Risk Factors for Non-Communicable Diseases at Baseline and Their Short-Term Changes in a Workplace Cohort in Singapore
Abstract
:1. Introduction
2. Materials and Methods
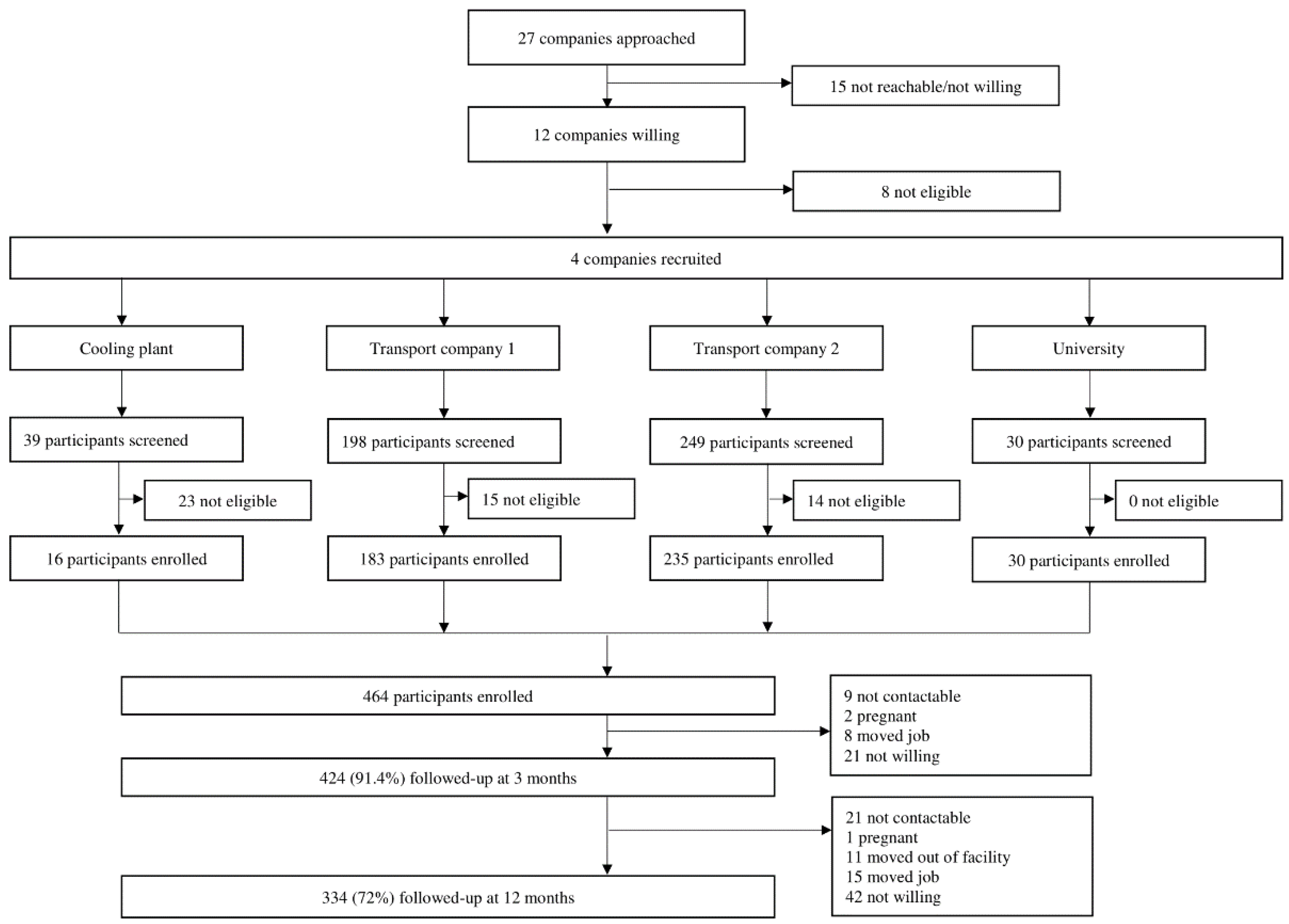
2.1. Study Design and Participants
2.2. Measurements
2.3. Definitions
2.3.1. Behavioural Risk Factors
2.3.2. Clinical Risk Factors
2.4. Statistical Analysis
2.5. Ethics Approval
3. Results
3.1. Behavioural and Clinical Risk Factors at Baseline
3.2. Changes in Risk Factors Over Three and 12 Months
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- NCD Countdown 2030 collaborators. NCD Countdown 2030: Worldwide trends in non-communicable disease mortality and progress towards Sustainable Development Goal target 3.4. Lancet 2018, 392, 1072–1088. [Google Scholar] [CrossRef]
- World Health Organization. Global Status Report on Noncommunicable Diseases 2014; World Health Organization: Geneva, Switzerland, 2014. [Google Scholar]
- Leon, D.A. Cities, urbanization and health. Int. J. Epidemiol. 2008, 37, 4–8. [Google Scholar] [CrossRef] [PubMed]
- International Diabetes Federation. IDF Diabetes Atlas, 8th ed.; International Diabetes Federation: Brussels, Belgium, 2017. [Google Scholar]
- Phan, T.P.; Alkema, L.; Tai, E.S.; Tan, K.H.; Yang, Q.; Lim, W.Y.; Teo, Y.Y.; Cheng, C.Y.; Wang, X.; Wong, T.Y.; et al. Forecasting the burden of type 2 diabetes in Singapore using a demographic epidemiological model of Singapore. BMJ Open Diabetes Res. Care 2014, 2, e000012. [Google Scholar] [CrossRef] [PubMed]
