stress variability in summer and during heat warnings: A case study using the UTCI in Berlin, Germany. Int. J. Biometeorol. 2018, 62, 29–42. [Google Scholar] [CrossRef] [PubMed]
- Anderson, M.; Carmichael, C.; Murray, V.; Dengel, A.; Swainson, M. Defining indoor heat thresholds for health in the UK. Perspect. Public Health 2013, 133, 158–164. [Google Scholar] [CrossRef] [PubMed]
- Roberts, D.; Lay, K. Variability in Measured Space Temperatures in 60 Homes; National Renewable Energy Laboratory Technical Report, NREL/TP-5500-58059; U.S. Department of Energy: Golden, CO, USA, 2013; pp. 1–47.
- Roaf, S.; Crichton, D.; Nicol, F. Adapting Buildings and Cities for Climate Change—A 21st Century Survival Guide, 2nd ed.; Architectural Press: Amsterdam, The Netherlands, 2009. [Google Scholar]
- WHO (World Health Organization). Heat-Waves: Risks and Responses; Health and Global Environmental Change Series; No. 2; WHO Regional Office for Europe: Copenhagen, Denmark, 2004; Available online: http://www.euro.who.int/__data/assets/pdf_file/0008/96965/E82629.pdf (accessed on 10 March 2018).
- Tamerius, J.D.; Perzanowski, M.S.; Acosta, L.M.; Jacobson, J.S.; Goldstein, I.F.; Quinn, J.W.; Rundle, A.G.; Shaman, J. Socioeconomic and outdoor meteorological determinants of indoor temperature and humidity in New York City dwellings. Weather Clim. Soc. 2013, 5, 168–179. [Google Scholar] [CrossRef]
- Hawkins-Bell, L.; Rankin, J.T. Heat-related deaths—Philadelphia and United States, 1993–1994. Morb. Mortal. Wkly. Rep. 1994, 43, 453–455. [Google Scholar]
- Bernhard, M.C.; Kent, S.T.; Sloan, M.E.; Evans, M.B.; McClure, L.A.; Gohlke, J.M. Measuring personal heat exposure in an urban and rural environment. Environ. Res. 2015, 137, 410–418. [Google Scholar] [CrossRef]
- Kuras, E.; Hondula, D.; Brown-Saracino, J. Heterogeneity in individually experienced temperatures (IETs) within an urban neighborhood: Insights from a new approach to measuring heat exposure. Int. J. Biometeorol. 2015, 59, 1363–1372. [Google Scholar] [CrossRef]
- Kovats, R.; Hajat, S. Heat Stress and Public Health: A Critical Review. Annu. Rev. Public Health 2008, 29, 41–55. [Google Scholar] [CrossRef]
- Chan, N.Y.; Stacey, M.T.; Smith, A.E.; Ebi, K.L.; Wilson, T.F. An empirical mechanistic framework for heat-related illness. Clim. Res. 2001, 16, 133–143. [Google Scholar] [CrossRef]
- Klinenberg, E. Heat Wave: A Social Autopsy of Disaster in Chicago; University of Chicago Press: Chicago, IL, USA, 2002. [Google Scholar]
- Nguyen, J.L.; Schwartz, J.; Dockery, D.W. The relationship between indoor and outdoor temperature, apparent temperature, relative humidity, and absolute humidity. Indoor Air 2014, 24, 103–112. [Google Scholar] [CrossRef] [PubMed]
- Ormandy, D.; Ezratty, V. Health and thermal comfort: From WHO guidance to housing strategies. Energy Policy 2012, 49, 116–121. [Google Scholar] [CrossRef]
- Haines, A.; Kovats, R.S.; Campbell-Lendrum, D.; Corvalan, C. Climate change and human health: Impacts, vulnerability and public health. Public Health 2006, 120, 585–596. [Google Scholar] [CrossRef] [PubMed]
- Fouillet, A.; Rey, G.; Laurent, F.; Pavillon, G.; Bellec, S.; Guihenneuc-Jouyaux, C.; Clavel, J.; Jougla, E.; Hémon, D. Excess mortality related to the August 2003 heat wave in France. Int. Arch. Occup. Environ. Health 2006, 80, 16–24. [Google Scholar] [CrossRef] [PubMed]
- Hajat, S.; Kovats, R.S.; Lachowycz, K. Heat-related and cold-related deaths in England and Wales: Who is at risk? Occup. Environ. Med. 2007, 64, 93–100. [Google Scholar] [CrossRef]
- Kjellström, K.; Lemke, B. Health Impacts of Workplace Heat on Persons with Existing Ill Health. Systematiska kunskapsöversikter; 11. Arbete och Hälsa 2017, 51, 1–69. [Google Scholar]
- Van Loenhout, J.A.F.; le Grand, A.; Dujim, F.; Greven, F.; Vink, N.M.; Hoek, G.; Zuurbier, M. The effect of high indoor temperatures on self-perceived health of elderly persons. Environ. Res. 2016, 146, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Rahman, J.; Fakhruddin, S.H.; Rahman, A.K.; Halim, M.A. Environmental heat stress among young working women: A pilot study. Ann. Glob. Health 2016, 82, 760–767. [Google Scholar] [CrossRef]
- Asamoah, B.; Kjellström, T.; Östergren, P.-O. Is ambient heat exposure levels associated with miscarriage or stillbirths in hot regions? A cross-sectional study using survey data from the Ghana Maternal Health Survey 2007. Int. J. Biometeorol. 2018, 62, 319–330. [Google Scholar] [CrossRef]
- Cox, B.; Vicedo-Cabrera, A.M.; Gasparrini, A.; Roels, H.A.; Martens, E.; Vangronsveld, J.; Forsberg, B.; Nawrot, T.S. Ambient temperature as a trigger of preterm delivery in a temperate climate. J. Epidemiol. Community Health 2016, 70, 1191–1199. [Google Scholar] [CrossRef]
- Lundgren, K.; Kuklane, K.; Gao, C.; Holmér, I. Effects of heat stress on working populations when facing climate change. Ind. Health 2013, 51, 3–15. [Google Scholar] [CrossRef]
- Hanna, E.G.; Kjellström, T.; Bennett, C.; Dear, K. Climate change and rising heat: Population health implications for working people in Australia. Asia Pac. J. Public Health 2011, 23 (Suppl. 2), 14S–26S. [Google Scholar] [CrossRef] [PubMed]
- Bassil, K.L.; Cole, D.C. Effectiveness of public health interventions in reducing morbidity and mortality during heat episodes: A structured review. Int. J. Environ. Res. Public Health 2010, 7, 991–1001. [Google Scholar] [CrossRef] [PubMed]
- Bell, M.L.; Dominici, F. Effect modification by community characteristics on the short-term effects of ozone exposure and mortality in 98 US communities. Am. J. Epidemiol. 2008, 167, 986–987. [Google Scholar] [CrossRef] [PubMed]
- Wells, J.R.; Schoemaecker, C.; Carslaw, N.; Waring, M.S.; Ham, J.; Nelissen, I.; Wolkoff, P. Reactive Indoor Air Chemistry and Health—A Workshop Summary. Int. J. Hyg. Environ. Health 2017, 220, 1222–1229. [Google Scholar] [CrossRef] [PubMed]
- Salthammer, T.; Zhang, Y.; Mo, J.; Koch, H.M.; Weschler, C.J. Assessing human exposure to organic pollutants in the indoor environment. Angew. Chem. Int. Ed. Engl. 2018, 57, 12228–12263. [Google Scholar] [CrossRef] [PubMed]
- Potera, C. Climate Change Impacts Indoor Environment. Environ. Health Perspect. 2011, 119. [Google Scholar] [CrossRef] [PubMed]
- IIASA (International Institute for Applied Systems Analysis). Global Energy Assessment. Ch.10—Energy End-Use: Buildings, 2012. Available online: http://www.iiasa.ac.at/web/home/research/Flagship-Projects/Global-Energy-Assessment/GEA_CHapter10_buildings_lowres.pdf (accessed on 20 March 2018).