- Cahalin, L.P.; Kaminsky, L.; Lavie, C.J.; Briggs, P.; Cahalin, B.L.; Myers, J.; Forman, D.E.; Patel, M.J.; Pinkstaff, S.O.; Arena, R. Development and Implementation of Worksite Health and Wellness Programs: A Focus on Non-Communicable Disease. Prog. Cardiovasc. Dis. 2015, 58, 94–101. [Google Scholar] [CrossRef]
- Proper, K.; Mechelen, W. Effectiveness and Economic Impact of Worksite Interventions to Promote Physical Activity and Healthy Diet; World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- Ministry of Manpower Singapore. Explore Statistics and Publications. Available online: https://stats.mom.gov.sg/Pages/ExploreStatisticsPublications.aspx#PublicationSearch (accessed on 10 September 2019).
- Health Promotion Board, Singapore. National Population Health Survey (NPHS). Available online: https://www.hpb.gov.sg/community/national-population-health-survey (accessed on 25 May 2019).
- Health Promotion Board, Singapore. Health Promotion Board Annual Report 2017/2018; Health Promotion Board: Singapore, 2017/2018.
- World Health Organization. STEP Wise Approach to Surveillance (STEPS); World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Dunleavy, G.; Sathish, T.; Nazeha, N.; Soljak, M.; Visvalingam, N.; Bajpai, R.; Yap, H.S.; Roberts, A.C.; Quoc, T.T.; Tonon, A.C.; et al. Health Effects of Underground Workspaces (HEUW) cohort in Singapore: Study design and baseline characteristics. Epidemiol. Health 2019, 41. [Google Scholar] [CrossRef]
- Vosko, A.M.; Colwell, C.S.; Avidan, A.Y. Jet lag syndrome: Circadian organization, pathophysiology, and management strategies. Nat. Sci. Sleep 2010, 2, 187–198. [Google Scholar] [CrossRef]
- Health Promotion Board Singapore. National Health Survey 2010; Health Promotion Board: Singapore, 2010.
- Chiuve, S.E.; Fung, T.T.; Rimm, E.B.; Hu, F.B.; McCullough, M.L.; Wang, M.L.; Stampfer, M.J.; Willett, W.C. Alternative Dietary Indices Both Strongly Predict Risk of Chronic Disease. J. Nutr. 2012, 142, 1009–1018. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Hoffmann, G. Diet Quality as Assessed by the Healthy Eating Index, Alternate Healthy Eating Index, Dietary Approaches to Stop Hypertension Score, and Health Outcomes. J. Acad. Nutr. Diet. 2018, 118, 74–100. [Google Scholar] [CrossRef]
- Bull, F.C.; Maslin, T.S.; Armstrong, T. Global physical activity questionnaire (GPAQ): Nine country reliability and validity study. J. Phys. Act. Health 2009, 6, 790–804. [Google Scholar] [CrossRef]
- World Health Organization. Global Recommendations on Physical Activity for Health; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- World Health Organisation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004, 363, 157–163. [Google Scholar] [CrossRef]
- World Health Organization. The Asia-Pacific Perspective: Redefining Obesity and Its Treatment; World Health Organization: Geneva, Switzerland, 2000. [Google Scholar]
- Sathish, T.; Kannan, S.; Sarma, S.P.; Razum, O.; Sauzet, O.; Thankappan, K.R. Seven-year longitudinal change in risk factors for non-communicable diseases in rural Kerala, India: The WHO STEPS approach. PLoS ONE 2017, 12, e0178949. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health, Singapore. Executive Summary on National Population Health Survey 2016/2017; Ministry of Health: Singapore, 2016/2017.
- Junghoon, K. Longitudinal Trend of Prevalence of Meeting Physical Activity Guidelines among Korean Adults. Exerc. Med. 2017, 1, 2. [Google Scholar]
- Yarborough, C.M., 3rd; Brethauer, S.; Burton, W.N.; Fabius, R.J.; Hymel, P.; Kothari, S.; Kushner, R.F.; Morton, J.M.; Mueller, K.; Pronk, N.P.; et al. Obesity in the Workplace: Impact, Outcomes, and Recommendations. J. Occup. Environ. Med. 2018, 60, 97–107. [Google Scholar] [CrossRef] [PubMed]
- Thankappan, K.R.; Sathish, T.; Tapp, R.J.; Shaw, J.E.; Lotfaliany, M.; Wolfe, R.; Absetz, P.; Mathews, E.; Aziz, Z.; Williams, E.D.; et al. A peer-support lifestyle intervention for preventing type 2 diabetes in India: A cluster-randomized controlled trial of the Kerala Diabetes Prevention Program. PLoS Med. 2018, 15, e1002575. [Google Scholar] [CrossRef] [PubMed]
- Urban, L.E.; Weber, J.L.; Heyman, M.B.; Schichtl, R.L.; Verstraete, S.; Lowery, N.S.; Das, S.K.; Schleicher, M.M.; Rogers, G.; Economos, C.; et al. Energy Contents of Frequently Ordered Restaurant Meals and Comparison with Human Energy Requirements and U.S. Department of Agriculture Database Information: A Multisite Randomized Study. J. Acad. Nutr. Diet. 2016, 116, 590–598. [Google Scholar] [CrossRef]
- Aune, D.; Giovannucci, E.; Boffetta, P.; Fadnes, L.T.; Keum, N.; Norat, T.; Greenwood, D.C.; Riboli, E.; Vatten, L.J.; Tonstad, S. Fruit and vegetable intake and the risk of cardiovascular disease, total cancer and all-cause mortality-a systematic review and dose-response meta-analysis of prospective studies. Int. J. Epidemiol. 2017, 46, 1029–1056. [Google Scholar] [CrossRef]
- Finer, N. Medical consequences of obesity. Medicine 2006, 34, 510–514. [Google Scholar] [CrossRef]