- Akeiber, H.; Nejat, P.; Majid, M.Z.A.; Wahid, M.A.; Jomehzadeh, F.; Famileh, I.Z.; Calautit, J.K.; Hughes, B.R.; Zaki, S.A. A review on phase change material (PCM) for sustainable passive cooling in building envelopes. Renew. Sustain. Energy Rev. 2016, 60, 1470–1497. [Google Scholar] [CrossRef]
- Seppänen, O.A.; Fisk, W.J. Summary of human responses to ventilation. Indoor Air 2004, 14, 102–118. [Google Scholar] [CrossRef] [PubMed]
- Lindemann, U.; Skelton, D.A.; Oksa, J.; Beyer, N.; Rapp, K.; Becker, C.; Klenk, J. Social participation and heat-related behaviour in older adults during heat waves and on other days. Z. Gerontol. Geriatr. 2017, 51, 543–549. [Google Scholar] [CrossRef]
- Parsons, K. Human Thermal Environments: The Effects of Hot, Moderate, and Cold Environments on Human Health, Comfort, and Performance, 3rd ed.; CRC Press: Boca Raton, FL, USA, 2014. [Google Scholar]
- Anderson, B.G.; Bell, M.L. Weather-related mortality: How heat, cold, and heat waves affect mortality in the United States. Epidemiology 2009, 20, 205–213. [Google Scholar] [CrossRef]
- Forzieri, G.; Cescatti, A.; Batista e Silva, F.; Feyen, L. Increasing risk over time of weather-related hazards to the European population: A data-driven prognostic study. Lancet Planet. Health 2017, 1, e200–e208. [Google Scholar] [CrossRef]
- Gasparrini, A.; Guo, Y.; Hashizume, M.; Lavigne, E.; Zanobetti, A.; Schwartz, J.; Tobias, A.; Tong, S.; Rocklöv, J.; Forsberg, B.; et al. Mortality risk attributable to high and low ambient temperature: A multicountry observational study. Lancet 2015, 386, 369–375. [Google Scholar] [CrossRef]
- Åström, D.O.; Schifano, P.; Asta, F.; Lallo, A.; Michelozzi, P.; Rocklöv, J.; Forsberg, B. The effect of heat waves on mortality in susceptible groups: A cohort study of a Mediterranean and a northern European City. Environ. Health 2015, 14, 30. [Google Scholar] [CrossRef] [PubMed]
- Brake, D.J.; Bates, G.P. Limiting metabolic rate (Thermal Work Limit) as an index of thermal stress. Appl. Occup. Environ. Hyg. 2002, 17, 176–186. [Google Scholar] [CrossRef] [PubMed]
- ISO (International Standardization Organization). Ergonomics of the Thermal Environment—Assessment of Heat Stress Using the WBGT (Wet Bulb Globe Temperature) Index; ISO 7243; ISO: Geneva, Switzerland, 2017. [Google Scholar]
- ISO (International Standardization Organization). Ergonomics of the Thermal Environment—Analytical Determination and Interpretation of Heat Stress Using Calculation of the Predicted Heat Strain; ISO 7933; ISO: Geneva, Switzerland, 2004. [Google Scholar]
- Malchaire, J. Occupational heat stress assessment by the Predicted Heat Strain model. Ind. Health 2006, 44, 380–387. [Google Scholar] [CrossRef] [PubMed]
- Malchaire, J.; Piette, A.; Kampmann, B.; Mehnert, P.; Gebhardt, H.; Havenith, G.; Den Hartog, E.; Holmer, I.; Parsons, K.; Alfano, G.; et al. Development and Validation of the Predicted Heat Strain Model (PHS). Ann. Occup. Hyg. 2001, 45, 123–135. [Google Scholar] [CrossRef]
- Malchaire, J.; Kampmann, B.; Havenith, G.; Mehnert, P.; Gebhardt, H. Criteria for estimating acceptance exposure times in hot working environments: A review. Int. Arch. Occup. Environ. Health 2000, 73, 215–220. [Google Scholar] [CrossRef] [PubMed]
- Gameiro da Silva, M.C. Measurements of comfort in vehicles. Meas. Sci. Technol. 2002, 13, R41–R60. [Google Scholar] [CrossRef]
- Nilsson, H.; Holmér, I.; Bohm, M.; Norén, O. Definition and theoretical background of the Equivalent Temperature. In CABCLI Consortium; Swedish Institute of Agricultural and Environmental Engineering: Florence, Italy, 1999. [Google Scholar]
- WHO (World Health Organization). Health Impact of Low Indoor Temperatures: Report on a WHO Meeting; WHO Regional Office for Europe: Copenhagen, Denmark, 1987. [Google Scholar]
- Nicol, J.F.; Roaf, S. Adaptive thermal comfort and passive architecture. In Advances in Passive Cooling; Santamouris, M., Ed.; Routledge: London, UK, 2012. [Google Scholar]
- Nicol, J.F.; Humphreys, M.A. Adaptive thermal comfort and sustainable thermal standards for buildings. Energy Build. 2002, 34, 563–572. [Google Scholar] [CrossRef]
- Olesen, B.W. International standards for the indoor environment. Indoor Air 2004, 14, 18–26. [Google Scholar] [CrossRef]
- Fanger, P.O. Thermal Comfort: Analysis and Applications in Environmental Engineering; Danish Technical Press: Copenhagen, Denmark, 1970. [Google Scholar]
- ISO (International Standards Organization). Ergonomics of the Thermal Environment—Assessment of the Influence of the Thermal Environment Using Subjective Judgement Scales; ISO 10551; ISO: Geneva, Switzerland, 1995. [Google Scholar]
- deDear, R.J.; Brager, G.S. Thermal Comfort in naturally ventilated buildings: Revisions to ASHRAE standard 55. Energy Build. 2002, 34, 549–561. [Google Scholar] [CrossRef]
- Nicol, J.F. Adaptive thermal comfort standards in the hot-humid tropics. Energy Build. 2004, 36, 628–637. [Google Scholar] [CrossRef]
- Chappells, H.; Shove, E. Debating the future of comfort: Environmental sustainability, energy consumption and the indoor environment. Build. Res. Inf. 2005, 33, 32–40. [Google Scholar] [CrossRef]
- Boerstra, A.C.; te Kulve, M.; Toftum, J.; Loomans, M.G.L.C.; Olesen, B.W.; Hensen, J.L.M. Comfort and performance impact of personal control over thermal environment in summer: Results from a laboratory study. Build. Environ. 2015, 87, 315–326. [Google Scholar] [CrossRef]
- Matzarakis, A. The Heat Health Warning System of DWD—Concept and Lessons Learned. In Perspectives in Atmospheric Sciences; Karacostas, T., Bais, A., Nastos, P., Eds.; Springer: Cham, Switzerland, 2017; pp. 191–196. [Google Scholar]
- Rosenfelder, M.; Koppe, C.; Pfafferott, J.; Matzarakis, A. Effects of ventilation behaviour on indoor heat load based on test reference years. Int. J. Biometeorol. 2016, 60, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Pfafferott, J.; Koppe, C.; Reetx, C. Extention of the Heat health Warning System by indoor heat prediction. In Proceedings of the Climate and Constructions International Conference, Karlsruhe, Germany, 24–15 October 2011. [Google Scholar]
- Pfafferott, J.; Becker, P. Erweiterung des Hitzewarnsystems um die Vorhersage der Wärmebelastung in Innenräumen. Bauphysik 2008, 30, 237–243. [Google Scholar] [CrossRef]
- Smargiassi, A.; Fournier, M.; Griot, C.; Baudouin, Y.; Kosatsky, T. Prediction of the indoor temperatures of an urban area with an in-time regression mapping approach. J. Expo. Sci. Environ. Epidemiol. 2008, 18, 282–288. [Google Scholar] [CrossRef]
- Fountain, M.; Brager, G.; de Dear, R. Expectations of indoor climate control. Energy Build. 1996, 24, 179–182. [Google Scholar] [CrossRef]
- Lundgren-Kownacki, K.; Dalholm Hornyanszky, E.; Tuan, A.C.; Alkan Olsson, J.; Becker, P. Challenges with using air-conditioning in an increasingly hot climate. Int. J. Biometeorol. 2017, 62, 401–412. [Google Scholar] [CrossRef]
- Kwok, A.G.; Rajkovich, N.B. Addressing climate change in comfort standards. Build. Environ. 2010, 45, 18–22. [Google Scholar] [CrossRef]
- Zhang, H.; Arens, E.; Huizenga, C.; Han, T. Thermal sensation and comfort models for non-uniform and transient environments, part II: Local comfort of individual body parts. Build. Environ. 2010, 45, 389–398. [Google Scholar] [CrossRef]