- Emberson, J.R.; Whincup, P.H.; Morris, R.W.; Wannamethee, S.G.; Shaper, A.G. Lifestyle and cardiovascular disease in middle-aged British men: The effect of adjusting for within-person variation. Eur. Heart J. 2005, 26, 1774–1782. [Google Scholar] [CrossRef]
- Goettler, A.; Grosse, A.; Sonntag, D. Productivity loss due to overweight and obesity: A systematic review of indirect costs. BMJ Open 2017, 7, e014632. [Google Scholar] [CrossRef]
- Watanabe, K.; Kawakami, N.; Otsuka, Y.; Inoue, S. Associations among workplace environment, self-regulation, and domain-specific physical activities among white-collar workers: A multilevel longitudinal study. Int. J. Behav. Nutr. Phys. Act. 2018, 15, 47. [Google Scholar] [CrossRef]
- Inoue, M.; Toyokawa, S.; Inoue, K.; Suyama, Y.; Miyano, Y.; Suzuki, T.; Miyoshi, Y.; Kobayashi, Y. Lifestyle, weight perception and change in body mass index of Japanese workers: MY Health Up Study. Public Health 2010, 124, 530–537. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.; Buys, N.; Wang, X. Effectiveness of a workplace-based intervention program to promote mental health among employees in privately owned enterprises in China. Popul. Health Manag. 2013, 16, 406–414. [Google Scholar] [CrossRef] [PubMed]
- Nakao, M.; Nishikitani, M.; Shima, S.; Yano, E. A 2-year cohort study on the impact of an Employee Assistance Programme (EAP) on depression and suicidal thoughts in male Japanese workers. Int. Arch. Occup. Environ. Health 2007, 81, 151–157. [Google Scholar] [CrossRef] [PubMed]
- Thankappan, K.R.; Shah, B.; Mathur, P.; Sarma, P.S.; Srinivas, G.; Mini, G.K.; Daivadanam, M.; Soman, B.; Vasan, R.S. Risk factor profile for chronic non-communicable diseases: Results of a community-based study in Kerala, India. Indian J. Med. Res. 2010, 131, 53–63. [Google Scholar]
| Characteristics | N = 464 |
|---|---|
| Age (years), n (%) | |
| 21–30 | 153 (33.0) |
| 31–40 | 121 (26.1) |
| >40 | 190 (40.9) |
| Men, n (%) | 369 (79.5) |
| Ethnicity, n (%) | |
| Chinese | 296 (63.8) |
| Malays | 99 (21.3) |
| Indians | 48 (10.3) |
| Others a | 21 (4.5) |
| Education, n (%) | |
| Primary and secondary | 49 (10.6) |
| Pre-college | 250 (53.9) |
| College and above | 165 (35.6) |
| Monthly income, n (%) | |
| <S$4000 | 331 (71.3) |
| ≥S$4000 | 133 (28.7) |
| Marital status, n (%) | |
| Single b | 184 (39.7) |
| Married | 280 (60.3) |
| Years employed in the current company, median (IQR) | 3 (1–7) |
| Work location, n (%) | |
| Underground | 142 (30.6) |
| Aboveground | 322 (69.4) |
| Job type, n (%) | |
| Control room staff | 140 (30.2) |
| Office staff | 225 (48.5) |
| Workshop staff | 99 (21.3) |
| Job category, n (%) | |
| Managers and admin personnel | 112 (24.1) |
| Engineers, technicians, and traffic controllers | 334 (72.0) |
| Customer service | 18 (3.9) |
| Work hours/week, mean (SD) | 42.8 (6.4) |
| Shift work (yes), n (%) | 166 (35.8) |
| Risk factors | N = 464 |
|---|---|
| Behavioural risk factors | |
| Current smoker a, n (%) | 113 (24.4) |
| Alcohol use (in the last 12 months) b, n (%) | 248 (53.5) |
| Total minutes of physical activity/week, median (IQR) | 375 (120–900) |
| Physically inactive c, n (%) | 107 (23.1) |
| Sedentary behaviour (hours/day) d, mean (SD) | 6.7 (3.7) |
| Fruit and vegetable servings/day e, median (IQR) | 3.6 (2.2–5.6) |