- Walløe, L. Arterio-venous anastomoses in the human skin and their role in temperature control. Temperature 2015, 3, 92–103. [Google Scholar] [CrossRef] [PubMed]
- Taylor, N.A.S.; Machado-Moreira, C.A.; van den Heuvel, A.M.J.; Caldwell, J.N. Hands and feet: Physiological insulators, radiators and evaporators. Eur. J. Appl. Physiol. 2014, 114, 2037–2060. [Google Scholar] [CrossRef] [PubMed]
- De Groot, D.W.; Gallimore, R.P.; Thompson, S.M.; Kenefick, R.W. Extremity cooling for heat stress mitigation in military and occupational settings. J. Therm. Biol. 2013, 38, 305–310. [Google Scholar] [CrossRef]
- Chakroun, W.; Ghaddar, N.; Ghali, K. Chilled ceiling and displacement ventilation aided with personalized evaporative cooler. Energy Build. 2011, 43, 3250–3257. [Google Scholar] [CrossRef]
- Vesely, M.; Zeiler, W. Personalized conditioning and its impact on thermal comfort and energy performance—A review. Renew. Sustain. Energy Rev. 2014, 34, 401–408. [Google Scholar] [CrossRef]
- Zhao, M.; Gao, C.; Wang, F.; Kuklane, K.; Holmér, I.; Li, J. A study on local cooling of garments with ventilation fans and openings placed at different torso sites. Int. J. Ind. Ergon. 2013, 43, 232–237. [Google Scholar] [CrossRef]
- Kuklane, K.; Gao, C.; Holmér, I. Ventilation solutions in clothing. In Proceedings of the 10th Joint International Scientific Conference CLOTECH: Innovations in Textile Materials and Protective Clothing, Warszawa, Poland, 20–21 September 2012; Technical University of Lodz Press: Lodz, Poland, 2012; pp. 205–212. [Google Scholar]
- He, Y.; Li, N.; Wang, X.; He, M.; He, D. Comfort, energy efficiency and adoption of personal cooling systems in warm environments: A field experimental study. Int J. Environ. Res. Public Health 2017, 14, 1408. [Google Scholar] [CrossRef] [PubMed]
- Gagnon, D.; Romero, S.A.; Cramer, M.N.; Jay, O.; Crandall, C.G. Cardiac and thermal strain of elderly adults exposed to extreme heat and humidity with and without electric fan use. JAMA 2016, 316, 989–991. [Google Scholar] [CrossRef]
- Jay, O.; Cramer, M.N.; Ravanelli, N.M.; Hodder, S.G. Should electric fans be used during a heat wave? Appl. Ergon. 2015, 46 Pt A, 137–143. [Google Scholar] [CrossRef]
- Gupta, S.; Carmichael, C.; Simpson, C.; Clarke, M.J.; Allen, C.; Gao, Y.; Chan, E.Y.Y.; Murray, V. Electric fans for reducing adverse health impacts in heatwaves. Cochrane Database Syst. Rev. 2012, 7, CD009888. [Google Scholar] [CrossRef]
- Gao, C.; Kuklane, K.; Wang, F.; Holmér, I. Personal cooling with phase change materials to improve thermal comfort from a heat wave perspective. Indoor Air 2012, 22, 523–530. [Google Scholar] [CrossRef] [PubMed]
- Pan, C.S.; Chiang, H.C.; Yen, M.C.; Wang, C.C. Thermal comfort and energy saving of a personalized PFCU air-conditioning system. Energy Build. 2005, 37, 443–449. [Google Scholar] [CrossRef]
- Kuklane, K. An approach with 2 phase changes (PCM+) improves and prolongs the cooling effect. In Proceedings of the 7th European Conference on Protective Clothing, Izmir, Turkey, 23–25 May 2016. [Google Scholar]
- El Hourani, M.; Ghali, K.; Ghaddar, N. Effective desiccant dehumidification system with two-stage evaporative cooling for hot and humid climates. Energy Build. 2014, 68, 329–338. [Google Scholar] [CrossRef]
- Keitsch, M. Sustainable architecture, design and housing. Sustain. Dev. 2012, 20, 141–145. [Google Scholar] [CrossRef]
- Givoni, B. Climate Considerations in Building and Urban Design; John Wiley and Sons: New York, NY, USA, 1998. [Google Scholar]