| <5 servings of fruit and vegetables/day, n (%) | 306 (66.0) |
| AHEI-2010 score, mean (SD) | 22.7 (8.3) |
| Clinical risk factors | |
| Weight (kg), mean (SD) | 72.8 (17.2) |
| BMI (kg/m2), mean (SD) | 25.6 (5.2) |
| Overweight or obesity f, n (%) | 311 (67.0) |
| Central obesity g, n (%) | 160 (34.5) |
| Continuous variables | Age-adjusted mean change (95% CI) from baseline to three months | p | Age-adjusted mean change (95% CI) from baseline to 12 months | p |
| AHEI-2010 score | 0.60 (−0.26 to 1.47) | 0.17 | 0.78 (−0.18 to 1.73) | 0.11 |
| Fruit and vegetable servings/day a | −0.12 (−0.37 to 0.12) | 0.32 | −0.12 (−0.47 to 0.24) | 0.52 |
| Total minutes of physical activity/week | −240.7 (−407.4 to −74.1) | 0.001 | −290.3 (−459.7 to −120.8) | <0.001 |
| Sedentary behaviour (hrs/day) b | −0.20 (−0.51 to 0.10) | 0.19 | 0.10 (−0.21 to 0.42) | 0.53 |
| Weight (kg) | 0.23 (0.03 to 0.43) | 0.024 | 0.50 (0.25 to 0.75) | <0.001 |
| BMI (kg/m2) | 0.08 (0.01 to 0.14) | 0.031 | 0.15 (0.06 to 0.23) | 0.001 |
| Categorical variables | Odds ratio (95% CI) | p | Odds ratio (95% CI) | p |
| Current smoker c | 0.92 (0.85 to 1.01) | 0.07 | 1.03 (0.94 to 1.13) | 0.55 |
| Alcohol use (in the last 12 months) d,* | -- | -- | 0.86 (0.73 to 1.00) | 0.05 |
| <5 servings of fruit and vegetables/day | 1.14 (0.91 to 1.44) | 0.25 | 1.33 (1.03 to 1.73) | 0.030 |
| Physically inactive e | 1.40 (1.10 to 1.79) | 0.006 | 1.64 (1.25 to 2.14) | <0.001 |
| Overweight or obesity f | 1.01 (0.94 to 1.09) | 0.77 | 1.15 (1.02 to 1.29) | 0.018 |
| Central obesity g | 1.05 (0.91 to 1.21) | 0.49 | 1.14 (0.96 to 1.35) | 0.13 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sathish, T.; Dunleavy, G.; Soljak, M.; Visvalingam, N.; Nazeha, N.; Divakar, U.; Bajpai, R.; Thach, T.-Q.; Cheung, K.L.; Vries, H.d.; et al. Risk Factors for Non-Communicable Diseases at Baseline and Their Short-Term Changes in a Workplace Cohort in Singapore. Int. J. Environ. Res. Public Health 2019, 16, 4551. https://doi.org/10.3390/ijerph16224551
Sathish T, Dunleavy G, Soljak M, Visvalingam N, Nazeha N, Divakar U, Bajpai R, Thach T-Q, Cheung KL, Vries Hd, et al. Risk Factors for Non-Communicable Diseases at Baseline and Their Short-Term Changes in a Workplace Cohort in Singapore. International Journal of Environmental Research and Public Health. 2019; 16(22):4551. https://doi.org/10.3390/ijerph16224551
Chicago/Turabian StyleSathish, Thirunavukkarasu, Gerard Dunleavy, Michael Soljak, Nanthini Visvalingam, Nuraini Nazeha, Ushashree Divakar, Ram Bajpai, Thuan-Quoc Thach, Kei L Cheung, Hein de Vries, and et al. 2019. "Risk Factors for Non-Communicable Diseases at Baseline and Their Short-Term Changes in a Workplace Cohort in Singapore" International Journal of Environmental Research and Public Health 16, no. 22: 4551. https://doi.org/10.3390/ijerph16224551
APA StyleSathish, T., Dunleavy, G., Soljak, M., Visvalingam, N., Nazeha, N., Divakar, U., Bajpai, R., Thach, T.-Q., Cheung, K. L., Vries, H. d., Soh, C.-K., Christopoulos, G., & Car, J. (2019). Risk Factors for Non-Communicable Diseases at Baseline and Their Short-Term Changes in a Workplace Cohort in Singapore. International Journal of Environmental Research and Public Health, 16(22), 4551. https://doi.org/10.3390/ijerph16224551