- Ng, E. Policies and technical guidelines for urban planning of high-density cities—Air ventilation assessment (AVA) of Hong Kong. Build. Environ. 2009, 44, 1478–1488. [Google Scholar] [CrossRef]
- Johansson, E.; Spangenberg, J.; Lino Gouvêa, M.; Freitas, E.D. Scale-integrated atmospheric simulations to assess thermal comfort in six different urban tissues in the warm humid summer of São Paulo, Brazil. Urban Clim. 2013, 6, 24–43. [Google Scholar] [CrossRef]
- Yahia, M.W.; Johansson, E. Landscape interventions in improving thermal comfort in the hot dry city of Damascus, Syria—The example of residential spaces with detached buildings. Landsc. Urban Plan. 2014, 125, 1–16. [Google Scholar] [CrossRef]
- Wilhite, H. The conditioning of comfort. Build. Res. Inf. 2009, 37, 84–88. [Google Scholar] [CrossRef]
- Mirchandani, H.G.; McDonald, G.; Hood, I.C.; Fonseca, C. Heat-related deaths in Philadelphia—1993. Am. J. Forensic Med. Pathol. 1996, 17, 106–108. [Google Scholar] [CrossRef]
- Vandentorren, S.; Bretin, P.; Zeghnoun, A.; Mandereau-Bruno, L.; Croisier, A.; Cochet, C.; Ribéron, J.; Siberan, I.; Declercq, B.; Ledrans, M. August 2003 heat wave in France: Risk factors for death of elderly people living at home. Eur. J. Public Health 2006, 16, 583–591. [Google Scholar] [CrossRef] [PubMed]
- Chen, F.; Wittkopf, S.K.; Ng, P.K.; Du, H. Solar heat gain coefficient measurement of semi-transparent photovoltaic modules with indoor calorimetric hot box and solar simulator. Energy Build. 2012, 53, 74–84. [Google Scholar] [CrossRef]
- Hilliaho, K.; Nordquist, B.; Wallentén, P.; Hamid, A.A.; Lahdensivu, J. Energy saving and indoor climate effects of an added glazed façade to a brick wall building: Case study. J. Build. Eng. 2016, 7, 246–262. [Google Scholar] [CrossRef]
- Alawadi, E.M. Using phase change materials in window shutter to reduce the solar heat gain. Energy Build. 2012, 47, 421–429. [Google Scholar] [CrossRef]
- Chua, K.J.; Chou, S.K.; Yang, W.M.; Yan, J. Achieving better energy-efficient air conditioning—A review of technologies and strategies. Appl. Energy 2013, 104, 87–104. [Google Scholar] [CrossRef]
- Desideri, U.; Proietti, S.; Sdringola, P. Solar-powered cooling systems: Technical and economic analysis on industrial refrigeration and air-conditioning applications. Appl. Energy 2009, 86, 1376–1386. [Google Scholar] [CrossRef]
- Ghazali, A.M.; Malek, A.; Rahman, A. The Performance of Three Different Solar Panels for Solar Electricity Applying Solar Tracking Device under the Malaysian Climate Condition. Energy Environ. Res. 2012, 2, 235–243. [Google Scholar] [CrossRef]
- Allouhi, A.; Kousksou, T.; Jamil, A.; Bruel, P.; Mourad, Y.; Zeraouli, Y. Solar driven cooling systems: An updated review. Renew. Sustain. Energy Rev. 2015, 44, 159–181. [Google Scholar] [CrossRef]
- Gang, W.; Weng, S.; Xiao, F. District cooling systems and individual cooling systems: Comparative analysis and impacts of key factors. Sci. Technol. Built Environ. 2017, 23, 241–250. [Google Scholar] [CrossRef]
- Jusuf, K.S.; Wong, N.H.; Hagen, E.; Anggoro, R.; Hong, Y. The influence of land use on the urban heat island in Singapore. Habitat Int. 2007, 31, 232–242. [Google Scholar] [CrossRef]
- Trygg, L.; Amiri, S. European perspective on absorption cooling in a combined heat and power system—A case study of energy utility and industries in Sweden. Appl. Energy 2007, 84, 1319–1337. [Google Scholar] [CrossRef]
- ESTIF (European Solar Thermal Industry Federation). Solar Cooling—State of the art. Key Issues for Renewable Heat in Europe (K4RES-H). 2010. Available online: http://www.estif.org/fileadmin/estif/content/policies/downloads/D23-solar-assisted-cooling.pdf (accessed on 20 March 2018).
- Lundgren, K.; Kjellstrom, T. Sustainability challenges from climate change and air conditioning use in urban areas. Sustainability 2013, 5, 3116–3128. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhou, G.; Lin, K.; Zhang, Q.; Di, H. Application of latent heat thermal energy storage in buildings: State-of-the-art and outlook. Build. Environ. 2007, 42, 2197–2209. [Google Scholar] [CrossRef]
- Silva, T.; Vicente, R.; Rodrigues, F. Literature review on the use of phase change materials in glazing and shading solutions. Renew. Sustain. Energy Rev. 2016, 53, 515–535. [Google Scholar] [CrossRef]
- Medina, M.A.; King, J.B.; Zhang, M. On the heat transfer rate reduction of structural insulated panels (SIPs) outfitted with phase change materials (PCMs). Energy 2008, 33, 667–678. [Google Scholar] [CrossRef]
- Aranda-Usón, A.; Ferreira, G.; López-Sabirón, A.M.; Mainar-Toledo, M.D.; Zabalza Bribián, I. Phase change material applications in buildings: An environmental assessment for some Spanish climate severities. Sci. Total Environ. 2013, 444, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Kylili, A.; Fokaides, P.A. Life Cycle Assessment (LCA) of Phase Change Materials (PCMs) for building applications: A review. J. Build. Eng. 2016, 6, 133–143. [Google Scholar] [CrossRef]
| Metabolic Rate (Class) | Metabolic Rate (W) | WBGT Reference Limit for Person Acclimatized to Heat (°C) | WBGT Reference Limit for Person Unacclimatized to Heat (°C) |
|---|---|---|---|
| Class 0 Resting metabolic rate | 115 | 33 | 32 |
| Class 1 Low metabolic rate | 180 | 30 | 29 |
| Class 2 Moderate metabolic rate | 300 | 28 | 26 |
| Class 3 High metabolic rate | 415 | 26 | 23 |
| Class 4 Very high metabolic rate | 520 | 25 | 20 |
| Adaptation Level | Example Actions |
|---|---|
| Behavioral | adjusting clothes and body movement such as posture and activity; - adjusting conditions including opening or closing of windows; - creating ventilation/draught; - taking a cold shower; - applying water on face/neck, hands or using wet towels; - adjusting the thermostat; - installing ceiling and table fans; - taking a siesta during the hottest hours of the day; - customizing cooking by the day and, for example, not using oven; - change blinds to block unwanted sunlight; - move between rooms (i.e. from kitchen to cooler areas such as a basement) [76,77]; - using ventilation solutions in clothing (described further in text below); - using personalized table fan cooling (described in the text below); |
| Physiological | - conduct regular physical exercise; - adopt a systematic heat exposure regime to induce acclimatization [48]. |
| Psychological | - create awareness of the thermal environment. Here, perceptions can be influenced by the individual’s previous thermal experiences and thus expectations of the building in which the person accommodates [78]. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lundgren Kownacki, K.; Gao, C.; Kuklane, K.; Wierzbicka, A. Heat Stress in Indoor Environments of Scandinavian Urban Areas: A Literature Review. Int. J. Environ. Res. Public Health 2019, 16, 560. https://doi.org/10.3390/ijerph16040560
Lundgren Kownacki K, Gao C, Kuklane K, Wierzbicka A. Heat Stress in Indoor Environments of Scandinavian Urban Areas: A Literature Review. International Journal of Environmental Research and Public Health. 2019; 16(4):560. https://doi.org/10.3390/ijerph16040560
Chicago/Turabian StyleLundgren Kownacki, Karin, Chuansi Gao, Kalev Kuklane, and Aneta Wierzbicka. 2019. "Heat Stress in Indoor Environments of Scandinavian Urban Areas: A Literature Review" International Journal of Environmental Research and Public Health 16, no. 4: 560. https://doi.org/10.3390/ijerph16040560
APA StyleLundgren Kownacki, K., Gao, C., Kuklane, K., & Wierzbicka, A. (2019). Heat Stress in Indoor Environments of Scandinavian Urban Areas: A Literature Review. International Journal of Environmental Research and Public Health, 16(4), 560. https://doi.org/10.3390/ijerph16040560






